Alice Springs Hospital (ASH) services a unique population. The catchment area exceeds 1 million km2, yet contains an estimated 41 000 population, of whom approximately 40% identify as being of Indigenous race1.
The poor health of the Indigenous population has been well documented and includes higher rates of chronic co-morbid disease, which is present at a younger age2,3, while access to and continuity of care has been demonstrated as suboptimal3. The gap between Indigenous and non-Indigenous life expectancy has been well described4, and the vast majority of this gap has been attributed to the effects of chronic disease5.
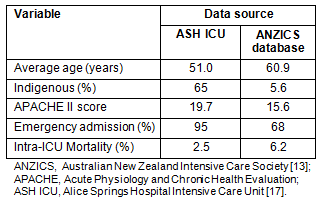
As a consequence, the service population presenting to the ASH Intensive Care Unit (ICU) is markedly different to that seen within other units across the country (Table 1), and there is a perception that many of the patients discharged from the ASH ICU, remain at increased risk of further acute episodes. There is a strong suspicion that this is associated with increased morbidity and functional loss. It is thought that intervention/s that reduce/s morbidity and functional loss may reduce re-admissions, but there is no baseline data regarding morbidity in the post-ICU period for this group.
There is, however, a growing body of international research on specific population groups that demonstrates persisting functional deficits6, including reduced achieved six-minute walk distances7. These studies have predominantly been undertaken in large tertiary institutions in capital cities, and there is little data on the outcomes for rural patients.
To further investigate this an exploratory pilot study was undertaken to assess the ability to identify, and the logistics to follow up patients thought to be at 'high risk' of subsequent morbidity, and to assess the tools for quantifying any persisting morbidity. In this case series we present selected data focussing on functional outcomes from this study.
Table 1: Comparison of Alice Springs Hospital
Intensive Care Unit caseload with national data8,9
This prospective longitudinal observational pilot study was conducted in the ASH ICU, a regional medical and surgical ICU that has 200-250 admissions annually.
Participants
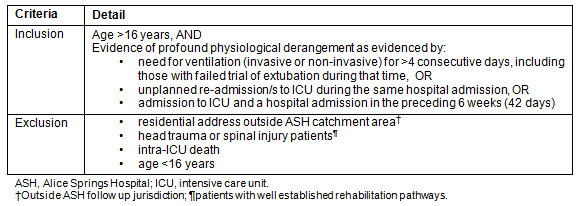
Patients admitted to the ASH ICU, and defined as high risk were prospectively recruited to the study when eligibility criteria were met (Table 2). There are little data identifying patients at risk for future morbidity, and the only factors associated to date are age and duration of ICU admission6. Profound respiratory disease or acute respiratory distress syndrome (ARDS) could be extrapolated as a risk factor7. We thus based our definition on both a time component (>4 days), a level of physiological derangement (requiring ventilation), or apparent untreated disease processes (ICU admission with preceding hospital admission). Recruitment to the study occurred between February and August 2009, with follow up occurring over the subsequent 6 months.
Table 2: Inclusion and exclusion criteria
Information regarding smoking status and a history of alcohol abuse was collected at the time of admission. Patients were considered to meet the criteria for alcohol abuse if there was a history of alcohol withdrawal seizures, documented liver disease (ultra-sound demonstrated evidence of fatty liver, cirrhosis, or endoscopically proven varicies with known portal hypertension) in the presence of alcohol use, more than two alcohol related emergency department presentations (assaults while intoxicated, gastrointestinal bleeding, alcoholic pancreatitis, aspiration pneumonia), or if the patient admitted to heavy alcohol ingestions. The ICU admission details including the primary reason for admission and admitting service (medical or surgical), and data regarding the patient's course during their ICU admission was recorded. Length of stay (LOS) for ICU was defined as the time period from ICU admission to ICU discharge, and hospital LOS was defined as the time from ICU admission to hospital discharge. At ASH all trauma patients are admitted under the general surgical service. Any documented intervention with a discharge planner was recorded. The patient's local clinic (as recorded in their medical records, or their local geographical clinic for rural Indigenous patients) was contacted at the time of their six-month review to ascertain the time to first local medical officer (LMO) review, and the presence or absence of a discharge summary in the clinic notes related to their index admission.
