Introduction
Because the likelihood of successful defibrillation decreases rapidly within the first few minutes of a cardiac arrest1, the concept of nurse-initiated defibrillation becomes more important2,3. In recognition, several authors propose that all personnel whose occupations require them to perform cardiopulmonary resuscitation (CPR) should be trained to defibrillate4,5. In Australia, rural and remote areas are faced with crucial shortages of medical practitioners, this means nurses in these areas have to care for acutely ill people more often in the absence of medical or allied health support6. Coupled with this, frequently there are not enough advanced life support (ALS) qualified staff to cover all shifts7-9. In these settings, nurses initiate and maintain basic life support (BLS) until additional ALS or medical support arrive, usually from outside the hospital8,9. Indeed the more geographically isolated the hospital, the less likely that facility is to have 24 hour medical coverage, a nurse permitted to defibrillate or a defibrillator available9. Rural nurses are now in the vulnerable position of undertaking duties traditionally performed by the doctor. While the benefit of nurse-initiated defibrillation is not disputed, it is not known if the role will be embraced.
Although there is ample information to support the benefits of early defibrillation in the pre-hospital setting, there is little information on the use of defibrillators by nurses' in-hospitals. For example, the true effectiveness of resuscitation programs is not known, how well people retain what they learn (for example defibrillation) or even whether they will perform these skills in a true emergency remains unknown1. Hence, it is difficult to predict whether nurses will actually use a defibrillator in a cardiac arrest. Coady postulates that while nurse-initiated defibrillation programs may be meeting the objective of allowing more nurses to defibrillate, early defibrillation by nurses is not actually happening10. Our understanding of defibrillation beliefs of rural nurses in Australia is deficient. Increasing an understanding will assist in designing interventions that will promote successful defibrillation practices and, consequently, successful patient outcomes. Despite policy change within hospitals to allow nurses to defibrillate, currently there is no research that utilises a systemic theoretical approach to investigate the predictors of nurses' intentions to use a defibrillator. Exploring the determinants of attitudes and intentions toward early defibrillation may attain insight into early defibrillation intentions of nurses. Arguably, the Theory of Planned Behavior (TPB) is currently a dominant theoretical framework used to explain the relationship between attitudes and actions11-18. Hence this study incorporated the constructs and concepts of the TPB to elicit the defibrillation beliefs of nurses. These elicitation beliefs can then be used to develop items for subsequent questionnaire development. Consistent with the theory by eliciting nurses' beliefs, future quantitative studies can be implemented using survey instruments to determine the influence of these beliefs on defibrillation intentions and actions.
Theoretical framework
For a number of years social scientists have shown a growing interest in the relationship between attitudes and actions19. This interest led to the development the Theory of Reasoned Action (TRA) and TPB18-20. According to the TRA the immediate antecedent of any given behavior is the individual's intention to perform the behavior. A person's intentions are determined by their attitudes towards the behavior and their perception of whether or not persons important to them think that they should or should not perform the behavior (subjective norm). TRA is appropriate when the desired behavior is under a person's volitional control19. Because people do not have complete control over their behavior, in 1985 the TPB evolved from the TRA18. The TPB is essentially an extension of the TRA and adds perceived control as the third determinant of intention. The TPB is appropriate for behaviors that are both under volitional and non-volitional control. The TPB has been tested with a variety of health behaviors such as health-care workers glove use21, exercise22-25, smoking26-29, sunbathing30, alcohol use14, condom use31,32, low-fat diet33, getting hormone replacement therapy34 and attitudes toward providing care for suicidal patients35. Equally, the predictive power of TPB is well established in health psychology research12,36,37. The aim of this study is not to predict intentions but to utilise a theoretical framework to elicit a beginning understanding of the defibrillation beliefs of rural nurses.
Methods
This research was non-experimental and descriptive-exploratory in nature, incorporating focus group interviews and survey data. Exploratory research was chosen to investigate phenomena about which we know little or nothing, to identify variables for use in subsequent study and to generate hypotheses for subsequent quantitative research. Focus group interviews are a qualitative research method that involves a number of people with common experiences being interviewed by the researcher (or moderator) for the purpose of eliciting ideas about a specific topic and to develop questionnaire items38,39. Data collection by focus group interviews has been used extensively in market research, social science and health care research39,40. During the last decade focus group interviews have increased in popularity in nursing research 40 and have been successfully incorporated with the constructs of the TRA and TBA41,42.
