Stroke is the third leading cause of death in Scotland after coronary heart disease and cancer, and is a major cause of long-term disability1,2. Research has shown that good care which includes early multidisciplinary assessment, specialist rehabilitation and well-organised discharge and follow up improves survival and minimises disability3-5. The nature of stroke and the complexity of needs following a stroke present a huge challenge to service providers.
Epidemiological data on stroke informs service provision6. It is important to configure stroke services to reflect the local health culture7, and where appropriate, the rural environment. Planners and clinicians require data on stroke incidence and outcome8. However, such data are limited, especially in Scotland, and are largely acquired from hospital-based practice9. Not all patients enter hospital, and those that do may represent a biased group10.
Approximately one-fifth of Scots live in rural areas. It is important to include a rural perspective in relation to health issues11, as inadequate provision and inaccessibility of health-service provision in rural areas may be detrimental, particularly for some groups of rural societyz12,13. Studies in the 1990s have addressed the impact of distance and rurality on the outcome of particular diseases, asthma, diabetic retinopathy and cancer, and have shown poorer outcomes for rural residents14-16.
Stroke is mainly a disease of the elderly and many rural areas have a high proportion of elderly residents12.There is evidence that stroke care should be organised within specialist units and should be available for the duration of the illness4. However, the best way to provide care in areas with scattered populations in remote rural and island settings, such as Highland and the Islands of Scotland, is unclear. Highland Region alone covers an area of 26 000 km2, and this geography presents challenges to providing a stroke service. This study was designed to explore whether stroke care and outcome was affected by remoteness and rurality.
Methods
This was a community-based survey to assess outcome of stroke and provision of services to stroke patients across Highland, Orkney, Shetland and the Western Isles. Highland and the Islands (Orkney, Shetland, the Western Isles) of Scotland include a population of approximately 280 000 over 26 000 km2 (Highland alone) and 42 inhabited islands (Orkney, Shetland and Western Isles), served by approximately 114 medical practices.
Patients suffering a stroke are usually seen acutely by a general practitioner who will either refer the patient to hospital or arrange further management at home. Patients could be identified at acute presentation when they would be notified by a general practitioner, or during the early stages of treatment when notification could come from a hospital clinician or practitioner, or during the rehabilitative stage by other health, social care professionals or voluntary/charitable organisations. Notification was made by completing a project-specific form. Daily and weekly contact was made with local clinicians and practitioners. The study attempted to identify all first-ever strokes occurring in Highland and the Islands of Scotland during a 12-month period.
The study population comprised patients over the age of 18 years with a first-ever stroke registered with one of the collaborating general practitioners. The recruitment of an individual was based on their ability to meet all of the following inclusion criteria:
- Resident within Highland, Orkney, Shetland or the Western Isles of Scotland
- A clinically apparent first-ever stroke occurring between 1 May 2001 and 30 April 2002
- Aged 18 years or over
Health and social care professionals, the voluntary sector and charitable organisations specifically involved in caring for stroke patients in Highland and the Islands were informed of the study and invited by letter to participate.
The study was prospective in nature with follow-up at 1, 3 and 6 months post-stroke to collect data on incidence, functional ability ('limitation in activities'), and the use of health and social care and voluntary sector services. Outcomes, in terms of limitation in activities, were measured by the Barthel Index (BI)17. Data collection consisted of a self-completed patient questionnaire and a professional service use data sheet. To maximise response rate to the questionnaire, one reminder letter and questionnaire was sent 2 weeks following the first mailing. Completion was by the patient or a nominated carer. A pragmatic definition of stroke was adopted, in which stroke was considered to be primarily a clinical diagnosis relying on clinical observations18. The WHO definition for the diagnosis of stroke or cerebrovascular accident was used19. Although this definition includes subarachnoid haemorrhage, patients with this diagnosis were excluded from this study. Information was requested on severity at the acute phase of the stroke. However, since subjects were enrolled into the study at varying time points after the acute event, the data were not used in analysis due to potential unreliability.
A generic definition of rurality was chosen, which classifies settlements by sparsity (population density/settlement size) and remoteness (journey time)13,20. This classification was developed for use with the Scottish Household Survey by the Environment and Rural Research Branch of the Scottish Executive's Social Research Division21. For the analysis, the 8-fold classification was collapsed into three categories:
- Urban/accessible: urban, accessible small town and accessible rural categories were grouped together (any settlement of at least 10 000 inhabitants or within 30 min driving time of a settlement of 10 000 or more).
