According to the World Health Organization (WHO), the group of people over the age of 60 is growing more rapidly than any other age group1,2. Both the scientific community and the general public have been examining ways to improve wellbeing and to prevent disease at every stage of life3. The healthcare system is one means to improve wellbeing and prevent disease, even in later life. Evidence shows that good medical services have contributed to an increase in average life span since 19504,5.
A series of research reports have described associations between the supply of primary care physicians and various health outcomes, such as cardiovascular and cancer mortality6-8. However, this favourable association of medical resources with health has not always been accepted. McKeown put forth the view that the improvements in population health in the industrialised world from the late 1700s to the present are not due to life-saving advancements in the field of medicine or public health, but can be attributed to improvements in overall standards of living, especially in diet and nutritional status, due to better economic conditions9.
There is strong association between diet and cardiovascular diseases (CVD)10; however, the majority of these studies have been evaluated in the hospital setting11-14. Nutrition counselling is a supportive process that sets priorities, establishes goals and creates individual action plans, acknowledging and fostering responsibility for self-care15. Dieticians' nutrition counselling frequently facilitates behaviour change in individuals. However, the role of nutritional services in improving a population's health status has not been well evaluated and documented, and there are limited data regarding impact on quality of life, particularly among the older population. The aim of the present study was to evaluate the association between public and private nutritional services and the prevalence of hypertension, hypercholesterolemia, diabetes and obesity, in a sample of men and women aged over 65 years, living on selected Greek islands and the Cyprus Republic.
Context
In the study area, the Cyprus Republic (796 740 population) and Crete (601 131 population) are classified as 'large' islands, while other islands are considered to be 'small' or 'moderate' in size (population varies from 2723 to 107 879). In some of these islands (ie Samothrace, Lemnos), communication with the mainland is infrequent, especially during winter. The population density varies between 15 persons/km2 (Samothrace) and 236 persons/km2 (Syros). The majority of the islands consist of rural areas and their populations derive income from primary production (foods, farming and fisheries), tourism and the promotion of trade. The Cyprus Republic is the exception, having the infrastructure of a single-country island.
These 10 islands were selected to test the research hypothesis of the present study because they were included in the MEDIS (Mediterranean Islands) Study16-18 of 2005-2009 (a health and nutrition survey aimed to evaluate a number of bio-clinical, lifestyle, behavioural and dietary characteristics of elderly people living on Mediterranean islands), and therefore current information about the distribution of CVD risk factors was available.
Study design
Data were collected in 3 stages. First, information about nutritional services was collected from dieticians practising on selected Greek islands included in the previous MEDIS study16 (ie Syros, Naxos, Corfu, Zakynthos, Cephalonia, Crete, Limnos, Lesvos and Samothrace), as well as in the Cyprus Republic. In the second stage, the MEDIS participants were re-interviewed in relation to their usage of nutritional services. Finally, the health status of the MEDIS participants was retrieved from MEDIS Study data.
The first two stages took place during 2010. Dieticians and the MEDIS study participants were interviewed face-to-face by a group of experienced field-investigation dieticians and physicians. Interviews were of approximately 20 min duration. Before the interviews, participants were informed about the aims of the study and gave their consent to participate by providing the requested information.
The rate of dieticians' participation was high, with the number interviewed as follows: 2 dieticians from Naxos (100% participation rate), 2 from Syros (50%), 4 from Lesvos (100%), 1 from Zakynthos (100%), 12 from Crete (60%), 3 from Cephalonia (100%), 9 from Corfu (50%), and 55 from Cyprus Republic (39%). There were no practising dieticians on the islands Samothrace and Limnos. The low participation rate in the Cyprus Republic was attributed to contact difficulties (incorrect dietician telephone numbers and addresses).
