The prevalence of overweight and obesity in Canada has increased drastically in the past 20 years1. According to current data, 44% of off-reserve Canadian Aboriginal youth aged 12 to 17 years are overweight and 20% are obese, and this is far higher than the national average2. A decline in traditional lifestyles contributes to the problem as it is characterized by reduced levels of physical activity and an increased reliance on market foods3,4. However, these changes do not fully explain the recent rise in rates of overweight and obesity.
Concurrent with the obesity epidemic, a reduction in sleep duration among adults and youth has been observed5-8. Throughout adolescence, sleep needs remain relatively constant at approximately 9 hours per night9. Several reviews confirm an inverse linear relationship between sleep duration and risk of overweight and obesity in youth10-14. This relationship may be stronger among boys than girls11,13, and tends to weaken with age13,15,16. Inadequate sleep has been linked to obesity via disruption in energy balance; including changes in appetite hormones leading to energy dense food choices, insulin resistance, decreased energy expenditure due to sleepiness, and increased waking hours available for eating8,17,18.
Longitudinal studies have shown a reduction in physical activity levels among youth in favor of sedentary pass-times, for example television, computer/video games, and internet use (screen time, collectively)19. Between 1988 and 2004, time spent watching television among Canadian youth remained relatively constant (9 hours weekly), while in 2004 an increase in video gaming and computer use (less common in 1988) accounted for an average of 20 hours of total weekly screen time2. Canadian Aboriginal youth are more likely to be 'high' television watchers than non-Aboriginal youth; almost half watch at least 15 hours per week20. Screen time is also significantly higher among youth with a television in their bedroom21-23. This is of concern as the positive association between screen time and obesity is well documented24. Proposed mechanisms include displacement of physical activity25,26; increased energy intake (snacking, influence of food advertisements)27-29; and reduced resting metabolic rate related to physical inactivity30. In view of recent trends in obesity and sedentary activity, current Canadian guidelines recommend limiting screen time to no more than 2 hours per day31.
Shortened sleep and increased screen time may coexist, for example television viewing habits have been shown to influence sleep patterns32,33. Youth who spend more time watching television tend to have shorter sleep durations33,34, as do those who have a television in their bedroom35. There is little research on the contribution of sleep habits and television viewing to the prevalence of overweight and obesity in on-reserve Aboriginal youth in Canada. This study examined the relationships between sleep, screen time habits and body mass index (BMI) in a convenience sample of on-reserve First Nation (FN) youth in northern and southern Ontario, Canada.
Study design and population sampling
This was an observational population-based study of cross-sectional design. Self-reported dietary and lifestyle information were collected from convenience samples of youth aged ten to 18 years between at various time points between October 2004 and June 2010 in the school setting, using the Waterloo Web-based Eating Behavior Questionnaire (WEB-Q)36. This study included five northern, remote (distant from major urban centers), isolated (not readily accessible by land) FN communities (reserves) of the western James Bay and Hudson Bay region (Moose Factory, Fort Albany, Kashechewan, Attawapiskat, and Peawanuck FNs) and one southern non-remote FN community (Christian Island) in Ontario, Canada. The northern communities are accessible only by plane year-round and by ice road in winter months. Participation was voluntary and the sample included all students in grades 6 to 10 attending local community schools who were present at the time of data collection; no students were excluded for any reason. Youth in the communities are generally of FN heritage. Data collection times were planned to coincide with those when most students would be in school and often took place over at least 2 days in an attempt to increase participation (students absent on one day could complete the survey on a subsequent day). Further, because travel to the remote communities is time and resource intensive, data collection was scheduled to coincide with planned trips to the communities for a variety of projects that corresponded with the research team's evolving relationship with communities in the region. Thus, data collection spanned a long time period.
Culturally appropriate passive parental consent procedures were used. Participants' active consent was obtained following an introductory screen of the WEB-Q.
Survey methodology
The WEB-Q, developed by Hanning et al at the University of Waterloo, is a web-based tool used to collect self-reported school-day dietary information using a 24 hour recall36. In this study, the WEB-Q was also used to question participants on physical activity, leisure time activities, and various health perception and behavior questions. The WEB-Q has been validated in multi-ethnic grades 6 to 8 students in Ontario, and more recently in the FN community of Fort Albany, Ontario36.
Sleep habits
Questions regarding weekday sleep habits were included within the WEB-Q. Participants were asked 'What time do you usually go to bed on a school night?', with the following possible responses: (a) before 9 pm, (b) between 9 and 10 pm, (c) between 10 and 11 pm, (d) between 11 pm and 12 am, (e) between 12 and 1 am, and (f) after 1 am. Response categories were collapsed to 'before 10 pm', 'between 10 pm and 12 am', and 'after 12 am' to ensure adequate cell size counts for contingency analyses. Usual sleep duration was assessed with the question: 'How many hours of sleep do you usually get on a school night?', with the following possible responses: (a) more than 9 hours, (b) 7 to 8 hours, (c) 5 to 6 hours, (d) 3 to 4 hours, (e) less than 3 hours. Based on the established sleep needs of youth (9 hours per night)9, response categories were collapsed into 'greater than or equal to 9 hours', '4 to 8 hours', and 'less than 4 hours' to differentiate between adequate, somewhat inadequate and severely inadequate sleep.
