Human resources are the most critical component of any health system. South Africa faces serious challenges with regards to human resources for health including chronic shortages of key categories of healthcare workers, skewed distribution between public and private health sectors and geographical maldistribution1. The overwhelming majority (±70%) of medical practitioners are based in the private sector in South Africa2. It has been estimated that private sector outpatients services are utilised by at most approximately 32% of South Africans3. In the public sector, the ratio of general practitioners to uninsured population is alarmingly low at approximately 1:42004,5. A vacancy rate of 42.5% for public sector health professional posts was reported in 20102.
Within the public sector, there is further maldistribution between urban and rural areas4. Urban provinces tend to have much higher health professional-to-population ratios than rural provinces. For example, in the urban province of Gauteng, the number of health professionals in the private and public sectors per 10 000 population in 2010 was 69.2; this number was 44.8 for the Eastern Cape, a largely rural province6,7. It is estimated that there is on average one general practitioner for 7692 people in rural areas in South Africa4. Limpopo Province, which is mostly rural, had approximately two-thirds of their professional nurse posts and more than 80% of their medical practitioner posts unfilled in 20102.
In response to the country's human resources for health crisis, the National Department of Health decided to introduce the clinical associate program as one of the measures to increase the number of healthcare workers in underserved areas8. Although their placement in South Africa is not limited to rural areas, this cadre does form an important part of South Africa's Department of Health's strategy to increase access to healthcare practitioners in rural areas7. Clinical associates are university-trained mid-level medical workers8. Similar cadres of health workers exist throughout the world although they are known by different names: physician assistants in the USA, medical assistants in Tanzania and clinical officers in Malawi8,9. Several countries in Africa and Asia have relied on this category of health worker to provide much-needed surgical and medical services at district hospitals and community health facilities9.
In South Africa, clinical associates are designated to work at the level of the district hospital7,8. It is required that a clinical associate work under supervision provided by a medical practitioner8. According to South Africa's Department of Health7, it is envisaged that clinical associates will work within surgical, medical and maternity units as well as outpatients and emergency departments7. Their work involves assessment and management of patients with acute and chronic conditions8. Clinical associates will also be involved with basic surgical procedures such as incision and drainage7.
To register with the Health Professions Council of South Africa as a clinical associate, the individual must first complete a three-year Bachelor of Clinical Medical Practice (BCMP) degree8. Walter Sisulu University in the rural Eastern Cape was the first South African university to introduce the BCMP degree in 2008 followed by the two urban Gauteng-based universities (University of Pretoria (UP) and University of Witwatersrand) in 20098. The BCMP degree at UP is coordinated by the Department of Family Medicine and uses a practice-based authentic learning approach. During their 3 years of training, students gain practical experience in history-taking, physical examination, patient management and clinical procedures at various hospitals, in addition to academic work at the university8. The facilities currently being used by UP for training include urban (Gauteng Province and military) and rural (Mpumulanga Province) hospitals.
If clinical associates are to be one of the solutions to rural shortage of health professionals, it is important that the recruitment and educational program of BCMP students takes into account the factors that have been found to be associated with rural practice intent. The link between rural origin and health sciences students' intention to practise in a rural area or actual rural practice has been explored in previous studies. A survey amongst final-year medical students at eight South African universities found that students originating from rural areas or small towns were more inclined to work in rural settings than those from cities10. In a qualitative study conducted amongst 15 rural-based healthcare professionals in South Africa, rural origin was identified as an important factor in influencing the decision to practise in a rural area11.
Some studies have examined the relationship between health sciences students' source of funding for their studies and their rural practice intentions. Australian and New Zealand medical students were more likely to have rural practice intentions if their studies were being funded by a scholarship12. In that study, scholarships without bonded arrangements seemed to be a stronger predictor than bursaries with mandatory service12. In research amongst Nepalese medical students, those with Ministry of Education scholarships requiring service in a rural area were significantly more likely to indicate an intention to practise in a rural setting13.
