There has been much discussion and debate in the literature regarding overall health dissemination research1-4, specifically as it relates to cancer prevention and control2,5-7. Underlying this discussion is the recognition of a 'chasm' between research-tested, evidence-based public health interventions and what occurs in practice8. As identified in the literature, there is a dearth of effectiveness research, minimal reporting on external validity and process evaluation, and limited dissemination and implementation research2,3,6,9-17. Additionally, some scholars lament the current dissemination pathway, which is often dependent on funding priorities, grant awards, peer-reviewed publications, and passive diffusion to the practice community. This pathway further exacerbates the lack of translation of effective research programs into public health practice17,18. The end result can be little or no impact on cancer incidence, morbidity and mortality.
In an effort to help accelerate the decades-long transformation of research to practice19, government agencies such as the Centers for Disease Control and Prevention (CDC) are promoting the use of evidence-based interventions (EBIs) in comprehensive cancer control efforts across all 50 states, tribes and territories20 and among its 37 Prevention Research Centers21. Similarly, the National Cancer Institute (NCI) has an office within the Division of Cancer Control and Population Sciences dedicated to dissemination and implementation science22. These government entities have also made progress in making evidence-based cancer control interventions available to the practice community in a 'one-stop shopping' web format. The NCI, CDC, American Cancer Society (ACS), Substance Abuse and Mental Health Services Administration, Agency for Healthcare Research and Quality, and Commission on Cancer have collaborated to co-sponsor 'Cancer Control P.L.A.N.E.T.' (http://cancercontrolplanet.cancer.gov/), a web portal which outlines 5 steps to developing a comprehensive cancer control plan or program23. Specifically, steps 3 and 4 of 'Cancer Control P.L.A.N.E.T.' provide practitioners with links to research reviews (eg Guide to Community Preventive Services, Cochrane Reviews) and a database of research-tested intervention programs (RTIPs) which users can consider adapting and implementing in their own communities. There are RTIPs available for breast, cervical and colorectal cancer screening, diet and nutrition, informed decision making, physical activity, sun safety, public health genomics, survivorship, and tobacco control.
Despite this web-based 'push' of evidence-based cancer control interventions to practitioners, there is little understanding of how these programs are adapted and implemented in real-world communities with varying populations, infrastructure, personnel, and resources as compared with the carefully controlled, multi-year, well-funded, studies from which they originated. Researchers, practitioners, and government agencies have advocated for further investigation into communities' abilities to identify core components of an intervention, maintain programmatic fidelity (ie adherence, dosage, delivery) while allowing for contextual adaptation, and to recognize barriers or sources of mismatch between the intervention and real-world implementation and outcomes3,10-12,14,15,24-26. Moreover, these investigations rarely occur in medically underserved communities such as rural Appalachia where the cancer burden is elevated and cultural barriers, lower socioeconomic status, poor health behaviors, and limited access to health services are also present27,28.
Based on 2001-2003 cancer surveillance data, Wingo et al report that overall cancer incidence rates are higher among Appalachian men (568.7 per 100 000 cases) and women (415.1) compared with their non-Appalachian counterparts (539.4 and 398.6, respectively)29. Related to this, Appalachians experience higher rates of lung cancer incidence and mortality due to elevated smoking rates in the region29,30. For example, in 2009 Kentucky and West Virginia had the highest prevalence of adult current smoking in the USA at 25.6%31. Incidence and mortality rates for colorectal and cervical cancer are also higher in Appalachia29,30,32,33 due in part to smoking, poor diet, physical inactivity, and lower rates of cancer screening34-40. These cancer disparities are compounded by a poorer economic and educational outlook compared with the rest of the country. Notably, in the fiscal year 2012, 186 of the 420 Appalachian-designated counties (44%) are considered 'distressed' or 'at-risk' based on employment, income and poverty indicators41. Similarly, 12 of the 13 Appalachian-designated states have high school completion rates which are less than the national percentage, and all 13 states have lower college completion rates41. Related to access to health care, data from a 2004 Appalachian Regional Commission report indicated that 297 of 406 Appalachian counties (73%) were classified as whole or in-part health professional shortage areas42. Finally, varying cultural traits have been linked to Appalachians and the cancer experience, including religiosity, fatalism, self-reliance, strong family and social networks, storytelling traditions, and the important of place43-45.
As a result of the above, it is understandable that cancer control organizations within Appalachia have questioned the applicability of health interventions and programs designed outside the region to their population. However, few of the available EBIs originate in rural communities such as Appalachia and are developed with different populations in varied geographic settings with a focus on internal validity, consequently requiring some level of adaptation when implemented in the real world. Therefore, the purpose of this research was to understand and describe community organizations' experiences with adapting and implementing evidence-based cancer control interventions in West Virginia, the only state wholly within Appalachia. This assessment aligns with Chen's call for more focus on 'viable validity', which centers on ordinary practitioners' (ie stakeholders) views and experiences with research-tested interventions in real-world settings46.
