Mental health research has revealed that the manifestation of most mental health issues begins in adolescence1. Mental health problems are a major burden of disease for adolescents, with 20% of Australian 12-16 year-olds having some form of mental disorder2, and reports indicating that between 4% and 25% of adolescents experience depression3-6. While depression is the leading contributor to the global burden of disease in middle-to-high income countries and for those aged 15-44 years, as well as the leading cause of disability7, early interventions are possible to improve long-term outcomes and reduce the burden of mental health problems8.
The prevalence of mental health issues in adolescence is of particular concern as adolescents with depression also experience difficulties in other aspects of their lives9. Depression is often associated with physical co-morbidities such as chronic health problems10 and psychiatric co-morbidities, which tend to be externalised problems for males and internalised problems for females3,11,12. It is also associated with negative outcomes such as mental health problems in adulthood11,13. Depression in adolescence is particularly concerning due to its link to suicidal ideation14-16, deliberate self-harm, attempted suicide and suicide completion8,9,16-18.
This study aims to establish the relationship between community characteristics in rural/remote areas and the prevalence of depression in rural adolescents, taking into account gender differences. It is important to examine the effects of rurality on mental health because there is ongoing debate regarding whether people in rural regions are at a disadvantage due to the lack of accessible mental health services19.
Previous research has identified particular rural community characteristics, rather than rurality in itself, as relevant to mental health outcomes. These include: poorer physical health10,20; the health status of Indigenous people20,21; rapid social change caused by globalisation10,22; higher poverty and unemployment compounded by higher priced commodities10,20,21,23; fewer educational opportunities20; fewer social opportunities and social exclusion for defying community norms23; youth migrating to cities10,21; the poor migrating to rural areas10; unpredictable environmental issues (ie drought, bushfire)21; lack of facilities and specialists21; risky employment (ie mining) and health practices (ie increased alcohol consumption and tobacco use)21; and socioeconomic status (SES)3,24.
The studies of both Paykel et al25 and Eckert et al26 which were based on data collected from adults aged 16 to 64 years, found that by placing individual variables associated with depression into their analyses, place of residence was not a significant predictor of depression. Boyd et al reported poor availability and accessibility of health services in Australian rural areas as a barrier to adolescents seeking help for mental health issues1. Structural difficulties in service provision, such as poor public transport and limited choice of health professionals, further impacted on help-seeking behaviour.
There is limited work to date examining the prevalence of depression in rural and metropolitan Australian adolescents. Sawyer et al conducted a nation-wide Australian survey which accumulated proportionate data from both metropolitan and non-metropolitan samples, and carried out analyses investigating residency and gender differences between the samples3. They found that Australian males and females aged 6-17 years had similar rates of depressive disorder in metropolitan areas (3.9 and 3.8%, respectively) while males had almost double the rate of depressive disorder than females in non-metropolitan areas (4.6 and 2.4%). The authors did not comment on the significance of the interaction between gender and residence. These findings are contrary to the majority of literature on adolescent depression which reports that during adolescence a significant gender difference emerges with twice as many females as males suffering from depression12,14,27.
In a ten-year longitudinal study using a New Zealand metropolitan sample, Hankin et al found that at age 15 years, 4% of females were diagnosed with depression but only 1% of males had this diagnosis12. Both genders experienced a rapid rise in depression rates from age 15 to 18 years; however, the rise in females was more dramatic, increasing the gender difference (23% of females and 11% of males). These rates may reflect different risk and protective factors operating for boys and girls. For example, girls have been reported to have better mental health literacy regarding depression, show more concern for those with depression, be more likely to think help should be sought for depression, and be better able to recognise depression and depressive symptoms18.
The gender difference found by Sawyer et al3 could also be explained by different risk factors operating in metropolitan versus non-metropolitan areas. For example, a rural environment may be more protective for females11. This is an area of some debate, with competing stereotypes: in one case the rural community is constructed as supportive and health enhancing; in the other, rural areas are associated with deprivation, lack of services and hardship28. In reality, rural areas are not homogenous as existing categories of rurality do not encompass the social, economic, cultural and environmental diversity of non-metropolitan regions29. There is a great deal of variation and combining different rural communities in analyses may average out differences, obscuring the real picture10,21. Nevertheless, the advantages of categorising rurality using an established measure such as the Accessibility/Remoteness Index of Australia Plus (ARIA+), is that it allows simple and stable classification for measuring access to service centres within a region30.