Screen time
Questions regarding screen time were included within the WEB-Q. Participants were asked whether they had access to a computer and the internet at home, and whether they had a television in their bedroom ('yes' or 'no' responses). After-school screen time was assessed using the questions 'How many hours of television do you watch after school?' and 'How many hours do you spend using the internet or playing video games after school?', with the following possible answers: (a) 1 hour or less, (b) 1 to 2 hours, (c) 3 to 4 hours, (d) 5 to 6 hours, (e) 7 hours or more. Given the nature of the response categories, television and internet time could not be combined to determine total screen time. Responses refer specifically to leisure screen time, and not to productive screen time (eg for homework purposes), and are therefore likely an underestimate of total time spent on screen-based activities. However, the focus of the current study was leisure screen time as this is the activity that is most concerning. Productive screen time and sedentary activity (eg homework, reading) does not appear to be related to overweight and obesity37-39. Current Canadian Sedentary Activity Guidelines recommending limiting screen time to 2 hours or less per day31; responses were therefore categorized into 'less than or equal to 2 hours' and 'more than 2 hours'.
Participants were questioned about after-school physical activity using the question 'In the past week, how much of the time after school did you spend outside?', with the following possible responses: (a) almost none of the time, (b) some of the time, (c) most of the time, (d) all of the time. It was presumed that time outside would be spent being at least moderately active. They were also asked how many times in the past week they were physically active in the evening, with the possible responses: (a) none, (b) one time, (c) 2 to 3 times, (d) 4 to 5 times, (e) 6 to 7 times. These response categories were collapsed into 'none', '1 to 3 times', and '4 to 7 times'. Weekend effects were not assessed.
Anthropometric measurements
Demographic, as well as height and weight information was collected using the WEB-Q. Trained research assistants measured participants using a wall-mounted measuring tape; an analog scale was available for participants to measure their own weight. Individuals then imputed their height and weight information into the WEB-Q, and BMI was calculated electronically. This means that while participants had the opportunity to have their height and weight measured, data used in the analysis all represent self-reports based on these measurements. Despite the use of self-reports, since height and weight variables were directly measured prior to reporting, they are more likely to be accurate than usual self-reported values. Participants were classed as normal (includes underweight), overweight, or obese according to the International Obesity Task Force age- and gender-specific categories for children and youth40.
Statistical analyses
All analyses were conducted for the entire sample of respondents per question and by sex to account for possible differences in physical activity and sleep patterns. For each categorical variable, descriptive cross-tabulations and Pearson's χ² tests were used to compare any differences across the three BMI categories (normal, overweight, obese). Adjusted standardized residuals (ASRs) were used to determine the location of any significant variation from 'expected' values, based on the proportion of participants in the total sample by BMI and sex. Statistical Package for the Social Sciences (SPSS) software v19.0 (www.spss.com) was used for all statistical analyses; significance level was set a priori at p ≤0.05.
Ethics approval
Approval for the study was granted by Chief and Council (ie locally elected FN governing body) and/or Education Authority (similar to a school board) and/or participating school, and the University of Waterloo Office of Research Ethics (ORE#15402).
Participant characteristics
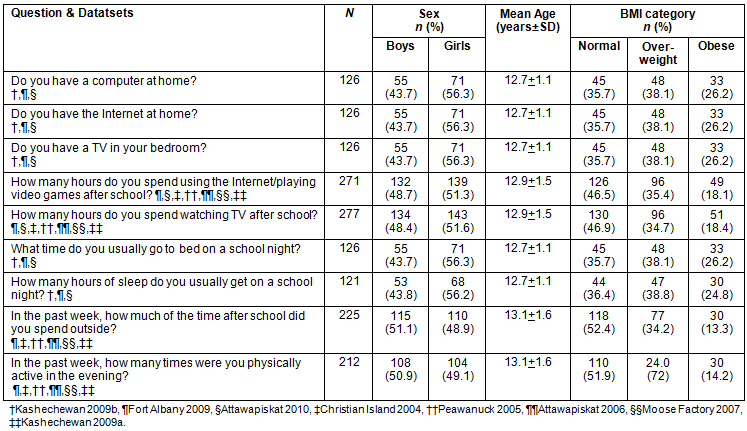
Participant characteristics are listed (Table 1). All students present on the day of the surveys completed the assessment. Datasets included in the analysis were Christian Island 2004 (n=38), Peawanuck 2005 (n=7), Attawapiskat 2006 (n=44), Moose Factory 2007 (n=67), Kashechewan 2009a (n=66), Kashechewan 2009b (n=42), Fort Albany 2009 (n=25), and Attawapiskat 2010 (n=59). A total of 348 participants were included in the study; however, since not all questions of interest were asked at each data collection, subsets of the total population were used for each analysis. Participants were excluded if they failed to answer the question of interest.
