Mental health literacy has been defined as 'knowledge and beliefs about mental disorders, which aid in their recognition, management, and prevention' (p396)1. Depression literacy is a specific type of mental health literacy and is defined as the ability to recognize depression and make informed decisions about treatments for depression2. Jorm et al proposed that like health literacy, people with high mental health literacy would have similar knowledge and beliefs about mental disorders and treatment for mental health and medical professionals (eg use similar names to describe symptoms and see medical and mental health professionals as appropriate treatment providers)3.
The prevalence and impact of mental health and depression literacy has been studied extensively in Australia3-10 and also in Canada, India, and among African-American clergy2,6,7,11-14. The study of mental health literacy began in 1995 when Jorm et al3 explored the mental health literacy of a representative sample of Australians, using vignettes depicting a person experiencing the symptoms of a major depressive disorder and schizophrenia. That study revealed that only 39% of Australians could correctly label the depression vignette, and that doctors, counselors and a close friend and family were most frequently cited as sources of help for the symptoms described in the vignette. Partly due to these findings, the Australian government launched a national depression initiative aimed at improving mental health literacy8,9,15. A follow-up study of mental health literacy revealed that the ability to correctly label a vignette describing depressive symptoms had increased from 39% to 67% when the depression initiative was in its third year7.
Studies have also shown that rates of depression literacy vary among populations2,6,7,11 and there is evidence that men have lower mental health literacy compared with women2,16. There is a paucity of research on the depression literacy of rural Americans. This gap in research is particularly problematic given that people living in rural areas have lower rates of specialty mental health service utilization, despite experiencing equivalent prevalence of mental disorders to those in more urban areas17-19. The research on mental health literacy in rural populations has primarily been conducted in Australia, where researchers have not found a rural-urban difference in the ability to identify depression; however, it was found that those living outside major cities regarded counselors or psychologists as less helpful than those who lived in major metropolitan cities4.
Research has demonstrated that due to a shortage of mental health specialists in rural areas, primary care and informal networks such as the religious community have become the 'de facto' mental health system20,21. Additionally, rural populations have been found to have lower perceived need for and utilization of specialty mental health providers (eg counselors) than urban populations4,21,22. Due to these unique factors in rural help-seeking, this study also examined how depression literacy is related to perceived need for and utilization of a doctor, counselor, or religious leader.
Perceived need is the belief that treatment is needed23. Because perceived need is a personal, subjective judgment it does necessarily correspond with the evaluation and diagnosis of a health professional24. A person does not decide to seek treatment until they perceive the need to do so (unless they are persuaded by someone else). Research on the rural population supports the idea that perceived need is important in the decision to seek mental health treatment. For example, outreach activities targeted to rural populations are not successful unless they can convince individuals that treatment is needed21,25.
In addition to perceived need, this study explores the relationship of depression literacy with utilization of a medical provider, mental health specialist, and religious leader for emotional problems. Knowledge about symptoms and illness processes can potentially impact on when and whether people seek help. In the health literacy literature, low health literacy has been associated with delayed help-seeking for prostate cancer, while improved health literacy has been associated with increased utilization of mammography services26-28. Similarly, lack of mental health literacy has been associated with delays in seeking treatment for mental health issues16. The choice of a medical, specialty mental health, and religious leader or alternative as variables in this study stemmed from previous research that rural populations often rely on medical and alternative healer providers and utilize specialty mental health services less than their urban counterparts4,20-22. Exploring these relationships may increase understanding of how knowledge and labeling of symptoms influences utilization decisions for rural populations.
The primary purpose of this study was to determine rates of depression literacy and variables related to depression literacy in a rural, mid-southern US sample. In addition, a person's ability to label depressive symptoms accurately was assessed as related to perceptions of need and utilization of treatment from a: (i) primary care provider; (ii) counselor or therapist; and (iii) preacher or pastor. Because depression literacy has been hypothesized in the literature to increase concordance of professional and public opinions about need for mental health treatment3, it was hypothesized that:
- Those with higher depression literacy will have a higher perceived need for a doctor or counselor than a religious leader.
