Dear Editor
Introduction
Many women in the rural areas of developed countries hope to deliver their baby in their home-town clinic. However, many pregnant women in developing countries have no choice but to deliver their baby in a small birthing-house. Thus, many deliveries, especially those considered as low risk, are handled in a rural area with limited resources. This context has been reported on in this Journal1,2. However, a delivery can be regarded as 'normal' only after the fact, which holds true especially for postpartum hemorrhage (PPH).
Postpartum hemorrhage can occur in women who were considered to be at low risk. For instance, a rural Australian GP obstetrician encountered PPH in 10.3% of cases2. The treatment of PPH begins with fundal massage, the administration of uterotonic agents and then bi-manual uterine compression. If these fail to achieve hemostasis, we must perform the second line treatment. Modern obstetrics has many such treatment strategies: trans-arterial embolization3, uterine compression sutures4, or hysterectomy. Recently, intrauterine balloon tamponade using a Sengstaken-Blakemore tube5 or Bakri's catheter (designed specifically for uterine tamponade)6 has been also employed; these intrauterine balloon tamponade are usually be attempted before the employment of the more invasive treatments mentioned above. However, Sengstaken-Blakemore tubes or Bakri's catheters are expensive and thus their availability in the rural settings is unlikely. I will therefore describe two simple, alternative ways to treat PPH in rural settings.
Uterine tamponade using a 'condom-catheter balloon'
The first is uterine tamponade using a 'condom catheter balloon'. A condom, tied to the tip of a Foley catheter with suturing silk, is placed in the uterus (Fig1). The condom is inflated with saline using gravity after the Foley catheter is connected to a bottle of saline using an intravenous set. Via the Foley catheter, the condom is inflated with approximately 2007-4008 mL saline until the bleeding is reduced. To my knowledge, there have been five case reports or case series demonstrating the effectiveness of a 'condom-catheter balloon', with hemostasis achieved in 94-100% of the patients8. We usually use a metreurynter (water-filled balloon), an intrauterine devise to induce labor contractions, because Japanese regulations prohibit the use of a condom as an intrauterine device. Thus, although we have no experience in its use, a 'condom-catheter balloon' is a reasonable measure. No serious side-effects have been reported7,8.
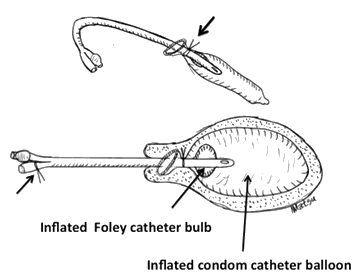
Figure 1. Schematic presentation of a condom-catheter balloon.
Upper: Before insertion. A condom is tied over the proximal end of a Foley no 16 catheter (any manufacturer) (arrow).
Lower: After insertion. The condom catheter-balloon is inserted into the uterine cavity. The Foley catheter bulb is inflated, which prevents the condom catheter-balloon from sliding out of the uterine cavity. Then the condom catheter balloon is inflated, which compresses the uterine cavity (bleeding surface). The outlet of the condom may be located either within the cervical canal (this figure) or within the uterine cavity. The outer end of the Foley catheter should be tied with suturing silk (arrow). The balloon is usually kept inflated for 8-48 hours until hemostasis is confirmed.
The 'holding the cervix' technique
The second alternative is the 'holding the cervix' technique, which we devised. As described in previous publications9,10, the uterine cervix should be closed by round forceps placed simultaneously over the anterior and posterior cervical lips (Fig2) to prevent the outflow of blood. The uterus fills with blood, which may tamponade the bleeding surface, leading to hemostasis. Manipulation of the cervix, increasing the uterine contraction11, may also work for hemostasis. Of approximately 200 PPH patients undergoing this procedure at our institute, hemostasis was unsuccessful in only three9,10. I believe that every rural clinic would be equipped with round forceps or a similar alternative.
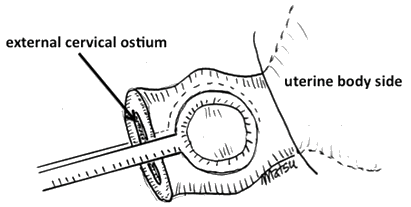
Figure 2: Holding the cervix technique. The uterine cervix should be closed by round forceps.
