Introduction
Rural Australians are not only less healthy than urban Australians1, but they also have more restricted access to healthcare services, due to a combination of a limited range and insufficient numbers of health professionals2. Most medical services, including more complex birthing, anaesthetic and surgical procedures, are provided by rural GPs with additional procedural skills training.
However, the number of rural generalist doctors providing these important services is falling, perhaps for several reasons. First, procedural training is not easy to arrange, although rural procedural training is becoming more organised through the Regional Training Providers contracted to provide training to the standards of the Royal Australian College of General Practitioners (RACGP) and the Australian College of Rural and Remote Medicine (ACRRM)3,4. Second, smaller rural hospitals are either closing or changing their service mix to exclude acute procedural care, further jeopardizing he viability of rural economies5-7. Third, the high cost of professional indemnity cover is a strong disincentive. Finally, there are some concerns that increased rates of patient transfer by road and air to regional hospitals may contribute to a deskilling of rural hospital staff.
This trend is worrying, because the alternatives to local rural care also face hurdles. Sending rural people to urban specialist medical practitioners and facilities may not be appropriate, for three reasons: (i) rural people are known to often choose either delayed or no treatment if that treatment requires substantial absence from home8; (ii) urban facilities may not have the capacity to absorb the additional workload; and (iii) the rising cost of emergency transport may not be sustainable. Another alternative - training more generalist specialists in larger rural communities - faces similar recruitment and retention problems, and the training is hard to find in this era of increasing sub-specialisation.
One important issue in the discussion of the quality of rural procedural care is that most quality indicators are based on analysis of large numbers of cases with some selection control. These conditions are not possible in rural primary care practice, where the procedures are performed by small teams of local health professionals on an occasional basis. Most specialty colleges mandate a minimum number of procedures for maintenance of competence and almost all rural generalists would fail to meet those minimum requirements. This raises the question, 'Is procedural generalism compatible with high quality?' A MEDLINE search using the key words 'quality of health', 'rural health', 'procedures', 'anaesthesia', 'surgery', 'obstetrics', and 'quality indicators' failed to identify any strong evidence that the quality of rural procedural care in developed nations is poor. Indeed, there was some evidence supporting the safety of particular rural procedures9-11. This article reports a study that investigated the quality of procedural care in anaesthetics, surgery and obstetrics by rural generalists in rural hospitals.
Methods
The study consisted of a multiple-perspective analysis of a series of real clinical cases collected prospectively over a 6 month period in rural hospitals. Rural procedural generalist medical practitioners were recruited from all States through ACRRM, with the following inclusion criteria: had completed appropriate postgraduate procedural training; and currently practising in RRMA 3-7 communities. Each was asked to enrol five consecutive consenting patients undergoing a medical procedure. It was intended to include both urgent and elective cases. A member of the research team (RE) then contacted each consenting patient to explain the project and to obtain formal consent. Data were collected by questionnaire and telephone interview from the participating rural doctor, another health professional at the rural hospital, the patient (before and after), and a member of the patient's family, providing demographic data, details on the procedure, and commentary on why the procedure was performed in the rural hospital, which in combination produced a detailed case study for each patient event. Sample questions from the doctor questionnaire and the patient interviews (pre- and post-procedure) are included (Appendix I). Steps in the review process were, as follows:
- All material was de-identified.
- All cases were reviewed by a rural generalist with similar procedural experience and an urban-based specialist in the relevant procedural specialty.
- A sampling strategy was devised to identify a representative 'sample' of all cases. The strategy involved two distinct components: (i) grouping cases into those that had, and had not, received written comments of any type from a reviewer; and (ii) random selection of nearly equal samples from each group identified in (i).
- Clinical information for a total of 30 cases was reviewed by a medical administrator, while transcripts of interviews with patients and family members for 20 cases were reviewed by a rural consumer.
Thus, although all cases were reviewed by at least two reviewer groups, each case was not reviewed by all four reviewer groups.
