Suicide is an important public health problem1. Suicide rates vary among areas, and over time; however, common risk factors included male gender, poverty, mental illness and substance misuse2, and rates are also high in some rural areas3,4. Higher rural rates may be related to a number of influences. These include isolation, limited support or reluctance to access support, access to lethal methods of self-harm and, in some parts of the world, limited access to medical care following self-harm5.
There is good evidence that many people have contact with services prior to their death by suicide6,7. The Scottish suicide prevention strategy Choose Life has training of health and social care staff as a major part of its requirements8. The training is intended to raise awareness among service providers and improve response to suicide risk.
The Highland Council area is the largest local authority area in the UK. It covers an area of more than 26 000 km2, approximately one-third of the land area of Scotland, but has less than 5% of the Scottish population. In Scotland, there have been previous studies in the north-east of the country9,10, but rates of contact prior to suicide for the Highland area are unknown. The work in north-east Scotland did not differentiate between contact rates in different types of area, and no other previous study appears to have examined this.
This study aimed to identify contact rates prior to death by suicide in the Highlands of Scotland, and to establish whether contact rates varied between rural and urban areas.
The names of Highland residents dying by suicide or undetermined intent, and whose deaths were registered in Scotland during 2001-2004 were obtained from the General Registrar Office for Scotland (NHS Highland residents who died anywhere in Scotland would be identified by this mechanism).
Relevant health service databases were then searched to identify the person's GP, and whether they had general hospital or psychiatric case notes. There are no non-NHS hospitals in the north of Scotland, and therefore searches of these sources are likely to have identified all service contacts. General practice case notes were obtained from practitioner services, and hospital case notes requested from storage.
In a pilot phase, 20 records of each type (general practice, general hospital and mental health) were identified at random, and data extracted independently by three assessors. Results were compared, and a set of standard forms and definitions agreed. All case notes were then re-examined using the standard definitions and forms.
The standard forms were used to collect information from the case notes, and results were recorded on a computer database (Microsoft Access). Categorical data such as the frequency of contact by geographical area were compared using the χ² test. Continuous data, including age by category of contact with services, were compared using the Mann-Whitney U-test. The SPSS software package (www.spss.com) was used to obtain the two-tailed level of significance.
Ethics approval
Ethics approval was obtained through the North of Scotland Research Ethics Committee (#05/S0901/12).
Demography
In total, 177 residents of the Highland Council area died by suicide (n=106) or undetermined intent (n=71) in the period 2001-2004 (136 male). Age distribution is shown according to sex (Fig1).
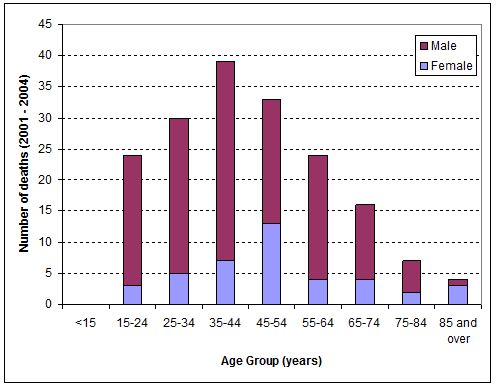
Figure 1: Age distribution of people dying by suicide or undetermined intent Highland Council Area, 2001-2004.
Previous service contact
At least one set of health service case notes was identified on 175 people (98.9%). General practice records were located for 167 people (94.4%), psychiatric hospital records on 87 people (49.2%) and general hospital records on 142 (80.2%). The overlap between the three groups of case notes is shown (Fig2).
All the individuals except one were registered with a GP. The one person not registered had never been registered with a GP in Scotland. In seven cases the general practice case notes were missing, and two had been transferred to other areas and had not returned. When known case notes were not available, these individuals were excluded from the specific service contact rates (Table 1), because it was not possible to identify the time of their contact.
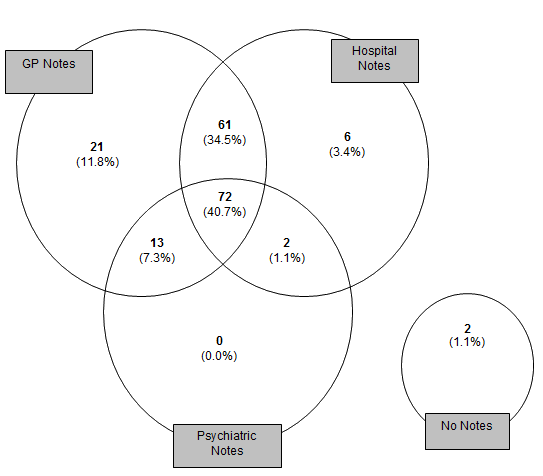
Figure 2: Case notes reviewed.
