Low birth weight (LBW) is a known risk factor for neonatal death1-7. However, well-organized programs for determining infant birth weight are often lacking in rural areas of low-income countries, where most infants are born at home. In such areas, the infant's relative size at birth, as assessed by the mother, is often the only available indicator of birth weight8. Thus, LBW and the conditions experienced by many LBW infants in these areas often go undetected8-10. The establishment of a system for identifying LBW infants in community settings is, therefore, needed.
One country in which such a system is needed is Nepal. According to the 2011 National Demographic and Health Survey (DHS), 64% of infants born in Nepal were not weighed at birth11. Among the infants weighed and whose weight could either be recalled by their mothers or had been recorded in writing, 12% were LBW infants. This appears to reflect improvement from the previous DHS in 2006, which found that 83% of infants were not weighed at birth and the prevalence of LBW infants was 17%12. However, previous studies have suggested that the prevalence of LBW infants, as determined from birth records, might not reflect the true prevalence of LBW in the population because most infants weighed are born to mothers with a higher socioeconomic status living in urban areas13,14. Indeed, the prevalence of LBW was reported to be 43% by one study conducted in Nepal from 1998 to 200115 and 25% and 28% by two studies conducted in 200416,17; these percentages are much higher than those reported by the DHS. Such observations suggest that a nationwide mechanism for accurately and reliably detecting and caring LBW infants is needed.
Spring scales have been shown to be effective in the identification of LBW infants in community settings17,18. During a trial of a community-based neonatal sepsis-management intervention program in Dhanusha district, Nepal19, female community health volunteers (FCHVs) were involved in weighing newborns at birth using spring scales to identify LBW infants and to assist their mothers in making follow-up visits and/or referring infants to health facilities if they showed any signs of distress. FCHVs are a cadre of approximately 50 000 local volunteers selected by a local mothers' group to address reproductive and child health issues under the auspices of Nepal's Ministry of Health. They have been operating since 198820.They attend two 9-day basic initial training sessions and a 5-day refresher training session every 5 years. As these volunteers are found in every geographical/administrative unit called Village Development Committees (VDCs) throughout Nepal and live within the community, they have good access to newborns.
The current study was designed to determine whether the use of FCHVs to detect LBW infants and initiate prompt, appropriate action for those infants' care is feasible, with the understanding that FCHVs already engage in numerous child healthcare activities throughout the nation. This study specifically examined (1) the sensitivity and specificity of the measurements obtained by FCHVs using spring scales and compared them with the sensitivity and specificity of the maternal assessments of infant size; (2) their knowledge of appropriate management of LBW and very low birth weight (VLBW) infants and the skill of FCHVs in zeroing spring scales; and (3) FCHV performance and coverage of FCHV visits and weight measurement. The overall goal of this study was to provide evidence of the feasibility of interventions that may lead to a decrease in neonatal mortality in resource-limited settings.
Study setting
This cross-sectional study was conducted in the Dhanusha district of Nepal between February and May 2011 as part of a cluster randomized controlled trial. The larger study was entitled 'A cluster-randomized controlled trial to test the effectiveness of women's groups for neonatal survival and improved maternal and infant nutrition and of community-based neonatal sepsis management for neonatal survival'. The overall aim was to assess the impact of community-based activities implemented by FCHVs on neonatal mortality in Dhanusha district from April 2008 to April 201119. Dhanusha is a Terai (plains) district in the central region of Nepal, has a population of approximately 777 000, 89% of which live in rural areas21,22. In the central Terai region, approximately 67% of women are reported to deliver their babies at home11. Dhanusha district comprises one municipality and 101 VDCs. Each VDC has a population of 4000 to 17 000, operates one health facility staffed by government-employed community health workers, including auxiliary health workers, auxiliary nurse midwives, and village health workers; and is divided into nine wards served by one FCHV.
