There is evidence in literature that health science students from rural backgrounds are more likely to opt for eventual rural practice, so one strategy to improve access to health care in rural areas is to increase the number of rural-origin students admitted for training1-3. Health science faculties in South African universities still have a low proportion of students from rural areas, with Tumbo and colleagues suggesting an average of 26% over the four-year period encompassing the years 1999 to 20024, with little change over the past decade; this is despite South Africa having a rural population close to 50%3.
Although it is clear that rural-origin students are more likely to work in rural areas after qualification than urban-origin students, this is by no means a direct relationship3,5,6. The majority of rural-origin students still ultimately practice in urban areas3,7. Career aspirations of students are shaped by a variety of factors, including the students' value system, religious beliefs, traditional values and socio-political convictions8. Personal values such as desire to serve the underserved3, and a sense of vocational commitment have been found to be significant predictors of rural practice9. The aspiration to specialize as a family physician is controversial, with Dunbabin and Levitt5 proposing this is predictive of later rural practice and de Vries and colleagues suggesting that in South Africa this is not the case6. Given the need in South Africa for greater numbers of healthcare professionals in rural areas, it is important to understand the ambitions of rural-origin students in the health sciences, as well as motivators and challenges faced, if we are to ensure better uptake of rural careers.
In considering factors that may affect the career aspirations of rural-origin students, it is important to consider whether their basic and social needs are being met, or whether they are unlikely to reach self-actualization. In South Africa, rural-origin students are often from disadvantaged backgrounds and thus face financial challenges. They have migrated from home communities to cities to attend university, and thus may have safety and security concerns. Being away from home, the particular social needs of rural-origin students may not be met such that they may feel isolated. Migrating from one place to another might also come with changes in culture, weather, lifestyle and language, and there is a need to adapt to those changes. Some changes are challenging, therefore, people who have migrated, including students, need support. For most people, this tends to come from their families, but when families are absent the social aspect of the support is missing.
Some challenges are common to any student adjusting to tertiary education, often away from home and family support. However, there are also challenges that are specific to those from rural areas, which must be identified and addressed in order to support the eventual retention of these students as graduates. It is difficult for rural-origin students to enter medical schools because of their high school and family background. Rural high schools tend not to have the infrastructure and support required to enable students to meet university entry requirements, whether those are based on performance in school leaving exams or subject choices at school, such as mathematics and sciences4. There is evidence that fewer rural-origin students end up qualifying, with higher drop our rates among this cohort, and migration increases the likelihood of the rural-origin student failing a year2. An additional challenge faced by rural-origin students in South Africa is that the language for learning at the nine universities offering health sciences is not necessarily the mother tongue of the majority of rural-origin students.
The support given to students should align with the career aspirations of students, as it might encourage them to either choose rural practice or not. This includes academic, social and financial support4. Ross suggests that it is not only academic support that is needed but peer support, in particular peer support from other rural students2. In addition to this, Ross suggests an external mentor who is able to keep in regular contact with the rural-origin student to provide encouragement and other support as necessary, even financial support. Mentors who understand the context the student comes from are also extremely beneficial2.
Tertiary institutions can play a significant role in addressing the recruitment and retention of rural-origin students by including rural practice in their curriculum. Despite some suggestions in the literature that curriculum exposure is not a significant factor in ultimate choice of a rural career3,5, Orpin and Gabriel highlight the importance of undergraduate experiences in relation to rural practice9. Some studies show that rural placement and rural exposure during training are likely to increase the proportion of health professionals practicing in rural areas8. In an Australian study, students were keen to work in rural areas because rural practice was included in the curriculum and the university catered for rural students10. Yet poor rural placement experiences during undergraduate training are likely to have the opposite effect, and are therefore worse than no exposure9. Curriculum therefore needs to be carefully planned and needs to include strategies that will encourage students from any background, whether rural or urban, to eventually see a need to practice in rural areas.
