Between one and two million migratory agricultural workers (MAWs), primarily from Mexico and Central America, leave their homes each year to plant, cultivate, harvest and pack fruits, vegetables, and nuts in the USA1. While in the USA, most lack health insurance, a permanent residence, and a regular healthcare provider2. The Public Health Service Act 1962 defines MAWs as individuals whose principal employment is in agriculture on a seasonal basis, who have been employed within the last 24 months, and who live in temporary housing units provided by employers3. For almost two decades, researchers have documented the existence of barriers involving medical services including lack of transportation, high cost, and inadequate English language proficiency4-6. As a result, MAWs and their families have been recognized as a medically underserved population4-6. Poor access to medical care continues to exacerbate health problems among members of this population6. Mobility, hazardous occupations, cultural diversity, and low socioeconomic status place migrants, and particularly migrant children, at high risk for inadequate medical care and preventable health problems5.
Agriculture has been documented as one of the most hazardous working environments for both adults and children7. Migratory agricultural workers experience high rates of occupational illness and injury8; those sustaining injuries do not always receive treatment9. Occupationally, MAWs experience unintentional injuries associated with repetitive or unusual motion (pain, sprains, and dislocations) and to single events (cuts and tears, followed by fractures and crush injuries)2. Migratory agricultural workers face multiple hazards from occupational exposures to their eyes and skin from pesticides and other agricultural chemicals2. Environmental conditions including wind, dust, allergens, and ultraviolet light can also contribute to short and long-term health issues for MAWs2.
Relatively little is known about the health of this population10. Information on need, access to medical care and providing medical services to children is not well documented11. Over the past two decades, documented barriers to medical services have included transportation11,12, cost2, and language2. Medical-access barriers involving migrant families were found to be largely non-financial13. Difficulties with transportation have resulted in migrant family members not receiving medical services11. Reports of lack of transportation have gone unheeded14. Non-financial barriers increase the risk of inadequate medical care by preventing individuals from obtaining needed services14.
A lack of education is not thought to be a barrier for farm workers and their families15. Federal assistance programs, such as women, infants and children (WIC) that target female MAWs, have been effective in helping them obtain services for their children10. Migratory agricultural workers family members rarely have consistent healthcare providers; many children do not receive immunizations at recommended intervals11. Perceptions that healthcare provider staff members are disrespectful further inhibit the delivery of medical services to MAWs11.
In many areas of the USA, medical services for MAWs are available at community/migrant health centers. Problems with access may cause these centers to be underutilized. If users cannot travel to a service provider's location, the issue of barriers to care becomes moot. When community/migrant health centers are not located near agricultural areas, barriers to care and issues of access are problematic.
Most published studies have been based on data obtained from providers of healthcare services12. Recommendations of MAWs have been largely overlooked12. The primary purpose of this study was to describe issues associated with barriers to access and receiving medical care from the perspective of MAWs rather than providers. The secondary purpose was to suggest strategies for reducing these barriers.
Data source and participants
The study area encompassed approximately 3774 km2 (2345 miles2). According to data acquired from the Ohio Department of Health and outreach staff from various migrant service providers, there were 19 licensed migrant camps housing 314 families with an estimated population of 1925 MAWs and family members. Approximately 450 were under the age of 14 years. There were no publicly funded or safety-net clinics within a 80 km (50 mile) radius of the camps. There were five hospitals located within a 80 km radius of the 19 camps, but they were only able to provide emergency room care.
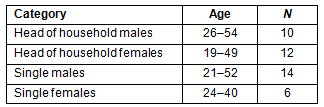
A convenience sample of 42 MAWs living in employer-provided camps was used to populate focus groups (Table 1); all participants were older than 18 years. Four focus group discussions were conducted to obtain information used in developing the survey instrument that was subsequently administered to a second convenience sample of 157 adults also living in employer-provided camps.
Table 1: Focus group participants' demographics
Focus groups
Four focus group discussions were scheduled. Questions for the focus groups were developed and later reviewed by a panel of individuals who were familiar with migrant health issues. The questions centered on issues that had a direct bearing on access or use of health services. Each focus group was led by a female and a male Hispanic. The focus group sessions were conducted in Spanish, audiotaped, transcribed, and translated from Spanish into English by a certified translator. The sessions provided qualitative data concerning the views and experiences of MAWs and their use of healthcare services in Northwest Ohio.
Eleven specific issues about MAW access to health care emerged during the focus group sessions: crop demands, employer demands, weather, cost, travel distance, availability of transportation, lack of interpreter, hours of operation, waiting time, attitude of staff, and no childcare services. Questions in the survey phase of the research were designed to gain a better understanding of these issues.