Project background
In February 2007, the NCI-funded Appalachia Community Cancer Network (ACCN), located in the Mary Babb Randolph Cancer Center at West Virginia University, released a request for proposals for community-based cancer education mini-grants (funding was made possible through a charitable foundation). Because West Virginia is recognized to have increased cancer incidence and mortality29,47,48 the funding request required applicants to:
- Focus on rural populations with limited access to cancer education programs and resources.
- Address one of the following priorities: breast/ cervical/ prostate/ colorectal cancer; lung cancer and tobacco education; or physical activity and nutrition.
- Utilize an evidence-based cancer control intervention in their programmatic design. Applications included a narrative statement of need, a work plan, an evaluation plan, and a budget with justification.
Prior to the March 2007 grant application deadline, NCI's former Mid-Atlantic Cancer Information Service (CIS) Partnership Program offered a technical assistance workshop for 32 individuals representing 23 organizations. Using NCI's curriculum, Using What Works: Adapting Evidence-Based Programs to Fit Your Needs49, CIS staff trained attendees on the process of identifying, adapting, and implementing research-tested interventions for community-based programs. The training incorporated an example of adapting and implementing an intervention in rural West Virginia to give participants hands-on experience. At the conclusion of the workshop attendees were given the mini-grant application. Organizations that did not attend the training were sent the request for proposals via email. Additionally, ACCN offered technical assistance with proposal development and subsequent program implementation.
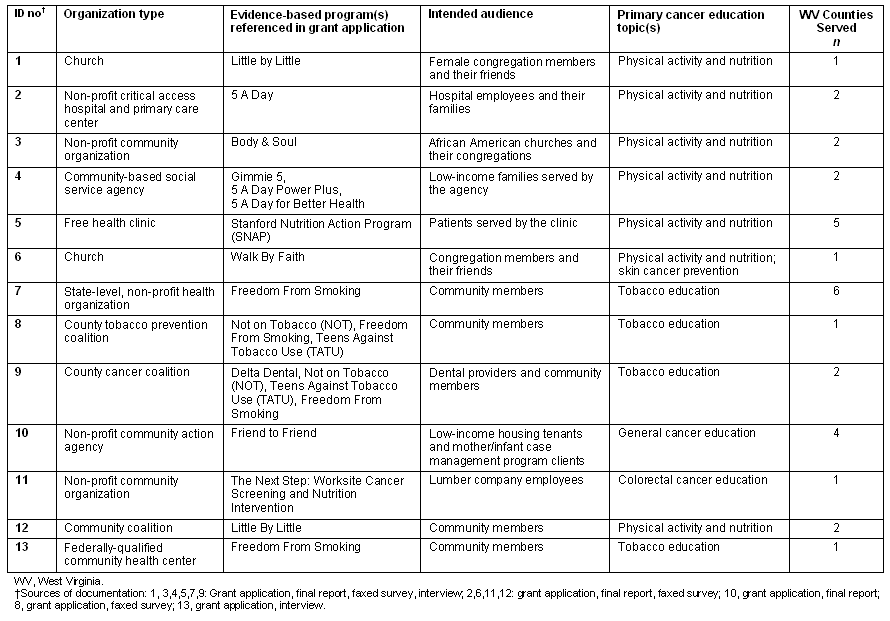
Thirteen grant applications were received and after undergoing a formal review, all 13 proposals were selected for funding. Each community organization was awarded $3,500 for program implementation starting 15 April-30 November 2007. Grantees collectively covered 30 West Virginia counties and included local coalitions, faith-based entities, non-profit community organizations, social service agencies, and health clinics (Table 1). Each grantee was asked to submit a final programmatic report at the end of the funding period.
Table 1: Grantee characteristics
A case study approach was selected to examine the collective experience of the 13 grantees' that were awarded the ACCN mini-grant funding. In this instance, the ACCN grant program is the case, which was bound by time and place50-53. This analytic approach was chosen for several reasons. Foremost, case study research focuses on the 'how' and the 'why' in order to gain a deeper understanding of a process rather than outcomes50-52. Case studies also allow for consideration of context, application, and decision-making in real-life situations51,52. While retrospective in nature, the case study findings are highly relevant to current events51 such as the debate and discussion related to health dissemination research. Notably, both Green and Campbell advocate case study research as a supplement to experimental dissemination research designs13,54. Finally, this type of descriptive research relies on the integration of diverse, multiple sources of data such as program documentation, reports, and interviews with program participants to provide a holistic description of the case being studied51-53,55.