As 30% of the Australian population lives in rural or remote areas21, and depression has been shown to be associated with negative health outcomes, it is important to understand the relationship between depression, gender and rural residency. Understanding the interplay of these factors would assist the development of more appropriate prevention and intervention strategies.
In this study, it was hypothesised that the prevalence of depressive symptoms would vary with the degree of remoteness, SES, gender and the perception of rural community characteristics (long waiting lists and lack of available health professionals). Based on the majority of previous work in this area, it was expected that: (i) rural females would have a higher prevalence of depression than males; (ii) higher degrees of remoteness and lower SES would be related to higher rates of depression; and (iii) adolescents who screened as depressed would perceive health services in rural communities to have long waiting lists and insufficient health professionals. In addition, these relationships were also examined separately for male and female adolescents because previous research has suggested the likelihood of gender differences11,18,28.
Participants
Approximately 3008 Year 9 to 12 students from the 23 schools were invited to participate. Participation rates were low and only 531 students participated (18%). Of those who participated, 55.7% were female, 98.5% were born in Australia and 4.3% identified as Aboriginal or Torres Strait Islander. Ages ranged from 13 to 18 years with a mean age of 15.08 years (SD=1.21), and ARIA+ scores ranged from 0 to 14.54 with a mean ARIA+ score of 4.73 (SD=2.39). The SES scores ranged from 749 to 1124 with a mean SES score of 912.51 (SD=32.52), indicating a low SES sample.
Measures
This study is a component of the Adolescent Mental Health, Behaviour and Life Experiences Study (unpubl. data; authors). The questionnaire included demographic questions covering age, gender, and home postcode as well as the 6-Item Kutcher Adolescent Depression Scale (KADS-6)31. The KADS-6 is designed to assess symptoms consistent with DSM-IV diagnoses of major depressive disorder32. The scale consists of 6 items in which respondents indicate the frequency of symptoms using a four point scale ranging from 0 (hardly ever), 1 (much of the time), 2 (most of the time) to 3 (all of the time). It has been demonstrated that the 6 item KADS has high sensitivity (92%), good specificity (71%), and good test-retest reliability (Cronbach's α of 0.80) using a cut-off score of 632, as well as having a high correlation with the Beck Depression Inventory (BDI)33. In the current study, a cut-off score of 6 was used to determine whether adolescents screened as depressed. The KADS-6 had a Cronbach's α of 0.83.
Home postcode was used to measure degree of remoteness as measured by the ARIA+30. For participants (n=23) who did not specify their home postcode, school postcode was used. The SES was determined from the Australian Bureau of Statistics (ABS) Socio-Economic Index of Relative Socio-Economic Advantage and Disadvantage (SEIFA) (SEIFA National Mean=1000; SD=100). This gives an indication of the socio-economic conditions in a neighbourhood area, based on information collected in the 2006 Australian Census34. Lower scores indicate more socio-economic disadvantage.
A section in the questionnaire required participants to select possible reasons for difficulty seeking mental health care in rural areas from a list. The possible causes explored in this study were insufficient mental healthcare professionals, and long waiting lists.
The ARIA+ measures access in terms of remoteness along the road transport network from populated localities to service centres30. For each locality, distance to service centres is converted to a ratio to the mean which produces a continuous variable with remoteness values ranging from 0 to 1535. An ARIA+ score of zero indicates high access to services and 15 indicates very poor access to services.
Procedure
The principals of public schools in South Australia located outside of metropolitan Adelaide were sent information about the study and an invitation to participate. School principals were then contacted by telephone to discuss participation. Seventy-two schools were contacted and, of those, 23 schools participated. School principals could elect for students to self-administer the questionnaire in hard copy or electronic form. Schools that agreed to participate were sent a list of contacts for local, state and national mental health professionals and services to distribute to students following completion of the questionnaire.
