Context
In India 60-70% of the population live in rural villages. The rural population suffers from a burden of disease and disorders due to the non-availability of appropriate healthcare personnel and facilities1,2.
In Indian rural areas, there is a preponderance of certain health problems, such as a high suicide rate, incidences of certain types of mental health problems and degrees of health problems associated with the physical nature of work in rural primary industries1,2. In addition, a range of social, economic, geographic, infrastructural and cultural factors affect the health of Indian rural individuals and the adequacy of rural health services3-5.
The Indian rural population has a higher proportion of elderly people compared with the national average1-3. Abuse of alcohol and the use of smokeless tobacco is a significant problem among rural youth. Rural hospitals are half as likely to provide emergency mental health care as are urban hospitals1-6. Rural residents have greater transportation difficulties for health care compared with urban residents and this is particularly so for vulnerable groups such as the elderly or disabled persons. Rural residents have difficulties accessing food retailers for fresh fruit and vegetables which has implications for diet-linked diseases6. Rural housing difficulties associated with the limited supply of low cost housing and the poorer quality of housing in rural areas (especially in relation to dampness) may be associated with homelessness, asthma and respiratory infection, and certain other infections such as tuberculosis6. Unemployment is higher in rural areas and linked with limited employment opportunities, seasonal and part-time work, low wages, decline in agricultural labour force, and work-related stress and risks1-6.
Some villages have a medical facility available but few doctors are willing to accept posts in these rural hospitals3,5,6. Doctors who do work with rural patients may be professionally isolated and lack the opportunity for continuing education.
Government policy response
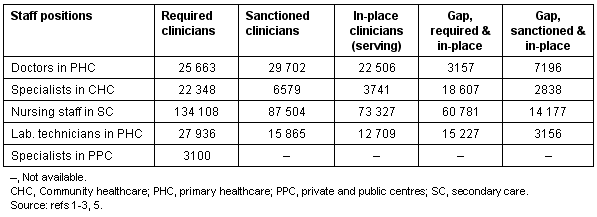
In the period 1951-2000, using a series of five-year plans to effect health sector reform, the Indian Government established a number of small hospitals and dispensaries in small rural villages (Table 1)1-3,5. However, the operation of these hospitals was compromised by the lack of medical staff1,2. By the Tenth Plan (1995-2000) manpower still fell short of what was sanctioned and required (Table 2)1-3.
Table 1: Progress in establishing healthcare centers in Indian rural areas (1951-2000)
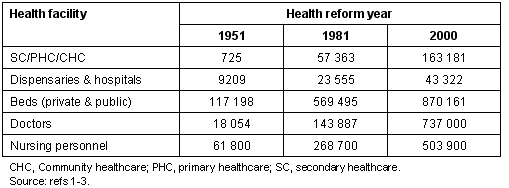
Table 2: Healthcare during the Tenth Plan (1995-2000): health manpower in primary healthcare centres
Policy shortfalls
In India, interaction among components of the healthcare system has been suboptimal. There are no well organized referral linkages between primary, secondary and tertiary care institutions2,5. Gaps persist in manpower and infrastructure function in the government sector, especially at the primary healthcare level in remote, rural mainly hilly areas where tribal people live in the forests, and in urban slum areas where healthcare needs are greatest1. The referral structure is poor, as is the coordination of government, voluntary and private sector services 2,3.
Among the plethora of hospitals there are massive inter-state, inter-district, urban-rural differences in appropriate management and distribution of manpower, diagnostic and therapeutic services, and pharmaceuticals1. The availability and utilisation of services are poorest in the most needy remote rural areas in districts or states2,5.
Issue
- Biotelemetry is the remote detection and measurement of a condition, activity, or function relating to a man or animal.
- Telehealth is the process of telemetering and controlling health related data.
- Telemedicine is the telepresence of medical experts with the ability to act and interact in an offsite environment by making use of virtual reality technology. Telemedicine reduces the cost of medical practice and brings expertise into remote areas7.
