The concept of vertical integration of education in medicine has been present for many decades in Australia, primarily in teaching hospitals. In this article we define vertical integration in medical education as 'a grouping of curricular content and delivery mechanisms, traversing the traditional boundaries of undergraduate, postgraduate and continuing medical education, with the intent of enhancing the transfer of knowledge and skills between those involved in the learning/teaching process'.
Despite a 30 year history of increasing community based medical education in Australia; there was little impetus for vertical integration until the past 8 years (1990s)1-3. During this time the conjunction of four Australian Commonwealth Government rural health strategies have impacted on medical education. These strategies of funded continuing medical education4, regionalised general practice vocational training administered by General Practitioner Education and Training (
This article will discuss aspects of vertically integrated education and will describe examples observed as a result of our experience within the local Riverland context. Our aims are for this analysis to assist with the current wider debate regarding the educational rationale for vertical integration in medical education, and also to inform regarding effective methods for the implementation of vertical integration.
Methods
This article is based on the authors' extensive collective experience with undergraduate, postgraduate and continuing professional education in the Riverland of South Australia. Of the authors, DR remains a Riverland general practitioner after 30 years, with experience in undergraduate and postgraduate teaching systems, and is a member of the Regional Education Committee of the Riverland Division of General Practice; PW is Professor of Rural Medicine at Flinders University and has been in academic rural practice for 9 years, with a significant previous history of initiating and supervising innovative undergraduate and vocational training programs, and is a member of the Regional Education Committee of the Riverland Division of General Practice; BM has coordinated state wide rural undergraduate medical education programs, and is now the inaugural Director of the Sturt-Fleurieu General Practice Regional Training Consortium, established in 2001, with overall responsibility for the regional vocational postgraduate training program, and PS has been an Administrator of both undergraduate medical education for 7 years and also of regional continuing medical education. These training programs will be described in further detail.
Riverland demography
The Riverland region is an area consisting of 5 main towns, Waikerie, Barmera, Berri, Loxton and Renmark with a total population of 33 000 (Fig 1). The area is situated 250 km north-east of Adelaide, with intertown distances comprising an east-west axis distance of 110 km and a north-south axis distance of 35 km. The 5 towns are serviced by 5 group medical clinics and 2 solo general practices with a combined general practitioner (GP) workforce of 35. A hub-and-spoke model of hospital services, administered through individual hospital boards by a regional health authority, has resulted in higher level medical services and procedures provided at the central hospital in Berri, with primary medical care and hospital services provided in the 4 peripheral towns.
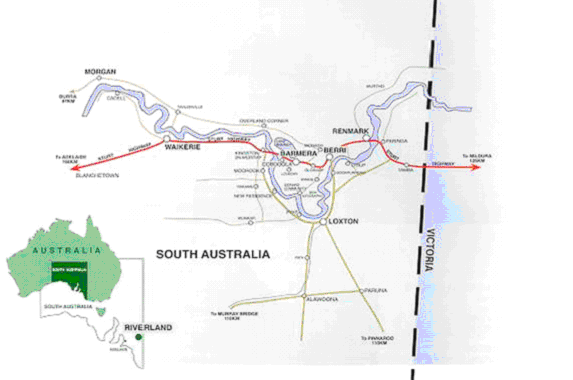
Figure 1: Map of the Riverland in South Australia, area context for the model of vertical integration in medical education.
In the peripheral towns, general medical services are provided by resident GPs through private medical clinics. These clinics also supply medical services for hospital inpatients, with visiting medical staff operating as independent contractors. There are no dedicated hospital medical staff in these towns. Specialist services are supplied either by regional specialists who visit the peripheral towns, or by specialists who visit the Riverland towns on a periodical basis.
In Berri, resident specialists provide services that require higher level hospital facilities, especially for surgical procedures. Specialists from outside the region also visit periodically to provide services not available from resident specialists. There are two surgical trainees providing hospital-based surgical care. GPs in Berri provide non-specialist services to the hospital, and provide emergency assessment and care. There are the three levels of medical education in the region.