Setting and site
The sites selected for this study were two acute care hospitals in rural Australia (RRMA Classification). Each of these hospitals was in located 'other rural areas' (RRMA Classification 5) in separate towns and had 25 and 30 beds.
Participants
Consistent with focus group discussions, a purposive sampling method was employed in order to elicit the target populations' salient beliefs. To ensure adequate group sizes, all nurses working in the selected hospitals were identified as the target sample and invited to participate in the study. Recruitment did not start until ethical approval was received. Following this, the researcher met with the Directors of Nursing (DONs) from each of the participating sites to outline the research and gain approval for access. Three focus group interviews were held. Because saturation of responses occurred, a fourth group was not conducted. While the intent of the study was not to generalise, rather to provide an understanding of a topic, transferability was facilitated through data saturation. Prior to commencing each focus group interview, participants were informed both verbally and in writing that they were under no obligation to participate and were advised they could withdraw their participation at any stage.
Instrument
Prior to the conduct of the focus groups a question guide was developed to focus and guide discussions41,42,43. Criteria developed by Ajzen and Fishbien provided the framework to guide the development of focus group questions18,19,43. Ajzen posits that an individual has the capability of holding six to nine salient beliefs at one given time. The open-ended format to elicit information about salient beliefs allowed participants to respond to the questions suggested by Ajzen. For this study the following focus group questions were asked of all participants:
- What are the advantages and disadvantages of you being able to use a defibrillator? (Behavioral beliefs)
- Who approves or does not approve of you being responsible for the use of defibrillators in your clinical area? (Normative beliefs)
- Can you identify any events that might influence your decision to use or not use the defibrillator if there was a cardiac arrest on your ward today? (Control beliefs).
While these questions were used to guide the discussions, the interviews remained flexible to clarify responses and probe topics identified by the participants.
Although focus group interviews can be used as a sole method of data collection, many authors use focus group interviews in conjunction with other methods39. The use of questionnaires can supplement transcripts by providing an accurate sense of who was in the group44. Subsequently, demographic data were collected using a survey. Information collected included participants' sex, career length, current level in the career structure, employment status, professional and educational qualifications and whether they were permitted to initiate defibrillation. With the demographic data, questions derived from the literature elicited information about participants' competence with BLS and ALS, defibrillator preference and who was the person currently responsible for initiating defibrillation.
Data analysis
Quantitative data from the questionnaire were analysed using Statistical Package for Social Scientists (SPSS) vers 6.1 (SPSS Inc; Chicago, IL, USA) for Macintosh. Statistical analysis included the use of descriptive statistics to summarise the characteristics of the sample.
In accordance with the authors of the theoretical framework, content analysis was used to analyse the data from the elicitation study19. With content analysis, content categories were identified and texts were systematically coded so that the content could be analysed numerically39. Each of the audio-taped interviews were transcribed verbatim by the researcher within 48 hours of the focus group discussion and checked for accuracy. To facilitate confidentiality all identifying information was removed and each participant was assigned a pseudonym. The transcriptions of interview tapes were read and reread to further develop a close familiarity with the data and to identify key words, quotations and phrases. A list of key ideas, quotations, words, and phrases that reflected the language and feelings of the participants and groups were identified and coded according to the behavioral beliefs45. Common quotations were then grouped under broad belief codes. These codes were labeled directly from the spoken language of the participants, for example 'not having to wait'. Next, similar coded segments of text were categorised (beliefs), organised by their frequency and counted. Codes were then arranged in descending order of frequency of occurrence and the top 75% of all beliefs were referred to as the beliefs of the target population19.
Results
Demographics
The study sample consisted of 10 females and two males (one participant chose to not complete the questionnaire but participated in the focus group discussion). The range of participants' experience in nursing was from two to 38 years (mean 19.6 years; SD = 12.6) with over half of the participants being Level Two nurses or above (n = 8). Similarly, half (n = 7) of the sample held some level of tertiary qualifications. Participant characteristics are shown (Table 1).
Table 1: Participant characteristics

Two of the 12 participants identified that they were not currently assessed as competent to perform BLS. The remaining 10 participants had been assessed competent in BLS within the last 12 months.
