Cardiovascular disease accounted for 30% of deaths globally in 20051. Non-communicable diseases increasingly impact health, with prevention and management of such diseases identified internationally as a key target for healthcare agencies and workers2. Cardiovascular disease, as a leading cause of death, has been identified as one of the central disease foci where prevention, identification of people at risk and evidence-based management of disease lowers morbidity and mortality3.
Best practice guidelines provide consistent evidence that exercise, education, behavioural interventions and support are beneficial to people after an acute cardiac event and for the prevention of further events4. Secondary prevention cardiac rehabilitation, refers to programs that facilitate recovery from acute cardiac events, promote lifestyle changes and modify risk factors in order to reduce the likelihood of further cardiac-related events5. The core components of cardiac rehabilitation are similar to primary prevention models and include lifestyle education (ie physical activity and exercise, diet and weight management, and smoking cessation); risk factor management; psychosocial wellbeing; drug therapy and long-term management strategies6.
In Australia, both government and non-government agencies provide cardiac rehabilitation programs (CRPs) and these are often associated with acute-care settings where individuals have received treatment for a cardiac event or surgery. Increasingly Australian healthcare providers are also adopting chronic disease self-management models to deliver cardiac rehabilitation7. Central to self-management is problem-solving, decision-making, resource utilization, patient-healthcare provider partnership, and action planning leading to self-efficacy8. Evidence to support the role of self-management in chronic diseases such as cardiovascular disease continues to grow8-10, with the National Heart Foundation of Australia recognising the central role of self-management approaches to cardiac rehabilitation in both primary and secondary prevention strategies11.
In Australia and other socioeconomically developed countries, people in regional areas experience a higher prevalence of all risk factors associated with chronic disease, as well as higher levels of cardiovascular disease than their urban counterparts12,13. Lower access to health resources and fewer healthcare workers have been suggested as reasons for these disadvantages14. Despite evidence that rural and remote residents experience the greatest burden of cardiovascular disease and require services at a higher level15, their needs are poorly addressed. The site of this research is a prime example of rural inequity. In this location 27% of rural residents live with cardiovascular disease, and this is well above the 16% national average16; however, there has been no provision of cardiac rehabilitation locally.
Despite the recognised benefits of participation, access to CRPs in rural Australia is low17-19. Home-based cardiac rehabilitation using self-management with telephone contact, home visits or a combination of these have been identified as effective and potentially valuable for rural and remote populations15,20. However there is also recognition of the need to offer participants options and choices about how they might complete cardiac rehabilitation in order to meet the range of individual needs and preferences.
Improving funding allocation for rehabilitation programs has been identified and targeted by the Heart Foundation as a strategy for improving cardiovascular health11. Funding availability can restrict service provision, and limit use of space, consumables and the staff required to support a program15. Such was the case in the setting chosen for the pilot program of rural cardiac rehabilitation, where healthcare providers expressed a need for such a program but were constrained by lack of resources.
In addition to ensuring programs are available, it is also necessary to consider maximising participation rates. Endorsement of programs by GPs, together with ease of access and transportation, are strategies that have increased attendance21, rural program participants can be particularly vulnerable to the barriers of travel distance22. Anecdotal evidence from the clinicians in the hospital where the cardiac rehabilitation was provided confirmed the experience of their rural colleagues and findings from the literature that rural residents are unable to attend cardiac rehabilitation because of distance, travel requirements and the importance assigned by medical practitioners.
The benefits of cardiac rehabilitation have been established and providers must aim to reach the broadest range of participants for maximum benefits. The development of a research office in the acute-care setting and an established relationship with private and public healthcare providers in a rural community provided an opportunity to develop and deliver a CRP in collaboration with the local community. The intent of the research team was to investigate the feasibility of delivering a rural CRP while fostering further collaboration among local healthcare providers. The structure of the pilot program, if deemed successful, together with participant outcomes, were intended to guide the teams' decisions related to the ongoing delivery of the program.
