Diabetes as a worldwide epidemic
Type II diabetes mellitus (T2DM) has become a worldwide epidemic. From an estimated 2.8% global prevalence (171 million persons) in 2000, its prevalence rose to 347 million cases in 20081 and is expected to rise up 5.3% (438 million cases) by 20302,3. Once thought to be related to affluence and development, countries in the process of economic development now face the largest burden from diabetes2,4. Diabetes poses an enormous public health burden, accounting for 11.6% of global health spending and 6.8% of global all-cause mortality5. Undiagnosed diabetes, more serious in developing countries with limited surveillance resources and more extensive rural areas with reduced healthcare access, worsens the burden6. Undiagnosed diabetes was 3.5 times more prevalent in low socio-economic status groups than in high7. Income-related health disparities are particularly important in developing countries or Indigenous populations. Diabetes prevalence is exhibits considerable ethnic disparities4,8. Diagnosed diabetes among US Hispanics and non-Hispanic Blacks was twice the rate of non-Hispanic Whites6,9. Similarly, total diabetes was higher among Hispanic than non-Hispanic White populations in 46 states, with undiagnosed diabetes higher among Hispanics in all 50 states10.
Many anthropologists have been concerned with the high prevalence of diabetes among Indigenous peoples worldwide11-14. Yet prior to the 20th century, diabetes was virtually unknown among Indigenous peoples11-13,15. The dramatic rise occurred within the span of several decades: Australian Aborigines in 1932, Pima Indians between 1937 and 1954, and American Indian and First Nations peoples in the 1940s11-13,15-18. By 1987, most Indigenous populations had diabetes prevalence and diabetes mortality rates several times higher than comparable Caucasian populations11,12.
Diabetes is a complex multi-factorial disorder19, with genetic19 and environmental11,12,20,21 determinants. Anthropologists have often tended to favor one or the other side, biomedical or cultural, as the predominant explanation. Medical anthropologists are concerned with the subjective lived experience of people with diabetes and the ways bodily illnesses reflect sociocultural power relationships4,22,23. However, biological anthropologists have often favored unidentified 'thrifty genotype' genetic susceptibilities among Indigenous peoples to explain their high prevalence of diabetes11,12,24,25.
Statistical evidence from genome-wide association studies has implicated numerous regions in elevated diabetes risk26. However, independent replication rates are very low and causal variants remain unknown26,27. The rapid (<2-3 generations) emergence of diabetes does seem incongruous with a common genetic etiology for 300 million Indigenous people in thousands of cultures across the globe28,29.
The drastic rise in diabetes prevalence among Indigenous peoples in the 20th century seems more likely to be explained by known social factors than unknown genetic risks19,22,28,30,31. An understanding of culturally constructed models of diabetes causality is necessary for designing effective public health interventions32,33. And an exclusive focus on subjective experience risks overlooking known biomedical determinants of diabetes22. A middle way is suggested that incorporates both biological and cultural stress and stressors in diabetes etiology22,34.
This article is a review of the anthropological literature on the prevalence and incidence of diabetes in modernizing populations from an anthropological perspective. This review focuses on the role of psychosocial stress, broadly conceived as modifiable behavioral or social determinants, in environments characterized by modernization and economic development.
Definitions and measures of stress
The human stress response stems from the body's reaction to physical, biotic, and/or sociocultural stimuli resulting in the need to appraise adaptive activity34. Contemporary stress research derives from Hans Selye, who recognized that stress has both adaptive and destructive effects and proposed to measure stress by hormones that maintain or disturb physiological homeostasis35. Stressors included both internal (nervous tension) and external (infectious) factors, and could cause both specific (affecting particular bodily systems) and non-specific (whole-body) responses35. Stressors could be bad (distress), which can lead to exhaustion and ill health, or good (eustress), which provides a healthy level of tension.
The vague definition of stress as wear and tear on the body, made it difficult to measure the effects of stress on health35-38. But the theoretic distinction between stress as a psychophysical state, and stressors as noxious environmental stimuli, allowed study of external social stressors, subjective mental or emotional states, and their relationship36-38. Since homeostasis was maintained by the neuroendocrine system, stress could be measured objectively by hormones of the hypothalamic-pituitary-adrenal (HPA) axis, and disturbed homeostasis could increase disease susceptibility36,38. Chronic stress resulted in fatigue, led to exhaustion, reduced resistance and increased ill health due to disturbed homeostasis and eventually caused disease or death39. This notion of allostasis contrasts to homeostasis and refers to an alternative but dysfunctional physiological set point induced by various stressors including aging and measured by various biomarkers40,41.
The following operational definitions are used in this article:
- Physiological stress refers to the general adaptation response involving the HPA axis and is measured by levels of 'stress hormones' (adrenalin, norepinephrine, cortisol) that underlie the human body's adaptive response to external stimuli.
- Psychological stress refers to subjectively perceived mental or emotional states, as measured by various survey instruments, open-ended interviews or other self-reports.
- Psychosocial stress refers to objective measures of external sociocultural stressors associated with modernization or acculturation, including socioeconomic status, lifestyle incongruence (LI), urbanization, chronic (migration, trauma) or acute (familial or work-place conflicts) stressors, changes to traditional lifestyles (diet, physical activity) and environmental stressors (toxins, extreme weather events). These stressors are similar to the social determinants of health studied by public health practitioners42.
- Nutritional stress refers to under-nutrition, over-nutrition or malnutrition, particularly in the perinatal period, as it pertains to Barker's theory of the developmental origins of chronic disease20,25.
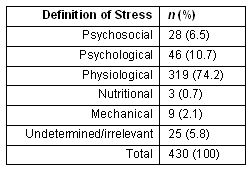
A literature review was performed in PubMed using the MeSH search terms 'diabetes' in [title] and 'stress' [text]. The initial search identified 3702 articles. A review of the 430 most recent (March 2009-March 2011) articles revealed that 74% of the articles concerned physiological stress (Table 1). However, most of these (192 articles, or 60% of the category and 45% of the total) concerned oxidative stress and only 6 (1.8% of the category and 1.4% of the total) concerned the HPA axis or the physiological stress response. A review of these abstracts identified 83 articles of potential interest. Refinement of this literature search, by adding the terms 'anthropological' or 'anthropology' or 'ethnographic' or 'indigenous' in the text, reduced results to 35 articles. Of these, only 5 articles were of potential interest, 2 of which were used here22,43. A subsequent refinement added the search terms 'Hispanic' or 'Mexican-American' or 'Mexican' in the text and returned 3 articles, none of which were pertinent to this topic. These meager results indicated that a formal literature search using PubMed was inadequate to the task.
Table 1: Multiple definitions of stress identified in PubMed search ('diabetes'[title] AND 'stress'[all fields]), by count and percentage.