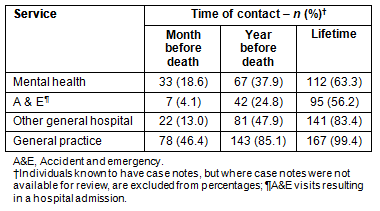
Table 1: Health service contacts in people dying by suicide
or undetermined intent Highland Council Area, 2001-2004
Service contacts
The previous service contact, as described above, for the different services is shown (Table 1). In some cases there were records in the general practice notes of specialist mental health service contact (for example, clinic letters and discharge letters) and information from these was also used in calculating total contacts. Any contacts relating only to the last episode of harm that led to death were excluded.
Contacts in the month prior to death: In total, 93 people (52.5%) had a recorded contact with an NHS Highland service in the month before their death. Of these, 32.2% (n=57) were in contact with one of the three services, 18.1% (n=32) with two and 2.3% (n=4) with all three.
General practice: The 78 people who had contact with a GP in the month before death, had a total of 159 contacts in that four week period: 41 people saw a GP once; 15 saw a GP twice; eight three times; ten four times; three five times; and one person saw a GP nine times.
Of the group of 78 people who saw a GP in the month before their death, 39 (50%) reported substance misuse or mental health problems. General practice records noted that 21 of these reported substance misuse problems, and in the majority (n=19 ), the substance being used was alcohol alone.
Twenty-four people consulted GPs with mental health related problems in the month prior to death, of whom 18 had a diagnosis of depression. Of the 24 people noted to have a mental health problem, six were also in the group noted to have a current substance misuse problem. General practitioners noted self-harm in four people in the month before their death.
General hospitals: In total, 22 people had general hospital contacts in the month before their death. One attendance followed self-poisoning, and three were for treatment of alcohol-related harm, including one in which intent to self-harm was suspected. The remaining attendances were for treatment of other physical illnesses.
Mental health services: Of the 33 people seen in the month before death, 16 had a diagnosis of mental illness, four of substance misuse problems, and six of both mental illness and substance misuse. The remainder had no specific diagnosis recorded in the month before death.
The commonest mental illness recorded was depression (n=20, 60.6%) followed by schizophrenia (3, 9.1%), personality disorder (2, 6.1%) and bipolar affective disorder (1, 3.0%). In eight instances, deliberate self-harm was recorded in records in the month prior to death.
The final mental health service contact was with a psychiatrist (n=12), a community psychiatric nurse (7), a specialist addiction nurse (3), other mental health nurses (6), a psychologist (1) and mental health support workers (2). In two further cases, a psychiatrist and mental health nurse had seen the person together at the last mental health service contact.
History of substance misuse, mental illness and deliberate self-harm
A history of deliberate self-harm, and diagnoses of mental illness and substance misuse were identified in the three types of case notes. Higher rates of self-harm, substance misuse and mental illness were recorded in the GP notes than in the other notes. Across all three sources, 68.9% had a record of mental illness, 52.5% of substance misuse, and 40.1% of self-harm.
For many people with a record of mental illness, more than one lifetime diagnosis was noted. The commonest noted lifetime diagnoses were depression (97 people, 54.8%) followed by anxiety (33, 19.6%); personality disorder (20, 11.3%); panic attacks not otherwise described (12, 6.7%); schizophrenia (10, 5.6%); paranoid psychosis (10, 5.6%) and bipolar affective disorder (9, 5.1%). Anxiety was mentioned as a symptom for 47 people (26.5%).
Of people for whom a history of substance misuse was recorded, 53 had used alcohol alone, 10 used drugs alone, and 30 had a history of both alcohol and drug misuse at some point in their lifetime.
Other risk factors
In people seen by a GP in the month before death (n=78), GPs noted potentially stressful life events for 19 people. The commonest issue recorded was relationship difficulties (9) followed by divorce or separation (3) and work stress (3). Of this group of 19, either substance misuse or mental illness was also noted for 13.
The GPs recorded physical ill-health in 16 of the people they saw in the month before death. This included many different diagnoses, including two people with cancer.