A pilot rural CRP was offered to local people following cardiac surgery, diagnosis of cardiovascular disease and/or identification by health practitioners as being at risk of developing cardiovascular disease. The researchers relied on the health practitioners to identify those at risk by assessing factors such as being overweight, having diabetes, family history and high cholesterol. Sessions were held at the local community health centre in a conference room weekly in June and July 2010.
Recruitment and ethics approval
Participants were recruited from both the major tertiary hospital and medical centres in the rural community. All participants provided signed consent to participate in the research. However, if any had wished to participate in the program and not the research, access would have been granted, in keeping with the primary healthcare principles of access and equity. Ethics approval was sought and provided by the Tasmanian Health and Medical Human Research Ethics Committee (H11042).
Hospital: The research team provided information about the program to the cardiac rehabilitation nurses at the major tertiary hospital, including a participant information sheet and consent form. Referral to cardiac rehabilitation was offered to all cardiac patients as part of their normal care. The nurse identified community residents, provided them with an information sheet, and offered the patient a choice of where they would prefer to undertake their cardiac rehabilitation. The nurse then provided participant details to the research team.
Community: The research team disseminated program and study information to two medical centres in the rural community. General practitioners and practice nurses identified potential participants, that is those who had a formal diagnosis of cardiac disease, or who were at risk of developing it, and would therefore benefit from program attendance. The GPs referred these patients to the program; practice nurses provided patients with the information sheet and notified the research team of participant details.
The program
A chronic disease self-management model (CENTREd) with a focus on participant-centred engagement was adopted to guide the 7 week program. The CENTREd model incorporates a focus on the 'SNAPPS' healthy behaviours of Smoking cessation, Nutrition, Alcohol restraint, Physical activity adoption, Psychosocial wellbeing and Symptom-management7. Healthcare professionals in the area where the rehabilitation was provided had previously completed CENTREd training (funded by the Australian Better Health Initiative: a joint Australian, State and Territory government initiative, 2009-2010).
The first session of the CRP was an introduction to the concepts of goal setting, action planning and problem solving. Each subsequent session was of approximately 2 hours duration and focused on a SNAPPS behaviour. In keeping with the self-management focus, following each session participants identified and implemented a personal action plan for change, focussed on SNAPPS behaviours. At the following session participants shared their experience in implementing their goals and the group worked together to find solutions. Facilitators also participated in goal setting, action planning and problem solving to build rapport and demonstrate collaboration. Augmenting the program, and further engaging local providers in delivery, public and private allied-health professionals from the community who had expertise in specific areas provided additional information to assist participant knowledge and understanding. A nurse from general practice and a community health nurse were mentored in the role of facilitator in order to continue the program after the pilot.
Analysis
Participants completed the Health Education Impact Questionnaire (HeiQ)23 at the first and last sessions, and at 6 month follow up. The validated questionnaire measures the impact of health education across 8 domains: health directed behaviour; positive and active engagement in life; emotional wellbeing; self-monitoring and insight; constructive attitudes and approaches; skill and technique acquisition; social integration and support; and health service navigation. In addition, at completion of the program data was collated regarding attendance and acceptability from both participant and facilitator viewpoints. Participants were invited to comment on what they found helpful or not so helpful in the program, and suggestions were invited for future programs. These comments were contributed during a feedback session in the final sessions, and also in completion of the HeiQ questionnaire, which also elicited program evaluation data.
A total of eight participants, four men and four women, completed the program and received certificates. A further two people were recruited to the study but did not attend any sessions (despite follow up their reasons for non-attendance were not obtained). In addition to the eight participants, one participant (a support person) attended the first session but did not wish to continue. Detailed information about session attendance is provided (Table 1).