Once the undergraduate training is completed, many health science students make their first career choices: whether to return to serve communities immediately or to specialize, whether to spend some time practicing overseas, or even whether to emigrate. Rural-origin students are less likely to want to work overseas6. However, for the rural-origin student, there may be a tension between the desire to attain the highest possible qualification, or specialize, and the need to return to the family and community of origin. Financial obligations, and income or potential for earning, are among the most significant factors in career aspirations and decisions11. For rural-origin students in a study by de Vries and Reid, a sense of feeling needed was an important factor in the decision to practice in rural communities3.
Studies of international medical students in foreign countries or environments have shown that they experienced greater stress and lower health-related quality of life than local students12, and that 'language barriers, communication skills, cultural differences, financial burdens, heavy workloads and discriminatory bottle necks were key factors that hindered their adaptation to the local culture'13. One qualitative study of indigenous Australian medical students' perceptions of their training found that their progress through medical school was associated with 'student support, course content and styles of learning, personal qualities such as confidence and coping skills, discrimination and distinctive cultural issues pertinent to indigenous students'14. These and other students pointed towards the need for stronger support systems targeting such students15.
If we are to ensure the throughput and success of rural-origin students in health sciences, it is important to understand who these students are, what motivates them and the factors involved in the formation of their career choices. Many factors may shape the career aspirations of students, for example, money, personal development or other factors such as a change in the area of interest11. One quantitative study of senior medical students of rural origin in Australia did not find many significant differences to their urban counterparts, indicating that their initial discrepancies in background had less of an effect over time16. In the South African context, it is still unclear what the aspirations and motivations of rural-origin students are, and how these change over the years of study in the city. Do they start with a level of idealism and lose it, and if so what influences this? What degree of accountability do they feel towards their home communities, and how likely are they to return and work in their home community or one like it? Are there particular experiences within the curriculum that influence them to return? This study explores these questions in South Africa using qualitative methods.
With regard to a definition for rural areas, there is no consistency about the criteria used to define urban and rural areas in health research and policy internationally, including in South Africa; however, South African government policies refer to rural areas as those that are non-metropolitan17. For the purposes of this study, rural areas are defined as those outside of metropolitan areas, and categorized as farming, tribal or traditional areas by StatsSA in the national census. Wilson and colleagues defined rural-origin students as those completing primary and/or secondary school education in a rural setting18. For the purpose of this study, rural origin is defined as completing high school in rural areas. Career aspirations are defined as a cluster of needs, motives and behavioral intentions that individuals articulate with respect to different career field options.
The aim of this study is to understand the aspirations of undergraduate health science students of rural origin with regard to their future career plans. The objectives of the study were as follows:
- to explore and identify the key issues facing rural-origin students with regard to their future career plans
- to describe the relative importance of the issues facing rural-origin students across the years of study in order to show trends
- to report the findings and make appropriate recommendations.
The study is descriptive and has been designed in two distinct phases, a qualitative phase followed by a quantitative phase. Only the qualitative data are reported in this manuscript. The results of the qualitative phase of the study were used to formulate the questionnaire for later quantitative data collection, which will be reported elsewhere.
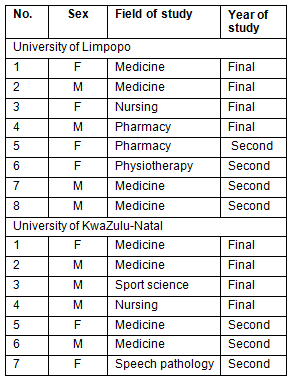
A purposive sample of 16 students of rural origin was taken. Students were in two different years of study, second year and final year, and at two different universities, University of Limpopo and University of KwaZulu-Natal One student sampled was unable to participate in the interview, resulting in 15 interviewees in total (Table 1). At each of the universities, one second-year volunteer and one final-year volunteer who lived in a rural area at least until the end of high school and were willing to be interviewed were requested from each of four different health science programs, with half of students being selected from medical school and half from the health science faculties. Due to the distribution of students in the health sciences, this is an appropriate representation of students.
Table 1: Participants' biographical details
Data were collected to explore the key factors, motivators and challenges of students of rural origin using the free attitude technique for individual interviews of purposively selected subjects. Individual interviews were chosen instead of focus groups in order to elicit personal and individualized issues rather than general issues2. Subjects were given an information sheet about the project and requested to sign informed consent after they had had an opportunity to ask questions about the project. Interviews took place between August 2010 and October 2010 at both universities.