Table 1: Characteristics of study participants by question
Sleep, screen time and physical activity behavior
Frequency of responses to sleep, screen time, and after-school physical activity behavior questions are shown (Table 2); ASRs for each question are also shown (Table 3). A significant positive relationship between time using the internet or playing video games after school (p=0.022) and BMI, and a significant negative relationship for time spent outside after school (p=0.033) and BMI were found for boys only. Compared with the composition of the total sample, a higher than expected proportion of obese boys spent greater than 2 hours on the internet or playing video games daily (56.7%). The number of obese boys who reported spending 'most of the time' outside after school was less than expected (9.5%), while the number who spent only 'some of the time' outside was more than expected (61.9%). At the same time, the number of normal weight boys who spent only 'some of the time' outside after school was less than expected (26.7%). While not significant for the population as a whole, adjusted standardized residuals suggest a significantly lower proportion of obese individuals in the total population spent 'most of the time' outside after school than expected (16.7%). Although the relationship between having a television in the bedroom and BMI did not reach significance, for both the total population and boys alone, ASRs suggest a significantly higher than expected proportion of obese individuals had a television in their bedroom (66.7% in total population, 68.8% of boys).
Table 2: Frequency of sleep, screen time, and physical activity behavior responses by BMI category in First Nations youth
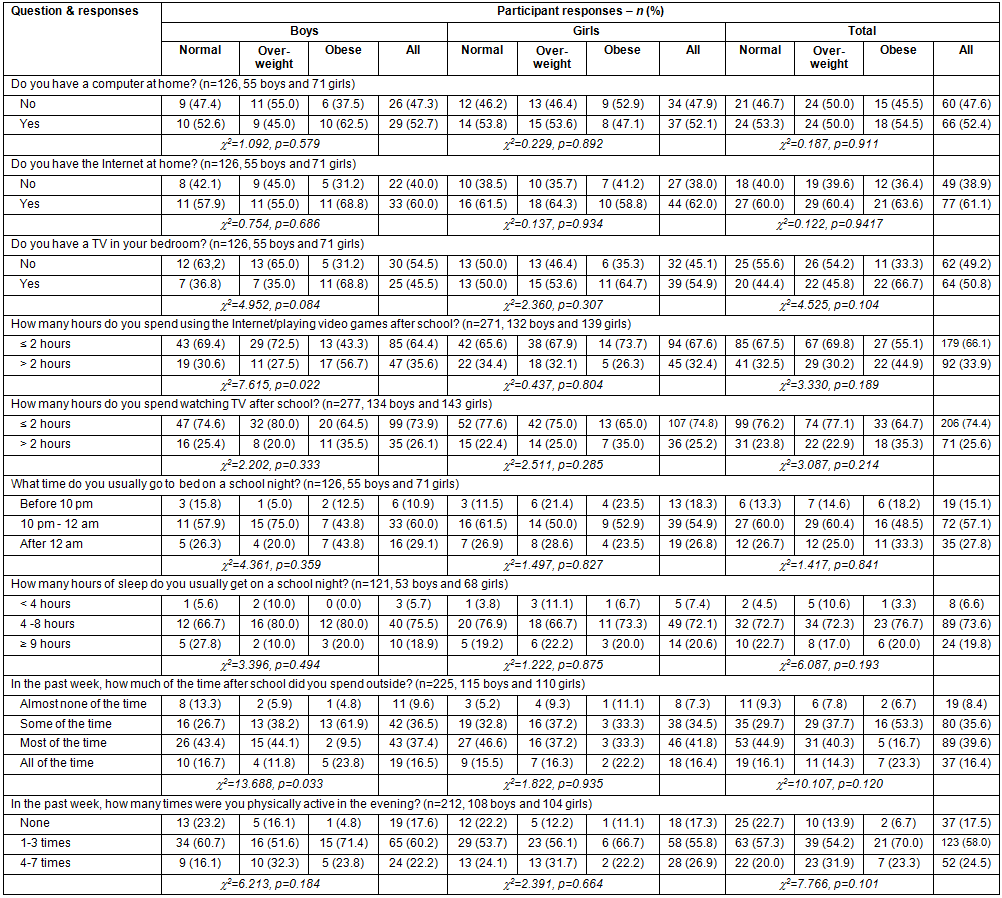
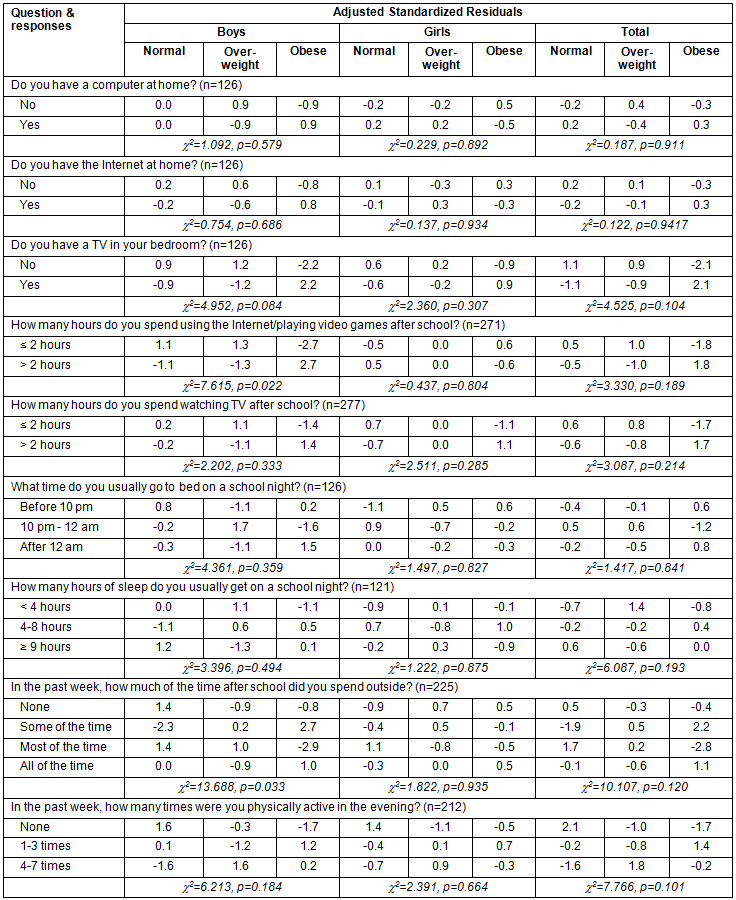
Table 3: Adjusted Standardized Residuals for sleep, screen time, and physical activity behavior by BMI category in First Nations youth
Discussion
The contribution of sleep and screen time behaviors have not been thoroughly investigated among on-reserve FN youth in Canada, and information for the general Aboriginal population (off-reserve) is scarce. The current study provides an initial investigation in a relatively small sample of on-reserve FN youth. The communities studied were small, all having a population of less than 2500 and the smallest, Peawanuck, having a population of less than 250. Though every effort was made to include as many youth as possible during data collection, small sample size is a known limitation of the current research. Nevertheless, the relationships explored add to the limited information on the potential associations between sleep, screen time, and BMI in on-reserve FN youth and provide a foundation for future research in larger samples.
In the sample of FN children and youth who answered questions about screen time, 74.4% reported watching 2 hours or less of television after school per day, while 66.1% reported spending 2 hours or less on the internet or playing video games. Nevertheless, this could amount to up to 3.9 hours of total screen time in some individuals. The available data included only after-school screen time and does not account for other times of the day. However, there remains 25.6% of youth watching more than 2 hours of television and one-third spending more than 2 hours playing video games or surfing the internet daily. Not surprisingly, this is a concern for FN youth across Canada as well as American Indian youth. Results of the First Nations Regional Health Survey, which provides information