The most common reason for non-participation was that the school did not have the time to participate, either due to commitment to other research or lack of resources such as time and teachers to supervise administration of the questionnaire (n=27). Other reasons for non-participation included difficulty establishing contact with the school principal (n=12), the study not appealing to staff or students (n=4), discomfort with the subject matter of the survey (n=3), and difficulty getting consent forms returned (n=3). Questionnaire completion began in May 2010 and continued through to August 2010.
Data analysis
The data were analysed using SPSS v18.0.2 (www.spss.com). Chi-square tests were used to examine the relationship between gender and depression, and perceptions of waiting lists and availability of health professionals and depression. Mann-Whitney U-tests were used to examine the relationship between ARIA+ scores, gender and depression. Independent-samples t-tests were used to examine relationships between SES, gender and depression. Findings were considered significant at p ≤0.05.
Ethics approval
Ethics approval was obtained from the University of Adelaide, School of Psychology Ethics Committee (#10/07) and the South Australian Department of Education Ethics Committee.
A small number of participants had missing data on one or more measure (maximum missing data=8 participants on KADS, 1.51%). These participants were not included in analyses involving these measures.
Depression
Overall, 18.1% of participants (n=95) screened positive for depression on the KADS. On an item of the KADS that measured depressed mood ('Over the last week, how have you been 'on average' or 'usually' regarding the following items: Low mood, sadness, feeling blah or down, depressed, just can't be bothered'), 28.7% of participants (n=151) responded that they experienced low mood, sadness or depression much of the time, 11.6% (n=61) most of the time, and 1.1% (n=6) all of the time. Of some concern were responses to the KADS item assessing suicide and self-harm ('Thoughts, plans, or actions about suicide or self-harm'), with 12.4% (n=65) of participants reporting occasional thoughts about suicide or self-harming, 4.0% (n=21) reporting frequent thoughts, and 3.6% (n=19) reporting suicidal or self-harming plans or actions.
Gender
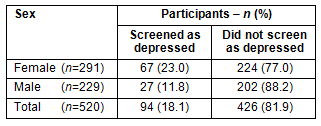
A 2 x 2 χ² was carried out to test whether there was a significant relationship between gender and depression. Altogether 23% of females and 11.8% of males screened positive for depression on the KADS (Table 1). The χ² value of 10.92 had an associated probability of p=0.001, df=1. However, Cramer's V was found to be 0.15, indicating only 2.25% of the variation in the frequency of depression can be explained by gender.
Table 1: Prevalence of depression among females and males
Degree of remoteness, depression and gender
As ARIA+ scores were not normally distributed, a Mann-Whitney U-test was conducted to investigate whether the ARIA+ scores of those who screened positive for depression on the KADS differed significantly from those who did not. The Mann-Whitney U was found to be 18577.0 (z=-1.32) with an associated probability of p=0.19 indicating differences between the two groups were not significant.
A Mann-Whitney U-test revealed no significant difference between the ARIA+ scores of females who screened as depressed (Md [median value]=4.15, n=67) and those who did not (Md=4.46, n=224), U=6959, z=-0.90, p=0.37, r=-0.05. There was no significant difference between the ARIA+ scores for males who screened as depressed (Md=3.83, n=27) and those who did not (Md=4.15, n=202), U=2357.5, z=-1.15, p=0.25, r=-0.08.
Socioeconomic status, depression and gender
An independent-samples t-test was conducted to compare the SES of those who screened as depressed and those who did not. There was no significant difference in SES for participants who screened as depressed (M=909.99, SD=28.50) and those who did not (M=912.93, SD=33.62); t(518)=0.79, p=0.43 (two-tailed). The magnitude of the differences in the means (mean difference=2.94, 95% CI: -4.36 to 10.24) was very small (eta-squared=0.001).
There was no significant difference in SES for females who screened as depressed (M=909.70, SD=28.77) and those who did not (M=914.12, SD=29.28); t(287)=1.09, p=0.28 (two-tailed). There was also no significant difference in SES for males who screened as depressed (M=912.33, SD=27.46) and those who did not (M=911.83, SD=37.97); t(226)=-0.07, p=0.95 (two-tailed).
