Introduction
In any healthcare delivery system an appropriate structure is essential to promote comprehensive scope, continuity, integration of components and operational efficiency. Patients must be able to easily access healthcare workers and/or health centers in their own community. In the first contact with a healthcare practitioner, particularly if that contact is with a GP, 90% of patient needs can be met. If the initial problem cannot be managed, the decision will be made to refer the patient to a specialist or hospital outpatient department (OPD)1.
The referral system offers one strategy for making the best use of hospitals and tertiary healthcare services, but all patients should be seen first by a primary healthcare physician who decides whether a referral is necessary (Fig 1). In other words, access to hospital care should be through primary healthcare centers, except for emergency cases where patients may access the hospital directly via the hospital's emergency department2. This avoids system inefficiencies such as disadvantaged groups suffering from a lack of specialist care due to specialist doctors being overwhelmed by inappropriate self-referrals.
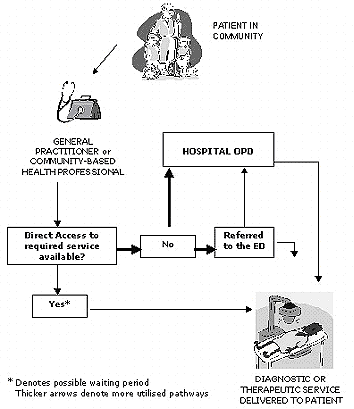
Figure 1: The referral pathway.
Active participation of the patient and their family (in the case of a minor) in the referral process leads to an effective outcome and a high level of satisfaction for care-givers and patients, and a reduction in health costs3.
However, in spite of a referral structure, there may be situations where people by-pass a primary-care contact. Unnecessary self-directed referral makes the specialist system inefficient and leads to problems for the individual and the healthcare system, such as:
- Accrual of unnecessary costs to the system
- Payment difficulties for the patient
- Lack of comprehensive healthcare information for the patient
- Lack of planned referral and its benefits of continuity of care
- Lowered standards of specialist care due to overburdening
- Compromising the established referral system
- Patient transportation problems
- Inequitable patient access to components of the system
- Reduction in patients' sense of value of the referral system
- Reduction in patients' trust of the healthcare system
- Patient and physician diverging in understanding the purpose of and necessity for referral
- Weakened communication of and transfer of patient data between primary contact and secondary care
- Reduction in feedback and follow up after treatment procedures4-5.
Although it is thought that a referral system can lead to cost-effective utilization of health services, there is little published data about its effect on health services and its impact on the health of those in the community. The present study examined patterns of patient self-referral direct to specialist (private) and hospital OPD clinics (public) in three health insurance structures in the rural Kashan region, Islamic Republic of Iran, and aimed to establish the reasons for patient self-referral to specialists in the Kashan region.
The aim of the present study was to contribute to a better understanding of the variations in the Iranian healthcare delivery system, so that this information may assist change/restructuring of the three-level Iranian healthcare insurance system.
The setting
Geographic: Kashan city is one of the 17 cities of Isfehan Province, and it covers an area of 4415 km2, which is 4% of the total province. It is 205 km from Isfahan. It is located in the north of the province and south of Qom (Fig 2). It is 235 km south west of Tehran, the capital of Iran. It is on the main route to the south east of Iran. In the Kashan region in central Iran, a racially diverse population of approximately 285 395 live (84% urban and 16% rural) in a hot dry climate. The city is located on the eastern slopes of the Karkas mountains and on the western edge of the Kavir Desert. Kashan is an historically important centre with links back approximately 7000 years. Kashan can be accounted as one of the archaic cities of Iran. Archaeological discoveries in the Siyalk Hillocks which lie 4 km west of Kashan reveal that this region was one of the primary centres of civilization in the pre-historic ages. Kashan is one of the university precincts of Iran. There are 8 theological schools with approximately 2000 theologians, 5 universities, both state and private, with approximately 15 000 students. In addition to education, Kashan is of great agricultural importance and much of its land is under cultivation with crops such as cotton, cereals and vegetables. The production of rose-water from ancient rose gardens is of economic and historic significance. The industrial development of Kashan is advanced and its hand- and machine-woven carpets are world-famous and among the most important export items of the country. Kashan city is an important industrial centre with over 350 industrial facilities.
