Palliative care is a relatively new approach to practice in Canada, beginning in Montreal and Winnipeg in the early 1970s1,2. Much of its development since then has happened in urban centres, with service delivery models created for a specialty healthcare team and urban health infrastructure3. Palliative care also requires an interdisciplinary team approach3. Rural communities have lagged behind and are just beginning to provide integrated palliative care services that assist in keeping dying people at home in their home communities, rather than having them seek services in geographically distant urban centers4. Having access to palliative care in rural communities respects the individuals' wish to die at home, surrounded by families and friends5.
There are many challenges to providing healthcare services in rural settings, such as low retention of existing health professionals6,7, inability to attract new professionals8, and lack of specialist services9. Professionals who do work in rural settings apply generalist practice principles in order to provide a variety of services within the community along a continuum of care from birth to death. Palliative care is one component of rural generalist practice, and thus is characterized by the same rural health dynamics and challenges such as professional isolation and limited access to continuing education10. It is important that rural professionals work together when it comes to meeting the needs of their palliative clients, as their complex issues extend beyond medical needs and include psychological, social and spiritual needs11. An interprofessional and collaborative approach is required to ensure that their palliative clients are having their needs effectively met in a timely and efficient manner12.
Interprofessional collaboration (IPC) has been on the radar of policy-makers for some time in order to address demands on healthcare systems and changes to the healthcare workforce13-15. Research indicates IPC has positive effects on both the healthcare system and health outcomes14. Promoting IPC in rural communities could relieve some of the challenges associated with rural work environments16,17 and help improve rural health status, which overall is poorer in rural and remote communities than in urban areas18,19.
A growing body of literature has produced models for IPC in practice20-24. These models help to define interprofessional collaborative practice, and identify core competencies required by professionals to work within these contexts. Way, Jones and Busing25 outlined seven essential elements for successful IPC: (1) responsibility and accountability, meaning that all partners actively participate in decision-making and accept shared responsibility; (2) coordination that includes efficient and effective planning, which reduces duplication of efforts or fragmentation of care; (3) communication of both content and relationship; (4) cooperation that involves acknowledgement and respect of other disciplines' professional opinions; (5) assertiveness, whereby practitioners confidently express the perspectives of their own profession with knowledge that these will be respected; (6) autonomy by individual care providers to independently make decisions and carry out treatment plan; and (7) mutual trust and respect, binding all the other elements together.
IPC may be well conceptualized in the literature, but there is little evidence to support the transferability of these elements into rural healthcare practice or rural palliative care practice. Kelley proposed10 and validated26 a conceptual model for developing and delivering palliative care in rural communities. The model has its roots in community capacity development theory, a bottom-up approach that builds on the collaboration of local professionals. In the model, the metaphor of a tree is used to depict the growing of a rural palliative care program. There are four sequential phases in the model: having necessary antecedent community conditions, experiencing a catalyst for change, creating a local team, and growing the palliative care program. This model has validated the need to form a local interagency, interprofessional team as a foundation for growing the rural palliative care program; however, it does not offer insight into the intra-group processes involved in their IPC.
The purpose of this research is to bridge the knowledge gap that exists with respect to rural IPC, particularly in relation to phases 3 and 4 of the Kelley model for developing rural palliative care outlined above. It examines the working of these teams and highlights the elements that are important to rural collaborative processes. Understanding the process of how rural teams form and continue to function will help further the current understanding of IPC in the context in which these professionals work. No literature could be located that examined rural health teams from the IPC perspective.
For the purpose of this qualitative study, naturalistic and ethnographic research strategies were employed to understand the experience of rural IPC in the context of rural palliative care team development. Purposive sampling was used to recruit key informants that were members of rural palliative care teams as participants. The seven elements of collaborative practice introduced by Way et al25, as previously outlined, provided a preliminary analytic framework to begin exploring the data. Analysis progressed using a process of interpretive description to embrace new ideas and conceptualizations that emerged from the patterns and themes of the rural health providers' narratives27. The questions of particular interest that guided this work were: What are the collaborative processes of a rural palliative care team? To what extent are Way et al's25 seven elements of IPC representative of rural teams? Are there any additional elements present when examining the experiences of rural teams? The use of Way et al's IPC framework was appropriate given the researchers' awareness of the phenomenon under study and did not limit the inductive approach to analysis27. Strategies such as concurrent data collection and analysis, constant comparative analysis and iterative analysis allowed emerging new understandings to be placed within a larger IPC perspective.