FCHV activities
After being informed of a birth at home, FCHVs visited and weighed infant(s) using a spring scale (Super Samson Spring Balance; Salter Brecknell, India). This scale, a 28 cm, 120 g device, indicates the weight of an infant using a color-coded system by which red indicates that an infant weighs 0 to 1999 g; yellow, 2000-2499 g; and green, ≥2500 g. Using recording forms containing three pictures of spring scales with their indicators colored green, yellow, or red, the FCHVs selected the picture of the spring scale that corresponded with the color of the indicator that they observed upon weighing each infant. Thus, even FCHVs unable to read were able to classify the neonates into the three categories, namely, normal birth weight (NBW, ≥2500 g), LBW (2000-2499 g), or VLBW (<2000 g) infants. VLBW infants were defined as infants weighing below 2000 g in this study. This weight range was based on the results of Yasmin et al. who indicated that the mortality rate of infants weighing below 2000 g is higher than those weighing 2000-2499 g in South Asia23. In addition, Darmstadt et al. defined infants with weights below 2000 g as VLBW in an Indian study of weight measurement using spring scales18.
The FCHVs had received training on using the spring scales during a 5-day training program on neonatal sepsis management provided by local health workers in 2007, with refresher training in 2008. From their training, they were aware that the weight displayed on the scale before zeroing was 100 g, requiring them to zero the scale prior to weighing the infant and after attaching the weighing sling and cloth; otherwise, the total weight of an infant could be overestimated, risking misidentification of a LBW infant as a NBW infant.
The FCHVs were tasked with identifying every birth in their working area, obtaining a birth weight within 24 hours where possible, and visiting each baby three or four times to check for danger signs of sepsis19. For the purposes of this study, after an FCHV had weighed an infant, she immediately reported the result to a supervisor by telephone. Then a supervisor re-weighed the infant as soon as possible using a calibrated digital scale with 10 g gradations (SECA 834®; SECA, Hamburg, Germany) to assess whether the FCHV had correctly categorized the infant. Each study supervisor had more than 4 years of experience as a healthcare worker in community health services.
As part of their 5-day training session, the FCHVs had also learned the protocol for management of LBW and VLBW infants. For each LBW infant, they had been instructed to inform the mother that her infant was smaller than normal and show her how to identify any signs of illness or weakness. In addition to the normal follow-up visits 3, 14, and 28 days after birth for NBW infants, they conducted a follow-up visit 7 days after birth to determine if the infant showed any signs of infection. If a LBW infant showed any of 10 danger signs suggesting neonatal sepsis during any of the visits or had been categorized as VLBW, the FCHV was to immediately refer the mother to a health facility.
Data collection
FCHV determination of weight using a spring scale: After an FCHV had weighed an infant using a spring scale, the infant was re-weighed by a supervisor using a calibrated digital scale to determine the accuracy of the FCHV's measurement. The measurement provided by the digital scale was considered the gold standard with which the accuracy of the FCHV's measurement and the maternal assessment of relative size at birth was assessed.
Maternal assessment of relative birth size: When visiting mothers to weigh their neonates using an electronic scale, supervisors asked them to describe their initial perception of their infants' relative birth size as very small, smaller than normal, normal, or larger than normal. By this means, supervisors could ascertain whether mothers could correctly identify LBW infants.
Assessment of FCHV skill, protocol knowledge, and FCHV characteristics: To assess the level of FCHV knowledge regarding management of LBW and VLBW infants and spring-scale usage, supervisors conducted interviews with all the FCHVs. They asked FCHVs to describe the protocol for weighing infants, to demonstrate their knowledge of zeroing a spring scale; and to provide data regarding their age, literacy level, work experience, and training history.
FCHV performance: To assess FCHV performance, 10 new mothers within each VDC per month were questioned regarding antenatal, delivery, and postnatal practices throughout the study period. This dataset was created as part of the broader study, as described previously19. Data regarding maternal recall of whether an FCHV had visited and weighed each neonate were extracted from this larger dataset.
Statistical analyses
The sensitivity and specificity of the spring-scale measurements, as well as maternal perceptions of relative birth size, were calculated by comparing them to the respective electronic-scale measurements. FCHV performance in terms of correct- and miscategorization of birth weight category was analyzed using logistic regression. First, univariate logistic regressions were conducted with correct categorization as the dependent variable, and age, literacy, work experience, training received and number of infants weighed as explanatory variables. Then the effect of each of the explanatory variables in turn was adjusted for all the others together as potential confounders in a multiple logistic regression model. All data were analyzed using Stata 11 software (StataCorp LP; http://www.stata.com).