The link between rural exposure during training and rural practice intention and eventual rural practice has been explored. A systematic review by Wilson et al14 found moderate evidence for the influence of clinical attachments in rural settings on medical students' likelihood of considering practice in a rural area14. Wilson et al14 highlight the possibility of selection bias influencing the association, as the rural attachments are generally optional14. Local supervision and support during these attachments also appeared to influence students to consider practice in a rural setting14. In the qualitative study by Couper et al11 in South Africa, the decision to work in a rural area was facilitated by rural exposure during training (eg a rural elective or work during university vacations)11.
In creating this new cadre of health worker in South Africa the assumption by the various stakeholders was that clinical associates would work in district hospitals in South Africa and would to some extent fill the void left by a shortage of medical practitioners in rural areas. There was a need for evidence to support this hypothesis. In addition, the proportion of BCMP students intending to work in urban areas, migrate to other countries and pursue medical degrees has human resource implications. The objectives of the study were, therefore, to determine the practice intentions and practice preferences of BCMP students with regards to geographical location and to determine the future study plans of BCMP students. An additional objective was to determine the factors associated with rural practice intentions directly after graduating as this may be useful in adapting the recruitment strategy and strengthening the educational programs of the three BCMP programs in South Africa in order to increase the output of clinical associates willing to work in rural areas.
This was a cross-sectional study of clinical associate (BCMP) students attending UP in 2011. The study population consisted of first-, second- and third- year students. Only students present on the days the survey was conducted were included in the study. Sampling was not required as there were only 216 BCMP students in total at UP in 2011.
The dependent variable of interest in the study was urban-rural practice intention (intention to practise in either a rural or an urban area) directly after graduating. This categorisation was based on a closed-ended question that required students to select a statement that best described their practice intentions directly after graduating from the BCMP program. The independent variables included age, gender, race, degree year, area where student had lived most of his/her life, area where secondary schooling was completed, self-description of type of area (urban/rural) where student had lived most of his/her life, funding source for studies and rural exposure during training. Rural exposure during training was based on whether the student had rotated to at least one rural district hospital at some point since commencing clinical associate training. Other variables studied included practice intentions 5 years following graduation, urban-rural practice preference (preference to practise in either a rural or an urban area), future study intentions and preferences, and preferred country of practice.
The measurement tool was a self-administered electronic questionnaire. The majority of questions were closed-ended and these were of different types including multiple choice and Likert scale. The survey was conducted in late October and early November 2011. The existing UP computer-based training (CBT) platform developed by the company Umfundi was used to administer the questionnaire. The questionnaire was available in English only as this is the dominant language of instruction. The questionnaire consisted of four sections: sociodemographic characteristics, practice intentions, practice preferences and perceptions of the BCMP program.
Data analysis was then conducted using Stata v12 (Statacorp; http://www.stata.com). The area where the student had lived most of his/her life and the area where secondary schooling was completed were classified as falling either within a district or metropolitan municipality. This approach was adopted due to difficulties in sourcing an official list that classified areas as urban and rural. Proportions were calculated for the majority of variables. Bivariate analysis was conducted with respect to practice intention directly after graduation and various sociodemographic variables. Depending on the expected cell counts, Pearson's χ2 test or Fisher's exact test was used to confirm statistical significance. A logistic regression model was developed for rural practice intention directly after graduating using the independent variables from the bivariate analysis that were significantly associated with it at a 10% significance level in the initial full logistic regression model.
Ethics approval
The overarching study, 'A multidisciplinary investigation of Authentic Learning in the BCMP Curriculum', received ethics approval (56/2011) from UP's Faculty of Health Sciences Research Ethics Committee in March 2011. The questionnaire used in this survey was submitted as an amendment to this overarching study and was approved by the Research Ethics Committee in October 2011.
Response rates
The total number of BCMP students at UP in 2011 was 216. As the survey took place on the days of the students' computer-based examinations, only the 210 who wrote the examinations were included in the study. Of the 210 students, 149 (71.0%) agreed to participate in the study. With respect to the year groups, 58.9% (43/73) of the first-years, 71.1% (64/90) of the second-years and 89.4% (42/47) of third-years present on the days of the survey agreed to participate. Overall 69.0% (149/216) of all students registered for the BCMP degree at UP in 2011 participated in the study. With respect to the year groups, 55.8% (43/77) of all registered first-years, 69.6% (64/92) of all registered second-years and 89.4% (42/47) of all registered third-years participated in the survey.