The interview rate for MEDIS participants was 79% and this was similar among the islands. The MEDIS Study population consisted of 1486: 744 men (aged 75±7 years) and 742 women (73±7 years), who were enrolled during 2005-2009. Individual island representations were Cyprus n=300; Lesvos n=142; Samothraki n=100; Lemnos n=150; Syros n=151; and Naxos n=145 in the Aegean Sea; and Cephalonia n=115; Corfu n=149; and Zakynthos n=103 in the Ionian Sea; and Crete, n=131. Detail of the MEDIS Study is available elsewhere16.
The present study's design, procedures and aims were approved by the Institutional Review Board of the Harokopio University.
Information about nutritional services and practices
Information regarding the number of covered and legislated dietician job positions (ie in hospitals, health care centres) within the public sector was retrieved through the departments of the Hellenic Ministry of Health (Administration Sanitary Districts), the Cypriot Ministry of Health and the two dietetics associations (the Hellenic Association of Hospital Dieticians and the Cypriot Dietetic Association). The number of dieticians in private practice was obtained from the Hellenic Dietetic Association, the Hellenic Technological Association of Dieticians and Nutritionists, the Cypriot Dietetic Association, and from local telephone directories.
Information about the role of nutritional services in the public or private sector was obtained from participants using a standard questionnaire that included both quantitative and semi-quantitative questions, and was developed for the purposes of this project. The questions were based on recommendations from the Writing Group of the Nutrition Care Process and the European Federation of the Associations of Dieticians (EFAD) regarding the role of nutritional and other healthcare services and practices usually followed in westernised societies19,20.
The number of persons who suggested an older person should visit a dietician was recorded as a possible score of between 0 (patient alone decided to visit a dietician) and 5 (5 persons suggested visiting a dietician). Responses to questions about the clinical reason/s for visiting a dietician were coded from 0 (negative answers) to 13 (positive answers) for 13 possible reasons provided (Table 1).
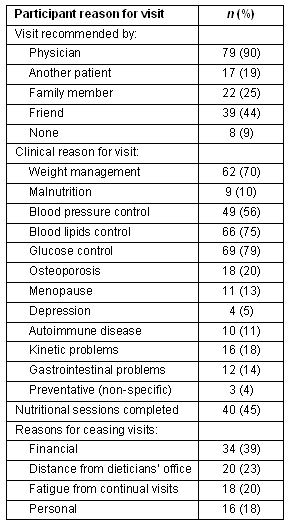
Table 1: Study dieticians' (n=88) reports of participants' stated reasons for consultation
The participants from the MEDIS Study were asked, 'Have you utilised nutritional services?' 'How do you evaluate the nutritional services in your area?' and 'Do you know any nutrition education program organized by the community that take part in your area of residence?'.
Evaluation of the prevalence of cardiovascular disease risk factors of the referent population
The prevalence of classical CVD risk factors, such as hypertension, hypercholesterolemia, diabetes and obesity, of the studied population was obtained from the published results of the MEDIS study16-18. A cumulative 'morbidity index' (range 0-4) indicating the overall burden of CVD risk factors of the referent population was developed based on whether the prevalence of hypertension, hypercholesterolemia, diabetes or obesity for a specific island was below or above the whole population median. Islands with a prevalence of each condition below the median value received the score 0, islands above received score 1.
Statistical analysis
Continuous variables are presented as median (1st, 3rd quartile) due to their skewed distributions. Categorical variables are presented as frequencies. Poisson regression was applied to evaluate whether dieticians' characteristics and the nutritional services were associated with the population-specific count of people having hypertension, hypercholesterolemia, diabetes and obesity. The total number of participants per island was included in all models as covariate. Results are expressed as β-coefficients with 95% confidence intervals. The Akaike information criterion was used to test the model's goodness-of-fit.