Perception of waiting lists as too long and depression
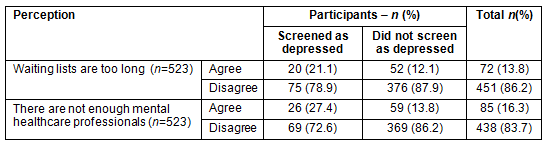
A 2 x 2 χ² analysis revealed that screening positive for depression was significantly related to the perception that waiting lists were too long (χ²=10.54, p=0.001, df=1) which explained 2% of the variance in frequency of depression (Cramer's V=0.14). A χ²-test for independence (with Yate's continuity correction) indicated a significant association for females between depression and the perception of waiting lists as too long, χ²(1, n=291)=9.35, p=0.002, phi=0.19. There was no significant association for males, χ² (1, n=229)=0.500, p=0.48, phi=0.07 (Table 2).
Perception of availability of health professionals and depression
A 2 x 2 χ² analysis revealed that depression was significantly related to the perception that there were not enough mental health professionals (χ²=5.19, p=0.02, df=1) which explained 1% of the variance in frequency of depression (Cramer's V=0.10). A χ²-test for independence (with Yate's continuity correction) indicated a significant association in females between depression and the perceived unavailability of mental health services, χ² (1, n=291)=5.88, p=0.02, phi=0.15. The association was not significant for males, χ² (1, n=229)=0, p=1.0, phi=0.02 (Table 2).
Table 2: Perceptions of rural community characteristics for depressed and not depressed adolescents
Discussion
This study aimed to explore the prevalence of depression in rural adolescents in relation to degree of remoteness, SES and the perception of rural community characteristics, taking gender differences into account. The community characteristics considered were the availability of mental health services and service waiting lists. The percentage of adolescents who screened as depressed on the KADS-6 (18%) was higher than that reported among rural adolescents by Sawyer et al3; however, the KADS-6 is a screening measure rather than a diagnostic tool. Despite this, the current finding is consistent with other literature4-6.
The results are concerning because 41% of participants reported having low mood much of the time or more often and 20% experienced occasional or more frequent self-harm or suicidal thoughts, plans or actions. While similar numbers of males and females participated in this study, low participation rates may reduce the representativeness of this sample for rural adolescents. Because questionnaires were implemented in school, students who were absent and school-leavers, who may have higher psychological morbidity, would also have been excluded from the study. In addition, data were obtained by self-report, participants completed questionnaires during class time when others were present, and questionnaires administered in hardcopy were returned to teachers following completion. Though teachers were advised that the questionnaire was intended to be confidential, participants may have been reluctant to fully disclose information in this context.
Nevertheless, this research suggests that depression remains an issue of considerable concern among South Australian rural adolescents, especially with remote areas having fewer qualified mental health professionals and mental health services36.
Gender and depression
Despite the finding of Sawyer et al that non-metropolitan males experienced higher rates of depression than females3, the present study found that females were more likely than males to screen as depressed on the KADS-6 (23.0% and 11.8%, respectively). This difference was consistent with the majority of the literature on adolescent depression which suggests higher rates of depression in females12,14,27.
Rural residency may be associated with numerous mental health risk factors, such as deprivation, hardship, and a lack of mental health services28. These factors may contribute to a high incidence of depression for both males and females.
Degree of remoteness, depression and gender
While the incidence of depression was high in this sample, there was no evidence of a link between ARIA+ scores and depression. The general perception that rural communities are at heightened risk of mental illness due to their degree of remoteness24 was not supported in this study. However, these results are consistent with other research that has shown that it is not rurality per se that affects the prevalence of adolescent depression in rural regions. Rather, it may be that community characteristics or particular stressors such as life events and interpersonal relations37 are triggers.
An advantage of using ARIA+ is that it can be applied to any level of geography, including geocoded latitude and longitude points30. However, this is also a limitation. This methodology has to work with a number of assumptions which may not always be accurate (eg levels of car ownership and road conditions)35. It is assumed that people living in an area have access to road transport; however, people in rural areas have more limited access to roads and public transport systems than metropolitan populations. In addition, ARIA+ does not allow for differences in terms of road quality and serviceability in calculating distance to service centres. However, ARIA+ was used in this study due to its advantages in differentiating between areas in terms of levels of accessibility when compared to other remoteness classifications such as the Rural, Remote and Metropolitan Areas (RRMA) classification35.