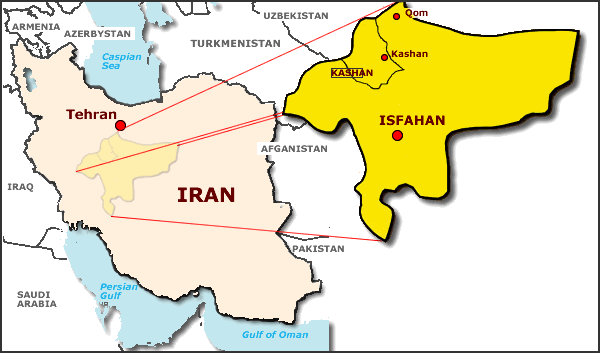
Figure 2: Map of the Kashan region in the province of Isfehan, Iran.
Rural demographics and health indicators: In Kashan, there are no significant variations between urban and rural areas. Even the most remote area is only 70 km from hospitals in Kashan city. In rural areas the birth rate per 1000 population is 17.6, the death rate per 1000 population 6.2 and annual rate of increase is 1.05%. The number of people per family is 3.77 urban and 3.6 rural. In rural areas the neonatal mortality rate per 1000 live births is 15, and infant mortality rate per 1000 live births is 14.74 (stillbirth rate is 0.29%). The mortality rate for those under 5 years per 1000 live birth is 21.5. Overall, the global fertility rate is 1.48 children (1.46 urban and 1.40 rural), and the maternal mortality rate is zero. The neonatal low birth weight (less than 2500 g) is less than 5%, and the rate of weight : age ratio with 2 variances from the mean in children under 5 years is 2.2%. Life expectancy at birth for males and females is 68.5 years and 71.4 years, respectively. Of the Kashan population, 7% is over 65 years of age; however, in rural areas 15% is over 65 years of age).
Per capita gross domestic product is US$1753, and total expenditure in the health area is 6.5%. Unemployment in the rural areas is low due to agriculture and traditional industries, such as hand weaving carpets. Piped water is accessible to 99.80% of the urban population and 99.63% of the rural population. In rural areas, 99.24% have access to electricity, 38.2 to telephone, and nearly all have easy transportation to the city centre. Rural health centres have ambulances on stand-by 24 h/day. There is universal access to the healthcare system, and the contact rate of individuals with a medical doctor is approximately 7 times/year. As in university precincts the world over, the area has a high proportion of specialists, with a GP : specialist ratio of (1.2).
The three health insurance structure
According to health system classifications, the Kashan University of Medical Sciences is responsible for health planning, implementing health programs and monitoring the health status of the community. The health of the 42 000 rural population is managed by 33 'health houses' (the lowest level of health care delivered by two healthcare workers and a GP available for one visit/patient per week) and the financial assistance of the Rural Health System Insurance. Patient co-payment is very low.
In the urban area, the health of the population of approximately 250 000 is managed by staff at 39 health centres, and four general and specialist hospitals. In the urban area, over 80% of the population is covered by one of a number of compulsory insurance plans such as health insurance, therapeutics insurance, social security insurance (state insurance for low-income urban workers), owner insurance. All these health plans are subsidised by the state government and co-payment is low; however, each person is free to select private insurance by paying additional out-of-pocket premium.
The rest of the population of approximately about 15 000 is insured for healthcare by the philanthropic Imam Khomeini Welfare Committee (IKWC) and pay no cost for treatment; however, they are bound to a closed referral system for their care.
Except for the self-insured and the non-insured, all clients in the three insurance system are assigned to one of a variety of insurance plans, according to, for example, their job, place of residence or economic situation. Doctor's-office visits for private-sector patients, outpatients in public healthcare clinics and hospital admission wards are stratified by insurance status.
The three insurance stratas and their referral routes include:
- Imam Khomeini Welfare Committee (closed-loop referral system): IKWC is a philanthropic organisation, and any family or person, urban or rural, who meets the criteria can be supported by this system. Patients visit the GP assigned at first contact. If necessary, the patient is assigned to a medical or surgical specialist or hospital for treatment, or to a paramedical clinic. In this system all clients have been assigned to GPs who contract with IKWC and every time patients need to, they will contact their specific GP. If the GP diagnoses that the patient needs referral to a specialist, he must complete the referral form and transfer the patient to an assigned specialist who is contracted to IKWC. This process of referral and assignment continues to hospital and higher levels of the healthcare system.
- Rural Health System Insurance (semi-closed-loop referral system): This system was constructed by the State Government and Health Ministry in order to expand health services in rural and remote regions. Patients in rural areas are visited by a GP. All patients covered by rural insurance, social security insurance, therapeutic services insurance, self-insured (private) and the non-insured (open referral system) are free to go to any healthcare worker, health centre, any specialist, super specialist or hospital, but the therapeutic services insurance representatives must be informed and will control the mix of services.
