The 'Health-Promoting School' (HPS) concept (introduced by WHO in 19981) and the 'Focusing Resources on Effective School Health' (FRESH) framework (introduced by UNESCO, UNICEF, WHO and the World Bank in 20002) is a well-known approach for promoting health to pupils, teachers, families, and entire communities through schools. Its core components are 'school health policy', 'skills-based health education', 'health services' and 'healthy psychosocial and physical environment'. Another important implementation strategy for HPS is the collaboration between the health and educational sectors at three different levels: international, national and local (provincial, district, and schools)3. This approach has been adopted and implemented in many countries for more than a decade.
An award scheme for healthy schools as a means of implementing the HPS concept has been popular in European countries4,5. It provides a structured framework, health-related targets and external support to help schools become HPS. Under such schemes, indicators that must be achieved usually need to be shown and the schools' levels of achievement are assessed through observation, interview, questionnaire, and/or the checking of documents. It requires audit teams to judge the achievement of schools. In Asia, award schemes have been adopted in several areas including Thailand and Hong Kong6-8. In Thailand, the award scheme is implemented with a self-evaluation system that aims to raise awareness and to solve health-related problems through school-related personnel (teachers, pupils, parents and community) using a comprehensive school health check list that lists the goals that must be achieved in order to become an HPS6,7. Some other Asian countries such as Lao PDR and Cambodia, use school health self-evaluation systems which were created by a simplification of the award scheme9,10.
Niger is a Sub-Saharan country with a Human Development Index value of 0.261, which ranks 167th among 169 countries measured11. The general education system in Niger consists of primary (6 years), junior secondary (4 years), senior secondary (3 years), and tertiary education (2-4 years). Primary education usually begins at the age of seven, but sometimes begins later in rural areas. The primary school enrolment rate in 2008 was 68%, with an achievement rate of 48% among the enrolled pupils12. At the time of writing, 48% of the primary schools in Niger were built of permanent material such as concrete, 15% had latrines, and 16% had a water point.
In Niger, the Bureau Santé Scolaire (School Health Office: BSS, Appendix I, II) was constituted in 2003 and established in 2005 with the aim of strengthening HPS as a national program13,14. This bureau is administered by the Ministry of National Education; however, personnel from the Ministry of Public Health are attached to the BSS to encourage coordination with each sector.
To introduce the HPS concept in Niger, a low-cost method was required that was in line with the budgetary constraints of developing countries. Several conditions were used to achieve this. First, of all of the typical HPS components it was decided to concentrate on promoting a healthy environment. Second, since the varied training required for the implementation of HPS usually involves a high level of expenditure, a method that did not require government officers and teachers to be trained was conceived, in which a simple document which described some sample activities for improving hygiene status in primary schools was developed and distributed. It was designed to be easily read and understood and for the activities to be readily performed. A pilot test was conducted with the cooperation of the West African Centre for International Parasite Control (WACIPAC), the Japan International Cooperation Agency (JICA) and other partners in the Tahoua region in 2008.
This article aims to evaluate the efficacy and sustainability of the self-assessed Healthy Activity Guide. The effect of this pilot project on health/hygiene issues in primary schools in Niger was examined.
Study region
The Niger Tahoua region is located approximately 400 km east of Niamey (Fig1). In 2008, there were 1999 primary schools, including public, private and community schools, under 16 Inspections du Enseignement de Base (Inspectorate for Basic Education [IEB], Appendix I)12.
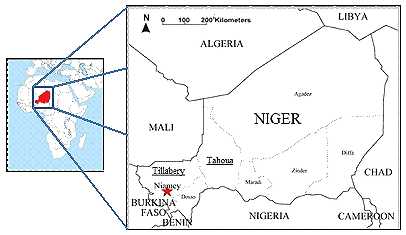
Figure 1: Map of Niger showing the study area.
Development of tools and implementation
A self-evaluation check list was developed, that focused only on healthy environment and hygiene. At the same time, to reduce costly training a healthy activity guide was developed which demonstrated some sample activities that could be undertaken to achieve a healthy environment and good hygiene. It described practical ideas regarding what should be done, how it should be implemented and why the activities were necessary. Both documents were distributed to 220 primary schools in the Tillabéry region, which surrounds Niamey, the capital city of Niger (Fig1).