Socioeconomic status, depression and gender
The survey conducted by Sawyer et al with Australian adolescents revealed a higher prevalence of mental health problems among adolescents living in low SES families3. Though Eckert et al suggested that SES, as a psychosocial determinant of health, plays an important part in prognosis of mental illness24, this study found that the incidence of depression was not significantly related to SES. This may be due to the low SES of the sample as a whole. In South Australia, adolescents from higher SES families may be more likely to attend high school in city based non-government boarding schools. In addition, the current study did not recruit participants from non-government schools. These two factors probably contributed to the current sample being of lower SES than South Australian rural adolescents overall. To overcome this issue and obtain more representative samples of non-metropolitan adolescents, other approaches to recruiting adolescents should be considered. This would allow the relationship of depression to SES to be considered more definitively. Future work should also consider broadening the assessment of SES as the SEIFA is based on postcode, which in rural and remote areas can include significant diversity of SES; inclusion of parent education or occupation may result in more precise estimation of SES. Research could also explore other psychosocial determinants of health such as stressful life events24 and loss together with socio-demographic characteristics and lifestyle behaviours among rural adolescents, which may contribute to the incidence of depression.
Though this study did not support the hypotheses that the degree of remoteness and SES were related to depression, these may still emerge as significant factors for rural adolescents if compared with metropolitan adolescents. Thus, future research could further explore these relationships using adolescent participants from both metropolitan and non-metropolitan areas.
Perception of waiting lists as too long, lack of mental health professionals and depression
Depression was significantly related to the perception of long waiting lists and fewer mental health professionals. Considering the high rate of those who screened positive for depression, this perception is quite concerning as it may affect help-seeking attitudes of residents in non-metropolitan communities. For instance, if adolescents believe that there is a long wait for professional help and that little help is available, it seems probable that they are less likely to seek help. There are numerous factors that could influence this perception. It could be that lack of service availability is a genuine feature of the rural communities this sample was drawn from, and those who screened as depressed had better system knowledge due to previous engagement. Alternatively, because depression is related to pessimistic thinking12,38, it may be that those who are depressed think more negatively about their likelihood of being able to access support. Other potential factors include, but are not limited to, poor mental health literacy and limited knowledge of how to access mental health supports. Further understanding of the relationship between the perception of rural community characteristics, help-seeking behaviours, and service availability may enhance service utilisation and provision according to population characteristics.
Analyses revealed significant associations between depression and perceptions of waiting lists and unavailability of mental health care for females. This may be a reflection of previous findings that females are more likely than males to identify symptoms of depression and be willing to seek help for mental health issues18. Through help-seeking, females may have a better awareness of service availability.
More research is needed to understand the relationships between factors associated with adolescent depression in a rural context and variables that mediate these relationships. Samples from both metropolitan and non-metropolitan areas could be compared to identify any differences in factors operating in each context. Furthermore, low participation rates could have resulted from difficulty having consent forms returned to schools. Most principals and teachers believed this was due to logistical difficulties rather than the failure of parents or students to consent. Hence, to overcome this barrier, methodologies such as more active pursuit of consent (ie telephone calls to parents, notices in school newsletters) or other recruitment approaches could improve participation rates.
The high incidence of depression among rural Australian adolescents is concerning, especially for females. The rate of depression in this sample was related to perceptions of the availability of mental health support, and was not related to SES or degree of remoteness as measured by the ARIA+. Females who screened as depressed were particularly susceptible to negative perceptions regarding the availability of mental health services within their communities. This research indicates that continuing health initiatives are required to enhance the mental health of rural South Australian adolescents. Areas to target may include improving the availability of mental health services, improving mental health literacy, promoting awareness of available mental health services within regions, and promoting help-seeking behaviour for those with mental health difficulties. Finally, consideration should be given to the gender differences identified when developing future mental health initiatives.
