Local health governance in Nepal
Good governance is defined as the traditions and institutions by which authority in a country is exercised for the common good1,2. The building blocks of good local governance include citizen participation, partnerships among key local-level actors, capacity of local actors across all sectors, institutions of accountability, and a pro-poor orientation3,4. In this article, good local health governance is confined to the concept that the peripheral public health facilities are managed in participatory and accountable ways through active engagement and empowerment of the local Health Facility Operation and Management Committee (HFOMC).
Nepal is divided into five development regions, 14 zones and 75 districts, with each district further divided into village development committees and municipalities5. Nepal has a two-tier system of local governance, with village development committees and municipalities as the lower tier and district development committees as the higher tier6. The Nepalese primary healthcare system operates through the primary healthcare centres, health posts and the sub-health posts, which are located at peripheral, below district levels, with the aim to serve the mostly rural population. The National Health Policy ensures that there is at least one such institution in each village development committee or municipality7,8.
Despite having a well-structured network of service delivery, the health system faces several challenges, including absence of good governance in the health facilities, characterized by understaffing and absenteeism; poor supervision and monitoring; poor community participation; lack of transparency, ownership and accountability; and a mismatch between plans and actual health needs9,10.
To address these health system issues, the Ministry of Health and Population of Nepal decentralized health services in 2003 by handing over 1433 peripheral health facilities in 28 districts to HFOMCs, as one of the overarching sector reform strategies and a key approach to achieving the Millennium Development Goals11,12. The main purpose of this initiative is to make these local committees responsible for managing the affairs of the health facilities13.
Health Facility Operation and Management Committee and its capacity
Each HFOMC consists of 9 to 13 representatives from the village development committee/municipality. In order to foster social inclusion and ensure everyone has a voice in the health facility management, membership includes the health facility in-charge, the village development committee chairperson and elected members, school teachers, female community health volunteers, dalit (disadvantaged caste) and women members. Ideally, committee members are selected following a public meeting. Some are selected by virtue of their posts, and the rest of the members are nominated by the other members of the committee at the public meeting12-14.
By policy, HFOMCs, which work as local health bodies, are supposed to manage funds, human resources, and health programs locally. It is expected that once the HFOMCs assume full ownership of local health facility management, the committees would meet at their health facilities at least once a month to discuss health issues brought by different community groups, identify local health problems, prioritize them, develop and implement action plans and mobilize local resources. In addition, they prepare annual and periodic health plans, supervise and monitor health facilities, and review the progress of health facilities periodically. The main source of funding for HFOMCs is a fixed amount of budget, coming either directly through the District Public Health Offices to health facilities or through the District Development Fund of the District Development Committees to village development committees and then to the HFOMCs. HFOMCs also get funds from their village development committees/municipality, non-governmental organizations and the local community12.
However, the handing-over of the management and operation of local health facilities to HFOMCs was not matched by an equivalent increase in the managerial capacity of their members, and hence potentially there were no major changes in service delivery and governance.
Very little is known about the functionality of such committees; optimal capacity building models for improving their effectiveness; and their contribution to local health governance, either in Nepal or elsewhere. The objective of this article, therefore, was to discuss an approach and lessons learned on how good local governance at peripheral health facilities of Nepal can be strengthened through the active engagement and capacity building of HFOMCs.
The Nepal Family Health Program II, a bilateral project funded by the United States Agency for International Development, shared the responsibility of capacity building of these HFOMCs together with the Government through implementation of the Health Facility Management Strengthening Program in a phased manner in 13 districts in 2008. These districts were a mix of those with devolved authority (handed-over) and those where this process had not yet begun.
Health Facility Management Strengthening Program approach
The program aimed to foster good governance in health facilities by empowering and building the capacity of the HFOMCs, through training and monitoring/follow up. Building on the lessons from the past experiences of different organizations14,15, the program approach focused on capacity building of HFOMCs as a continuous process.
