Over two-thirds of the northern British Columbia (BC) population lives in rural communities1,2 and almost one in five people living in northern BC (17.5%) identify as Aboriginal1, which includes First Nations (FN), Inuit, and Métis. Northern BC covers approximately 600 000 km2 or two-thirds of the province2. People living in these areas face unique challenges in accessing and using the health system. There are typically fewer primary healthcare (PHC) providers per capita3, large geographic distances between these providers and needed medical technology (eg diagnostic imaging, stress testing), less availability of public transportation, and harsh winter driving conditions1. The lower socioeconomic status of rural residents compounded by services dispersed across large geographic areas can create financial barriers that affect access to health care1,4.
Despite Canada's universally accessible healthcare system and millions spent in renewing its PHC system5,6, rural residents, especially those who are Aboriginal, are hospitalized more often for conditions that are treatable in a PHC setting7. Moreover, inequities between Aboriginal and other Canadians persist on virtually every measure of health and social status. For example, Aboriginal people have lower life expectancy, decreased access to health services, and disproportionately high rates of preventable, chronic and acute health conditions8-10.
More work is needed to inform healthcare renewal in ways that are relevant to rural and Aboriginal communities. The 'right to health' (ie the right to enjoy the highest attainable standard of physical and mental health11) is different from 'the right to be healthy' due to there being many factors beyond healthcare systems' control that influence health12. Rather, the right to health is better understood as the right to a healthcare system that provides equal opportunity to enjoy the highest attainable level of health12, regardless of geography or economic means. This includes access to medical care and other factors crucial to health and wellbeing such as child care, education, housing, environmental protection13.
Engaging residents of rural and FN communities in research is the key to informing the next wave of innovations designed to more effectively address health and healthcare inequities. This is particularly important in FN reserve communities because provincial and federal jurisdictional responsibilities concerning the delivery of services create additional complexities14-16. Too often, solutions to health and healthcare inequities are based on work completed in urban areas. Those living in rural and Aboriginal communities remain markedly under-represented in research, raising important ethical and legal concerns and limiting the generalizability of study findings outside urban centres17,18. This lack of engagement of rural communities where almost 20% of the population is Aboriginal, and the paucity of research including rural residents, is likely to be linked to the complexities of conducting research in these contexts, particularly regarding recruiting study participants. Without such engagement, however, urban-centric research will continue to inform PHC service delivery for rural, remote and Aboriginal people, which could result in ill-tailored strategies and poor outcomes.
Understanding and using effective strategies in recruitment in these settings is one way in which researchers can strive for inclusive samples. In the USA and other countries, much attention has been paid to determining which strategies are optimal for recruiting minorities into research since the National Institutes of Health's Revitalization Act 1993 (enforced in 1994, revised in 2001), which mandates the inclusion of minorities in federally-sponsored research studies. However, no one strategy has been found effective for all situations, particularly in the context of collecting data from rural participants who may be American Indians. Indeed, different articles propose a variety of 'best practices' based on specific situations rather than promoting a single solution19-25. Researchers are faced with a broad range of strategies from which to choose, and must rely on their experience, goals, and training to guide them in determining which practice/s to select for a particular study. Few resources are available to guide successful recruitment strategies in Canada's rural, remote and Aboriginal communities.
The purpose of this article is to report on a set of successful strategies that were trialed with rural and Aboriginal communities in northern BC. The majority of Aboriginal communities in northern BC are FN reserve communities. These strategies could assist researchers in achieving equitable recruitment, that is, recruitment where residents have the same opportunity to participate in a study despite the wide geographic dispersion between communities. These strategies are in line with the required conscientious approach for working with Aboriginal people, including those who are FN, given their experiences of long-standing inequities and marginalization26, as defined by the main funders of research in Canada27.