- Those with high depression literacy will be more likely to have sought help from a doctor or counselor than a religious leader.
Defining rurality
The present study incorporated a definition of 'rural' posed by Crumartie and Bucholts29, along with consideration of population size, adjacency to urban areas, and economic influence to distinguish rural participants. Specifically, 'rural' was defined as living in a town of less than 5500 people that is situated outside the major commuting and economic patterns of the metropolitan area (ie living at least 30 min outside major cities with populations ≥30 000). Participants were recruited at local rural grocery stores to increase the likelihood that their economic activity was centered in the rural community. Further information about the definition of the sample is available elsewhere30.
Recruitment and sample
Participants were recruited inside and outside local grocery stores in two towns with populations less than 5500. These towns were located 45 min and 2 hours from major metropolitan areas. Research assistants sat at a table containing posters, flyers, and information about the study. People passing by who showed an interest in the study were asked if they would like to help with a survey from the University of Arkansas. The research protocol was explained and people who were interested signed up for the study by providing their name, telephone number, and the best time to be called. Each person completing the survey was mailed a US$15 gift certificate to the local grocery store. Only people who showed interest in the study were asked to participate.
The recruitment materials and study methods were approved by the University of Arkansas Institutional Review Board (IRB) and steps were taken to ensure the confidentiality of participants (eg participants were not required to provide their family name and were given the choice to call to sign up rather than leave their contact information with the recruiters).
This recruitment strategy was used to gain access to a rural community sample that conducts its business within the local community, and is similar to the Rost et al approach to recruitment25. Unlike in urban areas, most rural areas only have one grocery store, and according to the Center for Rural Affairs (a non-profit Nebraska-based organization), commerce through the local grocery stores consists mostly of people who live and work within these communities. Those who work outside the community, or commute, are more likely shop in the areas where they work31.
A total of 268 participants were recruited (34.8% male, 64.8% female), and of 39% (n = 105) were successfully contacted by telephone and agreed to participate (35% of the women and 46% of the men who were initially recruited: χ2 = 2.9, df = 1, p = 0.09). Due to difficulty recruiting men for the study and in order to have a representative sample, there was increased effort made to have recruited men complete the survey. Most of the participants lived in the counties that contained the grocery store they visited (87.3%); the remainder indicated they lived in neighboring counties. Some of those recruited were not contacted due to completion of data collection (n = 40). Three attempts were made to reach each participant by telephone and messages were left when possible. No further contact attempts were made for those who were not reached after 3 attempts (n = 89), for those recruited but declined to participate (n = 3), or for participants whose telephone number was incorrect or the number was disconnected (n = 31). Of the 105 people contacted who completed the interview (44% male); six were excluded from the sample because their reported zip (postal) code was for a city with a population more than 5500. Therefore, the total number of participants included in the final sample was 99, of which 43% were male (Fig1).
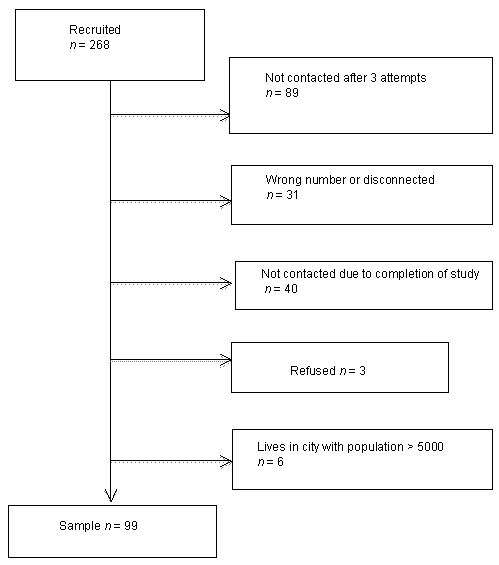
Figure 1: Consort diagram.