Phase I: In 2008, the program was implemented in 55 of the 160 health facilities of 4 districts. The districts ranked low in the Human Development Index, had a high proportion of marginalized populations, and had health facilities that had been handed over to the HFOMCs. It was designed as a two-year project that involved an initial self-assessment of the capacity of the HFOMC, followed by three days of basic training, and then two-day and one-day review workshops. A standard training package endorsed by the Government of Nepal was used to facilitate the training and workshops. Its major contents included purpose and process of decentralization, roles and responsibilities of HFOMCs, right to health, social audit, health facilities management, supervision and monitoring, resource mobilization, social inclusion in health, and identification and prioritization of local health needs using the participatory planning process. Promotional and advocacy activities were also carried out at the community and district levels to build trust and support among community members towards HFOMCs and health facilities15.
The HFOMCs receive technical support visits from the project staff. This is a monitoring and support method developed to improve the performance of HFOMCs. The visits involve assessment of HFOMC functioning, collection of relevant information, and the provision of necessary support to the HFOMCs. An observation cum record review tool was developed and used to assess and collect data by observing HFOMC meetings and reviewing their meeting minutes and health facility service data. All HFOMCs received the visits on a monthly basis from nine project staff.
Phase II: In 2010, after favourable results demonstrated through the visits, the scale of the program was expanded throughout the four districts and in an additional nine districts. In consequence, the program covered all the 612 health facilities in 13 districts, including seven non-handed over districts. Since health sector decentralization was yet to go into full swing, the structure, function and authority of both handed-over and non handed-over districts were almost the same. The interventions were modified in such a way that all training and review workshops were completed within the first year (Fig1).
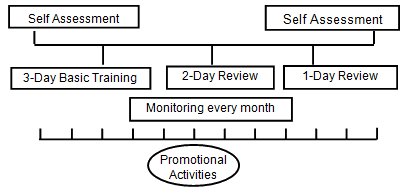
Figure 1: The Health Facility Management Strengthening Program approach.
Lessons learned from the 55 health facilities helped in strengthening the monitoring system in phase II. New indicators were added to the existing tool to measure good health governance. A new interview tool was developed to assess knowledge and empowerment of members including local resource mobilization. Staffing was re-structured, with one officer deployed to look after two districts and a locally hired assistant to follow up the program in each district. With this staffing structure the HFOMCs received fewer visits from the project staff than before, but each HFOMC received a visit at 3-4 month intervals.
Methods
This article analyses the outcomes of the program using monitoring data collected from 2605 visits to HFOMCs between July 2008 and October 2011. In phase I, baseline information was collected from 50 of the 55 HFOMCs. Throughout the period, 2605 observation/record reviews were completed and used for the analysis. Additionally, in phase II, 2924 HFOMC members were also interviewed during the monitoring visits. Data collected between July 2010 and October 2010 was not used for analysis, as the revised database was still being tested.
Monitoring tools and indicators were field tested before finalization. In this article three-year trend analysis is presented where data was available starting from phase I and compared with baseline if available. For the new indicators added in phase II, quarterly trend analysis of one-year data is presented.
The data from the monitoring tools were recorded in an electronic summary sheet developed in Microsoft Excel for each project district every month and then submitted to the regional office. There the data from the summary sheets were aggregated and submitted to the project office every month. The database has a built-in mechanism to check data entry errors. A data quality assessment carried out by the funding agency in 2010 showed that quality of the monitoring data and indicators was within acceptable limits. As one of the projects implemented was a bilateral program of Ministry of Health and Population and United States Agency for International Development, ethical clearance for the collection of monitoring data was not required. While collecting data during monitoring visits, verbal consent from HFOMC members was sought, and explanations about how the data collected might be used in the future was given. The first author was the overall in-charge of the Health Facility Management Strengthening Program providing technical oversight to the project while the second author was responsible for project monitoring.