 Due to these limitations, three additional procedures were incorporated to identify pertinent literature. First, similar searches were conducted on GoogleScholar: 'diabetes' and 'stress' in the title returned 2010 references, while 'diabetes' and 'anthropology' in the title returned 4 articles, one of which was used here44. Second, abstracts of the 83 PubMed articles were reviewed and the 2010 GoogleScholar references were browsed to determine their relevance to the research question. Third, it was quickly determined that a better method to identify pertinent historical and recent studies was to use a combination of snowball sampling from the bibliographies of found references22,44,45, and opportunistic sampling from PubMed when retrieving known abstracts, to identify further substantive articles of interest.
Due to these limitations, three additional procedures were incorporated to identify pertinent literature. First, similar searches were conducted on GoogleScholar: 'diabetes' and 'stress' in the title returned 2010 references, while 'diabetes' and 'anthropology' in the title returned 4 articles, one of which was used here44. Second, abstracts of the 83 PubMed articles were reviewed and the 2010 GoogleScholar references were browsed to determine their relevance to the research question. Third, it was quickly determined that a better method to identify pertinent historical and recent studies was to use a combination of snowball sampling from the bibliographies of found references22,44,45, and opportunistic sampling from PubMed when retrieving known abstracts, to identify further substantive articles of interest.
Study limitations
The main study limitation identified was the inadequacy of search engine results using PubMed and GoogleScholar. While this approach can be a good starting point for systematic reviews of biomedical topics, it was inadequate to identify a sufficient number of references on the desired topic. Another limitation was the multi-dimensional and often incompatible definitions of stress used across a wide range of studies, which resulted in large numbers of irrelevant hits in both Pubmed and GoogleScholar. Finally, the number of studies identified that address T2DM as related to stress in ethnic populations or anthropological perspectives was limited.
Theories about stress and chronic disease
Psychosocial stress and chronic disease: The very diversity of studies on stress and diabetes (Table 1) suggested a need to better characterize and categorize the nature of stress and help ensure better comparability among studies46. Two major theoretical perspectives on chronic diseases and stress were identified: psychosocial stress (sociocultural and psychological) and biomedical stress (physiological or hormonal and nutritional). Theories on stress and chronic disease distinguish between subjectively perceived stress (a private mental or emotional state), external factors that induce stress (sociocultural stressors),physiological changes involving the HPA axis that underlie behavioral responses to stressors, and nutritional stress2,21,36-38. Psychosocial stress can be psychological (subjective psycho-emotional states) or sociocultural (social support, financial issues, chronic familial or workplace conflict, acute traumatic events). Psychological stress, as subjective psycho-emotional states (anxiety, depression) can be inferred from verbal reports, written questionnaires or open-ended interviews. The impact of stress can vary depending on personality, interpretation, social support and coping style36,37,47-49. The sociocultural context and cultural meaning of events can influence how psychosocial stressors are interpreted47,49,50. Psychological stress can affect health status by increasing behavioral risk factors, such as tobacco or alcohol consumption51,52.
Physiological stress can be measured by levels of stress hormones (adrenalin, norepinephrine and cortisol)51. Persistent elevation of stress hormones in people exposed to social situations normatively described as 'stressful' (including spousal loss, workload and migration) suggested a connection between subjective psycho-emotional states and their social causes51. Stress hormones can increase diabetes risk by stimulating release of glucose or insulin and lead to obesity and hyperinsulinemia11,51.
Stressors themselves can be chronic (everyday stress) or acute (migration, traumatic life events), and either sociocultural (including environmental) or nutritional in nature2,46,47. Excessive chronic stress can eventually lead to emotional, physical, and behavioral breakdown39. Social stressors included crowding, occupational mobility, social isolation, family breakdown, migration, urbanization and economic development36-38. Acute stressors are traumatic events that demand psychological, behavioral or social readjustment, such as migration, divorce or job loss48,49. Chronic stressors derived from discord related to routine social roles, including family, job, marriage or money48,49. Specific psychosocial stressors were related to health outcomes in modernization49,50. It has been argued that the stress of modernization differs from both acculturation (Western education, speaking English) and biomedical risk factors (diet, obesity, physical activity)48-50,53. Specifically, lifestyle incongruence is the disjunction between people's desired socioeconomic status and their actual attainment and can lead to chronic disease48,49. Lifestyle incongruence is primarily a theory of consumption during modernization9,49,50.
These theoretical developments provided a research focus for studies of stress and diabetes and indicated a need to measure a variety of stress processes or social stressors37,38. In Cassell's theory, social stressors produce non-specific effects on health36-38. This lack of etiological specificity meant that there are no 'stress diseases' but only altered incidences of routine diseases due to stress36-38. Consequently, all disease outcomes (rather than particular diseases of interest) must be studied to characterize the effects of exposure to social stressors37.
Nutritional stress and chronic disease: Nutritional stress is another stress theory related to modernization. The developmental origins of chronic disease postulates that perinatal malnutrition leads to chronic disease in adulthood. Fetuses adapt in utero to their nutritional milieu, as determined by maternal condition and diet during pregnancy and previous nutritional experience54,55. The fetus responds to under-nutrition by altering changing hormone production, tissue sensitivity to hormones, and growth rates. The result is reduced fetal growth rates, low birth weight (LBW), stunting, reduced rates of postnatal growth, and altered organ/body weight ratios55. The timing of malnutrition can impact different organs differently, depending on critical growth periods affected55. Therefore, unlike psychosocial stress, nutritional stress can induce etiological specificity.
The developmental origins model proposed that diabetes can be a long-term consequence of the hormonal changes induced by maternal malnutrition20,21. This model proposed that early-life malnutrition led to decreased fetal insulin, insulin-like growth factors and glucose which control fetal growth, thus leading to reduced fetal growth rates and permanently altered insulin and glucose metabolism20,55. The thrifty phenotype hypothesis posits fetal and early life malnutrition impose nutritional thrift upon the individual, leading to impaired pancreas development and increased susceptibility to T2DM20,21. Low birth weight also induces pre-diabetic traits of high blood glucose and insulin, insulin resistance, and impaired beta cell function30,56-59. Subsequent childhood over-nutrition resulted in accelerated childhood growth insulin resistance, glucose intolerance, obesity and T2DM diabetes in later life20,21,60. Offspring glucose and insulin levels were associated with low maternal BMI independently of offspring birth weight55,60. The developmental origins model postulates that prenatal nutritional stress permanently altered physiological and metabolic pathways. Subsequent nutritional stress, including obesity and nutritionally poor diets, can lead to T2DM in mid-life61.
Epidemiological studies have suggested that adult non-communicable chronic diseases have a host of determinants, from genetic and adult lifestyle factors to environmental factors acting in early life62. In summary, psychosocial stress in conjunction with nutritional deficits can potentially explain the diabetes epidemic in modernizing countries and among Indigenous peoples worldwide.
