The majority of Australians reside in urban areas, with only one-third of the population (34%) residing in rural or remote regions1. Non-urban residents have been reported to have poorer health status than those living in urban areas2, and health status has been observed to decline with increasing remoteness1. Distance presents an enormous challenge to health-service providers in rural and remote Australia. Health professionals in such areas may be required to provide services to relatively small populations with significant healthcare needs, across large and diverse geographical regions3.
Past research has shown that pharmacists, like most other health professions, have been under-represented in rural and remote regions4. Data from 2006 reported that the national Australian pharmacist workforce comprised 15 539 pharmacists. The average age of the pharmacist workforce is 40 years, and the majority work in urban environments5. In addition, many remote communities are without a pharmacist, and rely on other health professionals such as the local general practitioner, registered nurse6, Aboriginal Health Worker or the Royal Flying Doctor Medical Chest7 for medication supply. Limited access to pharmacists and pharmacy services may be contributing to the health inequities experienced by rural and remote Australians.
There have been a number of initiatives to increase the number of pharmacists working across all areas of Australia. In particular these initiatives have implications for the number of pharmacists working in non-urban areas. Initiatives have focused in two areas: increasing the pharmacy workforce, and providing incentives for pharmacists to work outside major urban centres. The number of pharmacy schools in Australia has doubled over the past 10 years8 and pharmacy schools in regional Australia have been established. The Rural Pharmacy Programs, funded by the Australian Government, have also been implemented to address workforce shortages. This program comprises various initiatives designed to recruit, train and retain pharmacists in rural and remote areas, to encourage pharmacists to establish pharmacies and work outside of urban centres.
Although these initiatives have been established, there is limited information on the current pharmacy workforce, in particular on the distribution of the rural and regional pharmacy workforce and what are the drivers and barriers for rural and remote pharmacy practice.
Research aim
The aim of this research was to explore and describe the current non-urban pharmacy workforce and to identify barriers and drivers to rural and remote pharmacy practice. The specific objectives of the study were to:
- Describe the demographics and professional roles of the rural and remote registered pharmacist workforce in Australia.
- Explore factors that may affect the rural and remote pharmacist workforce, such as pharmacy education, rural background and professional satisfaction, as well as the drivers and barriers that influence pharmacists to practise in rural and remote areas.
A mixed-methods approach was used, comprising a qualitative national consultation, a quantitative rural/remote pharmacist workforce survey and a literature review.
National consultation process
The aim of the national consultation process was to identify themes, barriers and facilitators relevant for rural and remote pharmacists to inform the development of the national survey.
Semi-structured interviews (n=83) and focus groups (n=15, 143 participants) were conducted throughout Australia in 2009. A convenience sample of participants was identified from a number of stakeholders with an interest in rural and remote pharmacy, practising rural/remote pharmacists, pharmacy academics, as well as representatives from peak pharmacy organisations. The research team identified potential participants. Snowball sampling was used to recruit further participants to the study to ensure a diverse range of views. The study was advertised in national pharmacy online and print media to further target potential participants. Interviews and focus groups followed a pre-defined interview schema and were conducted by members of the research team. The interviews and focus groups were digitally recorded and transcribed verbatim. Common themes were identified and collated by all members of the research team.
Rurality
Rurality was defined using the Rural, Remote and Metropolitan (RRMA) classification9. Rural and remote practice was defined as all RRMA classes excluding class 1 (capital cities) and class 2 (other metropolitan); that is, RRMA classes 3-7. Although a pharmacy-specific geographical classification system, The Pharmacy Access/Remoteness Index of Australia (PhARIA)10, exists, this system classifies regional centres with more than 9 pharmacies in the same category as major metropolitan cities, irrespective of their geographical location or access to other facilities, and was therefore not considered suitable for this study.
Rural/remote pharmacist workforce survey
Based on the findings of the qualitative work and the literature review, a 45-item survey was developed to further explore the relevance of the issues identified in the qualitative consultation. The survey comprised a combination of Likert scale questions, closed ended categorical questions and open-ended free-text questions. A five-point Likert scale was used to explore professional satisfaction (24 items) and personal satisfaction (11 items). Respondents were asked to indicate the extent of their agreement with these statements in relation to their current pharmacy practice. Items with mean scores of 4 and over, and an agreement level greater than 80% between like items, were classified as 'satisfiers'. Items with means scores less than 3, and agreement levels less than 35%, were seen as potential 'dis-satisfiers'. Agreement levels for satisfaction/dissatisfaction were determined by consensus within the research team.