Thirty selected primary schools were observed twice (before and after observation) and principals and teachers were interviewed. The results of these observations were that 87% (26/30) of schools showed some improvement in hygiene status. From the interviews, several points of improvement emerged, such as 'the contents of the check list and the activity guide do not correspond well' and 'the school activities were decided by Comité de Gestion des Etablissement Scolaire (COGES, Appendix II) at the beginning of the academic year, so it was difficult to perform the activity due to the pre-allocated budget'. To solve these problems and to simplify the program as much as possible, the self-evaluated check list was integrated with the Healthy Activity Guide. The document was modified to a 'question and answer' form that listed '10 key questions (10QC) to help your school obtain a better sanitary environment' (10 questions clés pour arriver à un meilleur environnement sanitaire de votre école). Along with the 10 questions, the list contained explanations of the usefulness and solutions of each of the points addressed by the 10QC (Appendix III).
The 10QC were distributed to all primary schools in Tahoua at principal meetings (Cellule d'Animation Pédagogique [CAPED], Appendix II) in each Secteur Pédagogique ([SP], Appendix I,II) held in August 2008, before the start of the 2008 academic year. Instructions on the use of the 10QC were explained at the meeting by education and health sector personnel.
Data collection and data analysis
Quantitative analysis: To explore the change of attitudes to health/hygiene issues, the budget and number of planned activities related to health and hygiene for the years 2007-2009 were collected from their respective COGES Action Plans and compared. Implementation status was examined using data from the COGES Activity Reports of the same years. Three-year Action Plans and Activity Reports for the year 2009 were collected from primary schools in Tahoua through BSS. The CODES Activity Report data for the years 2007 and 2008 were collected from 'Schools for All', another JICA project (unpubl. data, 2010). The budget, number of activities, implementation status and other parameters were compared by χ2 test, Fisher's exact test, Kruskal-Wallis rank test or Mann-Whitney U-test, depending on data type. Analyses were performed using the Stata v11.0 statistical software (StataCorp, USA).
Focus group discussions and telephone interviews: Sixteen Conseillers Pédagogiques ([CP], Appendix II), 15 principals and 15 COGES members from 15 primary school communities were invited to participate in the focus group discussions (FGDs). A total of eight FDGs, with two groups of CPs, three groups of principals, and three groups of COGES members, were conducted in Niamey in November, 2010. The grouping criteria were as follows:
- Group CP1: CPs from SPs that submitted their Action Plans for 2007 and 2008 to BSS (10 CPs)
- Group CP2: CPs from the SPs that did not submit their Action Plans for 2007 and 2008 to BSS (6 CPs)
- Group Principal1: Principals from schools where the number of health-related activities increased in 2008 after distribution of the 10QC (5 principals).
- Group Principal2: Principals from schools where the number of health-related activities did not change in 2008 after distribution of the 10QC (5 principals).
- Group Principal3: Principals from schools where the number of health-related activities decreased in 2008 after distribution of the 10QC (5 principals).
- Group COGES1: COGES members from schools where the number of health-related activities increased in 2008 after distribution of the 10QC (5 COGES members).
- Group COGES2: COGES members from schools where the number of health-related activities did not change in 2008 after distribution of the 10QC (5 COGES members).
- Group COGES3: COGES members from schools where the number of health-related activities decreased in 2008 after distribution of the 10QC (5 COGES members).
- Principals and COGES members came from the same schools.
A trained moderator facilitated all FGDs and in-depth interviews were performed with a trained facilitator and a note-taker. The FGD guides were developed in French, the official language in Niger. Most of the FGDs and all of the interviews were conducted in French. However, three FGDs for COGES community members were conducted in Hausa, one of the local languages, for the better understanding of the participants. The FGD guide for these FGDs was translated by the moderator. All FGD notes and interviews were recorded in French. All opinions were categorized by each FGD.
Focus group discussion topics The topics explored were: (i) use of the 10QC; (ii) ways in which the 10QC was used; (iii) current use of and reasons for use of the 10QC; (iv) impression of the 10QC; and (v) difficulties in using the 10QC and the support that was required. These topics were subject to minor changes to suit each group.