Riverland Parallel Rural Community Curriculum
Overseas experience with medical student training suggests that the training of rural origin students through early and repeated rural exposure results in a greater likelihood of practice in rural area13. In 1996 Flinders University engaged GPs in the Riverland of South Australia in order to establish the Riverland Parallel Rural Community Curriculum, known as the PRCC14. This program enabled selected students to undertake an entire year of clinical study based in rural practice. This was a pioneering program established under a Federal Government grant awarded through the Rural Undergraduate Steering Committee of the federal Department of Health and Aged Care (1994). The BM BS course offered to graduate entrants by Flinders University extends over 4 years, with the examination at the conclusion of the third year constituting a substantial ranking hurdle for students. Eight students can be accommodated in the region during their third year of medical studies.
Prior to the inception of the PRCC, local general practitioners, through longstanding arrangements with the University of Adelaide and Flinders University accepted medical students on short-term attachments generally not exceeding 4 weeks. There were no longer term attachments available.
Sturt-Fleurieu General Practice Training Consortium
A Ministerial review of GP training in Australia was initiated in 1997 with the specific intent of examining undergraduate medical education, vocational training and continuing medical education for GPs, and how these elements might be more closely integrated to promote general practice15. As a result of this review, training arrangements for general practice changed dramatically with the formation of a central administrative body, General Practice Education and Training (GPET) ( www.gpet.com.au), the introduction of a regional and contestable system of training, and as a result of the tender process, the development of regional general practice training providers (RTP). Sturt-Fleurieu General Practice Education and Training (SFGPET) ( http://www.sfgpet.com.au), consisting of the Riverland, Barossa Valley, Murray Mallee, Adelaide Hills and Southern Divisions of General Practice, Flinders University, the Royal Australian College of GP (RACGP) and the Australian College of Rural and Remote Medicine (ACRRM) was successful in the tender process and commenced registrar training in 2002. Approximately 50 registrars live and work in this region as part of the GP training program. Prior to the inception of SFGPET, vocational trainees for general practice were attached for a relatively short time to group general practices, operating under a centrally administered RACGP training program.
The notion of Flinders University medical undergraduates, especially PRCC alumni becoming graduate vocational trainees with the Sturt-Fleurieu consortium is attractive, and is one of the goals of investment by Flinders University in both activities.
Riverland Division of General Practice
A functional Division of General Practice is in place in the Riverland, working with the Riverland Health Authority to involve the region's 35 GPs in workforce and health service planning. It is the principal coordinator and supplier of continuing professional development (CPD) events for these doctors.
Results
Indicators of vertical integration
Active inclusion of undergraduate and postgraduate students in CPD events: Riverland Division of General Practice policy has included the awarding of associate member status to PRCC students and Sturt-Fleurieu registrars resident in the area. Aside from their welcomed status, this means that the Division has enabled the students to be present at, and to participate in, CPD activities supported by the Division.
The CPD curriculum has been based on a needs analysis performed on a recurrent basis. This has avoided the tendency to automatically respond to pharmaceutical companies offering to provide a CPD event and allowed greater flexibility in programming to meet the needs of rural doctors, registrars and students. Some teaching events have combined all recipient groups, with others aimed at a particular level, such as the GP obstetricians. When events have been aimed at one particular level, with others invited, we have noted the fostering of a supportive culture so that the non-principal recipients have also gained education and given input. In that way, benefits have been generated that enable learning for all involved. GPs and PRCC administration have acted with initiative to identify local registrar and CPD events that could be useful to the students.
The Division has also hosted regional CPD meetings for both medical practitioners and nurses on a regular basis with structured input from resident specialists in surgery, anaesthetics, orthopaedics and obstetrics. Attendance at these meetings has been useful for students in that they have gained an opportunity to observe a number of aspects of each discipline and to appreciate the teamwork that is required across the region in order to achieve best practice. Appreciation of the teamwork has engendered collegiality and respect between those at different levels of training and practice.
Active inclusion of undergraduate medical students in postgraduate training sessions: Sturt-Fleurieu postgraduate training consortium has placed a significant emphasis on simulation training, especially in the management of medical emergencies. This has presented an opportunity for engagement of PRCC students, as these skills, at a lesser level, are also required by the undergraduate curriculum. A clinical skills laboratory is currently under development in the Riverland for use by healthcare professionals, trainees, and students in the region.