Ethics approval
This study was approved by the Nepal Health Research Council (approval no. 269) and the ethics committee of the Institute of Child Health and Great Ormond Street Hospital for Children, UK (approval no. 04PC01). As preliminary research had revealed that most women in the study areas are illiterate and that requesting a signature or thumbprint for written consent is not culturally acceptable, study information was provided orally, and consent for participation was obtained orally at the time of data collection.
FCHV characteristics
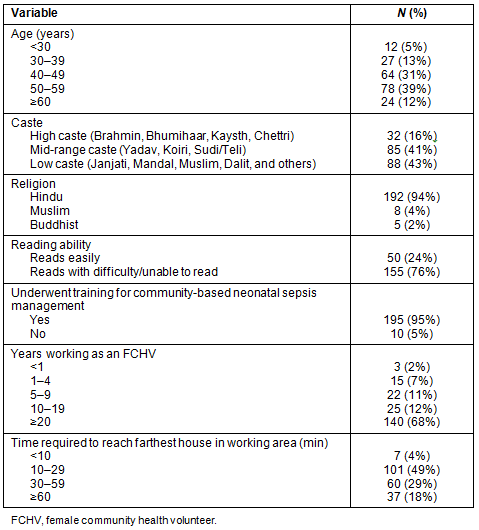
Table 1 shows the demographics and work experience of the 205 FCHVs examined in the study. Demographically, the FCHVs were of a mean age of 47 years and represented a range of predominantly plains ethnicities, primarily Hindu, Maithili-speaking. In terms of education, skills, and employment, nearly 75% were illiterate or barely literate, more than 90% had worked as FCHVs for more than 5 years, almost 70% had 20 years of work experience as FCHVs, and 53% could reach the farthest point in their assigned areas within 30 minutes by foot.
Table 1: Demographics of female community health volunteers (N=205)
Sensitivity and specificity of birth-weight screening by FCHVs
A total of 462 infants were weighed using both spring and electronic scales within 72 hours of birth. On average, each FCHV weighed three infants (range, 1-11 infants) over the sampling period. The mean time from birth to weight measurement was 12 hours for the FCHVs and 22 hours for the supervisors, yielding a mean time difference in FCHV and supervisor measurement of 10 hours (range, 0-54 hours).
The prevalence of LBW was 28%, based on the electronic scale weights. On the other hand, the prevalence of LBW, based on spring scale weights, was 25%, including false positives (Table 2). The sensitivity of the spring scales for detecting LBW was 89%, with a specificity of 99%. Similarly, the sensitivity and the specificity of identifying VLBW by a spring scale were 86% and 100%, respectively (Table 2). The lag time between spring- and electronic-scale measurement of miscategorized infants ranged from 0 to 29 hours, with 17 of the 20 miscategorized infants being weighed within 10 hours.
Sensitivity and specificity of maternal perception of infant size
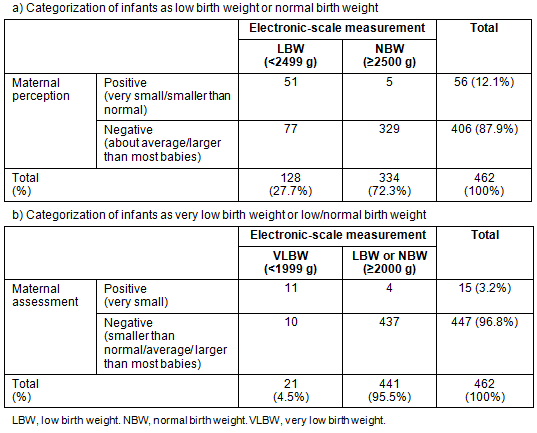
The prevalence of LBW according to maternal perception of infant size as small was 12%, with a sensitivity of 40% and a specificity of 99% (Table 3). The sensitivity and specificity of maternal detection of VLBW were 52% and 99%, respectively.