Procedures
Participants who were contacted and gave verbal informed consent over the telephone before beginning the survey. The survey took approximately 15 min to complete.
Measures
Sociodemographic information: A variety of sociodemographic variables were assessed during the interview including age, sex, ethnicity, and educational attainment (Table 2).
Depression literacy: Depression literacy was assessed with a vignette created by Rost et al25 that describes a person experiencing symptoms consistent with a major depressive episode (Fig2). The vignette was modified to direct address style but otherwise retained all essential elements of the story. The vignette was created to be used in both rural and urban samples and therefore was not modified to reflect a rural lifestyle. After the vignette was read to participants they were asked whether they thought the situation described in the vignette was a problem for them, and those who answered 'yes' were asked what they would call the problem.
Participants were considered to have high depression literacy if they:
- Reported that the situation described in the vignette was a problem.
- Accurately labeled the problem 'depression' (or used some form of the word).
Participants were considered to have low depression literacy if they:
- Did not consider the situation a problem.
- Provided any other label for the vignette (eg stress).

Figure 2: Vignette used to determine depression literacy (adapted from Rost et al24).
Coding for the high and low depression literacy variables was conducted by the first author (TD) and was also coded independently by a contributor to the manuscript. All answers that included 'depression', 'depressed', 'depressive' were coded as high depression literacy. Any discrepancies were discussed and resolved. All answers coded 'not a problem' and any other label that did not include a form of the word 'depression' were coded as low depression literacy. If a participant provided more than one label, their response was coded as high depression literacy if any of those labels met the criteria; otherwise the response was coded as low depression literacy.
Depression symptoms: Self-reported symptoms of mental illness in the past year were assessed using a modified version of the Brief Symptom Inventory-18 (BSI-18)32. The BSI-18 has been demonstrated to have good internal consistency, with Cronbach's α = 0.89 and item-to-item correlations of 0.37-0.7033. For the current study, only 17 of the 18 questions were used because the question related to suicidal ideation was excluded (due to IRB concerns about non-clinician students asking participants about suicidal ideation over the telephone). To expand the time period for measured symptomology, the BSI-18 instructions were also modified by asking people to endorse whether they had experienced symptoms in the past year, rather than the past week. For the purposes of this study, the Depression Index score was computed according to the BSI-18 instructions, adjusting for the omission of one item32. Despite the modifications made to the measure, the scoring allows for the omission of one item per scale and the internal reliability of the Depression Index score was good (α = 0.84)30.
Perceived need for services: To measure perceived need for services, participants were asked to imagine they were experiencing the symptoms in the vignette. A question then assessed if the participants believed they should seek help from: (i) a doctor; (ii) a counselor or therapist; and (iii) a religious leader. Each response was recorded on a 4 point scale from 'definitely yes' to 'definitely no'. Higher scores indicated greater perceived need for that service30.
Service utilization: Lifetime use of medical professionals, specialty mental providers, and religious or alternative healers for emotional, mental health or substance abuse problems was measured using a series of questions from the National Survey of American Life34. Mental health service utilization was defined as seeking the help of a psychiatrist, psychologist, social worker, or counselor for an emotional or substance abuse problem at some point in the past. Medical service utilization was defined as seeking the help of a primary care physician or specialty physician (eg obstetrician, cardiologist) for an emotional or substance abuse problem at some point in the past. Utilization of a religious leader was defined as seeking the help of a religious leader or alternative healer for an emotional or substance abuse problem at some point in the past30.
Statistical analyses
The relationship between high depression literacy and various demographic, psychiatric, utilization, and perceived need variables was explored by conducting bivariate analyses. Bivariate analyses (Χ2, Fisher's exact tests, and t-tests) were conducted to examine the relationships among the variables measured. Multivariable logistic regression analyses were conducted to better understand how variables related to depression literacy and to test hypotheses 1 and 2 examining how demographic and depression literacy related to perceived need for and utilization of services for emotional problems. The regression analyses predicting depression literacy and perceived need were conducted with the entire sample (n = 99), while the analysis predicting service utilization was limited to participants who endorsed lifetime help-seeking for an emotional problem (n = 45). Statistical significance was set at an α level of 0.05; however, due to the exploratory nature of this study, only predictors with odds ratios above 1.5 or below 0.5 were considered relevant to the findings of this study.
