The quality, composition, and distribution of a health workforce is widely recognized as a crucial determinant of health system performance1. Committed and qualified health workers are needed to deliver services to meet the needs of a community2. The most challenging element of health workforce provision internationally is ensuring that rural and remote populations have access to trained health workers3, and Indonesia is no exception, especially in regard to meeting the health needs of those who live in remote and very remote areas.
In 2006, WHO reported that Indonesia was among 57 countries suffering a critical shortage of health workers (doctors, nurses and midwives), with a health workforce ratio of less than 2.5 per 1000 population1. A study conducted by Indonesia's Ministry of Health (MOH) in 2006 found that more than 50% of community health centers in remote areas were without medical doctors, compared with approximately 10% in non-remote areas. This pattern is similar for other health personnel types4.
Indonesia's vast size and difficult geography presents a tremendous challenge to those concerned with health service delivery. For instance, it is difficult to place doctors on remote islands or in mountainous or forest locations5, and rural and remote areas suffer from a shortage of all essential health workers (ie doctors, midwives, nurses, nutritionists and sanitarians [tertiary educated environmental health officers]). Of those health workers willing to serve in such areas, generally their period of service is very short term. The reasons for this include communication difficulties, lack of basic and social facilities, low salary, low or no compensation, high living costs, lack of security and unclear career options6.
According to Indonesia's Ministry of Health Decree No. 949 of 2007, there are two degrees of remoteness, namely remote areas and very remote areas, and this division is based on geographical position, access to transportation and the social economy (Table 1)7.
Table 1: Differences between remote and very remote areas7
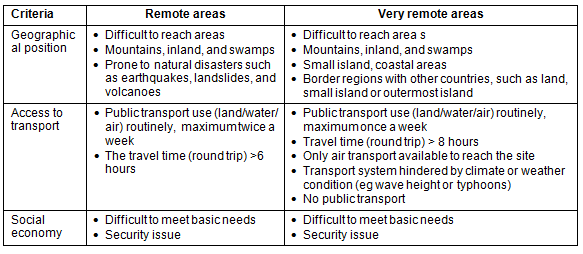
The Indonesian Government has implemented policies to support the recruitment and deployment health workers in rural and remote. These include compulsory service, contracted staff and Special Assignment.
Compulsory service
According to Law No. 8 of 1961, all university graduates including health workers are obliged to serve at least 3 years in government facilities8. This was followed by Government Regulation No. 1 of 1988, which required doctors and dentists to work in private or government health facilities, a university or the military for a minimum of 5 years to complete their compulsory service8. President Instruction No. 5 of 1974 supported this policy by employing health workers to work compulsorily as civil servants9.
The MOH was given the authority to determine health workers' placement location and this program was controversial because it was considered an infringement of human rights as it offered an unattractive income, unattractive location and long waiting times for deployment, especially to more favored areas10, for example locations where remuneration was higher and there was a lower level of civil conflict. In addition, the number of civil service postings, popular with doctors and dentists were limited, and there was a long waiting time for placement.
With the proclamation of Law No. 13 of 2003, compulsory service no longer applied11. This meant greater freedom for health professionals to choose their career or work location, and few are willing to serve in remote districts. As a result, many less favored districts now suffer shortages of certain health professionals.
Contracted staff
The ability of the government to recruit health workers as civil servants was limited, and an attempt to redress this resulted in President Decree No. 37 of 1991, which marked the implementation of a new policy 'Contracted staff' or Pegawai Tidak Tetap (PTT)12. Under this policy, doctors and dentists were obliged to work as temporary staff on a contract basis for a certain period. Coinciding with this was a similar scheme where the government assigned midwives to rural areas through the Village Midwife Program10.
Under the PTT policy, doctors, dentist and midwives served for a minimum 6 months and up to 3 years, depending on the location criteria. The contract could be renewed twice13. Under this program, PTTs who served in remote areas were rewarded with increased opportunities to be employed as a civil servant (PNS) and monetary incentives according to their length of service. For example, service in certain remote locations or disaster areas entitled the PTT who completes 1 year of service to be considered to have given 2 years. However doctors could terminate their contract early and many health centers in remote areas still lacked doctors4.
To motivate health workers to be deployed to remote and very remote areas willingly, since 2006 the MOH has implemented new policies for PTTs (Table 2)13:
- Offer vacancies only in remote and very remote posts.
