Introduction
In Australia, doctors choosing to specialise in general practice undertake 3 years post-registration training as general practitioner (GP) registrars. The first year is spent in hospital practice and the following 2 years in general practice in a working apprenticeship alongside a more experienced colleague, a GP supervisor. GP supervisors are required to provide clinical supervision, direct observation and regular tutorials. The expected level of GP supervisor input reduces as the GP registrar gains experience. Vocational registration as a general practitioner is achieved on completion of training and passing the Fellowship examination of the Royal Australian College of General Practitioners (RACGP). In addition, an independent training adviser monitors each GP registrar's progress throughout the training program.
One strategy to address the medical workforce shortage in rural and remote Australia has been to increase the number of doctors training as GPs in these areas. This has the dual function of increasing the rural and remote workforce in the short term, while in the longer term promoting the development of skills necessary for practice in regional areas.
Educational research has shown that the interaction between a learner and teacher affects both content (what is learned) and process (how the content is learned)1. Effective work-experience partnerships require both parties involved to have a clear understanding of the nature of the apprenticeship, the agreement between them and mutual benefit of it to both2. Ineffective partnerships may not capitalise on the potential opportunities for learning and risk the perception by either party of 'being used' by the other. This study was initiated in response to GP registrars' voicing concerns to their training advisors about learning and teaching in general practices in one remote region of Australia.
The area
The geographic area in question was Central Australia, in the Northern Territory (NT), classified as 'most remote' under the Australian Rural, Remote and Metropolitan classification system3 (Fig 1). The region, centred around Alice Springs, covers an area of more than half a million square kilometres and had a population of 48 000 at the time of the study. Of this population, 30 000 lived in towns and 18 000 lived in isolated desert communities; 33% were Indigenous Australians (Aborigines). The two hospitals (one base and one regional) were staffed by GPs with resident specialists in medicine, surgery, paediatrics, obstetrics, anaesthetics, emergency medicine, ear, nose and throat (ENT) and ophthalmology. Despite a visiting specialist service, specialist procedures often required patients to fly to a capital city more than 1500 km away.
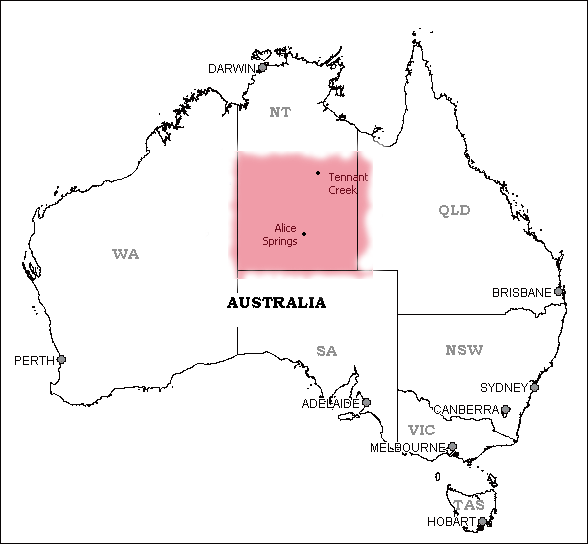
Figure 1: The pilot study area, the Central Australian region.
The issues
The issues of concern raised by GP registrars with their training advisors prior to this study were:
- The absence of formal teaching sessions
- The timing and topics of teaching that did occur
- Difficulty in accessing educational opportunities outside the practice
- Tension between service provision and achieving personal educational objectives
- The challenge of learning in private practice when income is dependent on the number of patients seen
- The degree of adaptation required by GP registrars when working at practices
The complaints of the GP registrars were puzzling because all the GP supervisors involved were committed and hardworking GPs. Some of the questions posed by the researcher were: did the GP registrars have unrealistic expectations of their supervisors, or were their expectations simply different? Or was it that the RACGP guidelines4 on training were not being applied at a time of significant workforce shortage when GP supervisors were working hard in difficult circumstances? And ultimately, did the rural and remote context of the GP training affect the teaching and learning of these doctors.
Aim
The aim of the study was to explore factors in the interaction between GP registrars and GP supervisors in the context of their practices that impact on the quality of GP registrar learning in Central Australia.