Assessment tools
Assessment tools included the Six Minute Walk Test (6MWT)10, and the Home And Community Care (HACC) functional assessment scale11 as a screen for functional disability.
The 6MWT has been well studied and is recognised as an easy, cheap, and well-tolerated assessment that produces a comparable measure, the six minute walk distance (6MWD). The 6MWD provides an indication of functional status, as well as predicting morbidity and mortality for heart or lung disease10,12, and reference equations exist that predict performance13. The 6MWT was conducted at hospital discharge and at 6 months under the supervision of a medical officer (primarily the first author).
The HACC functional assessment scale is used as a screening tool to indicate the need for further functional assessment11,14. It consists of a questionnaire that identifies deficiencies in functional status - either basic activities of daily living (BADL) including washing oneself, dressing etc, or domestic activities of daily living (DADL) including managing finances, medications, shopping etc. The questionnaire was administered by a medical officer (primarily the first author).
As crude measures of persisting morbidity, the number of hospital re-admissions required in the 6 months following ICU discharge were recorded, and at 6 months patients were asked whether they had returned to work.
Statistical methods
Median results are reported due to the small sample numbers. Variables were analysed using appropriate non-parametric tests (Statistica v10; Statsoft; Tulsa, USA).
Ethics approval
The study received ethics approval from the Central Australian Human Research Ethics Committee (#2009.09.02). Informed consent was obtained from patients prior to their discharge from the ICU.
The study cohort consisted of 18 of a potential 26 patients who met inclusion criteria between February and August 2009. Eleven (61%) were recruited on the basis of requiring invasive ventilation for more than 4 days. Details of inclusion and exclusion criteria are provided (Fig1).
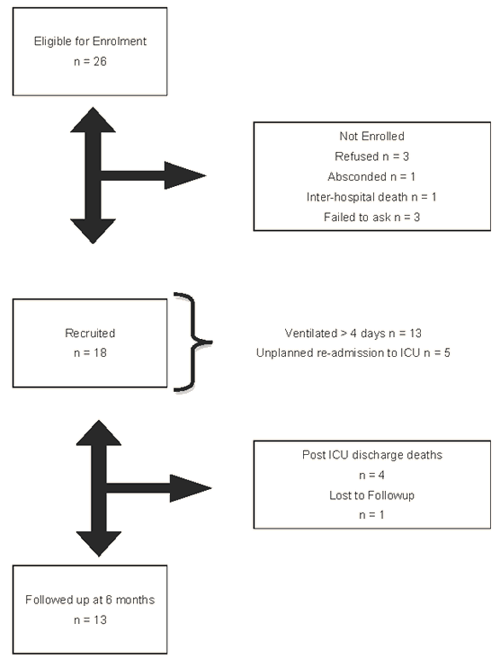
Figure 1: Cohort flow diagram.
Demographics
Patient demographics, ICU admission details and hospital course are presented (Tables 3,4). Fourteen (78%) of the cohort were Indigenous and all patients required emergency admission. Sepsis contributed to the admission reason in 13 (72%) of the cohort, and was the primary reason for admission in 8 (44%).
Table 3: Cohort demographics (N=18)
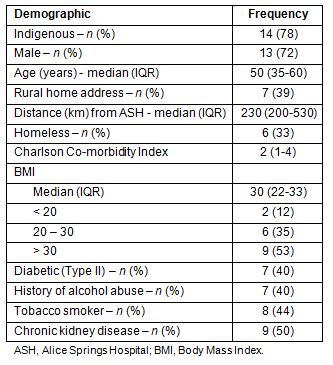
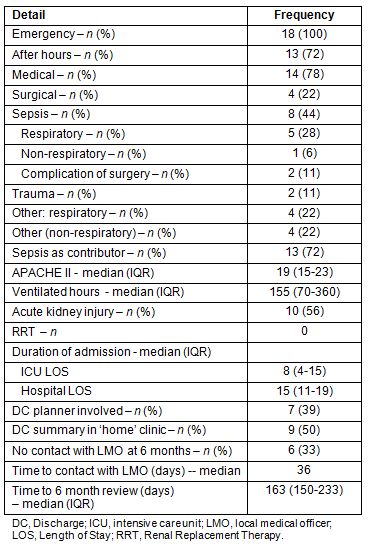
Table 4: Intensive Care Unit admission details and admission course
Follow up
One patient was lost to follow up, one patient had not been discharged from hospital 6 months following their ICU discharge and four patients died between hospital discharge and six-month review. Median time to six-month review was 163 days, and 237 days for the homeless sub-group (p=0.06). Nine patients had no record of a discharge summary in the case records at their home clinic, and one-third of the cohort had not been reviewed by their local medical officer (LMO) at 6 months, although four had died in that time period. Other details of the follow-up period are provided (Table 4).