Context of the study
The Northern Health (NH) Authority of BC (one of six Health Authorities) approached the present research team with a request to examine the effectiveness of a new format for the delivery of PHC: Group Medical Visits (GMVs) occurring in their health authority. Northern Health, together with its healthcare providers, has and continues to develop innovative ways to deliver health services and ensure better access to care for its residents1. One such innovation is the use of GMVs delivered in a physician's practice, a space provided by NH, or a community clinic located on a FN reserve. In many rural communities across Canada, the majority of Aboriginal residents live on a FN reserve. A reserve is a small portion of what might have some time been part of a nation's traditional territory, which is protected by legislation for the use and benefit of a FN28.
Primary healthcare services provided in GMVs are offered in a group format rather than in the traditional individual patient-healthcare provider format. The GMVs generally consist of 12-15 patients who often have a medical condition in common (eg diabetes), facilitated by a healthcare provider, typically a family physician or nurse practitioner. The GMVs include health education provided in a group setting and individualized medical care, which may include physical examinations, the diagnoses of illnesses, writing prescriptions, referrals to specialists and orders for laboratory testing. The GMVs allow healthcare providers to see multiple patients at once, thus increasing patients' access to care and their own productivity29,30. This increased productivity can greatly benefit both healthcare providers and patients, who may have to travel long distances to provide and receive care, respectively. The GMVs provide patients with the added benefit of attending all their medical appointments in one setting, with other members of their community, in a supportive environment31,32.
The data informing this article were collected within the context of a larger mixed-methods study where the purpose was to examine the impact of GMVs on the quality of PHC from patients' and providers' perspectives. This larger study consisted of a distributed research team who worked as faculty at the University of BC ([UBC] Vancouver) and University of Northern BC ([UNBC] Prince George) and decision-makers in NH Authority. A qualitative component involved conducting in-depth interviews with patients (n=29) who had attended GMVs and healthcare providers and other allied health professionals (n=34), such as nutritionists, social workers, medical office assistants and community health workers, who had been involved in delivery of GMVs in the past 12 months. This was followed by a patient-experience survey to patients in practices or reserve communities where GMVs were being delivered. Patients who had and those who had not attended a GMV in the past 12 months were eligible to participate. The results reported here are focused on recruitment for the survey.
The patient experiences survey was developed based on previous work by Wong et al33 and past research33-35. The survey reflected important dimensions of PHC such as accessibility, continuity (informational, relationship, and management continuity), patient activation, sociodemographic characteristics and self-reported health status. Publicly available items and scales were used to develop an item pool. Final items and scales based on their previously known psychometric characteristics (adequate reliability and validity) and their ability to adequately measure each PHC dimension. Pilot testing (n=20) was previously conducted to clarify meanings of the items and work out survey administration33. The final survey instrument consisted of approximately 200 questions and took 45-60 min to complete.
Participants
In order to administer the patient experience survey, the researchers worked with FN reserve communities (n=5) and primary care practices (n=6) located in NH Authority of BC. The communities ranged in size from 200 to 76 000 people. The regional hospital is in Prince George, a community known as BC's northern capital36. Participating communities in the study were from 100 to 1000 km from Prince George. The research team had contact with one member from each community who was identified as the community partner. Differing positions held by community partners included: PHC coordinators (n=3), medical office assistants (n=2), practice managers (n=3), community health nurses (n=4), a nurse practitioner (n=1), a community health representative (n=1), and a community administrator (n=1). The community partners and Health Authority decision-maker partners helped to identify and recruit primary care practices offering GMVs. Eligibility criteria of patients included: (i) age 19-90 years; (ii) English speaking; (iii) no cognitive impairments; and (iv) had visited a family doctor or nurse practitioner in one of the participating practices within the past 12 months. The GMV participants included patients who were receiving care for chronic conditions, weight loss, prenatal care, or general wellness (eg women's health).