- Remote rural: remote small towns and remote rural (any settlement between 30 and 60 min driving time of a settlement of 10 0000 or more).
- Very remote: very remote small towns and very remote rural areas (any settlement more than 60 min driving time from a settlement of 10 000 or more).
Cases were identified using overlapping methods and hot pursuit techniques22. All practitioners from health and social care sectors, such as general practitioners, hospital clinicians, allied health professionals, community nurses, social workers, nursing and residential homes, voluntary and charitable organisations were encouraged to notify patients.
Data collected on the patient questionnaire included: place of residence and domestic circumstances (home alone or with carer) at time of follow up, health and social care services used, medication before and after stroke event, co-morbidities, BI and the Stroke-adapted Sickness Impact Profile to assess functional ability. Data on use of services were collected by self-completed proformas from health and social care professionals, and voluntary and charitable organisations. Data from questionnaires and proformas were entered into a purpose-built database designed in Microsoft Access 97 and then transferred for statistical analysis to SPSS, vers. 10.0 (SPPS Inc; Chicago, IL, USA). Descriptive statistics are presented. Continuous variables are shown as mean, median or percentiles, categorical variables as percentages. c2 (Chi-squared) analyses were used where appropriate. As some respondents did not complete all elements of the Stroke adapted Sickness Impact Profile, this was not used in analysis.
The study was approved by the research ethics committee of each participating area. Written informed consent was obtained from all patients. If the participant was cognitively impaired, dysphasic, or had altered consciousness, consent was obtained from the next of kin or carer.
Results
Reported incidence and notification of patients
Three hundred and three patients were notified with a suspected first-ever stroke. The resulting crude incidence of reported stroke was 1.1 per 1000 population. The notification and recruitment process of the project is shown (Fig 1). Of the 303 patients notified, 239 (78.9%) were sent a consent form. The remaining 64 patients were not sent a consent form due to a number of reasons such as death before notification; cases notified anonymously, the suspected stroke occurring outside the study time period; or considered by a health professional to be inappropriate to contact. Of the 239 patients who were sent a consent form, 118 (49.4%) agreed to take part in the study. Of these, 114 were recruited. Four were not recruited because two were found to be outside the time period, one died between consent being given and consent being received and one had not suffered a stroke. Of the 114 patients recruited, 85 were included in the final data set. Exclusions from the final data set were due to a variety of reasons such as: not having a first stroke; suffering the stroke outside the study time period; and where the diagnosis was unclear.
Of those notified, 159 were female, 136 male. Eight patients among 14 notified anonymously had no information on sex. The mean (SD) age was 74 (10) years. Of those notified, where settlement category was known (n = 284), 54% were from urban/accessible areas, 12% from remote rural areas and 34% from very remote areas.
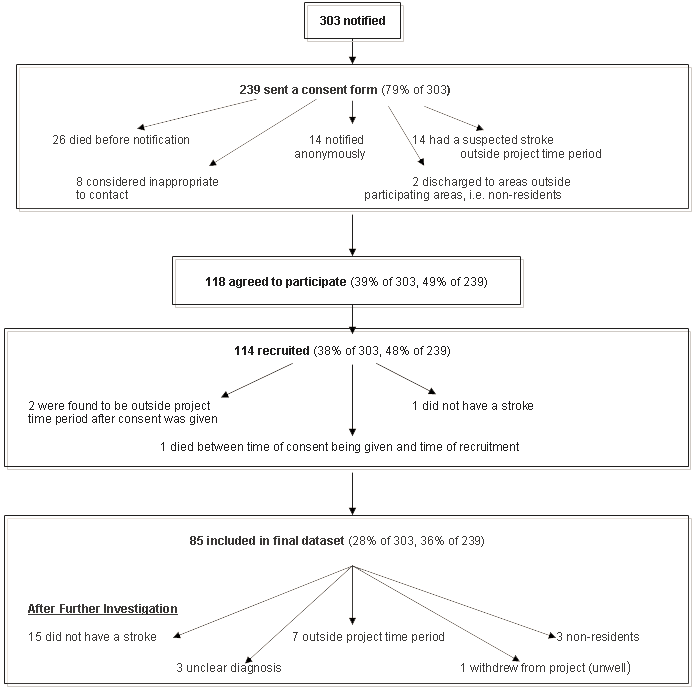
Figure 1: Stroke patient recruitment and notification.