Table 2: Identification of low birth weight and very-low-birth-weight infants by electronic- and spring-scale measurement
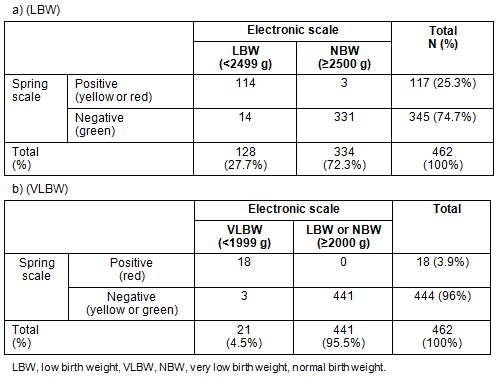
Table 3: Comparison of use of maternal assessment and electronic-scale measurement in infant weight categorization
FCHV knowledge and skills
All FCHVs were able to specify which spring-scale colors indicated NBW, LBW, and VLBW infants. Seventy per cent of FCHVs could describe the protocol for managing both LBW and VLBW infants, 15% could describe the management of either LBW or VLBW infants and 15% could not describe either protocol. Among FCHVs with reading ability, 80% could describe the correct action to take upon identification of high-risk infants, while 66% of those with no or poor reading skills could answer correctly.
Ninety-six per cent of the FCHVs were able to zero the scales when asked to demonstrate weighing an infant to their supervisor. Among those who were able to zero scales, 46% zeroed the spring scales using a wrapping cloth and sling, as they had been taught during their training; 22% used only a sling; and 28% used neither a sling nor wrapping cloth.
FCHV performance
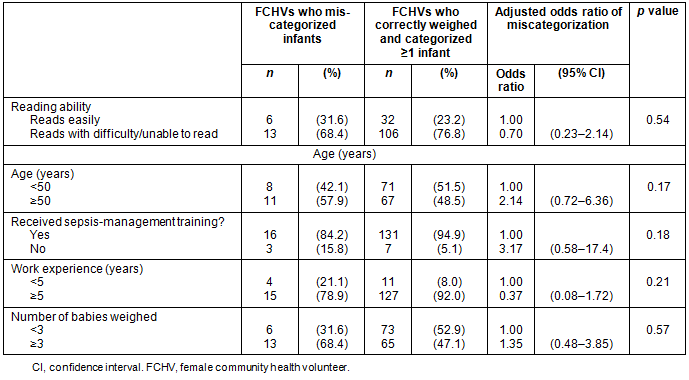
Using a subset of the surveillance dataset of the cluster randomized controlled trial, which covered the period between April 2008 and April 201119, FCHVs visited 44% of the infants born in their assigned areas and weighed 67% of the infants whom they had visited. Review of the dataset for the present study reveals that 157 of the 205 (77%) FCHVs weighed at least one infant using a spring scale and then contacted their supervisor to reweigh the infant using an electronic scale during the study period of February to May 2011. The remaining 48 (23%) FCHVs either did not contact their supervisor after conducting a spring-scale measurement or did not weigh any infants during the data-collection period. Among the 157 FCHVs who performed at least one spring-scale measurement, 19 categorized the observed weights incorrectly, but only one did so twice during the study period. No differences in odds of weight miscategorization were found in relation to FCHV background characteristics or the number of infants weighed (Table 4).
Table 4: Demographics of female community health volunteers who miscategorized
birth weights and those who correctly weighed and categorized at least one infant
Discussion
Analysis of the study data revealed the prevalence of LBW was 25% when determined by spring-scale measurement, 28% by electronic-scale measurement, and 12% by maternal perception of infant size. Considering electronic-scale measurement as the gold standard, the sensitivity of LBW detection by the FCHVs using spring-scale measurement was 89%, while that using maternal perception was only 40%. Although maternal perception of relative birth size has been widely used to estimate birth weight, analysis of its reliability has yielded mixed results8,11,13,14,24,25. The results of this study indicate that use of maternal perception may lead to underestimation of the true prevalence of LBW and VLBW, and weight determination by FCHVs using spring scales is a much more accurate means of measurement that provides a more realistic indication of the prevalence of LBW and VLBW infants.