- All patients covered by the compulsory social security insurance, therapeutic services insurance, self-insured (private) and the non-insured (open referral system): These patients are free to go to any healthcare worker, health centre, any specialist or hospital for a low payment. In an emergency situation any hospital must admit the patient.
Methods
A random sample of 1036 individuals was selected from people attending outpatient clinics and specialist office visits in the private health sector. The sample size was estimated according to prior studies in which almost 50% patients were self-referred (calculated as p = 0.05, confidence coefficient 95% and error coefficient 3% of the number of the sample size 1036). Of the subjects, 413 (40%) were insured by the IKWC; 145 (14%) by the rural health system insurance; and 478 (46%) were covered by social security, therapeutic services insurance, out of pocket and other cost-payment procedures (free to contact any caregiver).
The patients or parents (if the patient was a minor) were interviewed individually in the waiting room by means of a questionnaire before or after their specialist visit, regardless of their type of referral. The questionnaire contained a series of items about demographic factors, referral type and patient reasons for self-referral. In order to improve questionnaire validity and reliability, the researcher conducted a pilot study on 100 subjects and consulted with experts and informed peers in the university.
In order to gather the data without error, interviewers were trained in two sessions, and the researcher as coordinator monitored and controlled the process of the research.
The self-referral rate in the triple insurance structure according to the public or private sector was calculated. The data were statistically analysed using a c2 test.
Ethical approval
Ethical issues such as research planning, implementation, data analysis and presentation received ethical permission from the Research Deputy of Health, University Research Director. All health centres and physicians involved, and all patients or parents gave permission during the research implementation.
Results
The number of patients attending doctors' offices and outpatients' specialty clinics according to the type of referral in the private and public sector are shown (Tables 1-3). In the IKWC closed-loop referral system and the Rural Health System Insurance, 6.8% and 29.7% of patients were self-referred directly to the specialist and hospital, respectively. In the open referral system, 75.5% of patients were self-referred.
Table 1: Referral type of patients from the Imam-Khomeini Welfare Committee (closed system) according to private or public sector specialist services
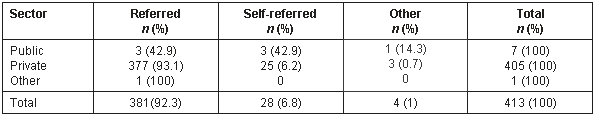
Table 2: Referral type rural health system insurance (semi-closed system) patients according to private or public sector specialist services
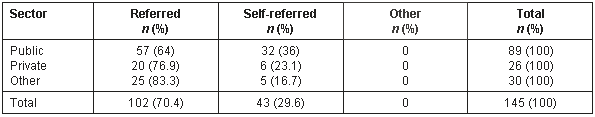
Table 3: Referral type open referral-system patients according to private or public sector specialist services
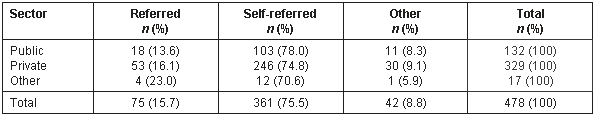
Table 4: Referral source according to insurance structure type
There was a significant association between the structure of the healthcare system and patient self-referral to specialty care (c2 = 504; p <0.0001; Table 4).
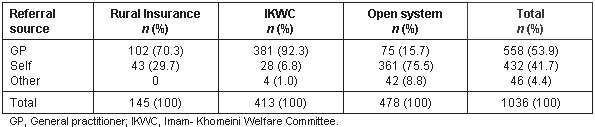
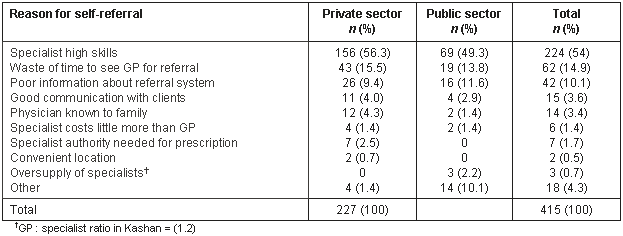
The self-referral rate to the public sector was 60.5%, while to the private sector it was 36.4%. There was a significant association between type of sector and self-referral to specialty care (c2 = 449; p <0.001; Tables 1-3). The main reason patients gave for bypassing GPs and self-referring to specialists were (Table 5): the specialist's high degree of skill in the specific area of the health problem (54%); that it was a waste of time to see the GP for a referral (14.9%); and that the patient's information about the referral system was poor (10.5%).