Procedures
Once FN communities and rural practices had consented to participating in the study, recruitment of participants was tailored according to direction from the community partners. The research team worked closely with its community partners to recruit a convenience sample of potential participants. In some places the research team presented information on the study and provided 'sign-up forms' for patients interested in participating. In other places, recruitment of potential participants included attending health fairs where all practices had agreed to participate, having the community health worker recruit potential participants, traveling to communities to administer the survey face-to-face and administering the survey at the end of a GMV appointment. Information about the study and survey was provided to all practices and community partners. Consent (signed or verbal) was obtained prior to administering the survey. For any practice able to collect 50 or more surveys, an aggregated report of patient experiences with their care was provided. For FN reserve communities, an aggregated report of patient experiences with their care was provided. Obligations to the study's community partners were defined in community-specific memoranda of understanding that required the research team to report on community-specific and overall findings before these could be released publicly. In addition, engagement with FN communities was guided by 'the 4 Rs' (Respect, Relevance, Reciprocity, Responsibility) framework adopted by the Network Environments for Aboriginal Research BC. Ethics Boards of the University of BC, University of Northern BC, and NH Authority Behavioral approved all procedures. These procedures are also consistent with Tri-Council guidelines for conducting research in Aboriginal communities27.
Participants were given the option of completing the survey in-person or via telephone. Contact information for patients who preferred to participate in the study via telephone was obtained from the sign-up form or by having the patient give permission to the community partner contact person to share their contact information with the research team. Once telephone contact information for a participant was received, a research assistant (RA) attempted to contact the patient via telephone a maximum of 9 times. Each community partner was given CA$50 in appreciation of their assistance with recruitment. Participants were given CA$15 in appreciation of their time.
Analysis
Regular team meetings occurred throughout the recruitment period. Notes were recorded about the management of the recruitment process. In addition, field notes were recorded by all RAs involved in the data collection process. Content analysis was conducted on these team meeting and field notes, focusing on issues related to the data collection process. Financial analysis was conducted on monetary resources spent on recruitment efforts in the various communities. Data were recorded regarding the number of times potential participants were contacted and the mode of interview. Descriptive statistics were conducted to examine whether there were differences according to mode of data collection, gender, and FN status. In order to examine the association between FN status and mode of data collection, Mantel-Haenszel common odds ratio estimates were conducted using SPSS (www-01.ibm.com/software/analytics/spss). Also conducted was a logistic regression to examine whether FN status remained statistically significant even after controlling for sex, education, employment status, age and health status.
A total of 398 people expressed initial interest in participating in the study. Once they were contacted, there was a 68% participation rate with 269 people (n=90 men, n=179 women) completing the survey. Of those who participated in the survey, 42% were from FN communities. Reasons for not participating included: not providing contact information or providing inaccurate contact information; declining prior to starting or mid-way through the survey; or inability to participate as a result of illness or death. In addition, a number of patients who did not participate continuously expressed interest in the study but were unable to participate due to being 'too busy'.
Content analysis: communication and coordination
The research team consisted of a large group of RAs as well as the investigators and decision-makers. The research team, its community partners, and the communities were geographically dispersed. Not surprisingly, the project required multiple modes of communication to assist coordination of the research team and community partners and for administering the surveys to patients. Content analysis showed that email was used extensively among researchers. Asynchronous communication through email allowed the team to carry out the tasks needed to complete the multiple ethics applications while working across dispersed geography. Synchronous communication, using teleconference and SkypeTM (voice over internet) for weekly team meetings, helped ensure that everyone was kept up-to-date of any changes in the project (eg transitions in community partners or upcoming events such as health fairs to recruit participants).
Telephone communication with community partners was crucial because not all clinics or community partners had regular access to or regularly used email. Moreover, although patients provided email addresses as a means of contact, the majority did not return email sent by the RAs. Over half of the survey data (54%) were collected by telephone. Skype was utilized in lieu of the telephone when possible because it was a cost-free alternative. Honoraria were sent in the form of money orders through registered mail to community partners who distributed them to participants who completed a survey. The signed receipts were faxed back to the research team.
Flexibility: tailoring recruitment strategies
Considerable time was required for building and maintaining relationships with community partners and also for traveling to recruit participants and administer surveys on-site. The research team used different strategies based on community partners' input for each study site. Strategies included: attending health fairs, attending GMVs to present the study and offering lunches to community residents to help gather all interested patients in a central location. Research team members were flexible in their recruitment approaches, following the direction of their community partners who understood their communities' contexts.