Logistic regression was used to evaluate the association between the aforementioned characteristics on the likelihood of having hypertension, hypercholesterolemia, diabetes and obesity above the population-specific median prevalence of these conditions (which was considered as at increased risk). Results are expressed in odds ratios and 95% confidence intervals. Deviance residuals and Hosmer-Lemeshow criterion have been used to evaluate the logistic models' goodness-of-fit. The Wald test was used to evaluate the strength of an association. Potential co-linearity between the variables was evaluated by the calculation of the correlation of estimates (values >0.4 suggested co-linearity and the variable being removed from the model). Thus, variables entered in each model were those that had a significant effect on the investigated outcome in the explanatory analysis and did not show any co-linearity. Nagelkerke's R2 was also calculated as a pseudo indicator of how much of the outcome variation was explained by the model. All tested hypotheses were two-sided. Finally, to further explore which of the dieticians' characteristics or nutritional services had the best classification ability in terms of low or high disease burden, discriminant analysis was applied using Wilks' Lambda as the statistic that discriminates the tested variables (ie lower values of the statistic suggest better discriminating ability; 1-lambda is the proportion of variance that is accounted to the specific factor). A p-value <0.05 was considered as statistically significant and SPSS v14 software was used for all calculations (www.spss.com).
Distribution of nutrition services in the studied islands
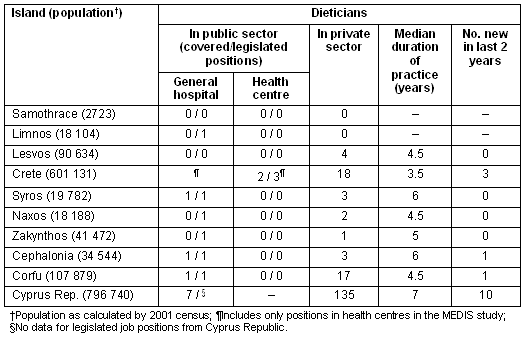
As mentioned, there was a great variation in the number of dieticians practising on the studied islands (eg from 0 to 20 in Crete and up to 142 in the Cyprus Republic (Table 2). The median duration of dieticians' practice on an island was 5 years, with the lowest only 6 months and the highest 30 years (both in the Cyprus Republic). On some islands almost one in four dieticians had been practising for less than 2 years. The percentage of legislated and available positions that were filled (according to the national health system plan) ranged in the public sector from 0% (ie no available positions filled) to 100% (ie all positions filled). In Samothrace and Lesvos there were no legislated job positions in the public sector.
Table 2: Distribution of practising dieticians on studied islands
Reasons using nutritional services among older individuals
The reasons presented for using nutritional services are based on information provided by the dieticians (Table 1). The most frequent reason for an older person to visit a dietician was on their physician's recommendation, followed by a friend's suggestion. The majority of the older individuals visited a dietician to consult about control of blood glucose levels, followed by control of blood lipids and weight management. Only 45% of the older clients completed their nutritional intervention sessions. Financial reasons (39%) and long distance from home to the dietician's office (23%) were the major reasons for ceasing visits.
Data analysis of the participants' responses revealed that only 33% reported visiting a dietician for nutrition counselling during the study period. Approximately 33% of the participants reported that nutrition services were absent from the island and 24% believed that these were inadequate. Almost 40% correctly believed there was no community nutritional education program on their island, with 60% responding that they were unaware of whether one existed.