Table 5: Private and public sector patients' reasons for self-referral according to private or public sector specialist services
There were also differences related to level of education and type of employment (Tables 6,7). For example, self-referral rate in illiterates was 23.1%, but in those who completed high school it was 70.8% (Table 6). This difference was statistically significant (c2 = 103.1; p<0.001).
Table 6: Referral type of patient according to subject's literacy
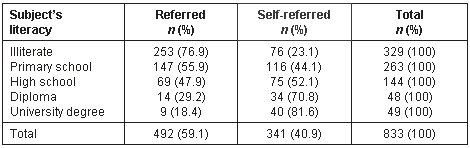
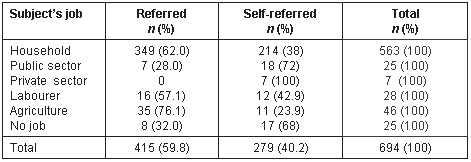
Table 7: Referral type of patient according to subject's job
Discussion
The marked reduction of patients from the IKWC structure (closed-loop referral system) attending hospital outpatients' clinics and specialists' private offices compared with patients from the other two levels of the insurance system (Tables 2,3) suggests that the load on specialist services could be reduced. As a result, more of the specialists' time could be devoted to patients who need specialist care; consequently, standards of care may rise. These findings are similar to other studies1,6,7 but different from one other2.
A closed-loop referral system that denies payment for self-referred patients, and reimburses patients at lower rate than a referred service is an important method of restricting self-referral. This finding of the present study is consistent with a US study7 that compared and contrasted the mix of services provided for consumers enrolled in alternative types of managed-care plans. The study documented patterns of generalist and specialist utilization in various practice settings, with a special emphasis on the point-of-service (POS) model7, which allows members to seek specialty services for a fee without first consulting with their primary-care physician or plan gatekeeper. The majority of patients enrolled in POS plans did not use their self-referral option. Having the option to self-refer is enough for most POS plan enrollees; 93% to 96% of enrollees did not exercise their POS option to obtain specialty care via self-referral during a 1-year interval. The potential downside of uncoordinated, self-referred service use in POS health plans is limited and counterbalanced by higher patient satisfaction with specialist services7. However, the few patients who did self-refer reported being more satisfied with their specialist than did patients who were referred to a specialist by their physician. The US study cited perceived barriers to specialist care as one of the greatest sources of consumer dissatisfaction with health maintenance organizations (HMO). Simply having the option to bypass the gatekeepers of managed care seemed to be enough for most people in POS health plans7. As POS plans gain popularity in Iran, these issues will become more important.
In the present study, the three most often given reasons for patients by-passing GPs and self-referring to specialists (specialist's high degree of skill; waste of time seeing the GP for a referral; and poor information about the referral system) are similar to those given by patients in other studies8-14 but differ from two other studies15,16.
The differences in referral related to level of education and employment are comparable with the results of another US study17. Other known variables predicting preference for the gatekeeper model are: living on the urban periphery; sickness-fund membership; low level of education; being male; fair or poor health status; having a permanent family physician; and being satisfied with the professional level of the family physician17. In some US studies, a significant correlation was found between practising self-referral and preference for self-referral13,16-20.
In the present study, self-referral to the public sector was greater than to the private sector. Such a difference may be caused by inflexible rules, low charges in the public sector, and people's opinion of the public sector as a philanthropic organization.
Despite the disadvantages of living in a rural area, the health indicators, morbidity and mortality of the rural population are comparable with the urban population of Iran. This may be, in part, due to the health and referral systems in rural areas, including the health monitoring of the IKWC and RHSI. In 2000, WHO approved the organisation of the Iranian health system as a model for other communities21.
Limitations
The present study was limited by failing to consider: that specialists attitudes weakened the referral system; variation in the distribution of health centres; place and time of interview session; subjects socio-cultural and economic factors effecting referral patterns; financial issues such as costs or payment both for care givers and patients; subjects' geographic closeness and access to specialists and health centres; and differences in health outcomes or the processes of care among the three groups. Although it is notable that the present study failed to investigate patient outcomes, the data collected will be useful for future investigations of this important domain.