Sociodemographic characteristics of participants
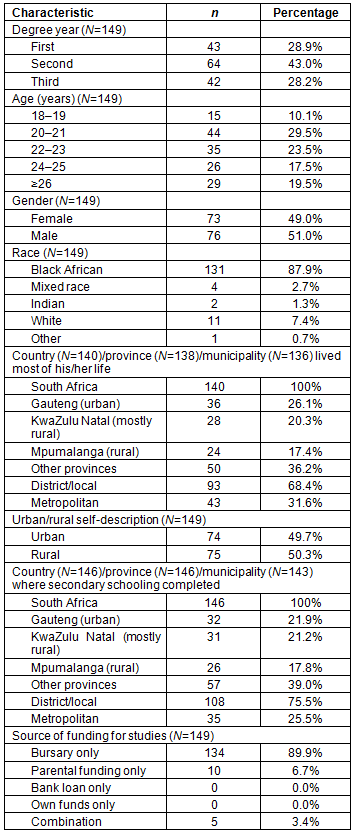
The vast majority of participants (70.5%) were between 20 and 25 years of age. Only 18.1% of participants had entered the BCMP program directly after completing their schooling. There were slightly more male (51.0%) than female (49.0%) participants. The participants were mainly Black African (87.9%). Gauteng (urban), KwaZulu Natal (mostly rural) and Mpumalanga (rural) were most frequently mentioned as the provinces where the participants had spent most of their lives and the provinces where secondary schooling was completed. Most of the participants (68.4%) had lived most of their lives in a district/local municipality as opposed to one of the eight metropolitan municipalities. Just over half (50.3%) of the participants described the area where they had lived most of their lives as rural. The main source of funding for the BCMP studies were bursaries, with 89.9% of students being funded solely by a bursary. The key sociodemographic characteristics of the participants are displayed in Table 1.
Table 1: Sociodemographic characteristics of participants
Practice intentions directly after graduating
Amongst the 146 participants that provided a response regarding their practice intentions directly after graduating, the majority (59.6%, n=87) intended to practise in a rural area in South Africa (Fig1). Substantially fewer (28.1%, n=41) intended to practise in an urban area directly following graduation. Just 11.0% of students did not intend to practise as clinical associates but planned on remaining in South Africa. Two students did not intend to complete the degree. None of the students intended to emigrate directly after qualifying. Amongst the 128 students who intended to practise as clinical associates directly after graduating, 68.0% (n=87) intended to work in a rural area and 32.0% (n=41) intended to work in an urban area. The reasons for selection of the place they intended to practise were bursary obligations (46.9%), family reasons (30.8%) and other reasons (22.3%).
Bivariate analysis: Table 2 displays the bivariate analysis of rural practice intentions of students directly after graduating, and sociodemographic and other characteristics. Only the students who intended to practise as clinical associates in South Africa directly after graduating were included in the analysis. There were no significant differences between male and female students (p=0.119) and younger and older students (p=0.623) with regards to their rural practice intention. Amongst third-year students, 92.1% had a rural practice intention compared to 56.1% of the second-years and 60.6% of the first-years. Black African students were more likely than students of other race groups to have an intention to practise in a rural area as were students funded by bursary only compared to those that received funding from other sources. Students who had lived most of their lives in a district municipality were more likely than those that had lived most of their lives in a metropolitan municipality to have an intention to practise in a rural area (p=0.008). Students who had self-described the area they had lived most of their lives as rural were more likely to have a rural practice intention than those who described it as urban (p<0.001). Those students that had had at least some rural district hospital exposure during training were more likely to have a rural practice intention than those that had had no exposure (p<0.001).