Free-text responses were used to identify barriers and drivers for rural practice. The draft survey was piloted by 14 rural pharmacists and changes identified during piloting were incorporated into the final survey design.
All registered pharmacists practising in non-urban locations (RRMA 3-7, n=3300) were identified from a commercial mailing list. Pharmacists were invited to participate in the study and sent a paper-based copy of the survey in April 2009. Once invalid addresses were excluded, the final number of registered pharmacists invited to participate in the study was 2783.
The invitation to participate also included a link to an on-line version of the study to allow participants to elect the medium in which they completed the survey. A de-identified code was used to ensure that each participant only completed one survey, either paper-based or online. To increase the participation rate, the pharmacist survey was also advertised in electronic and print-based pharmacy media.
Analysis
Data from the national survey was entered and analysed in Statistical Package for the Social Sciences (SPSS) version 19 (SPSS Inc; www.spss.com) . Data entry was double checked by an external person. Likert scale responses were analysed as linear variables11, and differences in mean scores between more-accessible (RRMA 1-3) and less-accessible (RRMA 4-7) respondents, and between hospital and community respondents, tested using t-test adjusted for non-equal variances to allow for disparate sample sizes. Free-text responses were collated and common themed by the research team to identify drivers and barriers.
Ethics approval
Ethics approval for the study was granted by Charles Sturt University Human Research Ethics Committee (2009/054).
National consultation process
Two hundred and forty-two participants took part in the qualitative national consultation. Within this group, 26 semi-structured interviews and 7 focus groups (89 participants) were held with practising rural pharmacists. Eight focus groups (54 participants) held with pharmacy students and 57 semi-structured interviews held with pharmacy education stakeholders (rural pharmacy academics, university placement coordinators, university heads of pharmacy schools).
The following main themes were identified from the qualitative process:
- Issues associated with increases in the pharmacy workforce.
- Need for rural/regional pharmacy schools to ensure ongoing rural pharmacist workforce.
- Perceptions regarding differences in professional roles between urban/non-urban pharmacists.
Issues associated with increases in the pharmacy workforce: Some concerns regarding a national oversupply of pharmacists were raised during the consultation process. Pharmacists working in remote areas were still experiencing pharmacist shortages; however, in regional and coastal areas the increased numbers of graduates appeared to be forcing new graduates out to rural areas. Pharmacists reported a positive impact on the availability of new staff, as well as on the opportunities to employ locum pharmacists.
Need for rural or regional pharmacy schools to ensure ongoing rural pharmacist workforce: The establishment of regional pharmacy schools in NSW, Queensland and Victoria was seen as an important factor supporting the rural/remote workforce. Participants felt that country students were more likely to return to rural communities if they had attended a regional pharmacy school.
Perceptions regarding differences in professional roles between urban and non-urban pharmacists: The professional roles of rural and remote pharmacists appeared to differ, depending on sector, pharmacy role and rurality. Rural hospital pharmacists reported having a very generalist role, more frequent on-call demands, and higher-quality relationships with medical staff than their counterparts in larger regional centres. Rural community pharmacists reported more regular and closer relationships with customers, often being the first point of contact; better quality relationships with GPs; feeling more respected by their customers for the professional roles they performed; and were also less competitive regarding market share than their urban colleagues. They reported higher workloads; spending more time on medication supply and less time in providing professional services, education, health promotion and business management, than urban hospital pharmacists.
National rural/ remote pharmacist survey
Over 650 pharmacists participated in the Rural/remote Pharmacist Survey (n=652), giving a response rate of 23.4% (n=652/2783). The majority of participants (83.0%, n=541) completed the paper-based survey. Forty-eight responses contained inadequate data for analysis and were excluded, giving a final response from 604 participants.
Respondent demographics
Mean pharmacist age varied with rurality. Overall, the mean age of respondents was 55.8 years. Those practising in remote areas were predominantly older pharmacists (47.4% n=309/643, >55 years) or younger pharmacists (26.3% n=169/643, under 35 years). Comparing the age distribution of respondents with that of all Australian pharmacists showed that rural/remote pharmacists were older than the current national pharmacy workforce (Fig1).
