Cardiovascular disease is the leading cause of death in the UK with 88 000 deaths per year the result of coronary heart disease1. The acute coronary syndromes (ACS) includes ST-elevation myocardial infarction (STEMI), non-ST-elevation myocardial infarction (NSTEMI) and unstable angina2. There is increasing evidence to support an early invasive approach to the investigation and management of these patients3, with percutaneous coronary intervention (PCI) being the main method of coronary revascularisation in ACS4-8.
Historically, PCI centres collocated with cardiothoracic surgical services, due to the need for emergency coronary artery bypass graft (CABG) following PCI. However, the need for emergency CABG related to PCI procedures is now less than 0.01%; thus, an increasing number of PCI services are in 'non-surgical' centres3. Local PCI provision may have advantages for the organisation of cardiac services and may improve access to invasive cardiac investigation. For example, evidence indicates distance from a catheter lab is inversely proportional the number of patients who receive PCI9,10.
In May 2010, a PCI service facility was introduced at Raigmore Hospital, Inverness. This location made it the most remote PCI service in the UK. The unit was set up with existing staff: two interventional cardiologists and two non-PCI cardiologists. The service was initially was delivered during limited hours (09.00 and 12.00 on four mornings per week). Prior to this new service, only diagnostic coronary angiography could be undertaken at Raigmore and, hence, the vast majority of patients requiring ACS investigation had to be transferred to one of three out-of-region centres. Such transfers inevitably involved treatment delays due to bed availability in tertiary centres, travel times (between 2.5 and 4 hours) and waiting time for transport.
Furthermore, these delays may have resulted in a more conservative approach to coronary disease. Not all patients who may benefit from an angiogram and angioplasty were necessarily referred. Previous studies have convincingly shown that geographical isolation from angiography and angioplasty services has been associated with less use of these services9,10. Indeed, historically NHS Highland had a low intervention rate and high CABG:PCI ratio (local data).
The introduction of a local PCI service would potentially lead to a larger proportion of patients from the Highlands being appropriately investigated and receiving timely revascularisation with PCI. Such improvements would have a knock-on impact of reducing bed usage, with potential cost savings. This study thus aimed to assess the impact of this new PCI service on coronary stenting, length of stay and inter-hospital transfers.
Study design
The study was an observational study comparing the treatments and outcomes of patients pre- and post-introduction of a local PCI service. These two groups were compared in respect to their age and sex composition, to assess whether outcomes might differ for reasons other than access to a local PCI service. The groups were then compared in terms of likelihood of receiving PCI, length of stay and proportion requiring transfer to another hospital.
Setting
Raigmore Hospital is a 600 bed regional centre serving the population of the Highlands of Scotland (approximately 210 000 people). It covers a large rural area (33 000 km2) with considerable travel times from patient residences to hospital. Within the region there are two district general hospitals, a rural island hospital and several community hospitals.
Patient selection
The pre-PCI initiative group was made up of consecutive patients admitted to Raigmore Hospital with an ACS during a 12 week period immediately before the introduction of the new PCI service. The post-initiative group was made up of consecutive patients admitted also with an ACS but during a 12 week period shortly after the implementation of the new service. A two-week implementation phase was excluded from analysis, as this included a small number of mainly elective PCI patients.
Data on all patients coded for an ACS during the above time periods were requested. International Classification of Diseases (ICD)-10 codes were used to identify patients eligible for inclusion, specifically I21.4 (NSTEMI), I21 and I22 (STEMI), and I20.00, I20.02, I20.09 (unstable angina). Those with an ICD code of I20.9 (angina, unspecified) were excluded, as it could not be verified if these were true ACS or, and more likely, chronic stable angina. Only the first two coding positions were included to ensure that the cardiac diagnosis was the precipitating reason for admission.
Data handling
All duplications (some patients had been entered twice in the patient administration system for the same admission) and those not discharged within the two time periods were manually excluded. The regional electronic patient administration system, electronic immediate discharge letters, catheter lab reports and discharge letters were used to identify where patients were transferred to and when they were discharged.