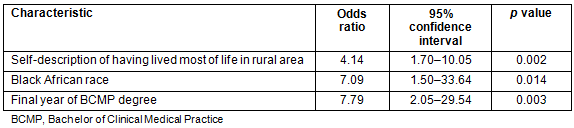
Multivariate analysis: The variables with p<0.1 on bivariate analysis were included in the initial full logistic regression model. Some categories were combined prior to inclusion in the model. With regards to year of study, first- and second-year were combined. With regards to race, the mixed race, Indian (South Africans of Indian descent), white and 'other' groups were combined to form a single category due to their small numbers. Similarly all sources of funding other than bursary only were combined. The final model following elimination consisted of the three variables shown in Table 3. Self-description of having lived most of one's life in a rural area (p=0.002), Black African race (p=0.014), and being in the final year of the BCMP program (p=0.003) significantly increased the likelihood of rural practice intention.
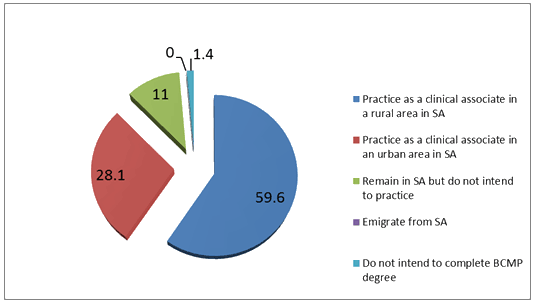
Figure 1: Practice intentions directly after graduating (%) (n=146).
Table 2: Rural practice intention of students intending to practise as clinical associates
in South Africa directly after graduating and student characteristics (bivariate analysis)
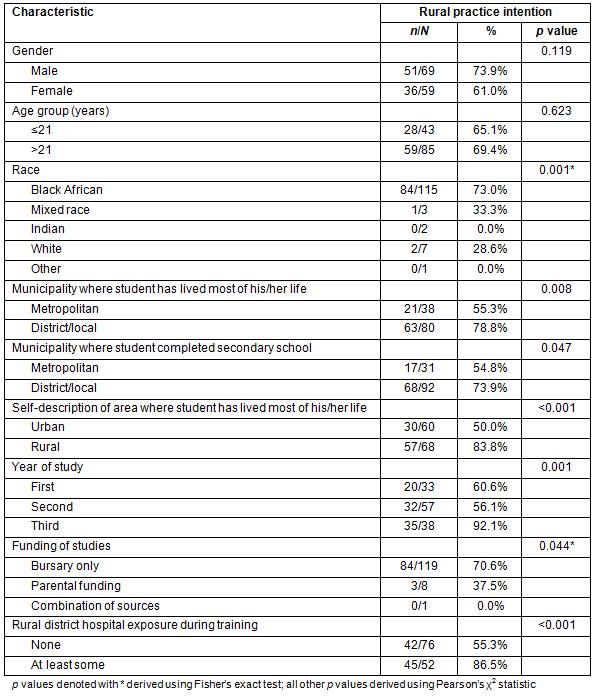
Table 3: Factors associated with rural practice intention of students intending
to practise in South Africa directly after graduating (multivariate analysis)
Practice intentions 5 years following graduation
Of the 121 students who indicated their practice intentions 5 years after graduating, 63 students intended to practise as a clinical associate in a rural area in South Africa, 33 students intended to practise as a clinical associate in an urban area in South Africa, 24 students intended to remain in South Africa but not practise as a clinical associate and one student intended to emigrate from South Africa.
Practice preferences
The majority of students (75%, n=111) stated a preference for working in South Africa even if their qualification was internationally recognised. A quarter of students (25%, n=37) indicated they would prefer to work abroad if the BCMP degree was recognised overseas. Their preferred locations included the UK (n=8), USA (n=8), Canada (n=4), Australia (n=3), New Zealand (n=3), France (n=3), Cuba (n=2), Lesotho (n=1) and Germany (n=1). If given complete freedom of choice (eg no bursary or family obligations) on where they could practise as a clinical associate, 53.4% (n=79) indicated a preference to practise in a rural area and 46.6% (n=69) indicated an urban preference.
Future study intentions and preferences
At some point following completion of the BCMP degree, 93.9% (n=139) of students intended to undertake either further full-time (50.0%) or part-time (43.9%) studies. In response to the open-ended question regarding the area of study they intend to pursue, 44.4% (n=56) indicated a medical degree and 20.6% (n=26) indicated a postgraduate BCMP degree. A further 9.5% (n=12) indicated a clinical specialty but it was not clear if this was specialisation as a clinical associate or a medical practitioner. The remaining students who completed the question specified other fields (20.6%, n=26) or were not sure of their future field of study (4.7%, n=6).