about the health of FN people in Canada (including those on-reserve) reports that 38.6% of FN youth spend more than 1.5 hours on sedentary activities each day, with 42.9% of boys and 12.7% of girls spending more than 1.5 hours/day on video games alone41. Among a sample of American Indian youth in California, 3.7 daily hours of television watching and 1.2 hours of computer use were reported42. In terms of the general Canadian population, the 2011 Active Healthy Kids Canada Report Card on Physical Activity for Children and Youth, based on information from the Canadian Health Measures Survey (2007-2009), indicates that youth spend an average 6 hours on screen time on weekdays43,44. In the present study, the large proportion of youth reporting more than 2 hours daily is of concern. The situation is worthy of being addressed given Canada's new Physical Activity Guidelines for Children and Youth which recommend limiting screen time to no more than 2 hours daily in order to minimize the health risks associated with excess sedentary behavior31.
The association between screen time and obesity is well known in the general population24, and high levels of screen time in the critical period of adolescence (as with the youth in our sample) is severely concerning, given that screen time independently and significantly predicts incident obesity later in life45. Further, recent evidence supports the notion that high levels of sedentary activity is associated with an increased risk of obesity and chronic disease, independent of physical activity levels30,33,46-48. In the current study, time spent playing video games and using the internet was found to be significantly associated with BMI category for boys, where a significantly higher proportion of obese boys (56.7%) spent more than 2 hours on the internet or playing video games daily relative to normal weight (30.6%) and overweight (27.5%) boys. This finding is consistent with the possible association between electronic game use and obesity suggested in the literature39,49-51. Many plausible explanations of the relationship have been discussed, including displacement of physical activity, reduced resting metabolic rate, and altered food consumption patterns such as increased consumption of total energy, fat and sugar25,29,30,33,38,52. Interestingly, the relationship between internet, video games, and BMI was not supported in girls in this study; it is possible that girls had less interest in video games and internet use than did boys, that the relationship in girls truly does not exist or that sample size was insufficient to detect a relationship. It should be noted that other sedentary behaviors (eg talking with friends) were not included in the survey, and could further influence sedentary time. It is possible that these types of activities may be more appealing to girls and contribute more substantially to sedentary activity. For example, the First Nations Regional Health Survey included activities such as reading and playing bingo41. Alternately, it is possible that the categorical nature of the response variables masks a difference in screen time between boys and girls. It is possible that within the equal to or greater than 2 hour/day category, boys are actually spending much more time on screen-based activity than girls, and this inactivity could correlate to excess weight. This is a plausible possibility given that it has been reported that FN boys in Canada are significantly more likely than girls to spend more than 1.5 hours per day on video games alone41.