The medical administrator and rural consumer reviewed only 30 and 20 cases, respectively, because we made a judgment that the variation between cases was very small with respect to the nature of their reviews. Further, the workload per case of the rural consumer reviewer was substantially higher than that of other reviewers, because entire transcripts of all interviewees related to each case had to be read, whereas other reviewers reviewed only the medical information.
Detailed concurrent coding was conducted during in-depth reading of interview transcripts by one of the researchers, followed by independent checking of a sample by another of the researchers. Atlas.ti software 2004 (Thomas Muhr, ATLAS.ti Software Development; Berlin, Germany) was further used to identify central themes from the detailed coding. Four such themes emerged: 'not just a number'; 'familiarity'; 'continuity'; and 'convenience'. Ethics approval was granted by the James Cook University Human Research Ethics Committee
Results
Recruitment of doctors and patients was more difficult than expected, particularly for surgical procedures. Doctors from States with substantial rural procedural medical practice comprised a majority of responders. Although 49 doctors agreed to participate, only 24 successfully recruited patients. Those who withdrew cited time management problems, particularly for more urgent procedures, when there was little time to obtain formal consent, distribute questionnaires and arrange telephone interviews. Hence, the majority of cases included in the analysis were elective procedures or, in the case of obstetric patients, at least known of in advance. Of the 24 doctors who did continue, all but one were male, with an average age of 49.4 (±6.5) years and range of 34-59 years. These doctors reported having spent a mean of 18.1 (±7.4) years in rural practice (responses ranged from 5-30 years). Those doctors not contributing cases were very similar demographically (age, gender, experience and distribution).
Complete data sets were obtained for only 17 cases, although in most cases only one data component was missing. The most common gaps were information from family members (only 36 were nominated, usually spouses), pre-procedure patient interviews (due to urgency), and other health professionals (some hospitals would not allow this). A total of 91 patient cases were available for the analysis.
Tables 1 and 2 summarise the location and discipline of participating doctors and the numbers of procedures by discipline. Most anaesthetic procedures were general anaesthesia. A majority of obstetric cases were normal vaginal deliveries, and the rest were assisted deliveries, including nine Caesarean sections. All 11 surgical cases were relatively minor procedures (mostly simple excisions and endoscopies). The patients were mostly female (78%), had a mean age of 39 years, and were in long-term relationships (59%).
Table 1: Location and procedural disciplines of participant doctors
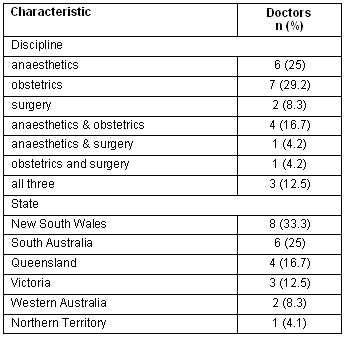
Table 2: Medical discipline of clinical cases

Case reviews
The quality ratings of case reviews by the rural consumer representative, medical administrator, peer rural doctors and urban specialists are summarised (Table 3). Reviewers were asked to rate the quality of care for each case from 1 to 5 (where 1 = excellent; 5 = very poor). The difference in these results achieved statistical significance (Pearson c2 value 89, df = 8, p <0.05), with the regional specialists rating the quality least highly, although this was due to greater use of the 'good' category rather than higher use of 'poor' categories.
Table 3: Comparison of average ratings by all reviewer categories
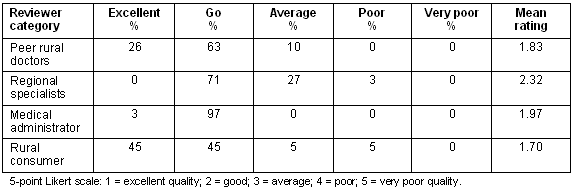
The rural consumer representative rated all 20 reviewed cases as appropriate to the rural context and expectations of rural people and only one case as containing processes not appropriate to the context and expectations of rural people.