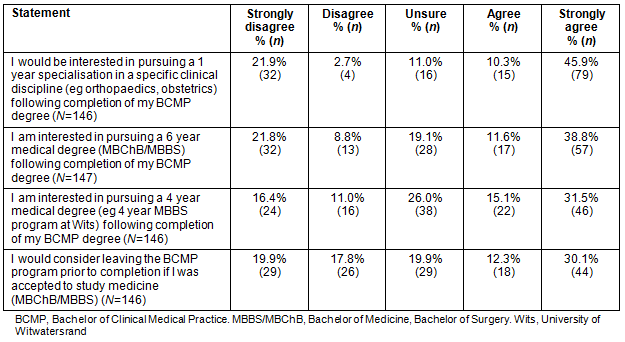
The students' interest in pursuing a medical degree and BCMP specialisation were elicited using Likert-scale questions. The results are displayed in Table 4. More than half the students appeared interested in a BCMP specialisation. Slightly more students were interested in pursuing a 6-year rather than a 4-year medical degree. A substantial number of students would consider leaving the BCMP program if they were accepted to study medicine. Of the 117 students who responded to the question regarding their preferred clinical discipline if a 1-year post-BCMP specialisation was offered, 20.1% (n=20) indicated orthopaedics, 16.2% (n=19) preferred obstetrics and gynaecology and 13.7% (n=16) indicated casualty or trauma. Paediatrics (n=14), anaesthetics (n=10), cardiology (n=10) and surgery (n=9) were also popular specialties amongst the participants.
Table 4: Participants' interest in pursuing further clinical associate and medical training
Discussion
Substantially more students intended to practise as clinical associates in rural areas (n=87) than urban areas (n=41) following graduation. At 5-years post-qualification, when there is unlikely to be any mandatory bursary obligations still in place, there is still a substantial difference in the numbers who intend to practise in a rural area (n=63) compared to an urban area(n=33). When asked about their practice preferences if they had complete freedom of choice, the gap between urban and rural intentions does narrow but the majority of students still favoured rural areas. As these BCMP students are among the first graduating in the country, there is no historical South African BCMP student data available for comparison purposes.
The findings of this study are in stark contrast to that of Burch et al15 amongst final-year medical students from nine African medical schools (including four South African medical schools), which found that only 4.8% of medical students were interested in practice in rural settings beyond mandatory training and bursary obligations15. The majority of participants (57%) in that study were South African, suggesting major differences in rural practice interest between South African BCMP students and South African medical students15. This comparison is important given that a key reason that the clinical associate program was developed in South Africa was to respond to the inequitable distribution of medical practitioners.
The findings of this study indicate that clinical associate students from a rural background are more likely than their urban counterparts to have rural practice intentions. Students who indicated having lived most of their lives in a rural area were significantly more likely to indicate an intention to practise in a rural area following graduation. These findings are similar to those of Jones et al12 amongst Australian and New Zealand medical students12. In that study, students who did not self-identify as being a rural person were significantly less likely to have rural practice intentions12.
Black African race was found to be a significantly associated with rural practice intentions. Due to the fact that a very small number of participants in the study were not Black African, an arbitrary category consisting of the white, mixed race, Indian (South Africans of Indian descent) and 'other' groups was created for multivariate analysis. In the light of this and the limitations of logistic regression with respect to the small numbers of participants that were not Black African, this result should be interpreted with caution. The link between the ethnicity of health professionals and their location of practice has been examined in previous studies but Wilson et al14, in their review, could only find one study in which ethnicity appeared to play a role in the location of practice14. That study found that Hispanic physicians in Colorado, USA, established practices in settings where the proportion of the impoverished population and percentage of Hispanic population was greater in comparison to areas where white physicians located their practices14,16.