The program defined 'governance' as the ability of the HFOMCs to ensure the following four outcomes:
- Community engagement in health facility management
- Mobilization of local resources by HFOMCs
- Increased responsiveness and accountability towards the community
- Inclusive health services.
Community engagement in health facility management
Community engagement in health facility management was measured by the following three indicators.
Effective HFOMC meetings: Effective meetings was defined as the percentage of HFOMCs that had held meetings in the previous month. The meeting needs to have a participation of 51% of HFOMC members with at least a dalit and woman member, a prepared action plan, and shared responsibilities among members. The regularity and effectiveness of meetings was considered an important variable to measure community engagement. In the baseline, only 38% of the HFOMCs had regular meetings. This value increased to 86% in the following years. The number of effective meetings also improved markedly from zero in the baseline to 57% in the third year (Fig2).
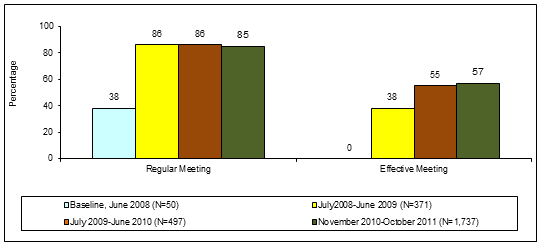
Figure 2: Regular and effective Health Facility Operation and Management Committee meetings.
Inclusion of dalit/women members in HFOMC decision-making: Inclusion of decision-making was defined as the percentage of HFOMC meetings at which at least one dalit or woman member raised issues. While only 30% of women or dalit members raised issues in year one, the proportion increased to 39% and 61% in the following years. However, challenges still remained for the effective participation of these groups due to educational, economic and cultural barriers.
Implementation of action plan: Action plan implementation was defined as the percentage of HFOMCs implementing at least one of the action plan activities of the previous month. In the first year, half of the HFOMCs implemented at least one activity of the previous month's action plan; this percentage was maintained above 60% in the succeeding years.
Mobilization of local resources by HFOMCs
This is defined as the percentage of HFOMCs receiving any kind of support from the village development committee and other organizations in the last 12 months. There was considerable improvement in mobilization of local resources, such as receiving cash or in-kind support from the village development committees and other organizations, as the program matured (Fig3).
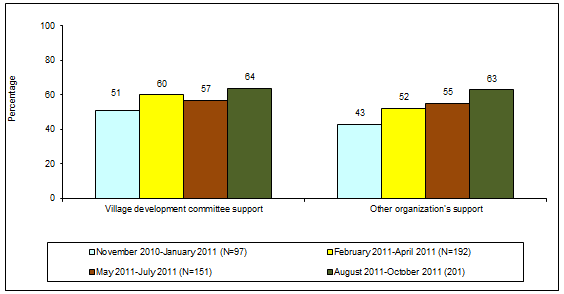
Figure 3: Local resource mobilization by Health Facility Operation and Management Committees.
Increased responsiveness and accountability towards the community
Increased responsiveness and accountability towards the community was measured by the following three indicators.
Routine service delivery & presence of service provider: Routine service delivery & presence of service provider was defined as the percentage of days on which the health facility was open in the previous month, and the availability of at least one technical staff member on the day of the visit. One of the major responsibilities of the HFOMCs is to hold health facility staff accountable to ensure that people are getting health services without interruption due to health worker absenteeism or health facility closure. There was improvement in the proportion of health facilities that were open during work days except in the last quarter (Fig4).There was universal presence of a technical staff member on the day of the visit.
Monitoring of Primary Health Care Out-Reach Clinic, immunization clinic and health facility by HFOMC members in last month: Monitoring is an important activity that ultimately fosters community accountability. The percentage of the clinics and health facilities monitored by HFOMC members was low in the first quarter, but increased slowly and was almost 50% in the last quarter (Fig5).
