Dental emergencies are often not optimally managed by medical primary care service providers1. In fact, dental complaints have been reported to constitute a significant proportion of total Emergency Department (ED) presentations, with overseas studies reporting figures from 1%2 to 3.8%3. These presentations can have a significant impact on service delivery in terms of the quality of the dental treatment provided as well as the redirection of acute services away from more serious presentations4. Effective and efficient management of dental presentations through the provision of education supported by appropriate dental emergency resources may benefit emergency medical service provision5-7. This study discusses the effectiveness of an educational workshop intervention through the uptake and perceived usefulness of resources used to treat dental emergencies, developed by author (TS) for Westmead Centre for Oral Health and supplied by the NSW Rural Doctors Network (NSW RDN).
Following a standardised four-hour multimodal educational workshop comprising a didactic slide presentation, case discussions, simulation and multimedia elements, participants were surveyed at 6 months using a single questionnaire type instrument. Topics included dental nomenclature, management of traumatic dental injuries, dental anaesthesia, dental infections and haemorrhage. Responses were returned by pre-paid post or email. One reminder letter or email was sent within four weeks to non-responders. The instrument had been piloted for content validity among ED clinicians after review from a multidisciplinary panel that included dentists and emergency physicians. Reliability was tested using Cronbach's split-half analysis (0.79) across comparable questions.
Participants were grouped according to numbers and clinician experience, to aid in statistical analysis (Fig1). Workshops were delivered by the same educator to the 242 voluntary participants invited to enrol. Participants included 18 emergency specialists, 62 general practitioners, 33 intern/resident/students, 70 emergency registrars and 59 career medical officer/non-emergency registrar/nurse practitioners. Participation was guided by factors such as personal interest in the subject matter, or availability due to rostering. Sites included 11 regional and rural Australian EDs, three rural medical conferences and one rural division of general practice. Workshops were conducted in the states New South Wales (NSW), Queensland and Victoria between 2009 and 2010. A number of resources (Fig2) were made available for order following the workshops. One hundred and seven dental resource units were supplied between October 2006 and June 2011. The majority were distributed throughout NSW (n=70), 58 of which went to rural locations. Additionally, the resource was sent to Queensland (17), Victoria (14), South Australia (3) and the Northern Territory (3).
The questionnaire included questions on whether the dental resource supplied by NSW RDN had been utilised to treat dental emergencies and the perceived usefulness of items contained within the resource. An open-ended question inviting comments regarding the resource was also included.
Completion of questionnaires was voluntary and data was de-identified to maintain privacy. Data analysis included frequencies and cross tabulations using chi-square tests with significance set at p<0.05. Calculations were performed using PASW statistics v18 (http://www.spss.com.hk/statistics/). Further data on the distribution of the dental resource was provided by the NSW RDN.
Ethics approval
This multi-site study had both University of Sydney and Concord Repatriation General Hospital human research ethics approval (CH62/6/2009-010) as well as relevant site-specific approvals.
There were 181 workshop participant questionnaires returned at 6 months, a response rate of almost 75%. The majority of responders were in rural practice (54%) and urban (37%) practice with the remainder remote.
Almost 30% of respondents had used the dental resource in the past 6 months, with 96.6% having received no further dental education within the last 6 months.
A significant correlation (p=0.02) existed between professional category and use of the dental resource, with emergency registrars (41.2%) and specialists (37.5%) having used the dental resource most within their group, while GPs (10.3%) made least use of this resource (Fig1).
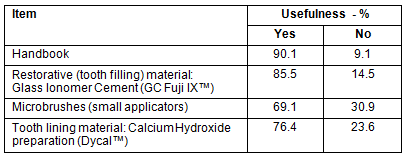
Of the individual items making up the dental resource, the Dental Handbook (90.1%) was deemed most useful and the microbrushes (69.1%) least useful (Table 1).
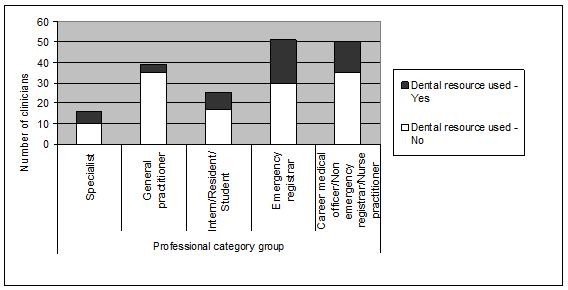
Figure 1: Medical team use of dental resource.
Table 1: Reported usefulness of items within the dental resource
There were 27 responses to the open-question regarding the dental resource. Positive feedback regarding the usefulness predominated (n=12) ,as well as comments relating to availability and access to this resource (11). Comments were also made that items in the resource went missing (3) and that the handbook 'fell apart' (1).
Discussion
Dental emergencies, which constitute 1% to 3.8% of ED presentations in UK and US studies1, commonly present to primary care providers who may be unable to access dental expertise. Subsequently, these providers find themselves managing these presentations with limited knowledge and resources. The high response rate achieved by our study may in part be attributed to the high relevance and benefit participants placed on this education activity. Such strategies have been found most effective in improving response rates to surveys involving physicians8.
This study has shown the perceived usefulness of the items that make up the dental emergencies resource following a multimodal workshop; these items are listed (Fig2). Education in the use of the resource was conducted on dental simulation models during the multimodal workshops in which participants were instructed to repair a complicated and an uncomplicated crown fracture, as well as splinting of teeth following an avulsion. This was to educate participants in the management of common traumatic dental injuries. Instruction was also given in dental anaesthesia (for pain control), management of intra-oral haemorrhage and dental infections, all of which can present as emergencies9.

Figure 2: Contents of dental resource.