In FN communities, a history of colonization, continued inequities in health care, and a perception of being over-researched with little apparent benefit, resulted in some distrust in the value of the study37,38. For these reasons, attaining equity in recruitment required researchers and RAs to have competency with regard to FN cultures, sensitivity to distinct community circumstances, as well as confidence and tact in order to resolve unexpected misunderstandings as they arose.
First Nations community clinics often employ one or more staff members from the community to liaise between clinic and community, and outside visitors, such as researchers. The boundary between clinic and community is more permeable than in an urban centre: the clinic setting is a part of the community, and so visits to the clinic should be as respectful as when visiting a community member's home. Trust and relationship-building was reinforced by gestures of reciprocity, such as bringing food for clinic staff and community members when researchers expected to garner survey data. Assisting with set-up and break-down of the area used for research activities, such as stacking chairs and washing dishes, fostered engagement between researchers, staff, and community members, and reinforced the likelihood of return visits by researchers being welcomed.
At times, flexibility was required to accommodate the needs of individual community members, such as interviewing an Elder in their home. Conversely, it was also important for researchers to treat with sensitivity circumstances that may be indicative that a return visit should be postponed or avoided, for example a funeral in the community, or the perception that the community or clinic staff may feel over-researched or over-extended.
In trying to ensure all those interested in the study were able to participate, an RA was available to administer a telephone interview at varying times of the day, early evening hours, and also on weekends. While the telephone offered a flexible way to administer the survey, some participants, particularly those in smaller communities, did not own a phone. Some participants provided a phone number at a community centre, a local supermarket, or a neighbor's house, where it was difficult or impossible to reach them.
Factors that the RA needed to consider when traveling to the communities included: being prepared for challenges such as running out of fuel and having no cell phone coverage; the amount of time required for transit; the safety issues associated with driving on icy roads where animals crossing the road is a frequent occurrence; and last minute changes in plans for reasons given above. Moreover, problem-solving skills were required to successfully navigate field work in rural communities where running out of blank surveys with no place to make additional copies left community members discontented because they had traveled to participate.
Descriptive analysis
If initial contact was made in a telephone call, the RA mainly arranged a time, mode of interview, and date that would be most convenient for the participant to complete the survey. Over half of the participants completed the survey by telephone on the first phone call, with a number of follow-up calls made in an attempt to contact all who expressed initial interest (Table 1). Over two-thirds of participating men completed the survey after initial contact. Participation rates by both men and women substantially decreased after four contact attempts.
Table 1: Contact attempts
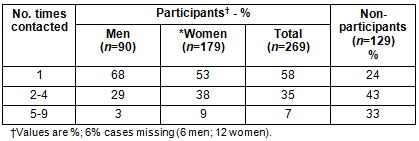
Approximately two-thirds of FN participants were women (63%) and over two-thirds of non-FN participants were women (68%). Significantly more participants (54%) opted to complete the survey by telephone (p<0.01; Table 2). In the whole sample, more men (59%) and fewer women (27%) completed the survey in person (p<0.05). More FN men and women completed surveys in person rather than completing the survey by telephone. Even after controlling for sex, education, employment status, age and health status, FN respondents were less likely to complete the survey by telephone compared with non-FN respondents (odds ratio=3.45, 95% confidence interval: 1.79-6.67), perhaps reflecting limited local access to phones.
Table 2: Mode of Interview
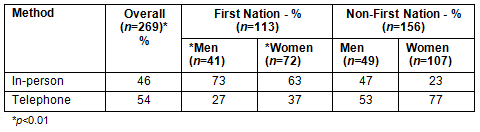
Distribution of financial resources
Attention was paid to equity in recruitment in relation to the time and resources expended for recruitment in the different communities. In part, the recruitment strategies were tailored according to input from community partners. However, some rural communities required more travel time compared with recruiting participants from communities where there was direct geographic access by road or air. For some communities, research team members flew to a central location and then drove for 2 to 4 hours. To access other communities two flights or ferry trips were required. Many of these rural areas had limited cell-phone coverage, making travel to and from more challenging logistically. Costs also varied depending on whether an RA lived closer to participating communities. Research team members from UBC and UNBC had to travel longer distances to reach remote communities, which cost up to 17 times more than traveling to areas located closer to Prince George. In the study, a total of CA$14,000 was spent on travel to the various communities, where most of the costs were associated with transportation (44%) followed by meals (13%) and accommodation (13%). Not surprisingly, more resources were spent traveling to the places farthest from Prince George.