Methods
Literature review
Few studies have been published on the experience of GP registrars learning in Australia or in any remote area. Farmer and Taylor surveyed GP registrars in South Australia and Australia's NT by questionnaire, from February 1985 to May 19885. The two main variables found that affected GP registrar satisfaction with education were the daily patient load and the quality of supervision. The GP supervisor's personal and professional relationships with the GP registrar, the time spent in teaching, case review activities, and regular and adequate feedback were the most important factors.
Critical incident analysis of competent or poor professional practice framed another study of GP registrar learning in their basic terms in Western Australia6. Although relationships with GP supervisors and practice staff were positive, difficulties in these relationships were found to account for 8% of negative critical incidents. The participants reported that they were expected to see too many patients per rostered hour, that they felt unsupported, and that they were often treated as medical students rather than inexperienced colleagues.
A survey of residents in family medicine training programs in Canada indicated that isolation, accommodation and supervision were commonly problematic for trainees in rural areas7.
Interview method and schedule
A qualitative research method was used to explore the subtleties and issues in the relationships between GP registrars and supervisors. An interview schedule was devised from issues raised by the Central Australian trainees with their training advisors, and from issues identified in the literature. The schedule consisted of six stems, each with a pair of polarised, provocative statements7 to generate discussion about the interaction between GP registrars, GP supervisors and their practices (Fig 2); it was based on the 'awareness-centred approach' described by Neighbour8.
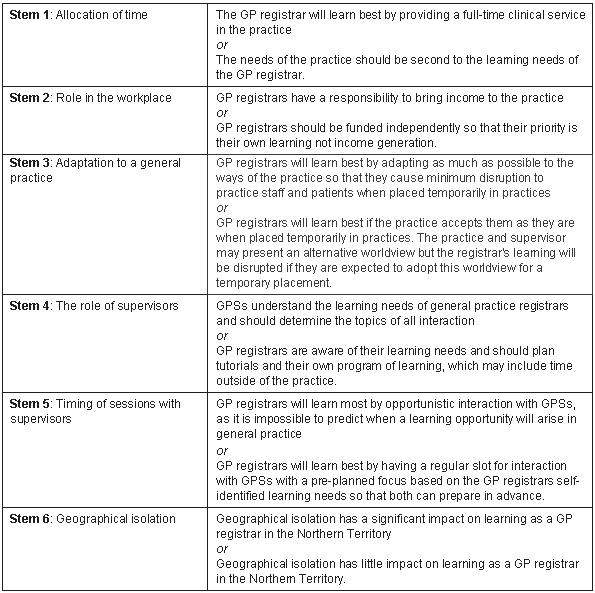
Figure 2: Interview schedule composed of pairs of polarised provocative statements used to generate discussion. GPR, General practitioner registrar; GPS, general practitioner supervisor).
Sample and recruitment
GP registrars working in Central Australia who had completed one six-month term of GP training were eligible for the study. Potential participants were informed of the study at a residential workshop in Darwin, NT. Six GP registrars met the entry criteria; all were female. One of the six participants was not able to be interviewed due to logistical reasons. A letter of introduction and a consent form was given to interviewees prior to interview.
GP supervisor and ethical approval
The State Education Manager of the RACGP training program approved the project. GP supervisors were informed of the project and the wording of the interview schedule, and none refused permission for their GP registrar to participate in the study. The Social and Behavioural Research Ethics Committee, of Flinders University, gave ethical approval for the study. Interview material was anonymous.
Interviewer
The interviewer was known to the GP registrars through her role as training advisor and GP educator in Alice Springs, NT. From experience in the field an expected answer to each stem was hypothesised and documented prior to conducting the interviews (Fig 3). In this way it was possible to make a comparison between the participants' and interviewer's ideas to identify the introduction of bias.
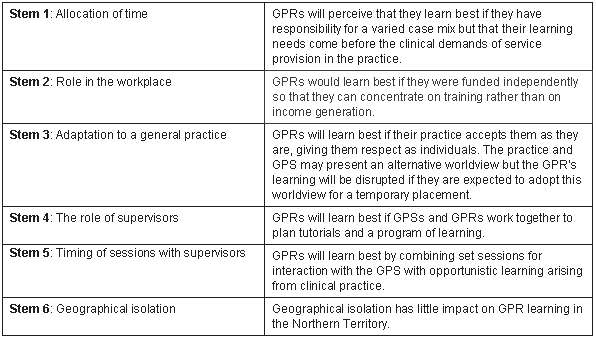
Figure 3: Hypotheses (expected answer to each stem) documented prior to the interviews. GPR, General practitioner registrar; GPS, general practitioner supervisor.