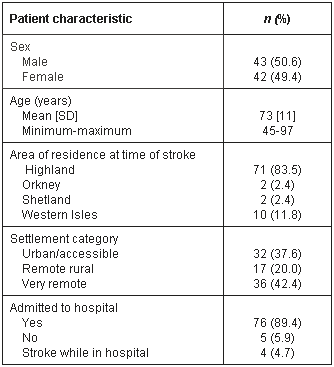
Characteristics of patients included in the final dataset are shown (Table 1). Cases included did not differ from all cases notified in terms of area of residence (c2 = 6.9, p = 0.074). However, when analysed as settlement category, a greater proportion of those included in the final dataset came from remote rural and very remote settlements (c2= 7.3, p = 0.025).
Table 1: Characteristics of included patients (n = 85)
Patient location
Patient location by settlement category at 1, 3 and 6 months is shown (Figs 2-4). Seventy-six patients (89.4%) were admitted to hospital following their stroke, 5 (5.9%) remained at home and 4 patients (4.7%) suffered their stroke while in hospital. Of the 76 patients, 9 (11.8%) were admitted to GP/Community hospitals, the remaining 67 (88.2%) to acute hospitals. Of the 5 patients not admitted to hospital, three came from remote rural and two from very remote settlements. None were from urban/accessible settlements. The majority of patients returned home from acute hospitals during the study period and the likelihood of returning home was not related to settlement category. However, a greater proportion of patients in remote rural settlements were admitted to community hospitals and remained there at 6 months (c2= 9.5, p = 0.009).
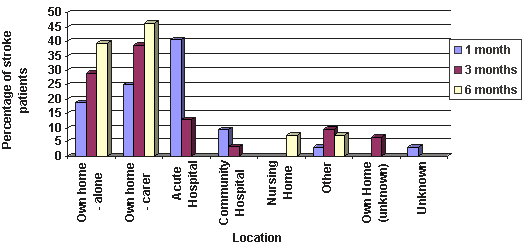
Figure 2: Patient location by settlement category at 1, 3 and 6 months post-stroke: urban/accessible.
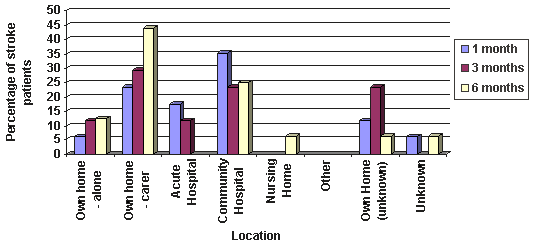
Figure 3: Patient location by settlement category at 1, 3 and 6 months post-stroke: remote rural.
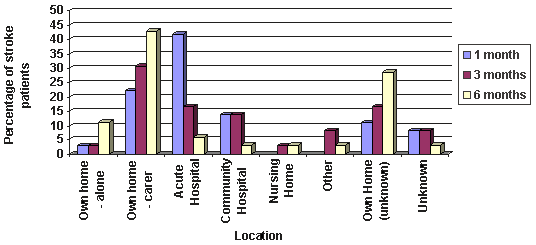
Figure 4: Patient location by settlement category at 1, 3 and 6 months post-stroke: very remote.
Functional ability ('limitation in activities')
Limitation in activities by settlement category at 1, 3 and 6 months and the proportion of patients in each functional ability level are shown (Figs 5-7, respectively). Approximately two-thirds had some degree of disability (or limitation in activities) after their stroke. Only one-third of patients classed themselves as independent across all time points. Overall, the BI score increased over time (ie, patients experienced a reduction in disability), with the average score at 1 month post-stroke being 82.5 (range 0-100), at 3 months 85 (range 5-100), and at 6 months 90 (range 5-100). However, when examined by settlement category, only patients from urban/accessible settlements showed a consistent increase in the BI score over the 6-month period post-stroke. Across all time points, a greater proportion of patients from remote rural settlements reported severe disability but this was not statistically significant.
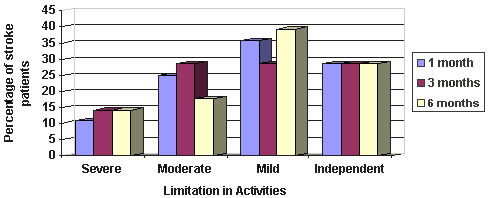
Figure 5: Limitation in activities at 1, 3 and 6 months post-stroke as measured by the BI: urban/accessible.