Research context
In 2007, Ontario Ministry of Health and Long-Term Care28 introduced the Aging at Home Strategy, which identified palliative/end-of-life care as a priority. Regional End-of-Life Care (EOLC) networks were developed with the task of assisting in the growth of palliative care throughout the province29. Consequently, rural communities across north-western Ontario began to look at how palliative care is delivered in their community. Community palliative care teams started to develop with an aim to facilitate the integration of palliative care services in their own community. The rapid development of rural palliative care teams and programs provided an opportunity to study and theorize their development26.
The research being discussed here was done in four rural communities in north-western Ontario, Canada (Table 1). This region of Ontario can be defined as rural and remote as per DesMeules et al's30 definition of rural and small town. North-western Ontario is comprised of the districts of Kenora, Rainy River and Thunder Bay (Fig1). It covers approximately 60% of the landmass of the province, but contains only 2% of its total population. The rural and remote areas include numerous small towns and First Nations communities. The distance between eastern and western boundaries is slightly over 1000 km, with a population density of 0.5 persons/km2. The only major urban community in the region, Thunder Bay, has a population of 109 000 and is considered remote in relation to Ontario's major population areas in the southern part of the province31.
Table 1: Demographic data of four rural communities in north-western Ontario, Canada (Populations and median
ages from Statistics Canada32; no. of deaths from Habjan et al33; distances to closest urban center
from http:// maps.google.com)
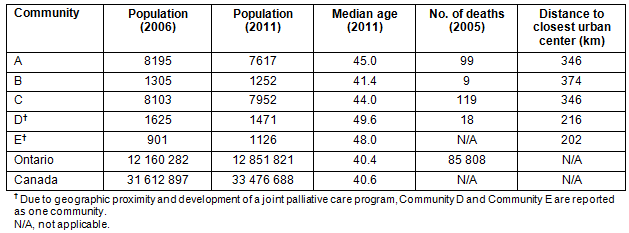
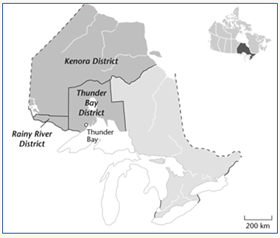
Figure 1: Districts of north-western Ontario, Canada.
Data collection and analysis
Data were collected between November 2008 and April 2009. Qualitative interviews were conducted with four team representatives/spokespeople (one for each community) and the regional community development worker, who had worked with 14 rural palliative care teams within the catchment area of the regional EOLC network. A semi-structured interview guide was developed and used to discuss collaboration in providing palliative care within each community. All interviews were audio-taped, transcribed verbatim, and checked for accuracy. Participant observation data (field notes) were also collected by the researcher during two palliative care team meetings in one of the communities. The transcribed and observational data were analyzed using a three-level approach of inductive analysis, whereby the coding of themes was done to reduce the data and provide a deep description of the story34. Rigour was maintained by triangulation of data sources. By using more than one source of data, the researcher was able to compare and cross-check the consistency of information35.
Ethics approval
Prior to data collection, the research protocol was reviewed and approved by the ethics review boards of Lakehead University (REB # 007-06-07) and McMaster University (REB #2007 161), Ontario.
At initial formation of the palliative care team in the communities studied, membership was made up of a very broad range of service providers and community members, including health care professionals, mental health workers and hospice volunteers, as well as clergy, funeral directors, lawyers and ambulance drivers. The breadth of community members who volunteered for the new team showed the interest and importance of palliative care in these communities, as well as confirming that palliative care inspired a holistic and inclusive community-focused approach. Over time, the teams self-selected a smaller core group of six to eight dedicated service providers who worked on developing the palliative care program. This core group, which became the rural palliative care team, had a diverse membership and consisted of both informal and formal healthcare and social service providers. Typically, members included nurses, a social worker, a hospice volunteer and a physician.