Identifying LBW and VLBW infants is necessary but not sufficient to care for these infants; such identification must be followed by provision of prompt, appropriate care for vulnerable LBW and VLBW infants. Most FCHVs demonstrated that they knew the correct actions to take after identifying LBW or VLBW infants, including providing appropriate information to the mothers and working as mediators between the mothers of at-risk infants and their local healthcare facilities. Data on whether the FCHVs had actually referred LBW and VLBW infants to healthcare facilities and whether the mothers visited these facilities with their at-risk infants were not available at the time of this study and will be reported in the trial paper.
Besides improving the accuracy of birth-weight measurement and prompting the use of appropriate care measures, use of FCHV weighing of infants at birth has several advantages. First, as FCHVs are already engaged in many reproductive and child health interventions in each VDC in Nepal, recruiting new people and establishing a new system to conduct birth-weight measurement would be unnecessary in any new childcare program. In previous studies of the weighing of infants using spring scales, the workers examined were newly hired and intensively managed throughout the course of the programs17,18; these tasks require provision of additional resources in terms of time and funding, which is often not feasible or sustainable in resource-limited settings. Current strategies for strengthening healthcare systems emphasize the integration of new programs into an existing system in order to utilize available resources, rather than adding completely new programs or investing in new resources26,27. Thus, utilizing FCHVs, an existing resource, to fulfill a new responsibility in the community, accords with this concept.
Second, FCHVs can overcome multiple barriers that may negatively affect weighing of newborn infants in remote, rural communities. Two such barriers are Nepal's mountainous terrain and the poor transportation system, which makes timely visits to the homes of neonates difficult for government health workers, who are thus not usually tasked with this responsibility. Unlike professional healthcare workers, who typically do not live in the communities that they serve in and are often not prepared or able to make home visits, the FCHVs examined lived in or near the communities and could make home visits relatively easily. Specifically, the present study showed that 53% of the FCHVs were able to arrive at the homes of clients within 30 minutes, and 75% were able to do so within 60 minutes. They were thus able to determine a neonate's weight within the first half-day of life, a critical period for survival of underweight neonates, as death typically occurs during the first few postnatal days28. Such promptness is also important for correctly categorizing infant weight, as breastfed neonates typically lose 3-7% of their birth weight within the first week of life29,30. Additionally, as cultural limitations would make it difficult or impossible for male healthcare workers to visit the maternal home within many rural areas of Nepal, employing a group of women who are well known within the community for this purpose increases the likelihood of obtaining infant weight data in these areas.
No statistically significant differences were found between the background characteristics of the FCHVs who had miscategorized infants and those who had not. Although the sample size was small, the results indicate that FCHV background variables, including age, literacy, training, and work experience, may not be very influential in determining how well FCHVs are able to conduct their tasks. However, when asked to describe the protocol, a greater percentage of the literate FCHVs correctly described the actions that they should take when they encountered with a high-risk infant. Thus, literacy may be important for program effectiveness and sustainability, and the FCHV system may benefit if a greater number of literate women are recruited.
Some FCHVs in the present study did not have the required level of knowledge and skills for the correct use of spring scales, leading some to zero the scale improperly, which may have led to overestimation of infant weight. Among the miscategorized cases, 85% (17 of 20) were overestimation of weight. One possible reason for such lack of accuracy may have been the lag of 3 to 4 years between the FCHVs' training and their application of their training to conduct weight measurement. Another reason may have been the provision of only minimal ongoing supervision of birth-weight measurement to ensure that it was being properly conducted. As supervision has been reported to improve the performance of healthcare workers31, allocation of more resources for more intensive supervision could improve FCHV performance, as has been shown in other studies involving the use of spring scales17,18. Although frequent on-site supervision is extremely difficult due to the geography of the study area, the integration of field level training and demonstration into the existing FCHV scheme, where possible, is likely to be beneficial.