Half (n = 7) of the participants were expected to initiate defibrillation on their ward, of these seven participants, four had been assessed as competent within the previous 12 months and the remaining three were currently undergoing defibrillation competency assessment. When asked to identify the type of defibrillator they used, the majority of participants permitted to defibrillate (n = 6) identified the manual defibrillator as the defibrillator of choice used in an arrest. When asked to identify the person responsible for defibrillation on their ward, half (n = 6) of the participants identified the nurse on the ward or nurses from other areas of the hospital. The remaining half identified the doctor from outside the hospital.
Participants in this elicitation study believed the doctor should be primarily responsible for defibrillation when using a manual external defibrillator, whereas the nurse should be the primary person responsible when using a semiautomatic external defibrillator. When asked to identify, in order of priority, reasons why they, as individuals, did not initiate defibrillation, the order of responses were: not considered my role; inability to recognise rhythms; not allowed; fear of harming the patient; fear of litigation and fear of harming themselves. The main reasons why defibrillation was delayed on the wards were: waiting for someone to arrive who can defibrillate; the user was unsure of the rhythm; the time taken for the defibrillator to arrive; and equipment failure.
Focus group questions were designed to elicit salient beliefs within the theoretical framework. Three constructs of behavioral, normative and control beliefs guided the development of the question and analysis of the discussions. Two behavioral beliefs, four control beliefs and four normative belief categories were elicited.
Behavioral beliefs
Two behavioral beliefs categories emerged from the open-ended question: 'What, if any, are the advantages of you being able to use a defibrillator?' Participants were congruent when discussing the advantages of nurses initiating defibrillation. The two categories were 'quicker response times' (15 responses) and 'increased success with resuscitation' (8 responses). An example of the analysis process is presented (Fig 1). Several participants had multiple responses to questions, consequently the numbers depicted may be greater than the total number of participants.
In rural settings where a doctor is not in the hospital 24 hours a day, when a cardiac arrest occurs the doctor has to communicate to the hospital from their home or practice. The participants related to the urgency of the situation and the importance of not having to wait. One participant explained:
... no medical officer on hand. You have to call them in and it may take 20 minutes for them to arrive - a lot of things happen.
Further, as the participants in the study were generally the first person on the scene of the arrest, they were often in a position to initiate defibrillation rather than waiting for the medical officer to arrive. As one participant commented:
... the sheer fact that there is not a doctor here, and you are able to see someone go into VT, VF, you are able to revert it and not have to wait [for the doctor]
Within the rural context of this study, there were circumstances where the skill mix of those attending the cardiac arrest warranted nurse-initiated defibrillation. Some participants noted that even when there was a doctor available, having nurses able to defibrillate reduced the time from collapse to defibrillation because often the nurse had more experience than many of the relieving medical staff. The reflections of two participants provide examples:
Oh, I remember an RN being with a private GP and if she hadn't shocked the patient the GP would still be standing there wondering what to do...
... the relieving medical superintendent from ... didn't know what to do and only because I said the patient needs defibrillating that we did it.
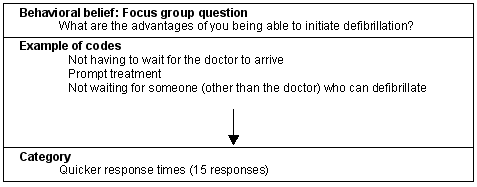
Figure 1: Belief category: Quicker response time.
The second belief that elicited a high number of responses was 'increased success with resuscitation' (Fig 2). Participants believed there was a relationship between nurse-initiated defibrillation and patient survival. The following data reflects participants' perceived advantages of their initiating defibrillation:
... the earlier you defibrillate them the better the outcome will be ...
the advantages are a higher success rate of reverting to a normal rhythm.
Participants noted patient survival was a determining factor in one hospital's decision to establish nurse initiated defibrillation programs.
I think it [nurse initiated defibrillation] was initiated by the RN because of the fact that there's not a doctor on the premises most of the time and if we waited for him to defibrillate it was often a life lost. So it was initiated out of that ...
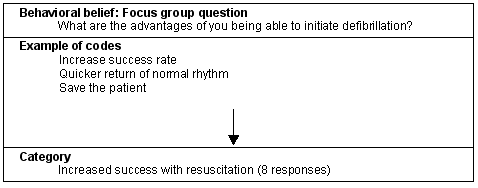
Figure 2: Belief category: Increased success with resuscitation.