Having a television in the bedroom has been pinpointed as a culprit for high levels of television viewing21-23,53 and increased risk of overweight in children54. In the current study, a high proportion (66.7%) of obese participants had a television in their bedroom, while a smaller (although still high) proportion of normal weight and overweight individuals reported having televisions in their bedroom (44.4% and 45.8%). This suggests a relationship between the presence of a television in the bedroom and being obese in this population. In the USA, a recent study reported that 43.9% of youth aged 6-17 years had a television in their bedroom55. The situation is likely to be similar in Canada, and an even higher proportion of youth with a television in the bedroom (66%) was found in the current sample of FN youth living in isolated communities. While not within the scope of the current study, the similarities between on-reserve FN youth and the general population is interesting and warrants further investigation. There currently exists too little information about the influence of having a television in the bedroom on television watching and obesity in Aboriginal youth to make a comparison.
Youth in the general population have had a decrease in physical activity levels in favor of sedentary activity19. In the current study, 56% of youth in the subset who answered questions regarding physical activity reported spending after school time outside 'most of the time' or 'all of the time'. Still, the vast majority (75.5%) reported being active in the evening three or less times per week; only 24.5% reported being active four-to-seven times per week (once every one-to-two days). Interestingly, when asked how many times they were active in the past week, a higher than expected proportion (22.7%) of normal-weight youth answered 'none'. This is of concern given that the new Canadian Physical Activity Guidelines recommend a minimum of 60 minutes daily of vigorous to moderate physical activity for children and youth aged 5 to 17 years56. Although after school is not the only time that youth have to spend in physical activity, the fact that a large proportion spent three or less evenings per week being physically active means that the remaining evenings are also likely to be spent being sedentary. This should not be surprising as physical inactivity is commonly reported in both Aboriginal and non-Aboriginal youth. The First Nations Regional Health Survey reported that 36.8% of boys and 51.3% of girls are considered inactive41, while in the USA, it has been reported that 37.2% of American Indian children and youth are inactive57. Among the general population of youth in Canada, only 9% of boys and 4% of girls meet the Canadian Physical Activity Guidelines44. According to Canada's new guidelines, more physical activity is better56, suggesting that steps should be taken to encourage increased after-school physical activity among the youth in this study. In the current study, a significant relationship was found between time spent being outside in the evening and BMI category in boys. Here, only 9.5% of obese boys reported spending 'most of the time' outside after school (less than expected), significantly lower than the proportion of normal weight (43.3%) and overweight (44.1%) youth reporting spending 'most of the time' being active after school. This parallels findings from the 2001-2009 Canadian Health Measures Survey, which studies the general population, showing that obese boys spend less time in physical activity than overweight and normal weight boys44. Similarly, weight was not a significant factor in the physical activity levels of girls44. The current findings are also congruent with both Canadian and American data showing that inactive Aboriginal and Native American youth are more likely to be obese than active youth20,58. Given the findings of the current study, and in light of the evidence of relationship between physical inactivity and obesity19,59,60, initiatives to increase physical activity levels among on-reserve FN youth are likely to be warranted.
Finally, the possible relationship between sleep time and BMI was explored. The relationship between short sleep duration and overweight and obesity has been demonstrated consistently10-14,17. In a nationally representative sample of children and youth aged 3 to 17 years in the USA, later bedtimes were also associated with being overweight15. In the sample of FN youth in the current study, this relationship was not supported, which is surprising. In a sample of Caucasian youth from Quebec, Canada, it was found that short sleep duration increased the odds of obesity even after adjusting for multiple confounders including socioeconomic variables, which would be expected to be different for FN people on-reserve, compared with the general population61,62. It is possible that other factors related to both sleep time and obesity need to be considered in this population. Likewise, it is possible that a true relationship does not exist for FN youth. A study of the correlations of various fitness and lifestyle measures to BMI in urban Native American youth yielded similar findings, in that there was no significant correlation between sleep time and BMI58. The National Sleep Foundation indicates that only one in five adolescents get the optimal nine hours of sleep on school nights63. Figures in the current study are similar, with only 19.8% of youth reporting sleeping at least 9 hours on a school night. The majority (73.6%) reported sleeping 5-8 hours nightly, with the remaining 6.6% sleeping 4 hours or less. More than half (57.1%) of youth reported going to bed between 10 pm and 12 am, with approximately one-quarter going to bed after 12 am. These results suggest that many of the on-reserve FN youth in this study may be experiencing sleep deprivation, which may result in excessive daytime sleepiness and hormonal changes, causing alterations in energy balance that can precipitate weight gain17. The inadequate sleep among youth in the current study is worthy of further attention given the established link between inadequate sleep and obesity.