The medical administrator reviewer rated 97% (29) of the cases as 'good' quality care, and 3% (1) 'excellent' (average = 1.97), and stated that all cases would expect to receive similar treatment in an urban facility. All but one case was regarded as being relatively cost-effective, because the patient was admitted for a colonoscopy:
This would normally not require the use of theatre in larger centre . . . ??Increased unit cost of procedure due to theatre overload.
Discipline-matched rural procedural doctors made the most comments, many critical, but rated the quality of care highly: 26% (19) cases were rated as 'excellent' quality care, 62% (46) 'good' and 10% (7) 'average' (average = 1.83). Further, peer reviewers judged that a total of 69% (51) cases appeared to have received high quality technical care. Most negative responses were due to inadequate information provided to make appropriate judgement. In approximately 50% of cases, reviewers felt that some additional information may have been helpful in making a judgement about quality. This included partograms for deliveries, pre-medication details, post-procedure details/plan, and detail of induction and Apgar scores.
IV fluids have been shown to improve recovery in all . . . patients, and more so if they have had bowel preparation.
No mention of foetal monitoring with CTG. I would have thought this appropriate in an augmented multipara especially with epidural. High skill level demonstrated by rotational vacuum.
Appears to have been delayed response to ongoing . . . than normal vaginal bleeding postpartum.
In 25 instances, peer doctors indicated that they would possibly have managed aspects of the procedure differently, but the differences were relatively minor and related to medication and technique differences, such as using multi-modal post-operative analgesia, and trying alternative medications to avoid post-operative nausea and vomiting.
The regional specialists rated 71% (56) of cases as 'good' quality care, 27% (21) 'average', and 3% (2) 'poor' (average = 2.32). Further, in 88% (71) of cases the specialists agreed that the care was appropriate. Specialists described in 13 cases how the patient's care may have differed in a larger, urban facility. The anaesthetic reviewer considered mostly technique-related differences, including the use of trained anaesthetic assistants. The obstetric reviewer would have discouraged vaginal birth after Caesarean section in a particular patient, more actively managed the 3rd stage of one labour, and attempted to decrease blood loss in a Caesarean section. In 33% (26) of cases specialists indicated that their judgments would have been helped by additional information, such as recovery records, patient age, and further pre-, peri- and post-operative details.
The views of patients and family members
Rural hospitals were regarded by patients and their families as friendly, personal and inviting environments that compared favourably with what they had either heard about, or previously experienced, in urban hospitals. They perceived less pressure for early discharge and found relative comfort in remaining close to family and friends. The qualitative analysis produced four themes: 'not just a number'; 'familiarity': 'continuity of care'; and 'convenience'.
Not just a number:
The thing that I find around here that I really appreciate about the whole service is the personalised attention that you get and they treat you like a person and not a number or somebody on a list or whatever. Generally, you know people from around the community that are involved in the health services and things too. It's probably the person-to-person contact. They're making you feel like a person, not a procedure. [Patient]
Familiarity:
Yes, like I said I feel comfortable in [locality 1] because it is a very nice close knit family and you feel really relaxed. . . . It is a very tight knit community and they all sort of dote over you really. It makes you feel really comfortable; you know that you have got the qualified nurses and a really qualified doctor and somebody that you feel really comfortable with. [Patient]
Continuity:
I don't think there's any disadvantage at all to having your child here, in fact I think it's more of an advantage because you're in your own community and you're with your own doctor and like I said, with the service that I got from my doctor and even the midwives that you bump into down the street at the post office, it just gives it a whole different concept to dealing with basically complete strangers in another hospital facility. [Patient]
Convenience:
We just felt that the smaller hospital could give us more attention; which they did. I actually stayed for six days just until I felt I was ready to go home. I had such a high level of care here. . .. It [larger urban hospital] is a very big hospital. You have to be out in three days, they are busy, and it is certainly not that they are any less competent. I just think that they are just so busy. [Patient]
Having friends and family pop in, it always feels good when you get visitors; it is convenient for all them as well. [Patient]
Family members quoted similar sentiments:
Well in a funny sort of way I think . . . maybe the care he got at [locality 1] was a little bit better because you can get lost in a big city and you just sort of become a number and there is so many different nurses and so many different doctors and you are not quite sure who you belong to. But here, it is just all the staff and you are not passed on to any other doctor - it is just him. You know the staff. . . you have got your own doctor . . . he didn't get passed off onto anybody else and within a few days you knew all the nurses that were on the shift because it is a smaller turnover. [Family member]
Patient satisfaction was high, as summarised (Fig 1). Overall, 83% (50) of patients indicated that they were 'very satisfied' with the care that they had received throughout their treatment. A further seven patients indicated they were 'satisfied' and three responded with 'indifferent'. A majority were 'very satisfied' with their doctor (90%; 54) and after hospitalisation, 95% (57) of patients indicated that they were either 'very satisfied' or 'satisfied' with the care they received at hospital.
