Dear Editor
Uganda, with a population of around 32 million people and a life expectancy at birth of 48 years for men and 57 years for women, is a country in sub-Saharan Africa with significant public health concerns1. An attempt was made to determine the priorities for a simple, evidence-based public health strategy to improve eye health in Mannya, a rural town in Uganda with very limited resources. Mannya is situated in South Western Uganda near the Tanzanian border. There is one healthcare facility in the town, which has an estimated population of 12 000 inhabitants. No ophthalmic services are in place either in Mannya or in any surrounding town. The nearest optometrist service is a 1-hour drive away in Rakai, while the nearest ophthalmological service is 135 km (a 3-hour drive) away, based at Ruharo Hospital.
Visual impairment is a significant public health problem across the world. Recent WHO estimates suggest approximately 314 million people are visually impaired globally, of whom 45 million are blind2. Importantly, 80% of this visual impairment is preventable or treatable, thus creating the impetus for a public health approach to addressing visual impairment2. In rural Uganda almost 5% of the population has been found to be visually impaired in a large population study of more than 4000 adults aged 13 years and over3.
Globally, the leading cause of visual impairment is uncorrected refractive error, with approximately 153 million people affected4. Visual impairment is defined as visual acuity < 6/18 in the better eye with current correction4. The leading causes of blindness are cataract (39%), uncorrected refractive errors (18%), glaucoma (10%), age-related macular degeneration (7%), corneal opacity (4%) and diabetic retinopathy (4%)2.
A survey was performed of patients self-presenting to the medical facility in Mannya with any eye condition or complaint. Eighty seven (87) patients were assessed. Assessment included visual acuity and a dilated fundus examination. Of the patients seen, 75% presented with reduced visual acuity. Of those with reduced visual acuity, the main causes were cataract (33%) and refractive error (30%) (defined as an improved visual acuity with pinhole). Glaucoma was the third leading cause of poor vision, responsible for 15% of cases.
The remaining 25% of patients presented with ocular symptoms such as irritation, but normal visual acuity. The majority of these cases were due to various forms of conjunctivitis (60%) and dry eye (20%).
An attempt was made to rationalize the priorities for the eye strategy. Priority was determined based on three factors: potential impact on visual acuity, ease of an intervention and disease burden (Fig1). This was particularly important given the limited resources available. We defined a high impact on visual acuity occurring if the visual acuity could be improved significantly by an intervention. Thus interventions such as correcting refractive error and cataracts were given high impact scores since they can improve acuity to normal/near-normal levels. In contrast, adequate treatment of glaucoma can prevent ongoing visual loss but does not restore vision loss that has already occurred due to glaucoma. Ease of intervention was determined based on both the resources required and the impact on a patient's lifestyle. Correction of refractive error was determined to be relatively 'easy', since this requires spectacle correction only. This is non-invasive and can be performed by optometrists and technicians, particularly given recent advances in autorefractor technology and ready-made spectacles5. Cataract surgery requires surgical expertise and equipment, but is a single quick procedure that can be performed in a cost-effective manner. In most cases glaucoma can be managed with long-term use of topical medications, but this is a chronic disease requiring regular intraocular pressure checks and dilated assessments of the optic nerve head.
Addressing refractive error was determined to be the first priority, as shown in Figure 1. The options for addressing refractive error are numerous and are beyond the scope of this piece, but the mainstay of treatment is spectacle correction. The second priority is the provision of cataract surgery, which is currently unavailable in the region. In general, the need for cataract surgery (the cataract surgery rate (CSR)) has been estimated at 2000-5000 cataract operations per million persons, per year6. In most of sub-Saharan Africa the CSR is less than 5007. Clearly, challenges exist to the provision of efficient and effective cataract surgery in the region.
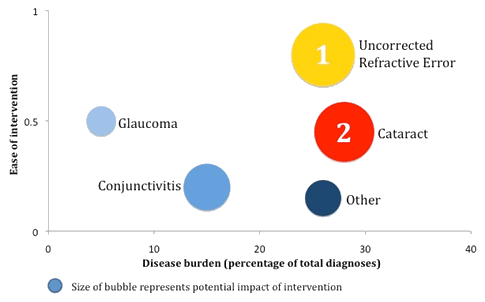
Figure 1: Priorities for intervention, Mannya, 2011.
In any public health strategy it is important to consider prevention of disease, as well as treatment options. Refractive error as yet cannot be effectively prevented. Only the minority of cataracts are due to secondary causes such as trauma. Most cataracts are 'age related' and the only prevention strategies include limiting exposure to UV-B radiation and stopping smoking8. Prevention of visual loss due to glaucoma would require early diagnosis and treatment and may be an important additional aspect to the public health strategy.
This study has allowed two clear priorities to address eye health to be determined. It is based on local information, which has been shown to be consistent with the international evidence base. One limitation of the study is the possible bias in the selection of patients for assessment since the patients self-presented for assessment. Further research is needed to determine how to most effectively address these two issues.
Alexander Hamilton
Ophthalmology registrar
Sydney Eye Hospital
Sydney, New South Wales, Australia
Sven Richter
Medical officer
Mannya Health Centre
Mannya, Uganda
References
1. World Health Organization. World Health Organization country statistics: Uganda. (Online). Available: http://www.who.int/countries/uga/en/ (Accessed 29 January 2012).
2. World Health Organization. WHO action plan for the prevention of avoidable blindness 2009-2013. (Online) 2010. Available: http://www.who.int/blindness/ACTION_PLAN_WHA62-1-English.pdf (Accessed 29 January 2012).
3. Mbulaiteye S, Reeves B, Karabalinde A, Ruberantwari A, Mulwanyi F, Whitworth J et al. Evaluation of E-optotypes as a screening test and the prevalence and causes of visual loss in a rural population in SW Uganda. Ophthalmic Epidemiology 2002; 9: 251-262.
4. Resnikoff S, Pascolini D, Mariotti S, Pokharel G. Global magnitude of visual impairment caused by uncorrected refractive errors in 2004. Bulletin of the World Health Organization 2008; 86: 63-70.
5. Shane T, Knight O, Shi W, Schiffman J, Alfonso EC, Lee R. Treating uncorrected refractive error in adults in the developing world with autorefractors and ready-made spectacles. Clinical & Experimental Ophthalmology 2011; 39: 729-733.
6. Lewallen S, Roberts H, Hall A, Onyange R, Temba M, Banzi J et al. Increasing cataract surgery to meet Vision 2020 targets; experience from two rural programmes in East Africa. British Journal of Ophthalmology 2005; 89: 1237-1240.
7. Foster A. Cataract and "Vision 2020 - the right to sight" initiative. British Journal of Ophthalmology 2001; 85: 635-637.
8. Brian G, Taylor H. Cataract blindness - challenges for the 21st century. Bulletin of the World Health Organization 2001; 79: 249-256.