Ways et al's25 seven essential elements of IPC emerged as relevant and useful to understand the experiences of rural palliative care teams. It was discovered that all seven elements were present in each team's collaborative practice, enmeshed with a distinctiveness of rural environment. These elements of rural IPC are described below as seven themes, as observed in collected data. Each of the main themes is elaborated and clarified with sub-themes, which are shown in Figure 2.
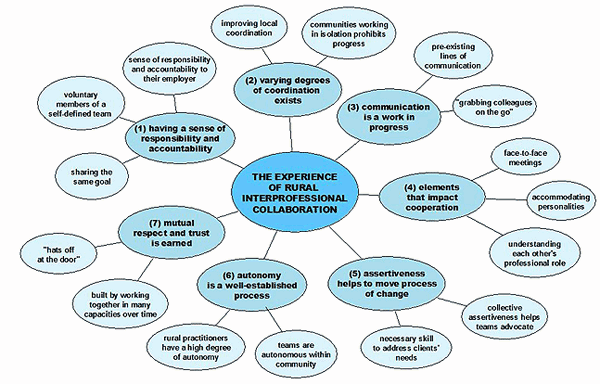
Figure 2: The experience of rural interprofessional collaboration - themes and sub-themes.
1. Having a sense of responsibility and accountability
Members of the team came together because they share the same goal, which is to improve quality of palliative care services in their community. They felt a personal and professional responsibility to help a very vulnerable population who had historically been underserviced in their community. They were motivated by their sense of social responsibility and accountability as community members.
The shared sense of responsibility and accountability amongst the team helped the members collaborate and kept the momentum of team-building going. The following participant comment below illustrates their shared goals:
... the responsibility I guess goes back to the care that is provided to the client. So any one who provides a service to the client is responsible for that service, and they bring that responsibility and accountability to the table.
The members participated because they wanted to; none were assigned or required to participate by their employers. The palliative care team viewed themselves as a voluntary self-defined team outside of any agency or organization:
These are not teams that are incorporated or have an official [status within an] official organization, per se ... they are just a voluntary group. And yet there's been a sense of commitment and accountability. This group gets together ... this is a team.
Although the members volunteered to be part of the team, they are still representing their organization and have a sense of responsibility and accountability to their employer. Team members were also willing to advocate for the team through their organization.
2. Varying degrees of coordination exists
The participants described different degrees of coordination that were taking place during the process of team development. A broader degree of coordination was occurring at the regional level, done by the EOLC network's community development worker. The coordination occurring at the local level was focussed on service provision and was done informally by different team members. Each community decided on their own unique process with respect to how to coordinate their efforts.
To address the issue of clients 'falling through the cracks' in service delivery and not receiving the appropriate and available palliative care, the local teams engaged in a process of meeting together and understanding the role of each person on the team. They began to identify the issues at hand, and they were slowly working together to make changes in their community. One tangible example of improving local coordination was described by an interview participant:
... if there is a problem of coordination, it is drawing in the right resources at the right time. Sometimes we do have problem of patients falling through the gaps ... so we are trying to work with that coordination, trying to improve it and seeing and exploring how we can improve it.
Many communities in north-western Ontario were simultaneously in the process of developing rural palliative care programs; however, they were all at different phases of development according to the Kelley model. Attempts were made by the regional EOLC network's community development worker to coordinate the processes in the communities by sharing strategies and information with each of the communities. Teams responded differently to this approach; some preferred to continue to work independently while others embraced the support. Progress was inhibited by communities working in isolation of each other. It was learned that working together on the same issue may foster faster delivery of quality palliative care programs. The community development worker shared the following about the rural teams:
... everyone isn't working on the very same thing at the very same time. A perfect example is, I just brought forward [from one particular health agency] an issue around the intake form ... that's exactly the point which I made a year ago. It was, 'we'll just let them deal with it and let them try it and see how things go'. But now several communities are asking the same questions.
3. Communication is a work in progress
Establishing good lines of communication is a process that develops over time and needs to be improved continually. An observed benefit to the teams was that many of the team members already worked together on a daily basis; therefore, lines of communication existed before the palliative care teams were established.