Enhanced in-house training sessions for both vocational and undergraduate students in general practices: Registrars training under Sturt-Fleurieu have been encouraged to be part of intrapractice CPD events with case review and topic presentation that has facilitated discussion between resident medical practitioners, registrars and students on a more informal basis. GPs have recognized that teaching in these forums aids their own learning, students have learned from researching topics for presentation at meetings, and registrars have recognized as they teach students that they have acquired particular advanced knowledge.
Improved involvement of local practitioners in University medical curriculum delivery: The University has encouraged increased involvement and understanding by resident medical practitioners of the curriculum aims, teaching processes, and the different nature of the curriculum that is taught in the PRCC. This curriculum differs from that taught at the University campus in Adelaide in that students do not learn from placements in discipline specific block teaching, but instead rely on clinical exposure to the case load presenting to rural general practices14. Resident GPs and specialists have become familiar with the construction of the PRCC and with the teaching that is required to deliver the curriculum. This was crucial in marking the PRCC as a long-term student attachment compared with a brief attachment of several weeks duration.
Prior to the inception of the PRCC, interaction between universities and regional practitioners occurred infrequently, on a sporadic basis. This has changed now, with the formation of a Riverland teaching faculty of the University. GP supervisors have been appointed in each town and all practitioners have been encouraged to derive maximum benefit from the provision of teaching for students based in their practices. One particular benefit of the teaching process is that the practitioner involved has acquired an opportunity to reflect on what they do and the reasons for it.
GP supervisors have used a variety of techniques to provide one to one teaching for PRCC students. They have recognized that when students occupy a purely observational role in GP attachments, their interest is soon lost. Students have therefore been encouraged to work alongside GPs encountering patients in various ways, resulting in the development of skills in history taking and examination, diagnosis, interpretation of investigations, and the formulation of management plans. This has occurred during consulting sessions in general practice, in accident and emergency practice, and in the management of hospital inpatients. GP supervisor observation and the provision of specific feedback to the student have been essential in optimizing the results of these activities. In addition, GP supervisor assistance with student research and understanding of issues arising from problem based learning cases has been programmed on a regular basis. Finally, the value of GP supervisors to students through the provision of specific assistance in pre-examination study has been highlighted in PRCC internal evaluations.
The involvement of resident medical practitioners in significant student assessment has required an understanding of the curriculum. With understanding have come opportunities to identify further aspects of linkage and curriculum delivery that have been implemented using a 'bottom up' approach. Sometimes local innovation created from this process has encouraged changes in policy in the wider University.
Closer involvement by local practitioners with curriculum delivery and assessment has occurred when local practitioners have contributed to teaching through the application of their special expertise and effort. Specific tutorials in internal medicine have been given by a general practitioner with particular interest in this discipline, while specialists in private practice have, in collaboration with university teaching departments, established special teaching modules in surgery and anaesthesia. Local general practitioner input to students' problem based learning has regularly occurred. There have also been frequent opportunities for teachers and students to discuss issues of student professional development, and a module of Personal and Professional Development must be successfully passed to allow graduation to the final year of the medical course. Pre-examination tutorial programs have been designed and conducted by medical practitioners within the region, who have also provided simulated formative clinical assessment examinations.
Riverland PRCC faculty members actively contribute to the writing of summative examination material, the setting of summative examinations, and the practical summative assessment of students at the conclusion of the third year of the medical course. None of these activities occurred prior to the year 2000.
The activity described above has altered university policy with regard to long-term regional student attachments. The Riverland PRCC is now regarded by the University as a program which encourages and delivers student development, which has been evidenced by improved examination performance by students and by their development of a sound clinical approach to patients. In addition the PRCC has been a model for the development of a further PRCC in the south-eastern region of South Australia16. The PRCC has influenced university policy by providing a template which may be adapted to engage medical practitioners in outer metropolitan areas. University policy has been further influenced by the establishment of the Flinders University Rural Clinical School administrative centre in the Riverland region that has brought benefit through the provision of other health related courses.