Others viewed increasing the patients' survival in terms of freeing the doctor to undertake other skills. Participants talked of the collaborative relationship with the doctors in the rural context and how often during a cardiac arrest there was reduced medical and nursing presence. Participants believed that having the nurse responsible for defibrillation freed the doctor to attend to other skills that were beyond the nurses' scope of practice, such as intubation and airway maintenance. Participant responses reflected this theme:
... they [the doctor] are quite happy doing the airway, they're usually happier when someone else defibrillates, because they can't do everything.
Overwhelmingly, participants expressed greater advantages than disadvantages of nurse-initiated defibrillation. However a few participants did note that a potential disadvantage to nurse-initiated defibrillation was the risk of harming the patient or themselves.
Injury to staff or yourself and injury to the patient...
Participants perceived the potential for injury to the patient was related to user competence with the equipment. The following extract was typical of participants' concerns about harming the patient:
...the disadvantage would be if some body jumped in not really knowing what they are doing
These comments initiated discussion about participants' perceived control over their ability to initiate defibrillation.
Control beliefs
Participants were asked to identify any events that might influence their decision to use or not use a defibrillator if there was a cardiac arrest on their ward on that day. The categories of control beliefs elicited were 'rhythm recognition' (22 responses), 'litigation' (15 responses), 'fear of harm to patient or self' (11 responses), and 'roles' (4 responses).
Generally participants expressed the belief that competence does not equate to confidence. While the participants were assessed as competent by the hospital and were expected to initiate defibrillation, five of the participants expressed hesitance, fearing or being stressed about initiating defibrillation. As one participant stated:
...you do feel a little bit extra stress ... you know, it is some body's life ....
Yes the stress on the RN, making the right decision, then if you don't know the rhythm...
The main contributing factors to these feelings were rhythm recognition, concerns about harming the patient and possible litigation. In each focus group, confidence with rhythm recognition clearly influenced the majority of participants' decisions to either initiate or not initiate defibrillation unsupervised. The modal beliefs and control belief categories are displayed (Fig 3).
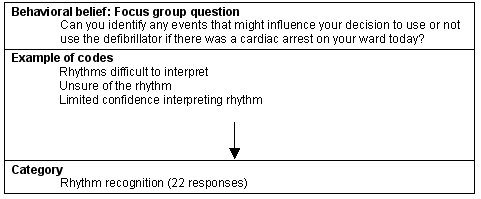
Figure 3: Belief category: Rhythm recognition.
Participants with less experience initiating defibrillation unsupervised indicated that even if they were the first person on the scene, they would wait for more experienced nurses or doctors to be present to confirm the rhythm and the need for defibrillation prior to defibrillating the patient. The following data extracts are typical of the feelings of the participants with little or no experience initiating defibrillation.
I think the first three or four times I would like to have a back-up standing right next to me.
I think it boils down to, if you are unsure you don't do it.
In situations where participants were unsure of the rhythm and there was no one around to verify it, they sought other means of clarifying the rhythm. As one participant explained:
we do the best we can, we take our orders from [the closest referral hospital]... the ECG would be faxed down and we would get our instructions.
Clearly participants with less experience would benefit from a supportive policy on what to do if there was no doctor available to confirm the rhythm.
The second control belief category that elicited a strong response was 'litigation'. The control belief categories are presented (Fig 4).
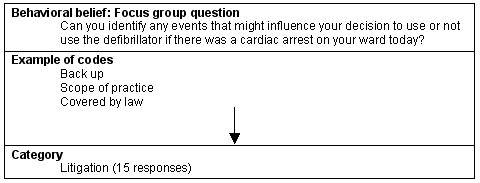
Figure 4: Belief category: Litigation.
Overwhelmingly, participants with least experience and confidence with initiating defibrillation were more likely to express concerns about the possibility of litigation. While participants believed that the hospital supported nurse-initiated defibrillation, they were less confident about the level of support they might receive from their professional body. A participant from the initial focus group reflected:
now days you need some one to back you up. It has to come from the QNC ... it is OK for the doctor to say it or the matron to say it [that nurses should initiate defibrillation] but it is not going to cover you in a court of law... the union are going to wipe you... It needs to be incorporated into the scope of practice...