Modelling older populations' health status in relation to reasons using nutrition services
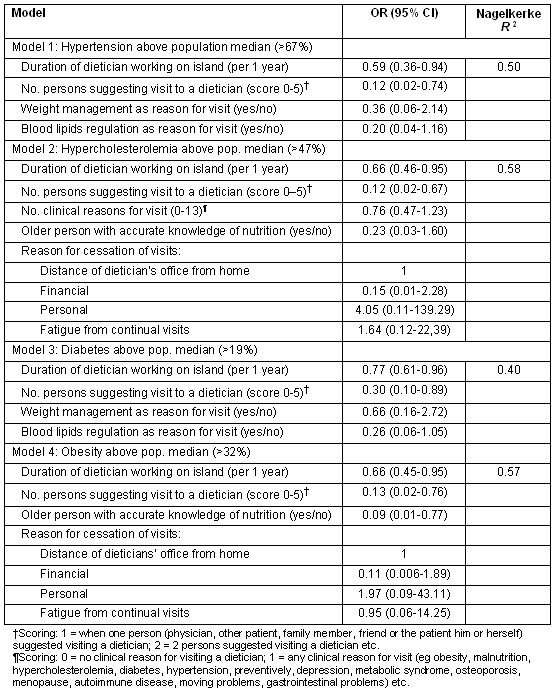
The median prevalence of the cardio-metabolic risk factors was found to be 67% for hypertension, 47% for hypercholesterolemia, 19% for diabetes and 32% for obesity (Table 3). The mean value of the 'morbidity index' was 1.7±0.3, suggesting that on average each individual had approximately two of the aforementioned CVD risk factors. The values of the index varied from island to island (Aegean islands 1.8±0.3 vs Crete 2.4±0.1 vs Ionian Islands 1.5±0.8 vs Cyprus 1.7±0.1, p<0.001). Poisson regression analysis revealed that the years of dieticians' presence on an island was associated with a lower prevalence of hypertension (β=-0.012±0.001, p<0.001), hypercholesterolemia (β=-0.007±0.001, p<0.001), diabetes (β=-0.012, p<0.001) and obesity (β=-0.012±0.002, p<0.001). Logistic regression analysis revealed that the longer the duration of a dietician practising on an island and the more people who suggested an older person visit a dietician, the lower the likelihood of the prevalence of hypertension, hypercholesterolemia, diabetes and obesity above the island-specific median of the referenced population (Table 3). There was no association between reasons for ceasing dietician consultations and population health status.
Table 3: Results of multiple logistic regression models applied to evaluate population health status in relation to nutritional services reported by participating dieticians (n=88) for both private and public healthcare systems
Based on the developed 'morbidity index', the hierarchical discriminant analysis revealed that the most significant discriminating nutritional service factors were: the number of dieticians practising in the private sector (Wilk's Lambda=0.004, p<0.001), followed by the number of dieticians on islands (Wilk's Lambda=0.01, p<0.001), the number of dieticians in the public sector (Wilk's Lambda=0.52, p=0.009) and the ratio of filled/available dietician's job position in hospitals (Wilk's Lambda=0.52, p=0.009). This explained the variation in the morbidity among older adults on the studied islands. Additionally, almost all values of Wilk's Lambda, except for the duration of a dietician's practice on the island, were close to 0, suggesting high discriminating ability. Further hierarchical discriminant analysis revealed that obesity (Wilk's Lambda=0.84, p=0.009) and a friend's suggestion to visit a dietician (Wilk's Lambda=0.84, p=0.01), followed by hypertension (Wilk's Lambda=0.88, p=0.04) were the most important clinical discriminating factors of the variation in morbidity among the islands.
Discussion
This work evaluated the impact of nutritional services offered by dieticians in the public or the private sector on the health status of a sample of older people living on Mediterranean islands. The study revealed that the presence of dieticians in the healthcare system was associated with a reduced likelihood of hypertension, diabetes, hypercholesterolemia and obesity among the older adult population studied. The number of dieticians working on an island was the most important factor explaining variation in morbidity.
Other studies have reported that a higher number of physicians is associated with a lower mortality from CVD and cancer6-8. It is remarkable that almost none of these studies evaluated the potential influence of other components of the healthcare system. In the USA and European Union, dieticians and nutrition practitioners work in the treatment and prevention of disease (administering medical nutrition therapy as part of medical teams), often in hospitals, medical organizations, private practice or other healthcare facilities. In addition, a large number of dieticians work in community and public health settings20,21.
In Greece, available data show moderate-to-adequate availability of physicians and deficits in nursing personnel, with wide discrepancies in their distribution within the country22,23. Recent Greek studies have also underlined the necessity for re-organisation of the national healthcare system24,25. Nevertheless, data regarding the number of dieticians are limited. This study revealed deficits in the supply of dieticians in the public sector on the studied islands. Furthermore, in some areas there was no dietician to offer nutritional services (ie assessment, diagnosis, intervention, monitoring and education). There were either no legislated job positions for dieticians (in hospital or health centres) or the job positions were vacant. Health centres and their rural satellite units are the cornerstone of the Greek primary healthcare system26. Moreover, except for Crete, none of the studied Greek islands had a health centre with a practising dietician. This finding concurred with the belief of the majority of older islanders that nutritional services and education programs in their area were absent and inadequate.