Table 1: Participants' weekly attendance at the program
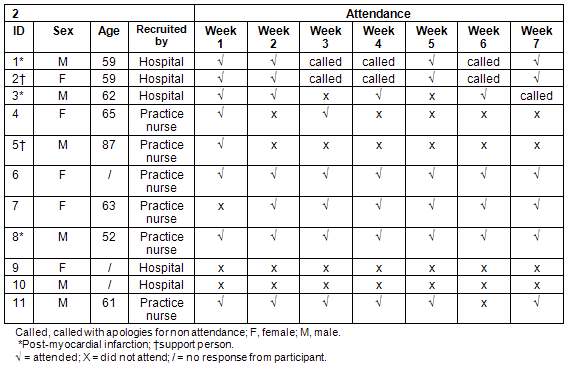
The reasons for regular participants' non-attendance included medical appointments, social events and personal issues. For example, participant 4 attended only two sessions, because she was required to provide carer support to a family member, and participant 3 identified and then attended only the sessions he believed would be of most benefit.
The HeiQ questionnaire indicated improvements for participants both pre- (n=7) and post-program (n=6) and again at 6 months (n=5). All participants completed the questionnaire pre-program but there was a lower response rate at the post-program and 6 month follow up. Pre-, post- and 6 month means and standard deviations are reported, as are mean changes from pre-program to 6 month follow up (Table 2).
Table 2: Health Education Impact Questionnaire mean and standard deviation at 3 time points
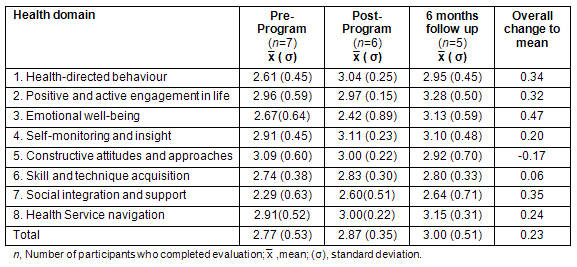
Means recorded pre- and post-evaluation demonstrate improvements across most health domains. The 6 month follow up showed stability or further improvements in most domains. Overall, the mean scores improved post-program and again at 6 months.
Participant feedback supported the notion that provision of the program locally removed barriers to attendance. It is of note that two participants (3 and 7) still had to travel for more than 30 min to attend, and they reported this as a partial barrier to attendance. Participants described the information provided about local resources, including healthcare professionals, sporting clubs and walking groups as beneficial. For example, participant 6 was active in a weekly Heart Foundation walking group and encouraged others to attend. The ongoing engagement of the group in building relationships to support healthy behaviours was evident in group discussions where there was encouragement among individuals to 'give things a go' and try activities offered in the community. The value of the program was further highlighted when all six participants who completed the post-program evaluation reported they would tell others that the program was worthwhile. All participants said their investment of time and effort in the program had provided benefits. The majority of participants also considered the content of the program relevant to their situation.
Qualitative comments indicated the self-management approach embedded in the program via the CENTREd model was of particular benefit. For example, one respondent noted it was 'Good to be accountable...' for reporting back on action plans. Another participant commented they 'Haven't felt threatened, my choices', recognising the supportive environment of the group as contributing to self-empowerment and participation. Others commented that the program was 'Holistic...the total me' and that they enjoyed the 'Local focus compared to seeing cardiologists [outpatient hospital clinics]'. The 'Personal approach' of the program was valued by group members who welcomed information provided by allied-health team members either as a 'refresher' or as developing new knowledge.
Healthcare professionals engaged in the delivery of the program provided feedback and noted that their involvement in the program was beneficial. The delivery of the program at the local community health centre highlighted their connection with the primary healthcare principles of access and equity. The program facilitators were from public and private healthcare providers in the local area and their involvement enhanced the private-public partnership, for example the general practice nurse planned further collaboration with the community health nurses. The community health nurse and practice nurse were each able to attend all but one session, indicating that delivery in the context of current practice was achievable. Those healthcare professionals who provided specialist information sessions also found the commitment to the course manageable, although the high level of questions received by the pharmacist suggested that more time could have been allocated to question and answer.