Subjects were interviewed by a trained interviewer using open-ended techniques to elicit in-depth information. An interview guide was used to ensure that key questions were asked if they did not arise spontaneously. Interviews were held in the vernacular or language of choice to ensure that the participants were free and confident in responding. Interviews were digitally recorded and the interviewer also kept notes of the process.
All interviews were fully transcribed and translated into English where necessary by the interviewers. Analysis was done with the aid of NVivo v8 software (www.qsrinternational.com).
Ethics approval
The study was approved by the University of KwaZulu-Natal and the University of Limpopo Research Ethics boards, numbers HSS/0966/09 and MREC/M/63/2010:IR, respectively.
Fifteen students were interviewed in total, eight from the University of Limpopo and seven from the University of KwaZulu-Natal. At each university, a selection of second and final year students was sampled, including an equal distribution of male and female students. Each sample included at least one medical student from each year of study as well as at least one student from the faculty of health sciences (physiotherapy, sports science, speech language pathology, nursing, pharmacy). Students' areas of origin included places such as Kimberley, Hammanskraal, Limpopo, Nkandla, Mtubatuba, Bizana, Paulpietersburg and Nongoma.
Who is the rural student?
Students had a strong sense of family belonging.
I am the youngest, my big brother is a doctor, another form of inspiration, my second brother is a pharmacist in Durban, my third one works in ABSA. My sisters are both working, my big sister is a dermatologist and my other sister deals with lab staff ... and my twin is doing second year in electrical engineering [at] WITS. That is another form of inspiration... L8
Positive role models were frequently identified as influential persons in their decision to pursue tertiary studies. These mentors were often significant high school teachers or principals who encouraged students to pursue a career in health sciences, assisted in university applications and continued support throughout their studies.
...my physical science teacher, my agricultural teacher and my mathematics teacher were very good teachers. They were dedicated to their work. I was their friend - if I was stuck I would go to them and they would help out... KZN2
I really did not know what pharmacy was but our teacher is the one who encouraged us to apply. They told us about different courses, they gave us career books and we had to choose the university that one would like to go to. L5
The motivation guiding which university to choose was often based not on an entirely free choice but was limited by financial considerations, proximity to family and the fact that acceptance was only granted at certain universities.
Medunsa was the only institution that allowed late applications so then I decided to come here because there was no other places... L2
I also applied to UKZN, UCT and also here and why I choose this university actually I was more interested in going to UCT but when I was talking to my parents they thought it was much far and there I will not come home more often and I will be more alone here. I have relatives around Pretoria and Gauteng so that is how I ended up in this university. L7
The motivation to study health sciences was often based on personal experience of the health system and the limitations thereof.
Since I was in standard four I have realised that our country is in shortage of medical practitioners ... my uncle died while on the way to the nearby hospital which is far away ... so I realised that if anybody in the family could have been a doctor, we could have saved his life so since then I realised that then I decided to be a doctor... L1
How are they different?
Students from rural areas face unique challenges to which other tertiary students are not exposed. Academically related skills formed a large portion of the challenges that students faced. The language of instruction was cited as aggravating this problem, as well as other technical issues associated with learning and using computers.
...self directed learning - that was difficult for us because they were giving you the topic and expect you to know everything about that... KZN1
The biggest challenge I had was a language problem because where I was coming from you were taught English in Zulu... KZN6
We did not have computers. I did not even know what to do when I saw a computer. L5
The motivation to succeed in their tertiary studies was compounded by the lack of education within previous generations.
I am the only one who is educated and who went to university. L5
Given the challenges that these students were facing and the unique nature of these challenges, support was also unique. Family, friends, religion, university mentors and financial aid all played important roles in this regard. Help was sought from other students from similar backgrounds and often individual persons were singled out as playing a pivotal role in the transition to urban university life.