The study was conducted in 4 phases between summer 2008 and fall 2009. The research team obtained copies of all 13 funded organizations' grant applications (100%) and 11 final programmatic reports (85%), phase 1. An initial brief, one-page faxed survey was sent to the 13 grantees to assess interest in participating in a one-hour telephone or face-to-face in-depth interview and to obtain preliminary responses to several of the questions which would be explored in detail during the interviews (phase 2). The survey was intended for the individual listed as the project coordinator on the original grant application. It was felt that these key stakeholders were the best individuals to describe the grant experience, considering these individuals were primarily responsible for writing and submitting the application; selecting, adapting, implementing, and evaluating the evidence-based cancer education program; and submitting final programmatic reports.
Eleven of the 13 agencies (85%) responded to the faxed survey; seven of the 11 survey respondents (64%) chose to participate in the interviews. A project coordinator that did not return the survey, but was contacted through a follow-up telephone call, also agreed to complete an interview. Overall, seven of the 13 grantees (54%) participated in the in-depth surveys (phase 3). For their convenience, interviewees could choose whether to complete the interview in person or by telephone; there were no differences in the interview scripts. Both the survey and the semi-structured interview guide were based on a previous questionnaire used to evaluate a national partnership between NCI, CDC, ACS and the US Department of Agriculture's Cooperative Extension Service, entitled Team Up: Cancer Screening Saves Lives, which promoted the use of evidence-based strategies to impact breast and cervical cancer disparities in 6 states56. The interview questions specifically examined rural organizations' perceptions of EBIs; their experiences in selecting, adapting, implementing, and evaluating the interventions; their definition of 'success'; sustainability of the current intervention and future use of EBIs; and their insights on maintaining intervention fidelity versus meeting the needs of local constituents.
All the authors of this article independently read and systematically reviewed the interview transcripts, survey results, grant applications, and final reports multiple times in order to immerse themselves in the data and to extract descriptive, thematic content related to the organizations' experiences with adapting and implementing evidence-based cancer interventions (phase 4). Summative results were refined by the research team through an iterative process of re-examining the various forms of documentation and interview content, debating and resolving themes, justifying differing viewpoints, and further examining content that departed from initial findings57. Based on the collectivity of documentation and interviews associated with the ACCN mini-grant program, major findings, themes, and specific illustrative examples elicited from the grantees are reported here.
The project was approved by the West Virginia University Institutional Review Board.
Cancer Information Service 'Using What Works' training
Overall, eight of the 13 funded organizations had representatives who attended the initial Using What Works training on adapting and implementing EBIs. Four of the seven interviewees attended the training, and all of them found the training helpful, particularly in learning about the 'Cancer Control P.L.A.N.E.T.' website as well as how to negotiate the adaptation and integrity of EBIs. However, four respondents in particular felt the available RTIPs were irrelevant to their small, rural Appalachian communities and felt challenged in identifying an appropriate program for their grant application. One participant explicitly stated that RTIPs 'should be taken back where they came from. They don't fit X County'. The three interviewees who did not attend the training were asked how they found out about EBIs. These individuals indicated that they either had previous experience with evidence-based programming, learned about it in their graduate degree programs, relied on one-on-one guidance from ACCN and CIS staff and/or had taught themselves through self-study of the Using What Works CD-ROM and 'Cancer Control P.L.A.N.E.T.' website. Notably, throughout the interviews and documentation reviews, there were no tangible differences between those respondents who attended the training and those who did not.
Overall perceptions of evidence-based interventions: Through both the survey and the interviews, participants were asked about their overall perceptions of EBIs and their required use in the ACCN mini-grant application. While 10 of the respondents agreed with the importance of using EBIs (most notably to avoid duplication of efforts and to build upon previously successful research programs), five interviewees specifically described the required use of EBIs as: 'expected', 'overwhelming', 'challenging', and 'restricting'. While participants were amenable to using EBIs in order to obtain funding, two interview respondents expressed fear that the required use of EBIs might deter other organizations from applying for funding, particularly those less knowledgeable or having less experience with EBIs. For example, organizations such as churches rely on volunteer members to lead health-based programming. As stated by one project coordinator:
Most of our [church] members are 'average' citizens who are unfamiliar with the [EBIs] concept and want to use what they believe will work.
Three interviewees reviewed specific Appalachian challenges. They lamented the widely dispersed and geographically isolated population. Older, less educated, and lower income populations present difficulties. Also communities often do not have large worksites, churches, or the staffing that can host health education programs. These respondents felt rural communities were a poor match for most of the available EBIs, requiring more time and effort to adapt the interventions.