Others contributors included the social worker and physiotherapist. While there was no dietician available to provide specialist information or advice, the nurses were able to successfully deliver that session, based on established Australian guidelines for healthy eating and recommended dietary guidelines. The information they provided about reading food labels was noted as particularly helpful by two participants.
Discussion
It has been established that cardiac rehabilitation delivers benefits to participants, including a key outcome of a 25% mortality reduction24, supporting the claim that cardiac rehabilitation should be delivered to all patients with cardiac disease6. As a result, other researchers have explored the best way to deliver cardiac rehabilitation20,25-28 and the core content of such programs29. Rural communities have also been the focus of investigations with the recognition that many rural people are disadvantaged in terms of access, despite experiencing higher levels of disease15,17,18,22. Such investigations support the need for a multifaceted, flexible approach to program provision which is aligned with community and individual needs30. The aim of this pilot study was to explore the feasibility, acceptance and support for delivery of a secondary prevention CRP in a rural community, while ensuring the quality of the program led to intended patient outcomes.
If lack of funding or resource support provides barriers to program provision, clinicians should consider innovative and cost-effective methods to enable delivery. At program inception the research team aimed to develop and deliver a CRP which served several purposes. Key among these was to provide a program which could be replicated by local providers at little cost, and would be sustainable in the community. The small grant of approximately AU$5,000 allowed the establishment of collaboration between acute and community care, with the acute-care team providing initial support. Funding for the program permitted the acquisition of resources that included questionnaire licensing, pamphlets, pedometers, exercise DVDs and development of participant and facilitator resource folders. There was no cost for the involvement of government and non-government healthcare professionals with the exception of time spent by the practice nurse at sessions, hire of premises, advertising or recruitment. Instead these was provided in-kind, as part of usual work duties.
At CRP completion, local healthcare providers stated they were firmly committed to continuing delivery of the program. Continuing delivery will be based on relationships that were established and enhanced during the program between government and non-government providers, and on the commitment of resources. The continued involvement of those in the acute-care sector will ensure expert advice and referral of clients. The pilot CRP approach was innovative in spreading the small ongoing cost among multiple providers who are committed to the program. For example the local pharmacist, a small business owner, provided time and expertise at no cost, because the benefit to the community was considered to be worthwhile without a large cost to the business itself. Publicly funded community health nurses and the management of the local health centre have also committed their time and space to ongoing program delivery. As such, this CRP is feasible and will continue to be well supported by the local community.
Highlighting the importance of local involvement, more than half the participants were recruited by a local practice nurse who was co-facilitator of the CRP. This nurse's established relationship with these participants appears to have been influential, according to their attendance rates. With the exception of the participant who had family obligations, the other four participants recruited by the practice nurse had the highest levels of attendance. This is consistent with previous research that has established the importance of healthcare providers' individual recommendations in highlighting potential benefits and taking into account the receptiveness of participants21,22,30. It highlights the role of utilising established relationships to improve program attendance as an area for further investigation. However, the support of community extends beyond the role of facilitators and healthcare professionals, as indicated by participant responses stating that they would recommend the program to others in the community. The impact of this should not be underestimated22 and can influence rates of attendance and the future participation of others.
The acceptance of the CRP was demonstrated by the positive response from local healthcare providers and their commitment to ongoing delivery. In addition, the evaluation suggests the program was successful for individual participants, providing immediate and ongoing benefits. For at least half the participants, the rural CRP provided an attendance opportunity that would not have been feasible if the course had been provided at the acute-care hospital. Although some participants were already taking steps to improve their own health, all believed the structure of the CRP provided additional information and motivation to achieve their goals.