Ethics approval
This study was permitted (verbally) by Bureau Santé Scolaire, Ministry of National Education, Niger.
Quantitative analysis
The proportion of schools that planned health-related activities increased after distribution of the 10QC and was stable 1 year after distribution (2007 vs 2008, p <0.001; 2008 vs 2009, p=0.981). The percentages were 47%, 79% and 80% in the years 2007, 2008 and 2009, respectively (Table 1). In terms of implementation, 44%, 48% and 65% of schools implemented at least one health-related activity in the years 2007, 2008 and 2009, respectively. The proportion in 2009 was higher than in the other 2 years (p <0.001).
The median budget for health-related activities in each year also increased (p = 0.0001). The budgets for health-related activities in the 2 years after distribution of the 10QC were higher than in the year before distribution (2007 vs 2008, p <0.0001; 2008 vs 2009, p=0.8414; Table 2). The budgets for other activities did not show any statistically significant changes (p=0.7378). Expenditure for health/hygiene activities increased one year after distribution (p=0.0001), as did expenditure for other activities (p=0.0267).
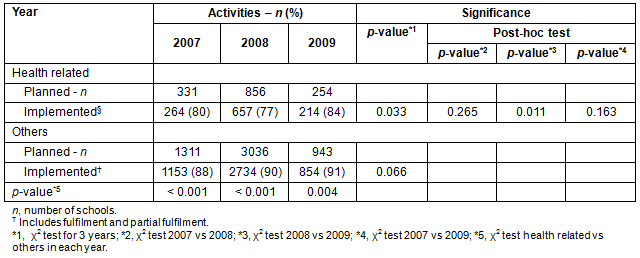
Fulfilment or partial fulfilment rates for health-related activities in the years 2007, 2008 and 2009 were 80%, 77% and 84%, respectively. For other activities, the rates for the same years were 88%, 90% and 91%, respectively (Table 3). The rate of health-related activities in 2009 was slightly higher than in 2008 (p=0.011), but not different from 2007 (p=0.163). Fulfilment/partial fulfilment rates of health-related activities were lower than those of other activities in all three fiscal years (2007, p <0.001; 2008, p <0.001; 2009, p=0.004).
Table 1: Number of schools that planned/implemented at least one health-related activity in Tahoua, Niger
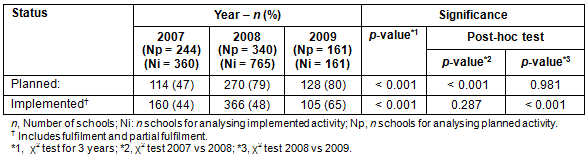
Table 2: Budget/expenditure planned/implemented by Comité de Gestion des Etablissement Scolaire per school (currency unit: Franc cfa)
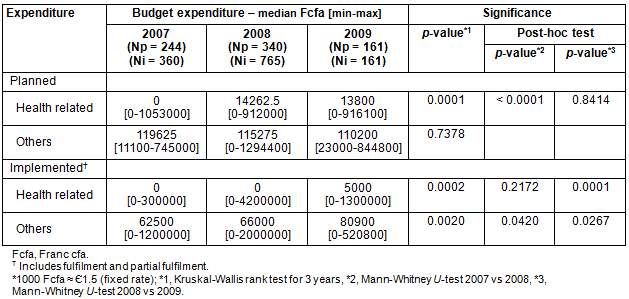
Table 3: Number of activities planned/implemented by Comité de Gestion des Etablissement Scolaire
Details of implemented health-related activities are shown (Fig2). The proportion of respondents that indicated 'purchase of cleaning materials' among health-related activities were 2%, 6% and 11% in the years 2007, 2008 and 2009, respectively, and tended to increase after distribution of the 10QC (p <0.001, post-hoc test; 2007 vs 2008, p=0.014; 2008 vs 2009, p=0.011). 'Cleaning activity' also increased after distribution of the 10QC and the proportion remained the same at one year after distribution. The proportions for the years 2007, 2008 and 2009 were 12%, 20% and 24%, respectively (p=0.003, post-hoc test; 2007 vs 2008, p=0.005; 2008 vs 2009, p=0.230). 'Purchase of hand-washing materials' did not show any change in the first year after distribution. However, at one year after distribution, the proportion increased significantly, with proportions for the 3 years of 2%, 1% and 7%, respectively (p<0.001; post-hoc test; 2007 vs 2008, p=0.311 and 2008 vs 2009, p <0.001). 'Fence construction/maintenance', on the other hand, tended to decrease after distribution with proportions for the three years of 19%, 14% and 10%, respectively (p=0.032, post-hoc test; 2007 vs 2008, p=0.079, 2008 vs 2009, p=0.157, and 2007 vs 2009, p=0.011). 'Purchase medicine' also decreased one year after distribution, with proportions for the 3 years of 6%, 7% and 2%, respectively (p=0.048, post-hoc test; 2007 vs 2008, p=0.669 and 2008 vs 2009, p=0.013). 'Latrine construction/maintenance' did not change significantly with proportions for the 3 years of 12%, 15% and 15%, respectively (p=0.485). The median expenditure for the activities that increased ranged from 2,000-10,000 Fcfa, whereas the median expenditure for activities which decreased or did not change ranged from 9,000-61,250 Fcfa. Overall, these expenditures indicate that relatively low-cost activities tended to increase and that relatively high-cost activities tended to decrease.