Conclusion
Recommendations
The authors recommend that the referral system in all primary healthcare settings ensures equity of access to the secondary and tertiary healthcare network by all members of the community, including the socially vulnerable. This is particularly important in rural areas. In Iran, raising public awareness of the referral system and the relevance of the GP as the source of referral is recommended in order to gain public cooperation and achieve effective and efficient handling of referral tasks.
In addition, clarifying private- and public-sector role definitions and relationships, and continuous control and monitoring of the quality of care are recommended in order to increase consumer satisfaction and orderly access to the healthcare system.
In conclusion, the findings of this study demonstrate the high degree of difference in the rates of referral by GP and self-referral according to the healthcare delivery system structure (insurance type and sector). Despite the limitations of the study, the findings may be regarded as preliminary to further research into this area of health-system design. Future studies may assist in redesigning healthcare systems to make them more equitable and efficient.
Acknowledgement
This study was supported by an Iranian Ministry of Health research grant.
References
1. Starfield B. Primary care: concept, evaluation and policy. New York: Oxford University Press, 1998; 213-241.
2. Holmes C. Toward the measurement of primary care. Health and society 1978; 56: 231-252.
3. Tawfik AM, Khoja AM, Al Shehri A, Aziz F, Khwaja MS. Patterns of referral from health centers to hospitals in Riyadh region. Eastern Mediterranean Journal 1997; 3: 236-243.
4. WHO. The hospital in rural and urban districts. Report of a WHO study group on the functions of the hospitals at the first referral level. Geneva: World Health Organisation, 1992; 11-18.
5. Rohrer JE. Planning for a community oriented health system. New York: American Public Health Association, 1996; pp: 21-37.
6. Hurley RE, Freud DA, Gage BJ. Gatekeeper effects on patterns of physician use. Journal of Family Practice 1991; 32: 167-174.
7. Braun BL, Fowles JB, Forrest CB, Kind EA, Foles SS, Weiner GP. Which enrollees bypass their gatekeepers in a point-of-service plan? Medical Care 2003; 41: 836-841.
8. Ronald MO, Porter RW. Improving care: a study of orthopaedic outpatient referrals. BMJ 1991; 302: 1124-1128.
9. Imanaka Y. Determinates of patient satisfaction and intention to continue services utilization: analysis of survey of outpatients at general hospital. Nippon Koshu Eisei Kasshi 1993; 40: 624-635.
10. Bradley EJ, Clark BS. Patient characteristics and consumer satisfaction on inpatient child psychiatric unit. Canada Journal of Psychiatry 1993; 38: 175-180.
11. Clancy CM, Franks P. Utilization of speciality and primary care: The impact of HMO insurance and patients related factors. Journal of Family Practice 1997; 45: 500-508.
12. Fredericson M. Medical acupuncture at a complementary medicine clinic: a 2-year retrospective study. Medical Acupuncture Online Journal 1997; 4: 1-6.
13. Trude S, Stoddard JJ. Primary Care Physicians and Mental Health Services. Journal of General Internal Medicine 2003; 18: 442.
14. McCarthy E. Open access newest managed care trend. American City Business Journals. (Online) 28 August 1998. Available: http://www.bizjournals.com/search.html (Accessed 12 May 2004).
15. Vinker S, Nakar S, Alon Z, Abu-Amar H, Sadovsky G, Hyam E. [Urgent, unscheduled self-referral by ambulatory patients.] Harefuah 1998; 135: 92-95. [In Hebrew]
16. Grumbach K, Selby JV, Damberg C. Resolving the gatekeeper conundrum: what patient value in primary care and referrals to specialist. JAMA 1999; 28: 261-266.
17. Gross R, Tabenkin H, Brammli-Greenberg S. Who needs a gatekeeper? Patients' views of the role of the primary care physician. Family Practice 2000; 17: 222-229.
18. Forrest CB, Weiner JP, Fowles J et al. Self-Referral in Point-of-Service Health Plans. JAMA 2001; 285: 2223-2231.
19. Forrest CB. Primary care in the United States. Primary care gatekeeping and referrals: effective filter or failed experiment? BMJ 2003; 326: 692-695.
20. Rosenblatt RA, Hart GL, Baldwin L, Chan L, Schneeweiss R. The generalist role of specialty physicians: is there a hidden system of primary care? JAMA 1998; 279: 1364-1370.
21. WHO. The world health report. (Online) 2004. Available: http://www.who.int/whr/2003/chapter7/en/index2.html (Accessed 3 August 2004).