Limitations and future research
As this was a pilot program, the number of participants was not sufficient to provide statistically significant results. Instead, the results support the need for further research, with participant numbers which allow for greater analysis of effect. The completed pilot, however, allows clinicians in other rural communities to make decisions about the feasibility of implementing similar programs and extending the sample size. Differences in community characteristics related to available resources and facilitators would need to be considered, as would the inclusion of a control group for comparison. The small sample size means this CRP can not claim to have reduced early mortality or made savings for the health system; however, larger reviews have indicated that CRPs addressing a range of modifiable risk factors improve health outcomes for primary and secondary prevention in patients28,31.
Demonstrated increased attendance and the availability of a CRP in this rural area indicate the pilot program was successful. It will continue to be delivered and evaluated. This approach has the potential to be used in other rural areas with minimal cost outlay, utilising the resource folder developed as part of the pilot which is structured to provide flexibility. Future participants will continue to be recruited from acute care following a cardiac event, and also from the local general practices. The continued collaboration and local involvement of healthcare providers is the key to this program's success.
Acknowledgements
The funding for providing this cardiac rehabilitation program came from a Huon Valley Health Services Advisory Committee small grant. The program would not have been successful without the support of clinicians from general practice, Cardiac Rehabilitation Unit, Royal Hobart Hospital, Huonville Community Health Centre, the Department of Health and Human services, participants in the program and the Huon Community generally.
References
1. World Health Organisation. Prevention of cardiovascular disease: guidelines for assessment and management of cardiovascular risk. Geneva: WHO, 2007.
2. World Health Organisation. Preventing chronic disease: a vital investment. Geneva: WHO, 2005.
3. World Health Organisation. Cardiovascular disease prevention and control: translating evidence into action. Geneva: World Health Organisation, 2005.
4. Australian Cardiovascular Health and Rehabilitation Association. Practitioner's guide to cardiac rehabilitation. Sydney, NSW: ACRA, 2008.
5. Human Services Victoria. Best practice guidelines for cardiac rehabilitation and secondary prevention. Melbourne, VIC: Victorian Government, 1999.
6. National Heart Foundation and Australian Cardiac Rehabilitation Association. Recommended framework for cardiac rehabilitation. National Heart Foundation of Australia, 2004. Available: http://www.heartfoundation.org.au/information-for-professionals/Clinical-Information/Pages/coronary-heart-disease.aspx (Accessed 1 April 2011).
7. Cameron-Tucker H. There is more to supervised exercise than exercise itself: a mixed methods study of supervised exercise with the chronic disease self-management program for people with COPD. PhD thesis. University of Tasmania, 2009.
8. Lorig K, Holman H. Self-management education: history, definition, outcomes, and mechanisms. Annals of Behavioral Medicine 2003; 26: 1-7.
9. Lorig KR, Sobel DS, Stewart AL, Brown BW, Bandura A, Ritter P et al. Evidence suggesting that a chronic disease self-management program can improve health status while reducing hospitalization: a randomized trial. Medical Care 1999; 37: 5-14.
10. Lorig KR, Sobel DS, Ritter PL, Laurent D, Hobbs M. Effect of a Self-Mangement Program on Patients with Chronic Disease. Effective Clinical Practice 2001; 4: 246-262.
11. National Heart Foundation of Australia. Secondary prevention of cardiovascular disease: a call to action to improve the health of Australians. Canberra, ACT: National Heart Foundation of Australia, 2010.
12. British Heart Foundation Health Promotion Research Group and Health Economics Research Centre. European cardiovascular disease statistics. Oxford: Department of Public Health, University of Oxford, 2008.
13. Lloyd-Jones D, Adams RJ, Brown TM, Carnethon M, Dai S, De Simone G et al. Heart disease and stroke statistics - 2010 update: a report from the American Heart Association. Circulation 2010; 121(7): e46-215.
14. World Health Organisation. Increasing access to health workers in remote and rural areas through improved retention: global policy recommendations. Geneva: WHO, 2010.
15. Dollard J, Smith J, Thompson D, Stewart S. Broadening the reach of cardiac rehabilitation to rural and remote Australia. European Journal of Cardiovascular Nursing 2004; 3(1): 27-42.