The year of BCMP study was also significantly associated with rural practice intentions in this study. Those students in their final year of study were more likely to have rural practice intentions when compared to the first- and second-year students combined. The possibility that this was due to them having more rural exposure was unlikely as rural district hospital exposure was included in the multivariate analysis and found not to be significantly associated with rural practice intentions. An explanation that has been suggested by their supervisors is that as the first group to qualify as clinical associates from UP, the final-year students see themselves as ground breakers and feel they have a responsibility to make the program successful by working where they are most needed.
Amongst the participants in the UP study, only one BCMP student intended to emigrate from South Africa within 5 years of graduating. This contrasts with data available for South African medical students. Amongst the South African medical students in the study by Burch et al15, 17.6% intended to practise outside Africa15. Van Wyk et al17 found that 18.5% of the 2005 cohort of University of KwaZulu Natal final-year medical students intended to practise outside South Africa17. In a study at South Africa's eight medical schools, 55% of the students that participated intended to work overseas10. Of these students, 73% planned to work overseas for up to 2 years, 20% for more than 2 years, and 7% planned on relocating overseas permanently10. The probable reason for 99.3% of participants in the UP study not intending to emigrate is that the BCMP degree is not internationally recognised. If it were recognised, 25.0% of participants would prefer working abroad. The choice of the UK, USA and Canada as the preferred destinations is not surprising and is consistent with research among African medical students15. These choices are probably due to economic, cultural and language considerations. It is also possible that the USA may be attractive due to its strong physician assistant program.
The vast majority of students intended undertaking further studies following completion of the degree. It is clear from both the open-ended question and the Likert-scale questions that a substantial number of students wish to pursue a medical degree. It is likely that many of the students entered the BCMP program when they were not accepted into a medical program and see BCMP as a route to an eventual medical degree. Surprisingly, more students appeared interested in pursuing a 6-year medical degree than a 4-year graduate medical degree. The fact that in South Africa the 4-year graduate degree is only offered at the University of Witwatersrand and some students may not have been aware of it could explain this finding. The potential loss of BCMP students and qualified clinical associates to medical programs has human resources implications. For those who complete their BCMP degree and then pursue a 6-year medical degree, this would effectively mean 9 years of training that is heavily subsidised by government before producing a medical practitioner.
A large number of students appeared interested in pursuing a specialisation in a specific clinical discipline following completion of their BCMP degrees. This option is not currently available in South Africa but is being considered. Respondents indicated a wide range of clinical discipline preferences, with orthopaedics being the most popular. Specialisation could create a career path and probably ensure greater retention as well as allowing for a greater possibility of task-sharing at the district level.
This study had some limitations. There was a low response rate amongst first-year students. Students' responses were based on their perceptions of what constitutes an urban or rural area as there is no clear-cut definition of urban or rural. To try to standardise the results, the areas where students spent most of their lives and completed their schooling were classified as either a metropolitan municipality or district/local municipality. As district municipalities may consist of some urban areas, using this classification is not an ideal proxy for urban and rural. Performing logistic regression on a relatively small number of subjects, as was the case in this study, is not ideal. The results of the multivariate analysis should be interpreted with this in mind and should be viewed as exploratory. As the profile of BCMP students at Walter Sisulu University and University of Witwatersrand may differ from those at UP, it is not possible to generalise these findings to all South African BCMP students.
This cadre of health worker is new in South Africa, and as such South African universities have a challenge of ensuring that what was intended (ie practice in rural and underserved areas) translates into practice. The findings of the study support the hypothesis that the clinical associate program could play a significant role in addressing the critical shortage of health professionals in rural settings in South Africa. The presence of qualified clinical associates at rural district hospitals will increase the number of clinicians and strengthen the clinical team, which should lead to improved patient care and reduce the load on overburdened rural medical practitioners. Given the dire need for clinicians in rural areas, consideration should be given to increasing clinical associate training and expanding to other universities. The results of the study also suggest that clinical associate training programs should continue to actively recruit students from rural areas.
This study has captured the practice intentions of the first cohort on the brink of entering this new profession and therefore provides a baseline for future studies - a luxury that few other health professions have had. This first cohort is unique as applicants to this program had no framework of reference. This early exploratory article published from South Africa should be followed up with a longitudinal review of UP BCMP graduates and their actual practice choices.