For healthcare and social service workers who share clients, the process for communication was established within their own organizational structure. The challenge was observed when trying to include people who may not have been in the formal circle of care. In order for all team members to receive the same information, email was used quite often to share meeting minutes or schedules. One participant expressed communication concerns still present:
We know that we have well established communications between doctors and [health care agency], between [health care agency] and service providers, between hospital and doctors; that has all been well established. But between getting the information to mental health, to palliative care volunteers we haven't worked on yet.
Communication among rural practitioners happens at all times of the day. Scheduling time to meet to discuss certain issues does not always work out for these busy generalists. However, they make good use of their time by sharing information with other team members when they are available or in passing. The idea of 'grabbing colleagues on the go' to provide them with pertinent client information was witnessed at the palliative care meetings; before and after the meeting, members were approaching each other to steal a bit of their time to share information. Although this system works well for most, a danger of relying too much on such informal communication patterns may miss some people who are not present at that particular time. One participant noted:
In the past I have seen where you are working on something and then you run into these people and you tell one person something and then you come to a meeting and they say, 'well I didn't hear that', and then you are thinking, 'oh well I told somebody'.
4. Elements that impact cooperation
Some elements can positively or negatively affect cooperation among team members. It was felt that certain individual personalities on the team can hinder cooperation and pose a challenge to how the team worked together. However, for the most part, the teams were working towards finding ways to foster a cooperative working environment by having face-to-face meetings and learning about other team members' professional roles in the community.
Cooperation among team members was sometimes impacted negatively by the personalities of some individuals. The teams needed to accommodate these personalities and by doing this were able to work towards creating a more cooperative atmosphere. As one participant stated: '... it is affected by personalities ... but we just respect everybody's personalities and we try to accommodate everybody's personality and needs'.
It is considered a rare opportunity for practitioners, working in different agencies, to be able to sit together in meetings and take the time to discuss issues related to their clients. Having the chance to meet face to face enhances cooperation between the team members as it is seen as a more efficient way than trying to coordinate efforts using email or phone. Through face-to-face meetings, the members discovered ways in which they could support each other in their practice; everyone's input was valued while working towards common goals. The high degree of cooperation on the team spilled over into the organizations they represented, combining the efforts to make a difference in their community in areas apart from palliative care. The community development worker expressed the following:
Getting people just sitting face to face at the same table as opposed to relating to each other through a letter from the organization has made, I think, a big difference. I've seen communities where there's a particular problem that an agency has with the [palliative care] volunteer program. They are having difficulty with visibility, like making themselves known, people remembering to refer, you know? That problem was brought to the table and it was 'Okay, what do we do about this?' and they worked together ... you know, that kind of cooperation. People are becoming aware of other people's realities and they've been willing to work together.
Not everyone on the team was familiar with the various organizations represented on the team or what role they play in palliative care. Some of the teams recognized the need to educate each other about their roles to foster cooperation and open the lines of communication. This practice not only improved the relationships between team members but also enhanced everyone's individual practice as they became aware of services that their clients could benefit from. As one team member stated:
Oh, we have wonderful cooperation between team members ... I introduced a process to update the team members because we have such a diverse group ... so each month that we meet, one of our members makes a presentation about the services that they have available to offer to clients.
5. Assertiveness helps to move the process of change
Assertiveness by the group and within the group helped create change in the communities, especially for certain resources in short supply. Since individual members of the team represented their agencies and clients, the team felt the meetings were a good place for everyone to speak up and be heard about the areas of concern.
By collectively asserting themselves, teams were able to advocate for resources in their community that would benefit all palliative care clients. Through this process, community organizations were able to see the individuals working together as a team, with a strong identity and common goals. The community development worker expressed the following:
... for instance, what little [rural community], they wrote a letter jointly to the counselling services because they were concerned about a counselling position that they weren't sure was going to be replaced, and they just wanted to make sure that the organization knew that they needed it for their palliative care team. So they were uniting to assert themselves and saying, 'We are a team and we know this concern'.
