The necessity to enrich undergraduate medical education with comprehensive exposure to general practice and community healthcare services has been unquestionable internationally for at least 40 years1-4. In the early 1970s, the medical school at the University of Minnesota had already developed a Rural Physician Associate Program (RPAP) where third-year medical students spent 9 to 12 months with a primary care physician, located in a rural Minnesota community4. Since then there have been many attempts to introduce community based programs in undergraduate medical curricula. In 2006 Hays described ten principles for implementing a new regional medical educational program, based on his experience in Australia5.
The shift to community-oriented medical education originated from acknowledging both the role of primary health care and the unique educational setting that it offers, compared with the intrinsic difficulties of the hospital based teaching6.
There is a broad spectrum of valuable knowledge, skills and attitudes to be learned by medical students in Primary Health Care (PHC)1. As a consequence the European Academy of Teachers in General Practice (EURACT) strongly suggests that medical schools across Europe include primary care rotations in their undergraduate studies7. Community based medical education implies, by definition, the need for a network of cooperating units and associated, properly trained teachers8. Collaboration and active involvement seems to be an important motivation for the engagement of primary care professionals in teaching as an everyday activity9.
Primary health care in Greece
Primary Health Care provision in Greece is defined as a three-part, public/private mix, meaning that public infrastructure (rural health centers and hospitals' outpatient clinics) coexists with Social Security's facilities (urban specialist group surgeries - 'polyclinics') and private for-profit providers (private physicians and laboratories)10.
Within this complex organizational structure, public, community based Health Centers (HCs) play a key role in the provision of PHC in the country. Health Centers were established from 1983 to 1989, as part of the introduction and implementation of the Greek National Health System (NHS). Health Centers are situated only in rural and semi-urban areas, since urban HCs (220 according to the NHS implementation plan) were never established11. The 204 currently operating HCs are tax-financed, staffed with full-time physicians and other health professionals, and offering their services to geographically defined population groups of 10 to 30,000 members10.
Introduction of Primary Health Care and General Practice attachment in the final year of undergraduate medical education
In Greece only the Medical School of the University of Crete had included PHC and GP attachment in its curriculum of undergraduate medical education12. Following the Greek experience and international trends13,14, the Aristotle University of Thessaloniki (AUTH) Medical School started, from the beginning of the new millennium, a gradual process to renovate its traditional undergraduate curriculum that was hospital based and theory overloaded. Therefore a series of pilot community based projects were implemented on a voluntary basis, both for students and teachers who evaluated these projects equally positively15.
This experience had a catalytic impact on the school's activities. In 2004, the Curriculum Committee introduced a 4 week attachment in PHC and GP in the final (6th) year of undergraduate medical studies, scheduled for implementation in the academic year 2009-2010.
This article focuses on the descriptive analysis of the process followed to establish and maintain a PHC Teaching Network. It also describes its effect on implementing community based undergraduate teaching in PHC and GP.
Establishing and maintaining the primary health care teaching network
The large number of students (approximately 350 students per academic year), and the compulsory nature of the PHC attachment, determined the need for inclusion of a large number of HCs and practices. A multi-professional teachers' network working in HCs had to be established to introduce the holistic approach and the teamwork mode of operation16,17. The encounter of the students with the community nurses, social workers, physiotherapists and administration personnel would enhance their understanding of the different roles and increase their respect for the other health professionals18. To achieve this goal a rotation program was designed that gave medical students protected time close to each health professional.
Enrollment of teachers and their engagement in the network was solely on a voluntary basis. The novelty of this procedure was that each professional was approached personally, instead through the HC that usually offers this service as a package in similar activities. Part of this approach was that teachers had the option to withdraw at any point. This self-selection procedure was adopted in order to attract health professionals committed to medical education, in a collaboration setting characterized by the school's inability to compensate the teachers.
Teachers had to be sufficient in number to accommodate the large number of students. Only a small number of students would be trained at the same period in any specific HC, thus meeting the principles of one-to-one teaching and allowing HCs to function undisturbed. The steps to build and support the network of teachers are summarized (Fig1).
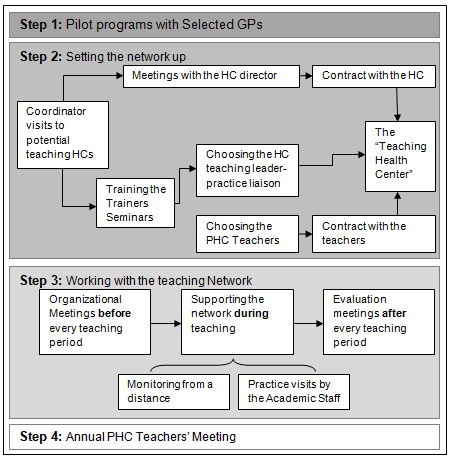
Figure 1: Steps/actions in building a primary health care teaching
network. HC, health center; PHC, primary health care.