Six-minute walk test
Data for six-minute walk distances (6MWDs) was available for 10 patients (four died between ICU discharge and 6 months, one was lost to follow up, two were unable to undertake the assessment (one due to blindness, one was paraplegic), and one patient refused. Six patients were able to complete the 6MWT at both time points. Median 6MWD and inter-quartile range (IQR) is depicted (Fig2). There was no significant improvement in distances achieved over the follow-up period (p=0.68) and the median 6MWD achieved at 6 months was significantly less than that predicted (p <0.05), with the distance completed being 44% of that predicted. When the analysis was repeated including only those patients able to completed the 6MWT at both time points, there was no substantial change in the outcome.
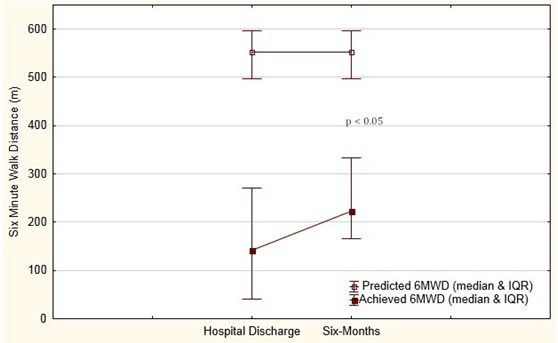
Figure 2: Six-minute walk distance (median & IQR).
Functional status
There was no significant change in BADL score between ICU discharge and hospital discharge (p=0.11), but a significant improvement in BADL score between ICU discharge and 6 months with median score increasing from 15.5 to 20 (p <0.05), with all patients except one who remained an inpatient at 6 months achieving a score consistent with full independence (Fig3). In contrast, DADL scores indicate persisting limitation in performing these tasks (Fig3). Median DADL score at hospital discharge was 18 (of a possible 30), with a non-significant improvement at 6 months to a median score of 25 (p=0.08).
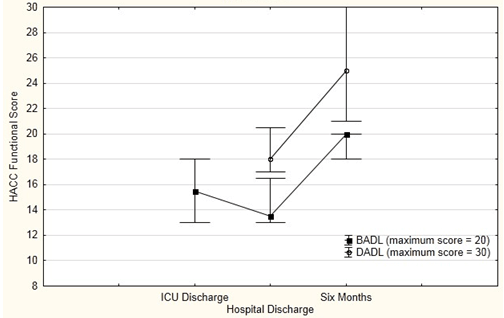
Figure 3: Home and community care functional score (median and IQR).
Morbidity
Twelve patients (66% of the cohort) required hospital re-admission, although none to ICU, and two-thirds of these had multiple re-admissions. Median time to first re-admission was 30 days (IQR 9-42).
Three of the cohort (all of whom were admitted under a surgical unit) had pre-morbid employment. At 6 months all had returned to work at least part-time.
Mortality
Four post-ICU deaths were recorded, all of which occurred after hospital discharge, producing an absolute mortality of 22%. All the deceased were Indigenous, and 75% were also homeless. Median time from ICU discharge to death was 72 days (IQR 34-133).
Discussion
This case series describes functional sequelae in a prospective cohort of patients thought to be at high risk for future morbidity. The data for this study was drawn from a larger pilot study examining the sequelae of an ICU admission, designed to evaluate the ability to identify and follow up a group of patients, the logistics involved in this task, the tools for assessment, and to quantify persisting morbidity, and mortality.
