Oral health is an important quality of life indicator and has systemic effects on general health1. Yet, dental care utilization and oral health outcomes in much of rural America are well below the rest of the nation, making it the fifth most important US rural health concern2,3. One approach that states have taken to ameliorate this problem is to fund dental education as a means to increase the supply of dentists. In 2000, 36 states had public dental schools4. Beyond increasing the total number of dentists, states are also looking at ways to attract dentists to rural and underserved areas. The focus of this study was to examine how a dental school in rural Southwest Virginia would influence the supply of dentists and dental utilization in that region. It may serve as a model for the expected impact of a dental school in other rural areas of the country.
The Southwest Virginia region is a rural, mountainous area consisting of seven counties and covering 8342 km2 (3221 miles2) with approximately 205 000 residents (Fig1). Only 28% of the population lives in high density areas containing 1000 or more residents 1.6 km2 (1 mile2) compared with the state average of 72.2%5. The low density, combined with the fact that the region has a low ratio of dentists to population (19 private practice dentists per 100 000 residents in 2007 compared with 53 and 54 for Virginia and the USA, respectively), means that individuals must travel further to reach their dentist6.
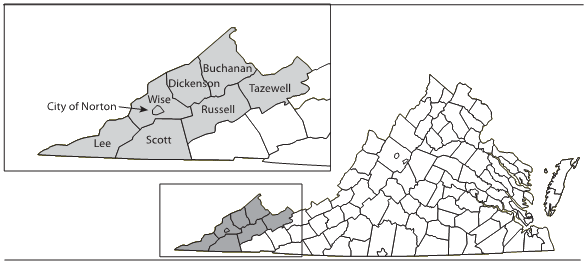
Figure 1: Map of Southwest Virginia.
Children and adults in Southwest Virginia experience relatively poorer oral health outcomes than either the state or nation. The Virginia Department of Health statewide screening of 8000 third graders in 2009 found that, by every measure, children in Southwest Virginia had poorer oral health outcomes by statistically significant margins7. Statewide, 15.4% of third-grade children had untreated caries, while 34.4% in Southwest Virginia had untreated caries7. Similarly, adult oral health is poorer in Southwest Virginia than the state average. Southwest Virginia adults who had visited a dentist or dental clinic within the past year for any reason ranged from 52.7% to 60.1%, between 1999 and 2008 compared with a Virginia utilization rate ranging from 70.7% to 76.4% and the national rate ranging from 69.8% to 71.3%8.
The low dental utilization does not appear to be due to a lack of interest in obtaining dental care. When dental services are provided at no or a reduced cost, a large number of people in the region attend. Since the Mission of Mercy (MOM), a foundation that provides free dental services, was founded in 2000, 46 500 patients have received free dental care across the state9. Many of those have been at the Remote Area Medical Clinics (RAM) held annually in the Southwest Virginia towns of Wise and Grundy, where dental care is among the most popular services. The 'Smiles for Children' program, which is Virginia's Medicaid dental program, also has had success at enrolling children in Southwest Virginia, having a higher rate of children enrolled than the rest of the state. Regional clinics that provide reduced price services, such as the Southwest Virginia Regional Dental Center and Clinch River Health Services, have long waitlists for dental services.
In an effort to expand the size of the dental workforce, increase dental service utilization and ultimately improve oral health outcomes in the region, one proposed policy intervention is to create a dental school in the Southwest region. The focus of this study was to examine a proposal for a dental school as a part of the University of Virginia's College at Wise, a four-year liberal arts school that draws the majority of its students from the Southwest region.
Dental schools come in many different sizes and configurations. To examine the likely effect of the proposed school in Southwest Virginia, a hypothetical dental school was developed under plausible assumptions as a baseline. A policy simulation was conducted by focusing on two different channels through which the dental school would likely affect the regional dental workforce and dental service utilization. First, some graduates are expected to be retained and supplement the local dental workforce. Second, students in the clinical phase of the pre-doctoral program and residents in a general dentistry residency program will provide clinical dental services to area patients. Dental clinical faculty who provide services intramurally (through the dental school) or extramurally (in private practice setting) offer a third channel for a dental school to contribute to the local labor force. Faculty member services provided to private patients is assumed to be fixed under the different policy simulations.