In considering the evolution of vertical integration in the Riverland region, it appears that the opportunity to establish effective linkages in the organizational system of education and training in a learner centred continuum of education was attractive. Evidence for this is demonstrated by the maturing processes of learning within the larger practices in each main town, and the willingness of resident GPs with little previous academic or teaching experience to become actively involved. In addition a horizontal integration of medical education was available at both undergraduate and postgraduate levels, integrating the disciplines of medicine, surgery, obstetrics, paediatrics, and psychiatry. This is very appropriate, as rural practice spans those disciplines and within group practices, individual practitioners have specific expertise in them.
Development and coordination of training programs in regional areas
In order to improve the regional curriculum taught at both undergraduate and postgraduate levels, continual dialogue has occurred between Flinders University academic staff at both central and rural teaching sites. The integration of delivery of these programs through Flinders University has created a critical mass of academic staff and administrative staff. Opportunities have been taken for joint authorship and presentation of research and teaching. This has encouraged shared credit and has engendered trust both within the local teaching faculty and within the cohort of employed university staff.
While there are no intern positions for junior and prevocational practitioners available in the Riverland, other programs in the Flinders University Rural Clinical School are associated with such positions under the RRAPP program6. Experience gained with resident intern positions should be readily transferable using University resources, which should assist in preventing duplication of work in other regions.
Integration of students with patient care teams: Students in the Riverland have taken an active role in patient care. This has enabled the formation of teams comprised of students, registrars and resident practitioners. Interestingly, the key motivation for this may be a workforce, rather than educational goal. Experienced rural medical practitioners have recognized that an opportunity to provide a significantly positive educational experience can result in an improved profile for their practices, especially to medical practitioners intending to reside in a rural location.
Thus an acceptance of medical students and registrars as part of a team providing medical services has occurred. Medical students have particularly appreciated this inclusiveness, and have been prepared to trade it for absence from their tertiary hospital during their principal year of preparation for clinical examinations. Despite the increased work placed on medical practitioners during the initial phases of the student year, the investment has often later been rewarded by the students' willing involvement in supervised clinical work. That involvement has added value to patient care, improved the profile of medical practice to the community, and has relieved the workload on individual practitioners17.
Development of an educational culture in regional areas: A culture of education and training has been found attractive to some GP registrars, who have been particularly sensitive to placements that have focused on them providing workforce relief, compared with those which have provided an educational experience that has enabled them to obtain skills that successfully equip them for general practice. Senior trainees have often been sought by students in a similar manner to hospital based students seeking assistance from registrars who are actively working towards postgraduate qualifications, and who consequently are capable of teaching.
Specific opportunities for integration with postgraduate training: The development of the undergraduate PRCC in the Riverland has provided two unique opportunities for integration with regional postgraduate training.
The first has been to monitor the progress of students through the undergraduate rural based program into their chosen domain of practice. Evidence already suggests that these graduates will move into general practice. As of 2003, a total of 26 PRCC graduates have completed pre-registration service positions with 19 (73%) commencing training in pathways leading to rural practice. Although SFGPET is still maturing, it is expected that many of these graduates will elect to stay in this region to complete vocational training.
Given the contestable nature of post-graduate training, consortia will be in competition with each other for applicants. It is therefore in the interests of SFGPET to attract applicants from the graduate pool supplied by Flinders University, and especially to focus on those who have perceived their rural experience to be of value.
The second has been to provide general practice registrars with the opportunity to be involved with undergraduate teaching. In teaching hospitals, registrars are often involved with teaching, especially in the emergency setting, or in the setting of day to day ward management. In the Riverland, registrars have been granted admitting privileges at local hospitals. Whilet their hospital based clinical activity is monitored by GP supervisors, there is usually an improvement in confidence and skill as they approach the qualifying examinations for vocational general practice. Their increased confidence is expressed to the students through teaching of basic clinical skills and diagnostic and management processes, with students allowed to manage cases, in concert with them. Internal evaluation of teaching programs conducted by the PRCC consistently indicates that one of its key strengths is the large number of opportunities for students to receive teaching on a one to one basis. It is likely that PRCC students develop sufficient experience and confidence to consistently achieve high marks in Objective Structured Clinical Examinations (OSCE). Thus we have strong evidence of vertical integration in medical education, resulting in a number of benefits.