The research participants felt strongly that assertiveness was not a negative concern for members on the team; in fact, it was strongly encouraged. Assertiveness was recognized as a necessary skill in order to advocate for clients and for addressing the larger system issues required for an improvement in services. Frontline healthcare workers were seen as the keepers of systemic concerns, and the ones who needed to make concerns known. The palliative care team was seen as a safe environment for these concerns to be brought forward. One individual commented:
If somebody ... has opinions that we are not expressing, then they need to bring it up ... everybody is pretty good about saying what they think. I don't think we have anybody who dominates ... there is ample opportunity, everybody gets a chance.
6. Autonomy is a well-established process
Autonomy was seen as a process that was well established within the rural organizations, allowing for practitioners to be generalists in their scope of practice. Within team members' individual organizations, they were able to establish that being part of the palliative care team is a valued aspect of their work, and were thereby able to devote time to it.
The community palliative care teams do not belong to any one organization or agency within the community; they are made up of employees from a number of sectors, including health care and social services, as well as other organizations in the community that are pertinent to achieving quality palliative care. Therefore, the teams themselves are considered a separate entity, and the members of the teams are striving to be recognized as autonomous by the broader community. As the community development worker stated: 'I think these teams are very autonomous. I don't think any one of them feel that the team belongs to anyone more or less than anyone else'.
Each of the team members volunteered time from their busy schedule, and even their personal lives, towards creating a palliative care team. The professionals added this role to their workload; however, they felt that being a rural practitioner gave them a high degree of autonomy in their place of employment. This autonomy allowed them to negotiate what they felt was important to their work.
For the team members, working in a rural community aided their involvement within the team because they have the freedom to define their role as they see fit. As one participant stated: 'I think within our organization, we all have a lot of autonomy and it makes it a lot easier to do this kind of work'. This is in part due to the generalist nature of the work done in rural communities and partly because they feel they can assert themselves within their organizations.
It was felt that the geographical distance between their satellite organization and the head organization prevented micro-management, and empowered them to take control of their professional role in the community. As another participant commented: 'Some other agencies would probably micro-manage and want to know exactly everything that you are doing, which makes it a lot more difficult'.
7. Mutual respect and trust is earned
The participants overwhelmingly felt that a degree of respect and trust exists between the team members. This respect was established over time by working together in their regular work life and being on the team.
At the beginning of the team creation process, the community development worker was meeting with teams in every community. She has been known in all communities through her role at the regional EOLC network. This allowed her to establish trust, impacting the development and growth of the team. She stated: 'I think I am comfortable with the community agencies. There is trust I think. It's based on time and number of experiences that we share'.
The community development worker also shared her belief that most of the team members had worked together in other capacities, and thus had established trust: 'It may have to do with the fact that these people do work together in other capacities outside the [team] ... there is a great camaraderie at the meetings'.
The trust and respect that exist between team members helped to foster equal relationships. They described this as 'hats are off at the door' for the team meetings. The usual hierarchical dynamics that normally exist in the clinical world do not seem to have an influence on how the members work together. Each member is seen for who she/he is, and not necessarily as her/his 'profession'. No competition between professions seems to be present, or a need to defend territory. The following comment was made by a participant:
We are very respectful of each other's opinions. Sort of hats are off at the door, you know, I am an old nurse and so the doctors are like a level above us nurses. But I feel comfortable calling her by first name when we are at the meeting. At these meetings we are all on a level playing field, and there isn't any of these, well I am a nurse and you are only a social worker.
The 'automatic teams' of rural practitioners
In addition to Way et al's25 seven essential elements of IPC, data have shown other components being experienced in rural teams. These components reflect a central element that the rural practitioners describe as automatic teams.
The practitioners' pre-existing relationships that were formed informally through social relationships, or formally through professional roles, provided the necessary foundation for rural IPC. The idea that rural practitioners already collaborate came through strongly in the data. Individuals who had come together to address the concern of palliative care in their community were those who had already been working together. These healthcare and social service providers were found to be not only involved in palliative care but also provide a wide array of services to their community, because the majority of the team members are generalist practitioners. Therefore, they are already aware of the benefits of collaboration, and many of the supports and processes of IPC have been well established prior to the creation of palliative care teams. The community development worker summarized this notion:
In [rural communities] you've almost got a team automatically ... you know we're the ones who are doing the work and nobody is paying any attention anyway. So let's roll up our sleeves and get it done.