- Shorten the period of service from 2 to 1 year for remote areas and 6 months for very remote areas.
- Increase financial incentives.
These policies have been applied to all PTT workers in very remote areas, regardless of the level of geographic barriers, availability of support facilities and other factors.
A medical specialist who serves in a very remote area earns 10,350,000 IDR or approximately 1150 USD per month (~1 USD = 9000 IDR; Table 2). A study by the MoH Indonesia in 2007 found the incentive package was moderately satisfactory to PTTs; however, even this did not have a significant impact on their willingness to stay in very remote locations14.
Table 2: Monthly salary and incentive for contracted staff15
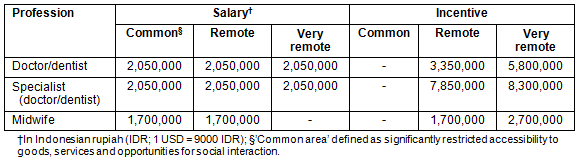
Data from the MOH in 2005 showed that 536 doctors applied the 55 posts in the West Java Province, resulting in a waiting lists of 481 doctors16.
In 2007, mandatory service for PTTs was formally changed by the MOH to voluntary service10. This meant that doctors could either join the service as a PTT or choose to have a career in the private sector. However the PTT scheme was still popular among new graduates and despite the voluntary nature of the program, there were still long waiting lists of doctors who had applied for particularly remote and very remote posts. By 2011, 32 978 health workers had actively served as contracted staff (Table 3).
Table 3: Contracted staff year 201012
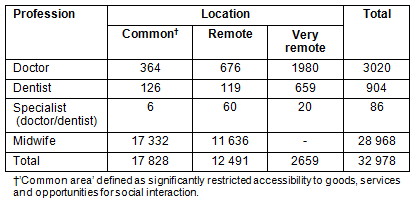
Very remote areas are more popular than remote areas with doctors and dentists due to differing incentives and policies according to the district (Table 2). This has improved the availability of health workers in the health centers and villages particularly in remote areas. In 2010, only 17% of the 9000 very remote health centers were without a doctor, compared with 30% of 8000 health centers in 200617.
However this policy has not addressed retention in these areas because the length of service is relatively short. As there is no bonding to retain doctors in remote areas, they naturally move to large urban areas for economic reasons17.
Special Assignment
This need for health workforce in remote and very remote areas was a priority for the Indonesia Government's 2009 National Summit and for the MOH '100 Days' program, the Special Assignment Program for Strategic Health Workers (in addition to the PTT scheme). Those strategic health workers included nurses, sanitarians, nutritionists and other health cadres. The first phase was to ensure the availability of 300 health workers to health centers located in undesirable locations such as remote, underserved, borderlands, areas of conflict and disaster areas18.
Health workers who join the Special Assignment Program receive travel expenses and additional incentives19 for a period of service of a minimum of 3 months and up to 1 year, renewable. The size of the incentive depends on remoteness or region (region I or region II). For instance, for service in region I the amount is 2,700,000 IDR per month and 1,700,000 IDR for region II18. The incentives were legislated in the Ministry of Health Decree No. 1235 of 200720 and Ministry of Health Decree No. 156 of 201018.
This program is expected to increase the retention of health workers, because recruitment is conducted at the local level and priority is given to local health workers. However, to increase the attractiveness of the program, opportunities for civil service employment after serving in a Special Assignment area should be embedded in the program. And due to the short term of nature of the contracts (Table 4), recruitment should be continuous to overcome the rapid change in serving health workers.
Table 4: Summary of health workers recruitment and deployment in Indonesia year 201015,16

In conclusion, various policy options have succeeded in improving an unbalanced distribution and shortage of health workers in Indonesia's remote and very remote areas. Most of the targeted programs used financial incentives as the main intervention; however, non-financial interventions should also be included in one comprehensive incentive package to retain these health workers, such as the provision of continuing professional education and eventual opportunities for civil service employment. In addition, as has been found in many other countries, the recruitment of health workers of rural background is likely to increase willingness to serve in remote and very remote areas. Greater responsibility granted to local governments in a decentralized context would seem essential.
Finally, evidence-based data and other detailed information relating to the health workforce is urgently required, as is further research into the impact of Indonesian Government policies on improving equity of access to health services and health care in rural, remote and very remote Indonesia.