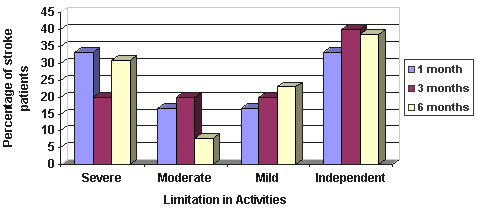
Figure 6: Limitation in activities at 1, 3 and 6 months post-stroke as measured by the BI: remote rural.
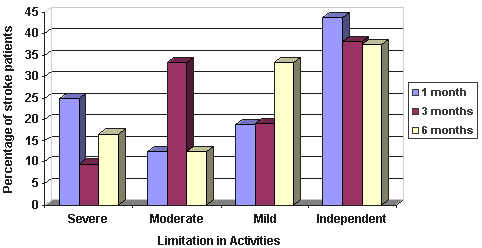
Figure 7: Limitation in activities at 1, 3 and 6 months post-stroke as measured by the BI: very remote.
Utilisation of health and social services
Use of health and social services reported by health care professionals, classified by settlement category, is shown (Figs 8-10). The service most commonly provided from the time of the stroke event at 1 and 3-months post-stroke was physiotherapy. However, the involvement of this service, along with the other core elements of a multidisciplinary stroke team, such as occupational therapy, and speech and language therapy, decreased with time, irrespective of settlement category. With respect to charitable organisations, services provided by Chest, Heart and Stroke Scotland (CHSS), for example Stroke Clubs and the Voluntary Stroke Services, increased over time. However, the percentage of patients being provided with stroke-specific and social support services over a 6-month period was low. Social services were the most commonly received service for all patients 6 months after their stroke. The uptake of services was similar across all settlement categories, with patchy use of services and low levels of use at 6-months post-stroke. The proportion of patients using any service at 1, 3 and 6 months did not differ between settlement categories (c2 = 17.9, p = 0.464; 23.2, p = 0.281; 29.8, p = 0.074 respectively). Rural patients did not therefore appear disadvantaged in service use.
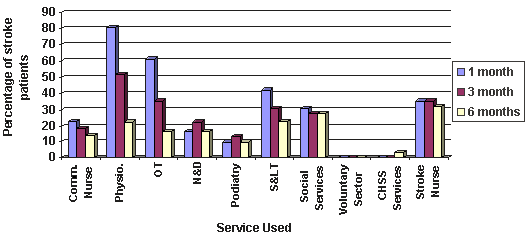
Figure 8: Patients receiving health and social services at 1, 3 and 6 months Post-Stroke: Urban/accessible. Comm. Nurse, community nurse; Physio, physiotherapy; OT, occupational therapy; N&D, nutrition & dietetics; S<, speech & language therapy; CHSS Services, Chest, Heart and Stroke Scotland Services.
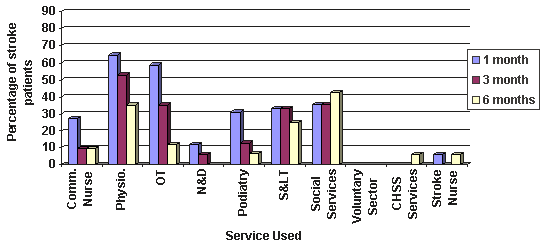
Figure 9: Patients receiving health and social services at 1, 3 and 6 months Post-Stroke: Remote rural. Comm. Nurse, community nurse; Physio, physiotherapy; OT, occupational therapy; N&D, nutrition & dietetics; S<, speech & language therapy; CHSS Services, Chest, Heart and Stroke Scotland Services.
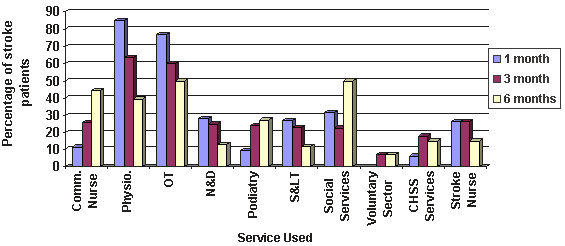
Figure 10: Patients receiving health and social services at 1, 3 and 6 months Post-Stroke: very remote. Comm. Nurse, community nurse; Physio, physiotherapy; OT, occupational therapy; N&D, nutrition & dietetics; S<, speech & language therapy; CHSS Services, Chest, Heart and Stroke Scotland Services.