Anthropological literature on modernization, stress and diabetes
Theories of psychosocial and nutritional stress and their impact on chronic disease are related to anthropological studies of modernization. Modernization is the process of economic and sociocultural change, by which traditional cultures industrialize and develop a capitalist economy characterized by division of labor, reduced importance of kinship, and changes in traditional lifestyles48,63,64. Modernization is related to increased chronic disease morbidity and mortality and is a major focus of contemporary medical anthropology48,65-67. The unique contribution of anthropological studies is that the global diabetes epidemic strongly impacts modernizing populations5,67 and occurs during the nutritional transition68,69 involving reduced physical activity, increased obesity and diets rich in processed carbohydrates1,20,70.
The real challenge in anthropological studies of diabetes is how to operationalize 'modernization'. Drastic lifestyle changes involving nutrition, activity patterns, residence, and psychosocial stress related to post-WWII modernization are related to diabetes among Indigenous peoples11,71. Urbanization is a composite variable for several aspects of modernization, including decreased physical activity, increased healthcare access, and differential access to Western foods72. Urbanization also correlates with access to wage-labor jobs and socioeconomic factors47,50. With some exceptions18,43,73, data to compare diabetes incidence or prevalence between Westernized and traditional Indigenous peoples are sparse12. Anthropologists have operationalized the lifestyle changes associated with modernization by measuring activity patterns, acculturation scales, affluence and consumption, dietary changes and nutrition, urbanization and other psychosocial factors11,18,71,73,74 (results in Table 2).
Psychological and physiological stress
Anthropological studies on subjective stress, though infrequent51, have been conducted74-77. Levels of epinephrine were higher in Westernized urban Samoans than in Samoans having a more traditional lifestyle as rural agriculturalists, but norepinephrine levels did not differ76,77. Rural villagers had higher levels of life satisfaction and emotional stability compared with urban Samoans, thus correlating stress hormone levels to subjective stress77. A study of Mexican-American migrant farm-workers in Wisconsin demonstrated associations between dopamine β hydroxylase (DBH, a norepinephrine precursor), acute stressors (familial separation, migration), and diabetic status78. A longitudinal study of children and young adults in the Dominican Republic demonstrated that several measures of chronic and acute household insecurity, especially poor maternal care, were associated with cortisol levels79.
Psychosocial stress
Overall lifestyle change: A generalized acculturation measure, including dietary change, anxiety and economic stress, was used to study cardiovascular disease (CVD) risk factors among rural Solomon Islands villagers80. Westernization was operationalized by a 12 point acculturation scale based on changes in culture (education, religion, access to Western medical care), diet (salt intake, Western foods), adult height (reflecting childhood nutrition) and economy (wage-labor jobs or swidden agriculturalists) changes80. They studied two risk factors for diabetes: obesity and hypertension. Acculturation was associated with hypertension, but not with obesity80.
The relationship between modernization and diabetes was studied in American Samoa81. The measure of modernization captured different degrees of participation in modern life, as measured by location of residence (modern, intermediate or traditional) and characterized by different degrees of connectedness to westernized areas (central harbor, paved roads, isolated rural areas)81. These locations also corresponded to differences in language, education, occupation and blood pressure (BP)81. Activity levels were categorized by occupational information recorded on health certificates81. More westernized males and those with more sedentary life-styles had elevated CVD-related mortality81. The effects of modernization on diabetes risk was not directly assessed, but there was a significantly higher age-adjusted incidence of diabetes-related mortality among Samoans (32.2 deaths/100 000 population) relative to the US (13.4 deaths/100 000)81.
Finally, 2 unspecified American Indian populations (Northern Plains, Southwest) were studied using a 25 item early-life traumatic events and a 30 item chronic stress instrument43. Results showed that diabetes in the Northern Plains population was associated with early-life trauma, while the Southwest population diabetes was associated with discrimination and community addiction problems43.
Lifestyle incongruence: Lifestyle incongruence refers to a discrepancy between material consumption (lifestyle) and economic means48. The effects of LI on BP in Western Samoa were studied using a 21 point scale for lifestyle/material possessions and an 8 point occupational scale82. For men, LI was associated with elevated systolic BP. For women, diastolic BP was higher when occupational rank exceeded lifestyle, the opposite of LI82. In American Samoa, LI also varied by sex83. The effects of modernization versus status incongruence on hypertension were directly compared in a Mexican community84. The modernization model predicted that stress accumulated with the degree of modernization and increased chronic disease risk84. Modern traits included wage-labor, Western education, urban residence, reduced kinship support network, and adoption of modern attitudes, behaviors and values84. They also measured subjectively perceived stress (anxiety, depression, life-satisfaction, recent life events, social support, tension and worry)85. The alternative explanation was lifestyle incongruence84,85. Results showed that systolic and diastolic BP increased with increasing modernization but not with LI84. Among the Mississippi Choctaw tribe, LI was associated with elevated non-fasting plasma glucose85, while psychological stress was associated with elevated diastolic BP85. These mixed results suggest that more research on the effects of LI and acculturation on diabetes is needed. Cultural factors may also modify the impact of lifestyle incongruence53.
Dietary change: The effects of traditional diet and dietary change, often conceptualized biomedically as adoption of a high-fat, high-carbohydrate, low-fiber diet, have been studied as a risk factor for diabetes among Indigenous peoples11,12,71. An interesting anecdote about the impact of refined carbohydrates on diabetes came from India in 1907. The earliest reported cases of diabetes occurred in areas near the first industrial rice mills, which removed most of the bran fiber from the grain71. By contrast, areas that continued to use traditional home-pounding of rice, which left half the bran fiber, had lower incidence of diabetes71.
Many traditional Australian Aboriginal, Pima Indians and Pacific islander foods protect against hyperglycemia by being digested more slowly than Western foods and result in lower levels of blood glucose and insulin86-88. Westernized diabetic Aborigines who temporarily (7 weeks) reverted to a traditional hunter-gatherer diet and lifestyle had improved blood glucose, insulin and triglycerides and reduced insulin resistance89. Pima Indians who ate a Western diet were 2.9 times more likely to develop diabetes, while those on a mixed diet were intermediate at 1.6 times more likely, compared with those eating a traditional diet88. Over-eating by non-diabetic Pima Indians increased plasma insulin90. Dietary changes among the Eastern Oklahoma Cherokee, including replacement of traditional beans, corn and squash with refined flours and a change from boiling or broiling to deep-frying, are thought responsible for the increase in diabetes prevalence, from 0% before 1941, to 13% in 197491. Traditional methods for processing wheat, including parboiling and baking whole grains, resulted in lower glycemic response compared to bread baked with industrially milled flours92. Unhealthy dietary changes often result from greater availability and affordability of energy rich, nutrition poor foods93. The increase in nutritional risk factors is an important factor in the increasing prevalence of diabetes and other chronic diseases in developing countries72.