Discussion
Some concern may arise that these procedures could expose patients to further trauma and subsequent infection, including puerperal endometritis. These procedures may also require some time to implement. Although the time required to insert a condom-balloon was not described8, I assume it would be less than 5 min for an experienced physician. I can usually perform the 'holding the cervix technique' within 1 min. Data also indicated that of the 18 patients who had a condom-balloon inserted, none showed injury due to this procedure and none had clinical findings suggestive of endometritis at the time of discharge to home8. The 'holding the cervix' technique induced no injury to the cervix and caused no adverse events, as previously described9,10.
However, we must consider the rural setting. Assembling the apparatus may take a lone rural practitioner away from the patient at the critical time of PPH. Thus, practically, non-invasive first line treatment (fundal massage, the administration of uterotonic agents, and bi-manual uterine compression) should be tried before employment of these procedures. In addition, simulation of these two procedures should be performed, and staff other than the physician or midwife may be able to assemble the apparatus.
Previously, we reported a severe acute epidural hematoma in a remote island, which was drained using a stainless steel wire (Kirschner) because there was no special equipment for skull trephination12. The patient recovered completely12. Postpartum hemorrhage sometimes causes maternal death if inadequately treated. For this reason, if rural medical facilities do not have adequate medical equipment in the case of PPH, alternative measures must be considered. The measures described here may be life-saving while waiting for transport.
Shigeki Matsubara MD, PhD
Department of Obstetrics and Gynecology
Jichi Medical University, Tochigi, Japan
References
1. Patterson JA, Foureur M, Skinner JP. Patterns of transfer in labour and birth in rural New Zealand. Rural and Remote Health 11(2):1710. (Online) 2011. Available: www.rrh.org.au (Accessed 4 September 2012).
2. Kirke AB. How safe is GP obstetrics? An assessment of antenatal risk factors and perinatal outcomes in one rural practice. Rural and Remote Health 10(3):1545. (Online) 2011. Available: www.rrh.org.au (Accessed 4 September 2012).
3. Matsubara S, Sato T, Nakata M. Vaginal artery embolization with a permanent embolic agent for intractable postpartum hemorrhage. Journal of Obstetrics and Gynaecology Research 2011; 37(4): 377-378.
4. Matsubara S, Yano H, Taneichi A, Suzuki M. Uterine compression suture against impending recurrence of uterine inversion immediately after laparotomy repositioning. Journal of Obstetrics and Gynaecology Research 2009; 35(4): 819-823.
5. Seror J, Allouche C, Elhaik S. Use of Sengstaken-Blakemore tube in massive postpartum hemorrhage: a series of 17 cases. Acta Obstetricia et Gynecologica Scandinavica 2005; 84(7): 660-664.
6. Bakri YN, Amri A, Abdul Jabbar F. Tamponade-balloon for obstetrical bleeding. International Journal of Gynaecology and Obstetrics 2001; 74(2): 139-142.
7. Bagga R, Jain V, Sharma S, Suri V. Postpartum hemorrhage in two women with impaired coagulation successfully managed with condom catheter tamponade. Indian Journal of Medical Science 2007; 61(3): 157-160.
8. Rathore AM, Gupta S, Manaktala U, Gupta S, Dubey C, Khan M. Uterine tamponade using condom catheter balloon in the management of non-traumatic postpartum hemorrhage. Journal of Obstetrics and Gynaecology Research 2012; 38(9): 1162-1167.
9. Matsubara S, Kuwata T, Usui R. Forceps holding the cervix for postpartum haemorrhage. Journal of Obstetrics and Gynaecology 2011; 31(6): 509-509.
10. Matsubara S, Kuwata T. Holding the uterine cervix may induce uterine contractions in atonic bleeding. Acta Obstetricia et Gynecologica Scandinavica 2011; 90(12): 1454-1455.
11. Yorifuji T, Tanaka T, Makino S, Koshiishi T, Sugimura M, Takeda S. Balloon tamponade in atonic bleeding induces uterine contraction: attempt to quantify uterine stiffness using acoustic radiation force impulse elastography before and after balloon tamponade. Acta Obstetricia et Gynecologica Scandinavica 2011; 90(10): 1171-1172.
12. Tokushige J, Matsubara S, Tanaka Y, Kato S. Trephination for acute epidural hematoma using stainless wire on a remote island. Journal of Emergency Medicine (in press).