Conclusions
Reported incidence, notification, recruitment and inclusion
The crude incidence of stroke reported in this study was lower than would be expected from published data23,24. This probably reflects under-reporting of cases, although there may be other contributory factors. The estimated age- and sex-standardised incidence of first-ever stroke in Scotland in 2000 was 2.29 per 1000 [Source: Information and Statistics Division (ISD), Common Services Agency], and that quoted in the 1994 SNAP Report10 was 2.98 per 1000. The present study included only patients who were resident and suffered their stroke in the study catchment area. In contrast, ISD figures include patients resident in the catchment area irrespective of where their stroke event occurred. It has been been suggested previously that 'health-status data pertaining to catchment areas consisting of small and rural communities is perhaps best used for trend analysis rather than for factual comment on health status'25. It is unlikely, however, that differences in catchment population would explain the difference between our reported incidence and ISD figures. The definition of first-ever stroke used in our study was identical to that used in the record linkage from which the ISD figures were obtained. However, the 1994 SNAP report data10 included transient ischaemic attacks, and may have included stroke as a secondary diagnosis, whereas our study included only primary diagnosis of stroke.
Under-reporting in our study may have occurred for several reasons. A substantial proportion of stroke patients die within 3-4 weeks after a stroke event26,27, and potential patients may have died prior to notification. Practitioners may have failed to notify cases because of uncertainty about the diagnosis, for example, where they were unsure if the patient had suffered a transient ischaemic attack. Professionals may have felt it inappropriate to notify patients at either end of the stroke-severity spectrum who also may not have been referred to health and/or social services, reducing other potential routes of notification. Doctors opting to manage patients at home may have been reluctant to report cases. We are aware from local research, in which scenarios were presented to GPs, that a significant proportion of stroke patients may be managed at home (JG Macfarlane, pers. comm., 2001). To determine stroke incidence accurately and allow time trends to be considered, a community-based stroke register would be required. This would also allow risk factors, co-morbidities and outcomes to be recorded28.
Location
The proportion of patients at home in urban/accessible and very remote settlements was similar at 6 months post-stroke. This is in keeping with previous observations that the majority of stroke patients admitted to hospital eventually return home. However, we found a higher proportion of patients living at home at 6 months compared with past studies in which, at 6 months, between 60% and 70% of survivors of first-ever stroke were living at home10,29. A greater proportion of patients in the remote rural category were admitted to community hospitals and remained there at 6 months. This may reflect greater availability of community hospital places in this category, but may also be influenced by stroke severity.
Limitation in activities
Only a third of our patients classed themselves as independent at 1, 3 and 6 months post-stroke. This is lower than would be expected from previous literature, which suggests that half of all stroke patients will regain independence, mostly within 6 months27,30. More patients reported severe disability/limitation in activities in our study than in published reports of outcome31. The reasons for this poor functional outcome remain unclear and are concerning. Although data collected on severity at onset of the stroke were considered unreliable due to collection at different time points, it is likely that our study population was biased towards those with milder strokes. This raises the possibility that rehabilitation of stroke patients throughout the participating areas is inadequate.
Utilisation of health and social services
Uptake of services was equivalent across all settlement categories. The use of rehabilitation services decreased over time, and social service use increased. Patchy uptake of services was apparent, the level of use at 6 months post-stroke being low. Patients may have been unaware of the existence of such services or felt they did not require them at their stage of recovery. However, the relatively poor functional outcome of our patients suggests that there is an unmet need for rehabilitation. Our findings are similar to past research which has shown that organised care and the level of specialist services provided may reduce or cease within a few months of discharge32, and that the involvement of health and social services in the long-term management of stroke patients is minimal33,34. In our study, physiotherapy was the most common, and occupational therapy the next most common, service received, as previously shown by others35,36. Although use of services was generally low, rural patients did not appear specifically disadvantaged. However, our data suggest that use of rehabilitation services needs to be enhanced irrespective of settlement category.