Conversely participants confident with their rhythm recognition skills were more likely to be of the opinion that to do nothing meant they ran the risk of litigation as one noted:
They can sue you for not doing anything ...
Participants expressing these views were more likely to strongly articulate the belief that defibrillation was a nursing role.
Another control belief that elicited a high number of responses from participants was fear of harming the patient or themselves (Fig 5). Like rhythm recognition, fear of harming the patient was closely associated with confidence and use of the electrical equipment. This was demonstrated by the comment:
Injury to yourself and injury to the patient. There are several injuries to people, because mainly using electricity ... the workplace health and safety aspects of it as well.
well basically the person could die if they did the wrong thing at the time. If they may have thought they are doing the right thing and weren't sure of them selves, there is always the risk of harm to the person involved, I mean litigation.
When discussing the issue of not harming the patient the concept of 'doing the right thing by the patient' was raised on several occasions. Knowing the patient personally in the community exacerbated these feelings of doing the right thing by the patient.
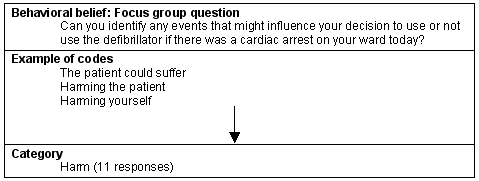
Figure 5: Belief category: Harm.
The last control belief elicited was 'roles'. While all participants agreed with the benefits of nurse-initiated early defibrillation, some participants viewed the role of defibrillation as primarily a medical role or the responsibility of a nurse with more experience. These participants believed that despite their being assessed as competent to initiate defibrillation, if the doctor was present, the responsibility and decision to initiate defibrillation reverted to the doctor. The reflections of one participant provide a clear example of these participants' thoughts on this category:
... if the doctor is there, you take your orders from the doctor
This perception may have arisen because there has been a fundamental shift in thinking from one where the doctor or senior nurse is responsible for initiating or ordering defibrillation, to one where defibrillation is now the responsibility of the first responder. Participants who had made this shift generally were more confident with defibrillation and expressed the belief that it was indeed their role to initiate defibrillation in a cardiac arrest (Fig 6). As one participant with many years experience initiating defibrillation noted:
Because we are comfortable with it [initiating defibrillation] we tend to step forward ... I have no hesitation ... as far as I am aware no one would challenge me in my decision to defibrillate.
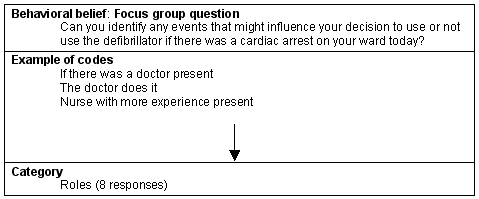
Figure 6: Belief category: Roles
Normative beliefs
To identify the normative referents, participants were asked to identify who would approve or not approve of them being responsible for the use of defibrillators in their clinical area. Four normative beliefs represent 100% of the responses, these were: patients; nurses; doctors; and the nursing registration body, the Queensland Nursing Council (QNC). Both groups identified similar referents who approve of their initiating defibrillation these were: 'registered nurses' (4 responses); 'senior registered nurses' (3 responses); 'the doctor' (6 responses); and 'the patients' (2 responses). Generally there was consensus that the move to nurse-initiated defibrillation was supported by medical officers within the hospitals:
you are going to expand the role because he [the hospital doctor] is quite good. Like he wants us to do as much as we can. So he will be definitely supportive of what we want to do.
Almost unanimously, participants could not identify with anyone who would disapprove of them initiating defibrillation. One participant 'new to initiating defibrillation' believed that others might disapprove of them initiating defibrillation, particularly if they perceived this to be their role. As one participant commented:
...it [support] depends if the person [the doctor or nurse] thinks that you are encroaching on their territory.
As previously noted, participants with little or no experience at initiating defibrillation expressed concern about their level of perceived support. This concern was particularly expressed within the context of possible adverse outcomes. Participants sought support from the doctor, the DON or professional nursing bodies. This next excerpt reflects participants' concerns about their level of support.
