Despite of the amount of effort spent increasing the number of physicians in rural communities in the USA, recently published reports indicate the rural physician shortage continues1,2. The Matriculating Student Questionnaire (MSQ) is a survey that is distributed to all first-year medical students in the USA prior to starting medical school3. Career plans reported on the MSQ are shown to be a significant predictor of practice type and location4. Findings from the 2008 MSQ revealed that only 2.3% of the responding students were planning to serve in a rural area5. Although the last 3 years of MSQ data illustrates a steady trend, the number of physicians per rural resident is expected to decline as the 'baby boomer' generation starts to age and require more medical attention. The United States Census Bureau predicted that the US population of those aged 65 years or older will increase by 60% between 2000 and 20306.
This rural physician shortage trend will especially affect the state of Idaho due to its unique geographic and demographic characteristics. Idaho is a rural state with 32 of its 44 counties considered rural7. During the year 2008, 52.4% of the residents of Idaho lived in these rural counties7,8. Of the 44 counties, 30 have one or more designated primary care shortage areas9. The American Medical Association reported that 17.4% of Idaho residents live in a designated primary care shortage area, and this is among the nation's highest for any state10.
Rural Idaho also has pre-existing physician access and shortage issues. In 2007, Idaho had the second lowest total number of physicians among the 50 other states2. Approximately two physicians are available to provide services to 1000 Idaho residents, which is 44% below the national average2. Idaho also has the sixth oldest physician workforce in the country, and 40% of Idaho physicians who are registered with the AMA were aged 55 years or older2. With a large projected population growth, especially among persons 65 years or older, Idaho will experience a significant decrease in its physician workforce due to retirement, and a substantial increase in the number of residents with greater medical needs. The American Academy of Family Physicians identified Idaho as one of the 5 states that would face serious shortages of family medicine physicians by 20201.
Idaho is one of the 6 states that do not have at least one medical school2. Without a medical school in Idaho, the state ranks 48th in the nation of the number of first-year medical school seats per capita11. Idaho is currently limited to a total of 4 residency programs total with 2 rural training tracks. A previous study reported that graduates of such an immersion training program subsequently returned to their communities as medical staff12. Rural Idaho communities are already limited, in contrast to their counterparts that have greater access with medical school and/or residencies when recruiting physicians. Consequently, recruitment and retention strategies become critical to addressing physician shortage problems in Idaho, and communities are anxious to better understand the factors involved. In the setting of limited resources, appreciating their relative importance from the physician's perspective is crucial. The ability to recruit and retain physicians directly affects the ability to provide adequate services to the community13.
The recruitment and retention of physicians in rural areas is affected by many factors, which can be conceptualized into 5 classes: geographic, financial, scope of practice, medical support, and hospital and community support.
Geographic class factors include spousal satisfaction in the community which has been identified as one of the most important factors impacting physician recruitment and retention in rural areas14-17. Another important geographic factor is proximity to extended family14,17. Climate or geographic features as well as recreational facilities had a positive influence on physician practice location14. Other geographic characteristics that influence practice location choices include an access to a variety of social activities, close distance to larger cities, cultural opportunities, shopping, being raised in a rural area and the education system14,15,18-20.
Financial class issues affect physicians' decisions on their practice location. In one study, over 70% of the responding medical students indicated that guaranteed income is important, and approximately 35% responded that long-term earning potential is one of their top three priorities when deciding whether to enter rural practice17. The mixture of payors influences physicians' current and potential income and is a factor influencing physician practice in rural areas15,18,21,22. Financial incentive programs such as federal loan waivers and bonus reimbursements are often available to physicians who choose to practice in rural areas, especially in health professional shortage areas18. Other significant financial factors predicting location of practice include employment status and part-time opportunities14,18,23.
Scope of practice class factors influence medical practices locations in rural areas. Type of practice was rated a very high priority among family physicians14. Physicians practicing in rural areas tend to provide a broad scope of practice24,25. This broad scope of practice may include practice differences from their more urban counterparts26-28. Rural practice also provides less competition and more clinical independence21. Other significant factors related to scope of practice include teaching opportunities, supervision of other health professionals, and emergency room coverage14,18,21,24.