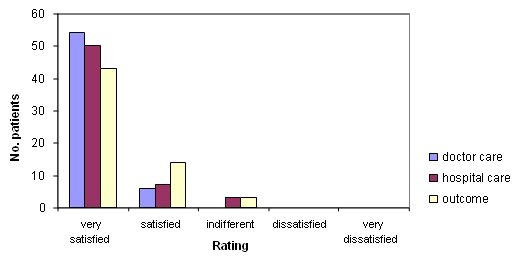
Figure 1: Patient satisfaction.
Although most patients rarely felt that there was any notable disadvantage to being treated at a rural hospital, most patients acknowledged that care at larger centres may involve a more extensive range of equipment and expertise. When given the option of having their procedure performed elsewhere, some patients recognised, or were even pre-warned, that in the event of an unexpected emergency, the local hospital would be limited in its capacity to respond. In these cases patients often justified their decision in terms of trusting the competency of staff and staff ability to monitor the situation appropriately, as well as confidence in the response of retrieval services.
You know that you can go down there [capital city], because the theatre is not always open at our hospital. I was told that if I went into labour and there seemed to be any hassles I might have to go to [capital city] anyway in an emergency. I knew that was always an option when theatre is not open on weekends every time. . .I think it works on one weekend on/one weekend off. Not 100% sure. When it was leading up to my due date, there were no theatre staff there for the three weeks up to my due date. I was hoping I wouldn't go into labour. They do an examination and if they think labour is going to progress it is fine, then you can stay. If they think it looks like there could be problem, they just either send you in your car or ambulance or by air to [capital city]. You know you options. I felt they would do the best for me. [Patient]
Although patients could quote many positive aspects about the care that they received at rural centres, there was some concern about availability issues including local understaffing and even a sense of fear about losing the services, even if less than ideally resourced.
Yeah, well you wouldn't want to lose the services that we've got. [Patient]
At the moment they are trying to take away the maternity ward and send it 30 kilometres down the road which we don't want. This is a thing going on with the government at the moment and the health board. We don't have that much control over that; we can sign a petition whether it does any good we don't know. . . . They are trying to cut a lot of the smaller hospitals out and when you are in the country and having a baby, I don't think you would like to go the extra 30 kilometres to have it . . . . If they take that service what else are they going to take? . . . I am not getting any younger but getting up around 75 I have got to travel an extra 30 kilometres to visit my wife and I don't see too well of a night now I mean it is a big problem for me. If I was in there and my wife had to do the driving, it would be a big problem for her of a night. Country driving is a bit different to the city. Down here you could run off the road and nobody would know you were there until the next day. These things are in the back of your mind, these things come up. [Patient]
Discussion
These results contribute further evidence, from a broader range of perspectives, to earlier research showing that rural medical procedural care can be of an acceptable quality9-11. There are caveats to this assertion, including the presence of trained and experienced medical and other health professional staff, appropriately equipped rural hospitals, and appropriate case selection. As seen from the information gathered here, the procedures included in the study were relatively simple procedures, relating to the kind of general procedures that are quite appropriately provided in smaller facilities, by staff with training in a relatively narrow range of procedures, as recommended by the relevant educational and professional organisations3,4.