We need some legal cover, that is how it is these days, you need some one to back you up. It has to come from the Queensland Nursing Council. It is all right for the doctor to say to it or the Matron to say it, but that is not going to cover you in a court of law - really. Because the unions are going to wipe you. It needs to be incorporated into the scope of practice or whatever. It just needs to be covered.
Participants believed that because there was no policy from the QNC endorsing nurse-initiated defibrillation, support did not exist.
Discussion
The purpose of this study was to elicit a beginning understanding of the defibrillation beliefs of rural nurses. The results of this study provide insight into nurse-initiated defibrillation from the rural nurses' perspective. The findings indicate that for these participant nurses the concept of nurse-initiated defibrillation was generally embraced. The central issues for nurse-initiated defibrillation programs in the rural setting that emerged from the results were issues related to consequences for patient, support and confidence with rhythm recognition. These observations were not dissimilar from previous studies that have examined the challenges and concerns of nurses when there is a change in the nurse's role46,47.
When considering the advantages of nurses being permitted to initiate defibrillation in the rural setting, the participants focused on the benefits for the patient. These included quicker response times and improved survival. The findings of this study provide empirical support for previous research within the rural context where nurses have voiced their frustrations at being acutely aware of interventions required, but have had to wait for the arrival of the doctor to initiate action48,49. Participants in the current study concurred with Jones and Cooke's observation that because they were often present when the patient collapsed and understood the patient required immediate intervention, not having to wait potentially increased patients' chances of survival. Conversely, participants expressed the concern of their initiation of defibrillation resulting in harm to the patient or the potential for litigation. It was these same concerns that participants identified as potential barriers to their initiating defibrillation.
While participants in this elicitation study believed that defibrillation was indeed a nursing responsibility that would benefit the patient, there appeared to be a relationship between nurses' level of confidence and the extent to which they embraced nurse-initiated defibrillation. When asked to identify events that might influence their decision to use or not use a defibrillator, participants' identified issues related to rhythm recognition, potential for harm to the patient, litigation and their role within the arrest team. In settings where nurse-initiated defibrillation was a newer concept, participants were clearly less confident about initiating defibrillation unsupervised. These participants believed there was the risk of harming the patient or possibly incurring litigation if they initiated defibrillation unsupervised. In large settings where cardiac arrests are a frequent occurrence there is ample opportunity for skills maintenance, but in the rural setting where cardiac arrests are less frequent, skill retention is more difficult and confidence is lost50,51,52.
When normative beliefs were scrutinised, participants sought approval from peers, including other nurses and doctors. This finding was not surprising because nurses working in rural settings often have a strong collaborative relationship with peers53. Participants in the current study sought support not only from peers but also the nursing profession to assure them that it was safe for them to initiate defibrillation. There was a belief expressed that the participants were being asked to undertake a new role without adequate legal support. This observation has been noted previously in the literature where rural and remote nurses have expressed the need to legitimise the practices that nurses were undertaking54.
The findings of the current study were consistent with previous studies where a reluctance to initiate defibrillation was evident when implementing nurse-initiated defibrillation programs in hospitals55. Where policies have changed to allow nurses in rural areas to initiate defibrillation, nurses are not the ones initiating early defibrillationd9. This study was consistent with the literature, in that despite an outward enthusiasm towards the benefits of extended use of defibrillators, feelings of anxiety related to performance and a reluctance to defibrillate were observed. Stewart cautioned that expecting nurses to undertake a new role that they may perceive to be excessively complex or difficult in an emergency situation may contribute to a state of 'learned helplessness' and a dependence on persons traditionally responsible for defibrillation to initiate defibrillation56. Or as was the case in this study, a reliance on the person traditionally responsible for defibrillation to supervise the new role. This observation was mirrored in Finn and Jacobs' study where it was noted that nurses in some rural hospitals were only permitted to initiate defibrillation under the supervision of the GP. If nurses are expected to initiate early defibrillation, efforts must be directed at challenging the existing defibrillation ethos within hospitals.