Interviews and analysis
The interviewer read out each pair of statements in turn. The GP registrars responded and further probing questions were asked until the GP registrar indicated that the subject was exhausted. The same interviewer conducted all the interviews, which were recorded and transcribed verbatim and identified by code. The verbatim transcript was edited to remove expressions of speech and sent to the interviewee for correction. The agreed edited and corrected version became the research record9. The responses were grouped and then content analysed per question.
Results
The five remaining GP registrar participants were interviewed between September and December 2001. Four interviews took place face-to-face and one was conducted by telephone. The duration of interviews was between 20 and 35 min. GP registrars based their answers on their total experience of training in general practice, not just their current practice.
Stem 1 - Clinical service or educational needs
All GP registrars considered that they learnt best by providing a clinical service but that they should not be in practice just to fill a service need. GP registrars thought placements benefited both the GP registrar and the practice. One GP registrar considered that the practice's needs should be second to that of the GP registrar, but not all the time. Others were happy to accommodate practice needs first, provided that their needs were not always secondary.
GP registrars agreed that access to support and back up from GP supervisors was essential, but regretted that this was not always available, despite what one mentioned as adequate financial support that should prevent any conflict between the needs of the practice and the needs of the GP registrar. One commented that her practice had not fulfilled the RACGP's Training Standard requirements and that she had to make difficult clinical decisions without access to advice. Another suggested that if practices gave GP registrars time and support initially, '...they would get more out of us in the long run' [Dr A].
GP registrars considered that they learnt best by seeing their own patients but '...there are certain things that we can learn better from the experts' [Dr B]. They reported that the current arrangements did not facilitate learning from 'experts' because this would result in a drop in income for the practice and the GP registrar.
Stem 2 - Financial arrangements
GP registrars realised that training in private general practice affected their learning and said that pressure should not be put on GP registrars to earn a certain amount of money otherwise mistakes would be made. The option of alternative funding, such as being salaried, for the first year of training in general practice was welcomed but still risked inequity because the workload varied between practices. A salaried option would allow GP registrars more time for teaching and utilisation of educational opportunities. GP registrars considered that earning their own income for the second year of training in general practice was appropriate training in time and practice management for qualifying as a GP. Unlike their Western Australian colleagues6, none of the GP registrars expressed concern that they were treated like medical students: instead they felt that they were treated just like other GPs. This meant, however, that their needs to learn and to be supported were often not acknowledged or met.
Stem 3 - Adaptation to practices
'It is impossible to go to a place and not affect the place and not be affected by it' [Dr B]. GP registrars disagreed with both statements in the pair presented (Fig 2), instead preferring some adaptation by both parties. It was felt that this required sensitivity and flexibility, which were considered essential skills for GP registrars to acquire. It would not be good in the long term '...if they let them get away without making any adjustments' [Dr E].
GP registrars saw Aboriginal Medical Services (AMS) as unique, requiring cultural sensitivity and significant adaptation. GP registrars commented that an AMS is not a suitable placement for a GP registrar in their first GP placement, and that AMSs should to provide more assistance with cultural safety and support for GP registrars.
Stem 4 - Support from GP supervisors
Most GP registrars said the topics of teaching should be agreed between the GP registrar and the GP supervisor. None considered that choosing topics should be left to the GP supervisor alone. One GP registrar said that some GP supervisors know little about the RACGP curriculum and examination so only the GP registrar should decide the topics, but another said that a good GP supervisor should be able to identify the GP registrar's blind spots.
GP registrars strongly supported the idea of seeking learning opportunities in other practices or from specialists.
Stem 5 - Timing of teaching
GP registrars all agreed that they needed both opportunistic learning and pre-planned tutorials. According to 'Dr D', the former was 'a quality thing' while the latter was 'a quantity thing ... You need both'.