The university has done something good. It is called ADP. [Name] was so helpful. Without her I think I would have gone home. She really helped me a lot. I think I can write a whole book about that. KZN3
... people were helping me. I think it was God who was giving to me. I never went hungry [once] I got this scholarship from WIRHE which provided for accommodation, for food, for everything that I would need. L1
Obtaining financial aid was often a challenge in itself and knowing how and when to apply for aid was frequently raised by students as a concern. Aid is often transferred late in the year once the student has already had to make financial sacrifices themselves.
I am using a bursary from Limpopo. I wrote them a letter and told them about my situation. As I explained earlier on that in my first year I struggled to pay for my fees. They said I must come and see them and they assessed the situation and they saw that there is a need for me to get help. L4
Friends were utilized not just for socialization or study purposes but also as social mentors and guides in the transition from rural to urban lifestyles.
Some of my friends I have found here are from urban areas. I found it advantageous being around them. I learn from them, learn what is expected academically like to do things electronically. L8
Role models external to the nuclear family often took on the traditional parental supportive role throughout the tertiary education.
I call him [school principal] 'dad' because I do not have a dad, he does not exist, but he is still alive so I stayed with him [school principal]. He is strict, a good person, a role model. If you see me I am a reflection of what he has made me. KZN5
Changes during the period of study
The change in environment from a rural to urban situation played a major role in adaption to university life. Academic, financial, emotional and social stressors were identified.
There is a big difference between urban and rural areas ... in rural areas the only thing you will be thinking is, 'How am I going to eat tomorrow'. There is nothing more to think about here, they all have food so they have other things to think about ... that was my biggest challenge. L4
Students' results were the same as in other studies, that a positive experience of rural medicine has the greatest impact on a future decision to take on a rural career8,10.
[the rural health component of the curriculum] has a positive impact on us as trainees ... it is not always the fact that you make a diagnosis based on the test results but it must depend on your clinical skills in case you do not have those facilities in hospitals. KZN1
... it will be better if in each module there is a visit like that one we did in community studies when we go in to rural areas and see how people live - their issues concerning health, visiting their clinics and see how far the facilities are from people and what their concerns are in terms of health ... KZN7
There appeared to be no marked difference overall between the responses of final year students and the responses of second year students with respect to their career aspirations. Most second year students had idealistic aspirations to return to work in rural areas, and this theme was generally maintained by the final year students. However, some final year students expressed a cynicism and a definite intention not to go back to their home areas.
Another thing, nursing in the rural areas is very poor, that is what I have noticed. Even if I finish I do not think I will go back there; medication takes maybe a month to get contraceptives, antibiotics, panados, these simple medications ... L3
However, a number of final year students were very clear about their vocations.
I personally would like to go and work at home since I saw the need to be a pharmacist and I would also like to go back and serve my own people. That was a priority in choosing the career in the first place and I believe I can make a difference if I can go back and work there. L4
Future career plans
The majority of students expressed a desire to return to their home area. They indicated they felt a desire and need to return to serve their communities.
I do not mind being in a rural or urban area as long as I will be practicing medicine ... not to be far away from home ... L2
I grew up there. I feel like I am obliged to give back to the community ... I feel I want to make a difference to my people, community and be a good community doctor. L7
Some students did, however, express a desire to attain the highest possible qualification first and wanted to specialize in order to serve a particular need that they had identified in their community.
I would like to specialise in Obs & Gynae or neurology. I saw teenagers who were pregnant so I want to create a place where I can tell them about the importance of contraception, the use of condoms and to counsel those mothers who are HIV positive and pregnant ... KZN1
I am planning to specialise. I would love to specialise in paediatrics and I would also like to have internal medicine ... but I would like to practice in the community for some time ... there are many things you can learn when you are in the community. CAL2
Some students' motivation and over-riding sense of duty towards their communities guided the decision to become an 'agent of change' in their communities.
I realised that if I can come here to the community, I may make a difference ... because my father died of a stroke ... L1
Despite the fact that students expressed a desire to serve their communities, they also cited job satisfaction, lifestyle options and career development as demotivating factors for returning to work in a rural area. A few students also listed hospital management as a factor that drives doctors away from rural hospitals.