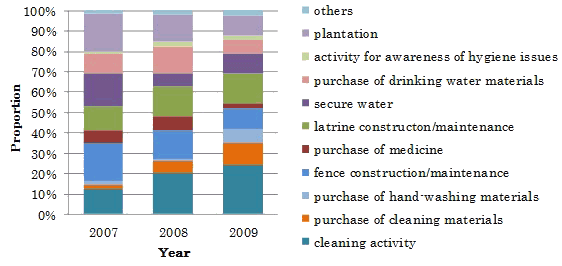
Figure 2: Details of health related activities implemented in 2007, 2008 and 2009.
Focus group discussions
Eleven CPs, 15 principals and 15 COGES members from 15 primary school communities participated in the FGDs. Five CPs in group CP2 could not participate in the FGD due to their participation in another workshop held in their school districts. As only one CP in group CP2 could participate, the method was changed to an in-depth interview using the same structured questionnaire as was used for the FGD. In-depth interviews were conducted by telephone with four out of the five CPs who could not participate in the FGD.
Use of the 10QC: The answers to the question whether they have distributed/used or knew about the 10QC were generally 'yes'. The answer was 'no', for 2 CPs and 1 COGES member. Where the answer was 'no', there appeared to be a lack of information exchanged between the officers. In these cases, some examples of the responses were:
I do not know that kind of document. I have just arrived for this post. I have never had a takeover discussion about it with my precursor or my colleagues. (CP in group CP2)
I have never seen it. I think our office never received this kind of document. (CP in group CP2)
Ways in which the 10QC was used: When the 10QC was introduced, CPs distributed and explained its use to school principals at the principals and teachers meeting with the cooperation of the officer from the health sector. In cases where the principals were absent, CPs visited primary schools to distribute it directly to principals and explain its use. Most of the principals and COGES members introduced activities from the 10QC to the COGES action plan. Principals also used it to raise awareness of the importance of hygiene to teachers, pupils and community members. Some examples of their responses are as follows:
We organized Assemblée Générale ([AG] meeting with teachers, parents and other community members) to raise hygiene awareness. We read the 10QC to them to help them understand the contents and, moreover, the importance of health and hygiene. (Principal in group Principal1)
We got inspiration from 10QC to initiate an elaborate action plan. (Principal in group Principal2)
It is simple, we acted on 10QC. (Principal in group Principal3)
Current implementation and reasons for use of the 10QC: All participants who were aware of the 10QC continued to use it. They expressed that health and good hygiene were necessary and assisted with study. They also expected that school awareness of health and hygiene spread to the wider community. Moreover, the principals thought that 10QC was useful for orientating teachers towards health and hygiene. Most COGES members said that it saved time to use the 10QC when they prepared an action plan because it clearly stated how to plan health expenditure. Participants also found that projects operated by NGOs or the government were able to collaborate with 10QC activities. Some example responses are listed below:
The NGO or government project organized training on how to use the toilet, and it was linked to one of the activities on the 10QC. (CP in group CP1)
COGES collaborated with government or NGO projects to implement their activities, such as preparation of cleaning materials, hand-washing stands, soaps etc. (CP in group CP1)
Hygiene is the base of education activities. We have to avoid diseases caused by lack of hygiene to promote a good school record among pupils. (Principal in group Principal1)
10QC is of collective interest to parents and pupils. It covers their interest in health. (Principal in group Principal3)
Impressions of the 10QC: Most impressions were positive. Participants said that the 10QC was simple and easy to understand. They noticed changes of behaviour such as toilet use, trash-can use, hand-washing, cleanliness of the body, clothes, and a change in attitudes to health after using 10QC. They also felt that if the school environment became clean, then class attendance and pupil health might improve, and that good practices might be passed on to the wider community. Some example responses follow:
10QC covers the theory and practice of health and hygiene matters. (CP in group CP1)
I heard that a pupil asked his/her parents to buy soap for hand-washing. (CP in group CP1)