Evidence-based interventions selection: Based on review of the grant applications, the majority of grantees (n=8) used 'Cancer Control P.L.A.N.E.T.' to identify their evidence-based cancer education intervention/s) (Table 1). The American Lung Association was also utilized as a resource; four organizations implemented 'Freedom From Smoking'®. While 9 of the funded organizations documented local partner support for their cancer education project in the grant application and final report, the intervention selection process was often left to the sole discretion of the project coordinator who also served as grant writer. Three coordinators had additional input from their staff, board members, and coalition members. Selection of the respective interventions was based on a number of factors. One factor was the organizations' knowledge of their target audience (ie socioeconomic status, age). Specific topics such as nutrition attracted interest due to impact on multiple diseases. Tobacco cessation was popular due to the recent passing of a 'clean indoor air' ordinance. Selection also was based on the project timeframe, logistics, staffing, and budget. The availability of collaborative partners was important. Programs that 'seemed doable or interesting' were selected as well as those with free or affordable program materials. One coordinator expressed concern regarding the selection process:
I think the biggest challenge that I felt was that when I was looking through the list...some of these things looked very specialized and were really well designed. I really didn't feel that a lot of those specifically, not just regionally or geographically, were a good fit for our economic demographic of very low income families.
Notably, three respondents commented on the importance of reviewing the various interventions in the context of their clients' literacy levels. One health educator stated:
I'm also very aware of the literacy issue for many of my patients. Folks don't need all the details, they want to know how this works at my house, how can this work in my life, so I'm always looking at that angle for almost anything we do here.
Six grantees indicated their constituents needed visual materials more than written materials.
Evidence-based interventions adaptation: Despite understanding the importance of maintaining fidelity of the original intervention, fidelity was often viewed as secondary to the community's needs. Of the project coordinators that responded to the survey and participated in the interviews, all adapted the original EBI in some manner. While the degree of adaptation varied among organizations, examples of adaptation included: modifying the method of delivery, adjusting program timelines due to the short grant period, creating new materials or tailoring existing materials to be more 'Appalachian', condensing information, developing additional activities, combining multiple programs, and modifying evaluation plans. One tangible example of adaptation was described by an interview participant:
I had to think of cramming 4 weeks of 'Give Me Five' programming into 45 minutes worth of time to get the one month of programming in.
The adaptation process was difficult for several of the project coordinators, particularly as it related to modifying the programs for low income Appalachian families. One individual commented:
I felt a little distraught throughout the [adaptation] process because I didn't think I was doing it right.
Another participant noted:
I felt like it was a lot of extra work that I didn't know if it was going to pay off in the end.
Additionally, one grantee lamented:
...it was adapted so much to the point where it would probably be a fine line to say whether or not you could even relate the impact we had on our families to any of those particular interventions.
However, throughout the case study process it was observed that coordinators' experiences with selecting and adapting their respective programs varied with their backgrounds (ie community volunteer versus healthcare or other professional). For example, those with professional backgrounds often chose programs such as Body & Soul and Freedom from Smoking® which include structured curriculum guides and instructional DVDs. One project coordinator with a Master of Public Administration degree conducted a focus group with her agency's clients to assess the intervention materials' readability and graphics and discuss clients' preferences for potential workshop formats. Interestingly, this same individual stated that had 'this been something that was not requiring me to use an evidence-based model, I would have not done all that'. While designed for use with adults, she commented that her modified curriculum was equivalent to something that might be used in an elementary school setting due to the lower health literacy among her clients.
Evidence-based interventions implementation: In implementing the adapted interventions, many of the organizations experienced notable barriers. Recruitment proved to be an issue for six of the programs. For example, one interviewee had no participants enroll in her organization's smoking cessation program despite conducting what she deemed a successful marketing campaign: 'We had an "If you build it, they will come mentality" which didn't work'. According to their final report, the grantee who partnered with a lumber company to conduct a work-site colorectal cancer screening and nutrition intervention determined The Next Step curriculum (to be implemented during company work hours) would have cost the lumber company $75,000 in lost labor; therefore, significant adjustments had to be made to their program. Rather than host the educational sessions during work hours, activities were held during shift changes and as part of the company's mandatory safety meetings. Other groups were confronted with technological issues such as computer, internet, DVD, and printer access.
Despite encountering barriers to implementation, all coordinators felt they were successful in meeting their initial project goals and objectives. Even though some programs failed to attract community participants or couldn't measure long-term behavior, respondents defined 'success' in a variety of ways. Success was defined by enthusiastic participation, increased health knowledge among constituents, establishment of relationships with healthcare professionals, implementation of behavioral changes such as diet changes and smoking reduction or cessation, evidence of community engagement around cancer prevention and screening, the establishment of collaborative community partnerships, health messages disseminated, and success in planting seeds for future projects. One project coordinator commented, 'I'm just happy if it changes one person' and another individual remarked, 'Small changes are what I am really proud to see with the population we work with'. Evaluation plans focused on process including activity listings and completion dates, the number of people reached through each activity, and listings of collaborative partners. Anecdotal reports of health behavior changes among community participants were included in a few final reports; changes included increased fruit and vegetable consumption, increases in physical activity, and decreased cigar consumption. Grantees were also given an opportunity to report any barriers encountered during the project, many of which are described here.