Our study explored service use, rather than service provision. Historically, health, social and voluntary services have tended to be less accessible in rural areas than in more densely populated areas13, elderly people in rural areas receiving fewer health care services than those in urban areas37. However, research carried out in the 1990s showed that access to health care in rural Nebraska was as good, if not better, than access to health care in urban parts of the same State38. Other researchers have reported better service provision in rural areas in specific circumstances and localities, for example community and social provision for older people (health visitors, district nurses, meals-on-wheels)12,39.
Our findings must be interpreted in the light of the relatively low proportion of patients who could be included in the final dataset. Patients from the remote rural and very remote categories were slightly over-represented in our final dataset, compared to all those notified. Our study suggests that patients developing a first-time stroke in remote and rural areas are not disadvantaged compared to those in urban/accessible areas with respect to outcome or to the utilization of health and social care services. However, functional outcomes could be improved for all patients and there may be a general unmet need for rehabilitation and support services.
Acknowledgements
The authors thank the numerous health and social services staff, voluntary sector and charitable organisations for providing essential information about service provision and patient progress, and Donalda Morrison and Kay Lackie for providing secretarial and administrative support in such an efficient manner throughout the study. Thanks also go to Highland NHS Board for affording Noelle O'Neill the opportunity to undertake the study, and to the Remote and Rural Area Resource Initiative (RARARI) for funding. The study findings were presented by NP O'Neill at Research on Remote and Rural Health, an Institute of Applied Health Sciences Seminar, University of Aberdeen, UK, 21 May 2003; and at International Rural Network Conference and Exchange of Experience, Inverness, Scottish Highlands, UK, 22-27 June 2003.
References
1. Royal College of Physicians of Edinburgh. In: Proceedings, Royal College of Physicians of Edinburgh Consensus Conference on Medical Management of Stroke, 26-27 May 1998. Edinburgh: Royal College of Physicians, 1998.
2. Health Department. Coronary Heart Disease and Stroke: Strategy for Scotland. Scottish Executive Health Department. Edinburgh: HMSO, 2002.
3. Health Department. Adding Life to Years - Report of the Expert Group on Healthcare of Older People. Scottish Executive Health Department. Edinburgh: HMSO, 2002.
4. Stroke Unit Trialists' Collaboration. Organised inpatient (stroke unit) care for stroke (Cochrane Review). In: The Cochrane Library, 1, 2002. Oxford Update Software. The Cochrane Library, 2002.
5. Langhorne P, Dennis MS, Kalra L, Shepperd S, Wade DT, Wolfe CDA. Services for helping acute stroke patients avoid admission (Cochrane Review). In: The Cochrane Library, 1, 2002. Oxford Update Software. The Cochrane Library, 2002.
6. Wilkinson PR, Wolfe DA, Warburton FG et al. A Long-term follow-up of stroke patients. Stroke 1997; 28: 507-512.
7. Coop J, Williams A, James M, Wills T. Shared-care stroke service helps to promote best practice. Guidelines in Practice 2001; 4: 45-52.
8. Oxfordshire Community Stroke Project. Incidence of stroke in Oxfordshire: first year's experience of a community stroke register. BMJ 1983; 287: 713-717.
9. Roberts MA, Allen A, Langhorne P, McEwen J, D'A Semple P. Organisation of services for acute stroke in Scotland - report of the Scottish stroke services audit. Health Bulletin 2000; 58: 87-95.
10. Webb J, Teo P, Stark C. Acute Stroke. Glasgow: Stroke Needs Assessment Programme, 1994.
11. Strategic Alliance for Rural, Northern and Remote Health Research (Canada). Rural, Remote, and Northern Health Research: The Quest for Equitable Health Status for all Canadians. The Rural Health Research Summit, Prince George, British Columbia, 1999.
12. Shucksmith M, Roberts D, Scott D, Chapman P, Conway E, and The Arkleton Centre for Rural Development Research, University of Aberdeen. Disadvantage in rural areas. Rural research report number 29. Rural Development Commission, 1996.
13. Deaville JA. The Nature of Rural General Practice in the UK -Preliminary Research (March 2001). A joint report from the Institute of Rural Health and the General Practitioners Committee of the BMA. Institute of Rural Health, 2001.
14. Jones AP, Bentham G, Horwell C. Health service accessibility and deaths from asthma. International Journal of Epidemiology 1999; 28: 101-105.
15. Leese GP, Ahmed S, Newton RW et al. Use of mobile screening unit for diabetic retinopathy in rural and urban areas. BMJ 1993; 306: 187-189.