Discussion
Ensuring equity in recruiting research participants from rural and FN communities, particularly across geographically dispersed settings, poses challenges to researchers. The results of this study are unique because it closely examined possible bias in FN and rural community recruitment, and proposed pragmatic strategies for improving equity in recruiting. The results suggest that increased investment of time and financial resources are required to ensure that participants from the most rural and from FN communities can participate in research. Evidence from this study suggests that nurturing relationships with community partners, using a blend of face-to-face interaction with them and reliance on multiple forms of technology were required. Undertaking multiple strategies, particularly with a geographically distributed research team, can enable researchers to strive towards including diverse perspectives. Tailoring recruitment methods can be supported by the research team being flexible and conscientious to the context-specific needs of each community.
Establishing and developing relationships with community partners, especially in rural and FN communities, is critical to successful primary data collection. The successful engagement of community partners and key contact people within these communities requires trusting relationships, respect, and honest, open, and constructive communication39. Where the research team had ongoing communication with the community partner, information exchange and data collection flowed more rapidly. Community partners were a bridge between the research team and the community residents. Having 42% of the sample include FN perspectives can be attributed to the engagement of community partners.
A high-functioning research team is needed when working across multiple communities. Importantly, while problem-solving skills may not be part of staff orientation, these skills are necessary in order to work within community contexts. Moreover, in order to carry out this kind of research, staff must also have strong technological skills40. Similar to Valaitis et al's41 experience in working with a geographically distributed team, an essential aspect of this dispersed research team was establishing a central place to overseeing communication processes and organizing the distribution of research materials and honorariums. Finally, having RAs cognizant with rural and FN community dynamics as the point of contact for each community enhanced communication and promoted continuity.
Limitation
This work is limited in that not all communities in NH who were offering GMVs were able to participate. Those who participated made up a convenience sample and therefore may not be representative of the more general rural and reserve population. Caution should be used in interpreting analysis of the survey results since the mode of recruitment by FN status needs to be taken into account. The recruitment strategies, however, were based on input from community partners. Future work needs to ensure equitable recruitment strategies and ability to more widely generalize to similar rural and Aboriginal populations.
Striving toward equity in recruitment of research participants in rural and FN communities is important. Their input into health research can be used to transform the delivery of health services in these areas. Yet research with these communities, particularly across geographically dispersed settings, poses challenges. Traveling across large geographic distances is time-consuming and costly; coordinating communication with a large virtual research team requires patience and cooperation; and the long length of this project required adapting to changing RAs and their schedules. Such issues require a commitment of substantial financial resources. However, it is important to continue to conduct such research to examine inequities in health services delivery by including the people that are most affected by the inequities, such as those living in rural communities, FN populations, and those living with multiple chronic illnesses, because evidence shows that current PHC services are not meeting their needs7,16, leading to worse health outcomes. While perhaps more costly, research that ensures participation opportunities for rural and FN communities is likely to better inform effective strategies to meet the needs of these communities, and to deliver more cost-effective care.
Acknowledgements
The authors thank their community partners and patients who took the time to participate in this study. They also thank the primary care practices, Northern Health Authority employees and communities, and other research assistants Meck Chongo, John Atkinson, and Anthony Gagne who made this work possible.
References
1. Northern Health Authority. 2011/12-2013/14 Service Plan. Prince George, BC: Northern Health Authority, 2011; 1-23.
2. Foster LT, Keller CP. The British Columbia Atlas of Wellness, 1st edn. Victoria, BC: University of Victoria, 2007; 1-10.
3. Watson DE, Mooney D, McKendry R, Martin D, McLeod C, Regan S et al. On the road to renewal: mapping primary health care in British Columbia. Vancouver, BC: Centre for Health Services and Policy Research, 2009.