The final sample (N = 99) was 43% male and 92% self-identified as White. Due to the low number of racial and ethnic minorities in this sample, race was not included in the regression analyses. The average age was 45.4 years (SD = 15.3); 57% reported an annual household income of less than US$25,000 and 18% had less than a high school education. Detailed demographic information is provided in Table 1 and elsewhere30.
Table 1: Sample demographic information (N = 99)32

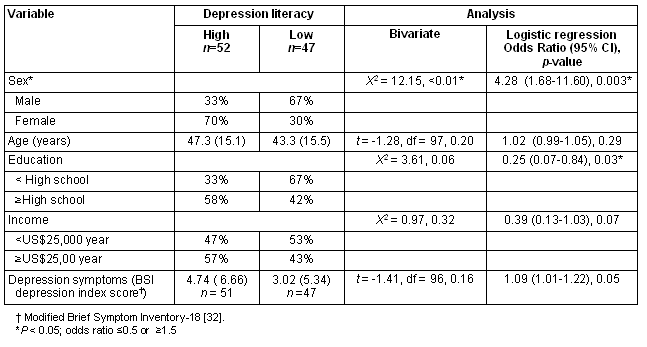
First, the prevalence of high depression literacy was determined the (eg the percentage calculated of those who both stated that the vignette would be a problem for them and accurately labeled the vignette) and the bivariate and multivariable relationships were explored among depression literacy, sex, age, income and education. Results revealed that only 53% of the total sample had high depression literacy. A large sex difference in depression literacy emerged, with 68% of women accurately identifying the symptoms as depression compared with only 35% of men (Χ2 = 12.15, p = 0.01). Education, age, and income (calculated as less than US$25,000 in annual income) did not have significant bivariate relationships with depression literacy. Additionally, depression symptoms on the BSI-18 (high depression literacy M = 4.74, SD = 6.66, n = 51; low depression literacy M = 3.02, SD = 5.34, n = 47) did not have a significant bivariate relationship with depression literacy (Table 2).
To better understand the relationship among these variables, a logistic regression analysis was conducted with age, sex, education (< high school) and income (< US$25,000/ year) as the independent variables and depression literacy as the dichotomous dependent variable. Results revealed sex (OR = 4.28, 95% CI = 1.68-11.60, p = 0.003), continued to have a significant relationship with depression literacy. Additionally, education had a significant relationship with depression literacy (OR = 0.25, 95% CI = 0.07-0.84, p = 0.03; Table 2) with those with less than a high school education being more likely to have low depression literacy.
Table 2: Bivariate and mulitvariable analyses by depression literacy status32
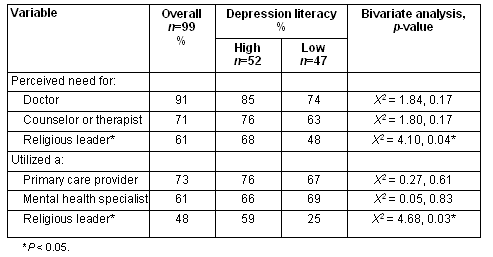
Next, the bivariate associations were explored between depression literacy and perceived need for and utilization of services for emotional problems (Table 3). There was not a statistically significant difference in the relationship of depression literacy and perceived need for a doctor or a counselor. There was a statistically significant relationship between depression literacy and perceived need for a religious leader with those with higher depression literacy being more likely to perceive a need for a religious leader and than those with low depression (Χ2 = 4.10, 0.04; Table 3). Results for utilization of services for emotional problems revealed that there was not a statistically significant relationship between depression literacy and utilization of a doctor or a mental health specialist for emotional problems. However, there was a statistically significant relationship among depression literacy and the utilization of a religious leader for an emotional problem (Χ2 = 4.68, 0.03). Those with high depression literacy were more likely to have sought help from a religious leader than those with low depression literacy (Table 3).