The pupils used to come to school without washing their faces, but now they are ashamed to come to school without washing their face. They also wash their hands with soap. (Principal in group Principal1)
Hand-washing behaviour transferred from pupils to parents. (Principal in group Principal2)
The number of pupils who have conjunctivitis decreased. (CP in group CP1)
The number of pupils who have ringworm, rashes or spots has decreased. (Principal in group Principal3)
Some villagers constructed toilets in their house. (COGES in group COGES1)
The whole village became clean. (COGES in group COGES1)
Difficulties and support needed in using the 10QC: All participants indicated difficult access to water. Another major problem was budgetary and material constraints, as is illustrated in the following responses:
It takes more than one hour on the back of a donkey to get water. (COGES in group COGES1)
There are only two small wells in our village. These wells supply water for about 3200 inhabitants. (COGES in group COGES3)
Our school does not have modern latrines. We can construct only traditional latrines due to budget limitations. It is unreliable, and breaks every rainy season and we have to reconstruct it every year. (Principal in group Principal2)
We have a limited budget. It is very difficult to decide which activity to give priority. (Principal in group Principal2)
We do not have any budget for monitoring. We cannot buy gasoline to visit schools. (CP in group CP1)
To solve these matters, respondents reported needing financial support, donation of materials such as brooms, soap, hand-washing stands, and construction of latrines and/or water points by the government or NGOs.
We cannot afford to construct modern latrines or water points. We just wait for a call from the government or NGOs for their projects. We do not know how to approach them. (COGES in group COGES1)
Respondents also indicated that there was a lack of understanding among teachers and community members, and a lack of collaboration with health officers, as is indicated in the following responses:
Community members did not understand. It was very difficult to collect contributions for COGES activities. (COGES in group COGES1)
Health officers rarely visited schools. I think collaboration with health officers to sensitize community members is necessary. (Principal in group Principal3)
We need health officers to inspect and authorize food vendors. (CP in group CP1)
I think that we should introduce health education to the primary school curriculum. (CP in group CP1)
10QC is clear enough to understand, but...actually it depended on the level of teacher. Some teachers did not have sufficient capabilities. We should reconsider teacher training programs and recruitment processes. (CP in group CP1)
It is better to integrate health education into the teacher training program. (CP in group CP1)
Discussion
Although the data used for analysis were based on a single pilot project and were collected in a cross-sectional manner, these primary schools in Niger exhibited a clear improvement in their health practices. The number of schools that implemented health/hygiene-related activities increased after the distribution of an uncomplicated written guide which introduced some simple activities without requiring any training. The major factors contributing to the success of this project were that it was simple, practical and open to collaboration.
The guide developed by the West African Centre for International Parasite Control Project (WACIPAC) was simple enough to be understood without training. Training, including awareness of health-related issues and activity planning, is an important factor for successful implementation of the HPS4,15-17. Some FGD participants in this study also reported that teachers lacked an understanding of the importance of hygiene. Thus, teacher training is seen as imperative to school health improvement. However, budget limitation in developing countries, even at the level of central government, are one of the most serious problems. As such, it is very difficult to organize cost-intensive training. In fact, even in developed countries, lack of funding impairs the implementation of HPS18-21. Therefore, simplification of implementation methods, to the point that they can be practiced without training, might be a better way to address the issue. The 10QC, which simply consists of printed A3 paper with some photographs, is inexpensive and requires little in the way of investment in materials.