Baseline dental school
As a baseline, a class size of 50 students was assumed, for a total of 200 students in the pre-doctoral program. A 50 student class size is the median for a cohort of recent and planned or proposed peer institutions with an institutional emphasis on rural public dentistry. The size of the residency program was assumed to be 24 postdoctoral residents, which is comparable to the dental program at nearby West Virginia University. It was also assumed that faculty perform fee-for-service dentistry once a week either within the program or in an extramural private practice, which is a typical allowance for most dental schools.
The simulation required several additional assumptions, which were drawn from current practice or from available studies. First, based on American Dental Association (ADA) data, academic attrition (for financial, academic, and other reasons) started at 2.5% in the first year and falls in later years10. Therefore, the graduating cohort is somewhat smaller than the first-year cohort. Second, the graduates choosing to settle in the region were drawn from the ranks of graduates who already resided in the Southwest region when they entered the program. Based on estimates from prior studies, it was assumed that 25% to 30% of local resident dental graduates will remain in the region11,12. Third, additions to the local dentist supply do not displace existing dental practices; they are a net rather than gross addition to the stock of dentists available in the region.
Fourth, dental school graduates who initially locate in the region would be subject to a risk of out-migration. Data from the 2009 US Census showed that the average Virginia resident with a professional degree had a 3% per year out-migration rate due to normal life-cycle and economic reasons (eg marriage/divorce, career changes, change of practice location, illness/retirement)13. While re-locations to other regions of the state occur at a higher frequency of 5%, there were no estimated migration rates for particular multi-county regions such as Southwestern Virginia. The conservative estimate of only a 2% out-migration reflects a stronger regional attachment of local graduates.
Finally, clinical faculty would contribute to the availability of dental services through faculty practices housed in the dental schools or in practices outside the school14. According to Bailit et al, faculty practices primarily treat insured and fee-paying middle and upper income patients15. Therefore, they have an effect on regional workforce levels but have little impact on utilization by the underserved. The model assumed that full-time faculty members who are dentists generally work one day per week seeing their own patients. The school is expected to employ 37 faculty members, which is comparable to the student-to-faculty ratios at other US dental schools. Therefore, the faculty members would add the equivalent of 7.4 dentists to the regional workforce. Of these, approximately 60% would be specialists, resulting in a contribution of 4.4 specialists and three generalists.
Educational pipeline
The number of local dental school graduates who are expected to stay in the region depends to a great extent on the number of people from the region who attend the school16. Three different levels of representation (low, medium, and high) of Southwest Virginia students in the dental school were examined (Table 1). The first scenario assumed that the dental school enrolls students from the region in the same proportion as Virginia Commonwealth University's (VCU) School of Dentistry, or 1.78% of each entering class is from the Southwest region. This level of representation was based on records from VCU showing a total of eight first-time students from Southwest Virginia out of a total of 450 students for the entering classes from fall 2005 to fall of 2009. At first glance, it may seem reasonable to conclude that a dental school in the region would naturally have a higher draw from the region than is currently true of VCU. However, the cost of attending the schools would be comparable and VCU, with its established reputation would still draw some of the qualified students from the region. So, even if there were more applicants due to the visibility of a regional program, admission would be competitive and eligible students would have choices about where to attend.
Table 1: Dental school simulation scenarios
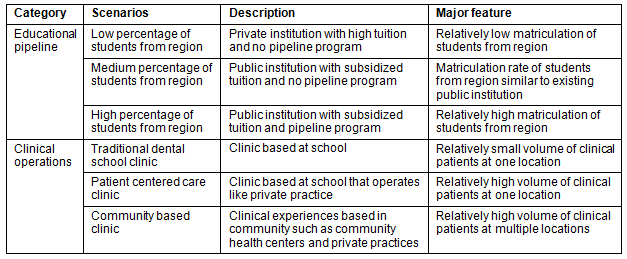
The second scenario assumed a lower percentage of Southwest Virginia residents enrolled in the dental school, based on the likelihood that the school would not receive an operational subsidy from the state and would need to charge tuition comparable to private dental schools. The VCU receives an annual state appropriation that reduces tuition costs. Therefore, a low 0.875% of each incoming class comes from Southwest Virginia, almost half the level of VCU, was assumed. The third scenario assumed that a successful regional dental education pipeline program is established, which raises the percentage of Southwest students at the school to 2.5%, roughly the same percentage as the region's share of the total state population.