As is consistent with the literature, patient comments reflected interest in accessibility, convenience, continuity of care, service sustainability and interpersonal aspects12,13. Clearly, several participants who chose to be cared for in their local rural hospital have concerns about the sustainability of these services. It is possible that some rural participants over-emphasised the positive aspects in defence of valued services. Never-the-less, we argue that it is appropriate to include consumer views in planning the location and accreditation of medical services.
The comments made by all groups of doctors were more technical in nature, and appeared to be remarkably congruent, except for the more frequent ratings of 'excellence' awarded by peer rural doctors than the urban specialists. This may be due to defence of rural service provision by rural doctors, who have observed the downgrading of other rural hospitals and the subsequent effect on rural communities5,7. An alternate explanation is that specialist reviewers, although supportive of rural generalist proceduralists in their own areas, are aware of the broader debate about the length of training and experience required to achieve competence in procedural disciplines. However, the peer rural doctors also made more frequent and more specific negative comments than the urban specialists, so another interpretation is that rural peers have a better understanding of the challenges of providing procedural services in rural facilities.
Limitations
In any relatively small survey there is the potential for recruitment bias. The doctors who agreed to participate may have been more confident of their abilities. Further, those patients who agreed to participate may have had either more or less confidence in the ability of their local healthcare team. The latter issue was addressed by requesting that consecutive patients be approached, and the data collected confirmed that this occurred in a majority of cases. In order to reduce the potential for selective recruitment, clinicians were required to notify the research team of recruited cases in advance. The exception to this was more urgent cases.
Conclusion
While the numbers of participating doctors and recruited patient cases were modest, this was a comprehensive and in-depth exploration of the quality of those procedures from the perspectives of patients, their families, peer rural doctors, urban specialists and a medical administrator. All groups rated the quality of care as being average or high in most cases, and the level of agreement between groups was high. Hence, this study supports the view that, where trained and experienced medical and other health staff are available in well-equipped rural hospital facilities, patients can receive care of similar quality to that expected by urban Australians. Further research is needed to examine procedural quality in a wider range of clinical cases, including those referred to larger hospitals, taking into account additional factors such as the level of equipment and other resources available in rural hospitals. This may allow for a deeper exploration of the impact of maintenance of facilities on the sustainability of quality services.
Acknowledgements
This project was funded by the National Health and Medical Research Council, Grant number 233502. Ethics approval was granted by the James Cook University Human Research Ethics Committee, approval number H1507. We would like to thank Professor A Rane, Associate Professor V Callanan, Associate Professor A Johnson, Dr R Turner, Dr Merefield, Dr T McLelland, Dr S Jackson and M Pincott for their contributions as case reviewers.
References
1. Strong K, Trickett P, Titulear I, Bhatia K. Health in rural and remote Australia - The first report on the Australian Institute of Health and Welfare on rural health. AIHW. Cat no PHE 6. Canberra: Australian Institute of Health and Welfare, 1998; vi-vii, 64, 21, 17, 34.
2. Australian Journal of Rural Health, Australian Medical Workforce Advisory Committee. The medical workforce in rural and remote Australia. AMWAC Report 1996.8. Sydney: AMWAC, 1996.
3. Royal Australian College of General Practitioners. Training Curriculum for General Practice. Melbourne: RACGP, 2004.
4. Australian College of Rural and Remote Medicine. ACRRM policy on training for rural and remote medicine. Brisbane: ACRRM, 2001.
5. Campbell D, Strasser R, Kirkbright S. Survey of Victoria's rural GPs in towns without a hospital. Moe, VIC, Australia: Monash University Centre for Rural Health, 1996.
6. Farmer J, Lauder W, Richards H, Sharkey S. Dr John has gone: assessing health professionals' contribution to remote rural community sustainability in the UK. Social Sciences Medicine 2003; 57: 673-686.
7. Petrucka PM, Wagner PS. Community perception of rural hospital conversion/closure: re-conceptualising as a critical incident. Australian Journal of Rural Health 2003; 11: 249-253.