Overall reflections: As the final step in the case study, participants' overall reflections of their experiences in selecting, adapting, implementing, and evaluating EBIs were assessed. Interview and survey participants described additional challenges and barriers to the overall process which ranged from community resistance to smoking cessation programs, to the need for more funding and time, to the inclusion of more Appalachian-specific recipes in the nutrition-based interventions. Regarding funding, six interviewees commented that while $3,500 was helpful, it was not enough money to fully conduct their projects, and there were also restrictions on how the money could be spent (ie salaries, computers, and transportation were non-allowable costs) and a significant amount of in-kind funding was needed to support the overall project, as documented in 12 of the 13 grant applications. One project coordinator expressed the following:
...it [the intervention] will never be a large scale success unless the money and timeframe are more realistic to more adequately show the full impact the program had on the community.
Yet many of these organizations are in need of grant funding and were grateful for the opportunity, regardless of the dollar amount. Others discussed the need for more training on a particular curriculum (eg train-the-trainer) before they offer it to the community and the need for more staff. It was also noted that more EBIs were needed that focused on rural, medically underserved populations, so organizations such as those in this case study have more options to choose from when selecting potential interventions to adapt and implement. Finally, three participants specifically remarked on the difficulty of changing behaviors related to diet, exercise, and smoking as well as measuring long-term outcomes such as cancer prevention.
None of the grantees sustained the complete intervention, but four of the coordinators mentioned that they were still using banners, pamphlets, CDs, and other materials from the project in their organization's other health-related programmatic activities. When asked if they would continue to use EBIs in the future, four interviewees would do so if it were a required component of the grant application, but called for more creativity in adapting the program to meet their constituents' needs. Four participants like the idea of using 'evidence-informed' approaches such as those broader strategies outlined in The Guide to Community Preventive Services, compared with a prescribed intervention. One interviewee noted evidence-informed 'sounds like a much sunnier alternative' and would allow for more flexibility. Regardless of the approach, one individual reiterated that 'testimonials from other organizations about their experiences in doing this type of programming' would help others become more comfortable in using EBIs. And finally, a director of a federally-qualified community health center made this concluding remark:
We're looking at evidence-based models now [for physical activity in the schools]...I think it gives you a definite argument as to why a program should be run, because you have the research to back you up, but again it's hard because some of those programs you do have to tailor. There are not very much of those programs tested and run in Appalachian West Virginia. I think we have a different ball-game here...We're all dealing with the same diseases across the US, but there is a definite culture difference here and sometimes it's very hard to breakthrough that barrier. You have to get very creative.
Discussion
To the authors' knowledge, this is only the second published assessment of the experiences of rural Appalachian community organizations in adapting and implementing evidence-based cancer control interventions. Bencivenga et al published results of a mammography-related EBI adaptation (American Cancer Society's Tell A Friend®) in one Appalachian Pennsylvania county58. The study findings echo many of the themes identified in focus groups with urban community organizations in Massachusetts, namely use of EBIs based on funding requirements, the need to modify the program to a specific population, the challenge of adaptation, the lack of organizational resources, and concerns related to interventions' requirements for literacy levels59. However, throughout the conversations with the case study participants, it was apparent that rural geography and the population composition of Appalachian West Virginia communities play a unique and challenging role in the adaptation and implementation process.
The present findings suggest that while making EBIs available to local practitioners is a step in the right direction for moving research to practice, these 'diffusion systems' (such as 'Cancer Control P.L.A.N.E.T.') are not enough15. There is a complex set of circumstances related to real-world adaptation and implementation which need further attention before long-term changes in cancer incidence, morbidity and mortality are realized. In other words, more focus is needed on the transportability of efficacious interventions to local settings60, such as in rural Appalachia.
As described by the key stakeholders, funding opportunities are readily appreciated and their overall perceptions of EBIs are favorable; however, the required use of EBIs to receive funding is not necessarily welcomed. This requirement is often seen as an immediate challenge, despite the provision of training and technical assistance. While researchers may 'push' EBIs to the practice community, there is not always a reciprocal 'pull' from the practitioner4,6,61. Intervention selection was based on a host of factors many of which were specific to the groups' organizational capacity, their constituents' sociodemographics and literacy levels, and the complexity of the interventions. All of the organizations adapted the original intervention to some degree. Some of the changes might be considered minor, such as giving the intervention materials an 'Appalachian look', whereas other changes were more substantial, such as condensing or eliminating program components, combining various parts of multiple programs, creating additional activities to supplement the original intervention, and modifying the method of delivery. All of these changes could potentially jeopardize the adapted program's viability, the fidelity-adaptation balance, and underlying theoretical and scientific foundation of the original intervention62. Despite the fact that guidelines and tools for balancing and measuring program fidelity-adaptation have been suggested24,26,49,62, they are often not easily understood, disseminated or utilized. For many of these project coordinators, the adaptation process was challenging and ultimately their constituents' needs outweighed the need to maintain scientific fidelity of the original program.