16. Campbell NC, Elliot AM, Sharp L et al. Rural factors and survival from cancer: analysis of Scottish cancer registrations. British Journal of Cancer 2000; 82: 1863-1866.
17. Mahoney FI, Barthel DW. Functional evaluation: the Barthel Index. Maryland State Medical Journal 1965; 14: 61-65.
18. Royal College of Physicians, London. Clinical Guidelines - Stroke. Royal College of Physicians, London, 2000.
19. World Health Organisation. Control of Stroke in the Community: Methodological Considerations and protocol of WHO Stroke Register. CVD/S/73/6. Geneva: WHO, 1973.
20. Scottish Executive. Availability of Services in Rural Scotland. Scottish Executive, 2002. (online)http://www.scotland.gov.uk/library5/rural/asrs-00.asp (accessed 6 Jan 2003).
21. Dudleston A, Hope S, Littlewood A, Martin C, Ormston R. Scotland's People: Results from the 2001 Scottish Household Survey, Vol 5: Annual Report. A Scottish Executive National Statistics Publication. Edinburgh 2002. (online) http://www.scotland.gov.uk/library5/society/spv5-00.asp (accessed 2 Sep 2003).
22. Thrift AG, Dewey HM, MacDonell RAL, McNeil JJ, Donman GA. Stroke Incidence on the East Coast of Australia - The North East Melbourne Stroke Incidence Study (NEMESIS). Stroke 2000; 31: 2087-2092.
23. Bugge C, Alexander H. Ayrshire and Arran Stroke Outcome Study (Final Report). Ayrshire and Arran Health Board, 1999.
24. Bamford J, Sandercock P, Dennis M et al. A prospective study of acute cerebrovascular disease in the community: the Oxfordshire Community Stroke Project 1981-86. 1. Methodology, demography and incident cases of first-ever stroke. Journal of Neurology, Neurosurgery and Psychiatry 1988; 51: 1373-1380.
25. The Advocate Institute, Pilot Project to Develop a Community Health Measure for Small and Rural Communities. The Advocate Institute, Canada 1999.
26. Moore A (Eds). Evidence Based Medicine in Practice: Secondary prevention of Stroke. London: Hayward Medical Communications, 1997.
27. Harwood RH. The epidemiology of stroke. British Journal of Cardiology 2001; 8: 507-513.
28. MacWalter RS, Coid DR, Fraser HW, Ersoy Y. The Dundee Stroke Register: Experience of the First Ten Years. Scottish Medical Journal 1999; 44: 103-105.
29. Bamford J, Sandercock P, Dennis M, Burn J, Warlow CP. A prospective study of acute cerebrovascular disease in the community: the Oxfordshire Community Stroke Project 1981-6. 2: Incidence, case fatality rates and overall outcome at one year of cerebral infarction, primary intracerebral and subarachnoid haemorrhage. Journal of Neurology, Neurosurgery and Psychiatry 1990; 53: 16-22.
30. Venables G. Prognosis, outcome and recurrence of stroke. British Journal of Cardiology 2002; 9: 103-105.
31. Bain M. Lothian Health - A Strategy for Stroke. Edinburgh: Lothian Health Board, 1999.
32. The Stroke Association. More Positive Steps - The District Stroke Coordinators Centenary Conference. London: Stroke Association, 2000.
33. Weddell JM, Beresford SAA. Planning for stroke patients: A four-year descriptive study of home and hospital care. London: HMSO, 1979.
34. Bugge C, Hagen S, Alexander H. Measuring stroke patients' health status in the early post-stroke phase using the SF36. International Journal of Nursing Studies 2001; 38: 319-327.
35. Beech R, Ratcliffe M, Tilling K, Wolfe C. Hospital Services for Stroke Care - A European Perspective. Stroke 1996; 27: 1958-1964.
36. Bugge C, Alexander H. Ayrshire and Arran Stroke Outcome Study (Final Report). Ayr: Ayrshire and Arran Health Board, 1999.
37. Schlenker, Powell MC, Goodrich GK. Rural-urban home health care differences before the Balanced Budget Act of 1997. Journal of Rural Health 2002; 18: 359-372.
38. Comer J, Mueller K. Urban-rural comparisons from a mid-western agricultural state. Journal of Rural Health 1995; 11: 128-136.
39. Cox J, Mungall I (Eds). Rural Healthcare. Oxford: Radcliffe Medical Press, 2000.