Instrument
A questionnaire containing 48 items was administered. Questions used in the survey were developed from a review of the literature and concerns obtained from the focus group sessions. The content of the final questionnaire was evaluated by members of the Health Issues Committee of the Hispanic/Latino Health Coalition of Northwest Ohio. The Health Issues Committee consisted of representatives from Henry County Health Department, Ohio Department of Job and Family Services, Fulton County Health Department, Women and Family Services, Latino Family Outreach-Lutheran Social Services, Rural Opportunities Inc, RIDGE Project, OSU Extension, Maumee Valley Parish Nurses, Putnam County Health Department and Williams County Health Department. This group included a variety of experts with experience in medical and dental healthcare programming including public health officials, social workers, nurses, and outreach workers. The researchers provided a final edit of the questionnaire prior to translation and data collection.
The questionnaire was translated into Spanish by a certified translator. Four certified bilingual interpreters were trained to administer the questionnaire and divided into two teams, each consisting of a male and a female. Data collectors administered the surveys at MAW camps on various days and times including weekends, evenings and during inclement weather. Assistance was provided for participants when needed while they responded to the survey. Respondents were offered a $5 store (Wal-Mart) gift card for their participation. Focus group participants were excluded from completing questionnaires. This was controlled for by conducting focus sessions in the early season only with MAWs that had definitive plans to work outside the study area when the survey was administered.
Statistical analysis
A total of 157 usable questionnaires were returned. Data were coded and entered into a computer for analysis. Five different subsets of respondents were used in analysis: all groups combined (n=157), male heads of households (n=39), female heads of households (n=37), single males (n=66), and single females (n=15). Statistical analyses were primarily descriptive. Statistical Package for Social Science v17.0 (www.spss.com) was used to calculate counts, means and percentages. A t-test was performed when needed to compare the means of different groups.
Individuals familiar with migrant health issues met after the data were analyzed. Strategies were suggested to address the barriers of access and receiving medical care identified in the study by MAWs.
Ethics approval
Ethics approval was obtained from the Bowling Green State University Office of Research Compliance (Human Subject Review Board Project Number: H08P303FX2).
The mean age of all respondents who lived in camps was 31.8 ± 10.6 years (n=154). A total of 83.4% respondents had not graduated from high school or earned a GED. One in ten (10.2%) were high school graduates and 2.5% had at least some college. Respondents (aggregated) indicated that they stayed in Northwest Ohio for an average of 18 ± 9 weeks each year. Females (single and heads of households) stayed longer (an average of 19.3 weeks) than did males (single and heads of households) who stayed an average of 17.4 weeks.
The majority of respondents agreed that if they were 'very sick' and a clinic was not available, they would visit the nearest hospital or emergency room. Single males, on average, were willing to wait the longest (4.4 days) to see a doctor for treatment of acute medical conditions compared with male heads of households who were willing to wait an average of 2.2 days.
Three categories of barriers associated with MAW access to medical care were examined: work environment, MAW resources, and healthcare clinic practices.
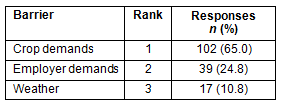
The major barriers associated with the work environment hampering access to medical services were crop demands, employer demands, and weather (Table 2). All percentages reflect numbers of respondents out of 157 indicating barriers.
Table 2: Barriers associated with work environment
The cost of service, travel distance, and transportation were barriers associated with MAW resources hampering their access to receiving medical services. On average, respondents (n=91) could afford to pay $20.50 ± 37.50 per week for healthcare services. The amounts they were willing to pay for medical services ranged from $0 to $200. Females reported being able to pay significantly less than males. As a group, respondents were willing to travel an average of 29.1 km (18.1 miles; range 0-129 km [0-80 miles]) to obtain medical services. Approximately half (50.1%) said that they had access to transportation for traveling to a medical clinic. Female heads of households had significantly less access to transportation compared with male heads of households (t=2.35; df=74; p<0.05). Details of barriers associated with MAW personal resources are provided (Table 3).
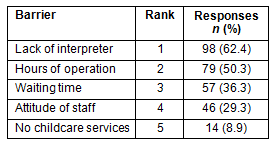
Barriers identified by MAWs associated with healthcare clinic practices included lack of an interpreter, hours of operation, waiting time, attitudes of staff, and no childcare services (Table 4). Respondents reported, on average, that the most convenient times (rounded to the nearest half hour) to visit a physician or medical clinic were between 13.00 and 18.30. Respondents ranked having childcare services available while visiting a doctor or medical clinic as being very important and indicated a preference for walk-in medical clinics compared with making an appointment.