Medical support class factors are important when physicians decide where to locate their practice. The working hours required for practice was identified as one of the top 10 most influential factors of current practice location, and it was significantly more important to female physicians14. A connection between rural practice location and long working hours is also reported in other studies18,20,22,24. Call responsibilities have also been identified as an important factor15,16,28,29. Specialist and other health professional availability is another factor influencing choice of a practice location14,15,18,19. Other medical support factors reported in previous studies include familiarity with medical community and resources, recruitment by colleagues, vacation and leisure time, and competent medical staff14,18,21.
Hospital and community support class factors influence choice of practice location. Professional development opportunities are important factor for physician decisions on practice location14,17. Funded learner-driven continuing medical education (CME) is also important to recruiting and retaining more physicians in rural communities16,17. Perceived medical need in a community has also been recognized as an important factor14,17,21. Technology, hospital equipment and facilities are other important factors for physicians' practice location preference14,16,19. Other hospital and community support factors identified in previous studies are the hospital's proactive vision for the future, flexibility of the hospital, relationship with patients and colleagues, number of hospital beds, housing allocation, and plans for capital investment17-19,30.
The number of published reports that documented successful case studies and/or strategies regarding rural physician recruitment is limited. Many previous studies extensively explored ways to increase the overall number of rural physicians; however, these studies' results may not be applicable in terms of increasing physician workforce in a particular rural community. As a result, many hospitals and communities still rely on expensive physician recruitment firms and/or their own experience-based recruitment strategies. Without having an opportunity to identify their communities' assets and capabilities of physician recruitment and retention, rural hospitals and communities with a historical challenge in recruitment and retention of physicians continue to experience physician shortage problems. Comparative analysis with peers can be difficult, and addressing biases within the community or between physicians and administrator views can be unintentional barriers.
The purpose of this study was to develop an evaluation instrument useful to rural Idaho communities' in their assessment of assets and capabilities related to physician recruitment and retention. Just as the Apgar score is used to quantify resources and capabilities of the newborn that are indicative of current functioning, the Community Apgar Questionnaire (CAQ) seeks to serve the same purpose for family physician recruitment to rural communities. The results of this study may help rural Idaho hospitals and communities to find improvement opportunities for recruitment and retention strategies.
This research was approved by the Boise State University Human Subjects Institutional Review Board.
Survey development
The CAQ was developed by the researchers based on literature reviews, site visits to rural Idaho communities, and discussions with rural physicians and hospital administrators. The CAQ consists of 5 major classes that are associated with the success level of recruitment and retention of physicians. These classes were identified to be:
- geographic
- economic
- scope of practice
- medical support
- hospital and community support.
Each class consists of 10 detailed factors on which respondents were asked to rate their advantage and importance level. The CAQ also included 3 open-ended qualitative questions. These questions were intended to cover any missing factors that may not have been included in the survey. The CAQ is provided (Appendix I), as is a glossary of terms used in the CAQ (Appendix II).
Selection and recruitment of target populations
The target population for the study was hospital administrators and physician leaders who had responsibilities for recruitment and retention of physicians in rural Idaho. The sample communities were selected based on site visits to rural communities and discussions with research colleagues at the Idaho Hospital Association, the Idaho Academy of Family Physicians, and the Office of Rural Health and Primary Care of the Idaho Department of Health and Welfare. Twelve rural communities with critical access hospitals were selected as the target sample. These 12 communities were categorized into 2 groups based on their historical success in recruitment and retention of rural family medicine physicians. Those with more success were assigned into the 'alpha (α)' group, and those with less success were classified into the 'beta (β)' group. These classifications were made based on site visits to rural communities, the discussions with research colleagues listed above, and input from physician leaders in the Family Medicine Residency of Idaho who have significant experience in placing family medicine physicians in rural Idaho communities. Hospital administrators in these communities were recruited to the study by phone and email and were asked to identify physician leaders in their hospitals. The selected physician leaders were recruited to the study in the same manner.
Survey administration
Cross-sectional structured interviews were conducted in the study. A consent form and the CAQ were mailed to the hospital administrators and physician leaders who agreed to participate in the study for their review prior to the interview visits. A one-hour interview was scheduled with each participant. A family medicine physician with rural practice and physician recruiting experience traveled to the participating communities to conduct structured interviews using the CAQ. One hospital administrator and one physician leader were interviewed for each participating community on a separate occasion. The consent form was reviewed with the interviewer and signed by respondents prior to the interviews. These interviews were held in private locations. Responses to the CAQ were recorded by the interviewer on a printed CAQ form.