4. DesMeules M, Pon R, Lagacé C, Heng D, Manuel D, Pitblado R et al. How healthy are rural Canadians? An assessment of their health status and health determinants. Ottawa, ON: Canadian Institute for Health Information, 2006.
5. Hutchison B, Levesque J-F, Strumpf E, Coyle N. Primary health care in Canada: systems in motion. Milbank Quarterly 2011; 89(2): 256-288.
6. Aggarwal M, Hutchison B. Toward a primary care strategy for Canada. In: Canadian Working Group for Primary Healthcare Improvement. Ottawa, ON: Canadian Foundation for Healthcare Improvement, 2012.
7. British Columbia Provincial Health Officer. Pathways to health and healing. Second report on the health and well-being of Aboriginal people in British Columbia. In: Provincial Health Officer's Annual Report 2007. Victoria, BC: Ministry of Healthy Living and Sport, 2009.
8. Browne AJ, Smye V, Rodney P, Tang SY, Mussell B, O'Neil JD. Access to primary care from the perspective of Aboriginal patients at an urban emergency department. Qualitative Health Research 2011; 21(3): 333-348.
9. Adelson N. The embodiment of inequity: health disparities in aboriginal Canada. Canadian Journal of Public Health/Revue Canadienne de Santé Publique 2005; 96(Suppl2): S45-S61.
10. Haskell L. Disrupted attachments: a social context complex trauma framework and the lives of Aboriginal peoples in Canada. Journal of Aboriginal Health 2009; 5: 48-99.
11. Minister of Public Works and Government Services. International covenant on economic, social and cultural rights. (Online) 2005. Available: http://www.pch.gc.ca/eng/1356367526364/1356368123623 (Accessed 1 May 2013).
12. Braveman PA, Kumanyika S, Fielding J, Laveist T, Borrell LN, Manderscheid R et al. Health disparities and health equity: the issue is justice. American Journal of Public Health 2011; 101(Suppl 1): S149-S155.
13. United Nations. The right to the highest attainable standard of health. (Online) 2000. Available: http://www.unhchr.ch/tbs/doc.nsf/%28symbol%29/E.C.12.2000.4.En (Accessed 6 May 2013).
14. Lavoie JG, Forget EL. The cost of doing nothing: implications for the Manitoba Health Care. Pimatisiwin: A Journal of Aboriginal and Indigenous Community Health 2008; 6: 105-119.
15. Lavoie JG, Forget EL, Browne AJ. Caught at the crossroad: First Nations, health care, and the legacy of the Indian Act. Pimatisiwin: A Journal of Aboriginal and Indigenous Community Health 2010; 8: 83-100.
16. Lavoie JG, Gervais L. Access to primary health care in rural and remote Aboriginal communities: progress, challenges and policy directions. In: J Kulig, A Moss (Eds); Rural health: a Canadian perspective. Vancouver, BC: UBC Press, 2011.
17. Kulig JC. Rural health research in Canada: assessing our progress. Canadian Journal of Nursing Research 2010; 42(1): 7.
18. Pong RW, DesMeules M, Read Guernsey J, Manuel D, Kazanjian A, Wang F. Health services utilization in rural Canada: are there distinct rural patterns? In: J Kulig, AM Williams (Eds); Health in Rural Canada. Vancouver, BC: UBC Press, 2011: 60-82.
19. Clarke HF. Research in nursing and cultural diversity: working with first nations peoples. Canadian Journal of Nursing Research 1997; 29(2): 11.
20. Corbie-Smith G, Thomas SB, St. George DMM. Distrust, race, and research. Archives of Internal Medicine 2002; 162(21): 2458-2463.
21. Ejiogu N, Norbeck JH, Mason MA, Cromwell BC, Zonderman AB, Evans MK. Recruitment and retention strategies for minority or poor clinical research participants: lessons from the Healthy Aging in Neighborhoods of Diversity across the Life Span study. Gerontologist 2011; 51(Suppl 1): S33-S45.
22. Carroll JK, Yancey AK, Spring B, Figueroa-Moseley C, Mohr DC, Mustian KM et al. What are successful recruitment and retention strategies for underserved populations? Examining physical activity interventions in primary care and community settings. Translational Behavioral Medicine 2011; 1(2): 234-251.