Contact in the month before death
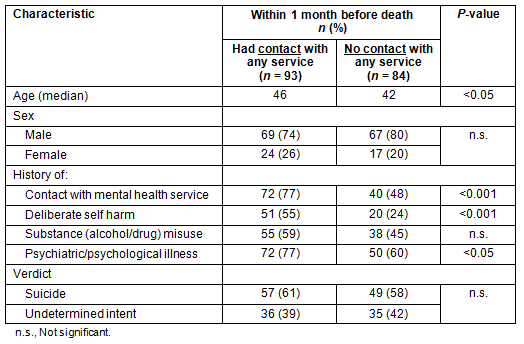
A comparison was made of people who were in recorded contact with any health service in the month before their death, and those who were not (Table 2). People not in contact with services in the month prior to death tended to be younger and to be less likely to have a known history of self-harm, psychiatric illness, or any previous mental health service contact. The death of people not in contact with services in the previous month was not significantly more likely to be recorded as being of undetermined intent.
Table 2: People dying by suicide or undetermined intent with and
without contact with any health service within 1 month before date of death
Differences by area of residence settlement type
Demography: There were no statistically significant differences among those who died by suicide in age or sex between Urban, Accessible Rural/Accessible Small Town and Remote Rural/Remote Small Town areas.
Service contact: There were no statistically significant differences in rates of GP contact in one month or one year prior to suicide. There were no significant differences among locations in lifetime or one-month general hospital contact rates.
However, people in Accessible Rural/Accessible Small Towns and Remote Rural/Remote Small Towns were less likely to have had a general hospital admission in the year before their death than those in urban areas (p<0.05).
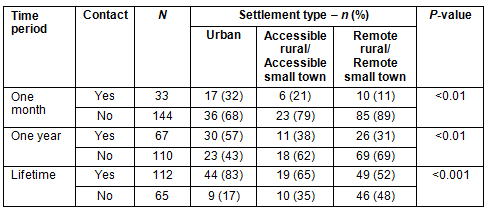
Mental health service contacts are shown (Table 3). People in urban areas were more likely to have had lifetime mental health service contacts, and contacts within one month and one year before death.
Table 3: Mental health service contact in people dying by suicide
or undetermined intent by time period of contact, and settlement type
History of illness
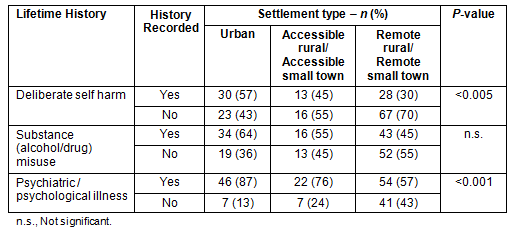
People in urban areas were significantly more likely to have had a mental illness diagnosed in their lifetime, and to have a recorded history of self-harm (Table 4). There was also a tendency towards more identification of a history of substance misuse in the urban group, although this was not statistically significant.
Table 4: Lifetime history of deliberate self-harm and mental ill-health by settlement type
Discussion
Service contacts
Over half the people who died by suicide or undetermined intent in the Highland Council area in the study period had contact with NHS services in the month before their death. The majority of these contacts were with primary care (46.4% of people), but 18.6% had been seen by specialist mental health services in the month before death. In the year before death, 85.1% had been in contact with primary care, and 37.9% with specialist mental health services.
These one-month contact figures are very similar to those reported in a review of service contact prior to suicide by Louma et al7. This study reported average contact rates in the month before death of 45% for primary care services, and 19% for specialist mental health services7. The contact figures for the year before death in the same systematic review were 77% for primary care and 32% for mental health services, suggesting slightly higher one-year contact rates in the Highland cohort than the average of the 40 studies in the meta-analysis.
Comparing people who were in service contact in Highland in the month before their death with those who were not, the non-contact group tended to be younger, and to be less likely to have a recorded history of mental illness or self-harm.
Previous mental health problems
In all, 69% of people had a history of mental illness, and 52.5% a history of substance misuse, mainly related to alcohol. The most common mental illness diagnosis was of depression. In a previous UK study, affective disorders and substance misuse problems were common in people dying by suicide after hospital discharge11. Anxiety was commonly recorded in the Highland group, and this is consistent with work suggesting that anxiety may be one of the mediating factors in whether people with mental illness and suicidal ideation go on to act on their thoughts12.
Differences by settlement type
There were no significant differences in age or sex in people dying by suicide or undetermined intent in different types of location. Despite this, there were significant differences in mental health service contact prior to death, and in having a recorded history of self-harm or mental ill-health.