Notwithstanding noted barriers during implementation (ie recruitment, technological problems, potential lost productivity), respondents reported perceived successful outcomes ranging from program attendance to small behavioral changes among clients to collaborative community partnerships. In responding to a 'wish list' request, it is apparent these groups desire more funding, time, flexibility, organizational resources, and training. In addition to more rural, Appalachian-oriented interventions, these organizations want more evidence and lessons learned from agencies that serve similar populations (ie rural, Appalachian, lower socioeconomic status, low literacy).
Limitations
Despite the informative nature of this case study, there are noted limitations to the research. Specifically, the data is retrospective and primarily based on the perspective of the interviewees at one point in time. Also acknowledged are staffing changes among the organizations which limited participation in the interviews and survey and the exclusion of other staff members involved in the projects. Further, one of the more notable critiques of case study research is lack of generalizability50,51. It is not possible to generalize the findings to other community groups in Appalachia or other rural communities; the findings are solely based on the documentation and experiences of the 13 West Virginia community partners who received the small cancer education grants. Additional insights from actual community members who participated in the cancer education projects would have also strengthened the results. Finally, staff from community organizations that chose not to apply for the mini-grants were not interviewed. Their perspective would have shed additional light on the initial Using What Works training and overall perceptions of EBIs and their required use in the grant application which may have served as a barrier to these potential grantees.
However, after considering these limitations, the authors believe this case study, which utilized both qualitative interviews and grant-related documentation, supports the concept of viable validity46, and focused on a unique geographic region of the country, contributing to the debate and discussion centered on dissemination and implementation research and the real world experiences in translating research to practice.
Both researchers and practitioners realize there is much work to be done as it relates to translating research to practice, but given the challenges articulated in this Appalachian-based exemplar, the field may benefit from further exploration and dialogue regarding the needs of each party. For example, more training and technical assistance is needed to provide practitioners with a firm understanding of the concept of 'evidence-based' public health; the advantages to implementing research programs which have been proven to be scientifically sound; how to select, adapt, implement and sustain EBIs while maintaining scientific fidelity; how to identify the core components of an intervention which can/cannot be modified; and conduct a meaningful evaluation. Conversely, academic researchers need a better understanding of the contextual circumstances practitioners encounter on a daily basis, including rural, lower socioeconomic status communities; Appalachian culture; limited formal public health/cancer control training for themselves and their staff; and limitations of organizational capacity, personnel, and financial resources.
To continue this line of inquiry, a shared partnership is warranted. This partnership would bond researchers and local practitioners to help bridge the chasm between research and practice in rural, medically underserved communities. Better health outcomes require a balance between research-tested interventions and population-specific application - with adaptation, implementation and evaluation playing key roles.
Acknowledgments
The authors acknowledge the Appalachia Community Cancer Network for facilitating access to the grantees and grant documentation as well as Cancer Prevention and Control at the Mary Babb Randolph Cancer Center, West Virginia University, for their support for this project. The authors would also like to thank Dr Erica Bresleau from the National Cancer Institute for sharing the 'Team Up: Cancer Screening Saves Lives' questionnaire from which the faxed survey and interview guide questions were developed. Finally, the authors thank the community-based organizations that participated in this case study.
References
1. Johnson JL, Green LW, Frankish CJ, MacLean DR, Stachenko S. A Dissemination Research Agenda to Strengthen Health Promotion and Disease Prevention. Canadian Journal of Public Health 1996; 87: S5-S10.
2. Bowen D, Sorensen G, Weiner B, Campbell M, Emmons K, Melvin C. Dissemination research in cancer control: where are we and where should we go? Cancer Causes and Control 2009; 20: 473-485.
3. Rabin BA, Brownson RC, Haire-Joshu D, Kreuter MW, Weaver NL. A glossary for dissemination and implementation research in health. Journal of Public Health Management and Practice 2008; 14: 117-123.
4. Kerner J, Rimer B, Emmons K. Introduction to the special section on dissemination-dissemination research and research dissemination: how can we close the gap? Health Psychology 2005; 24: 443-446.
5. Greenwald P, Cullen JW. The scientific approach to cancer control. A Cancer Journal for Clinicians 1984; 34: 328-332.
6. Glasgow RE, Marcus AC, Bull SS, Wilson KM. Disseminating effective cancer screening interventions. Cancer 2004; 101: 1239-1250.
7. Ellis P, Robinson P, Ciliska D, Armour T, Brouwers M, O'Brien MA et al. A systematic review of studies evaluating diffusion and dissemination of selected cancer control interventions. Health Psychology 2005; 24: 488-500.
8. Institute of Medicine. Crossing the quality chasm: a new health system for the 21st Century. Washington, DC: National Academy, 2001.
9. Glasgow RE, Lichtenstein E, Marcus AC. Public health matters. why don't we see more translation of health promotion research to practice? Rethinking the efficacy-to-effectiveness Transition. American Journal of Public Health 2003; 93: 1261-1267.