References
1. Boyd CP, Hayes L, Nurse S, Aisbett DL, Francis K, Newnham K et al Preferences and intention of rural adolescents toward seeking help for mental health problems. Rural and Remote Health 11: 1582. (Online) 2006. Available: www.rrh.org.au (Accessed 14 December 2011).
2. Moon L, Meyer P, Grau J. Australia's Young People: Their Health and Well Being 1999. AIHW Cat no. PHE 19. Canberra, ACT: AIHW, 1999.
3. Sawyer MG, Arney FM, Baghurst P, Clark J, Graetz B, Kosky R et al The Mental Health of Young People in Australia: Child and Adolescent Component of the National Survey of Mental Health and Well-being, Australia. Canberra, ACT: Mental Health and Special Programs Branch, Commonwealth Department of Health and Aged Care, 2000.
4. Boyd CP, Gullone E, Kostanski M, Ollendick TH, Shek DTL. Prevalence of anxiety and depression in Australian adolescents: Comparisons with worldwide data. Journal of Genetic Psychology 2000; 161(4): 479-492.
5. Lewinsohn PM, Rohde P, Seeley JR. Major depressive disorder in older adolescents: Prevalence, risk factors, and clinical implications. Clinical Psychology Review 1998; 18(7): 765-794.
6. Bartik W, Kowalenko N, Whitefield K, Wignall A (Eds). Anxiety and depression in young people: A collaborative rural and remote model. In: Proceedings, 6th National Rural Health Conference; 4-7 March 2001; Canberra, ACT: National Rural Health Alliance, 2001.
7. Mathers C, Fat DM, Boerma J. The global burden of disease: 2004 update. Geneva: World Health Organization, 2008.
8. Hernan A, Philpot B, Edmonds A, Reddy P. Healthy minds for country youth: help-seeking for depression among rural adolescents. Australian Journal of Rural Health 2010; 18(3): 118-124.
9. Sawyer MG, Arney FM, Baghurst PA, Clark JJ, Graetz BW, Kosky RJ et al The mental health of young people in Australia: Key findings from the child and adolescent component of the national survey of mental health and well-being. Australian and New Zealand Journal of Psychiatry 2001; 35(6): 806-814.
10. Judd FK, Jackson HJ, Komiti A, Murray G, Hodgins G, Fraser C. High prevalence disorders in urban and rural communities. Australian and New Zealand Journal of Psychiatry 2002; 36(1): 104-113.
11. Burns JJ, Cottrell L, Perkins K, Pack R, Stanton B, Hobbs G et al Depressive symptoms and health risk among rural adolescents. Pediatrics 2004; 113(51): 1313-1320.
12. Hankin BL, Abramson LY, Moffitt TE, Angell KE, Silva PA, McGee R. Development of depression from preadolescence to young adulthood: Emerging gender differences in a 10-year longitudinal study. Journal of Abnormal Psychology 1998; 107(1): 128-140.
13. Commonwealth Department of Health and Aged Care. National Action Plan for Promotion, Prevention, and Early Intervention for Mental Health. Canberra, ACT: Mental Health and Special Programs Branch, Commonwealth Department of Health and Aged Care, 2000.
14. Allison S, Roeger L, Martin G, Keeves J. Gender differences in the relationship between depression and suicidal ideation in young adolescents. Australian and New Zealand Journal of Psychiatry 2001; 35(4): 498-503.
15. Bourke L. Toward understanding youth suicide in an Australian rural community. Social Science and Medicine 2003; 57(12): 2355-2365.
16. Caldwell TM, Jorm AF, Dear KBG. Suicide and mental health in rural, remote and metropolitan areas in Australia. Medical Journal of Australia 2004; 181(7): S10-S4.
17. Pagliaro LA. Adolescent depression and suicide: A review and analysis of the current literature. Canadian Journal of School Psychology 1996; 11(2): 191-201.
18. Burns JR, Rapee RM. Adolescent mental health literacy: Young people's knowledge of depression and help seeking. Journal of Adolescence 2006; 29(2): 225-239.