The lower rates of recorded mental illness in rural areas in the present study may reflect a true difference in morbidity. Although internationally there are significant levels of mental ill-health in rural areas, rates in the UK may be lower because of lower levels of deprivation in many rural areas compared with urban areas. It is also possible, however, that the lack of specialist service contact in this group reflects under-identification of mental illness in rural areas, which could in turn relate to reduced help-seeking or to reduced service capacity.
In a recent series of WHO surveys, individuals who reported being suicidal but had not sought help were asked why they had not sought assistance. The commonest reasons were low perceived need, followed by attitudes such as a wish to deal with the problem alone. Stigma was rarely cited as a barrier to seeking care13. While this may reflect severity, it does raise the issue of whether attitudes to treatment vary in urban and rural areas.
Limitations
This descriptive study provides information on the service contacts of people dying by suicide, but not on how this compares with the general population. A previous Scottish study found that people dying by suicide were no more likely to have attended their GP in the month before their death than were age-matched controls14. The aim of this study, however, was to identify what opportunity there could be for service intervention, and whether there were differences according to location.
Psychological autopsies were not conducted and only routinely collected data were examined. It is possible, therefore, that the present work underestimates the percentage of people who had experienced mental illness, or who had self-harmed. General practitioners are able to exclude depression in people who present to them with a specificity greater than 80%, but they do not identify all cases15. A study of north-east Scotland also found that GPs tended to under-identify depression16.
In a review of psychological autopsies, Cavanagh et al reported that about 90% of people in 76 reports had a mental illness at the time of their death17 and this is considerably higher than our results from routine records alone. Some later work suggests lower rates of mental illness, however, particularly in people who do not present to services before their death18.
It is unlikely that UK service contact is markedly underestimated because, in general in the UK, almost all service contacts of patients are notified to their registered GP. Exceptions are confidential services, such as services for sexually transmitted infections, and some national screening programs.
Rural areas of the UK tend to have lower rates of mental illness, which may be related to lower rates of poverty compared with urban areas19. If the rate of mental illness in people dying by suicide in rural areas is lower than that in urban areas of Scotland, it may suggest a different combination of risk factors. It is also possible that this reflects either under-identification of illness, or a reluctance to present to services.
Implications for services
In this study, a substantial proportion of people had service contact shortly before their death by suicide. It is difficult to predict suicide, and there is often disagreement on the degree of risk present in an individual20. These findings do lend support to the Scottish strategy of training staff to recognise and respond to suicide risk, however, as many people will come in to contact with services prior to their death.
Almost half the people had no service contact in the month before their death. This indicates that continuing work on awareness of distress and signposting of help agencies is appropriate. The high prevalence of recorded mental illness emphasises the continued need for good quality, readily accessible treatment for mental illness.
Previous work in Highland has reported a higher death rate from suicide and undetermined causes than the national average, after adjusting for available measures of deprivation21. The identification of lower rates of mental health service use prior to death in rural residents is a new and striking finding. It is not clear whether this reflects a lower overall contact rate in rural areas of Scotland.
There was no difference in rates of GP contact in rural areas. The lower use of specialist mental health services may include lower perceived relevance of services, decreased recognition of illness by GPs, or decreased access to mental health services.
Hawton et al found that farmers who died by suicide often complained of physical symptoms22, but there is no apparent reason why GPs in rural areas would be less able to identify depression than their urban counterparts. Issues affecting likelihood of presentation and likelihood of referral or acceptance of referral may therefore be involved. This may be related to the likelihood of individuals identifying health and social care as appropriate responses to their problems.
In the absence of other studies, it is not possible to know if this represents a common pattern of decreased service use in rural areas. Understanding whether this is a widespread pattern, and what factors may influence it, requires exploration in future research.
Although specialist mental health services have an important role in suicide prevention in high risk groups, the great majority of people dying by suicide were not in contact with these services. As almost half of the people dying by suicide or undetermined intent had not been in contact with health services in the month before their death, population interventions are clearly important. Despite this, approximately half of the people who died had been in contact in the previous month, and so training for health service staff continues to be relevant to prevention efforts.
Acknowledgements
The project was suggested by Dr Michael Foxley. The authors are grateful to Dr Jim Douglas and Dr Alan Belbin for discussions of the role of primary care, and to Dr Eric Baijal and Dr Margaret Sommerville for supporting the work. The authors are also grateful for the cooperation and time given to this project by the hospital record managers and staff of Caithness General, Belford and Raigmore Hospitals; the contribution of the Practitioner Services Division, in particular Diane Thom and Gordon Grimmer; Michael Perera for helping in case note review, and to the Health Intelligence Team of NHS Highland, particularly Alasdair MacLennan, for analysis of the GROS data. This work was supported by NHS Highland.