10. Cohen DJ, Crabtree BF, Etz RS, Balasubramanian BA, Donahue KE, Leviton LC et al. Fidelity versus flexibility: translating evidence-based research into practice. American Journal of Preventive Medicine 2008; 35: S381-S389.
11. Durlak J, DuPre E. Implementation matters: a review of research on the influence of implementation on program outcomes and the factors affecting implementation. American Journal of Community Psychology 2008; 41: 327-350.
12. Mercer SL, DeVinney BJ, Fine LJ, Green LW, Dougherty D. Study designs for effectiveness and translation research: identifying trade-offs. American Journal of Preventive Medicine 2007; 33: 139-154.
13. Green LW. From research to "best practices" in other settings and populations. American Journal of Health Behavior 2001; 25: 165-178.
14. Glasgow RE, Emmons KM. How can we increase translation of research into practice? Types of evidence needed. Annual Review of Public Health 2007; 28: 413-433.
15. Rohrbach LA, Grana R, Sussman S, Valente TW. Type II translation. Evaluation and the Health Professions 2006; 29: 302-333.
16. Rychetnik L, Hawe P, Waters E, Barratt A, Frommer M. A glossary for evidence based public health. Journal of Epidemiology and Community Health 2004; 58: 538-545.
17. Green LW, Ottoson JM, García C, Hiatt RA. Diffusion theory and knowledge dissemination, utilization, and integration in public health. Annual Review of Public Health 2009; 30: 151-174.
18. Green LW. Making research relevant: if it is an evidence-based practice, where's the practice-based evidence? Family Practice 2008; 25: i20-i24.
19. Balas EA, Boren SA. Managing clinical knowledge for health care improvement. In: JMA Bemmel (Ed.). Yearbook of medical informatics 2000: patient-centered systems. Stuttgart: Schattauer, 2000; 65-70.
20. Given L, Black B, Lowry G, Huang P, Kerner J. Collaborating to conquer cancer: a comprehensive approach to cancer control. Cancer Causes and Control 2005; 16: 3-14.
21. CDC. Prevention research centers. (Online) 2011. Available: http://www.cdc.gov/prc/index.htm (Accessed 7 February 2011).
22. National Cancer Institute. Designing for dissemination. (Online) no date. Available: http://cancercontrol.cancer.gov/d4d/index.html (Accessed 7 February 2011).
23. Sood R, Ho P, Tornow C, Frey W. Cancer Control P.L.A.N.E.T. evaluation final report. (Online) no date. Available: http://cancercontrol.cancer.gov/IS/pdfs/CCPFinalReport.pdf (Accessed 4 October 2011).
24. Castro FG, Barrera M, Martinez CR. The cultural adaptation of prevention interventions: resolving tensions between fidelity and fit. Prevention Science 2004; 5: 41-45.
25. Brownson RC, Gurney JG, Land GH. Evidence-based decision making in public health. Journal of Public Health Management and Practice 1999; 5: 86-97.
26. US Department of Health and Human Services. Finding the balance: program fidelity and adaptation in substance abuse prevention. DHHS, 2002.
27. Couto RA, Simpson NK, Harris G. Sowing seeds in the mountains community based coalitions for cancer prevention and control. Bethesda: National Institutes of Health, National Cancer Institute, 1994.
28. Appalachian Regional Commission. Underlying socioeconomic factors influencing health disparities in the Appalachian Region. Final report. (Online) 2008. Available: http://www.arc.gov/assets/research_reports/SocioeconomicFactorsInfluencingHealthDisparitiesinAppalachianRegion5.pdf (Accessed 7 February 2011).
29. Wingo PA, Tucker TC, Jamison PM, Martin H, McLaughlin C, Bayakly R et al. Cancer in Appalachia, 2001-2003. Cancer 2008; 112: 181-192.
30. Huang B, Wyatt S, Tucker T, Bottorff D, Lengerich E, Hall H. Cancer death rates - Appalachia, 1994-1998. Morbidity and Mortality Weekly Report 2002; 51: 527-529.
31. Dube SR, McClave A, James C, Caraballo R, Kaufmann R, Pechacek T. Vital signs: current cigarette smoking among adults aged ≥18 years - United States, 2009. Morbidity and Mortality Weekly Report 2010; 59: 1135-1140.
32. Hall HI, Rogers JD, Weir HK, Miller DS, Uhler RJ. Breast and cervical carcinoma mortality among women in the Appalachian region of the US, 1976-1996. Cancer 2000; 89: 1593-1602.
33. Armstrong LR, Thompson T, Hall HI, Coughlin SS, Steele B, Rogers JD. Colorectal carcinoma mortality among Appalachian men and women, 1969-1999. Cancer 2004; 101: 2851-2858.
34. Murray CJL, Kulkarni SC, Michaud C, Tomijima N, Bulzacchelli MT, Iandiorio TJ et al. Eight Americas: investigating mortality disparities across races, counties, and race-counties in the United States. Public Library of Science Medicine 2006; 3: e260.