To simulate the effect of the increased number of local dental school graduates on regional dental utilization rates, several additional assumptions were required. Dentist productivity, which depends on a variety of factors including hours worked, number of operatories, number of auxiliaries etc11,17 was assumed to resemble that of the average dental practice in the region. To provide a more detailed and current picture of dentists practicing in the region, a Dental Needs Survey was conducted, in which 54 dentists operating in the region, and a random selection based on diverse geographic locations of 54 dentists practicing elsewhere in the state, were surveyed18. Results were based on a 51% response rate. The dentists who responded to the patient and dental visit questions and dental staff questions treated 1406 patients per full-time equivalent dentist per year. Therefore, each graduate who remained in the region was assumed to generate this number of patients, as well as treating the same percentage of indigent/Medicaid patients as the statewide average of 8%, as reported by respondents to the survey. Finally, it was assumed that all dentists retire after practicing for 35 years, an estimate consistent with an average retirement age of 62 years19.
Clinic models
The second pathway by which a dental school could affect regional dental health outcomes is through clinical services to patients. Three competing models for dental school clinical education were examined (Table 1): (i) the traditional dental school clinic; (ii) the patient-centered clinic; and (iii) the community-based clinic. Each model has a different mix of clinical care volume, revenue, clinical skill development, cost-effectiveness, and quality of patient care. These clinical models served as scenarios for estimating the relative magnitudes of their effects on dental health services in the Southwest region.
Traditional dental school clinics: Dental school clinics are set up as teaching laboratories. Students typically treat patients while faculty observe. Faculty do not treat patients. The typical fourth year student sees two patients a day, and many patients must make multiple visits for more complicated procedures. As a result, typical clinics see relatively few patients. The low volume of services provided and the generally low income of the patients mean that dental clinics do not generate enough income to cover costs. As a result, clinics often require subsidies in the range of $40,000-50,000/chair per year20.
Patient-centered clinics: This dental school model makes patient care rather than student education the central focus of the clinic20. Faculty, students and residents provide care in a delivery system similar to private practices, with auxiliary staff and increased attention paid to customer service and program financial viability. Relative to the traditional model, there is increased emphasis on improving clinic capacity utilization, for example by introducing modern clinic management methods, operating evening and weekend hours throughout the year, and scheduling shorter appointments20. These types of clinics generate lower net costs and give the faculty an opportunity to participate in clinics on an intramural basis for research or as a source of income to supplement their teaching salary.
Community-based clinics: The key feature of this teaching model is the assignment of students to community clinics and private practices for multiple-week clinical rotations21. First introduced by the University of Colorado, this model has since spread to other institutions. Evidence suggests that students in community settings are much more productive than the traditional clinical model because of the availability of auxiliary staff21. Bailit et al estimated that students in community-based clinics are three to four times more productive than when they are in traditional dental school clinics21. Bean et al found a similar productivity boost: students conducted twice as many procedures in less than half the time21. Overall, students can expect to treat six to eight patients each day at community-based clinics21,22. Given that patient-centered and community-based clinics are relatively new, further research is needed on the effect of these clinic models on student training, and quality of care data would be useful.
Comparing the clinic models
In order to estimate the effects of these clinical scenarios, some parameters were adopted from an analysis of the expansion of dental safety net options from Bailit et al and an analysis of the dental safety net23,24. These studies assumed that all patients treated by the clinic based students and residents are low-income patients, based on the preponderance of such patients in dental school clinics. Typical clinical charges are less than half of what is charged by a private practice, with uncompensated care an estimated 15 to 16% of the cost of all care provided by the clinic25. Faculty time in the student clinics is assumed to be restricted to instructing and assisting. For simplicity, resident productivity is assumed to be unaffected by the clinical model and will extrapolate from resident productivity patterns observed for pediatric dentistry and advanced education in general dentistry (AEGD) residents at the University of Connecticut School of Dental Medicine in Farmington. Each resident saw, on average, 415 patients during the year of the study, resulting in approximately 9960 patients who would be treated by a dental school clinic (24 residents at 415 patients per year each). Student clinic productivity depends critically on the clinical model, with patient-centered and community-based clinics being roughly three times more productive.