The effects of acculturation and dietary factors on CVD risk factors were studied in Yaqui and Tepehuanos Indian communities in Mexico52,94. Diabetes was assessed as a CVD risk, along with obesity and triglycerides52. A 12 point acculturation scale was used and included language use, media exposure and social relations95. The Yaqui Indians were more acculturated than the Tepehuanos, who were subsistence farmers with a vegetarian diet until Western foods were introduced in 199894. The Yaqui were more obese (48% vs 7% prevalence), had more hypertriglyceridemia (15% vs 43% prevalence), less LDL-cholesterol (34% vs 42% prevalence), and a remarkable 22-fold higher prevalence of diabetes (18.3% vs 0.8%) than the more traditional Tepehuanos52. Impaired fasting glucose was higher among the Yaqui (17%) than the Tepehuanos (5%)52. Neither total daily energy consumption nor total fiber intake differed between groups, but they did differ in the energy derived from saturated fats (1412 Kj/day Yaqui, 978 Kj/day Tepehuanos)52. The Yaquis' higher diabetes prevalence was attributed to their higher saturated fat consumption52.
A 64 item food questionnaire was administered in 12 Yaqui communities at 2 time-points, 1994 (traditional vegetarian diet) and 2004 (Westernized diet) to assess total caloric intake and food proportions derived from protein, carbohydrates and saturated and unsaturated fats96. Traditional foods (green vegetables, bread, beans, potatoes and mixed-root tortillas, occasional meat) and Western foods (refined flours, canned foods, pasta, soft drinks, and 'junk' food) were compared94. In 10 years of follow up, dietary saturated fat doubled while unsaturated fats declined by 75%, fiber intake declined from 53 g/day to 49 g/day, and total caloric intake increased from 1476 KCal/day to 2100 KCal/day94. These dietary changes were associated with increased overweight/obesity (11% to 22%), hypertriglyceridemia (3% to 17%), impaired fasting glucose (6% to 15%), and decreased HDL (71% to 10%)94. Hypertension prevalence doubled from 2% to 4%, and metabolic syndrome increased from 0% to 10%, although diabetes prevalence did not change at 1%52,94. Acculturation among the Tepehuanos Indians was characterized by dietary changes involving increased consumption of calories and saturated fats, reduced fiber and was associated with an increased prevalence of risk factors94.
Physical activity change: Decreased energy expenditure is primary feature of lifestyle change during modernization that can lead to obesity and diabetes71. Historically recent (>1930s) changes in activity patterns among Oklahoma Cherokee involved decreased walking and increased reliance on vehicular transportation and were associated in time with increased diabetes-related mortality (from 0 cases in 1941 to 26.2/100 000 in 1977), which was 63% higher than Caucasian rates91. Most studies on the role of reduced physical activity as a diabetes risk factor concerned the Pima Indians. Questionnaires were used to estimate the amount of time spent in various activities96. Traditional Mexican Pimas had 23 h/wk of occupational physical activity, compared with 5 h/wk for more Westernized Arizona Pimas96. These differences corresponded to higher prevalence of diabetes among Arizona Pima (38.2%) than Mexican Pima (6.2%)96. A later study confirmed these results, with Arizona Pimas having physical activity of 3.1 h/wk (female) to 12.1 h/wk (male), compared with Mexican Pima females (22 h/wk) and males (32.9 h/wk)97.
Prenatal nutritional stress
The only anthropological studies concerning the developmental origins of diabetes were conducted on the Pima Indians. Several large studies examined the relationship between known birth weights and serum glucose or insulin levels98,99. Diabetes prevalence and 2 hour fasting glucose concentration had a U-shaped relationship with birth weight98,99. The LBW Pima were more insulin resistant, after controlling for weight and height98. The highest adult prevalence of diabetes (52.4%) was found in the lowest one-third (<2500 g) and the highest one-third (>4500 g) of birth weights. High prevalence among high birth weight (HBW) babies was attributed to gestational diabetes99. The LBW babies were 3.8 times more likely to have diabetes as adults, compared with middle birth weight babies99. Only approximately 6% of Pima babies were LBW and there was no evidence of maternal nutritional stress during pregnancy, making Barker's developmental model an incomplete explanation of the high (≥40%) adult diabetes prevalence99. The high prevalence of diabetes among LBW babies was attributed to selective survival of diabetes-prone LBW infants through an unknown genetic mechanism99. In another study, HBW Pima babies exhibited a dose-response relationship between extent of bottle feeding with cow's milk and adult diabetes prevalence100. Diabetes at age 30-39 years had 20% prevalence among Pima babies exclusively breast fed for at least 2 months, 25% prevalence among the cohort with some breast feeding, and 30% prevalence among those exclusively bottle fed with cow's milk100. Perinatal nutritional stress associated with later-life diabetes seemed related to nutritional overload of cow milk bottle-feeding, or possibly a missing nutrient specific to breast milk which affected infant insulin sensitivity100.
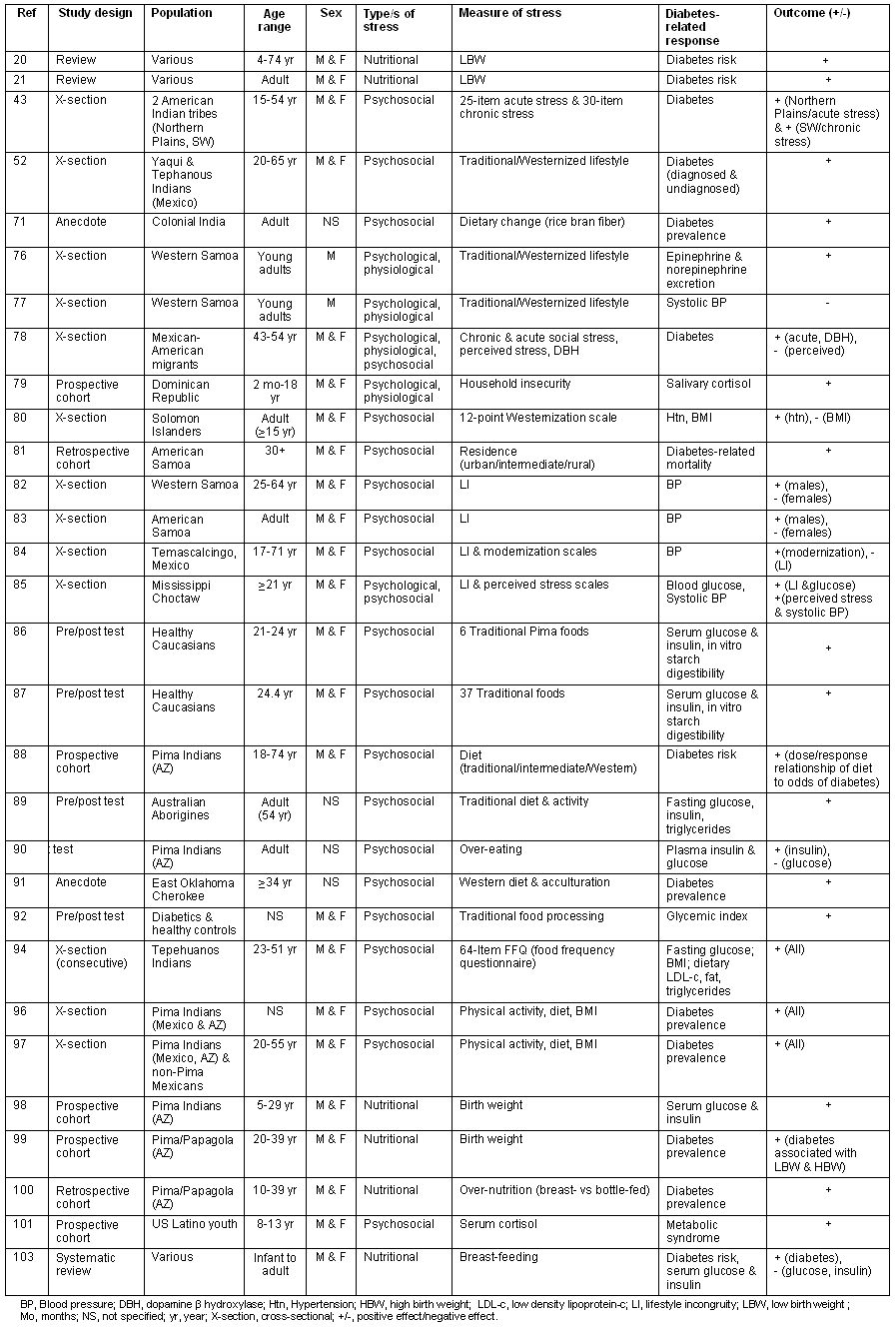
Table 2: Summary of ethnographic studies related to diabetes and stress20,21,43,52,71,76-92,94,96-102