Given the limited information on screen time and sleep behaviors of on-reserve FN youth in Canada, the current study lays a foundation for future research to clarify existing relationships among these factors and overweight and obesity. Consistent with patterns seen in the general population, youth in the current study demonstrated low levels of after-school physical activity and excess screen time relative to national guidelines. Both internet and video game screen time, as well time spent outside after school were associated with BMI category in FN boys, with obese individuals spending less time outside and more time in front of the screen than their non-obese counterparts. The same relationship was not found in girls; more study is needed to clarify what other sedentary activities or lifestyle factors may play a role for girls. Consistent with current literature, a greater than expected number of obese youth were found to have a television in their bedroom, suggesting a possible relationship. The current findings suggest a need for further investigation into the determinants of screen time and sleeping habits among FN youth, and possible initiatives to reduce screen time and increase physical activity levels to meet current guidelines, as well as to encourage adequate sleep among on-reserve FN youth.
Acknowledgments
The authors thank the FN communities for their participation in this research. They greatly appreciate those who assisted in data collection, and Alex Stephens for field transportation. This research was funded by the Canadian Institutes of Health Research, Canada's Research-Based Pharmaceutical Companies Health Research Foundation, Health Canada's First Nations and Inuit Health Branch, the Danone Institute of Canada, the Ontario Ministry of Research and Innovation, the Heart and Stroke Foundation of Ontario, and stipend support from CIHR Training Grant in Population Intervention for Chronic Disease Prevention: A Pan-Canadian Program (Grant #53893).
References
1. Sheilds M, Tjempkema M. Trends in adult obesity. Health Reports 2006; 17(3): 53-59.
2. Sheilds M. Overweight and obesity among children and youth. Health Reports 2006; 17(3): 27-42.
3. Kuhnlein HV, Receveur O, Soueida R, Egeland GM. Arctic Indigenous people experience the nutrition transition with changing dietary patterns and obesity. Journal of Nutrition 2004; 134(6): 1447-1453.
4. Swinburn BA, Caterson I, Seidell JA, James WPT. Diet, nutrition, and the prevention of excess weight gain and obesity. Public Health Nutrition 2004; 7(1A): 123-146.
5. Iglowstein I, Jenni OG, Molinari I, Largo RH. Sleep duration from infancy to adolescence: reference values and generational trends. Pediatrics 2003; 111(2): 302-307.
6. Cizza G, Skarulis M, Mignot E. A link between short sleep and obesity: building the evidence for causation. Sleep 2005; 28(10): 1217-1220.
7. Lauderdale DS, Knutson KL, Yan LL, Rathouz PJ, Hulley SB, Liu K. Objectively measured sleep characteristics among early-middle-aged adults - the CARDIA study. American Journal of Epidemiology 2006; 164(1): 5-16.
8. Van Cauter E, Knutson KL. Sleep and the epidemic of obesity in children and adults. European Journal of Endocrinology 2008; 159(Suppl 1): S59-S65.
9. Carskadon MA, Acebo C. Regulation of sleepiness in adolescents: update, insights, and speculation. Sleep 2002; 25(6): 606-614.
10. Cappuccio FP, Taggart FM, Kandala NB, Currie A, Peile E, Stranges S et al. Meta-analysis of short sleep duration and obesity in children and adults. Sleep 2008; 31(5): 619-626.
11. Chen X, Beydoun MA, Wang Y. Is sleep duration associated with childhood obesity? A systematic review and meta-analysis. Obesity 2008; 16(2): 265-274.
12. Marshall NS, Glozier N, Grunstein RR. Is sleep duration related to obesity? A critical review of the epidemiological evidence. Sleep Medicine Reviews 2008; 12(4): 289-298.
13. Patel SR, Hu FB. Short sleep duration and weight gain: A systematic review. Obesity 2008; 16(3): 643-653.
14. Nielson LS, Danielsen KV, Sørensen TIA. Short sleep duration as a possible cause of obesity: critical analysis of the epidemiological evidence. Obesity Reviews 2011; 12(2): 78-92.
15. Snell EK, Adam EK, Duncan GJ. Sleep and the body mass index and overweight status of children and adolescents. Child Development 2007; 78(1): 309-323.
16. Shi Z, Taylor AW, Gill TK, Tuckerman J, Adams R, Martin J. Short sleep duration and obesity among Australian children. BMC Public Health 2010; 10: 609-614.
17. Taheri S, Lin L, Austin D, Young T, Mignot E. Short sleep duration is associated with reduced leptin, elevated ghrelin, and increased body mass index. PLoS Medicine 2004; 1(3): e62.
18. Taheri S. The link between short sleep duration and obesity: we should recommend more sleep to prevent obesity. Archives of Disease in Childhood 2006; 91(11): 881-884.