Table 3: Differences in perceived need and past utilization of mental health services
for those with high and low depression literacy
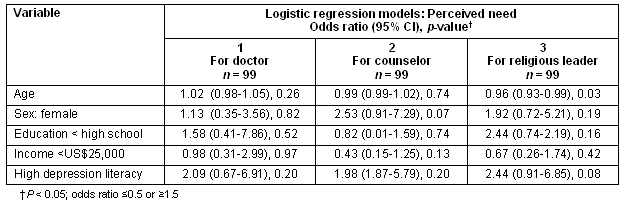
To test the first hypothesis that having higher depression literacy would be significantly associated with perceived need for a doctor and counselor but not a religious leader, a three logistic regression model was conducted predicting perceived need for a doctor, counselor, and religious leader with common predictors of perceived need (age, sex, income, and education) and depression literacy as predictor variables (Table 4). Contrary to the first hypothesis, results of the first and second regression equations revealed that none of the predictor variables in the equation were significant predictors of perceived need for a doctor or a counselor. After controlling for demographic and symptom variables, depression literacy was not a significant predictor of perceived need for a religious leader (Table 4).
Table 4: Logistic regression models predicting perceived need for a doctor, counselor and religious leader
To test the second hypothesis that having higher depression literacy would predict utilization of a medical provider and specialty mental health provider but not a religious leader or alternative healer, a three logistic regression model was conducted predicting past utilization of a medical provider, specialty mental health provider and religious leader or alternative healer with common predictors of utilization (age, sex, income, depression symptoms and education) and depression literacy as predictor variables; Table 5). Results of the first regression equation revealed that participants with more education were more likely to utilize a medical professional for an emotional problem (OR = 21.98, CI = 2.01-674.45, p = 0.03). Contrary to the second hypothesis, depression literacy was not significantly associated with utilization of a medical provider. The results of the second regression equation revealed that none of the independent variables was a significant predictor of utilization of a specialty mental health provider for emotional problems (Table 5). Results of the third regression equation revealed that depression literacy (OR = 10.08, 95% CI = 1.74-92.79, p = 0.02) was a significant predictor of utilization of a religious leader or alternative healer for emotional problems (Table 5).
Table 5: Logistic regression models predicting utilization of a medical professional
, mental health professional, and a religious leader or alternative healer among participants
that endorsed lifetime help seeking for emotional problems32

Discussion
The present study revealed that, while the vast majority of participants described the situation in the vignette as a problem, only 53% of respondents were able to accurately label symptoms described in the vignette as 'depression' or use some form of the word to describe it. This percentage is higher than the 39% and 48% reported in rural and urban Australian samples in 1995 and 20011,10. However, the percentage found in this sample is lower than 76% reported for a Canadian sample in 20062, 68% in an Australian sample and 81% in a rural Australian sample in 20046,7. This suggests that depression literacy has improved with time in some areas of the world but that some rural Americans may have lower depression literacy than rural residents in other parts of the world. Consistent with previous research, men in this study had lower rates of depression literacy than women2 and this effect remained after controlling for the age, education, income, and depression symptoms of the sample. Also consistent with previous literature6 was that participants who personally experienced symptoms of depression in the past year had higher depression literacy than those who did not experience depression. This is consistent with previous findings that a greater familiarity with depression, either from personal experience or knowing others who have suffered from depression, is associated with higher depression literacy5. Higher education levels were also associated with higher depression literacy in the present sample.