Data processing and analysis
The completed CAQs were sent to Boise State University and entered into SPSS v15 (www.spss.com) for statistical analysis by researchers at the Center for Health Policy. Numerical scores were assigned to the survey responses for advantages and challenges and for importance ratings using a 4 point Likert scale format. These scores were used to calculate the Community Apgar score. Descriptive statistics were used to report the overall responses to the CAQ. Non-parametric Mann-Whitney U-tests were employed to determine the statistical significance of difference in the self-rated advantage and importance level as well as Community Apgar score for each class between respondent types (hospital administrators vs physician leaders) and community types (α vs β). The completed were sent to Boise State University and were processed by researchers at the Center for Health Policy.
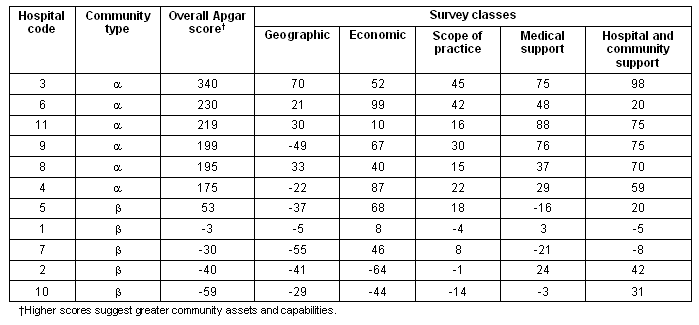
Eleven of the 12 invited communities participated in the study, resulting in a 91.7% participation rate. One beta community was not able to participate in the study due to healthcare leadership transitions. The overall responses to the CAQ are provided (Table 1). The following sections describe the results for advantages and challenges ratings, importance ratings and Apgar scores by class.
Table 1: Distribution of responses across survey items
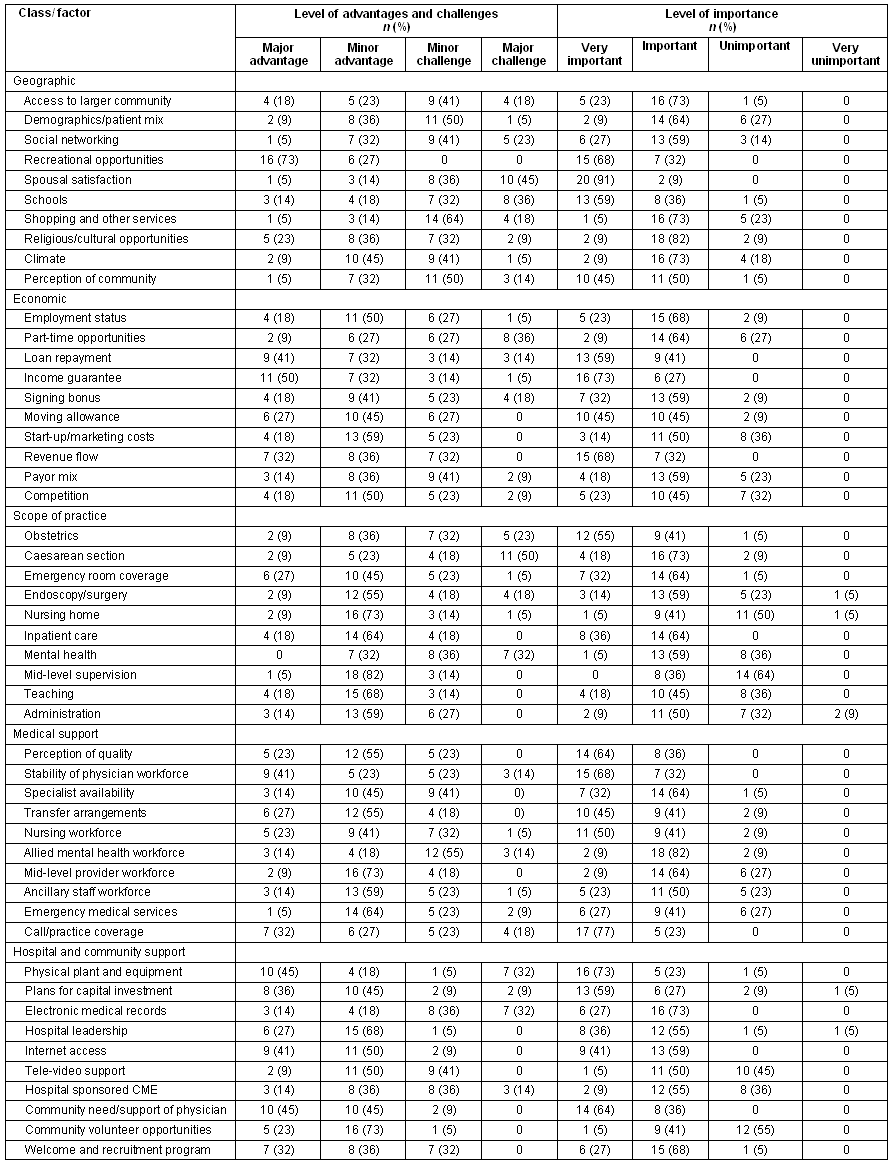
Community Apgar Questionnaire advantages and challenges findings
Respondents were asked to rate their community's perceived advantages and challenges for the 50 factors in 5 classes. These factors were rated on a 4 point Likert scale (major advantage, minor advantage, minor challenge, major challenge), and these scale values were converted into scores (major advantage = 2, minor advantage = 1, minor challenge = -1, major challenge = -2). Statistical differences of these scores by class were determined between respondent and community types.