35. Wewers ME, Katz M, Fickle D, Paskett ED. Risky behaviors among Ohio Appalachian adults. Preventing Chronic Disease 2006; 3: A127.
36. Yabroff K, Lawrence W, King J, Mangan P, Washington K, Yi B et al. Geographic disparities in cervical cancer mortality: what are the roles of risk factor prevalence, screening, and use of recommended treatment? Journal of Rural Health 2005; 21: 149-157.
37. Amonkar MM, Madhavan S. Compliance rates and predictors of cancer screening recommendations among Appalachian women. Journal of Health Care for the Poor and Underserved 2002; 13: 443-460.
38. Hall HI, Uhler RJ, Coughlin SS, Miller DS. Breast and cervical cancer screening among Appalachian women. Cancer Epidemiology Biomarkers & Prevention 2002; 11: 137-142.
39. Tessaro I, Smith SL, Rye S. Knowledge and perceptions of diabetes in an Appalachian population. Preventing Chronic Disease 2005; 2: A13.
40. Ahijevych K, Kuun P, Christman S, Wood T, Browning K, Wewers ME. Beliefs about tobacco among Appalachian current and former users. Applied Nursing Research 2003; 16: 93-102.
41. Appalachian Regional Commission. Appalachian Regional Commission. (Online) no date. Available: http://www.arc.gov/ (Accessed 15 August 2011).
42. Halverson JA, Lin M, Harner EJ. An analysis of disparities in health status and access to health care in the Appalachian Region. Washington, DC: Appalachian Regional Commission, 2004.
43. Dorgan KA, Hutson SP, Gerding G, Duvall KL. Culturally tailored cancer communication, education and research: the highways and back roads of Appalachia. Preventing Chronic Disease 2009; 6: 1-5.
44. Coyne CA, Demian-Popescu C, Friend D. Social and cultural factors influencing health in southern West Virginia: a qualitative study. Preventing Chronic Disease 2006; 3: A124.
45. Behringer B, Friedell GH. Appalachia: where place matters in health. Preventing Chronic Disease 2006; 3: A113.
46. Chen HT. The bottom-up approach to integrative validity: a new perspective for program evaluation. Evaluation and Program Planning 2010; 33: 205-214.
47. Lengerich E, Tucker T, Powell R, Colsher P, Lehman E, Ward A et al. Cancer incidence in Kentucky, Pennsylvania, and West Virginia: disparities in Appalachia. Journal of Rural Health 2005; 21: 39-47.
48. CDC. West Virginia fact sheet. (Online) 2011. Available: http://www.cdc.gov/nchs/pressroom/states/WV.pdf (Accessed 7 February 2011).
49. National Cancer Institute. Using what works: adapting evidence - based programs to fit your needs. (Online) no date. Available: http://cancercontrol.cancer.gov/use_what_works/start.htm (Accessed 7 February 2011).
50. Stake RE. The art of case study research. Thousand Oaks, CA: Sage, 1995.
51. Yin RK. Case study research design and methods. Thousand Oaks, CA: Sage, 2003.
52. Merriam SB. Qualitative research and case study applications in education San Francisco, CA: Jossy-Bass, 1998.
53. Patton MQ. Qualitative research and evaluation methods. Thousand Oaks, CA: Sage, 2002.
54. Campbell DT. Guidelines for monitoring the scientific competence of preventive intervention research centers. Science Communication 1987; 8: 389-430.
55. Creswell JW. Qualitative inquiry and research design choosing among five traditions. Thousand Oaks: Sage, 1998.
56. National Cancer Institute. Team up: cancer screening saves lives. (Online) 2009. Available: http://cancercontrol.cancer.gov/acsrb/teamup.html (Accessed 7 February 2011).
57. Schoenberg NE, Hatcher J, Dignan,MB. Appalachian women's perceptions of their community's health threats. Journal of Rural Health 2008; 24: 75-83.
58. Bencivenga M, DeRubis S, Leach P, Lotito L, Shoemaker C, Lengerich EJ. Community partnerships, food pantries, and an evidence-based intervention to increase mammography among rural women. Journal of Rural Health 2008; 24: 91-95.
59. Crisostomo J, Alexander-Molloy J, Viswanath K. PLANET MassCONECT focus group and key informant interview themes report. Cambridge: Havard School of Public Health, 2009; 1-33.
60. Schoenwald SK, Hoagwood K. Effectiveness, transportability, and dissemination of interventions: what matters when? Psychiatric Services 2001; 52: 1190-1197.
61. Curry SJ. Organizational interventions to encourage guideline implementation. Chest 2000; 118: S40-S46.
62. Smith E, Caldwell L. Adapting evidence-based programs to new contexts: what needs to be changed? Journal of Rural Health 2007; 23: 37-41.