Those at 'high risk' - defined in this study as profound physiological derangement, as reflected in a need for invasive ventilation of greater than 4 days, or unexpected ICU admission in the setting of a recent preceding hospital admission - were relatively easily recognised. Recruiting these patients in a busy ICU setting with a reasonably high staff turnover proved to be problematic, and eight patients who met eligibility were not invited to participate. Despite this, the demographics of the cohort recruited are very similar to the usual ASH ICU population (Table 1). When compared with national data the cohort is more likely to be Indigenous, younger, and sicker, requiring emergency admission. Seven of the patients recruited (40%) had a rural home address with a median distance from ASH of 230 km, suggesting retrieval from their primary healthcare clinic was required. The corollary of this observation is that retrieval, by its very definition, results in a time delay in receiving treatment in an acute-care setting.
There was a high rate of medical admissions in the study cohort compared with national data8, and the high rates of admission associated with sepsis highlight the previously documented impact of infection and bacteraemia in the Central Australian population15. This was thought to reflect the high burden of chronic disease within the Indigenous population, and the challenging socioeconomic setting in which the homeless, in particular, live. However, it is also possible that this reflects, in part at least, the relatively low rates of high-risk surgery undertaken at the ASH.
Alcohol abuse, thought to be a significant contributor to morbidity, and known to contribute to mortality in the Indigenous population of Central Australia16, remained a feature with seven (40%) either admitting to, or displaying signs of alcohol abuse, even by the relatively strict definition used in this study. All were Indigenous, and all but one of those abusing alcohol were homeless.
The low rate of documented discharge planner involvement during the index admission was compounded by the low rate of discharge summary completion, and may explain the high re-admission rate.
One-third of the cohort had not been reviewed by their primary LMO at 6 months, yet two-thirds of this group had had a hospital re-admission, and had therefore undergone a medical 'review' of sorts. Furthermore, two of the deaths occurred in the group that had not received an LMO review, but both had been re-admitted at least once. This is consistent with local data demonstrating poor follow-up rates for chronic disease3, and also suggests the hospital is utilised as the point of primary care for some patients. There was not, however, any significant relationship between the presence of a discharge summary at the home clinic and patients' review status.
The slightly longer median time to follow up in the homeless subgroup compared with the rest of the group (237 and 161 days, respectively) was thought to reflect the increased difficulty locating this highly mobile and itinerant population.
Assessment tools
Cardiorespiratory: Completed 6MWDs at 6 months showed a persisting limitation in one or both of cardiorespiratory and physical functioning, with distances achieved significantly below that predicted13, and no improvement in achieved distance over the follow-up period. The percentage of (presumed) recovery fell below that of a cohort of post-ARDS patients in a large Canadian study7. Whether this reflects progression of a chronic disease process, or a sequelae of the index admission could not be determined from these data.
Functional status: It was reassuring that median scores on the HACC BADL questionnaire suggested full independence in the basic activities of daily living at 6 months, while the small, non-significant deterioration between ICU and hospital discharge was attributed to the change in nursing ratio. However, the failure to attain a median score approaching full independence for DADL suggests scope for further allied health input into this group of vulnerable patients. The HACC scale used in this study is a screening tool, and in the normal course of events a failure to attain a full score on two or more of the DADL subscales would prompt a referral for formal assessment. As such 11 (62%) should have been referred for formal functional assessment, yet to the best of our knowledge only one patient received allied health input.
Other morbidity
The total number of hospital re-admissions was higher than that seen in a post-ARDS cohort7. The high rate of re-admission was thought to represent a number of compounding factors, including the absence of a discharge summary at the local primary treating clinic, the relatively low rates of LMO follow up, and the absence of documented discharge planning involvement, in addition to the burden of chronic disease.
Use of return to work rates as a marker of morbidity had questionable utility in this population, with only three of the cohort (all surgical patients) employed pre-morbidly.
Mortality
There were four deaths in the cohort, a mortality rate of 22%, substantially higher than that found in a large New Zealand trial investigating mortality rates following ICU admission17, although the numbers in the present study were small enough for this to have been the result of chance. All deaths were among Indigenous patients, and three of the four (75%) were homeless, producing an absolute mortality rate in the homeless subgroup of 50%. Furthermore, no deaths occurred during the index admission, median time to death was 73 days following ICU discharge, and those who died were a median age of 54 years.