In contrast to the stated hypothesis of this study, higher depression literacy was not significantly associated with perceived need for and utilization of a medical professional or mental health professional. In fact, both perceived need for and past utilization of a religious leader for emotional problems had strong bivariate associations with depression literacy, and depression literacy continued to have a significant relationship with utilization of a religious leader in multivariable analyses controlling for age, sex, education, income, and depressive symptoms. This association has not been reported in previous research.
These interesting findings may be related to several cultural and environmental factors in the rural area studied. First, it may be that cultural beliefs about depression include a spiritual component, prompting the perceived need for a religious leader, and that other explanations (eg following stress or due to fatigue) do not. It may also be that religious leaders in rural areas of the USA see counseling as an important part of their role and provide psycho-education and counseling for those in the community, prompting people in these communities to perceive a need to talk to religious leaders when they encounter depression specifically. This idea is supported by a study that found rural African American clergy have high depression literacy35. In contrast, research on services provided by rural and urban churches found that predominately African-American churches provide more mental health and social services than predominately White churches36; this, however, does not preclude a rural, predominately White sample from seeking mental health services from a religious leader.
Because of the preliminary nature of these findings, further research should be conducted to look at the specific relationship of depression literacy and the use of religious leaders for emotional problems in rural areas. Specifically, the relationship between being able to recognize symptoms of depression and choice of help-seeking providers should be explored in a larger sample. Also, qualitative studies of knowledge about and attitudes to mental health and religion should be explored to better understand this path of help-seeking. If rural Americans' beliefs about depression involve spirituality and religion in such a way that they are more likely to seek a religious leader when they recognize depression it will be important to: (i) include information about religion and spirituality in treatments for depression in this population; and (ii) provide education and assistance to rural religious leaders to improve the likelihood that they will link patients to appropriate services or provide services that will lead to improvement.
Limitations
This study has some important limitations. First, mental health service use was measured as past lifetime utilization and causal directions of mental health literacy to service use cannot be determined from the analysis. It is possible that a previous encounter with a helping professional, such as a religious leader who provided psycho-education about depression, may have increased depression literacy rates in participants, rather than depression literacy predicting willingness to seek help for emotional problems. Prospective studies can help address this limitation.
Second, although all of the participants in the study resided in towns with populations less than 5500, the sample was from a mid-southern US state with a predominately White population and may not be representative of the many rural or frontier areas in the USA; therefore, generalizations from this study to other rural populations should be made with caution. Also, recruiting outside grocery stores may lead to limited the generalizability of the sample due to selection bias (those who shop at the local grocery store and sign up for studies may be different from those who do not)31. However, as discussed, local grocery stores are considered social centers in rural areas and the study was attempting to recruit the type of people who would do their grocery shopping in a local grocery store and not commuters who do not have such ties to the local community.
Third, the survey did not employ a comparison group of urban American residents. Without this comparison group, it is impossible to determine to what extent the relations observed among the variables are unique to rural residents. Future studies should expand the study population to identify mental health literacy in other American populations. Finally, although the methods of this study are consistent with other measures of depression literacy, and studies have shown that this type of measurement can be used to measure changes in depression literacy1,4,5,10, the use of a hypothetical situation to simulate preferences and choices for treatment may not mirror the actual perceptions and choices people make when they are experiencing similar symptoms.
This study contributes to the current literature by investigating mental health literacy in a community sample of rural Americans. The results confirm previous findings that men have lower depression literacy compared with women. As such, campaigns to educate the public about mental illness, such as those launched in Australia, may do well to target men in particular8,9,15. The results of this study also suggest that rural Americans have lower depression literacy than populations in other developed countries. Finally, the connection of depression literacy and utilization of religious leaders should be further examined because these findings could have implications for addressing disparities in service utilization in rural populations through the religious community.
Acknowledgements
The authors acknowledge Tara McGahan MA, Arthur Andrews MA, Dara Dossett, and Megan Alexander for their help in recruitment, data collection, and data entry for this project. The authors also acknowledge Tia Carraway MS for her assistance in statistical analyses. This project was completed as part of the first author's dissertation study and was funded by an internal grant from the Marie Howell's Endowment to the University Of Arkansas Department of Psychology.