Advanced technologies have been developed to eliminate the barriers of distance and topography. Telehealth programs have been formulated in many countries1-20. In the USA, Europe, Australia, Canada and other countries, successful biotelemetry programs, or obtaining biological information at a distance, have been implemented5,6. Analytic surveys on telemedicine and doctor-patient communication, uses of telemetry in health care, clinical telemetry and patient monitoring, teleradiology, telesurgery, implant biotelemetry and telemetry of medical signals have been detailed by various researchers9-15. Such technological developments have assisted health care in rural India5,6.
Telehealth offers a solution to the problems of health care in rural and remote India where there are already many telehealth programs operating5,6,8. Existing telecommunication systems are being used to transmit clinical data from remote areas to major hospitals, and to transmit and receive specialist advice or consultation13,15. Radiotelemetry as well as the use of satellite and internet media are being used successfully in some areas1,2,16.
World Bank loans have been used in India to initiate projects to build up district hospitals. During the Tenth Plan it was resolved that optimal use would be made of facilities available in tertiary care institutions, and that the quality of services in and strength of linkages with secondary care institutions would be enhanced. Efforts are currently under way for the development of appropriate two-way referral system utilizing IT tools to improve communication, consultation and referral right from primary care to tertiary care levels.
Integration of all aspects of current healthcare programs requires a progressive convergence of funding, implementation and monitoring of all health and family welfare programs under a single field of administration beginning at and below district level. To this end, tele-linkages must still be built among villages, sub-centres, and primary healthcare centres. In addition, links from remote areas must be made with secondary healthcare centres, district and tertiary care centres, and major super-specialty institutions in other regions.
Advantages of rural telemedicine
The advantages of the use of telemedicine include improving care for rural patients and reducing professional isolation of healthcare professionals.
Providing healthcare services via biotelemetery makes specialty care more accessible. Video consultations from a rural clinic to a specialist can alleviate prohibitive travel and associated costs for patients. The existing problems of insufficient physicians will be eased by offering diagnostic consultations at a distance, and will facilitate access to distant colleagues. In this way, expert advice will be readily available to assist local health professionals. Rural telemedicine will also provide training opportunities for isolated or rural health practitioners. The building of a telecommunications infrastructure presents a vehicle for a disease surveillance and response at the district, state and national level.
Disadvantages of rural telemedicine
Among the disadvantages of telemedicine are increased expectations of health care, physician licensing issues, resistance to the technology, and the costs associated with installation.
Telemedicine widens the spectrum of possible interventions and increases service awareness and expectations of the population. However the escalating cost of health care is widening the gap between what is possible and what the individual or the country can afford11.
For an all-India telemedicine system to be successful, state licensing of physicians, with the impossibility of all specialists being registered in at least 20 states in order to treat patients India-wide, requires legislative reform by the Indian Government.
Until there is widespread acceptance of the technology, patient and physician resistance may be expressed in fear of malpractice suits due to lack of 'hands-on' interaction with patients.
Among barriers to the practice of telemedicine, the cost of installation, including hardware and infrastructure, is the greatest. To overcome this, installation should be staged. Once the system is installed, the cost of operation is low in terms of ongoing input, manpower and capital costs. Healthcare may be linked into already developed infrastructure. In terms of a reduction of morbidity and mortality of those living in rural India, the cost-saving would be high14.
Many potential telemedicine projects have been hampered by the lack of appropriate telecommunications technology. Regular telephone lines do not supply adequate bandwidth for most telemedical applications, and few rural areas have the cable wiring required for telemedicine. However, private corporations, telecommunications companies and technology manufacturers may produce the low-cost equipment and bandwidth for tele-internet usage under the auspices of corporate philanthropy. Once a telemedicine system is in place, a radical change is forecast and transition from the current grant- and self-funded projects, to a major self-sustaining industry within the healthcare field 8.
Lessons
An overview of health related problems in rural India has been given with the possible solution of biotelemetry. In line with the current international debate20 on the cost-analysis of such an approach, the initial costs for any biotelemetry program may be prohibitively high. However this must be set against the long-term advantages of improved health care in rural India.
However, research questions remain, among them:
- What is the cost of setting up a telemetry link between a single village and an urban hospital?
