Calcific aortic stenosis is the most common cardiac valve condition in the Western world, with age-related degeneration being the most common cause1. Aortic sclerosis is present in up to 25% of adults over the age of 65 years, with 16% of this patient group progressing to severe aortic stenosis within 7 years2,3. Thus, surveillance of this condition (usually by echocardiography) is advised, based on the degree of severity and presence of a bicuspid valve1. Aortic stenosis is usually identified by co-incidental echocardiogram finding, identification of a murmur or, in more advanced cases, through presentation with clinical symptoms. The first two situations rely upon clinical examination and referral for tests; the latter situation requires the patient to report their symptoms. Treatment of severe aortic stenosis normally involves surgical replacement or, more recently, percutaneous valve replacement1.
There is some evidence that rural populations may have a higher prevalence of certain cardiovascular diseases, such as heart failure4. In addition, in certain diseases rural patients appear to present later in their disease process compared with urban patients. For example, rural patients with colon or lung cancer have been shown to have more severe disease at presentation5, while outcomes in other more acute illness such as asthma are worse in rural patients6. The reasons for these differences are not clear. It is possible that access to doctors and tests may be more problematic in remote and rural areas. Access may be restricted by lower provision, unreliable transport networks or poor weather conditions. Rural populations are also potentially more stoic and therefore delay seeking medical assistance, although the evidence for this is generally anecdotal.
The aim of this study was to investigate whether patients with aortic stenosis who live in rural areas present later in their disease process compared with patients living in urban areas. The results of this study may be of interest to service providers because currently many echocardiogram services are centralised.
Design and setting
The study was performed in a remote Scottish regional hospital with a catchment population of 205 966.
The method was a retrospective analysis of a cohort of all patients diagnosed with aortic stenosis.
Patient identification
All patients with a diagnosis of aortic stenosis over a 9 year period (31 November 1999 to 1 December 2008) were identified using selected International Classification of Diseases-10 (ICD-10) hospital discharge codes: I06.0, I06.2, I08.0, I08.2, I08.3, I08.8, I42.1, I08.0, Q23.0, Q23.1, I06, I35.0, I35.1, I35.2, I35.8, I35.9, I39.1, Q23.0, Q23.8. Further, patients were identified from existing local echocardiographic databases. This is the only echocardiogram service for the North Highland Region and all patients who lived in the area who had an echocardiogram were included. Aortic stenosis was defined as a peak gradient of at least 25 mmHg across the aortic valve measured by Doppler. Patients with prior aortic valve replacement at presentation were excluded.
Clinical parameters
The following data were extracted for each patient: gender, age and peak pressure gradient across aortic valve (mmHg), presence of a non-native aortic valve and patient GP practice. Extracting data regarding GP practice allowed a Clinical Peripherality Index score to be assigned to each patient (0=most urban; 5=most rural). Clinical peripherality is determined by the nature of the practice and its location relative to secondary care and administrative and educational facilities. It has features of both gravity model-based and travel time/accessibility indicators7.
Data handling and statistical analysis
Data were stored in a secure and anonymised electronic database (Microsoft Excel). Data were analysed using descriptive statistics followed by ANOVA to explore for any effect of clinical peripherality. The level of significance was p <0.05.
Ethics approval
This survey used fully anonymised aggregate data collected during standard clinical management of patients. The primary goal of the study was to determine if there were deficiencies in service provision. Thus, as a service evaluation, formal ethical approval was not deemed necessary.
A total of 709 patients diagnosed with aortic stenosis were identified by the primary search. A total of 104 patients were excluded from the analysis (60 patients had an aortic valve replacement present at their first available echocardiogram; 22 patients had no detailed echocardiographic data available; 22 patients lived out of the study area), leaving a final cohort of 605 patients.
The mean patient age was 73 ± 13 years and 336 (54%) were male. The peak gradient on presentation was 41.1 ± 26.7 mmHg. There were no differences in age, gender, peak gradient or peak velocity versus Clinical Peripherality Index (Table 1).
Table 1: Participant characteristics according to Clinical Peripherality Index
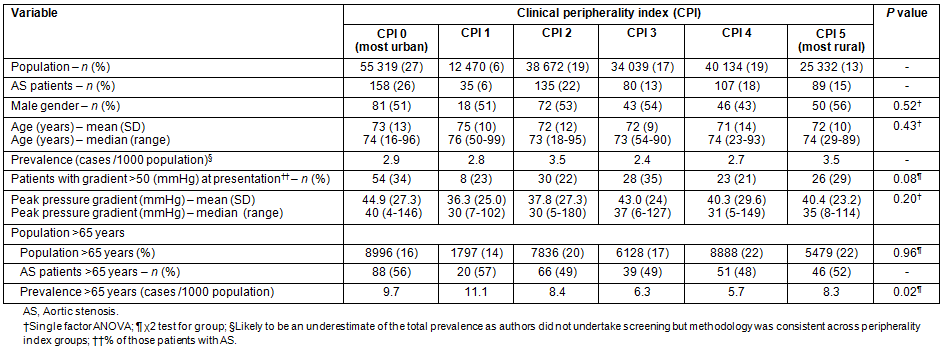
Discussion
This study has shown that in the remote area under study there was no rural gradient in terms of severity of aortic stenosis at presentation. This suggests that patients in the rural areas of the study do not present later in their disease trajectory, and that the current centralised provision of echocardiography service appears adequate for this patient population.