Further data analysis revealed that the longer a dietician was practising on an island, the lower the observed prevalence of hypertension, hypercholesterolemia, diabetes and obesity above the median level. Dietetic support is considered to be an important aspect of the prevention of these conditions, and diet with healthier lifestyle recommendations and emotional support may assist people to live better and longer27. Nutritional consultation can achieve beneficial changes in the quality of diet as well as the levels of CVD risk factors28,29. The aforementioned studies underline the major preventive role of nutritional services within the community, and the dietician's key role of nutritional educator in public health nutrition.
In this study, the most common medical reasons for visiting a dietician were diabetes control, followed by hypercholesterolemia, obesity and hypertension. The association between obesity, diabetes, hypercholesterolemia, combined with a lack of awareness of these in many of older individuals, may predispose to a higher risk of CVD and mortality30,31. However, few older people visited dieticians for preventative reasons.
As early as Hippocrates (460-370 BCE) it has been understood that prevention is better than treating a disease. Public health services should focus on this presumption because older adults are a population group with special needs, especially those living in rural or remote areas. Many lose interest in food, have chewing difficulties, experience difficulties in meal preparation and suffer from financial restraints32. Other studies have revealed that elderly inhabitants of rural areas are likely to suffer from poorer health due to the social exclusion of low access to services (health access), facilities and social networks23,33. The data from the present study supports this, because living a long distance from the dieticians' office (ie lack of mobility) was a major reason for ceasing nutritional sessions.
Nutritional education has the opportunity to improve the health and quality of life of older adults. Therefore, home and community nutritional care from visiting specialists could greatly benefit older people in rural areas34. The promotion of healthy aging should involve rectifying any lack of nutritional services (at home- or community-level) and improving the nutritional capacity of a region, for example, adequate an number of staff and infrastructure35. This provides a benefit not only to the recipients, but also may reduce stress on caregivers to assist in maintain their health and wellbeing36.
Limitations of this study
The present study is limited by its observational design, and therefore cannot provide causal relationships. In addition, the number of physicians on each island was not considered. However, all investigated islands had had an adequate number of physicians for primary and/or secondary health care for at least 10 years. Therefore, this factor was not included in the developed models because it would behave as a constant rather than a variable. As all communities in this study were based on remote islands, the findings of this study may not be generalizable to non-island communities.
However, the role of nutritional services seems to be underestimated in the majority of countries37, the presented findings provide evidence that dieticians may make a difference to the prevalence of chronic diseases among the older people. Dieticians, together with physicians and other general practitioners, may assist in better preventing disease burden and improving quality of life of the elderly population. These findings have important implications for rural and remote workforce policy and funding, reinforcing the need for a more accessible nutritional workforce in these regions.
Acknowledgements
The authors are particularly grateful to the participants from the islands of Cyprus, Lesvos, Samothrace, Crete, Corfu, Limnos, Zakynthos and Cephalonia, who participated in this research. The authors also express their gratitude to Professor C Lionis; Doctors C Lazarou, A Zeimbekis, F Anastasiou, P Stravopodis, A Skamagathis, E Gotsis, V Vountziouka and D Antoniadis; the Hellenic Association of Hospital Dieticians; the Cypriot Dietetic Association; and the Hellenic Technological Association of Dieticians and Nutritionists for their substantial assistance in retrieving about health and nutritional data. Finally, the authors thank the reviewers who assisted in improving the presentation of the findings and revealing the importance of the work. The study was performed under the auspices of the Hellenic Dietetic Association. Stefano Tyrovolas received a scholarship from the Hellenic Atherosclerosis Society and Foundation for Education and European Culture (IPEP) to undertake his PhD thesis, of which this work is part.