Teacher recruitment in rural health centers
The first step towards the realization of the attachment was building up a pool of committed and properly trained teachers, capable of providing comprehensive teaching. The target population first approached during the pilot project was the Sentinel Surveillance Network in Primary Care which is coordinated by the same academic team19. General practitioners contributing to this network report, on a weekly basis, the number of patients examined with specific syndromes.
In order to recruit health professionals as potential teachers, official correspondence was exchanged between the department and the HC staff describing the school's intention to incorporate PHC teaching in its curriculum and asking for their support and participation.
Thirteen HCs expressed initial interest, and introductory meetings open to all the staff were held in each HC. Presented in these meetings were the PHC and GP attachment objectives, the teaching content, and the teachers' responsibilities. Emphasis was given to the voluntary nature of the trainers' participation.
Training the Trainers seminars
Based on the experience gained during the pilot implementation of 'Training the Trainers' seminars, five training cycles with two seminars per cycle, were completed from August 2008 to June 2010. The periodic and repetitive structure of the seminars enhanced awareness among all health professionals. The most motivated health professionals participated in the early seminars, influencing their colleagues to take part in future seminars.
The seminar syllabus aimed to inform the multi-professional teaching staff about the framework for undergraduate teaching in PHC; to present the needs of medical students and their level of competence; to introduce the principles of medical teaching; to strengthen their medical communication skills and help them identify useful teaching opportunities. The specific lectures, teaching items and discussion topics that comprised each seminar are shown (Fig2).
The seminars provided the opportunity to create a homogenous group of teachers with explicit educational aims and objectives. At the completion of the training cycle, an honorary contract with the medical school was awarded.
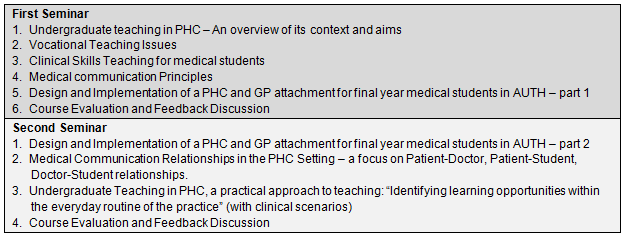
Figure 2: Topics covered in 'Training the Trainers' seminars.
AUTH, Aristotle University of Thessaloniki; PHC, primary health care.
Choosing the teaching 'leader' and the teaching 'practice liaison'
During the pilot phase, the need for a person in each HC with a profound interest in both medical education and primary health care and additional management skills became evident, especially because constant monitoring and immediate problem-solving was necessary. Although in the beginning there was one person to undertake all the responsibilities, it became obvious that separating educational and management roles was necessary; two different persons would undertake these roles, the 'teaching leader' and the 'teaching practice liaison', respectively.
Choosing a 'teaching leader' to coordinate the team of teachers was a challenge. Leaders should be role models in clinical education. Continuously aware of their role as teachers, giving emphasis to clinical competence but also professional responsibilities outside the confines of the HC, accompanied by general personal traits such as being genuinely nice, caring, warm, and committed to helping others are the main characteristics of a potential 'leader'20.
However, 'teaching practice liaison' is the title given by the practice to the person who will be responsible for contact with the academic centre and will organize the teaching in the general practice setting. The teaching practice liaison should be qualified with organizational and managerial skills, time availability, good relationships with the other teachers, good relations with the medical school, availability to participate in organizational meetings and, obviously, have a positive predisposition towards fulfilling such a part21. Even though the HC Director offered to fill this role, the teaching practice liaison could be another person on the PHC teaching staff or a person from the HC administration.
Organizational meetings before every teaching period
Holding an initial organizational meeting before the start of every teaching period helped to solve last minute issues. Teachers were given clarifications on the teaching schedule and the assessment tools. The students' personal teaching daily timetables were finalized (which student was assigned to which GP, what activities they would participate in each day).
Practice visits by the academic staff
The choice to visit every HC at least once during every teaching period proved to be a crucial activity in supporting the teachers and keeping them motivated. During these visits, the academic staff had the opportunity to encounter both students and teachers, to assess the quality of teaching directly and to give feedback to the teachers.