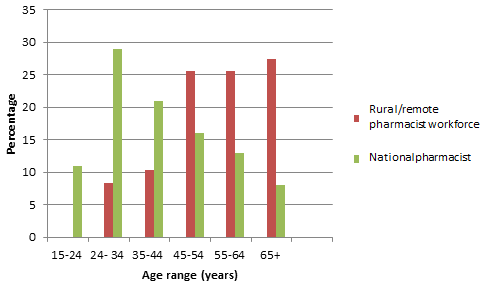
Figure 1: Age distribution of the rural/remote workforce
compared to the national pharmacist workforce. Data source5.
Respondents were predominantly of Australian origin (89.5%, n=583/652), with those born overseas coming from the United Kingdom (4.3%, n=28/652) or New Zealand (1.5%, n=10). More than half (55%, n=358/652) had a rural background, 46.7% (n=304/652) had a spouse with a rural background and, significantly, 60% (n=391/652) reported living outside a capital city during their childhood. Respondents' primary pharmacy qualifications were at undergraduate level (95.0%, n=619/652) of whom only 27.7% (n=181/652) reported holding post-graduate qualifications.
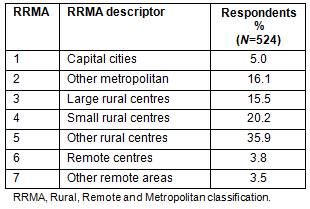
The majority (79%, n=414/524) of respondents lived in the higher population density states NSW (35.1%, n=184/524), Victoria (22.7%, n=119/524) and Queensland (22.5%, n=118/524). The distribution of respondents by rurality is shown in Table 1.
Table 1: Respondents according to their RRMA classification
Rural/remote pharmacist professional roles
The majority of survey respondents were community pharmacists (65.7%, n=428/652) with just over 10% working as hospital pharmacists (11.4%, n=74/652). Surprisingly 12.5% of the sample identified their primary role was as a locum pharmacist (n=82/652). The remainder worked as a hospital pharmacy manager (3.4%,) as an academic (1.1%), as facilitator for either the Medication Management Review or for the National Prescribing Service, or in other areas of pharmacy practice.
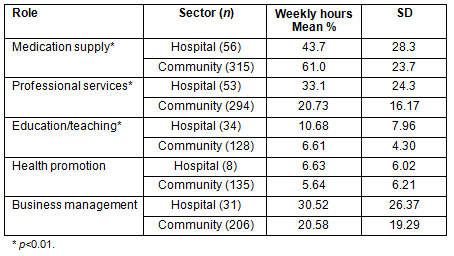
Over one-third (37.7%, n=198/524) of respondents reported working more than 40 hours per week, and of these 13.9% (n=73/524) reported working over 51-60 hours per week. Several significant differences emerged between community and hospital pharmacists when respondents were asked to specify the proportion of weekly hours allocated to different tasks (Table 2). Hospital pharmacists reported they spent significantly more time on the delivery of professional services and education and teaching, and less time on medication supply than pharmacists working in the community sector. Not surprisingly, within the community pharmacy sector, employees undertook significantly more medication supply (70.0% weekly hours) than owners (54.3 % weekly hours, p<0.01), and owners carried out significantly more business management (22.5% weekly hours) than employees (11.3 % weekly hours, p<0.01).
To determine if geographical location had an impact on professional roles, the weekly hour allocation was compared for pharmacists in more accessible locations (RRMA 1-3) with those in less accessible locations (RRMA 4-7). Pharmacists in more accessible regions spent a significantly higher proportion of their time on education and teaching (13.5 hours per week) than respondents in more remote regions (8.2 hours per week, p>0.05).
Table 2: Proportion of time per week allocated to key
professional tasks (% weekly hours) according to sector
Professional satisfaction
Professional satisfaction was measured by asking respondents (n=389-558) to indicate the extent of their agreement with 24 statements about their current pharmacy practice, on a five-point Likert-scale. Rural/remote pharmacists were generally found to be satisfied with their current role. The main 'satisfiers' were task variety, being appreciated by customers, ability to use advanced skills, appropriate remuneration, happiness in the work location, sound relationships with other pharmacists, a happy team and relationships with other health professionals (Table 3).