References
1. Mathers CD, Iburg KM, Salomon JA, Tandon A, Chatterji S, Ustün B et al. Global patterns of healthy life expectancy in the year 2002. BMC Public Health 2004; 4: 66.
2. World Health Organization. Active ageing: a policy framework. (Online) 2002. Available: http://whqlibdoc.who.int/hq/2002/WHO_NMH_NPH_02.8.pdf (Accessed 16 June 2010).
3. Stefanadis C. Seeking the secrets of longevity. Hellenic Journal of Cardiology 2010; 51: 479-480.
4. Watt GCM, Ecob R. Analysis of falling mortality rates in Edinburgh and Glasgow. Journal of Public Health Medicine 2000; 22: 300-336.
5. Mackenbach JP, Looman CW, Kunst AE, Habbema JD, van der Maas PJ. Post-1950 mortality trends and medical care: gains in life expectancy due to declines in mortality from conditions amenable to medical intervention in The Netherlands. Social Science & Medicine 1988; 27: 889-894.
6. Starfield B, Shi L, Macinko J. Contribution of primary care to health systems and health. Milbank Quarterly 2005; 83: 457-502.
7. Shi L. Primary care, specialty care, and life chances. International Journal of Health Services: Planning, Administration, Evaluation 1994; 24: 431-458.
8. Shi L, Macinko J, Starfield B, Wulu J, Regan J, Politzer R. The relationship between primary care, income inequality, and mortality in United States, 1980-1995. Journal of the American Board of Family Medicine 2003a; 16: 412-422.
9. McKeown T. The role of medicine: dream, mirage, or nemesis? London: Nuffield Provincial Hospitals Trust, 1976.
10. Keys A, Menotti A, Karoven MI. The diet and the 15-year death rate in the Seven Countries Study. American journal of Epidemiology 1986; 124: 903-915.
11. Jones C, Palmer TEA, Griffiths RD. Randomised clinical outcome study of critically ill patients given glutamine-supplemented enteral nutrition. Nutrition 1999; 15: 108-115.
12. Taylor S, Fettes SB, Jewkes C, Nelson RJ. Prospective, randomized controlled trial to determine the effect of early enhanced enteral nutrition on clinical outcome in mechanically ventilated patients suffering head injury. Critical Care Medicine 1999; 27: 2525-2531.
13. Kruizenga HM, Van Tulder MW, Seidell JC, Thijs A, Ader HJ, Van Bokhorst-de van der Schueren MA. Effectiveness and cost effectiveness of early screening and treatment of malnourished patients. American Journal of Clinical Nutrition 2005; 82: 1082-1089.
14. Delahanty LM. An expanded role for dieticians in maximising retention in nutrition and lifestyle intervention trials: implications for clinical practice. Journal of Human Nutrition and Dietetics: the Official Journal of the British Dietetic Association 2010; 23: 336-343.
15. Curry KR, Jaffe A. Nutrition counseling & communication skills, Philadelphia, PA: WB Saunders, 1998.
16. Tyrovolas S, Polychronopoulos E, Bountziouka V, Zeimbekis A, Tsiligiani I, Papoutsou S et al. Level of adherence to the Mediterranean diet among elderly individuals living in Mediterranean islands: nutritional report from the MEDIS Study. Ecology of Food and Nutrition 2009; 48: 76-87.
17. Tyrovolas S, Zeimbekis A, Bountziouka V, Voutsa K, Pounis G, Papoutsou S et al. Factors associated with the prevalence of diabetes mellitus among elderly men and women living in Mediterranean islands: the MEDIS Study. The Review of Diabetic Studies 2009; 6: 54-63.
18. Tyrovolas S, Lionis C, Zeimbekis A, Bountziouka V, Micheli M, Katsarou A et al. Increased body mass and depressive symptomatology are associated with hypercholesterolemia, among elderly individuals; results from the MEDIS study. Lipids in Health and Disease 2009; 8: 10.