'No opportunity ever happens' [Dr C]. Opportunistic learning was invariably GP-registrar initiated. The funding mechanisms for general practice were perceived as a barrier to GP supervisors teaching the GP registrar about difficult or unusual cases or practical procedures. Opportunities for learning joint injections or minor surgery were not used, nor were GP registrars able to directly observe the GP supervisors or others in clinical practice.
Pre-planned tutorials provided a forum for discussion of issues accumulated during the week and for preparation so that 'a good two way conversation' [Dr B] could develop. In some practices, tutorials were not given priority on the timetable and so did not occur, or else were held outside working hours. This did not comply with RACGP guidelines and was considered inappropriate by some of the participants.
- The current teaching system, as far as I can see, simply further devalues general practice by turning out undereducated GPs who have a bit of knowledge about things but can't speak confidently on a broad range of topics [Dr C].
Stem 6 - Isolation
GP registrars reported that geographical isolation was a significant factor affecting their learning. For most GP registrars the impact was negative, but the GP registrar who worked in a remote Aboriginal community believed the isolation to be positive. The clinic set up gave her time to check information in texts or the Internet, or to telephone specialists for advice. Specialists were particularly helpful with advice once they realised where she was working and helped her manage the patient rather than just suggest a referral. 'I've learnt more in 2 months in ... than I did in 2 years in Alice Springs' [Dr E; Alice Springs is the main town in the Central Australian region].
The GP registrars who considered geographical isolation a negative factor cited the lack of access to specialists, workshops and courses as significant, although the extra clinical responsibility taken by rural GP registrars was seen as an educational advantage. Teleconferencing, the main teaching medium used by the local training program, was seen as the best method available but was also understood to have limitations. Didactic-style lectures with pre-distributed handouts was seen as something that could work well, but the group discussions were found difficult by some. One GP registrar admitted to watching TV on mute at the same time as listening in to the teleconference. Accessing the Internet or satellite broadcasts was hard after a full day's work. One practice combined GP registrar sessions with continuing medical education for practising professionals but the GP registrar considered this insufficient for a training post.
These GP registrars had chosen to train in remote areas and were prepared to work at overcoming the isolation. They commented that training in remote areas should be voluntary not forced. One GP registrar who had worked in an urban general practice prior to entering the GP training was worried that doctors might train only in rural or remote areas. She felt it was important that those who wanted to work in the country should also experience how medical care can be delivered when there is ready access to specialists and investigations.
Discussion
Although the generalisability of this pilot study is limited by the small, all-female sample from one region, the issues raised are relevant and warrant further discussion and research.
The interview schedule (Fig 2) was effective in stimulating conversation, but it may have narrowed the discussion to just the issues presented. Stem 1, Clinical service or educational needs, was interpreted by GP registrars in varying ways and should be modified for clarity before any extension of the project. Stem 3, Adaptation to practices, was most effective when a specific example was used to explain statements.
Many of the answers were different from those recorded in the hypotheses. This suggests that the interviewer's own ideas did not affect the participants' answers and validates the findings. The use of a single researcher increased the likelihood of consistency among interviews; however, it did risk subjectivity in the analysis. One way to address this in further research is to triangulate registrar data with data collected from supervisors.
The participants' learning styles were not analysed but this could be included in an extension of the pilot project. It is possible that the learning environment described best suited 'active' learners while this cohort of GP registrars included 'theorists' or 'reflectors'11.
Summary and implications of findings
The GP registrars recognised the educational value of their clinical work in general practice but identified barriers to maximising the learning opportunities. They reported they would like to observe their GP supervisors and others in the practice during consultations and performing practical procedures, and to extend their learning to specialists or other resources in the area. This concurs with Brookfield's finding that observing role models is one of the most effective ways people can learn to think critically10. GP registrars perceived the main barriers to this were the current funding mechanism where income is dependent on contact time between the patient and their doctor, and a shortage of GPs in the region.
GP registrars often expressed their experience of insufficient support, particularly in Aboriginal Medical Services. According to Maslow's hierarchy12 such a lack of 'safety' may impair progression to self-actualisation and thus make unlikely the possibility of experiencing 'all conceptions' of learning13.