There is also evidence of vertical integration in metropolitan hospital based teaching with general practice registrars involved in high fidelity patient simulation teaching of interns based at Flinders Medical Centre as part of a joint research initiative with the Flinders University Clinical Simulation Unit.
Elements underpinning Vertical Integration
In order for vertical integration to emerge successfully within a region, it would appear that certain elements need to be fostered. These elements then contribute to a platform on which vertical integration rests, with the subsequent benefits accruing from the process being clearly evident to the participants. Our experience suggests that five such elements were identifiable in the Riverland.
1. Raised educational stakes: The educational stakes have been raised at the student level through the establishment of the PRCC. The region is responsible for providing an entire year of learning for students immediately prior to their major clinical examinations. All partners associated with the program have been keenly aware of their role in providing quality education. In a similar way, the establishment of SFGPET consortium has raised the educational stakes at registrar level, in that the region has become responsible for the registrar attaining vocational qualification in contrast with the responsibility previously vested in the RACGP training program.
The ownership of regional medical practitioners in the academic results of both undergraduate and postgraduate training is important. It should be noted that the university expects one set of (examinable) outcomes for all students, but has allowed a variety of paths for students to select in order to attain the required outcomes. This has resulted in the local evolution of plans for efficient and effective curriculum delivery.
2. Local ownership: Intrapractice continuing medical education events have illustrated an important principle that applies to the generation of the linkages that contribute to a vertically integrated educational system. The principle is that vertical integration within a local system relies on its generation from within the system itself. It is rarely delivered with success solely by agents outside the local system, but it may be assisted by their involvement.
3. Broad university role: The linkages between the training consortium and the University undergraduate programs have offered closer organizational ties. The key performance indicators lie in the delivery of education in practice for both undergraduates and registrars. The involvement of Flinders University through both undergraduate and postgraduate programs has added a consistent academic presence to the region in addition to providing a coordinating facility for education.
When medical practitioners have become involved in teaching they have been offered facilitation with their applications for University Academic Status. The medical and social capital of the region have been enhanced by the provision of academic medical services that have exposed and integrated potential new practitioners into education and training provided within the region. Practices now actively advertise their teaching status when recruiting new doctors. Community feedback has suggested that the status of education in the area has been enhanced by the University presence18.
4. Longer attachments: The opportunity for both students and registrars to spend longer periods of time in Riverland general practices has not only raised the stakes for the region, but also has enabled other benefits to occur. Longer attachments of students and GP registrars has encouraged trust and investment to build at the local and interpersonal levels, thus positioning vertical integration as a norm within the system, not as an exception. The longer attachments have also enabled the students and registrars to develop more significant roles in patient care, resulting in a team approach that has provided educational benefits, as discussed previously. Longer attachments are also important in allowing the development of a sufficient degree of student autonomy within the practice workforce enabling them to work under minimal supervision with consenting patients. This provides financial benefits to the practice because GP s are able to delegate duties to students thus creating time for them to provide clinical services to other patients.
5. Shared workforce vision: A workforce planning approach combining the Division of General Practice and the Regional Health administration has been crucial in enabling a shared understanding of direction, effort, and funds. A formal partnership between the Riverland Division of General Practice and the Riverland Health Authority has resulted in the creation of the Riverland Medical Workforce Advisory Group (RMWAG). This small but active group of five has contributed strongly to the increase in medical workforce in the region19. In working to stabilize the medical workforce, RMWAG has been able to advertise the PRCC as a successful community based undergraduate teaching program that has created opportunities for both registrars and experienced GPs to be part of an enhanced teaching environment that is supported by Flinders University. The recognition that education at all levels is required as part of a sustainable long term solution to workforce planning has underpinned the integration of education at the local level. Further evidence of the development of a vertically integrated environment has been the return to the region of undergraduate students as GP Registrars, which itself provides encouragement to the medical and wider community. The continuation of this process will be an important factor underpinning the outcomes of Riverland regional educational programs.