Acknowledgements
Thanks to Ms Erika de Bruyn, Department of Education Innovation, Ms Marisa Ishmael, Department of Education Innovation and BCMP students at the University of Pretoria.
References
1. Wadee H, Khan F. Human resources for health. In: S Harrison, R Bhana, A Ntuli, eds. South African health review 2007. (Online) 2007; 141-150. Available: http://www.hst.org.za/publications/south-african-health-review-2007 (Accessed 8 July 2012).
2. Lloyd B, Sanders D, Lehmann U. Human resource requirements for national health insurance. In: A Padarath A, S Fonn, eds. South African Health Review 2010. (Online) 2010; 171-178. Available: http://www.hst.org.za/publications/south-african-health-review-2010 (Accessed 8 July 2012).
3. McIntyre D. Private sector involvement in funding and providing health services in South Africa: implications for equity and access to health care. EQUINET Discussion Paper Series 84. (Online) 2010. Available: http://www.equinetafrica.org/bibl/docs/DIS84privfin%20mcintyre.pdf (Accessed 14 May 2013).
4. Cooke R, Couper I, Versteeg M. Human resources for rural health. In: A Padarath, R English, eds. South African Health Review 2011. (Online) 2011; 107-118. Available: http://www.hst.org.za/publications/south-african-health-review-2011 (Accessed 8 July 2012).
5. Republic of South Africa Department of Health. Delivery agreement for outcome 2: a long and healthy life for all South Africans. (Online) 2010. Available: http://www.info.gov.za/view/DownloadFileAction?id=135747 (Accessed 10 May 2013).
6. Matsoso MP, Strachan B. Human resources for health for South Africa: HRH Strategy for the Health Sector 2012/13-2016/17. In: A Padarath, R English, eds. South African Health Review 2011. (Online) 2011; 49-58. Available: http://www.hst.org.za/publications/south-african-health-review-2011 (Accessed 8 July 2012).
7. Republic of South Africa Department of Health. Human resources for health South Africa: HRH strategy for the health sector 2012/13 - 2016/17. (Online) 2011. Available: http://www.gov.za/documents/download.php?f=152486 (Accessed 8 October 2012).
8. American International Health Alliance. Clinical associates: a new kind of health professional in South Africa. (Online) 2011. Available: http://www.clinicalassociate.co.za/images/clina_booklet_final.pdf (Accessed 11 June 2012).
9. Lehmann U. Mid-level health workers: the state of the evidence on programmes, activities, costs and impact on health outcomes - A literature review. (Online) 2008. Available: http://www.who.int/workforcealliance/knowledge/resources/mlp_review/en/index.html (Accessed 11 June 2012).
10. de Vries E, Irlam J, Couper I, Kornik S. Career plans of final-year medical students in South Africa. South African Medical Journal 2010; 100(4): 227-228.
11. Couper ID, Hugo JFM, Conradie H, Mfenyana K. Influences on the choice of health professionals to practise in rural areas. South African Medical Journal 2007; 97(11): 1082-1086.
12. Jones M, Humphreys J, Prideaux D. Predicting medical students' intentions to take up rural practice after graduation. Medical Education 2009; 43(10): 1001-1009.
13. Huntington I, Shrestha S, Reich NG, Hagopian A. Career intentions of medical students in the setting of Nepal's rapidly expanding private medical education system. Health Policy and Planning 2011; 27(5): 417-428.
14. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health 9(2): 1060. (Online) 2009. Available: www.rrh.org.au (Accessed 26 January 2012).
15. Burch VC, McKinley D, van Wyk J, Kiguli-Walube S, Cameron D, Cilliers FJ, et al. Career intentions of medical students trained in six sub-Saharan African countries. Education for Health (Abingdon) 2011; 24(3): 614.
16. Fryer GE Jr, Green LA, Vojir CP, Krugman RD, Miyoshi TJ, Stine C, et al. Hispanic versus white, non-Hispanic physician medical practices in Colorado. Journal of Health Care for the Poor and Underserved 2001; 12(3): 342-351.
17. van Wyk JM, Naidoo SS, Esterhuizen TM. Will graduating medical students prefer to practise in rural communities? South African Journal of Family Practice 2010; 52(2): 149-153.