References
1. Jorm AF, Korten AE, Jacomb PA, Christensen H, Rodgers B, Pollitt P. "Mental health literacy": a survey of the public's ability to recognise mental disorders and their beliefs about the effectiveness of treatment. Medical Journal of Australia 1997; 166(4):182-186.
2. Wang J, Adair C, Fick G, Lai D, Evans B, Perry BW et al. Depression literacy in Alberta: findings from a general population sample. Canadian Journal of Psychiatry 2007; 52(7): 442-449.
3. Jorm AF. Mental health literacy. public knowledge and beliefs about mental disorders. British Journal of Psychiatry 2000; 177: 396-401.
4. Griffiths KM, Christensen H, Jorm AF. Mental health literacy as a function of remoteness of residence: an Australian national study. BMC Public Health 2009; 9: 92.
5. Eckert KA, Kutek SM, Dunn KI, Air TM, Goldney RD. Changes in depression-related mental health literacy in young men from rural and urban South Australia. Australian Journal of Rural Health 2010; 18(4): 153-158.
6. Bartlett H, Travers C, Cartwright C, Smith N. Mental health literacy in rural Queensland: results of a community survey. Australian and New Zealand Journal of Psychiatry 2006; 40(9): 783-789.
7. Jorm AF, Christensen H, Griffiths KM. The public's ability to recognize mental disorders and their beliefs about treatment: changes in Australia over 8 years. Australian and New Zealand Journal of Psychiatry 2006; 40(1): 36-41.
8. Jorm AF, Christensen H, Griffiths KM. Changes in depression awareness and attitudes in Australia: the impact of Beyondblue: the national depression initiative. Australian and New Zealand Journal of Psychiatry 2006; 40(1): 42-46.
9. Jorm AF, Christensen H, Griffiths KM. The impact of Beyondblue: the national depression initiative on the Australian public's recognition of depression and beliefs about treatments. Australian and New Zealand Journal of Psychiatry 2005; 39(4): 248-254.
10. Wright A, Harris MG, Wiggers JH, Jorm AF, Cotton SM, Harrigan SM et al. Recognition of depression and psychosis by young Australians and their beliefs about treatment. Medical Journal of Australia 2005; 183(1): 18-23.
11. Tieu Y, Konnert C, Wang J. Depression literacy among older Chinese immigrants in Canada: a comparison with a population-based survey. International Psychogeriatrics 2010; 22(8): 1318-1326.
12. Kermode M, Bowen K, Arole S, Joag K, Jorm AF. Community beliefs about treatments and outcomes of mental disorders: a mental health literacy survey in a rural area of Maharashtra, India. Public Health 2009; 123(7): 476-483.
13. Kermode M, Bowen K, Arole S, Pathare S, Jorm AF. Attitudes to people with mental disorders: a mental health literacy survey in a rural area of Maharashtra, India. Social Psychiatry and Psychiatric Epidemiology 2009; 44(12): 1087-1096.
14. Stansbury K, Schumacher M. An exploration of mental health literacy among African American clergy. Journal of Gerontology and Social Work 2008; 51(1-2): 126-142.
15. Highet NJ, Luscombe GM, Davenport TA, Burns JM, Hickie IB. Positive relationships between public awareness activity and recognition of the impacts of depression in Australia. Australian and New Zealand Journal of Psychiatry 2006; 40(1): 55-58.
16. Thompson A, Hunt C, Issakidis C. Why wait? Reasons for delay and prompts to seek help for mental health problems in an Australian clinical sample. Social Psychiatry and Psychiatric Epidemiology 2004; 39(10): 810-817.
17. Gamm LD, Hutchison LL, Dabney BJ, Dorsey AM. Rural healthy people 2010: a companion document to healthy people 2010. College Station, TX: The Texas A & M State University System Health Science Center, School of Rural Public Health, Southwest Rural Health Research Center, 2003.