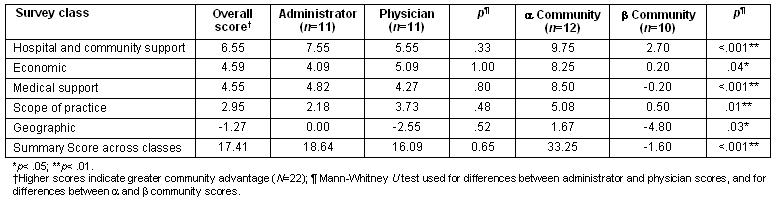
The advantages and challenges' mean scores for the 5 classes within the CAQ are given (Table 2). Class scores were calculated for each class by summing scores across 10 factors. A summary score was determined by summing the scores across 5 classes. Hospital and community support was identified as the most advantageous class associated with recruitment of retention of physicians, followed by economic, medical support, and scope of practice. Geographic class was the only challenging factor identified by respondents.
Hospital administrators and physicians had similar ratings on advantages and challenges both within and across classes. Comparisons between community types showed that alpha communities had significantly more advantages over beta communities in hospital and community support (p<.001), economic (p<.05), medical support (p<.001), scope of practice (p<.05), geographic (p<.05) classes and across the summary class composite (p<.001)
Table 2: Community advantages and challenges mean scores by class
Community Apgar Questionnaire importance findings
Respondents were asked to rate their perceived importance levels for the 50 factors in 5 classes. These factors were rated on a 4 point Likert scale (very important, important, unimportant, very unimportant), and these scale values were converted into scores (very important = 4, important = 3, unimportant = 2, very unimportant = 1). Statistical difference of these scores by class was determined between respondent and community types.
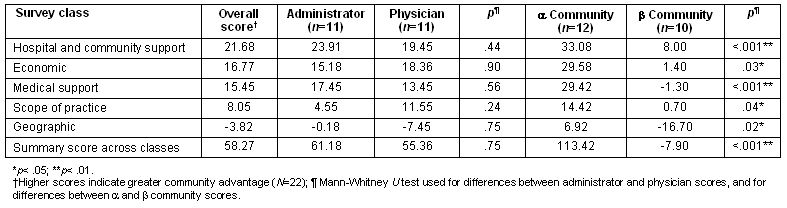
The importance mean scores is shown for the 5 classes within the CAQ (Table 3). Class scores were calculated for each class by summing scores across 10 factors. A summary score was determined by summing the scores across 5 classes. Medical support was identified as the most important class regarding recruitment and retention of physicians, followed by geographic, economic, hospital and community support, and scope of practice.
Although both hospital administrators and physicians considered medical support, geographic, and economic classes to be important, comparisons between respondent types showed that hospital administrators recognized medical support (p<.05), geographic (p<.001) and economic (p<.05) as significantly more important classes than did physicians. The summary score composite across classes also indicated that hospital administrators and physicians had a significantly different perception in the levels of importance (p<.05). Respondents in both alpha and beta communities had similar perceived importance levels both within and across classes.
Table 3: Community importance mean scores by class
Community Apgar Questionnaire Apgar findings
The following algorithm was used to calculate the Community Apgar score from advantage/challenge and importance scores.
Community Apgar score = advantage/challenge score × importance score: The Community Apgar score ranges from -8 to 8 with a higher score indicating a more developed community asset and capability related to recruitment and retention of physicians. Statistical difference of these scores by class was determined between respondent and community types.