A survey of the literature on stress and chronic disease identified four concepts of stress: physiological, psychological, psychosocial, and nutritional. To varying degrees, all are determinants of diabetes and should be studied in any comprehensive study. The anthropological survey demonstrated how studies of various anthropological populations undergoing modernization have operationalized stressors that influence diabetes risk. The remaining question of interest was how to measure modernization stressors in the US-Mexico border area, in order to study their influence on diabetes risk.
In fact, many of these stress concepts have empirical support in Hispanic populations. Hispanic youth with metabolic syndrome have higher serum cortisol than overweight healthy controls, as expected from physiological stress theory101. Acculturation measures in Hispanic populations are associated with reduced prevalence of breastfeeding103, which is associated with increased risk of diabetes in adulthood102, as suggested by the developmental origins model of diabetes20,21. Measures of modernization are associated with reduced dietary quality (decreased intake of fiber and fruit, and increased consumption of saturated fats and sugar) among diabetic Hispanics104,105. Hispanic household food insecurity is associated with increased consumption of poor-quality foods, including fats and sugar106. But no studies were found in the border area that addressed all four concepts of stress in diabetes etiology.
Several suggestions can be made for best practice. Throughout, the importance is underscored of a comprehensive view of stress and use of multiple indicators34,75. If blood samples can be collected, diabetes can be directly inferred by fasting glucose levels using established WHO criteria. Tissue sampling would also allow measurement of stress hormones (salivary cortisol, serum epinephrine). If blood sampling is not feasible, diabetes prevalence could be estimated by self-reporting (having been told by a physician that they are diabetic). Furthermore, the few available studies indicate that 'stress hormones' do not always measure stress76,77,79. In that regard, it may be inadvisable to collect tissues at all. Biomedical risk factors should be measured, including diet (by 24 hour recall or food frequency questionnaires [FFQs]), physical activity levels (to assess work and leisure activity patterns)104. Surveys should address the presence of barriers and motivating factors for increased physical activity107. Obesity (BMI) can be measured using basic anthropometry (height and weight) in either clinical or field situations. Lifestyle incongruence can be inferred using Dressler's instrument50. Childhood nutritional stress can be estimated by parental recall106, which is reliable up to 42 years later102. It can also be retrospectively estimated in adults by measurement of adult leg length (the difference between height and seated height)108-110. Acculturation can be measured by uni-dimensional scales, like the Short Acculturation Scale (SAS), which utilizes the single dimension of language use95 Such uni-dimensional acculturation scales have been criticized because culture is more than language, culture change is not identical to stress, and changes in diet and physical activity do not fully explain the increased risk of chronic disease encountered during modernization49,50,85,111. Multidimensional scales, like the Acculturation Rating Scale for Mexican Americans-Revised (ARMSA II), also measure the attitudes, beliefs, values and behaviors that constitute the actual processes of cultural change, while still incorporating language and social factors like immigration status and length of residence112-114.
Conclusion
In the authors' view, lifestyle changes, multidimensional acculturation scales, FFQs, subjective stress instruments115, and anthropometry are needed to fully assess the impact of stress as a determinant of diabetes. This knowledge can be used to design more effective public health interventions and accurately target diabetes prevention efforts toward individuals at greatest risk of developing diabetes in the US-Mexico border area or similar modernizing populations.
References
1. Danaei G, Finucane MM, Lin JK, Singh GM, Paciorek CJ, Cowan MJ et al, Burden of Metabolic Risk Factors of Chronic Diseases Collaborating Group (Blood Pressure). National, regional, and global trends in systolic blood pressure since 1980: systematic analysis of health examination surveys and epidemiological studies with 786 country-years and 5·4 million participants. Lancet 2011; 377(9765): 568-577.
2. International Diabetes Federation. Diabetes Atlas 2010. International Diabetes Federation, Brussels, Belgium. (Online) 2009. Available: http://www.diabetesatlas.org/content/prevalence-estimates-diabetes-mellitus-dm-2010 (Accessed 30 June 2010).
3. Wild S, Roglic G, Green A, Sicree R, King H. Global prevalence of diabetes. Estimates for the year 2000 and projections for 2030. Diabetes Care 2004; 27(5): 1047-1053.
4. Mendenhall E, Seligman RA, Fernandez A, Jacobs EA. Speaking through diabetes: rethinkign the significance of lay discourse on diabetes. Medical Anthropology Quareterly. 2010; 24(2): 220-239.
5. Colagiuri R. Diabetes: a pandemic, a development issue or both? Expert Reviews in Cardiovascular Therapy 2010; 8(3): 305-309.
6. Cowie CC, Rust KF, Ford ES, Eberhardt MS, Byrd-Holt DD, Li C et al. Full accounting of diabetes and pre-diabetes in the U.S. population in 1988-1994 and 2005-2006. Diabetes Care 2009; 32(2): 287-294.
7. Fisher-Hoch SP, Rentfro AR, Salinas JJ, Pérez A, Brown HS, Reininger BM et al. Socioeconomic status and prevalence of obesity and diabetes in a Mexican American community, Cameron County, Texas, 2004-2007. Preventing Chronic Disease 2010; 7(3): A53.