As a number of previous studies have mentioned, long-standing commitments from governments are needed to implement HPS17,18. However, some authors have noted that the existence of a government policy does not solely ensure the success of HPS and that a gap between policy and practice was sometimes observed19,21. Both the existence of a policy and a system to put it into action were necessary20,22,23. The 10QC was distributed to primary schools through the Ministry of National Education, as a national program. Moreover, the 10QC introduced practical ideas for improving health and hygiene. Implementation of the activities on the 10QC provided a system by which school health policy could be put into practice. Thus, this approach might improve the outcomes of the HPS initiative.
The concept of 'collaboration', as stated in a 1997 WHO report3, is an important factor in HPS success, and has been recognized as such by many authors19,21,24,25. In this context, 'collaboration' refers to intra-sector cooperation on health and education between NGO agencies, governments and communities. Formal ministerial level collaboration is essential for national policy development19, and this exists in Niger. However, as some FGD participants pointed out, cooperation might not succeed at the local level and strengthening local level collaboration is essential for the successful expansion of 10QC. Another collaboration that is also important for the successful HPS implementation is that among the related personnel/organization, school, family and community26. The COGES involvement in 10QC usage might be the most crucial factor for the success of health and hygiene activities in primary schools in Niger. The COGES is composed of a principal, teacher representative, parents and community members. These active and functional committees, which were initially formed by the JICA 'Schools for All' project to manage primary schools, already have strong partnerships with each other and have the capacity to influence the community. Furthermore, some studies have indicated that leadership and/or ownership were significant factors17,25. Leadership occurs via COGES because its members are elected by the whole community, and its activities are decided by the meetings and community participation.
Use of the 10QC to create a healthier environment in primary schools had a great deal of positive impact and very little negative impact. In Niger, most school activities depend on COGES management. As such, school activities are covered by the COGES budget, which is heavily constrained because it consists only of contributions from community members. In the present study, the tendencies for increased implementation of relatively low-cost activities and decreased relatively high-cost activities were evident. This resulted from management efforts of COGES that considered the balance of priority and the practicality of activities. Another fact revealed by this study was that the fulfilment rate of health-related activities was always lower than that of other activities. This also resulted from the balance of budget and priorities. Activities such as classroom construction, purchase of tables and chairs for pupils or purchase of blackboards and chalk were of higher priority than health-related activities. Collaboration with other organizations, especially in the health service domain, might be helpful for improving fulfilment of HPS components in the future.
Successful models of comprehensive self-evaluation systems have usually been implemented in countries where the school health management system has been well developed9,10. Those countries also have robust monitoring and evaluation practices. However, a school health management system has not been well-established in Niger. Despite this situation, positive results were evident. This may be because the 10QC was focused on only one component of HPS: a healthy environment. Establishment of health management systems and effective monitoring and evaluation are necessary for the expansion of HPS in the future.
A major limitation of this study are that the data used for the analysis only came from COGES reports, which were collected in a cross-sectional manner, with no observational data or information from pupils. This project was initiated as an international development program and not designed as a research program. Therefore, the project may have limited suitability for research. However, existing documents (action plan and activity report) provided reliable data sources. Although this cross-sectional data is not as effective as longitudinal matched data for evaluating long-term effects of a program, a clear tendency towards positive alterations in health-related behaviours was evident. Unfortunately, direct observations at the pilot site were not possible because of security issues. However, some insight into the health situation of pupils was reported by FGD participants. The involvement of other organizations/campaigns, such as government, NGOs, and international organizations, with the health and hygiene activities in primary schools was reported in the FGDs, and so the positive outcomes detected in this study might not be purely from the use of 10QC. However, even if the other projects influenced the COGES activities, this study indicated that 10QC use did not conflict with other health-related projects. Additionally, some of these projects implemented their activities in collaboration with community 10QC activities. Despite the established theory that there can be conflict when multiple projects which exist simultaneously at the same site27, synergy would be expected between the use of 10QC and the other projects.
The 10QC usage is effective in addressing health/hygiene issues because it is simple to implement, easy to understand and does not conflict with projects conducted by other organizations. This simple tool might be applicable to other developing countries with careful attention to the key factors that were learnt in this study.