Table 3: Mean levels of satisfaction with aspects of current pharmacy practice
(n= 389-558) on a scale of 1-5 (1=strongly disagree, 5=strongly agree)
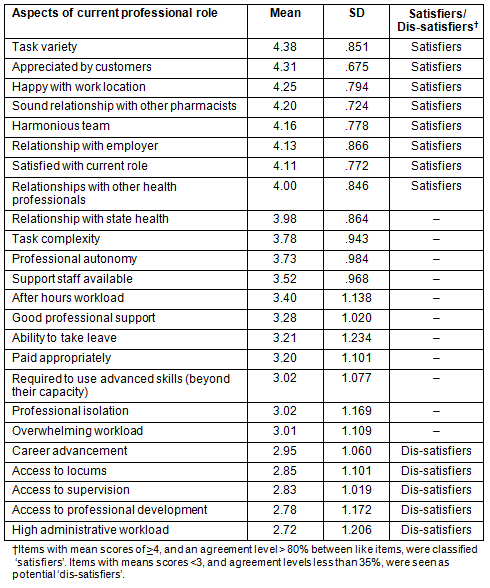
Dis-satisfiers could be classified as professional or personal. The main professional dis-satisfiers were high workload, lack of career advancement, limited access to locums, limited access to supervision, limited access to professional development, high administrative workload, inability to take leave, solo practice and professional isolation.
A number of personal satisfiers/dis-satisfiers were also identified. When compared with respondents in more accessible areas (RRMA 1-3), rural/remote respondents (RRMA 4-7) were significantly more satisfied with their connection to the local community outside of work (mean score RRMA 1-3 =3.94 vs RRMA 4-7 =4.26, p<0.05); their access to quality education for their children (mean score RRMA 1-3 =4.31 vs RRMA 4-7 =3.54, p<0.05); and their access to quality housing (mean score RRMA 1-3 =4.10 vs RRMA 4-7 =3.72, p<0.0).
Drivers and barriers influencing rural/remote pharmacy practice
To ascertain the drivers for rural practice, survey respondents were asked to list, as a free-text response, the three major reasons they decided to practise outside a capital city. Responses were collated and common themed by the research team to identify drivers and barriers.
The main drivers to rural and remote pharmacy practice were overwhelmingly lifestyle and quality of life; rural background; business and job opportunities, as pharmacies were seen as more affordable; family reasons to meet partner's needs or to return their family to a rural region; professional satisfaction and relationships with customers and health professionals.
The main barriers to rural and remote pharmacy practice were an inability to achieve a better work-life balance, spouse employment, children's education, career advancement, workload demands, securing a higher income, conflict in the workplace, or dissatisfaction with current practice or rural life.
Respondents were asked to identify strategies that could encourage retention of rural/remote pharmacists. Responses included higher remuneration, promoting the advantages of rural life, increased financial incentives, suitable accommodation, better work opportunities for their spouses, adequate locum support and improved access to professional development.
Discussion
The findings of this study highlight the diversity of the rural/remote pharmacist workforce. Rural/remote pharmacists work across a wide range of areas of diverse rurality and remoteness, in different pharmacy sectors and within different roles within these sectors. Despite this great diversity, a number of common elements were identified which characterize the rural and remote pharmacist workforce.
In the qualitative consultation, the impact of the national increases in the total number of pharmacists was an important consideration. Participants were aware of the rapid increase in the number of Australian pharmacy schools, and reported that the increased workforce was having a positive impact on the recruitment of pharmacists to most rural and regional areas. It was interesting to note that the establishment of regional pharmacy schools was seen an important contributor to the rural/remote pharmacist workforce. This was not for the training in rural/remote practice but the general assumption that rural background students attending regional pharmacy schools were more likely to practise in a rural or remote area once registered as a pharmacist. There is some evidence that students who train in a regional setting intend to work in a non-urban environment12; however, longitudinal tracking studies are needed to determine if this intention translates into practice. Rural background emerged as a key factor in determining whether or not a pharmacist chose rural or remote practice. Additionally, a substantive movement of rural pharmacists from one rural location to another was identified, but this shift was not being captured in the workforce data. Little is also known about the 40% of pharmacists who were not of a rural background, and further research is required for a richer understanding of these two issues.
Rural origin has previously been found to have a significant impact on retention of the health workforce13; therefore, finding more than half the sample with a substantial rural background adds support to the growing body of studies that rural background is associated with rural practice14-16.