Future options
The work and processes described above require consolidation. Administrative matters that relate to PRCC sustainability, for example, student housing, accommodation within practices with the provision of designated clinical and working space, and teaching program construction together with evaluation, require considerable ongoing work and planning through the Flinders University Rural Clinical School.
Sturt-Fleurieu GP Education and Training (SFGPET) has conducted training since 2002. It has recently sought accreditation within the national general practice training program. The national program is newly established, and will require consolidation as will the activity of SFGPET. Currently there are concerns that the distribution of prospective applicants for vocational training in general practice is biased towards other areas of Australia, and that the supply of candidates for training in South Australia will not be sufficiently high. SFGPET will require the development of strategies that will place it in a favorable position to attract vocational trainees for general practice.
There is a need for political advocacy, especially to State health authorities. Programs such as the PRCC, and that offered by SFGPET create hope for attraction of medical practitioners to rural South Australia. The majority of funding for these activities comes from the Commonwealth of Australia. To maximize results, involvement of the State government is essential.
While the PRCC is offered to students based in general practice, specialists play a vital role in the teaching of their disciplines. It is likely that specialists will consider themselves to be more supported when liaison and assistance is provided in a substantial and continuing manner by University departments. It is planned to provide this assistance through the Flinders University Rural Clinical School.
The continuing medical education curricula could be further developed by encouraging individual practitioners to use the new professional development program (PDP) developed by the ACRRM. The PDP requires practitioners to analyse their practice profiles and to tailor their continuing medical education to reflect that profile. Aggregating the profiles across the region could aid the Division of General Practice in deciding the most valuable continuing medical education options to pursue. This pursuit could be assisted by resources supplied by both ACRRM and the University. This would create an opportunity for students to begin the logging of experiences in a PDP program during their undergraduate years, which could contribute to a log assessment for future employment. We see an opportunity for ACRRM to engage students by extending an invitation to become involved in this process. ACRRM could also consider offering education to undergraduate students in partnership with Universities. This may be especially useful to students electing to spend significant time in rural teaching sites.
The further development of programs which address the relatively neglected area of training for junior and prevocational practitioners will achieve vertical integration on a wider scale. Mention has been made of potential activity within Flinders University Rural Clinical School that may assist this process.
Conclusion
Given the benefits to the Riverland medical education programs, it is not surprising that vertical integration of medical education is a popular goal in many rural regions throughout the world. Although different contexts will result in different functional arrangements, it could be argued that the five principles outlined in this paper can be applied in any region.
Vertically integrated educational systems in the Riverland have provided benefits at various levels. The region has benefited from the creation of an educational environment that has been significant in attracting both experienced practitioners and those in training. Thus workforce numbers have been positively influenced, and this has resulted in an improvement in patient access to medical services.
Medical practices have been assisted and invigorated through the development of an improved educational culture that offers strong incentives. Both senior and junior medical staff have derived professional development and satisfaction though involvement in the process.
Registrars have derived specific benefits, due to their involvement in teaching students. Both students and registrars, in preparing in a self directed manner for similar examination hurdles, have participated in a culture of learning, which has conferred academic benefits on them. Good academic results have been achieved by students and registrars. Not only have the individual students and registrars taken pride in the results, but also the senior teachers, nursing staff, and indeed the rural community have developed a sense of ownership. The partnership between Flinders University and the region has been enhanced through the development of a vertically integrated educational system.
Raising the educational and assessment stakes for the region, creating local ownership, enabling educational providers to span different levels of the education continuum, encouraging longer attachments of students and registrars, and articulating a shared vision of locally delivered multi-level medical education in workforce planning will encourage innovative local educational solutions that, for reasons of efficiency and effectiveness, are naturally vertically integrated.
References
1. Hays RB. A training programme for rural general practice. Medical Journal of Australia 1990; 153: 546-548.
2. Craig M. Rural practice - time to teach. Medical Journal of Australia 1995; 162: 231.
3. Hays RB. Integration of undergraduate and postgraduate general practice education - does it work? Australian Family Physician 1997; 26(Suppl2) : S83-S86.