The number of patients treated for the baseline dental school using a traditional clinical model was estimated based on a reported 2 927 250 patient visits to US dental schools in 2008-2009 and an average of 13 visits per patient during the year as reported by Bailit et al (this slightly overestimates productivity in a traditional clinic since some patient-centered and community clinic activities generate the patient counts)23. Bailit et al further estimated that senior dental students generate 75% of clinical patient contacts and junior students the remaining 25%. Based on a national headcount of 4906 seniors and 4960 juniors during the 2008-2009 school year, this implies that a senior student will treat approximately 34 patients and a junior student approximately 11 patients. Junior and senior cohorts of 49 each (accounting for attrition from an entering cohort of 50) would treat 2243 patients each year. Under the patient-centered and community-based model the number treated would be considerably higher. Bailit et al estimated that senior students would provide 60 days of care per year, treat seven patients per day, and have repeat visits per patient approaching 2.3. Under these high functioning clinic scenarios, an estimated 8948 patients ([49 senior students x 60 days x 7 patients per day]/2.3 visits per patient) could be treated each year.
Not all underserved patients would be expected to come from Southwest Virginia. In order to estimate the number of patients from within the region, the population potential of the Southwest region was compared to the population potential of counties with mean population centers (or population centroids) within 97 km (60 miles) of the population centroid for Wise County (where the dental school is assumed to be based). The regional population share is 63.3%, which is used in the traditional and patient-centered clinical scenarios. For the community-based model, the students and residents are assumed to be dispersed to locations throughout the region but have a much higher local share (90%) of patients due to restrictions on serving patients outside of the service area for the clinic.
Ethics approval
This study was reviewed by the University of Virginia Institutional Review Board and received exempt status.
Results vary by both the education pipeline and clinical models scenarios. The education pipeline component of the simulation reveals a large difference in the cumulative number of dentists who can be expected to remain in the region under different recruitment scenarios. In the first three columns of Table 2, the results are shown for the three local dental student enrollment scenarios: (i) the dental pipeline with high enrollment; (ii) VCU equivalent enrollment; (iii) and low enrollment under a private school funding model. The cumulative effect varies from a low of three to a high of nine dentists from 2020 to 2053. The last three columns show the estimated number of underserved patients who receive care as a result of the supply increase. Under the best-case scenario (dental pipeline), an estimated 1037 additional underserved patients receive dental care in 2053. Under the low uptake scenario (private school tuition), an estimated 363 additional underserved patients receive care.
Results for the clinical model component of the simulation (Table 3) reveal a stark difference in number of Southwest Virginia patients served, ranging from 7727 under the traditional clinic model to 17 017 under the community-based model.
Table 2: Number of clinical patients served
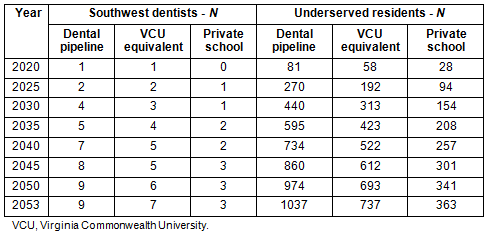
Table 3: Cumulative effects of dental school graduates on regional dentist supply and underserved patients
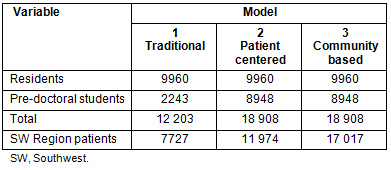
Combining the results of the dental pipeline and the clinic model, the range of possible outcomes for the number of additional dentists resulting from faculty who also practice privately, the number of graduates who choose to remain in the region, the number of newly served residents, and the dental utilization rate that could be expected in the region are shown (Table 4). In a low yield scenario (ie private school with a traditional clinic), potentially 8090 underserved patients (363 treated by graduate dentists and 7727 treated within the clinic) would receive care. The medium-yield scenario, with the patient-centered model and the percentage of students from the Southwest region equivalent to the percentage from Southwest Virginia who attend VCU, would result in 12 711 underserved patients receiving treatment. In a high yield scenario (ie dental pipeline program with community based clinics) could result in as many as 18 054 underserved patients receiving care.