A common characteristic for the majority of rural/remote pharmacists was the high level of professional satisfaction reported. Rural/remote pharmacists reported a wide variety in their professional work, report close relationships with other health professionals and perceive a sense of satisfaction from their customers, all of which contribute to professional satisfaction. Professional satisfaction did differ with rurality, with respondents in more remote areas (small rural, other rural and remote areas-RRMA 4-7) more satisfied in terms of task variety, professional autonomy, their use of advanced skills and remuneration than their more urban counterparts (urban and large rural centres, RRMA 1-3). Despite challenges with geographical and professional isolation, this increased professional satisfaction may be an important factor in the retention of pharmacists in rural/remote regions. Professional satisfaction has been identified as an important driver for the rural/remote workforce in other health professions such as medicine17, nursing18 and allied health19. Development and implementation of appropriate support mechanisms to foster professional satisfaction may have an important role in promoting recruitment and retention of the rural/remote pharmacist workforce.
Many of the barriers and drivers for rural or remote pharmacy practice identified in this study are similar to those frequently cited in the literature for other health professions. Medicine20, nursing21 and allied health22 have all identified barriers to rural/remote practice, including lack of access to continuing education and professional isolation. Although these may be common issues for many health professionals, solutions should be tailored to the individual profession, and pharmacy-specific strategies developed to encourage and support rural and remote pharmacy practice. Given the role differences between hospital and community pharmacy, sector-dependent strategies may also need to be considered.
Defining rurality remains problematic in the pharmacy context. In contrast to other health professions, which use the Australian Standard Geographical Classification for classifying rurality23, the PhARIA Index is used to define rurality for the purposes of government pharmacy initiatives. PhARIA takes the number of pharmacies into consideration in defining rurality, and as a result a number of regional centres and large rural towns have the same PhARIA classification as major capital cities. As government rural pharmacy funding and initiatives are PhARIA based, and generally define rural practice as PhARIAS 2-6, revision of the PhARIA system is desperately needed to ensure that pharmacists practising in large rural towns and regional centres are not disadvantaged by the classification system, as their needs and challenges are likely to be quite different from those of their urban counterparts.
Limitations
Use of a convenience sample for the consultative process is one limitation of this study; however, snowball sampling was also used to ensure a diverse range of views. Use of a commercial mailing list for identification of eligible rural/remote pharmacists was also problematic. Although it ensured participant confidentiality, contact details of a considerable number of rural/remote pharmacists were out of date, hence the exclusion of 517 potential rural/remote pharmacists from the study.
The aim of this study was to describe the rural/remote pharmacist workforce and to explore possible factors that may affect recruitment and retention of pharmacists to rural and remote areas. While the results presented provide an extensive overview of the rural/remote workforce, a comparable national study comparing rural/remote and urban pharmacists would further contribute to this discussion. Knowledge on why pharmacists chose to work in a particular geographical location, or why pharmacists chose to leave a location would further enrich our knowledge on what drives and sustains the rural/remote pharmacist workforce.
This study identified the strong rural background of existing rural and remote pharmacists, and the professional satisfaction driving retention of the rural/remote pharmacy workforce. It also identified a number of barriers such as an inability to achieve a better work-life balance, spouse employment, and children's education, which affect recruitment and retention of pharmacists in rural/remote Australia. While the majority of rural/remote pharmacists had a rural background, approximately 40% of the current rural/ remote pharmacist workforce come from urban backgrounds, and little is known of their motivations. A better understanding of this population might provide insight into improved methods of recruitment, retention and support for pharmacists working in rural and remote Australia.
Acknowledgements
The authors acknowledge and thank the rural/remote pharmacists who responded to the rural workforce study; and the pharmacists, students, placement coordinators, academics, and other key stakeholders who participated in interviews and focus groups. Without the input of these people the research would not have been possible. This Research to Track the Rural Pharmacy Workforce, and Identify the Role that Rural Programs have on the Retention of the Rural Pharmacy Workforce, was funded by the Rural Pharmacy Workforce Program Commissioned Project/Research Scheme as a component of the Rural Pharmacy Workforce Program (RPWP). The RPWP is funded by the Australian Government Department of Health and Ageing and managed by The Pharmacy Guild of Australia.
References
1. Australian Institute of Health and Welfare, Australia's health 2006. Canberra, ACT: Australian Institute of Health and Welfare, 2006.
2. Australian Institute of Health and Welfare, Rural, regional, and remote health - indicators of health. Canberra, ACT: Australian Institute of Health and Welfare, 2005.
3. Humphreys J. Delivering appropriate and accessible health care to meet the distinct and diverse needs of rural and remote populations. In: Inaugural rural and remote health scientific symposium; 6 July 2008; Brisbane, QLD; 2008.