8. Beard HA, Al Ghatrif M, Samper-Ternent F, Gerst K, Markides KS. Trends in diabetes prevalence and diabetes-related complications in older Mexican-Americans from 1993-1994 to 2004-2005. Diabetes Care 2010; 32(12): 2212-2217.
9. Cowie CC, Rust KF, Byrd-Hold DD, Gregg EW, Ford ES, Geiss LS et al. Prevalence of diabetes and high risk for diabetes using A1c criteria in the U.S. population in 1988-2006. Diabetes Care 2010; 33(3): 562-568.
10. Danaei G, Friedman AB, Oza S, Murray CJL, Ezzati M. Diabetes prevalence and diagnosis in US states: analysis of health surveys. Population Health Metrics 2009; 7:16.
11. Szathmary E. Non-insulin dependent diabetes mellitus among aboriginal North Americans. Annual Review of Anthropology 1994; 23: 457-482.
12. Young TK. Diabetes mellitus among Native Americans in Canada and the United States: an epidemiological review. American Journal of Human Biology 1993; 5(4): 399-413.
13. Young TK. The health of Native Americans. Toward a biocultural epidemiology. New York: Oxford University Press, 1994.
14. Ferreira ML, Lang GC (Eds). Indigenous peoples and diabetes. Durham, NC: Carolina Academic, 2005.
15. O'Dea K. Diabetes in Australian aborigines: impact of the western diet and life style. Journal of Internal Medicine 1992; 232(2): 303-317.
16. Bennett PH. Type 2 diabetes among the Pima Indians of Arizona: an epidemic attributable to environmental change? Nutrition Reviews 1999; 57(5part2): S51-S54.
17. O'Dea K. Westernization, insulin resistance and diabetes in Australian aborigines. Medical Journal of Australia 1991; 155(4): 258-264.
18. Yu Chy, Zinman B. Type 2 diabetes and impaired glucose tolerance in aboriginal populations: a global perspective. Diabetes Research and Clinical Practice 2007; 78(2): 159-170.
19. Permutt MA, Wasson J, Cox N. Genetic epidemiology of diabetes. Journal of Clinical Investigation 2005; 115(6): 159-170, 1431-1439.
20. Hales CN, Barker DJP. The thrifty phenotype hypothesis. British Medical Bulletin 2001; 60(1): 5-20.
21. Hales CN, Barker DJP. Type 2 (non-insulin-dependent) diabetes mellitus: the thrifty phenotype. Diabetologia 1993; 35(7): 595-601.
22. Rock M. Sweet blood and social suffering: rethinking cuase-effect relationships in diabetes, distress, and duress. Medical Anthropology 2003; 22(2): 131-173.
23. Young A. 1980. The discourse on stress and the reproduction of conventional knowledge. Social Science and Medicine 14(3): 133-146.
24. Neel JV. Diabetes mellitus: a "thrifty" genotype rendered detrimental by "progress"? American Journal of Human Genetics 1962; 14(4): 353-362.
25. Tuchman AM. Diabetes and race: a historical perspective. American Journal of Public Health 2011; 101(1): 24-33.
26. McCarthy MI. Genomics, type 2 diabetes, and obesity. New England Journal of Medicine 2010; 363(24): 2339-2350.
27. Lillioja S, Wilton A. Agreement am, ong type 2 diabetes linkage studies but a poor correlation with results from genome-wide association studies. Diabetologia 2009; 52(6): 1061-1074.
28. Benyshek DC, Watson JT. Exploring the thrifty genotype's food-shortage assumptions: a cross-cultural comparison of ethnographic accounts of food security among foraging and agricultural societies. American Journal of Physical Anthropology 2006; 131(1): 120-126.
29. Ferreira ML, Lang GC. Deconstructing diabetes. In: ML Ferreira, GC Lang (Eds). Indigenous Peoples and Diabetes. Durham, NC: Carolina Academic, 2005; 73-103.
30. Lindsay RS, Bennett PH. Type 2 diabetes, the thrifty phenotype - an overview. British Medical Bulletin 2001; 60(1): 21-32.
31. Benyshek DC, Martin JF, Johnston CS. A reconsideration of the origins of the type 2 diabetes epidemic among Native Americans and the implications for intervention policy. Medical Anthropology , 2001;<, ,, ,, em>
32. Schoenberg NE, Drew EM, Stoller EP, Kart CS. Situating stress: lessons from lay discourses, on diabetes. Medical Anthropology Quarterly 2005; 19(2, , , ): 171-193.
33. : Daniulaityte R. Making sense of diabetes: cultural models, gender and individual adjustment to Type 2 diabetes in a Mexican community. Social Science and Medicine 2004; 59(9): 1899-1912.
34. Brown DE. General stress in anthropological fieldwork. American Anthropologist 1981; 83(1):74-92.
35. Selye H. The stress of life. New York: McGraw-Hill, 1956.
36. Cassel J. The contribution of the social environment to host resistance. American Journal of Epidemiology 1976; 104(2): 107-123.
37. Cassel J. Psychosocial processes and "stress": theoretical formulation. International Journal of Health Services 1974; 4(3): 471-482.
38. Cassel J. An epidemiological perspective of psychosocial factors in disease etiology. American Journal of Public Health 1974; 64(11): 1040-1043.
39. Nixon P. The human function curve-a paradigm for our times. Activitas Nervosa Superior 1982; Suppl3(pt1): 130.
40. Crews DE. Composite estimates of physiological stress, age, and diabetes in American Samoans. American Journal of Physical Anthropology 2007; 133(3): 1028-1034.
41. McEwen BS, Stellar E. Stress and the individual. Mechanisms leading to disease. Archives of Internal Medicine 1993; 153(18): 2093-2101.
42. Marmot M, Wilkinson RG (Eds). Social Determinants of Health, 2nd edn. Oxford: Oxford University Press, 2005.
43. Jiang J, Beals, J, Whitesell NR, Roudibeaux Y, Manson SM, AI-SUPERPFP Team. Stress burden and diabetes in two American Indian reservation communities. Diabetes Care 2008; 31(3): 427-429.
44. Lieberman LS. Diabetes mellitus and medical anthropology. In: CR Ember, M Ember (Eds). Encyclopedia of Medical Anthropology. Health and Illness in the World's Cultures. Topics, vol 1. New York: Kluwer Academic, 2004; 335-352.
45. ML Ferreira, GC Lang (Eds). Indigenous peoples and diabetes. Durham, NC: Carolina Academic, 2005.
46. Paradies Y. A review of psychosocial stress and chronic disease for 4th world indigenous peoples and African Americans. Ethnicity & Disease 2006; 16(1): 295-308.
47. Dressler WW. Cultural dimensions of the stress process: measurement issues in fieldwork. In: G Ice, GD James (Eds). Measuring stress in humans. Cambridge: Cambridge University Press, 2006; 27-59.
48. Dressler WW. Psychosomatic symptoms, stress and modernization: a model. Culture, Medicine and Psychiatry 1985; 9(3): 257-286.