The results of this study were slightly incongruent with data from other studies where there were differences between rural and urban populations in treatment of cardiovascular disease4. There are several possible explanations for this. Firstly, Scotland has a National Health Service which is free to all at the point of access, which could negate some fiscal barriers that may exist in other healthcare populations (eg Australia). Furthermore, the north of Scotland is less isolated than remote areas of other countries, such as Australia. As such, Scottish urban-rural disease gradients could be more subtle. In addition, patients in the study area have access to echocardiography which is relatively easy for GPs to access. Although echocardiograph services may be geographically remote from patients' place of residence, in a recent local survey, rural GPs reported satisfaction with the current echocardiography service provision8.
Second, the disease process itself may also have had an impact. Unlike some cancers (colon and lung), where there is some evidence to suggest delayed diagnosis in rural patients5, aortic stenosis is a slowly progressing disease and this may have negated any clinical effect of a short delay in diagnosis in our cohort. However, it is still possible that a gradient may exist in more remote populations or among those with less easy access to primary care physicians.
Older patients may find it more challenging to access their healthcare professional and to travel to centralised echocardiography services. There appeared to be a trend towards a greater proportion of older patients in the remote areas but this was not statistically significant. There was a statistical difference in the proportion of patients over 65 years in each CPI group who were diagnosed as having aortic stenosis but this was not a linear relationship across the areas, and thus this difference does not appear to be related to rurality.
Potential limitations
The authors reported the prevalence of patients with known aortic stenosis in their location; however, it is possible that some patients with aortic stenosis were not identified and thus the true prevalence is likely to be higher than reported. However, all patients who had had an echocardiogram in the region over a 9 year period were captured and it is unlikely that a considerable number of patients with known aortic stenosis were missed. The urban-rural analysis of aortic stenosis was conducted using a Clinical Peripherality Index, which was based upon the location of patients' GP practices. It is possible, although unlikely, that an analysis by patients' home postcodes may have produced different results, although most patients, especially in rural areas, are registered with their local GP.
This study found no urban-rural gradient in the severity of aortic stenosis at presentation. This suggests that patients in this remote areas of Scotland do not present later in their disease trajectory and, as such, there is little requirement to improve the availability of echocardiography services or to enhance screening arrangements in rural areas for this patient population. Provision of more local echocardiography services could be one method of reducing the sometimes considerable distance that rural patients must travel to and from hospital appointments; however, these results show it would not be likely to improve access to care for patients with aortic stenosis.
References
1. Bonow RO, Carabello BA, Chatterjee K, de Leon AC Jr, Faxon DP, Freed MD, et al on behalf of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. 2008 focused update incorporated into the ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to revise the 1998 guidelines for the management of patients with valvular heart disease). Endorsed by the Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. Journal American College of Cardiology 2008; 52(13): e1-142.
2. Otto CM. Aortic stenosis: even mild disease is significant. European Heart Journal 2004; 25(3): 185-187.
3. Lindroos M, Kupari M, Heikkila J, Tilvis R. Prevalence of aortic valve abnormalities in the elderly: an echocardiographic study of a random population sample. Journal of the American College of Cardiology 1993; 21(5): 1220-1225.
4. Clark RA, McLennan S, Eckert K, Dawson A, Wilkinson D, Stewart S. Chronic heart failure beyond city limits. Rural Remote Health 5(4): 443. (Online) 2005. Available: www.rrh.org.au (Accessed 24 April 2013).
5. Campbell NC, Elliott AM, Sharp L, Ritchie LD, Cassidy J, Little J. Rural and urban differences in stage at diagnosis of colorectal and lung cancers. British Journal of Cancer 2001; 84: 910-914.
6. Jones AP, Bentham G, Horwell C. Health service accessibility and deaths from asthma. International Journal Epidemiology 1999; 28: 101-105.
7. Swan GM, Selvaraj S, Godden DJ. Clinical peripherality: development of a peripherality index for rural health services. BMC Health Service Research 2008; 8: 23.
8. MacKenzie E, Smith A, Angus N, Menzies S, Brulisauer F, Leslie SJ. Mixed-method exploratory study of general practitioner and nurse perceptions of a new community based nurse-led heart failure service. Rural Remote Health 10(4): 1510. (Online) 2010. Available: www.rrh.org.au (Accessed 24 April 2013).