19. Writing Group of the Nutrition Care Process/Standardized Language Committee et al. Nutrition care process and model part I: the 2008 update. Journal of the American Dietetic Association 2008; 108: 1113-1117.
20. European Federation of the Associations of Dietitians (EFAD). European dietetic competences and their performance indicators attained at the point of qualification and entry to the profession of dietetics. (Online) 2009. Available: http://www.efad.org/everyone/1653/7/0/32 (Accessed 5 June 2010).
21. Stitzel KF, American Dietetic Association. Position of the American Dietetic Association: the roles of registered dieticians and dietetic technicians, registered in health promotion and disease prevention. Journal of the American Dietetic Association 2006; 106: 1875-84.
22. Tountas Y, Karnaki P, Pavi E. Reforming the reform: the Greek national health system in transition. Health Policy 2002; 62: 15-29.
23. Oikonomou N, Tountas Y. Insufficient primary care services to the rural population of Greece. Rural Remote Health 11:1661. (Online) 2011. Available: www.rrh.org.au (Accessed 12 September 2011).
24. Souliotis K, Lionis C. Creating an integrated health care system in Greece: a primary care perspective. Journal of Medical Systems 2005; 29: 187-196.
25. Lionis C, Symvoulakis EK, Markaki A, Vardavas C, Papadakaki M, Daniilidou N et al. Integrated primary health care in Greece, a missing issue in the current health policy agenda: a systematic review. International journal of Integrated Care 2009; 9: e88.
26. Lionis C, Tziraki M, Bardis V, Philalithis A. Seeking quality improvement in primary care in Crete, Greece: the first actions. Croatian Medical Journal 2004; 45: 509-603.
27. Haveman-Nies A, de Groot LCPGM, van Staveren WA. Dietary quality, lifestyle factors and healthy ageing in Europe: the SENECA study. Age Aging 2003; 32: 427-434.
28. Brunner EJ, Rees K, Ward K, Burke M, Thorogood M. Dietary advice for reducing cardiovascular risk. Cochrane Database of Systematic Reviews 2007; 4: CD002128.
29. Thompson RL, Summerbell CD, Hooper L, Higgins JP, Little PS, Talbot D et al. Dietary advice given by a dietician versus other health professional or self-help resources to reduce blood cholesterol. Cochrane Database of Systematic Reviews 2003; 3: CD001366.
30. Dey DK, Lissner L. Obesity in 70-year-old subjects as a risk factor for 15- year coronary heart disease incidence. Obesity Research 2003; 11: 817-827.
31. Salihu HM, Bonnema SM, Alio AP. Obesity: what is an elderly population growing into? Maturitas 2009; 63: 7-12.
32. Baker H. Nutrition in the elderly: diet pitfalls and nutrition advice. Geriatrics 2007; 62: 24-26.
33. Haynes R, Gale S. Deprivation and poor health in rural areas: inequalities hidden by averages. Health Place 2000; 6: 275-285.
34. Millen BE, Ohls JC, Ponza M, McCool AC. The elderly nutrition program: an effective national framework for preventive nutrition interventions. Journal of the American Dietetic Association 2002; 102: 234-240.
35. Kamp BJ, Wellman NS, Russell C; American Dietetic Association; American Society for Nutrition; Society for Nutrition Education. Position of the American Dietetic Association, American Society for Nutrition, and Society for Nutrition Education: food and nutrition programs for community-residing older adults. Journal of the American Dietetic Association 2010; 110: 463-472.
36. Wellman NS, Rosenzweig LY, Lloyd JL. Thirty years of the Older Americans Nutrition Program. Journal of the American Dietetic Association 2002; 102: 348-350.
37. Tyrovolas S, Tountas Y, Polychronopoulos E, Panagiotakos DB. The implications of nutrition services within the health care system on the quality of life and longevity, in developed countries: a re-analysis of 38 studies. Central Europeam Journal of Public Health. 2011; 19: 13-9.