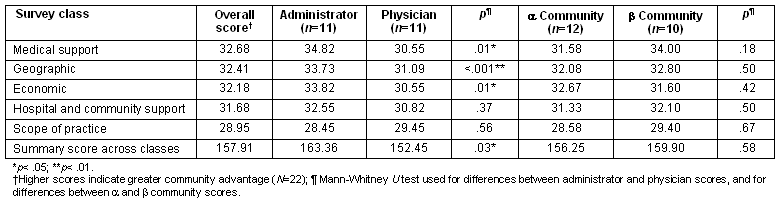
The mean Community Apgar scores are shown for the 5 classes within the CAQ (Table 4). Class scores were calculated for each class by summing scores across 10 factors. A summary composite score was determined by summing the scores across 5 classes. The hospital and community support class was identified as the most developed community asset and capability associated with recruitment and retention of physicians, followed by economic, medical support, scope of practice and geographic.
Table 4: Community Apgar mean scores by class
Hospital administrators and physicians had similar opinions regarding their community assets and capabilities. However, comparisons between community types revealed that alpha communities had significantly more developed community assets and capabilities than beta communities in all 5 classes, including hospital and community support (p<.001) and medical support (p<.001), geographic (p<.05), economic (p<.05), and scope of practice (p<.05). Overall, across the class composite measure, alpha communities showed significantly more developed community assets and capabilities than beta communities (p<.001).
The cumulative Apgar scores for alpha and beta communities are shown (Table 5). Cumulative Apgar scores are a sum of the Apgar scores for each of the 5 classes in the instrument. All alpha communities have higher cumulative Apgar scores than beta communities.
Table 5: Cumulative community Apgar score by hospital
Qualitative results
The CAQ contained 3 open-ended questions. Respondents were asked to identify the greatest barriers to recruitment and retention of family medicine physicians and potential solutions to overcome these barriers. They were also asked to identify the reasons why a successful physician candidate did not accept a position in the community and what he/she would ultimately do instead in terms of employment. The answers to these questions suggested that the CAQ included all relevant variables related to recruitment and retention of physicians to rural communities.
Discussion
Communities in the state of Idaho have experienced challenges with recruiting and retaining physicians due to unique factors of varying importance. Many pre-existing healthcare access and physician shortage problems among rural Idaho communities are expected to become more challenging because of recent aging and retirement trends. Limited community resources require addressing the most important factors affecting physician choices and satisfaction. Knowledge of these most crucial modifiable factors becomes invaluable to strategic planning, including understanding of comparative advantages in the marketing process. Therefore, recruitment and retention self-assessment becomes critical to addressing physician shortage problems in Idaho.
Previous studies have identified many factors influencing physicians' decisions on their practice location. Physicians, residents, and students have been reported to be influenced by factors categorized as geographic characteristics, financial issues, medical support, scope of practice, and community and hospital support when deciding their practice location. The purpose of this study was to develop an evaluation instrument useful in exploring rural Idaho communities' assets and capabilities regarding physician recruitment and retention. The CAQ was developed to assess and differentially diagnose the strengths and weakness of an individual community, as well as to provide information about the aggregate group. The CAQ assists in quantifying and visually demonstrating what has traditionally been a problem more commonly addressed by a more qualitative, expert-opinion approach. This instrument, accompanied by a growing database of aggregated data, also provides the opportunity for a community to gain peer comparison and time sequence comparison analysis.
Comparisons between community advantages and challenges scores by respondent types showed no statistically significant difference between hospital administrators and physicians in their perceived community's advantages and challenges. That is, respondents from the same community consistently identified their community's advantages and challenges. However, alpha communities had significantly greater advantages over beta communities in recruitment and retention of physicians in all CAQ classes and across classes. The hospital and community support class was identified as the most advantageous class for physician recruitment and retention, while the geographic class was identified as the least advantageous.
Comparison of community importance class scores between community types identified no significant difference among respondents in both alpha and beta communities. Thus, all the responding communities consistently recognized the classes of factors important in recruitment and retention. However, some differences in their importance levels of CAQ classes were observed between hospital administrators and physicians. Hospital administrators rated medical support, geographic, economic and the summary score higher in importance than physicians. That these areas appear to be more under the authority of hospital administrators may explain the differences in scores. Overall, the medical support class was identified as the most important class, while the scope of practice class was rated least important.