Table 3: Barriers associated with migratory agricultural workers' personal resources
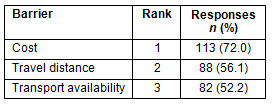
Table 4: Barriers associated with healthcare clinic practices
Respondents ranked agency outreach workers as the most common source for learning about available medical services in Northwest Ohio. Word-of-mouth was a distant second, followed by county Department of Job and Family Services. Rarely did respondents learn about services from supermarket or Laundromat bulletin boards (Table 5).
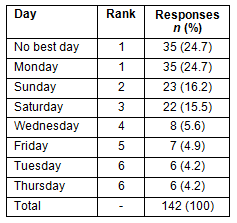
One in four (24.7%) preferred Monday as the single best day to visit a physician or medical clinic, while Sunday and Saturday were the second and third best days for respondents (Table 6).
Table 5: Sources of information about medical services
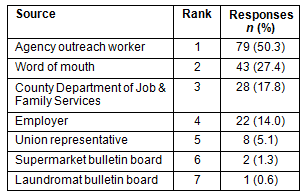
Table 6: Best day of the week to visit a physician or medical clinic
Discussion
This study was undertaken to improve understanding of factors that create or contribute to barriers for medical services that are sought by MAWs. This study identified three categories of barriers associated with MAWs accessing medical services (work environment, MAW resources, and healthcare clinic practices). The main goal of the study was to provide information for public, non-profit and private providers so that they might improve the delivery of medical services for MAWs. It is important to note that the suggestions are based on preference data collected from MAWs rather than from providers.
Crop demands, employer demands, and weather were the main barriers associated with the work environment. Crop demands cannot be postponed. Migratory agricultural workers earn their living by cultivating and harvesting fruits and vegetables. When crops are ripe they must be harvested. This urgency leaves little time for all but emergency healthcare concerns. Migratory agricultural workers risk losing their jobs if they miss work16. Taking time off during the middle of the work day is rarely an option during the harvest. This is probably why late afternoon and evening clinic hours are preferred. Inclement weather can provide opportunities for visiting a doctor or medical clinic. However, predicting the occurrence of inclement weather more than a few days in advance is often unreliable or essentially impossible. This is probably why MAWs favor walk-in clinics over appointments.
The inability to pay for service, travel distance, and transportation were the main barriers associated with MAW personal resources. Medical services can be very expensive2. Many people in the USA have some form of health insurance. A majority of MAWs are uninsured. In 2000, 85% of MAWs were uninsured, compared with 37% of all low-income adults17. Respondents ranked cost as the number-one barrier to medical care. The average annual income for a MAW family in the USA is $21,250 per year, making migrant farm work the second lowest paying job in the nation (after domestic labor)16. Respondents reported that they can afford to pay an average of $20.50 each week (range $0-$58.00) for medical visits. This is a considerable commitment (5.0% of their income on average; potentially 14.2% for individuals willing to pay the most money each week). When respondents are sick and a clinic is not available, they visit the nearest hospital or emergency room. The cost of this alternative is great to both MAWs and society.
Having access to some form of transportation can determine whether or not a MAW has access to medical services. Without transportation to a medical provider's office, all other barriers to care become non-issues. Having transportation becomes moot when medical clinics are not open on days or at times that are available to MAWs. It is important to note that public transportation is not commonly encountered in agricultural communities. It was not available in Northwest Ohio.
Even when transportation is available, the distance to a medical clinic or doctor's office can be a barrier to access. Restrictions on travel distances are often imposed by high fuel costs or travel time requirements. If available, mobile healthcare clinics can be used to address the transportation issue. Mobile units can deliver services directly at camps or be strategically positioned in areas where several camps are located.
Providing health services from mobile units has proven to be a highly successful method of service delivery5. It was found to be especially effective when camps were visited during non-work hours, which allowed people with no transportation or who couldn't leave the field to receive medical attention18. Cost (to purchase, operate, maintain, and staff) is a major factor why mobile units are not used more widely. Many clinics have vans to transport MAWs and their family members to and from clinics, but the number of vans available is inadequate to meet the needs of the population2. Where high fuel prices are an issue, providing MAWs with five- or ten-dollar gas cards may potentially improve access and utilization.