4. Australian Institute of Health and Welfare. Pharmacy labour force to 2001. AIHW cat. no. HWL 25 (National Health Labour Force Series no. 25). Canberra: Australian Institute of Health and Welfare, 2003.
5. Australian Government Department of Health and Ageing. Report on the audit of health workforce in rural and regional Australia. Canberra: Australian Government, 2008:.
6. Fiore S., et al., Support needs of supply nurses in rural and remote Queensland. Australian Journal of Rural Health, 2005; 13: 10-13.
7. Margolis S, Ypinazar V. Tele-pharmacy in remote medical practice: The Royal Flying Doctor Service Medical Chest Program. Rural and Remote Health 8(2): 937. (Online) 2008. Available: www.rrh.org.au (Accessed 28 March 2013).
8. Marriott J, Nation RL, Costelloe M, Galbraith K, Stewart P, Charman WN. Pharmacy education in the context of Australian practice. American Journal of Pharmaceutical Education 2008; 72(6): 131.
9. Australian Government Department of Health and Ageing. Review of the rural, remote, and metropolitan areas (RRMA) classification. Discussion paper (without prejudice). Canberra, ACT: Department of Health and Ageing, 2005.
10. GISCA, PHARIA. Pharmacy Access/remoteness Index of Australia. (Online) 2008-2009. Available: http://www.adelaide.edu.au/apmrc/research/projects/pharia/ (Accessed 28 March 2013).
11. Carifio J, Perla R. Resolving the 50 year debate around using and misusing Likert scales. Medical Education 2008; 42: 1150-1152.
12. Wilkinson JM, Simpson, MD. The first graduate cohort at Charles Sturt University: what impact on the rural pharmacist shortage? Journal of Pharmacy Practice and Research 32(1): 69-71. (Online) 2002. Available: http://search.informit.com.au/documentSummary;dn=474420749009185;res=IELHEA (Accessed 16 October 2012).
13. Wilkinson, D, Laven G, Pratt N, Beilby J. Impact of undergraduate and postgraduate rural training, and medical school entry criteria on rural practice among Australian general practitioners: National study of 2412 doctors. Medical Education 2003; 37(9): 809-814.
14. Chen T, Whitehead P, Aslani P. A census survey of rural/remote community pharmacists in NSW to identify recruitment and retention factors. Sydney: Faculty of Pharmacy, The University of Sydney, 2004.
15. Smith JD, White C, Luetsch K, Roufiel L, Battye K, Pont, L. What does the rural pharmacist workforce look like? Australian Pharmacist 30(12): 1037-1039. (Online) 2011. Available: http://search.informit.com.au/documentSummary;dn=687384238110142;res=IELHEA (Accessed 28 March 2013).
16. Harding A, Whitehead P, Aslani P, Chen T. Factors affecting the recruitment and retention of pharmacists to practice sites in rural and remote areas of New South Wales: A qualitative study. Australian Journal of Rural Health 2006; 14: 214-218.
17. Australian Institute of Health and Welfare. Health workforce in Australia and factors for current shortages. Canberra: Australian Institute of Health and Welfare, April 2009.
18. Molinari DL, Monserud MA. Rural nurse job satisfaction. Rural and Remote Health 8: 1055. (Online) 2008. Available: www.rrh.org.au (Accessed 28 March 2013).
19. Campbell N, McAllister L, Eley D. The influence of motivation in recruitment and retention of rural and remote allied health professionals: a literature review. Rural and Remote Health 12: 1900. (Online) 2012. Available: www.rrh.org.au (Accessed 28 March 2013).
20. Dunbabin JS, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health 3: 212. (Online) 2003. Available: www.rrh.org.au (Accessed 28 March 2013).
21. LaSala KB. Nursing workforce issues in rural and urban settings: Looking at the difference in recruitment, retention and distribution. Online Journal of Rural Nursing and Health Care 2000; 1(1). Available: http://www.rno.org (Accessed 28 March 2013).
22. O'Toole K, Schoo AM. Retention policies for allied health professionals in rural areas: a survey of private practitioners. Rural and Remote Health 10: 1331. (Online) 2010. Available: www.rrh.org.au (Accessed 28 March 2013).
23. Australian Government Department of Health and Ageing. Doctor connect. Available www.doctorconnect.gov.au/internet/otd/Publishing.nsf/Content/ra-intro (Accessed 28 March 2013).