49. Dressler WW. Culture, stress and disease. In: CF Sargent, TM Johnson (Eds.). Handbook of Medical Anthropology: Contemporary Theory and Method, revised edn. New York; Greenwood, 1996; 252-271.
50. Dressler WW. Culture and the risk of disease British Medical Bulletin 2004; 69(1): 21-31.
51. Pollard TM. Physiological consequences of everyday psychosocial stress. Collegium Antropologicum 1997; 21(1): 17-28.
52. Rodríguez-Morán M, Guerrero-Romero F, Brito-Zurita O, Rascón-Pacheco RA, Pérez-Fuentes R, Sánchez-Guillén MC et al. Cardiovascular risk factors and acculturation in Yaquis and Tepehuanos Indians from Mexico. Archives of Medical Research 2008; 39(3): 352-357.
53. Eckersley R. Is modern Western culture a health hazard? International Journal of Epidemiology 2006; 35(2): 252-258.
54. Barker DJ, Osmond C. Infant mortality, childhood nutrition, and ischemic heart disease in England and Wales. Lancet 1986; 1(8489): 1077-1081.
55. Barker DJP. The malnourished baby and infant. BMJ 2001; 60(1): 69-88.
56. Brufani C, Grossi A, Fintini D, Tozzi A, Nocerino V, Patera PI et al. Obese children with low birth weight demonstrate impaired beta-cell function during oral glucose tolerance test. Journal of Clinical Endocrinology and Metabolism 2009; 94(11): 4448-4452.
57. Cook JT, Levy JC, Page RC, Shaw JA, Hattersley AT, Turner RC. Association of low birth weight with beta cell function in the adult first degree relatives of non-insulin dependent diabetic subjects. BMJ 1993; 306(6873): 302-306.
58. Newsome CA, Shiell AW, Fall CH, Phillips DI, Shier R, Law CM. Is birth weight related to later glucose and insulin metabolism? A systematic review. Diabetes Medicine 2003; 20(5): 339-348.
59. Vaag A, Jensen CB, Poulsen P, Brøns C, Pilgaard K, Grunnet L et al. Metabolic aspects of insulin resistance in individuals born small for gestational age. Hormone Research 2006; 65(Supl3): 137-143.
60. Eriksson JG, Forsén T, Tuomilehto J, Jaddoe V W, Osmond C, Barker DJ. Effects of size at birth and childhood growth on the insulin resistance syndrome in elderly individuals. Diabetologia 2002; 45(3): 342-348.
61. Yajnik C. Interactions of perturbations in intrauterine growth and growth during childhood on the risk of adult-onset disease. Proceedings of the Nutritional Society 2000; 59(2): 257-265.
62. Gluckman PD, Hanson MA. Living with the past: evolution, development, and patterns of disease. Science 2004; 305(5691):1733.
63. Kobrin SJ. Industrialization and variation in social structure: an empirical test of the convergence hypothesis. Working Paper. Cambridge, MA: MIT Press 1975; 825-875.
64. Irwin PH. An operational definition of societal modernization. Economic Development and Cultural Change; 1975; 23(4): 595-613.
65. Baer HA, Singer M, Susser I. Medical Anthropology and the World System, 2nd edn. Westport, CN: Praeger, 2003.
66. Dunn FL, Janes CR. Introduction: medical anthropology and epidemiology. In: CR Janes, R Stall, SM Gifford (Eds.). Anthropology and Epidemiology. Dordrecht: D Reidel, 1986; 3-34
67. Stuckler D. Population causes and consequences of leading chronic diseases: a comparative analysis of prevailing explanations. Milbank Quarterly 2008; 86(2): 273-326.
68. Genuis SJ. Nutritional transition: a determinant of global health. Journal of Epidemiology and Community Health 2005; 59(8): 615-617.
69. Stettler N. Commentary: Growing up optimally in societies undergoing the nutritional transition, public health and research challenges. International Journal of Epidemiology 2007; 36(3): 558-559.
70. Lieberman L. Dietary, evolutionary and modernizing influences on the prevalence of type 2 diabetes. Annual Review Nutrition 2003; 23: 345-377.
71. Eaton C. Diabetes, culture change, and acculturation: a biocultural analysis. Medical Anthropology 1977; 1(2): 41-63.
72. Ezzati M, Vandern Hoorn S, Lawes CMM , Leach R, James WPT, Lopez AD et al. Rethinking the "diseases of affluence" paradigm: global patterns of nutritional risks in relation to economic development. Public Library of Science Medicine 2005; 2(5): 404-412.
73. Fall CHD. Non-industrialized countries and affluence. British Medical Bulletin 2001; 60(1): 33-50.
74. Scheder JC. A sickly-sweet harvest: farm-worker diabetes and social (in) equality. In: ML Ferreira, J Lang (Eds). Indigenous peoples and diabetes. Durham, NC: Carolina Academic, 2005; 279-334.
75. Goodman AH, Thomas RB, Swedlund AC, Armelagos GJ. Biocultural perspectives on stress in prehistoric, historical, and contemporary population research. Yearbook of Physical Anthropology 1988; 31: 169-202.
76. James GD. The relation of norepinephrine to blood pressure is independent of acculturation in Western Samoan men. American Journal of Hypertension 1989; 2(6pt1): 471-473.
77. James GD, Baker PT, Jenner DA, Harrison GA. Variation in lifestyle characteristics and catecholamine excretion rates among young Western Samoan men. Social Science and Medicine 1987; 25(9): 981-986.
78. Scheder JC. A sickly-sweet harvest: farm worker diabetes and social equality. Medical Anthropology Quarterly 1988; 2(3): 251-277.
79. Flinn M, England B. Childhood Stress and Family Environment. Current Anthropology 36 (5): 854-866
80. Page LB, Damon A, Moellering RC. Antecedents of cardiovascular disease in six Solomon Island societies. Circulation 1974; 49(6): 1132-1146.
81. Crews DE, MacKeen PC. Mortality related to cardiovascular disease and diabetes mellitus in a modernizing population. Social Science and Medicine 1982; 16(2): 175-181.
82. Chin-Hong PV, McGarvey ST. Lifestyle incongruity and adult blood pressure in Western Samoa. Psychosomatic Medicine 1996; 58(2): 131-137.
83. Bindon JR, Knight A, Dressler WW, Crews DE. Social context and psychosocial influences on blood pressure among American Samoans. American Journal of Physical Anthropology 1997; 103(1): 7-18.
84. Dressler WW, Mata A, Chavez A, Viteri FE. Arterial blood pressure and individual modernization in a Mexican community. Social Science and Medicine 1987; 24(8): 679-687.
85. Dressler WW, Bindon JR, Gilliland MJ. Sociocultural and behavioral influences on health status among the Mississippi Choctaw. Medical Anthropology 1996; 17(2): 165-180.
86. Brand JC, Snow BJ, Nabhan GP, Truswell AS. Plasma glucose and insulin responses to traditional Pima Indian meals. American Journal of Clinical Nutrition 1990; 51(3): 416-420.