Regarding the detection of VLBW neonates, the sensitivity and specificity using spring scales were 86% and 100%, respectively. Although conclusions are impossible to make due to the small sample size, results indicate that spring-scale measurement may be an effective means of identifying a group of infants at an even higher risk of death than LBW infants. Further studies should focus on analysis of the sensitivity of the detection of VLBW infants using spring scales and the effectiveness of possible interventions that may be taken-up by FCHVs for such infants.
The results of this study suggest that FCHVs can accurately identify LBW and VLBW infants using spring scales and that most have the knowledge necessary to take prompt action for the appropriate care of these infants. As use of FCHVs as newborn care providers allows for utilization of their logistical, geographical and cultural advantages, including a high level of access to infants, it has great potential to complement the Nepalese healthcare system. The establishment of a regular system of training and supervision involving more outreach of government health workers in the community is likely to further improve the performance of FCHVs and increase the effectiveness of this means of caring for high-risk infants in resource-limited settings.
Acknowledgements
This study was conducted in collaboration with Mother and Infant Research Activities (MIRA) within a project entitled, 'Community-based interventions for infant health in Nepal' funded by UBS Optimus Foundation, UK Department for International Development Towards 4&5 Consortium; USAID; a Wellcome Trust Strategic Award for the Population Science of Maternal and Child Survival (reference number 085417/Z/08/Z); and the Marion Esling Holy Trinity Legacy Fund. The authors are grateful to the health supervisors Durna Thapa, Chandramaya Thapa, Gagan Chaube, and Rupesh Yadav for their contributions to the sepsis-management program and data collection. The authors also thank all the FCHVs involved in the intervention, the Dhanusha District Public Health Office, and parents who allowed their babies to be weighed. Special thanks to Anni Pulkki-Brännström for statistical advice, the other members of MIRA Dhanusha for logistical support, and Leo Kawaguchi and Atusko Aoyama and other members of the Department of Public Health and Health Systems at Nagoya University for their helpful comments on the manuscript drafts.
References
1. Bhutta ZA, Darmstadt GL, Hasan BS, Haws RA. Community-based interventions for improving perinatal and neonatal health outcomes in developing countries: a review of the evidence. Pediatrics 2005; 115(Suppl 2): 519-617.
2. Darmstadt GL, Bhutta ZA, Cousens S, Adam T, Walker N, de Bernis L. Evidence-based, cost-effective interventions: how many newborn babies can we save? Lancet 2005; 365(9463): 977-988.
3. McCormick MC. The contribution of low birth weight to infant mortality and childhood morbidity. New England Journal of Medicine 1985; 312(2): 82-90.
4. McIntire DD, Bloom SL, Casey BM, Leveno KJ. Birth weight in relation to morbidity and mortality among newborn infants. New England Journal of Medicine 1999; 340(16): 1234-1238.
5. Barros FC, Victoria CG, Vaughan JP, Estanislau HJ. Perinatal mortality in southern Brazil: a population-based study of 7392 births. Bulletin of the World Health Organization 1987; 65(1): 95-104.
6. WHO/UNICEF. Home visits for the newborn child: a strategy to improve survival. Geneva: WHO/UNICEF, 2009.
7. Kutty VR, Shah P, Modi D, Shah S, Ramanathan M, Archana AR. Reducing neonatal mortality in Jhagadia Block, Gujarat: we need to go beyond promoting hospital deliveries. Journal of Tropical Pediatrics 2013; 59(1): 49-53.
8. Boerma JT, Weinstein K I, Rutstein SO, Sommerfelt AE. Data on birth weight in developing countries: can surveys help? Bulletin of the World Health Organization 1996; 74(2): 209-216.
9. Montagu D, Yamey G, Visconti A, Harding A, Yoong J. Where do poor women in developing countries give birth? A multi-country analysis of demographic and health survey data. PLoS One 2011; 6(2): e17155.
10. Kerber KJ, de Graft-Johnson JE, Bhutta ZA, Okong P, Starrs A, Lawn JE. Continuum of care for maternal, newborn, and child health: from slogan to service delivery. Lancet 2007; 370(9595): 1358-1369.