18. Hauenstein EJ, Petterson S, Rovnyak V, Merwin E, Heise B, Wagner D. Rurality and mental health treatment. Administration and Policy in Mental Health 2006; 34(3): 255-267.
19. Kessler RC, Chiu WT, Demler O, Merikangas KR, Walters EE. Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the national comorbidity survey replication. Archives of General Psychiatry 2005; 62(6): 617-27.
20. Weaver AJ. Has there been a failure to prepare and support parish-based clergy in their role as frontline community mental health workers: a review. Journal of Pastoral Care 1995; 49(2): 129-47.
21. Fox J, Merwin E, Blank M. De facto mental health services in the rural south. Journal of Health Care for the Poor and Underserved 1995; 6(4): 434-468.
22. Gamm LG, Stone S, Pittman S. Mental health and mental disorders - a rural challenge: a literature review. In: Rural healthy people 2010: a companion document to healthy people 2010. College Station, TX: Texas A & M State University System Health Science Center, School of Rural Public Health, Southwest Rural Health Research Center, 2003.
23. Maddux JE, Brawley L, Boykin A. Self-efficacy and health behavior: prevention, promotion, and detection. In: JE Maddux (Ed.). Self-efficacy, adaption, adjustment, theory, research, and application. New York: Plenum, 1995.
24. Rost K, Smith GR, Taylor JL. Rural-urban differences in stigma and the use of care for depressive disorders. Journal of Rural Health 1993; 9(1): 57-62.
25. Mojtabai R, Olfson M, Mechanic D. Perceived need and help-seeking in adults with mood, anxiety, or substance use disorders. Archives of General Psychiatry 2002; 59(1): 77-84.
26. Bennett CL, Ferreira MR, Davis TC, Kaplan J, Weinberger M, Kuzel T et al. Relation between literacy, race, and stage of presentation among low-income patients with prostate cancer. Journal of Clinical Oncology 1998; 16(9): 3101-3104.
27. Davis TC, Berkel HJ, Arnold CL, Nandy I, Jackson RH, Murphy PW. Intervention to increase mammography utilization in a public hospital. Journal of General Internal Medicine 1998; 13(4): 230-233.
28. Berkman ND, DeWalt DA, Pignone MP, Sheridan SL, Lohr KN, Lux L et al. Literacy and health outcomes. Evidence Report/Technology assessment no. 87; ARHQ pubn no 04-E007-2. Rockville, MD: Agency for Healthcare Research and Quality, 2004.
29. Cromartie J, Bucholtz S. Defining the "rural" in rural America. Amber Waves 2008; 6(3): 28-34.
30. Deen TD, Bridges AJ, McGahan TC, Andrews AA. Cognitive appraisal of specialty mental health services and their relation to mental health service utilization in the rural population. Journal of Rural Health 2011; (in press).
31. Bailey JM. Rural grocery stores: importance and challenges. Lyons, NE: Center for Rural Affairs Rural Research and Analysis Program; 2010 October 2010.
32. Derogatis LR. BSI-18: Administration, scoring and procedures manual. Minneapolis, MN: National Computer Systems, 2000.
33. Zabora J, Brintzenhofe-Szoc K, Jacobsen P, Curbow B, Piantadosi S, Hooker C et al. A new psychosocial screening instrument for use with cancer patients. Psychosomatics 2001; 42(3): 241-246.
34. Wang PS, Lane M, Olfson M, Pincus HA, Wells KB, Kessler RC. Twelve-month use of mental health services in the united states: results from the national comorbidity survey replication. Archives of General Psychiatry 2005; 62(6): 629-640.
35. Stansbury KL, Brown-Hughes T, Harley DA. Rural African American clergy: are they literate on late-life depression? Aging and Mental Health 2009; 13(1): 9-16.
36. Blank MB, Mahmood M, Fox JC, Guterbock T. Alternative mental health services: the role of the black church in the south. American Journal of Public Health 2002; 92(10): 1668-1672.