Table 4: Dental school workforce and utilization impacts by scenario
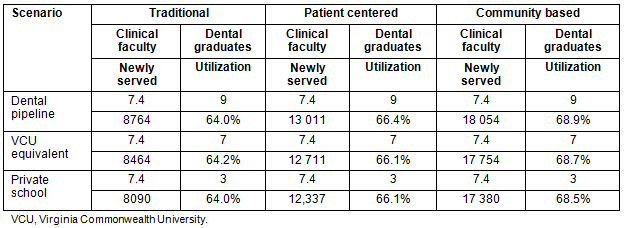
Even with the high yield scenario and the strong assumption that these patients would not otherwise access care, the utilization rate increases from its current 60.1% to 68.9%. This level still falls well below the rates observed both in USA (71.3%) and statewide (75.2%). Under the low-end scenario, the increase of 8090 patients treated would only translate into an increase in the dental utilization rate to 64%.
Evaluation of the effect of clinical services on utilization rates depends on the extent that services offered by dental school clinics displace services currently offered to patients on public insurance or pro bono to those without insurance. Displacement of the latter would tend to improve profitability of existing practices while displacement of the former could have the opposite effect. The Dental Needs Survey reveals a difference in the environment that dentists in Southwest Virginia work in and indicates that the region could accommodate the additional dentist workforce that results from the policy simulations. Southwest region dentists were more likely to perceive a regional disparity in providers and a need for policy assistance. In the Southwest region 28% of dentists indicated that they thought there were an inadequate number of dental providers in the region to meet demand for dental services, versus none of the dentists from elsewhere. One-quarter of Southwest region dentists reported that they had difficulty hiring dentist associates versus none in the Virginia benchmark group.
Discussion
One goal of building a dental school in Southwest Virginia is to increase the regional supply of dentists. In order to improve the prospects for retaining graduates it is important to have students from the region enter the dental pipeline. Two factors that are likely to limit the increase in dental graduates remaining in the region are the high tuition costs arising from attending an unsubsidized dental school program and the shortage of a qualified pool of applicants with adequate academic preparation. The average first-year in-state tuition of a state-supported school is $20,725 compared with a private unsubsidized school at $46,50426. Debt incurred from attending state-supported schools (private and public) is $142,671 compared with $204,734 for private unsupported schools27. The high cost helps explain the relatively high socioeconomic backgrounds of new dentists. Of dentists graduating in 2008, 42.9% were from families with incomes of $100,000 or more compared with only 21.2% from families with incomes of $50,000 or less27. The comparable figures for Southwest Virginia residents in these income categories are 8.4% and 60.5%, respectively. It is not clear that many residents would have both the ability and the economic resources to attend a regional dental school.
Entrance into dental school is highly competitive, typically requiring students to have a 3.5 grade-point average or higher from a selective undergraduate institution. The region has a significantly lower portion of the population that has graduated from high school or college than the national or state average. Census data from the 2005-2009 American Community Survey show that 85.8% of Virginia's adults are high school graduates, compared with 70.8% for the Southwest region. Similar disparities exist for adults with a bachelor's degree, where Virginia's average is 33.4% and the Southwest region average is 11.5%. Therefore, central to building the supply of dentists is providing sufficient financial support to regional dental students and building up the education pipeline to ensure that students are prepared for entry and successful completion of dental school.
A second goal of a dental school is to increase utilization rates, particularly among low-income residents. Dental schools clinics benefit lower income residents because they are able to provide dental services at a lower cost than private sector providers. First, students and residents offer their services below private rates to ensure that they receive adequate experience under the supervision of instructors. Second, federal funds for Graduate Medical Education (GME) help cover the costs of training dental residents. Third, dental schools may partner with organizations such as Federally Qualified Healthcare Centers (FQHCs), which receive federal funds to operate their clinical programs. Finally, Virginia may choose to modify existing laws to allow dental schools access to federal Medicaid matches for the administrative expenses of running their clinical programs, as has been done in other states15.
In addition to the estimated increases in dentist supply and utilization, the establishment of a regional dental school can have several other positive (albeit difficult to measure) benefits. First, dental schools may create new continuing education curricular opportunities for the area's dental workforce that would enable providers to improve their skills, knowledge, and patient care. Second, a dental school could serve as a demonstration laboratory and technology transfer center that disseminates information about new management methods, technology, and procedures in dentistry, helping to improve dentist productivity in the region. Third, a dental school could stimulate a greater level of public awareness about oral health care through both formal public outreach programs and a larger number of healthcare educators providing leadership roles in the community.