Recommendation
The use of 10QC was expanded into a nationally-adopted standard after this pilot project. An effective, simple and low-cost monitoring and evaluation system should be developed to sustain the implementation of school health policy in Niger. As the existing 10QC is limited to the healthy environment goal of HPS, its extension to cover other HPS components should be considered.
Acknowledgements
The authors acknowledge the tremendous support of Mr Mounkaila Mahamadou, Ms Mariama Tahirou, both from Bureau Santé Scolaire, the Ministry of National Education, Mr Aboudou Yacouba from Organisation Nigerienne des Educateurs Navaturs (ONEN) and Mr Seyni Yacouba form Direction Départementale de la Santé Public et lutte contre les Endémies (DDSP/LCE) in Dosso, to conduct focus group discussion. The authors thank the Niger Ministry of National Education, the Japan International Cooperation Agency (JICA), the JICA office in Niger, and the 'Schools for All' project in Niger, for their cooperation with the project. The authors are grateful to all staff of Bureau Santé Scoraire, the Ministry of National Education, Niger, for their contribution to intervention and data collection. This work was supported by a Grant for Research on Global Health and Medicine (21A-3, 24A-2) from the Ministry of Health, Labour and Welfare, Japan.
References
1. World Health Organization. WHO's Global School Health Initiative: Health-Promoting Schools. (Online) 1998. Available: http://www.who.int/school_youth_health/media/en/92.pdf (Accessed 2 March 2012).
2. United Nations Educational, Scientific and Cultural Organization. World Education Forum; 26-28 April 2000; Dakar, Senegal, 2000. Available: http://unesdoc.unesco.org/images/0012/001211/121117e.pdf (Accessed 15 February 2012).
3. World Health Organization. Promoting Health through Schools. (Online) 1997. Available: http://whqlibdoc.who.int/trs/WHO_TRS_870.pdf (Accessed 12 February 2012).
4. Moon AM, Mullee MA, Rogers L, Thompson RL, Speller V, Roderick P. Helping schools to become health-promoting environments-an evaluation of the Wessex Healthy Schools Award. Health Promotion International 1999; 14(2): 111-122.
5. Rogers E, Moon AM, Mullee MA, Speller VM, Roderick PJ. Developing the 'health-promoting school' -- a national survey of healthy schools awards. Public Health 1998; 112(1): 37-40.
6. Bundy D, O'Connell T, Drake L, Baker S, Abrioux E. School Health, Nutrition and HIV/AIDS Programming: Promising Practice in the Greater Mekong Sub-Region. (Online) 2009. Available: http://www.schoolsandhealth.org/Documents/SHN%20and%20HIV_AIDS%20progs%20-%20Good%20Practice%20in%20Greater%20Mekong%20sub-region.pdf (Accessed 17 August 2013).
7. Ministry of Public Health and Ministry of Education, Kingdom of Thailand: Standard Criteria for Assessment of Health Promoting Schools, Primary School Level (Educational level 1-2). Bangkok, Thailand: Ministry of Public Health and Ministry of Education, no date.
8. Lee A, Cheng FF, St Leger L. Evaluating health-promoting schools in Hong Kong: development of a framework. Health Promotion International 2005; 20(2): 177-186.
9. Yoshimura N, Jimba M, Poudel KC, Chanthavisouk C, Iwamoto A, Phommasack B et al. Health promoting schools in urban, semi-urban, and rural Lao PDR. Health Promotion International 2009; 24(2): 166-176.
10. Akiyama T, Win T, Maung C, Ray P, Kaji A, Tanabe A, et al. Making schools healthy among Burmese migrants in Thailand. Health Promotion International 2013; 28(2): 223-232.
11. United Nations Development Programme. Human Development Report 2010. (Online) 2010. Available: http://hdr.undp.org/en/reports/global/hdr2010/chapters/en/ (Accessed 12 February 2012).
12. Ministry of National Education, Republic of Niger: Statistiques de l'éducation base 2008-2009. Niamey, Niger: Ministry of National Education, 2009 (in French).
13. Ministry of National Education, Republic of Niger: Arrêté N° 0000213/MEB/A/SG, 2003. Niamey, Niger: Ministry of National Education, 2003 (in French).