87. Thorburn AW, Brand JC, Truswell AS. Slowly digested and absorbed carbohydrate in traditional bush foods: a protective factor against diabetes? American Journal of Clinical Nutrition 1987; 45(1): 98-106.
88. Williams DE, Knowler WC, Smith CJ, Hanson RL, Roumain J, Saremi A et al. The effect of Indian or Anglo dietary preference on the incidence of diabetes in Pima Indians. Diabetes Care 2001; 24(5): 811-816.
89. O'Dea K. Marked improvements in carbohydrate an lipid metabolism in diabetic Australian Aborigines after temporary reversion to traditional lifestyle. Diabetes 1984; 33(6): 596-603.
90. Kashiwagi A, Mott D, Bogardus C, Lillioja S, Reaven GM, Foley JE. The effects of short-term overfeeding on adipocyte metabolism in Pima Indians. Metabolism 1985; 34(4): 364-370.
91. Wiedman DW. Adiposity or longevity: which factor accounts for the increase in type II diabetes mellitus when populations acculturate to an industrial technology? Medical Anthropology 1989; 11(3): 237-253.
92. Jenkins DJA, Wolever TMS, Jenkins AL, Giordano C, Giudici S, Thompson LU et al. Low glycemic response to traditionally processed wheat and rye products: bulgur and pumpernickel bread. American Society for Clinical Nutrition 1986; 43(4): 516-520.
93. Brimblecombe JK, O'Dea K. The role of energy cost in food choices for an Aboriginal population in northern Australia. Medical Journal of Australia 2009; 190(10): 549-551.
94. Rodríguez-Morán M, Guerrero-Romero F, Rascón-Pacheco RA. Multidisciplinary Research Group on Diabetes of the Instituto Mexicano Del Seguro Social. Dietary factors related to the increase of cardiovascular risk factors in traditional Tepehuanos communities from Mexico. A 10 year follow-up study. Nutrition, Metabolism and Cardiovascular Disease 2009; 19(6): 409-416.
95. Marin G, Sabogal F, Marin BV, Otero-Sabogal R, Perez-Stable EJ. Development of a Short Acculturation Scale for Hispanics. Hispanic Journal of Behavioral Sciences 1987; 9(2): 183-205.
96. Valencia ME, Bennett PH, Ravussin E, Esparza J, Fox C, Schulz LO. The Pima Indians in Sonora, Mexico. Nutrition Reviews 1999; 57(5pt2): S55-S58.
97. Schulz LO, Bennett PH, Ravussin E, Kidd JR, Kidd KK, Esparza J et al. Effects of traditional and Western environments on prevalence of type 2 diabetes in Pima Indians in Mexico and the U.S. Diabetes Care 2006; 29(8): 1866-1871.
98. Dabelea D, Pettitt DJ, Hanson RL, Imperatore G , Bennett PH, Knowler WC. Birth weight, type 2 diabetes, and insulin resistance in Pima Indian children and young adults. Diabetes Care 1999; 22(6): 944-950.
99. McCance DR, Pettitt DJ, Hanson RL, Jacobsson LT, Knowler WC, Bennett PH. Birth weight and non-insulin dependent diabetes: thrifty genotype, thrifty phenotype, or surviving small baby genotype? BMJ 1994; 308(6934): 942-945.
100. Pettitt DJ, Forman MR, Hanson RL, Knowler WC, Bennett PH. Breastfeeding and incidence of non-insulin dependent diabetes mellitus in Pima Indians. Lancet 1997; 350(9072): 166-168.
101. Weigensberg MJ, Toledo-Corral CM, Goran MI. Association between the metabolic syndrome and serum cortisol in overweight Latino youth. Journal of Clinical Endocrinology and Metabolism 2008; 93(4): 1372-1378.
102. Owen CG, Martin RM, Whincup PH, Smith GD, Cook DG. Does breastfeeding influence risk of type 2 diabetes in later life? A quantitative analysis of published evidence. American Journal of Clinical Nutrition 2006; 84(5): 1043-1054.
103. Gibson MV, Diaz VA, Mainous III AG, Geesey ME. Prevalence of breastfeeding and acculturation in Hispanics: results from the NHANES 1999-2000 study. Birth 2005; 32(2): 93-98.
104. Ayala GX, Baquero B, Klinger S. A systematic review of the relationship between acculturation and diet among Latinos in the United States: implications for future research. Journal of the American Dietetic Association 2008; 108(8): 1330-1344.
105. Mainous III AG, Diaz VA, Geesey ME. Acculturation and healthy lifestyle among Latinos with diabetes. Annals of Family Medicine 2008; 6(2): 131-137.
106. Rosas LG, Harley K, Fernwald LC, Guendelman S, Mejia F, Neufeld LM et al. Dietary associations of household food insecurity among children of Mexican descent: results of a binational study. Journal of the American Dietetic Association 2009; 109(12): 2001-2009.
107. Mier N, Medina AA, Ory MG. Mexican Americans with type 2 diabetes: perspectives on definitions, motivators and programs of physical activity. Preventing Chronic Disease 2007; 4(2): 1-8.
108. Asao K, Kao WHL, Baptiste-Roberts K, Bandeen-Roche K, Erlinger TP, Brancati FL. Short stature and the risk of adiposity, insulin resistance and type 2 diabetes in middle age. The Third National Health and Nutrition Examination Survey (NHANES III), 1988-1994. Diabetes Care 2006; 29(7): 1632-1637.
109. Lawlor DA, Ebrahim S, Smith GD. The association between components of adult height and type II diabetes and insulin resistance: British women's heart and health study. Diabetologia 2002; 45(8): 1097-1106.
110. Wadsworth MEJ, Hardy RJ, Paul AA, Marshall SF, Cole TJ. Leg and trunk length at 43 years in relation to childhood health, diet and family circumstances: evidence from the 1946 national birth cohort. International Journal of Epidemiology 2002; 31(2):383-390.
111. Eckersley R. Is modern Western culture a health hazard? International Journal of Epidemiology 2006; 35(2): 252-258.
112. Wallace PM, Pomery EA, Latimer AE, Martinez JL, Salovey P. A review of acculturation measures and their utility in studies promoting Latino health. Hispanic Journal of Behavioral Sciences 2010; 32(1): 37-52.
113. Thomson MD, Hoffman-Goetz L. Defining and measuring acculturation: a systematic review of public health studies with Hispanic populations in the United States. Social Science and Medicine 2009; 69(7): 983-991.
114. Cuéllar I, Arnold B, González G. Cognitive referents of acculturation: Assessment of cultural constructs in Mexican Americans. Journal of Community Psychology 1995; 23(4): 339-356.
115. Cohen S, Kamarck T, Mermelstein R. A Global Measure of Perceived Stress. Journal of Health and Social Behavior 1983; 24(4): 385-396.