There are also some barriers to establishing a dental school that are unique to rural regions. One obstacle would include the high cost of establishing the necessary administrative and academic infrastructure and physical plant at an institution without existing accredited graduate/professional level health programs (eg a medical school). There may also be additional costs to operating a school-based clinic in a low-density rural region. The longer travel distances could present a challenge to attracting clinical patients, particularly during certain times of the day and seasons of the year (eg winter storm events). The result could be increased recruitment, marketing, and transportation costs. The lower oral health literacy levels among vulnerable populations in the region could also mean more resources may need to be dedicated to oral health literacy programming and outreach.
Finally, a Southwest dental school would also face hurdles recruiting qualified faculty. There is already a growing number of faculty vacancies at existing dental schools, a problem likely to become more pronounced in coming years with a sizeable increase in the number of dental schools, an aging faculty workforce, and continued or growing disparities between private dentists and dental school faculty salaries27-29. Faculty recruitment may be a formidable challenge, particularly for two-earner families where occupational matches in a rural region can be more challenging than for larger metro areas with thicker labor markets30. Furthermore, faculty members would have a more difficult time establishing extramural practices in the community because of a lack of sufficient demand in close proximity to the school.
Given the formidable challenges in building a dental school in a rural region, combined with the potentially low benefits, it is worth considering whether there are more cost-effective ways to improve oral health in the region. Bailit and D'Adamo discuss a number of oral health interventions that appear promising31. Iowa's 'I-Smile program', for example, has developed a virtual dental home for children where regional dental hygiene coordinators coordinate care among health agencies, families, and dental offices. Enhanced Medicaid reimbursement programs have proven in a number of states that they can significantly increase utilization rates, although not to the level of private insurance. Finally, Bailit and D'Adamo found school-based dental care programs using mobile FQHCs dental units, as is done in central Connecticut, is potentially the best way to overcome the cultural and transportation barriers to utilizing dental services faced by low-income children31. It would be worth exploring further the costs and benefits of these and similar programs relative to what is likely to be achieved by a dental school.
A new dental school in Southwest Virginia would result in an increase in the dentist workforce and utilization rates. The number of dentists who are likely to remain in the region is a function of the percent of students who are from Southwest Virginia. The representation of Southwest students in the entering class will depend on both the cost of the local dental school, as well as the educational preparation available in the region. While increasing the dental workforce will increase utilization rates, the bulk of the utilization impacts would result from the clinical training of students and residents and is sensitive to the configuration of clinical operations. Ultimately, a dental school would lead to an improvement in dental utilization levels, but would leave the region below US and statewide benchmarks.
References
1. U.S. Department of Health and Human Services, National Institutes of Health and Centers for Disease Control and Prevention. Annual report - Oral health in the U.S. (Online) 2002. Available: http://drc.hhs.gov/report.htm (Accessed 4 January 2011).
2. U.S. Department of Health and Human Services. Healthy people 2010, 2nd edn. Washington, DC: U.S. Government Printing Office, 2000.
3. Fos P, Hutchison L. The state of rural oral health: A literature review. In: L Gamm, L Hutchison, B Dabney, A Dorsey (Eds); Rural Healthy People 2010: A companion document to healthy people 2010. Vol 2. College Station, TX: The Texas A&M University System Health Science Center, School of Rural Public Health, Southwest Rural Health Center, 2003; 131-142.
4. Bailit HL, Beazoglou TJ. State financing of dental education: impact on supply of dentists. Journal of Dental Education 2003; 67(12): 1278-1285.
5. U.S. Census Bureau. Population estimates. Washington, DC: USCB, 2011.
6. U.S. Department of Health and Human Services, Health Resources and Services Administration. Area resource file 2009-2010. Washington, DC: Bureau of Health Professions, Office of Workforce Policy and Performance Management, 2011.
7. Virginia Department of Health. Dental Basic Screening of Third Grade Children. Richmond: VA, 2009.
8. Centers for Disease Control and Prevention, Office of Surveillance, Epidemiology, and Laboratory Services. Behavior Risk Factor Surveillance System (BRFSS). Atlanta, GA: CDC, no date.