The emergency Dental Handbook was found to be the most useful item contained within the resource, as it provided information supported by photographs on tooth nomenclature and anatomy, dental anaesthesia, crown fractures, avulsions and luxations, suturing and mixing of materials. Pages were of thin cardboard laminated to facilitate durability and decontamination in ED settings.
Glass Ionomer Cement (GC Fuji IX?) and calcium hydroxide (Dycal?), which were also deemed highly useful by respondents, have been suggested for use in the emergency treatment of teeth10-12 as well as for use in emergency dental kits6. The long shelf life, ease of use, low cost, safety and effectiveness of these materials make them ideal for use outside the dental surgery. The microbrushes, which are used to apply Dycal? in cases of pulpal exposure, were deemed less useful. This can be explained by the less frequent occurrence of this type of injury and therefore the lower utilisation of this resource.
Approximately half of the dental resource units were provided at no cost to NSW rural hospitals, with those supplied outside NSW were provided on a cost-only recovery basis, in the vicinity of AU$300.
There was surprisingly no association between practice location and use of the dental resource. This may suggest that all locations, from metropolitan to remote, found the items provided by the dental resource equally useful. This hypothesis is consistent with the many requests received by the workshop facilitator (TS) to deliver dental workshops to metropolitan EDs to enable them to better manage dental presentations.
It is likely that cost, access and service hour availability are reasons why many patients with these dental complaints present to EDs3 rather than dental surgeries. Responders who used items in the dental resource were more likely to be emergency registrars and emergency specialists. This is not surprising given that most of the educational workshops were conducted in hospital EDs where the resource was more likely to be available. There was an agreed strategy between the workshop facilitator (TS) and the NSW RDN that the dental emergency resource would be made available to participants who had undergone the workshop training, as hospital EDs most commonly sourced training and therefore would make most use of the resource. In this study, general practitioners were less likely to be associated with hospital EDs, compared to emergency registrars, and this would explain lower use of this resource be GPs. Our results need to be interpreted in light of the proportions of the different clinician groups in our sample who attended the original workshops, as this may affect access to the resource.
Seventy percent of respondents had not used the dental resource in the previous 6 months. This may be explained by possible lack of access to this dental resource, or the clinicians may have been working in areas of medicine where there was no need for this resource. Levels of access to the resource was not specifically recorded but, in light of the usual distribution patterns of the resource, could be assumed to be less in rural general practices. An alternative explanation would be patient presentation patterns with dental emergencies.
As 63% of study respondents were either rural or remote practicing clinicians, the education intervention, together with the supporting resource, would appear more relevant to rural practicing clinicians.
Responses to open-ended questions were generally positive, with typical comments including 'great resource', 'great to have and I take it to all my rural locums', 'returned to Sweden and lack the kit' and 'very, very useful'.
Comments pertaining to resource access and availability included 'kit not funded for in Queensland', 'need kit at current hospital I am working at' and 'waiting for delivery of kit'. Such comments help validate the usefulness of the items contained within the dental emergencies resource.
The effectiveness of a brief multimodal workshop on educating primary care clinicians in the management of dental emergencies can be shown by the uptake and use of appropriate supporting resources. Such resources can potentially help primary care providers in their delivery of effective treatment for such presentations. There may also be particular relevance for rural and remote practice, where access to dental services can be more limited.
The items contained within the dental emergencies resource provided by the NSW RDN were positively endorsed by clinicians who made use of such a resource and missed by clinicians who could not access the resource.
References
1. Skapetis T, Gerzina T, Hu W. Review article: Management of dental emergencies by medical practitioners: recommendations for Australian education and training. Emergency Medicine Australasia 2011; 23(2): 142-152.
2. Hill CM, Burford K, Thomas DW, Martin A. A one-year review of maxillofacial sports injuries treated at an accident and emergency department. British Journal of Oral and Maxillofacial Surgery 1998; 36(1): 44-47.
3. Manski R, Cohen LA, Hooper FJ. Use of hospital emergency rooms for dental care. General Dentistry 1998; 46(1): 44-47.
4. Rowley ST, Sheller B, Williams BJ, Mancl L. Utilization of a hospital for treatment of pediatric dental emergencies. Pediatric Dentistry 2006; 28(1): 10-17.
5. Subhashraj K. Awareness of management of dental trauma among medical professionals in Pondicherry, India. Dental Traumatology 2009; 25(1): 92-94.
6. Lobay K. Introducing emergency dental kits into Edmonton hospitals. Canadian Journal of Emergency Medicine 2010; 12(1): 73.
7. Needleman HL, Stucenski KW, Forbes P, Chen Q, Stack AM. Massachusetts emergency departments' resources and physicians' knowledge of management of traumatic dental injuries. Dental Traumatology 2012; online early version, accessed 1 July 2012.
8. VanGeest JB, Johnson TP, Welch VL. Methodologies for improving response rates in surveys of physicians. A systematic review. Evaluation & the Health Professions 2007; 30(4): 303-321.
9. Douglass AB, Douglass JM. Common dental emergencies. American Family Physician 2003; 67(3): 511-516.
10. Hewlett ER, Mount GJ. Glass ionomers in contemporary restorative dentistry-A clinical update. Journal of the Californian Dental Association 2003; 31(6): 483-493.
11. Beaudreau R. Oral and dental emergencies. In: J Tintinalli, J Stapczynski, D Cline, O Ma, R Cydulka, G Meckler (Eds). Tintinalli's emergency medicine: a comprehensive study guide, 7th edn. New York: McGraw-Hill, 2011.
12. McIntosh MS, Konzelmann J, Smith J, Kalynych CJ, Wears RL, Schneider H et al. Stabilization and treatment of dental avulsions and fractures by emergency physicians using just-in-time training. Annals of Emergency Medicine 2009; 54(4): 585-592.