Three identified themes are encompassed within the 'automatic teams' element: process of rural collaboration, supports to collaborative process, and indirect benefits of collaboration. Themes and sub-themes are illustrated in Figure 3.
Process of rural collaboration: The demands placed on rural service providers are extensive. Nevertheless, the practitioners sensed a need to come together and address the issue of palliative care service delivery in their communities. There is an undeniable resource drought in rural communities, both human and financial. However, these circumstances do not deter the service providers from working together and finding solutions. The prevalent feeling of team members is 'we just do it'. Progress is being made because the members feel a responsibility to their clients and their community. The process and structure of the teamwork in rural community is both unique and informal in nature; these unique and informal characteristics are required in order to meet the demands of team members' busy schedules. Rural generalist practice creates informal collaboration because the process is developed over time by working together and making connections, as needed, to serve clients. Most of the present team members had acted as a team without being called as such. Personal relationships that develop out of being in a small community added to the confidence in the relationships.
The rural teams are also unique in the structure and processes of collaboration. They are made up of self-selected community members who make each team in each community unique. The team profiles display the variety of professionals involved, from nurses, social workers and physicians, to funeral home workers, lawyers and ambulance drivers. Having members on the team with a wide variety of professional backgrounds allows for representation of different services, such as government, private and not-for-profit sectors, giving the team a voice in all service areas. The process of collaboration has also been unique in each community, given unique sets of issues and goals, which teams work on and prioritize.
Supports to collaborative process: Many supports are in place for a collaborative process, and they became evident when speaking with rural practitioners. The primary support is the fact that these practitioners apply a generalist approach to their practice, which is very common in rural communities. The working relationships pre-dated the formation of palliative care teams; many elements of collaboration were already established: 'everybody knows each other' when living and working in rural communities. However, the piece that has kept the palliative care teams moving forward is the local leadership, which assisted in the coordination of team development. In addition was recognition that the community does not have all the resources necessary to provide good palliative care readily available. The team was open to receiving outside community support, such as clinical expertise, not available in rural communities, as well support to strengthen the collaborative process.
Indirect benefits of collaboration: Secondary benefits to the collaborative process were observed: informal networking improves services in the community and is not only limited to palliative care. The team members also recognized the importance of face-to-face meetings; this essential piece of collaborative process improved the participants' practice outside of the mandate of the team.
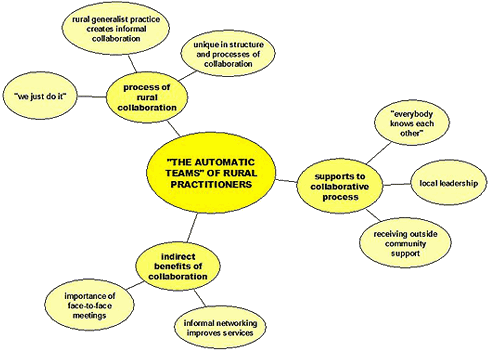
Figure 3: The 'automatic teams' of rural practitioners.
The purpose of this research was to gain an understanding of the processes and structures of IPC during the development of rural palliative care teams and programs. The process of development of palliative care teams, as per Kelley's model10, is now enhanced through the analysis of the dynamics of interprofessional collaboration, which provides momentum for the work. Responsibility and accountability, coordination, communication, cooperation, assertiveness, autonomy, and mutual trust and respect were observed in those rural communities studied. These seven elements, previously identified by Way et al25, were not only evident in development of palliative care teams but also essential to their functioning. The formal coming-together as a team in a collaborative way helped to improve palliative care in these rural communities.
The research has shown that Ways et al's25 essential elements of IPC were very much integrated in rural teams' collaborative practice, and thus validated the applicability of these elements in a rural context. However, all seven elements were implemented with a rural twist: the distinctiveness of rural environment was observed in each element. Another element, specific to rural context, was observed, that being the 'automatic teams' of rural practitioners - the collaboration had been established informally and almost automatically between rural practitioners. There are a limited number of healthcare and social service practitioners available in rural communities; by necessity, they are used to working together in all aspects of their work. How rural practitioners work together is an important process to understand. They face enormous challenges and obstacles in providing the type of care they feel their clients need and deserve. IPC is an automatic and informal process that helps rural practitioners provide quality of care.