14. Ministry of National Education, Republic of Niger: Arrêté N° 00098/MEB/A/BSS, 2005. Niamey, Niger: Ministry of National Education, 2005 (in French).
15. Aldinger C, Zhang XW, Liu LQ, Pan XD, Yu SH, Jones J et al. Changes in attitudes, knowledge and behavior associated with implementing a comprehensive school health program in a province of China. Health Education Research 2008; 23(6): 1049-1067.
16. Zhan XW, Liu LQ, Zhang XH, Guo JX, Pan XD, Aldinger C et al. Health-promoting school development in Zhejiang Province, China. Health Promotion International 2008; 23(3): 220-230.
17. Deschesnes M, Trudeau F, Kébé M. Factors influencing the adoption of a health promoting school approach in the province of Quebec, Canada. Health Education Research 2010; 25(3): 438-450.
18. Rissel C, Rowling L. Intersectoral collaboration for the development of a national framework for health promoting schools in Australia. Journal of School Health 2000; 70(6): 248-250.
19. Stewart DE, Parker E, Gillespie A. An audit of health promoting schools policy documentation. Journal of School Health 2000; 70(6): 253-254.
20. Stokes H, Mukherjee D. The nature of health service/school links in Australia. Journal of School Health 2000; 70(6): 255-256.
21. Deschesnes M, Martin C, Hill AJ. Comprehensive approaches to school health promotion: how to achieve broader implementation? Health Promotion International 2003; 18(4): 387-396.
22. St Leger L. Australian teachers' understandings of the health promoting school concept and the implications for the development of school health. Health Promotion International 1998; 13(3): 223-235.
23. Lee A, Cheng FF, Yuen H, Ho M, Lo A, Fung Y et al. Achieving good standards in health promoting schools: preliminary analysis one year after the implementation of the Hong Kong Healthy Schools Award scheme. Public Health 2007; 121(10): 752-760.
24. Lee A, Tsang C, Lee SH, To CY. A comprehensive "Healthy Schools Programme" to promote school health: the Hong Kong experience in joining the efforts of health and education sectors. Journal of Epidemiology and Community Health 2003; 57(3): 174-177.
25. Inchley J, Muldoon J, Currie C. Becoming a health promoting school: evaluating the process of effective implementation in Scotland. Health Promotion International 2007; 22(1): 65-71.
26. The European Network of Health Promoting Schools. In: Proceedings, First Conference of the European Network of Health Promoting Schools "The Health Promoting School - an investment in education, health and democracy"; 1-5 May 1997; Thessaloniki-Halkidiki, Greece, 1997. (Online) 1997. Available: http://www.euro.who.int/__data/assets/pdf_file/0013/120307/E72971.pdf (Accessed 15 February 2012).
27. Office of the United Nations High Commissioner for Human Rights. Frequently Asked Questions on a Human Rights-based Approach to Development Cooperation. (Online) 2006. Available: http://www.ohchr.org/documents/publications/faqen.pdf (Accessed 2 March 2012). __________________________________
Appendix I: Organizational chart
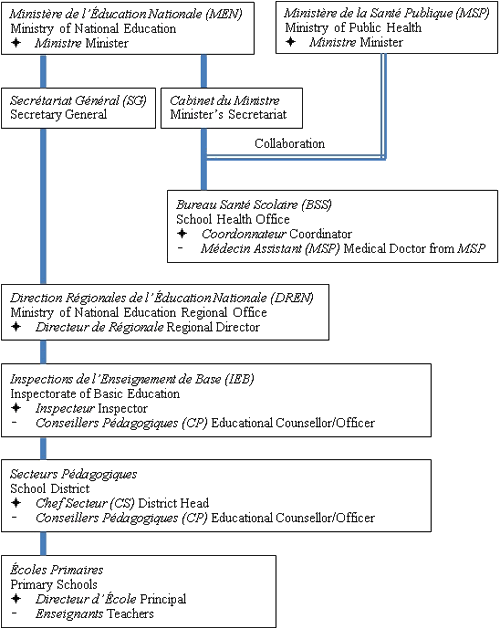
Appendix II: Glossary

Appendix III: Ten key questions