Statistical analysis
All data was entered into SPSS Version 19 ((SPSS Inc; www.spss.com). The age and gender composition using a t-test and χ2 test to assess whether differences in treatment or outcomes identified might be due to sociodemographic differences. Cardiac diagnoses were compared between groups using a χ2 test.
Management pre- and post-service implementation was then compared, using a χ2 test to assess if patients were more or less likely to be treated invasively. A second χ2 test was then used to assess if specific treatment of those treated invasively differed, specifically whether an angiogram only, PCI or CABG were utilised.
Finally, differences in outcomes were examined. Proportions who died during the period of the study were compared using a χ2 test, as were proportions requiring transfer to another hospital. Mann-Whitney tests were used to assess differences in time to PCI, and to compare length of hospital stay between the two groups.
Ethics approval
This is a retrospective review of service provision utilising data already collected as part of clinical care and therefore did not require ethical approval.
Patient characteristics
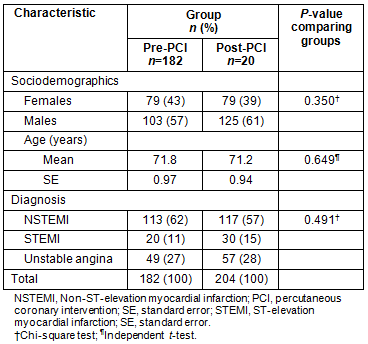
An overview of the sociodemographic composition of the two groups and their cardiac diagnosis is provided (Table 1). There were 182 patients in the pre-PCI group and 204 patients in the post-PCI group. Comparison of the two groups indicates them to be very similar, with no statistically significant differences in terms of age, gender or cardiac diagnosis.
Table 1: Participants' characteristics
Invasive versus conservative ACS treatment
An overview of the management of patients pre- and post-service introduction is given (Table 2). The proportion of patients treated non-invasively was similar in the pre- and post-PCI groups (49% pre vs 53% post, p=0.428).
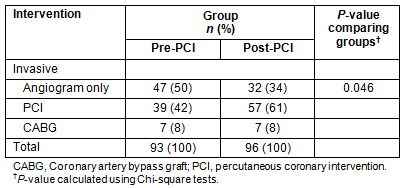
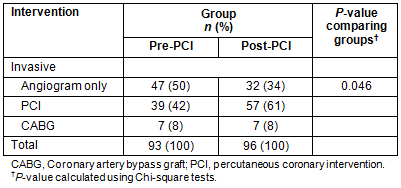
However, evidence is provided of a difference in the management of those treated invasively (Table 3). Patients admitted post-introduction of a local PCI service were more likely to have PCI (61% vs 42%) and less likely to receive an angiogram only (34% vs 51%), with proportions receiving CABG remaining largely unchanged (8% before and after). The difference in management of those treated invasively was statistically significant (p=0.046).
Table 2: Medical management of participants
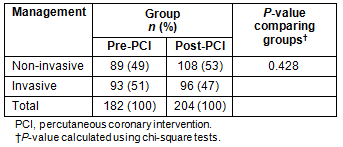
Table 3: Intervention utilised with participants treated invasively
Time to PCI
Findings are shown for the specific outcomes on which this article focuses (Table 4). A date of PCI was available for 21 patients in the pre-PCI group (54% of those receiving PCI) and 37 patients in the post-PCI group (65% of PCI patients). Median time to PCI prior to the introduction of the new service was 10 days. However, after the introduction of the service, the equivalent figure was only 5 days, a reduction of 50%. This reduced time to PCI was statistically significant (p=0.002).
Table 4: Outcome of percutaneous coronary intervention
Hospital transfers
As also shown in Table 4, prior to the implementation of the new service, 75 patients (41%) were transferred compared with 43 patients (21%) after its introduction. This reduction was also highly significant (p<0.001). Furthermore, Cramer's V (0.22) indicated a moderate association between hospital transfers and the introduction of the PCI initiative.