Evaluation meetings after every teaching period
Every teaching cycle was completed with a final evaluation meeting. All evaluation data collected and processed beforehand were presented to the participants. Our experience during the first year of implementation showed that this was the most important and constructive effort for the continuous improvement of the PHC and GP attachment.
Annual primary healthcare teachers' meeting
The annual PHC Teachers' meeting at the end of the academic year provided the opportunity for academic staff to meet PHC teachers and medical students. This was an educational meeting that enabled evaluation and critical analysis of the experience gained. Besides its value in the improvement of all activities, it appeared to be one of the most effective events in strengthening the network.
Supporting and monitoring the network from a distance
During the academic year and especially during teaching periods, an open channel of communication with teachers and students existed both by telephone and by email. This provided an opportunity to solve minor teaching issues in real time.
Teachers from different rural HCs do not have many opportunities to discuss matters with each other. A web-based discussion board would bridge the 'distance' between teachers and provide a place for educational and organizational issues to be discussed.
The initial setting and the attributes of the above described intervention reveal the importance of the undertaken challenge.
The lack of previous educational experience in PHC within the medical school and of academic culture among PHC professionals initially caused negative reactions among the academic staff and the senior healthcare staff. The straightforward and enthusiastic support from the leadership of the medical school and collaboration with the local NHS administration had a critical impact in overcoming these reactions.
The lack of compensation for teachers is certainly unusual among the many medical schools that have incorporated community teaching in their undergraduate curricula. In the UK, a GP undertaking teaching responsibilities is well remunerated, although there may be variation among medical schools22,23.
The lack of funding made the search for alternative incentives imperative24. Our PHC teaching staff most valued student feedback, routine practice visits and topic-specific training25,26.
Based on the above mentioned constraints, this initiative focused on the formulation and maintenance of a PHC teaching network, an innovative approach that produced valuable experience.
The already functioning Sentinel Surveillance Network in PHC provided an ideal opportunity to pilot the intervention and evaluate the process. Having worked together for years on a voluntary basis, the GP members of this network enthusiastically taught medical students in their practices.
The opportunity of working in collaboration with other practices is often mentioned as additional motivation for participating in the training process2,3,27. Those opportunities are provided through organizational, evaluation and continuing education meetings held by the medical school. The large number of organizational and evaluation meetings during the first year of implementation, contributed in making small but important adjustments through the academic year and, enhanced the team spirit and effectiveness of the teaching network.
The final annual meeting gave the opportunity to academic staff to present the positive results of the first implementation of the PHC and GP attachment. The PHC teachers presented their approach and experience and the medical students presented selected parts from their portfolios and discussed their experience.
In contrast with common practice where undergraduate medical teaching is undertaken mainly by GPs28,29, we expect our approach to give the opportunity to students to encounter and appreciate the role of all the health professionals in PHC, which can be further investigated when the course evaluation is completed.
In conclusion, introducing community teaching as a component of a Greek undergraduate medical curriculum demands extensive planning and long-term preparation. Pilot programs give the opportunity to create a teaching schedule that fits both the specific characteristics of a given medical school as well as the PHC units that will train the students. The large number of students, in conjunction with the voluntary nature of teaching, requires the involvement of many rural PHC units and the maximum engagement of PHC team members. Creating a self-selected and committed multi-professional teaching network proved to be a crucial step towards the success of the PHC and GP attachment.
Acknowledgements
The authors express their gratitude to Anne Stephenson, Senior Clinical Lecturer, Senior Clinical Advisor and Director of Community Education, King's Undergraduate Medical Education in the Community Team (KUMEC) and to Ron Bailey, Teacher Development Lead in KUMEC - (Department of Primary Care and Public Health Sciences, King's College London School of Medicine) for their valuable input during the editing of the final version of this manuscript.
References
1. General Medical Council. Tomorrow's Doctors. Outcomes and standards for undergraduate medical education. London: General Medical Council, 2009.
2. Davis W, White B. Introduction. In: W Davis, B Jolly, G Page, A Rothman, B White B (Eds); Moving medical education from the hospital to the community. Report of the Seventh Cambridge Conference on Medical Education. Ann Arbor, MI: University of Michigan Medical School, 1995.
3. Oswald N. Where should we train doctors in the future? BMJ 1991; 303: 71.
4. Verby J, Lenarz G, Garrard J. Evaluation of an alternative clinical experience: the Minnesota Rural Physician Associate Program. Journal of Medical Education 1974; 49: 696-698.
5. Hays R. Guiding principles for successful innovation in regional medical education development. Rural Remote Health 6: 516. (Online) 2006. Available: http://www.rrh.org.au/journal/article/516 (Accessed 9 July 2012).