I think one factor that drives doctors away [from rural areas] is hospital management - most of the hospitals are poorly managed ... KZN2
However, despite all their many challenges and the obstacles they face, most rural students are motivated by a strong desire to change their community from adversity into success. They do not wish to escape the hardships, but rather view themselves as having a duty to use their now privileged position to the benefit of the community.
... after graduating I should go back there and make myself to be a mayor because one day I see myself as a minister of health ... if I go back to my community they should be able to say, 'This is a leader and we want him to lead us' ... KZN6
Discussion
Health science students of rural origin studying at universities in the South African context face specific challenges related to the nature of the contrast between rural and urban life, in addition to the more generic adaptations that confront all students on entering tertiary education. The shortage of medical personnel and the enormity of the developmental challenges of rural communities in South Africa is a significant contextual element in this study. Thus, the poverty of these students' backgrounds, as well as their disadvantage in terms of language, technology and finances on entering tertiary education in the city, adds an additional layer of challenge to the generic adaptations required of them. The data from this study suggest that these challenges are mitigated to a certain extent by support from family and peers, as well as from specific student support programs. If these were enhanced and optimized, they would have a beneficial effect on the ultimate success of rural-origin students.
It would appear that the choice to study one of the health sciences for rural students is not so much a rational choice from a range of equal options but, rather, more pragmatically taking an opportunity that is available. This reflects the limited choices that rural citizens experience on many levels. Many students' motivation is derived from personal and family experiences of lack of access to health services, and this emerges repeatedly from the data. The somewhat naive aspiration that the student will return as the savior of the community is nevertheless a powerful symbolic motivator, created and maintained by role models and family members, but subject to erosion by more attractive possibilities in the urban environment. Although not apparent in this study, a general loss of idealism through the course of the curriculum has been documented in studies in other contexts. It will be measured in the South African context through the second phase of this study, using these qualitative results to construct an appropriate tool.
The importance of family allegiances and the sense of responsibility towards their communities of origin that the respondents repeatedly express are possibly stronger in South Africa than the international literature indicates, since individual ambition is often subjugated to the collective identity in the African context. These and other cultural aspects that are important to students who come from more traditional or indigenous communities deserve to be examined in greater detail, particularly in view of the emphasis on recruiting a greater proportion of students from rural areas.
It has been postulated that some students from rural backgrounds would see admission into tertiary education as an opportunity to escape from a cycle of poverty towards greater social mobility and prospects in urban environments, and that they would therefore be unlikely to return to work in rural areas after completing their studies. However, this hypothesis has not been borne out by any data from this study and the contrary has emerged as a strong theme, namely the commitment and sense of accountability that students feel towards the improvement of their communities of origin.
With regard to curriculum design, exposure to rural practice is clearly important in preparing students for future career planning, but the data do not differentiate between those who were planning to choose rural practice from the start and those who are influenced by experiences in the curriculum to choose rural practice. As identified in the literature, this remains an area for further research19.
The limitations of this study include that the sampling was from only two universities as different contexts at other universities may have rendered different data. As with all qualitative research, the results cannot be directly generalized, but are valid as such for the participants in their respective situations.
In order to support rural students in their studies, academic, financial, emotional and social stressors need to be addressed. Universities need to strengthen existing support structures as well as aid the development of further support that is needed.
The academic curriculum should include more sustained and positive exposure to rural health at all levels and in all fields of training. In this way, rural communities will benefit from the services of academic institutions and students will be encouraged to return to work in these areas.
Specialist services are often viewed as the only way to address an underserviced community; yet, the reality is that such communities require comprehensive generalist services with an efficient and reliable referral system in place. Students should be informed that competent generalist skills could address the needs of a community at a district health level.
Acknowledgments
The authors thank Ngkatiseng Molefe of the University of KwaZulu-Natal for her assistance with data collection and transcription of audio recordings. They also thank Busisiwe Ntuli-Ngcobo and Sibongile Mabuza of the University of Limpopo for their assistance with data collection.
References
1. Jones GI, DeWitt DE, Cross M. Medical students' perceptions of barriers to training at a rural clinical school. Rural and Remote Health 7: 685. (Online) 2007. Available: www.rrh.org.au (Accessed 3 November 2012).