References
1. WHO. World health report 2006. Geneva: WHO, 2006.
2. WHO. Joint WHO/AAAH Conference on getting committed health workers to underserved areas: a challenge for health systems. Geneva: WHO, 2009.
3. WHO. Increasing access to health workers in remote and rural areas through improved retention. Geneva: WHO, 2010.
4. Ministry of Health of Indonesia. Identification on health personnel need for health facilities in the remote, borderline, social conflict and disaster areas and other less favorite areas. Jakarta: MoH, 2006.
5. Chomitz KM, Gunawan S, Azrul A, Ismail N, Widiyarti. What do doctors want? developing incentives for doctors to serve in Indonesia. (Online) 1998. Available: http://econ.worldbank.org/external/default/main?menuPK=64166093&pagePK=64165259&piPK=64165421&theSitePK=469382&repNo=WPS1888 (Accessed 20 March 2011).
6. Egger D, Lipson D, Adams C. HRH: Achieving the right balance: the role of policy making processes in managing HRH problems. (Online) 2011. Available: http://www.who.int/hrh/documents/en/right_balance.pdf (Accessed 2 February 2011).
7. Ministry of Health Indonesia. Decree no. 949 of 2007. (Online) 2007. Available: www.ropeg-depkes.or.id/news/2008/desember/new_a1.pdf (Accessed 20 March 2011).
8. Government of Indonesia. Law No. 8 of 1961 and Government Regulation No. 1 of 1988. Jakarta: Government of Indonesia, 1961, 1988.
9. Government of Indonesia. President Instruction No. 5 of 1974. (Online) 1974. Available: http://dapp.bappenas.go.id/website/peraturan/view.php?id=9321&file=pdf (Accessed 19 April 2012)
10. World Bank. Indonesia's doctors, midwives and nurses; current stock, increasing needs, future challenges and options. Jakarta: World Bank, 2009.
11. Government of Indonesia. Law No. 13 of 2003. (Online) 2003. Available: www.bpkp.go.id/uu/filedownload/2/40/258.bpkp (Accessed 19 April 2012)
12. Kurniati A, Efendi F. Human Resources for Health in Indonesia. Jakarta: Salemba Medika, 2012.
13. Kurniati A, Efendi F. Viewing decentralization as an opportunity: in improving. availability of health workers in underserved areas. (Online) 2011. Available: www.aaahrh.org/4th_conf_2009/Kurniati_INDONESIA.pdf (Accessed 20 March 2011).
14. Kurniati A. Incentives for medical workers and midwives in very remote areas an experience from Indonesia. In: Proceedings, 2nd Conference of Asia Pacific Action Alliance on HRH; 12-14 October 2007; Beijing, China; 2007.
15. Sedyaningsih ER. Strategi dan Kebijakan Kementerian Kesehatan Menuju Universal Coverage dan Pemenuhan Serta Pemerataan Fasilitas Tenaga Kesehatan. (Online) 2011. Available: http://www.kebijakankesehatanindonesia.net/sites/default/files/images/Paper-Bu-Menkes.pdf (Accessed 20 March 2011).
16. BPPSDMK. Deployment of Health Workers Through Special Assignment Program. (Online) 2010. Available: http://www.slideshare.net/nersbaspal/rengun-dtpk-2010plus1 (Accessed 19 April 2012).
17. Kompas. 1600 Health Centers Unattended by Doctors. (Online) 2010. Available: http://health.kompas.com/read/2010/10/05/06535159/1.600.Puskesmas.Indonesia.Tanpa.Dokter (Accessed 16 April 2012).
18. Ministry of Health Indonesia. Decree no. 156 of 2010. (Online) 2010. Available: http://www.ighealth.org/id/regulation/downloadfile/35/Kepmenkes-156-Tahun-2010 (Accessed 19 April 2012).
19. Ministry of Health Indonesia. Waiting List of the PTT Program. (Online) 2012. Available: http://www.depkes.go.id/index.php/berita/pengumuman/723-daftar-antrian-dokter-ptt-dan-dokter-gigi-ptt.html (Accessed 16 April 2012).
20. Ministry of Health Indonesia. Decree No. 1235 of 2007. (Online) 2007. Available: http://perpustakaan.depkes.go.id:8180/bitstream/123456789/611/3/KMK1235-1207-G.pdf (Accessed 19 April 2012).