- Would better use of such funds be to increase the pay of rural health professionals, and so make a rural posting more attractive?
- How much will it cost to maintain the links?
- Are there technicians capable of maintaining the system?
- Which aspects of medical care will show a measurable improvement in healthcare status for the rural population?
- Will health indicators (access to clean water, access to better housing, dental care, suicide prevention, prevention of substance abuse, prevention of spousal abuse etc) be improved by telemedicine? Would it be better to provide training and employment for rural individuals already resident in the village who could apply their training for people they know well and whose language they understand?
References
1. Ghosh S. Information and communication technologies. Kurukshetra (India) 2001; Nov: 2-6.
2. Dhakha BL, Mann JS. Information technology: an engineering approach in transfer of technology. Kurukshetra (India) 2002; Dec: 18-23.
3. Sangole S. Primary health care in disadvantaged urban areas. Employment News (New Delhi), 2003; 28(1): 8-9.
4. Mishra SN, Pal C. Development of rural infrastructure with special reference to telecommunication. Kurukshetra 2002; May: 22-27.
5. Ramachandran P. Health care during the tenth plan. Employment News (New Delhi), 2003; 27(43): 6,7.
6. Chaudhary TH. Telecommunication-in the tenth plan. Economical Political Weekly, 2001; 36(34); 1-6.
7. Burrow M. A telemedicine tested for developing and evaluating telerobotic tools for rural health care. In: no Eds Medicine Meets Virtual Reality II: Interactive Technology and Healthcare, Visionary Applications for Simulation Visualization Robotics. San Diego: Aligned Management, 1994: 15-18.
8. Government of India, Department of Space. Indian Space Research Organisation Annual Report 2002-2003. (Online) 2003. Available: http://www.isro.org (Accessed 16 February 2004).
9. Singh VR. Biotelemetry of tympanograms and acoustic reflex patterns in human ear. Biotelemetry V 1980; 5: 331-335.
10. Miller EA. Telemedicine and doctor-patient communication: an analytical survey of the literature. Journal of Telemedicine and Telecare 2001; 7: 1-17.
11. Hanley J. Uses of telemetry in healthcare. Biotelemetry 1990; 15: 196-198.
12. Bracale M, Scarpetta G. Telecommunications in healthcare systems. Biotelemetry, 2000; 25: 199-202.
13. Jeutteur DC, Telemetry of biomedical signals. Medical & Life Sciences Engineering 1994; 13: 131-145.
14. Singh VR, Parshad R. Transducers for biotelemetry. PA Neukomm (Ed.) Biotelemetry II. Basel: Karger, 1974; 28-29.
15. Jeutteur DC. Clinical uses of biotelemetry. IEEE-EMBS 1983; 2: 19.
16. Singh VR. A strain gauge jaw force transducer. In: TB Fryer, HA Miller and H Sandler. (Eds). Biotelemetry III. New York: Academic, 1976; 263-266.
17. Jennett P, Jennett PA, Scott RE et al. Policy implications associated with the socio-economic and health system impact of telehealth: A case study from Canada. Telemedicine Journal and e-Health, Special Canadian Issue 2004; 10: 77-83.
18. Jennett P, Hailey D, Ohinmaa A, Scott R, Thomas R, Anderson C. The socio-economic impact of telehealth: Evidence now for health care in the future. Final Report. Volume 1: State of the Science Report. University of Calgary. (Online) 2003a. Available: http://www.ahfmr.ab.ca/grants/docs/state_of_science_reviews/Jennett_ES.pdf (Accessed 25 June 2003).
19. Jennett P, Hailey D, Ohinmaa A, Scott R, Thomas R, Anderson C. The socio-economic impact of telehealth: Evidence now for health care in the future. Final report. Volume 2: Policy Report. University of Calgary. (Online) 2003b. Available: http://www.ahfmr.ab.ca/grants/docs/state_of_science_reviews/Jennett_Pres.pdf (Accessed 25 June 2003).
20. Singh VR. Current advances in telemedicine. Procedings, Conference on Telemedicine: A vision turned mission. March 19 2004, Delhi, India. 2004.