References
1. Abel WD, Martin JS. Suicide: a preventable public health problem. West Indian Medical Journal 2008; 57(2): 79-80.
2. Windfuhr K, Kapur N. International Perspectives on the Epidemiology and Aetiology of Suicide and Self-Harm. In: RC O'Connor, S Platt, J Gordon (Eds); International Handbook of Suicide Prevention: Research, Policy and Practice. Chichester: Wiley-Blackwell, 2011; 27-57.
3. Hirsch JK. A review of the literature on rural suicide: risk and protective factors, incidence, and prevention. Crisis 2006 27(4): 189-199.
4. Stark C, Riordan DV. Rurality and Suicide. In: RC O'Connor, S Platt, J Gordon (Eds); International Handbook of Suicide Prevention: Research, Policy and Practice. Chichester: Wiley-Blackwell, 2011; 253-273.
5. Stark C, Riordan V, O'Connor R. A conceptual model of suicide in rural areas. Rural and Remote Health 11: 1622. (Online) 2011. Available: www.rrh.org.au (Accessed 29 May 2012).
6. Pirkis J, Burgess P. Suicide and recency of health care contacts: a systematic review. British Journal of Psychiatry 1998; 173(12): 462-474.
7. Luoma JB, Martin CE, Pearson JL. Contact with mental health and primary care providers before suicide: a review of the evidence. American Journal of Psychiatry 2002; 159(6): 909-916.
8. Scottish Executive. Choose Life: A National Strategy and Action Plan to Prevent Suicide in Scotland. Edinburgh: Scottish Executive, 2003.
9. Ramayya A, Campbell M, Callender JS. Death by suicide in Grampian 1974-1990. Health Bulletin 1996; 54(1): 37-44.
10. Nicoll KS, McGee MA, Callender JS. Death by suicide in Grampian 1991-1999: comparison with a previous study. Scottish Medical Journal 2004; 49(2): 44-47.
11. Hunt IM, Kapur N, Robinson J, Shaw J, Flynn S, Bailey H et al. Suicide within 12 months of mental health service contact in different age and diagnostic groups: National clinical survey. British Journal of Psychiatry 2006; 188: 135-142.
12. Nock MK, Hwang I, Sampson N, Kessler RC, Angermeyer M, Beautrais A et al. Cross-national analysis of the associations among mental disorders and suicidal behavior: findings from the WHO World Mental Health Surveys. PLoS Medicine 2009; 6(8): e1000-1123.
13. Bruffaerts R, Demyttenaere K, Hwang I, Chiu W, Sampson N, Kessler RC et al. Treatment of suicidal people around the world. British Journal of Psychiatry 2011; 199: 64-70.
14. Power K, Davies C, Swanson V, Gordon D, Carter H. Case-control study of GP attendance rates by suicide cases with or without a psychiatric history. British Journal of General Practice 1997; 47(417): 211-215.
15. Mitchell A, Vaze A, Rao S. Clinical diagnosis of depression in primary care: a meta-analysis. Lancet 2009; 374: 609-619.
16. Cameron IM, Lawton K, Reid I. Appropriateness of antidepressant prescribing: an observational study in a Scottish primary-care setting. British Journal of General Practice 2009; 59(566): 644-649.
17. Cavanagh JTO, Carson AJ, Sharpe M, Lawrie SM. Psychological autopsy studies of suicide: a systematic review. Psychological Medicine 2003; 33: 395-405.
18. Owens C, Booth N, Briscoe M, Lawrence C, Lloyd K. Suicide outside the care of mental health services: a case-controlled psychological autopsy study. Crisis 2003; 24(3): 113-121.
19. Paykel E, Abbott R, Jenkins R, Brugha TS, Meltzer H. Urban-rural mental health differences in Great Britain: findings fron the National Morbidity Survey. Psychological Medicine 2000; 30(2): 269-280.
20. Pearson A, Saini P, Da Cruz D, Miles C, While D, Swinson N et al. Primary care contact prior to suicide in individuals with mental illness. British Journal of General Practice 2009; 59(568): 825-832.
21. Stark C, Hopkins P, Gibbs D, Belbin A, Hay A. Population density and suicide in Scotland. Rural and Remote Health 7: 672. (Online) 2007. Available: www.rrh.org.au (Accessed 29 May 2012).
22. Hawton K, Simkin S, Malmberg A. Suicide and stress in farmers. London: The Stationery Office, 1998.