6. Oswald N. Why not base clinical education in general practice? Lancet 1989; 43: 148-149.
7. Tandeter H, Carelli F, Timonen M, Javashvili G, Basak O, Wilm S et al. A 'minimal core curriculum' for Family Medicine in undergraduate medical education: a European Delphi survey among EURACT representatives. European Journal of General Practice 2011; 17: 217-220.
8. Leeuwenhorst Working Party. Second European conference on the teaching of general practice. The general practitioner in Europe. Medical Education 1976; 10: 235-236.
9. Heidenreich R, Chenot JF, Kochen MM, Himmel W. Teaching in practice: a survey of a general practice teaching network. Medical Teacher 2006; 28: 288-291.
10. Ministry of Health and Welfare. Health, Health Care and Welfare in Greece. Athens: Ministry of Health and Welfare, 2003; 42-49.
11. Tragakes E, Polyzos N. Health Care Systems in Transition - Greece. Copenhagen: World Health Organisation Regional Office for Europe, 1996.
12. University of Crete. Clinic of Social and Family Medicine, Faculty of Medicine, University of Crete. (Online) 2012. Available: http://www.fammed.uoc.gr/Joomla/ (Assessed 12 October 2012).
13. Association of University Teachers of General Practice. Undergraduate Medical Education in General Practice, Occasional Paper 28. London: Royal College of General Practitioners, 1984.
14. General Medical Council. Tomorrow's Doctors. Recommendations on Undergraduate Medical Curriculum. London: General Medical Council, 1993.
15. Panagopoulou E, Kavaka N, Giannakopoulos S, Aslanoglou T, Smyrnakis E, Kiranou M et al. Integrating communication, clinical and research skills in medical education: The Daisy Project. Education for Health 2006; 19: 106-110.
16. World Health Organisation. The World Health Report 2006 - Working together for health. Geneva: World Health Organisation, 2006.
17. Riesenberg LA, Little BW, Wright V. Nonphysician medical educators: a literature review and job description resource. Academic Medicine 2009; 84:1078-1088.
18. Humphris D. Multiprofessional working, interprofessional learning and primary care: a way forward? Contemporary Nurse 2007; 26: 48-55.
19. Gavana M. Planning, implementing and assessing a sentinel surveillance network in primary health care. [PhD Thesis] Thessaloniki: Aristotle University of Thessaloniki, Medical School. Available: http://invenio.lib.auth.gr/record/113495/files/mgavana phd.pdf (Assessed 29 August 2011).
20. Althouse L, Stritter F, Steiner B. Attitudes and approaches of influential role models in clinical education. Advances in Health Sciences Education 1999; 4: 111-122.
21. King's Undergraduate Medical Education in the Community (KUMEC). The KUMEC Practice-Liaison Booklet. King's College London. (Online) 2011. Available: http://www.kcl.ac.uk/medicine/research/divisions/hscr/study/undergradops/KUMEC/Teachers/practice-Liaison-Booklet.pdf (Assessed 12 October 2012).
22. Gray J, Fine B. General practitioner teaching in the community: a study of their teaching experience and interest in undergraduate teaching in the future. British Journal of General Practice 1997; 47: 623-626.
23. Wilson A, Fraser R, McKinley RK, Preston-Whyte E, Wynn A. Undergraduate teaching in the community: Can general practice deliver? British Journal of General Practice 1996; 46: 457-460.
24. Page S, Birden H. Twelve Tips on Rural Medical Placements: What has worked to make them successful. Medical Teacher 2008; 30: 592-596.
25. Cook V, Nicholson S. How can GP teachers be supported to make good teaching even better? Education for Primary Care 2006; 17: 17-23.
26. Smyrnakis E, Panos A, Stardelli T, Chainoglou A, Gavana M, Kondylis E et al. Introducing Primary Health Care clerkship in a hospital centred curriculum. In: Proceedings, 40th Annual Scientific Meeting of the Society for Academic Primary Care; 6-8 July 2011; Bristol, UK. SAPC, 2011.
27. Howe A. Teaching in practice: a qualitative factor analysis of community-based teaching. Medical Education 2000; 34: 762-768.
28. Stephenson A, Bailey R. Community Teaching Handbook for practices and Teachers 2010-2011. London: Department of General practice and Primary Care, King's College London, 2010.
29. Teaching Opportunities for GPs. UCL Medical School, Community Based teaching 2011-2012. Research Department of primary Care and Population Health. (Online) 2011. Available: http://www.ucl.ac.uk/pcph/undergrad/cbt/tabbed-box/teaching-opps-booklet (Accessed 5 March 2013).