This study shows that rural IPC can be facilitated between members of different backgrounds and experiences, which can include people from non-medical and medical sectors, and also from the general public. Recruiting and preparing professionals to practise in rural communities is challenging. The information on the processes and structures that support IPC could help to prepare students and new professionals when they consider practising in rural communities. Learning the culture of rural IPC is likely required for those incoming practitioners new to rural practice.
Acknowledgements
This research was funded by a Canadian Institutes of Health Research Interdisciplinary Capacity Enhancement Grant, CIHR ICE grant HOA-80057, entitled Timely Access and Seamless Transitions in Rural Palliative/End-of-Life Care.
References
1. Brooksbank M. Palliative care: where have we come from and where are we going? Journal of the International Association for the Study of Pain 2009; 144(3): 233-235.
2. Marchildon GP. Health systems in transition: Canada. Toronto, ON: University of Toronto Press, 2005.
3. Williams A, Crooks V, Whitfield K, Kelley M, Richards J, DeMiglio L, et al. Tracking the evolution of hospice palliative care in Canada: a comparative case study analysis of seven provinces. BMC Health Services Research 2010; 10(147): 1-15.
4. Wilson D, Truman C, Thomas R, Fainsinger R, Kovacs Burns K, Froggatt K, et al. The rapidly changing location of death in Canada, 1994-2004. Social Science & Medicine 2009; 68(10): 1752-1758.
5. Wilson D, Justice C, Sheps S, Thomas R, Reid P, Leibovici K. Planning and providing end-of-life care in rural areas. Journal of Rural Health 2006; 22(2): 174-181.
6. Daniels ZM, Vanleit BJ, Skipper BJ, Sanders ML, Rhyne RL. Factors in recruiting and retaining health professionals for rural practice. Journal of Rural Health 2007; 23(1): 62-71.
7. Penz K, Stewart N, D'Arcy C, Morgan D. Predictors of job satisfaction for rural acute care registered nurses in Canada. Western Journal of Nursing Research 2008; 30(7): 785-800.
8. Williams A, Cutchin M. The rural context of health care provision. Journal of Interprofessional Care 2002; 16(2): 107-115.
9. MacLean MJ, Kelley ML. Palliative care in rural Canada. Rural Social Work 2001; 6(3): 63-73.
10. Kelley ML. Developing rural communities' capacity for palliative care: a conceptual model. Journal of Palliative Care 2007; 23(3): 143-153.
11. Saunders C. Social work and palliative care: the early history. British Journal of Social Work 2001; 31(5): 791-799.
12. Doyle D. The IAHPC manual of palliative care, 3rd edn. (Online) 2013. Available: http://hospicecare.com/about-iahpc/publications/manual-of-palliative-care (Accessed 2 May 2014).
13. HealthForce Ontario. Interprofessional care: a blueprint for action in Ontario. Government of Ontario (Online) 2007. Available: http://www.healthforceontario.ca/en/Home/Policymakers_and_Researchers/Interprofessional_Care/Resources (Accessed 2 May 2014).
14. Health Professions Network Nursing and Midwifery Office, Department of Human Resources for Health. Framework for action on interprofessional education & collaborative practice. (Online) 2010. Available: http://whqlibdoc.who.int/hq/2010/WHO_HRH_HPN_10.3_eng.pdf (Accessed 15 May 2012).
15. World Health Organization. Declaration of Alm-Ata 1978. Report of the International Conference on Primary Health Care, Alma-Ata, USSR, 6-12 September 1978. (Online). Available: http://whqlibdoc.who.int/publications/9241800011.pdf (Accessed 2 May 2014).
16. Miedema B, Hamilton R, Fortin P, Easley J, Tatemichi S. The challenges and rewards of rural family practice in New Brunswick, Canada: lessons for retention. Rural and Remote Health 9(2): 1141. (Online) 2009 Available: www.rrh.org.au (Accessed 23 January 2012).