23. Nicholson LM, Schwirian PM, Klein EG, Skybo T, Murray-Johnson L, Eneli I et al. Recruitment and retention strategies in longitudinal clinical studies with low-income populations. Contemporary Clinical Trials 2011; 32(3): 353-362.
24. UyBico SJ, Pavel S, Gross CP. Recruiting vulnerable populations into research: a systematic review of recruitment interventions. Journal of General Internal Medicine 2007; 22(6): 852-863.
25. Yancey AK, Ortega AN, Kumanyika SK. Effective recruitment and retention of minority research participants. Annual Review of Public Health 2006; 27: 1-28.
26. Tang SY, Browne AJ. 'Race' matters: racialization and egalitarian discourses involving Aboriginal people in the Canadian health care context. Ethnicity & Health 2008; 13(2): 109-127.
27. Government of Canada. TCPS 2-2nd edition of tri-Council policy statement: ethical conduct for research involving humans. (Online) 2011. Available: http://www.pre.ethics.gc.ca/eng/policy-politique/initiatives/tcps2-eptc2/Default/ (Accessed 6 May 2013).
28. Government of Canada. Indian Act. R.S.C., 1985, c. I-5. (Online) 2013. Available: http://laws-lois.justice.gc.ca/eng/acts/I-5/page-1.html#h-2 (Accessed 6 May 2013).
29. Noffsinger EB. The drop-in group medical appointment model: a revolutionary access solution for follow-up visits. New York, NY: Springer, 2009; 21-67.
30. Carlson B. Shared appointments improve efficiency in the clinic. Managed Care 2003; 12(5): 46.
31. Miller D, Zantop V, Hammer H, Faust S, Grumbach K. Group medical visits for low-income women with chronic disease: a feasibility study. Journal of Women's Health 2004; 13(2): 217-225.
32. Trento M, Passera P, Tomalino M, Bajardi M, Pomero F, Allione A et al. Group visits improve metabolic control in type 2 diabetes: a 2-year follow-up. Diabetes Care 2001; 24(6): 995-1000.
33. Wong ST, Peterson S, Black C. Patient activation in primary healthcare: a comparison between healthier individuals and those with a chronic illness. Medical Care 2011; 49(5): 469-479.
34. Primary Health Care. Pan-Canadian primary health care indicators. (Online) 2011. Available: http://www.cihi.ca/CIHI-ext-portal/pdf/internet/INFO_PHC_INDICATORS_EN.pdf (Accessed 6 May 2013).
35. Haggerty J. Operational definitions of attributes of primary health care: consensus among Canadian experts. Annals of Family Medicine 2007; 5(4): 336-344.
36. City of Prince George. Official Host City - 2015 Canada Winter Games. (Online) 2011. Available: http://princegeorge.ca/Pages/default.aspx (Accessed 6 May 2013).
37. Brunger F, Bull J. Whose agenda is it? Regulating health research ethics in Labrador. Intellectual Property and Ethics 2011; 35(1-2): 127-142.
38. Stoddart ML, Jarvis B, Blake B, Fabsitz RR, Howard BV, Lee ET et al. Recruitment of American Indians in epidemiologic research: the Strong Heart Study. American Indian and Alaska Native Mental Health Research 2000; 9: 20-37.
39. Ramsden VR, McKay S, Crowe J. The pursuit of excellence: engaging the community in participatory health research. Global Health Promotion 2010; 17(4): 32-42.
40. Moffitt PM, Mordoch E, Wells C, Martin Misener R, McDonagh MK, Edge DS. From sea to shining sea: making collaborative rural research work. Rural and Remote Health 9(2): 1156. (Online) 2009. Available: www.rrh.org.au (Accessed 6 May 2013).
41. Valaitis R, Martin-Misener R, Wong ST, MacDonald M, Meagher-Stewart D, Austin P et al. Methods, strategies and technologies used to conduct a scoping literature review of collaboration between primary care and public health. Primary Health Care Research and Development 2012; 13(3): 1-18.