Comparison of community Apgar class scores between respondent types identified no significant difference but there were significant differences in all CAQ classes and the summary CAQ score between alpha and beta communities. Comparisons between community types using the CAQ instrument indicated that alpha communities had significantly more developed community assets and capabilities related to recruiting and retaining physicians than did beta communities . This result correlates with its classification criteria, in which alpha communities were identified as communities with a historical success in recruitment and retention of physicians. This data supports the validity of the CAQ, which was developed to assess the success levels regarding physician recruitment and retention among rural Idaho communities. The highest rated Apgar class was hospital and community support while the lowest was geography.
In the open-ended questions, spousal satisfaction was the most frequently reported barrier. Respondents described lack of spousal satisfaction as a 'deal breaker' for both recruitment and retention of physicians. Respondents identified that inadequate employment opportunities and the lack of cultural opportunities were associated with spousal dissatisfaction. Further research is recommended to explore factors associated with spousal satisfaction and dissatisfaction.
Limitations
One of the major limitations of this study was the limited number of sample communities. Eleven of the 12 communities recruited participated in the study. One critical access hospital administrator and one physician leader were interviewed for each community. In addition, these communities were selected as a targeted sample based on site visits and discussions with research colleagues at the Idaho Hospital Association, the Idaho Academy of Family Physicians, and the Office of Rural Health and Primary Care of the Idaho Department of Health and Welfare. Although a careful selection process was introduced to assure the quality of samples, they may have been biased and may not represent the target population.
Another limitation of this study was the data collection method. Because the face-to-face interview method was used in the study, a response bias may have occurred. Some respondents may have felt uncomfortable sharing their opinions on certain factors such as a relationship with their communities and their hospitals' economic status. In addition, although the use of non-parametric tests was appropriate considering the sample size and the format of the instrument, some significant relationships may not have been detected due to the limited statistical power.
Effective strategies for recruitment and retention of physicians will remain a crucial issue for communities in Idaho and elsewhere. Utilization of the CAQ and the aggregate peer database is a targeted response to this problem. Application advantages of this instrument include its unique quantification approach to a traditionally qualitative description of the issues. The tool could be used to track a community's progress in comparison with their real-time peers, or with regard to their own progress over time, similar to the clinical use of the Apgar scores in newborns. This instrument is designed to be a real-time assessment tool providing guidance for the most helpful interventions at the present time.
Acknowledgements
This research was funded by the Idaho Department of Health and Welfare, State Office of Rural Health and Primary Care, through a grant from the US Department of Health and Human Services, Health Resources and Services Administration, Rural Hospital Flexibility Program (grant no. H54RH00039). Financial contributions to this research were also made by Boise State University and the Family Medicine Residency of Idaho. The authors thank Steven Millard, President of the Idaho Hospital Association, for his assistance in this research. The authors also thank Benjamin Tverdy and Sean Wasden, research assistants in the Center for Health Policy, for editorial assistance with the manuscript.
References
1. American Academy of Family Physicians. Family physician workforce reform: recommendations of the American Academy of Family Physicians (draft reprint 305b). (Online) 2006. Available: http://www.aafp.org/online/en/home/policy/policies/w/workforce.html (Accessed 20 May 2009).
2. Association of American Medical Colleges, Center for Workforce Studies. Recent studies and reports on physician shortages in the US. Washington, DC: AAMC, 2009.
3. Association of American Medical Colleges. Matriculating Student Questionnaire (MSQ). (Online) No date. Available: http://www.aamc.org/data/msq/start.htm (Accessed 24 August 2009).
4. Rabinowitz HK, Diamond JJ, Markham FW, Paynter NP. Critical factors for designing programs to increase the supply of retention of rural primary care physicians. JAMA 2001; 286: 1041-1048.
5. Association of American Medical Colleges. Matriculating Student Questionnaire (MSQ): all schools summary report. Washington, DC: AAMC, 2008.
6. United States Census Bureau. US interim projections by age, sex, race, and Hispanic origin 2000-2050. (Online) no date. Available: http://www.census.gov/population/www/projections/usinterimproj/ (Accessed 27 August 2009).
7. United States Department of Agriculture, Economic Research Service. Rural definitions: state-level maps Idaho. (Online) no date. Available: http://www.ers.usda.gov/Data/Ruraldefinitions/ID.pdf (Accessed 25 August 2009).