16. Australian Bureau of Statistics. National Health Survey: 2007/08. Cat no. 4364.0. Canberra, ACT: AGPS, 2009.
17. Parker E, O'Connor Fleming M, Tooth L, Humphries RJ. Developing a cardiac rehabilitation education resource for rural health workers in Queensland: reviewing the process and outcomes. Australian Journal of Rural Health 2002; 10: 15-19.
18. Wachtel TM, Kucia AM, Greenhill JA. Unstructured cardiac rehabilitation and secondary prevention in rural South Australia. Contemporary Nurse 2008; 29: 195-204.
19. Aoun S, Rosenberg M. Are rural people getting HeartSmart? Australian Journal of Rural Health 2004; 12: 81-88.
20. Blair J, Corrigall H, Angus NJ, Thompson DR, Leslie S. Home versus hospital-based cardiac rehabilitation: a systematic review. Rural and Remote Health 11(1):1532. (Online) 2011. Available: www.rrh.org.au (Accessed 1 May 2011).
21. Jackson L, Leclerc J, Erskine Y, Linden W. Getting the most out of cardiac rehabilitation: a review of referral and adherence predictors. Heart 2005; 91: 10-14.
22. De Angelis C, Bunker S, Schoo A. Exploring the barriers and enablers to attendance at rural cardiac rehabilitation programs. Australian Journal of Rural Health 2008; 16: 137-142.
23. Osborne RH, Elsworth GR, Whitfield K. The Health Education Impact Questionnaire (heiQ): An outcomes and evaluation measure for patient education and self-management interventions for people with chronic conditions. Patient Education and Counselling: An International Journal for Communication in Health Care 2007; 66: 192-20.
24. Ades PA. Cardiac rehabilitation and secondary prevention of coronary heart disease. New England Journal of Medicine 2001; 345(12): 892-902.
25. Davies P, Taylor F, Beswick A, Harris-Wise F, Moxham T, Taylor RS. Promoting patient uptake and adherence in cardiac rehabilitation (Protocol). Cochrane Database Systematic Reviews 2008; CD007131. DOI: 10.1002/14651858.CD007131.
26. Harris DE, Burgess N. Cardiac rehabilitation in community settings. Journal of Cardiopulmonary Rehabilitation 2003; 23(4): 250-259.
27. Walters DL, Sarela A, Fairfull A, Neighbour K, Cowen C, Stephens B et al. A mobile phone-based care model for outpatient cardiac rehabilitation: the care assessment platform (CAP). BMC Cardiovascular Disorders 2010; 10(5): 1-8.
28. Clark A, Hartling L, Vandermeer B, McAlister F. Meta-analysis: secondary prevention programs for patients with coronary artery disease. Annals of Internal Medicine 2005; 143(9): 659-672.
29. Balady GJ, Williams MA, Ades PA, Bittner V, Comoss P, Foody JM et al. Core components of cardiac rehabilitation/secondary prevention programs: 2007 update: a scientific statement from the American Heart Association Exercise, Cardiac Rehabilitation, and Prevention Committee, the Council on Clinical Cardiology; the Councils on Cardiovascular Nursing, Epidemiology and Prevention, and Nutrition, Physical Activity, and Metabolism; and the American Association of Cardiovascular and Pulmonary Rehabilitation. Circulation 2007; 115(20): 1069-1073.
30. Briffa TG, Kinsman L, Maiorana AJ, Zecchin R, Redfern J, Davidson PM et al. An integrated and coordinated approach to preventing recurrent coronary heart disease events in Australia. Depression 2009; 3(4): 683-686.
31. 33. Lavie CJ, Thomas RJ, Squires RW, Allison TG, Milani RV. Exercise training and cardiac rehabilitation in primary and secondary prevention of coronary heart disease. Mayo Clinic Proceedings 2009; 84(4): 373-383.