11. Ministry of Health and Population, New ERA, ICF International. Nepal Demographic and Health Survey 2011. Kathmandu: Ministry of Health and Population, New ERA, ICF International, 2012.
12. Ministry of Health and Population, New ERA, ICF International, Nepal Demographic and Health Survey 2006. Kathmandu: Ministry of Health and Population, New ERA, ICF International, 2007.
13. Moreno L, Goldman N. An assessment of survey data on birthweight. Socal Science & Medicine 1990; 31(4): 491-500.
14. Blanc AK, Wardlaw T. Monitoring low birth weight: an evaluation of international estimates and an updated estimation procedure. Bulletin of the World Health Organization 2005; 83(3): 178-185.
15. Christian P, Khatry SK, Katz J, Pradhan EK, LeClerq SC, Shrestha SR. Effects of alternative maternal micronutrient supplements on low birth weight in rural Nepal: double blind randomised community trial. British Medical Journal 2003; 326(7389): 571.
16. Osrin D, Vaidya A, Shrestha Y, Baniya RB, Manandhar DS, Adhikari RK. Effects of antenatal multiple micronutrient supplementation on birthweight and gestational duration in Nepal: double-blind, randomised controlled trial. Lancet 2005; 365(9463): 955-962.
17. Mullany LC, Darmstadt GL, Coffey P, Khatry SK, LeClerq SC, Tielsch JM. A low cost, colour coded, hand held spring scale accurately categorises birth weight in low resource settings. Archives of Disease in Childhood 2006; 91(5): 410-413.
18. Darmstadt GL, Kumar V, Shearer JC, Misra R, Mohanty S, Baqui AH. Validation of accuracy and community acceptance of the BIRTHweigh III scale for categorizing newborn weight in rural India. Journal of Perinatology 2007; 27(10): 602-608.
19. Shrestha BP, Bhandari B, Manandhar DS, Osrin D, Costello A, Saville N. Community interventions to reduce child mortality in Dhanusha, Nepal: study protocol for a cluster randomized controlled trial. Trials 2011; 12: 136.
20. Government of Nepal and USAID. An analytical report on national survey of female community health volunteers of Nepal. Kathmandu: Government of Nepal and USAID, 2007.
21. Sharma H, Goutam R, Vaidya S. District demographic profile of Nepal 2002. Kathmandu: Informal Sector Research and Study Centre, 2002.
22. Sharma N, Joshi S, Bhandari H, Bhusal M, Pandey H. District and VDC profile of Nepal 2010. Kathmandu: Intensive Study and Research Centre, 2010.
23. Yasmin S, Osrin D, Paul E, Costello A. Neonatal mortality of low-birth-weight infants in Bangladesh. Bulletin of the World Health Organization 2001; 79(7): 608-614.
24. Channon AA, Padmadas SS, McDonald JW. Measuring birth weight in developing countries: does the method of reporting in retrospective surveys matter? Maternal and Child Health Journal 2011; 15(1): 12-18.
25. Channon AA, Can mothers judge the size of their newborn? Assessing the determinants of a mother's perception of a baby's size at birth. Journal of Biosocial Science 2011; 43(5): 555-573.
26. Frenk J. Reinventing primary health care: the need for systems integration. Lancet 2009; 374(9684): 170-173.
27. World Health Organization. Report of the Alma Ata international conference on primary health care. Geneva: World Health Organization, 1978.
28. Lawn JE, Cousens S, Zupan J. 4 million neonatal deaths: when? where? why? Lancet 2005; 365(9462): 891-900.
29. Maisels MJ, Newman TB. Jaundice in full-term and near-term babies who leave the hospital within 36 hours. The pediatrician's nemesis. Clinics in Perinatology 1998; 25(2): 295-302.
30. Marchini G, Fried G, Ostlund E, Hagenas L. Plasma leptin in infants: relations to birth weight and weight loss. Pediatrics 1998; 101(3 Pt 1): 429-432.
31. Rowe AK, de Savigny D, Lanata CF, Victoria CG. How can we achieve and maintain high-quality performance of health workers in low-resource settings? Lancet 2005; 366(9490): 1026-1035.