4. Holub L, Williams B. The general practice rural incentives program, development and implementation: progress to date. Australian Journal of Rural Health 1996; 4: 117-127.
5. RUSC Committee. Rural doctors: reforming undergraduate medical education for rural practice. Canberra: Australian Government Publishing Service, 1994.
6. Mugford B, Martin A. Rural rotations for interns: a demonstration program in South Australia. Australian Journal of Rural Health 2001; 9(Suppl): S27-S31.
7. Glasgow N. Vertical integration of general practice education - what currently is happening, and what helps or hinders such integration? Final Report. Canberra: Academic Unit of General Practice, Canberra Clinical School, University of Sydney, 2002.
8. Moores DG, Woodhead-Lyons SC et al. Preparing for rural practice: enhanced experience for medical students and residents. Canadian Family Physician 1998; 44: 1045-1050.
9. Ramsey PG, Coombs JB et al. From concept to culture: the WWAMI program at the University of Washington School of Medicine. Academic Medicine 2001; 76: 765-775.
10. Worley PS, March R et al. Scanning the horizon of training for general practice. Medical Teacher 2000; 22: 452-455.
11. Bowman R, Crouse B. Community driven approach: the rural component community-driven medical education: The rural component. UNMC Public Site (www.unmc.edu) (online) 2002. http://www.unmc.edu/Community/ruralmeded/community_driven_JRH.htm (accessed 11 December 2003).
12. Heady H. West Virginia Rural Health Education Partnerships West Virginia (online) 2002. http://www.unmc.edu/Community/ruralmeded/model/medsch/west_virginia_rural_health_educa.htm (accessed 11 December 2003).
13. Verby JE. The Minnesota rural physician associate program for medical students. Journal of Medical Education 1988; 63: 427-437.
14. Worley PS, Silagy C et al. The Parallel Rural Community Curriculum: an integrated clinical curriculum based in rural general practice. Medical Education 2000; 34: 558-565.
15. Commonwealth Department of Health and Aged Care, General practice education: the way forward. The report of the Ministerial Review of General Practice Training. Canberra: Commonwealth Department of Health and Aged Care, March 1999.
16. Walters L., Worley P, Mugford B. Parallel Rural Community Curriculum: is it a transferable model. Rural and remote Health 3 (online), 2003: 236. Available from: http://rrh.org.au (accessed 11 December 2003).
17. Worley PS, Kitto P. A hypothetical model of the financial impact of student attachment on rural general practice. Rural and Remote Health. 1. (Online), 2001: 83. Available from: http://rrh.org.au (accessed 11 December 2003).
18. Oswald NO. Parallel Rural Community Curriculum (PRCC) Final Evaluation Report. Adelaide, SA: Flinders University, 2002.
19. Lehmann D, Rosenthal D. Forward planning on recruitment and retention of General Practitioners. In: Proceedings, Australian College of Rural and Remote Medicine Scientific Meeting, May 2002. Australia. 2002.
Abstract
Introduction: Vertical integration of medical education is currently a prominent international topic, resulting from recent strategic initiatives to improve medical education and service delivery in areas of poorly met medical need. In this article, vertical integration of medical education is defined as 'a grouping of curricular content and delivery mechanisms, traversing the traditional boundaries of undergraduate, postgraduate and continuing medical education, with the intent of enhancing the transfer of knowledge and skills between those involved in the learning-teaching process'.
Methods: Educators closely involved with vertically integrated teaching in the Riverland of South Australia present an analytical description of the educational dynamics of this system.
Results: From this analysis, five elements are identified which underpin the process of successful vertical integration: (1) raised educational stakes; (2) local ownership; (3) broad university role; (4) longer attachments; and (5) shared workforce vision.
Conclusions: Given the benefits to the Riverland medical education programs described in this paper, it is not surprising that vertical integration of medical education is a popular goal in many rural regions throughout the world. Although different contexts will result in different functional arrangements, it could be argued that the five principles outlined in this article can be applied in any region.
Key words: community, medical education, Riverland, South Australia, vertical integration of medical education.
You might also be interested in:
2006 - Health and information in Africa: the role of the journal Rural and Remote Health