17. Penz K, Stewart N, D'Arcy C, Morgan D. Predictors of job satisfaction for rural acute care registered nurses in Canada. Western Journal of Nursing Research 2008; 7(1): 12-26.
18. Pong R, Desmeules M, Lagac C. Rural-urban disparities in health: how does Canada fare and how does Canada compare with Australia? Australian Journal of Rural Health 2009; 17(1): 58-64.
19. Canadian Institute for Health Information. How healthy are rural Canadians? An assessment of their health status and health determinants. (Online) 2006. Available: https://secure.cihi.ca/estore/productFamily.htm?pf=PFC1180&lang=en&media=0 (Accessed 2 May 2014).
20. Arredondo P, Shealy C, Neale M, Logan Winfrey L. Consultation and interprofessional collaboration: model for the future. Journal of Clinical Psychology 2004; 60(7): 787-800.
21. Bronstein L. Index of interdisciplinary collaboration. Social Work Research 2002; 26(2): 113-123.
22. Canadian Interprofessional Health Collaborative. A national interprofessional competency framework. (Online) 2010. Available: http://www.cihc.ca/files/CIHC_IPCompetencies_Feb1210.pdf (Accessed 1 April 2010).
23. Gilbert JH. Interprofessional education for collaborative, patient-centred practice. Nursing Leadership 2005; 18(2): 32-38.
24. Pollard KC. Non-formal learning and interprofessional collaboration in health and social care: the influence of the quality of staff interaction on student learning about collaborative behaviour in practice placements. Learning in Health and Social Care 2008; 7(1): 12-26.
25. Way D, Jones L, Busing N. Implementation strategies: "Collaboration in primary care - family doctors & nurse practitioners delivering shared care". (Online) 2000. Available: http://www.eicp.ca/en/toolkit/hhr/ocfp-paper-handout.pdf (Accessed 23 January 2012).
26. Kelley ML, Williams A, DeMiglio L, Mettam H. Developing rural palliative care: validating a conceptual model. Rural and Remote Health 11(2):1717. (Online) 2011. Available: http://www.rrh.org.au/assets/article_images/article_print_1717.pdf (Accessed 23 January 2012).
27. Thorne, S, Kirkham, SR, O'Flynn-McGee K. The analytic challenge in interpretive description. International Journal of Qualitative Methods 3(1): 1. (Online) 2004. Available: http://www.ualberta.ca/~iiqm/backissues/3_1/pdf/thorneetal.pdf (Accessed 14 April 2013).
28. Ontario Ministry of Health and Long-Term Care. Ontario's aging at home strategy. (Online) 2007. Available: http://www.health.gov.on.ca/en/public/programs/ltc/33_ontario_strategy.aspx (Accessed 2 May 2014).
29. Dudgeon D, Vaitonis V, Seow H, King S, Angus H, Sawka C. Ontario, Canada: using networks to integrate palliative care province-wide. Journal of Pain and Symptom Management 2007; 33(5): 640-644.
30. DesMeules M, Pong RW, Read Guernsey J, Wang F, Luo W, Dressler MP. Rural health status and determinants in Canada. In: J Kulig, A Williams (Eds). Health in rural Canada. Vancouver, BC: UBC Press, 2011; 23-43.
31. Northwestern Ontario District Health Council. Annual long-term care service plan for Northwestern Ontario. Thunder Bay, ON: Northwestern Ontario District Health Council, 2001.
32. Statistics Canada. Census profile. (Online) 2011. Available: http://www12.statcan.gc.ca/census-recensement/2011/dp-pd/prof/index.cfm?Lang=E (Accessed 28 January 2013).
33. Habjan S, Diamond L, Kelley ML. Northwestern Ontario palliative care needs assessment (2008). (Online) 2008. Available: http://cerah.lakeheadu.ca/research-reports (Accessed 23 November 2011).
34. Thorne S. Data analysis in qualitative research. Evidence Based Nursing 2000; 3(3): 68-70.
35. Patton MQ. Enhancing the quality and credibility of qualitative analysis. Health Services Research 1999; 34(5): 1189-1208.