GP registrars reported that the geographical isolation of Central Australia had a significant impact on their learning. While Rourke and Rourke's Canadian study6 focussed on isolation from family and friends, the present study's isolation was experienced as distance from educational resources. This is an important consideration for those involved in developing community-based medical education in rural and remote Australia14. Strategies to overcome isolation from educational opportunities must be developed and trialled. Following the recommendation of one GP registrar that training occur in a variety of rural and urban settings would increase GPs' future ability to practise in a variety of settings.
The questions about whether the GP registrars had unrealistic expectations, whether their expectations differed from their GP supervisors, or whether the RACGP recommendations were not being implemented because of workforce shortages were explored. In one case the RACGP recommendations were not adhered to. The practices concerned have implemented changes. For most, however, the issue seemed to be that the expectations of GP registrars and their GP supervisors did not match, and that learning opportunities to improve the match were thwarted by structures.
GP supervisors are doctors first and teachers second: they are ethically obliged to see patients first and teach second. It is possible that training medical practitioners in areas of workforce shortage may create a negative learning experience and decrease their enthusiasm to stay in that geographic area.
Currently in the Central Australian region, time constraints, funding structures and workforce shortages prevent the GP registrar with GP supervisor interaction necessary for providing and reaching full educational potential. It may well be that strategic supports for registrars and supervisors must be developed to ensure that training GP registrars in remote settings is both educationally sound and provides the workforce benefits intended.
Acknowledgements
The author would like to acknowledge the contribution of the general practice registrars and Dr Halia Silins who supervised the project and Dr Janice Orrell for her assistance in the development of the interview schedule. This study was conducted as partial fulfilment of the Graduate Certificate in Tertiary Education at Flinders University, South Australia.
References
1. Commonwealth Department of Health and Aged Care. Enhancing rural education and training for health professionals. Regional health strategy fact sheet 2. (Online, 2000). Available: www.health.gov.au/budget2000/fact/ruralfact2.htm (accessed 3 September 2003).
2. Marton F, Ramsden P. Improving learning: new perspectives. London: Kogan Press, 1988.
3. Grant J, Marsden P, King RC. Senior house officers and their training II. Perceptions of service and training. BMJ 1989; 299: 1265-1268.
4. Office of the Medical Advisor, General Practice Branch, Health Services Division, Department of Health and Aged Care. Rural, Remote and Metropolitan Area (RRMA) Classification in General Practice Australia. Canberra: Department of Health and Aged Care, 2000.
5. Royal Australian College of General Practitioners National Training Posts Standards Committee. Standards required of RACGP teaching posts. Melbourne, Vic: Royal Australian College of General Practitioners Publications, 2000.
6. Farmer E, Taylor S. Assessment of teaching by Family Medicine Programme vocational trainees. Australian Family Physician 1990; 19: 549-557.
7. Diamond MR, Kamien M, Sim MGB, Davis J. A critical incident study of general practice trainees in their basic general practice term. Medical Journal of Australia 1995; 162: 321-324.
8. Rourke JTB, Rourke LL. Rural family medicine training in Canada. In Proceedings, Issues affecting rural communities, 10-15 July 1994; Townsville, Australia. ERIC [database] http://www.askeric.org/Eric/ (accessed 1 September 2003).
9. Neighbour R. The inner apprentice: An awareness-centred approach to vocational training in general practice. Newbury, UK: Petroc Press, 1992; 206.
10. Stake RE. The art of case study research. London: Sage, 1995.
11. Brookfield S. Understanding and facilitating adult learning. Milton Keynes, UK: Open University Press, 1986.
12. Honey P, Mumford A. The manual of learning styles. Maidenhead, UK: Peter Honey, 1992.
13. Maslow AH. Motivation and personality. In Neighbour R (Eds). The inner apprentice: an awareness-centred approach to vocational training in general practice. Newbury, UK: Petroc Press, 1992.
14. Marton F, Dall'alba G, Beaty E. Conceptions of learning. International Journal of Educational Research 1983; 19: 277-300.
15. Habbick BF, Leeder SR. Orientating medical education to community need: a review. Medical Education 1996; 30: 163-171.
16. Royal Australian College of General Practitioners. RACGP Training Program (2nd edn) Melbourne: Royal Australian College of General Practitioners Publications, 1999.