Limitations
This was a study designed to test the feasibility and logistics for a larger scale prospective study, and to assess the tools for assessment. As such, issues pertaining to small numbers are a limitation. Compounding this, a relatively high proportion of patients (n=8) were not recruited despite meeting eligibility criteria. The small number recruited also means that confounders, such as the effect of a medical or surgical primary diagnosis could not be accounted for. Other limitations include the use of a prediction formula which is based on non-Indigenous data, and which has not, despite being widely used in such a setting, been validated in a post-ICU population13. In addition, there was no attempt to estimate pre-morbid exercise tolerance. Despite this, the authors believe that important morbidity data relating to rural patients were derived, and that these data warrant wider dissemination to act as an impetus for further research
This study confirms that there is persisting morbidity in a group of high-risk, predominantly Indigenous ICU patients who survive their index admission. Although there are inherent problems in following up a highly mobile and itinerant population - a fact that will be known to many who have worked in Indigenous health - it shows that follow up is both feasible and valuable. This research provides the groundwork for a prospective comparative multicentre study to better quantify these deficits, compare them with other cohorts, and to suggest interventions to reduce this burden of morbidity. Such a study is warranted on the basis of the present results.
References
1. Australian Bureau of Statistics. Experimental Estimates and Projections, Aboriginal and Torres Strait Islander Australians. Canberra, ACT: Australian Bureau of Statistics, 2009.
2. Preventable Chronic Disease Educators. Preventable Chronic Disease Baseline Data Report 2009/10. Alice Springs, NT: Department of Health and Families, Unit CAHD; 2010.
3. Brown A. Acute coronary syndromes in indigenous Australians: opportunities for improving outcomes across the continuum of care. Heart, Lung and Circulation 2010; 19(5-6): 325-336.
4. Australian Institute of Health and Welfare. Australia's Health 2008. Canberra, ACT: AIHW, 2008.
5. Australian Institute of Health and Welfare. The health and welfare of Australia's Aboriginal and Torres Strait Islander people, an overview 2011. Cat no. IHW 42. Canberra, ACT: AIHW, 2011.
6. Desai SV, Law TJ, Needham DM. Long-term complications of critical care. Critical Care Medicine 2011; 39(2): 371-379.
7. Herridge MS, Tansey CM, Matte A, Tomlinson G, Diaz-Granados N, Cooper A et al. Functional disability 5 years after acute respiratory distress syndrome. New England Journal of Medicine 2011; 364(14): 1293-1304.
8. Drennan K, Hart G, Hicks P. Intensive Care Resources and Activity: Australia & New Zealand 2006/2007. Melbourne, VIC: ANZICS, 2008.
9. Hatch F, Wyatt M. Alice Springs Hospital Intensive Care Unit 2007 ICU/HDU Statistics. Alice Springs, NT: Alice Springs Hospital, 2008.
10. Enright PL. The six-minute walk test. Respiratory Care 2003; 48(8): 783-785.
11. Green J, Eager K, Owen A, Rob G, Quinsey K. Towards a Measure of Function for Home and Community Care Servives in Australia: Part 2 - Evaluation of the Screening Took and Assessment Instruments. Australian Journal of Primary Health 2006; 12(1): 82-90.
12. Solway S, Brooks D, Lacasse Y, Thomas S. A qualitative systematic overview of the measurement properties of functional walk tests used in the cardiorespiratory domain. Chest 2001; 119(1): 256-270.
13. Enright PL, Sherrill DL. Reference equations for the six-minute walk in healthy adults. American Journal of Respiratory and Critical Care Medicine 1998; 158(5Pt 1): 1384-1387.
14. Department of Health and Aging. National Program Guidelines for the Home and Community Care Program. Canberra, ACT: Department of Health and Aging, 2007.
15. Einsiedel LJ, Woodman RJ. Two nations: racial disparities in bloodstream infections recorded at Alice Springs Hospital, central Australia, 2001-2005. Medical Journal of Australia 2010; 192(10): 567-571.
16. Senior K, Chenhall R, Ivory B, Stevenson C. Moving Beyond the Restrictions: The Evaluation of the Alice Springs Alcohol Management Plan. Darwin, NT: Menzies School of Health Research, 2009.
17. Hicks PR, Mackle DM. Cause of death in intensive care patients within 2 years of discharge from hospital. Critical Care Resuscitation 2010; 12(2): 78-82.