2. Ross AJ. Success of a scholarship scheme for rural students. South African Medical Journal 2007; 97(11): 1087-1090.
3. de Vries E, Reid S. Do South African medical students of rural origin return to rural practice. South African Medical Journal 2003; 93(10): 789-793.
4. Tumbo JM, Couper ID, Hugo JF. Rural-origin health science students at South African universities. South African Medical Journal 2009; 99(1): 54-56.
5. Dunbabin JS, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health 3: 212. (Online) 2003. Available: www.rrh.org.au (Accessed 3 November 2012).
6. de Vries E, Irlam J, Couper I, Kornik S, Members of the Collaboration for Health Equity through Education and Research (CHEER). Career plans of final-year medical students in South Africa. South African Medical Journal 2010; 100(4): 227-228.
7. Birks M, Al-Motlaq M, Mills J. Pre-registration nursing degree students in rural Victoria: characteristics and career aspirations. Collegian 2009; 17(1): 23-29.
8. Couper ID, Hugo JF, Conradie H, Mfenyana K, Members of the Collaboration for Health Equity through Education and Research (CHEER). Influences on the choice of health professionals to practice in rural areas. South African Medical Journal 2007; 97(11): 1082-1086.
9. Orpin P, Gabriel M. Recruiting undergraduates to rural practice: what the students can tell us. Rural and Remote Health 5: 412. (Online) 2005. Available: www.rrh.org.au (Accessed 3 November 2012).
10. Veitch C, Underhill A, Hays RB. The career aspirations and location intentions of James Cook University's first cohort of medical students: a longitudinal study at course entry and graduation. Rural and Remote Health 6: 537. (Online) 2006. Available: www.rrh.org.au (Accessed 3 November 2012).
11. She L, Wu B, Xu L, Wu J, Zhang P, Li E. Determinants of career aspirations of medical students in Southern China. BioMed Central Medical Education 2008; 8(59): 1-7.
12. Kurre' J, Scholl J, Bullinger M, Petersen-Ewert C. Integration and health-related quality of life undergraduate medical students with migration backgrounds - results of a survey. Psychosocial Medicine 8: Doc07. (Online) 2011. Available: http://www.ncbi.nlm.nih.gov/pubmed/22049300 (Accessed 25 October 2011).
13. Malau-Aduli BS. Exploring the experiences and coping strategies of international medical students. BioMed Central Medical Education 11: 40. (Online) 2011. Available: http://www.ncbi.nlm.nih.gov/pubmed/21702988 (Accessed 3 November 2012).
14. Garvey G, Rolfe IE, Pearson SA, Treloar C. Indigenous Australian medical students' perceptions of their medical school training. Medical Education 43(11): 1047-55. (Online) 2009. Available: www.ncbi.nlm.nih.gov/pubmed/19874497 (Accessed 3 November 2012).
15. Sreeramareddy CT, Shankar PR, Binu VS, Mukhopadhyay C, Ray B, Menezes RG. Psychological morbidity, sources of stress and coping strategies among undergraduate medical students of Nepal. BioMed Central Medical Education 7: 26. (Online) 2007. Available: www.ncbi.nlm.nih.gov/pubmed/17678553 (Accessed 3 November 2012).
16. Durkin SR, Bascomb A, Turnbull D, Marley J. Rural origin medical students: how do they cope with the medical school environment? Australian Journal of Rural Health 2003; 11: 89-95.
17. Rai M. Operational definitions of urban, rural and urban agglomeration for monitoring human settlements scores. In: Proceedings, 25th Conference on Regional and Urban Statistics and Research. 30 August-1 September 2006; Wroclaw University of Economics, Poland; 2006.
18. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professional to rural and remote areas. Rural and Remote Health 9: 1060. (Online) 2009. Available: www.rrh.org.au (Accessed 3 November 2012).
19. Barrett FA, Lipsky MS, Nawal Lutfiyya M. The impact of rural training experiences on medical students: a critical review. Academic Medicine 86(2): 259-263. (Online) 2011. Available: journals.lww.com/academicmedicine/Fulltext/2011/02000/The_Impact_of_Rural_Training_Experiences_on.28.aspx (Accessed 3 November 2012).