8. Veitch PC, Sheehan MC, Holmes JH, Doolan T, Wallace A. Barriers to the use of urban medical services by rural and remote area households. Australian Journal of Rural Health 1996; 4: 104-110.
9. Cameron B. Outcomes in rural obstetrics, Atherton Hospital, 1981-90. Australian Journal of Rural Health 1998; 6: 46-51.
10. Woolard L, Hays RB. Rural GP obstetrics in NSW. The Australian and New Zealand Journal of Obstetrics and Gynaecology 1993; 33: 240-242.
11. Watts RW, Bassham M. Training, skills, and approach to potentially difficult anaesthesia in general practitioner anaesthetics. Australian Journal of Rural Health 1994; 6: 706-709.
12. Sutherns R. Adding women's voices to the call for sustainable rural maternity care. Canada Journal of Rural Medicine 2004; 9: 156-163.
13. Cleary PD, Edgman-Levitan S. Health care quality. Incorporating consumer perspectives. JAMA 1997; 278: 1608-1612.
APPENDIX I
Example questions from participant interviews
Doctor Interview
- Do you recall the cases that you nominated for this study?
- How has the follow-up care gone - anything interesting happened since?
- Any further reflections on the cases?
Patient pre-procedure interview
- What condition have you been seeing this doctor for?
- What procedure will you be having?
- What hospital will you be having this procedure in?
- Why did you see this particular doctor for your procedure? (e.g. only doctor in town, family doctor, recommended by friends/family)
- Were you given any alternative hospitals for where you were to have your procedure?
- Are you happy to have the procedure done at this hospital?
- Would you say that it was easy to get an appointment with the doctor that suited you?
- How far did you have to travel to see this doctor?
- How satisfied are you with the service that this doctor has provided so far for this particular condition? (Prompts interpersonal skills, professional behaviour, takes time, technical quality, good doctor - why?)
- All things considered, how would you rate the quality of the care that you have received so far? Excellent, good, indifferent, bad or terrible?
Patient post-procedure interview
- How satisfied have you been with the service that the doctor has provided you
- What have been some of the positive and negative features of the doctor's service?
- On a scale of 1-5 how happy have you been with the care that you have received at the hospital? What reasons could you give me for this?
- What were the advantages and disadvantages of receiving treatment at this hospital (as opposed to another hospital)?
- How satisfied are you with the result of the procedure?
- Overall, how would you rate the quality of care that you have received at this hospital?
- Overall, how would you rate the quality of care that you received from this doctor in particular?
- Do you think that the care provided by a hospital and doctor in a larger centre would be better / worse / or the same as the care that you have received here? What reasons?
- Would you recommend this hospital to family and/or friends?
- Would you recommend this doctor to family and/or friends?
Family member interview
- To start off with, I would just like to know what the implications of [patient]'s condition were for you and [patient]'s family before the procedure (i.e. how has [patient]'s condition affected yourself and [patient]'s family?).
- Was [patient] given any alternatives for where he/she was to have the procedure?
- At the time, were you happy with the decision to have the procedure at this hospital?
- What other options did [patient] have?
- How involved were you in the decision to have the procedure here? (If not very much then continue to question 3.)
- What factors influenced the decision to have the procedure performed here?
- What would have been the impact of having the procedure performed in a larger centre? (i.e. where there would most likely be greater travel requirements)
- Was [patient] given any alternatives as to what procedure they were to have?
- How far did [patient] have to travel to see the doctor? Is this reasonable?
- Do you think that access to the doctor or the hospital could have been improved in any way?
- On a scale of 1-5 (where 1 = very happy and 5 = not very happy at all) how happy have you been with the care that [patient] has received at the hospital? What reasons?
- Overall, how would you rate the quality of care that [patient] has received at this hospital?
- Overall, how would you rate the quality of care that [patient] has received from this doctor?
- Do you think that the care provided by a hospital and doctor in a larger centre would be better / worse / or the same as the care that [patient] has received here?