Display of citizen charter: The percentage of health facilities that displayed the citizen charter in a visible place on the day of visit defined this indicator. In the first quarter it was reported that 83% of the health facilities displayed the charter, and this rose to 94% in the last quarter.
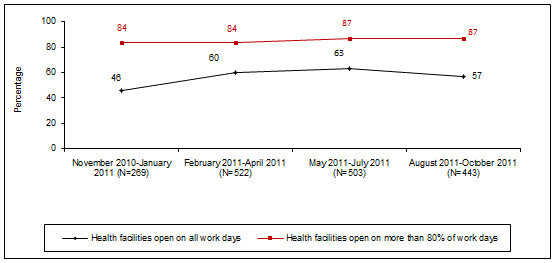
Figure 4: Proportion of health facilities open on all work days and on >80% of work days in the previous month.
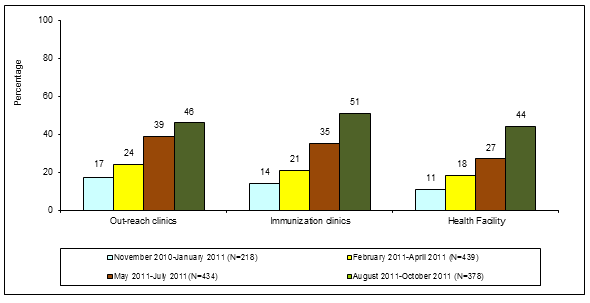
Figure 5: Proportion of out-reach clinics, immunization clinics
and health facilities monitored by Health Facility Operation and Management Committee members.
Inclusive health services
Inclusive health services were measured by the following two indicators.
Identification of excluded groups and implementation of special program: Identification of excluded groups and implementation of special program was defined as the percentage of HFOMCs that assessed the health needs of marginalized communities and implemented at least one activity to address those needs. Such assessment increased over time and was reported to be 62% in the last quarter. Also, of those HFOMCs that conducted such assessment, the proportion that implemented their action plans also increased (Fig6).
Service utilization by dalits: This usage was defined as the ratio of dalit proportion among health facility clients versus dalit proportion in the catchment population. This ratio was 1.41 in the first year, increased to 1.44 in the second year and reached 1.47 during the third year.
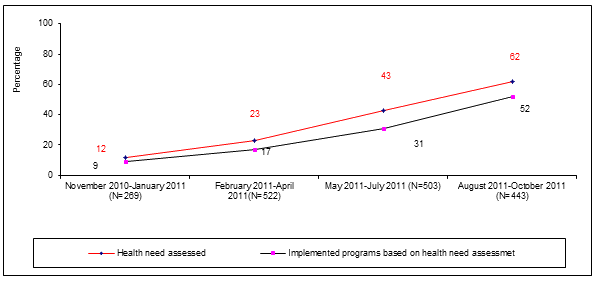
Figure 6: Proportion of Health Facility Operation and Management
Committee that assessed health needs and implemented programs.
Limitations
Although the project succeeded in developing reliable indicators to measure governance to a certain extent, it could not cover all the dimensions, owing to the multi-dimensional nature of governance. Similarly, not all indicators were available in the baseline information. Since this article used routine monitoring data to demonstrate the effectiveness of the program, a more rigorous evaluation is required as a next step in order for the model to be more widely adapted.
Future directions
The Health Facility Management Strengthening Program highlighted the importance of continuous engagement rather than a one-time event to strengthen the capacity of HFOMCs. A sound capacity building was very important for its success. The function of HFOMCs was largely determined by the right selection procedure of members through public meetings; the amount of support provided by health facility staff, district authorities and the wider community; and the sense of volunteerism and team spirit among the members. Education and livelihood empowerment were both imperative to ensure effective participation of dalit/women members in decision-making.