8. United States Department of Agriculture, Economic Research Service. State fact sheets: Idaho. (Online) no date. Available: http://www.ers.usda.gov/StateFacts/ID.htm (Accessed 25 August 2009).
9. United States Department of Health and Human Services, Health Resources and Services Administration. Find shortage areas: HPSA by state & county Idaho. (Online) no date. Available: http://hpsafind.hrsa.gov/HPSASearch.aspx (Accessed 25 August 2009).
10. American Medical Association. Idaho needs health reform to fix the Medicare physician payment formula. (Online) 2009. Available: http://www.ama-assn.org/ama1/pub/upload/mm/399/sgr-states-id.pdf (Accessed 23 August 2009).
11. MGT of America Inc. Medical education study final report for Medical Education Study Committee, Idaho State Board of Education 2007; Tallahassee, FL: MGT, 2007.
12. Smucny J, Beatty P, Grant W, Dennison T, Wolff LT. An evaluation of the rural medical education program of the State University of New York Upstate Medical University, 1990-2003. Academic Medicine 2005; 80(8): 733-738.
13. Cohn KH, Harlow DC. Field-tested strategies for physician recruitment and contracting. Journal of Healthcare Management 2009; 54(3): 151-158.
14. Szafran O, Crutcher RA, Chaytors RG. Location of family medicine graduates' practices: what factors influence Albertans' choices? Canadian Family Physician 2001; 47: 2279-2285.
15. Lu DJ, Hakes J, Bai M, Tolhurst H, Dickinson JA. Factors affecting the career choices of family medicine graduates. Canadian Family Physician 2008; 54(7): 1016-1017.
16. Rourke JTB, Incitti F, Rourke LL, Kennard M. Keeping family physicians in rural practice: Solutions favoured by rural physicians and family medicine residents. Canadian Family Physician 2003; 49: 1142-1149.
17. Jutzi L, Vogt K, Drever E, Nisker J. Recruiting medical students to rural practice. Canadian Family Physician 2009; 55(1): 72-73.
18. Full JM. Physician recruitment strategies for a rural hospital. Journal of Healthcare Management 2001; 46: 277-282.
19. Sargeant J, Allen M, Langille D. Physician perceptions of the effect of telemedicine on rural retention and recruitment. Journal of Telemedicine and Telecare 2004; 10(2): 89-93.
20. Pepper CM, Sandefer RH, Gray MJ. Recruiting and retaining physicians in very rural areas. Journal of Rural Health 2010: 26(2): 196-200.
21. Backer EL, Mcllvain HE, Paulman PM, Ramaekers RC. The characteristics of successful family physicians in rural Nebraska: a qualitative study of physician interviews. Journal of Rural Health 2006; 22(2): 189-191.
22. Weeks WB, Wallace AE. Rural-urban difference in primary care physicians' practice patterns, characteristics, and incomes. Journal of Rural Health 2008; 24: 161-170.
23. McMurray JE, Heiligers PJM, Shugerman RP, Douglas JA, Gangnon RE, Voss C et al. Part-time medical practice: where is it headed? American Journal of Medicine 2005; 118: 87-92.
24. Baker E, Schmitz D, Epperly T, Nukui A, Moffat-Miller C. Rural Idaho family physicians' scope of practice. Journal of Rural Health 2010; 26(1): 85-89.
25. Rabinowitz HK, Paynter NP. The rural vs urban practice decision. JAMA 2002; 287(1): 107.
26. Incitti F, Rourke J, Rourke LL, Kennard M. Rural women family physicians: are they unique? Canadian Family Physician 2003; 49: 320-327.
27. Chaytors RG, Szafran O, Crutcher RA. Rural-urban and gender differences in procedures performed by family practice residency graduates. Family Medicine 2001; 33(10): 766-771.
28. Hutten-Czapski P, Pitblado R, Slade S. Short report: scope of family practice in rural and urban settings. Canadian Family Physician 2004; 50: 1548-1550.
29. Beaulieu M, Rioux M, Rocher G, Samson L, Boucher L. Family practice: professional identify in transition. A case study of family medicine in Canada. Social Science & Medicine 2008; 67(7): 1153-1163.
30. MacDowell M, Glasser M, Fitts M, Fratzke M, Peters K. Perspectives on rural health workforce issues: Illinois-Arkansas comparison. Journal of Rural Health 2009; 25(2): 135-140.
__________________________
Appendix I: Community Apgar Questionnaire

Appendix II: Glossary of terms