Length of hospital stay and bed utilisation
The total length of stay for those patients treated invasively was reduced following the introduction of the local PCI service (median 8 vs 6 days, p=0.017; Table 4). Comparison of the total number of bed days showed the pre-PCI period of 1097 days was reduced to 870 days after the PCI service was in put in place.
Discussion
This study reports the impact of establishing a new PCI service in a remote region on the invasive management of patients with ACS. Despite the limited working hours of the new PCI service, the study has demonstrated a considerable reduction in delays for inpatient PCI, reduced length of stay and fewer transfers to out-of-region tertiary centres. There was a modest increase in the proportion of patients receiving PCI, although many continue to be treated conservatively with no inpatient angiography. The pre- and post-PCI groups were very closely matched in terms of sociodemographics and cardiac diagnosis, and therefore it is highly likely that the changes seen were the result of the availability of a local PCI service.
There are several potential advantages of a local service in terms of efficiency and reduced travel times. Providing more local access to such facilities may help overcome the recognised barrier that exists for patients who are treated at a distance from a catheter lab9,10, with results comparable to those of larger centres11.. In this study there was no change in the proportion of patients who received a coronary angiogram, probably as coronary angiography has been well established on-site for over 10 years. However, the development of a new PCI service increased the proportion of patients who subsequently received PCI and reduced the proportion of patients being referred for CABG (albeit small numbers). This is not surprising and somewhat encouraging, as prior to the PCI service, there was a higher than average CABG:PCI ratio in our area (local data).
Delays to PCI
With the emphasis placed on early coronary revascularisation, this PCI service has succeeded in reducing the wait for PCI. However, a significant proportion of patients still waited more than the maximum recommended time of 72 hours for an inpatient angiogram, demonstrating an unmet need and on-going insufficient service provision to meet demand. Given that approximately 70% of our patients were admitted to the same hospital as the new PCI service, this appears to reflect a lack of available capacity in the catheter laboratory rather than patient transfer or bed capacity issues.
Impact on hospital transfers
The number of transfers to an out-of-area centre was reduced dramatically. With further improved local access to PCI it would be envisaged that a greater number of patients could be treated locally. However, without a service that is not restricted in operational hours, it is likely that a proportion of patients would still require transfer to other out-of-region centres, and that transfer of inpatients for cardiac surgery would still be required.
Length of hospital stay
In this study, the introduction of a PCI service reduced the median length of hospital stay by 2 days. The total network bed days were significantly reduced. However, the total number of bed days spent at the new PCI centre was not, and there was actually a small increase with the introduction of a PCI service. Although many patients were treated more rapidly at the new centre, with a reduction in length of stay, others patients previously transferred to other centres on day 1 of their admission had been repatriated and treated locally. Thus, the vast majority of bed savings were seen in out-of-region tertiary centres.
However, the additional benefits to the patient of a local PCI service cannot be overemphasised. As well as avoiding long travel times, it avoids attending unfamiliar hospitals in a new city with different doctors at a time when patients are most vulnerable. It is also more convenient for families to visit. Furthermore local service level agreements would allow some repatriation of finance as a result of fewer referrals to the regional centre. There are also savings in ambulance service and the need for hospital staff to escort patients on long journeys.
Safety
The Highland initiative would suggest that PCI services in major surgical centres are an effective means for managing patients with ACS. Furthermore, New PCI services in other non-surgical centres have been shown to be safe and effective2,3,12. However, small-volume centres and operators appear to have less favourable results, and thus guidelines exist with minimum thresholds for new PCI centres in terms of the centre (≥400 PCI per year) and operator (≥75-150 PCI per year)13. Thus, a critical mass of PCI cases is required to safely support a local service, and on-going clinical review is required to ensure safety. Our centre reports to the national PCI database and results are comparable with national averages. Indeed, although the numbers are small there was a non-significant reduction in death rate following the introduction of the PCI service. No patient was transferred for emergency CABG following PCI.