Lack of an interpreter, hours of service, waiting time, attitude of staff, and no childcare services were the main barriers associated with healthcare clinic practices. Language is a major barrier to health services utilization for MAWs2. The great majority of MAWs in the USA are Latino, and their primary language is Spanish2. Respondents rated not having an interpreter as main barrier to receiving medical care. Even where interpreters are available, a wide variety of linguistic dialects among MAWs can make simple English to Spanish translation or interpretation difficult2. Most community/migrant health centers have offices for health providers and usually have bilingual staff. However, when such facilities are not located near places of employment (the nearest community/migrant health center in the study area was more than 80 km [50 miles] away), MAWs are likely to seek healthcare services elsewhere, such as from a local health department, a non-profit agency or a private healthcare provider. These organizations are not likely to have bilingual staff. While some of these organizations may have access to interpreters, it is cost prohibitive to have them available on a continuous basis.
Office hours offered by providers and hours preferred by MAWs are not aligned. Operating medical clinics on days and hours that are not convenient for MAWs does little to benefit them even when they have the funds to pay for these services. Since MAWs cannot change the times they can access health services, providers must be willing to modify their hours of operation to accommodate these persons.
Providers with a better understanding of the culture can convey accepting attitudes, which may result in better relationship with more sharing of information to support better health outcomes19. The relationship between cultural attributes and attitudes of healthcare provider staff were not specifically examined in this study. Cultural attributes can also result in barriers for workers and their families to delay, or choose not to seek medical care2,20. One example of this is a common folk medicine belief that an imbalance of hot and cold forces within the body causes disease and illness. Persons attempt to self-treat their illnesses by using hot or cold treatments or herbal therapies to bring the body into balance19. More research in this area can help healthcare providers gain more appreciation of the folk medicine practices used in this culture. Providers with a better understanding of the culture are more likely to be more respectful of patients' values, which may result in better relationships with more sharing of information to support better health outcomes19. Having a better understanding about cultural differences helps ensure that the care being provided does not vary in quality because of personal characteristics.
The availability of childcare services while visiting a medical clinic or provider's office is important to some MAWs. Providers of medical services for MAWs should consider offering this service since it has the potential to reduce cancelled appointments or eliminate clients not attending as scheduled.
How MAWs learn about available medical service providers can influence utilization. Contrary to common beliefs about providing health information to underserved populations, respondents did not learn about services from supermarket or laundromat bulletin boards. The value of utilizing outreach workers to convey medical care information to MAWs cannot be underestimated.
Recommendations
Previous studies have reported that a majority of MAWs encounter barriers when trying to receive medical services. Strategies for providers to improve practices that should help reduce barriers to health care were developed using suggestions provided by MAWs. Acknowledging that implementing these strategies is limited by the availability of resources, the following strategies should be considered:
- provide transportation services to enable MAWs to visit medical providers (gasoline vouchers can assist those who have access to personal transportation)
- operate clinics between 13.00 and 18.30, especially on Mondays and weekends
- provide medical services to MAWs at clinics even if appointments have not been made
- utilize mobile clinics; locate the clinics close to camps
- employ bilingual staff whenever possible
- provide childcare services
- use agency outreach workers such as county Job and Family Services employees to promote availability of services
- offer several services in one place at one time (co-location) to reduce travel related barriers14.
Conclusions
Three general categories of barriers to health care for MAWs emerged from this study: work environment, MAW resources, and healthcare clinic practices. Work environment issues relate mostly to the employers of MAWs and this study did not delve into these. Future research could explore how MAW employers can help address work environment barriers. Because they are poor and have limited funds for the cost of transportation to clinics and the fees associated with accessing health care, personal resources created barriers for MAWs. Migratory agricultural workers barely get by and have little control over barriers associated with resources. Some strategies to address healthcare clinic practices barriers were developed by the group conducting the study. Migratory agricultural workers not having access to healthcare services can develop more severe and prolonged illnesses and often lead to the inappropriate use of more expensive forms of medical care, such as emergency rooms and urgent care centers21. By listening to what MAWs describe as barriers to health care, providers can help improve access which can reduce the use of 'high cost' emergency care. An improved quality life for MAWs is a hitherto unstated, but important goal.
Further research is needed to more deeply understand the effectiveness of the healthcare clinic practices strategies and explore other options. Examples of future research questions that could improve healthcare clinic practices include, what is the most effective method to provide transportation for MAWs? Are options other than gasoline vouchers and mobile units available? If mobile units are available, how often should they be dispatched to MAW neighborhoods? Since MAWs prefer 'walk-in appointments', what percentage of clinic appointments should be allocated for them? MAWs said that they learned the most about available medical services from agency outreach workers; can this effectiveness be replicated or applied to other sources of information?
