The current preferred treatment of acute ST-segment elevation myocardial infarction (STEMI) is primary percutaneous coronary intervention (PPCI). This is the optimal treatment provided it can be delivered within a reasonable time frame (90-120 min)1 of diagnosis. However, in remote areas many patients with acute STEMI may not have immediate access to a cardiac catheterisation laboratory (cath lab). One such area is the Highlands of Scotland where the potentially long transfer times to the nearest cath lab might lead to unacceptable delays to achieving coronary artery reperfusion, and thus thrombolysis in this area remains the mainstay of initial reperfusion strategy for many patients with acute STEMI.
We report a case of STEMI in a patient with hereditary haemorrhagic telangiectasia (HHT) and discuss the issues surrounding the immediate and subsequent treatment.
Case
A 57-year-old woman living on a Scottish island with a past medical history of HTT, hyperlipidaemia and hypothyroidism woke at 4.00 am with severe central chest pain associated with sweating and vomiting. Her husband called for an ambulance but unfortunately all three ambulances on the island were unavailable at the time due to other clinical cases, so she was driven to the local hospital and arrived shortly after.
She was assessed promptly and an ECG performed at 4.19 am which revealed ST segment elevation in leads II, III, aVF, V5 and V6, consistent with a diagnosis of an infero-lateral STEMI (Fig1).
Initial treatment with aspirin 300 mg and clopidogrel 300 mg, sublingual glyceryl trinitrate, diamorphine 2.5 mg and metoclopramide 10 mg was promptly given at 4.25 am. After taking a clinical history and assessing the patient as per protocol, the decision had been made to administer thrombolysis (due to potentially long transfer times to the nearest cath lab). As preparations were made for thrombolysis, the patient then revealed her diagnosis of HHT, which only came to light when using the local thrombolysis contraindications check list. The diagnosis of HHT had been made 15 years previously. The patient had previously confirmed pulmonary telangiectasia but no documented cerebral involvement, and the symptoms from her HHT were limited to occasional epistaxis and chronic microcytic anaemia treated with oral iron replacement.
At this stage, advice was sought from the regional centre. After discussion, as the bleeding risk was deemed high, the patient was not given thrombolysis; the standard intravenous heparin (5000 IU bolus) was given instead as a pragmatic compromise, with a plan for immediate transfer of the patient to the nearest cath lab.
An air ambulance transfer was not possible due to inclement weather conditions (fog). The patient was transferred by road to the nearest cath lab where she arrived at 9.50 am. Coronary angiography via the right radial approach revealed a complete occlusion of a small distal coronary artery branch of the circumflex artery. Following aspiration and ballooning, there was poor flow in the very small distal vessel, so treatment was conservative and no stent was inserted.
The patient was subsequently transferred to the coronary care unit for ongoing treatment. Troponin I was raised at 2.55 μg/L (normal value <0.04 μg/L), renal function was normal, haemoglobin was 99 g/L and mean corpuscular volume was 72.9 fL.
She was commenced on standard treatment with aspirin 75 mg, atorvastatin 80 mg, bisoprolol 2.5 mg and perindopril 2 mg (all once daily). Because of the potential bleeding risk, and the fact that no coronary stent had been deployed, a second antiplatelet was not administered. Transthoracic echocardiogram demonstrated mild to moderate left ventricular systolic dysfunction. The patient was discharged home on day 3 and has remained well.
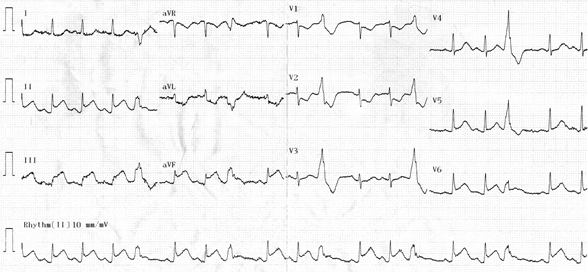
Figure 1: First ECG recorded after initial medical contact showing infero-lateral
ST segment elevation and reciprocal anterior ST segment depression, as well as ventricular ectopy.
This case report describes a difficult clinical situation where the management of a patient with a STEMI in a remote setting was further complicated by a rare pre-existing medical condition (HHT), which precluded the use of thrombolysis, while geographical remoteness and inclement weather conditions impeded immediate transfer of the patient to a cardiac cath lab.
In this case, no ambulances were available when the initial call for help was made. In our area the standard management is for every patient to have an ECG performed at the site of incident and for the administration of thrombolysis in the prehospital setting to be facilitated via telemetry-enabled decision support2,3. This was not possible in this case due to lack of ambulances; this is an issue in remote settings where the organisational resilience to multiple calls may be less than in urban centres. Furthermore, not all ambulances in remote areas are staffed with a paramedic crew and thus there may be variation in practice depending on which crew members are on shift.