19. Must A, Bandini LG, Tybor DJ, Phillips SM, Naumova EN, Dietz WH. Activity, inactivity, and screen time in relation to weight and fatness over adolescence in girls. Obesity 2007; 15(7): 1774-1781.
20. Ng C, Young TK, Corey PN. Associations of television viewing, physical activity and dietary behaviours with obesity in aboriginal and non-aboriginal Canadian youth. Public Health Nutrition 2010; 13(9): 1430-1437.
21. Robinson TN, Winiewicz DD, Fuerch JH, Roemmich JN, Epstein LH. Relationship between parental estimate and an objective measure of child television watching. International Journal of Behavioral Nutrition and Physical Activity 2006; 3: 43.
22. Van Zutphen M, Bell AC, Kremer PJ, Swinburn BA. Association between the family environment and television viewing in Australian children. Journal of Paediatrics and Child Health 2007; 43(6): 458-463.
23. Barr-Anderson DJ, van den Berg P, Neumark-Sztainer D, Story M. Characteristics associated with older adolescents who have a television in their bedrooms. Pediatrics 2008; 121(4): 718-724.
24. Swinburn B, Shelly A. Effects of television time and other sedentary pursuits. International Journal of Obesity 2008; 32(Suppl 7): S132-S136.
25. Jenvey VB. The relationship between television viewing and obesity in young children: a review of existing explanations. Early Child Development and Care 2007; 177(8): 809-820.
26. Rey-Lopez JP, Vicente-Rodriguez G, Biosca M, Moreno LA. Sedentary behaviour and obesity development in children and adolescents. Nutrition, Metabolism and Cardiovascular Diseases 2008; 18(3): 242-251.
27. Utter J, Neumark-Sztainer D, Jeffery R, Story M. Couch potatoes or french fries: are sedentary behaviors associated with body mass index, physical activity, and dietary behaviors among adolescents? Journal of the American Dietetic Association 2003; 103(10): 1298-1305.
28. Matheson DM, Killen JD, Wang Y, Varady A, Robinson TM. Children's food consumption during television viewing. American Journal of Clinical Nutrition 2004; 29(6): 1088-1094.
29. Lajous M, Chavarro J, Peterson KE, Hernández-Avila M, Lazcona-Ponce E. Screen time and adiposity in adolescents in Mexico. Public Health Nutrition 2009; 12(10): 1938-1945.
30. Salmon J, Bauman A, Crawford D, Timperio A, Owen N. The association between television viewing and overweight among Australian adults participating in varying levels of leisure-time physical activity. International Journal of Obesity and Related Metabolic Disorders 2000; 24(5): 600-606.
31. Tremblay MS, LeBlanc AG, Janssen I, Kho ME, Hicks A, Murumets K et al. Canadian Sedentary Behaviour Guidelines for Children and Youth. Applied Physiology, Nutrition, and Metabolism 2011; 36(1): 59-64.
32. Owens J, Maxim R, McGuinn M, Nobile C, Msall M, Alario A. Television viewing habits and sleep disturbance in school children. Pediatrics 1999; 104(3): e27.
33. Wells JCK, Hallal PC, Reichert FF, Menezes AMB, Araújo CLP, Victora CG. Sleep patterns and television viewing in relation to obesity and blood pressure: evidence from an adolescent Brazilian cohort. International Journal of Obesity 2008; 32(7): 1042-1049.
34. Padez C, Mourao I, Moreira P, Rosado V. Long sleep duration and childhood overweight/obesity and body fat. American Journal of Human Biology 2009; 21(3): 371-376.
35. Li H, Jin XM, Wu SH, Jiang F, Yan CH, Shen XM. The impact of media use on sleep patterns and sleep disorders among school aged children in China. Sleep 2007; 20(3): 361-367.
36. Hanning RM, Royall D, Toews J, Blashill L, Wegener J, Driezen P. Web-based food behaviour questionnaire: validation with grades six to eight students. Canadian Journal of Dietetic Research and Practice 2009; 70(4): 172-178.
37. Sisson SB, Church TS, Martin CK, Tudor-Locke C, Smith SR, Bouchard C et al. Profiles of sedentary behavior in children and adolescents: The US National Health and Nutrition Examination Survey, 2001-2006. International Journal of Pediatric Obesity 2009; 4(4): 353-359.
38. Danielsen YS, Júlíusson PB, Nordhus IH, Kleiven M, Meltzer HM, Olsson SJ et al. The relationship between life-style and cardio-metabolic risk indicators in children: the importance of screen time. Acta Paediatrica 2010; 100(2): 253-259.
39. Liou YM, Liou T-H, Chang L-C. Obesity among adolescents: sedentary leisure time and sleeping as determinants. Journal of Advanced Nursing 2010; 66(6): 1246-1256.
40. Cole TJ, Bellizi MG, Flegal KM, Dietz WH. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 2000; 320(7244): 1240-1243.