Limitations
It may be that the extreme geographical challenges faced in our area have resulted in more dramatic results than may be expected where existing PCI centres are not so distant. Nevertheless there are areas in other countries that have similar geographical challenges to the North of Scotland, and our findings may help guide service development in such areas. Delays to hospital admission are also likely to be a feature of hospitals even in areas with a less-dispersed population and thus PCI centres similar to the Highland initiative may be worth consideration in less remote areas. Furthermore, this study was performed over a relatively short period of time and it might be expected that the results would be more marked as internal referral pathways become more fully established. Due to the short time frame it was not possible to report subsequent reductions in admission with recurrent MI.
Current guidelines suggest an early invasive approach to the management of ACS with a particular emphasis on early follow-on PCI. The Highlands of Scotland have traditionally been underprovided for in terms of invasive cardiac facilities. The introduction of a local service did not increase the proportion receiving an angiogram as part of the inpatient management of their ACS, but it did result in a greater proportion of patients receiving PCI. Patients received PCI more quickly and spent less time in hospital. Although the number of transfers was reduced they were not diminished completely. Patients will still need to be transferred for cardiac surgery and out of hours PCI, as providing 24/7 access to PCI in a small centre is challenging. Maintaining links with other regional centres and clear patient pathways are necessary to provide optimal ACS care to patients in rural areas.
References
1. British Heart Foundation. Statistics Website. Coronary heart disease statistics 2010 edition. London: British Heart Foundation, 2010. Available: http://www.heartstats.org/datapage.asp?id=9075 (Accessed 1 December 2010).
2. Hillis GS. Management of stable angina and unstable angina/non-ST-elevation myocardial infarction. Medicine 2006; 34: 181-187.
3. Kelly D, Sinha M, Swallow R, Levy T, Radvan J, Rozkovec A, Talwar S. Percutaneous coronary angioplasty in a district general hospital: safe and effective - the Bournemouth model. British Journal of Cardiology 2008; 15: 244-246.
4. Scottish Intercollegiate Guidelines Network. SIGN 93. Acute Coronary Syndrome. Edinburgh; 2007; 7414.
5. Bassand JP, Hamm CW, Ardissino D, Boersma E, Budaj A, Fernández-Avilés F et al. Guidelines for the diagnosis and treatment of non-ST-segment elevation acute coronary syndromes. European Heart Journal 2007; 28: 1598-1660.
6. Van de Werf F, Bax J, Betriu A, Blomstrom-Lundqvist C, Crea F, Falk V et al. Management of acute myocardial infarction in patients presenting with persistent ST-segment elevation. European Heart Journal 2008; 29: 2909-2945.
7. Hoenig MR, Aroney CN, Scott IA. Early invasive versus conservative strategies for unstable angina and non-ST-elevation myocardial infarction in the stent era (Review). Cochrane Database of Systematic Reviews (Online) 2010; 3: CD004815.
8. Silber S, Albertsson P, Avilés FF, Camici PG, Colombo A, Hamm C et al. Guidelines for percutaneous coronary intervention. European Heart Journal 2005; 26: 804-847.
9. Leslie SJ, Henriksen PA, Timlin H, Stanton T, Spratt JC, Denvir MA. Urgent in-patient coronary angiography: a comparison of centres with and without cardiac catheter facilities. Scottish Medical Journal 2006; 51: 24-26.
10. MacLeod MCM, Finlayson AR, Pell JP, Findlay IN. Geographic, demographic, and socioeconomic variations in the investigation and management of coronary artery disease in Scotland. Heart 1999; 81: 252-256.
11. Brown DC, Mogelson S, Harris R, Kemp D, Massey M. Percutaneous coronary interventions in rural hospital without surgical back up: report of one year experience. Clinical cardiology 2006; 8: 337-340.
12. Smith LDR, Spyer G, Dean JW. Audit of cardiac catheterisation in a district general hospital: implications for training. Heart 1999; 81: 461-464
13. British Cardiovascular Intervention Society. Statement on the development and peer review of new PCI services. (Online) 2011. Available: http://www.bcis.org.uk/resources/BCIS_New_Site_Guidance_31012011.pdf (Accessed 3 February 2012).