To get the desired results in the districts where decentralization of human resources and funds management is yet to be completed13, capacity building of and giving authority to HFOMCs should happen in a parallel manner. Moreover, training should be recognized as only a component of overall capacity building of HFOMC, and thus capacity strengthening at the organizational and system levels, including resources, policies and structures, is also necessary10.
Conclusion
In conclusion, local health governance in peripheral health facilities can be fostered with active engagement of HFOMCs. Capacity building of HFOMCs based on the Health Facility Management Strengthening Program approach is instrumental to increase community engagement, improve mobilization of local resources, and ensure accountable and inclusive health services from the health facilities. The success will be sustained if this approach is institutionalized.
Acknowledgements
The program described in this article was supported under the NFHP-II program made possible by the generous support of the American people through the United States Agency for International Development (USAID), and implemented by JSI Research and Training Institute Inc. The authors are grateful to Dr Robin Houston, Ms Shriya Pant and Ms Khushbu Agrawal for their support for language editing.
References
1. Lewis M, Pettersson G. Governance in Health Care Delivery: Raising Performance. (Online) 2009. Available: www-wds.worldbank.org/external/default/WDSContentServer/IW3P/IB/2009/10/13/000158349_20091013151915/Rendered/PDF/WPS5074.pdf (Accessed 20 August 2012).
2. The World Bank. What is governance? (Online) 2011. Available: http://go.worldbank.org/G2CHLXX0Q0 (Accessed 20 August 2012).
3. UNDP. Local governance, human rights based approach and gender mainstreaming in the context of Europe and the CIS. Available: http://hrba.undp.sk/index.php/introduction/local-governance-human-rights-based-approach-and-gender-mainstreaming-in-the-context-of-europe-and-the-cis/182-local-governance (Accessed 19 January 2012).
4. UNESCAP. What is good governance? (Online) 2012. Available: www.unescap.org/pdd/prs/ProjectActivities/Ongoing/gg/governance.asp (Accessed 19 January 2012).
5. Ministry of Health and Population, New ERA, Macro International Inc. Nepal Demographic and Health Survey. Kathmandu: New ERA, 2006.
6. Fried-Ebert-Stiftung. Local governance. (Online) 2011. Available: www.nepaldemocracy.org/institutions/local_governance.htm (Accessed 8 June 2012).
7. Shankar R, Kumar P, Rana M, Dubey A, Shenoy N. A comparative study of drug utilisation at different levels of the primary health care system in Kaski district, Western Nepal. Journal of the New Zealand Medical Association 2001; 116(1182): 1-8.
8. Department of Health Services. Annual Report, 2006/2007. Kathmandu: Ministry of Health and Population, 2007.
9. Ailuogwemhe J, Rajbhandari R, Eirini I, Villar M, Dieterich M. Tackling Shortages of Health Care Workers in Rural Nepal: 'Train to Retain'. (Online) 2005. Available: http://nsi.edu.np/?site=yes (Accessed 18 January 2012).
10. Collins C, Omar M, Adhikari D, Emmel N, Dhakal MR, Thapa D. Developing Health Sector Decentralization in Nepal: Collaborative Policy Development. Kathmandu: British Council, 2003.
11. Ministry of Health and Population. Nepal Health Sector Program Implementation Plan II, 2010-2015. Kathmandu: MOHP, 2010.
12. Ministry of Health and Population, National Health Training Centre. Guideline for Handover and Operation of Local Health Facility. Kathmandu: MOHP, 2003.
13. Gurung G. Health sector decentralization in limbo: what are the bottlenecks? Nepal Medical College Journal 2011; 13(2): 138-141.
14. Gurung G. Capacity building is not an event but a process: lesson from health sector decentralization of Nepal. Nepal Medical College Journal 2009; 11(3): 205-206.
15. Nepal Family Health Program. Health Facility Management Strengthening Program. (Online) 2009. Available: http://nfhp.jsi.com/Res/Docs/TechBrief17-HFMSP_000.pdf (Accessed 24 August 2012).