41. The First Nations Information Governance Centre. RHS Phase 2 (2008/10) Preliminary Results. Ottawa: ON: The First Nations Information Governance Centre, 2011.
42. Babey SH, Hastert TA, Wolstein J. Adolescent sedentary behaviors: Correlates differ for television viewing and computer use. Journal of Adolescent Health 2013; 52(1): 70-76.
43. Active Healthy Kids Canada. The Active Health Kids Canada 2011 report card on physical activity for children and youth. (Online) 2011. Available: www.activehealthykids.ca (Accessed 1 October 2011).
44. Colley RC, Garriguet D, Janssen I, Craig CL, Clarke J, Tremblay MS. Physical activity of Canadian children and youth: accelerometer results from the 2007 to 2009 Canadian Health Measures Survey. Health Reports 2011; 22(1): 15-23.
45. Boone JE, Gordon-Larsen P, Adair LS, Popkin BM. Screen time and physical activity during adolescence: longitudinal effects on obesity in young adulthood. International Journal of Behavioral Nutrition and Physical Activity 2007; 4: 26.
46. Jakes RW, Day NE, Khaw KT, Luben R, Oakes S, Welch A et al. Television viewing and low participation in vigorous recreation are independently associated with obesity and markers of cardiovascular disease risk: EPIC-Norfolk population-based study. European Journal of Clinical Nutrition 2003; 57(9): 1089-1096.
47. Mummery WK, Schofield GM, Steele R, Eakin EG, BrownWJ. Occupational sitting time and overweight and obesity in Australian workers. American Journal of Preventative Medicine 2005; 29(2): 91-97.
48. Tremblay MS, Colley RC, Saunders TJ, Healy GN, Owen N. Physiological and health implications of a sedentary lifestyle. Applied Physiology, Nutrition, and Metabolism 2010; 36(6): 725-740.
49. Mota J, Ribeiro J, Santos MP, Gomes H. Obesity, physical activity, computer use, and television viewing in Portuguese adolescents. Pediatric Exercise Science 2006; 18(1): 113-121.
50. Schneider M, Dunton GF, Cooper DM. Media use and obesity in adolescent females. Obesity 2007; 15(9): 2328-2335.
51. Garvalhal MM, Padez MC, Moreira PA, Rosado VM. Overweight and obesity related to activities in Portuguese children, 7-9 years. European Journal of Public Health 2007; 17(1): 42-46.
52. Van den Bulk J, Van Mierlo J. Energy intake associated with television viewing in adolescents, a cross sectional study. Appetite 2004; 43(2): 181-184.
53. Jones KE, Otten JJ, Johnson RK, Harvey-Berino JR. Removing the bedroom television set: A possible method for decreasing television viewing time in overweight and obese adults. Behavior Modification 2010; 34(4): 290-298.
54. Adachi-Mejia AM, Longacre MR, Gibson JJ, Beach ML, Titus-Ernstoff LT, Dalton MA. Children with a television in their bedroom at higher risk for being overweight. International Journal of Obesity 2007; 31(4): 644-651.
55. Sisson SB, Broyles ST, Newton RL, Baker BL, Chernausek SD. television s in the bedrooms of children: Does it impact health and behavior? Preventative Medicine 2011; 2(1): 104-108.
56. Tremblay MS, Warburton DE, Janssen I, Paterson DH, Latimer AE, Rhodes RE et al. New Canadian Physical Activity Guidelines. Applied Physiology, Nutrition, and Metabolism 2011; 36(1): 36-46.
57. Foulds HJA, Warburton DER, Bredin SSD. Systematic review of physical activity levels in Native American populations in Canada and the United States in the last 50 years. Obesity Reviews 2013; 14(7): 593-603.
58. Gray A, Smith C. Fitness, dietary intake, and body mass index of urban Native American youth. Journal of the American Dietetic Association 2003; 102(9): 1187-1191.
59. Stamatakis E, Hirani V, Rennie K. Moderate-to-vigorous physical activity and sedentary behaviours in relation to body mass index-defined and waist circumference-defined obesity. British Journal of Nutrition 2009; 101(5): 765-773.
60. Jimenez-Pavon D, Kelly J, Reilly JJ. Associations between objectively measured habitual physical activity and adiposity in children: systematic review. International Journal of Pediatric Obesity 2010; 5(1): 3-18.
61. Chaput JP, Lambert M, Gray-Donald K, McGrath JJ, Tremblay MS, O'Loughlin J et al. Short sleep duration is independently associated with overweight and obesity in Quebec children. Canadian Journal of Public Health 2011; 102(5): 369-374.
62. Statistics Canada. 2006 Census: Aboriginal Peoples in Canada in 2006: Inuit, Métis and First Nations, 2006 Census: Findings. (Online) 2012. Available: http://www12.statcan.ca/census-recensement/2006/as-sa/97-558/index-eng.cfm (Accessed 11 March 2013).
63. National Sleep Foundation. Sleep in America Poll. Washington, DC: Sleep in America Foundation, 2006.