Providing healthcare services for MAWs and their families is complicated. Other than cost, what makes providing health care for this population challenging, are issues primarily related to mobility and differences in language and culture. Migratory agricultural workers continue to be an underserved population with increased risks of injury and illnesses. Further research should continue to explore barriers to health care from their perspective.
References
1. Holmes SM. An ethnographic study of the social context of migrant health in the United States. Public Library of Science Medicine 2006; 3(10): e448.
2. Arcury TA, Quandt SA. Delivery of health services to migrant and seasonal farmworkers. Annual Review of Public Health 2007; 28: 345-363.
3. United States Federal Government. United States Code: Title 42, The Public Health and Welfare. Chapter 6A, Public Health Service, Public Health Service Act, Title III, Part D, Section 330, Migrant Health. Washington, DC; US Government, 1962.
4. Albritton TA, Wagner PJ. Linking cultural competency and community service: a partnership between students, faculty, and the community. Academic Medicine 2002; 77: 738-739.
5. Gwyther ME, Jenkins M. Migrant farmworker children: health status barriers to care and nursing innovations in health care delivery. Journal of Pediatric Health Care 1998; 12(2): 60-66.
6. Mobed K, Gold EB, Schenker MB. Occupational health problems among migrant and seasonal farm workers. Western Journal of Medicine 1992; 157(3): 367-373.
7. Cooper SR, Cooper SP, Felknor SS, Santana VS, Fischer FM, Shipp EM et al. Nontraditional work factors in farmworker adolescent populations: implications for health research and interventions. Public Health Reports 2005; 120(6): 622-629.
8. Arcury TA, Quandt SA, Simmons S. Farmer health beliefs about an occupational illness that affect farmworkers: the case of green tobacco sickness. Journal of Agricultural Safety and Health 2003; 9(1): 33-45.
9. Earle-Richardson GB, Brower MA, Jones AM, May JJ, Jenkins PL. Estimating the occupational morbidity for migrant and seasonal farmworkers in New York State: a comparison of two methods. Annals of Epidemiology 2008; 18(1): 1-7.
10. Villarejo D. The health of U.S. hired farm workers. Annual Review of Public Health 2003; 24: 175-193.
11. Gentry K, Quandt SA, Davis SW, Grzywacz JG, Hiott AE, Arcury TA. Child healthcare in two farmworker populations. Journal of Community Health 2007; 32(6): 419-431.
12. Littlefield C, Stout CL. A survey of Colorado's migrant farmworkers: access to health care. International Migration Review 1987; 21: 688-708.
13. Weathers A, Minkovitz C, O'Campo P, Diener-West M. Access to care for children of migratory agricultural workers: factors associated with unmet need for medical care. Pediatrics 2004; 113(4): 276-282.
14. Klerman L V. Nonfinancial barriers to the receipt of medical care. Future of Children 1992; 2(2): 171-185.
15. Quandt SA, Clark HM, Rao P, Arcury TA. Oral health of children and adults in Latino migrant and seasonal farmworkers families. Journal of Immigrant and Minority Health 2007; 9: 229-235.
16. United States Department of Agriculture, Economic Research Service. Briefing rooms: Rural Labor and Education: Farm Labor. (Online) 2011. Available: http://www.ers.usda.gov/Briefing/LaborAndEducation/FarmLabor.htm#wages . (Accessed 1 February 2011).
17. Rosenbaum S, Shin P. Migrant and Seasonal Farmworkers. Health Insurance Coverage and Access to Care. Washington, DC: Kaiser Commission on Medicaid and the Uninsured, 2005.
18. Stein LM. Health care delivery to farmworkers in the southwest: An innovative nursing clinic. Journal of the American Academy of Nurse Practitioners. 1993; 5: 119-124.
19. Eggenberger S, Grassley J, Restrepo E. Culturally competent nursing care for families: listening to the voices of Mexican-American women. Online Journal of Issues in Nursing 2006; 3. Available: http://www.nursingworld.org/MainMenuCategories/ANAMarketplace/ANAPeriodicals/OJIN/TableofContents/Volume112006/No3Sept06/ArticlePreviousTopics/CulturallyCompetentNursingCare.html (Accessed 23 May 2012).
20. Arcury TA, Quandt SA, Cravey AJ, Elmore RC, Russell GB. Farmworker reports of pesticide safety and sanitation in the work environment. American Journal of Industrial Medicine 2001; 39: 487-498.
21. Schmalzried HD, Liszak J. A model program to reduce patient failure to keep scheduled medical appointments. Journal of Community Health 2012; 37(3): 715-718.