9. Virginia Dental Association. Mission of Mercy website. (Online) no date. Available: http://vdaf.org/Mom-Details/ (Accessed 20 June 2012).
10. American Dental Association. 2008-09 survey of dental education academic programs, enrollment, and graduates: Volume 1. Chicago, IL: ADA Survey Center, 2010.
11. Beazoglou T, Bailit HL, Myna V, Roth K. Supply and demand for dental services: Wisconsin 2010-2020. West Allis, WI: Wisconsin Dental Association, 2010.
12. Bailit HL. Oral health education study. Madison, WI: Wisconsin Department of Health Services, 2010.
13. U.S. Census. Current Population Survey, Annual Social and Economic Supplement. Washington, DC: USCB, 2009.
14. Lee JY, Stamm JW. Intramural faculty practice plans: Their place in contemporary education. In: LJ Brown, LH Meskin (Eds). The economics of dental education. Chicago, IL: American Dental Association, Health Policy Resources Center, 2004.
15. Bailit HL. New Mexico dental school feasibility study. Santa Fe, NM: New Mexcio Department of Health, Public Health Division, Health Systems Bureau, 2010.
16. Formicola A, Bailit HL, D'Abreu K, Stavisky J, Bau I, Zamora G et al. The dental pipeline program's impact on access disparities and student diversity. Journal of the American Dental Association 2009; 140(3): 346-353.
17. Conrad DA, Lee RS, Milgrom P, Huebner CE. Estimating determinants of dentist productivity. Journal of Public Health Dentistry 2010; 70(4): 262-268.
18. Wanchek T, Rephann T, Shobe W. Oral health and the dental care workforce in Southwest Virginia. Charlottesville, VA: Weldon Cooper Center for Public Service, University of Virginia, 2011.
19. Beazoglou T, Bailit HL, Heffley D. The dental work force in Wisconsin: Ten-year projections. Journal of the American Dental Association 2002; 133(8): 1097-1104.
20. Formicola AJ, Myers R, Hasler JF, Peterson M, Dodge W, Bailit HL et al. Evolution of dental school clinics as patient care delivery centers. Journal of Dental Education 2006; 72(2): 110-127.
21. Bailit HL, Beazoglou TJ, Formicola AJ, Tedesco LA. Financing clinical dental education. Journal of Dental Education 2007; 71(3): 322-330.
22. Formicola AJ. Dental school clinics as patient care delivery centers: A paradigm shift in dental education. Journal of Dental Education 2008; 72(3): 19-20.
23. Bailit HL, Beazoglou TJ, Demby N, McFarland J, Robinson P, Weaver R. Dental safety net: Current capacity and potential for expansion. Journal of the American Dental Association 2006; 137(6): 807-815.
24. Beazoglou TJ, Heffley D, Lepowsky S, Douglass J, Lopez M, Bailit HL. The dental safety net in Connecticut. Journal of the American Dental Association 2005; 136(10): 1457-1462.
25. Weaver RG, Valachovic RW. ADEA survey of clinic fees and revenue: 2003-04 academic year. Journal of Dental Education 2006; 70(4): 448-462.
26. American Dental Association. 2008-09 survey of dental education, tuition, admission, and attrition, Vol 2. Chicago, IL: ADA Survey Center, 2009.
27. Okwuje I, Sisson A, Anderson E, Valachovic RW. Dental school vacant budgeted faculty positions, 2007-08. Journal of Dental Education 2009; 73(12): 1415-1422.
28. Bailit HL, Beazoglou TJ, Formicola AJ, Tedesco LA, Brown LJ, Weaver RG. U.S. state-supported dental schools: Financial projections and implications. Journal of Dental Education 2008; 72(2Suppl): 98-109.
29. Nash KD, Brown LJ. Rate of return from a career as dental school faculty. In: LJ Brown, LH Meskin (Eds). The economics of dental education. Chicago, IL. American Dental Association, Health Policy Resources Center, 2004.
30. Kuthy RA, McKernan SC, Hand JS, Johnsen DC. Dentist workforce trends in a primarily rural state: Iowa: 1997-2007. Journal of the American Dental Association 2009; 140(12): 1527-1534.
31. Bailit HL, D'Adamo J. State Case Studies: Improving Access to Dental Care for the Underserved. Journal of Public Health Dentistry 2012; 72: 221-234.