19. Goldney RD, Taylor AW, Bain MA. Depression and remoteness from health services in South Australia. Australian Journal of Rural Health 2007; 15(3): 201-210.
20. Australian Institute of Health and Welfare. Australia's Young People, Their Health and Wellbeing. Canberra, ACT: Australian Institute of Health and Welfare, 2003.
21. Rajkumar S, Hoolahan B. Remoteness and issues in mental health care: Experience from rural Australia. Epidemiologia e Psichiatria Sociale 2004; 13(2): 78-82.
22. Ryland DH, Kruesi MJP. Suicide among adolescents. International Review of Psychiatry 1992; 4(2): 185-195.
23. Boyd CP, Aisbett DL, Francis K, Kelly M, Newnham K. Issues in rural adolescent mental health in Australia. Rural and Remote Health 6(1): 501. (Online) 2006. Available: www.rrh.org.au (Accessed 13 December 2011).
24. Eckert KA, Wilkinson D, Taylor AW, Stewart S, Tucker GR. A population view of mental illness in South Australia: Broader issues than location. Rural and Remote Health 6(2): 541. (Online) 2006. Available: www.rrh.org.au (Accessed 13 December 2011).
25. Paykel ES, Abbott R, Jenkins R, Brugha TS, Meltzer H. Urban-rural mental health differences in Great Britain: Findings from the National Morbidity Survey. Psychological Medicine 2000; 30(2): 269-280.
26. Eckert KA, Taylor AW, Wilkinson DD, Tucker GR. How does mental health status relate to accessibility and remoteness? Medical Journal of Australia 2004; 181(10):540-543.
27. Patton GC, Hibbert M, Rosier MJ, Carlin JB, Caust J, Bowes G. Is smoking associated with depression and anxiety in teenagers? American Journal of Public Health 1996; 86(2): 225-230.
28. Wainer J, Chesters J. Rural mental health: Neither romanticism nor despair. The Australian Journal of Rural Health 2000; 8(3): 141-147.
29. Kelly BJ, Stain HJ, Coleman C, Perkins D, Fragar L, Fuller J et al Mental health and well-being within rural communities: The Australian rural mental health study. Australian Journal of Rural Health 2010; 18(1): 16-24.
30. Department of Health and Aged Care. Measuring Remoteness: Accessibility/Remoteness Index of Australia (ARIA), revised edn. Occasional Papers New Series no. 14. Canberra, ACT: DHAC, 2001.
31. Kutcher SP, Chehil S. Suicide risk management: A manual for health professionals. Melbourne, VIC: Wiley-Blackwell, 2007.
32. LeBlanc JC, Almudevar A, Brooks SJ, Kutcher S. Screening for adolescent depression: Comparison of the Kutcher adolescent depression scale with the Beck depression inventory. Journal of Child and Adolescent Psychopharmacology 2002; 12(2): 113-126.
33. Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J. An inventory for measuring depression. Archives of General Psychiatry 1961; 4(6): 561-571.
34. Australian Bureau of Statistics (ABS). Census of Population and Housing: Socio-economic Indexes for Areas (SEIFA), 2006. Table 2. Postal Area (POA) Index of Relative Socio-economic Advantage and Disadvantage, 2006. (Online) 2006. Available: http://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/2033.0.55.0012006?OpenDocument (Accessed 16 December 2011).
35. Glover J, Tennant S. Remote Areas Statistical Geography in Australia: Notes on the Accessibility/Remoteness Index for Australia (ARIA+ version). Working Paper Series no 9. Adelaide, SA: Public Health Information Development Unit, 2003.
36. Inder KJ, Berry H, Kelly BJ. Using cohort studies to investigate rural and remote mental health. Australian Journal of Rural Health 2011; 19(4): 171-178.
37. Stark CR, Riordan V, O'Connor R. A conceptual model of suicide in rural areas. Rural and Remote Health 11(2): 1622. (Online) 2011. Available: www.rrh.org.au (Accessed 19 June 2012).
38. Eckert KA, Kutek SM, Dunn KI, Air TM, Goldney RD. Changes in depression-related mental health literacy in young men from rural and urban South Australia. Australian Journal of Rural Health 2010; 18(4): 153-158.