Nevertheless, this patient was quickly transferred to the local hospital within 20 minutes and prompt assessment occurred. The major issues in this case were the administration of antiplatelet and antithrombotic medications in a patient with HHT. Although this patient with known pulmonary telangiectasia was reported to have no cerebral telangiectasia, this does not confer a low risk of intracerebral bleed, and the risk of life-threatening pulmonary haemorrhage is also recognised4. HHT is a rare contraindication to thrombolysis, but other more common contraindications exist (Table 1). The decision not to administer thrombolysis in this case was a pragmatic clinical decision as there were no guidelines or published reports about how to treat patients with HHT who are having a myocardial infaction. The decision to withhold thrombolysis was based on the perceived risks of intra-cranial or intra-pulmonary bleeding, and the potentially catastrophic consequences of both, balanced against the potential risk of delayed treatment of an inferior myocardial infarction. In this case, a non-medical nurse prescriber was on shift who was able to initiate treatment with aspirin and clopidogrel and consider thrombolysis, but this is not always the case in rural hospitals with less than continuous 'doctor cover'.
Previous close work between the remote hospital and regional centre allowed immediate access by telephone to a consultant cardiologist and the case was discussed.
Once the decision had been made not to administer thrombolysis, transfer to a cath lab was found to be problematic due to inclement weather conditions. This illustrates another issue with remote patient care: despite availability of an air ambulance, weather may remain a barrier to prompt access to definitive case and thus remote patients remain at a potential disadvantage when compared with urban dwellers.
In this case, the patient had an occlusion of a relatively small distal vessel and made a good recovery from her myocardial infarction; thus the impact of the above issues on her individual case was less than it may have been had she had a more proximal vessel occlusion.
With respect to opportunities to avoid the myocardial infarction, despite hypercholesterolaemia, this relatively young, non-smoking, normotensive, female patient had few risk factors and would have been considered at low risk of a cardiovascular event. Following local guidelines, her low overall risk would not have warranted treatment of hypercholesterolaemia in the absence of other risk factors.
Table 1: Contraindications to the administration of thrombolysis in acute ST segment elevation myocardial infarction1

This case illustrates some of the issues encountered when providing health care in remote areas and the importance of close communication between remote hospitals and regional centres.
Where thrombolysis is frequently the chosen reperfusion strategy due to accessibility, it is important to have an increased awareness of pre-existing conditions that could constitute contraindications for thrombolysis and could lead to life-threatening complications. In this case, use of an established safety check list and early discussion resulted in appropriate withholding of thrombolysis.
In such situations, early discussion with a cardiac specialist centre is vital to provide support and help make the most appropriate individualised treatment decisions. This is especially important with rare conditions such as HHT, when antiplatelets and antithrombotic treatment rely mostly on expert opinion and anecdotal evidence5 in the absence of a sufficient evidence base to inform standardised therapies.
However, despite good network support, remote services are more likely to be variable - in our area not all ambulances are staffed with paramedics and not all community hospitals that receive patients with myocardial infarction can immediately prescribe appropriate drugs. Thus, potentially life-saving treatment with thrombolysis could be delayed. One could argue that the ability to deliver such therapies is even more critical in remote areas, where transfer to a cath lab for PPCI is not always possible.
This case illustrates that despite distances involved and potential delays, direct transfer to a cath lab may still remain a safer option compared to thrombolysis for some remote patients with STEMI.
Acknowledgements
The authors would like to acknowledge staff nurse Anne Grundy, nursing auxiliary Marie MacPhee, Dr Chris James, Dr Stephen Cross and the nurses of the Cath Lab and Coronary Care Unit who provided additional clinical care for this patient.
References
1. Steg G, James S, Atar D, et al. ESC guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation: The task force on the management of ST-segment elevation acute myocardial infarction of the European Society of Cardiology (ESC). European Heart Journal 2012; 33: 2569-2619.
2. Rushworth GF, Bloe C, Diack HL, et al. Pre-hospital ECG E-transmission for patients with suspected myocardial infarction in the highlands of Scotland. International Journal of Environmental Research and Public Health 2014; 11(2): 2346-2360.
3. Chapman A, Mort A, Bloe C, Leslie SJ. Thrombolysis for acute ST elevation MI: nurse delivered decision support for community staff in remote areas. Rural Remote Health 12: 2262. (Online) 2012. Available: www.rrh.org.au (Accessed 15 June 2015).
4. Ference BA, Shannon TM, White RI Jr, Zawin M, Burdge CM. Life-threatening pulmonary hemorrhage with pulmonary arteriovenous malformations and hereditary hemorrhagic telangiectasia. Chest 1994; 106(5): 1387-1390.
5. Devlin HL, Hosman AE, Shovlin CL. Antiplatelet and anticoagulant agents in hereditary hemorrhagic telangiectasia. New England Journal of Medicine 2013; 368(9): 876-878.