Implications
The use of TPB has been advantageous to gaining insight into the predictors of early defibrillation intentions of nurses. Nurses' beliefs relating to the use of defibrillators should form part of the essential components of any defibrillation education program. If there is to be an acceptance of defibrillation as an essential part of a nurse's role, inappropriate attitudes or beliefs about defibrillation should be explored because these may hamper implementation of such programs57. Simply permitting nurses to defibrillate is not enough. Educators are faced with the challenge of enhancing positive attitudes and addressing negative attitudes to ensure nurses actually attempt defibrillation. This can be achieved by reinforcing the benefits of early defibrillation and that nurse-initiated defibrillation does make a difference to patient outcome2.
Active involvement and encouragement from key staff members, such as nursing and medical administration and education personnel is paramount to nurses embracing and using defibrillators in hospitals. Traditional roles and perceptions that 'others' are responsible for defibrillation need to be challenged58. Nurses must be empowered to initiate defibrillation and to challenge the social order of nurses in cardiac arrests. Hospital policies should include clear statements of support to ensure that defibrillation becomes a primary, rather than an extended, role of nurses. Frequent education sessions should be provided.
Limitations
Generalisation in quantitative research is equivalent to transferability in qualitative research. The intent of this study was not to generalise, rather to provide a beginning understanding of the topic. Ensuring data was complete through data saturation facilitated transferability. Having noted this, given the limited sample size, the results of this study should be considered within the context of the aim of the study.
Conclusion
In conclusion, the constructs of the TPB provided a promising framework for providing a beginning understanding rural nurses' defibrillation behavior. Explaining and facilitating defibrillation behavior may be achieved through an understanding of the benefits of nurse-initiated early defibrillation on patient survival, the support of others, confidence and rhythm recognition. The TPB is a framework for pinpointing variables that are of greatest importance in explaining and understanding nurses' use of defibrillators. Facilitating our understanding and identifying the determinants of nurses' early defibrillation behavior will ultimately facilitate the goal of early defibrillation by nurses.
References
1. Cummins RO, Sanders A, Mancini E, Hazinski MF. In-Hospital Resuscitation - A statement for healthcare professionals from the American Heart Association Emergency Cardiac Care Committee and the Advanced Cardiac Life Support, Basic Life Support, Pediatric Resuscitation, and Program Administration subcommitties. Circulation 1997; 95: 2211-2212.
2. Soar J, McKay U. A revised role for the hospital cardiac arrest team? Resuscitation 1998; 38: 145-149.
3. Stewart JA. Why not let staff nurses defibrillate? American Journal of Nursing 1993; 93(12): 7.
4. Mancini EM, Kaye W. AEDs Changing the way you respond to cardiac arrest. American Journal of Nursing 1999; 99(5): 26-31.
5. Leslie GD. A position statement on resuscitation by all levels of nurse. Australian Critical Care 1996; 9(2): 48.
6. Hegney D, McCarthy A. Job satisfaction and nurses in rural Australia. Journal of Nursing Administration 2000; 30: 347-350.
7. Finn J, Jacobs I. Cardiac arrest resuscitation policies and practices: a survey of Australian hospitals. eMedical Journal of Australia 2003; 179: 470-474.
8. Finn J. Viewpoint. The role of nurses in cardiopulmonary resuscitation and defibrillation. Collegian: Journal of the Royal College of Nursing Australia 1996; 3(3): 31-34.
9. Pascoe H. Queensland rural and remote public health facility "Chain of survival" review (Masters of Further Education and Training). Toowoomba: University of Southern Queensland, 2000.
10. Coady EM. A strategy for nurse defibrillation in general wards. Resuscitation 1999; 42: 183-186.
11. Powell G, Goulet L. Recruiters' and applicants' reactions to campus interviews and employment decisions. Academy of Management Journal 1996; 39: 1619-1640.
12. Armitage C, Conner M. Efficacy of the theory of planned behavior: A meta-analytic review. British Journal of Social Psychology 2001; 40: 471-499.
13. Cheung S, Chan D, Wong Z. Re-examining the theory of planned behavior in understanding wastepaper recycling. Environmental and Behavior 1999; 31: 587-612.
14. Marcoux B, Shope J. Application of the theory if planned behaviour to adolescent use and misuse of alcohol. Health Education Research: Theory and practice 1997; 12: 323-331.
15. Sideridis GD, Kaissidis A, Padeliadu S. Comparison of the theories of reasoned action and planned behaviour. British Journal of Educational Psychology 1998; 68: 563-580.
16. Trafimow D. Condom use among U.S. students: The importance of confidence in normative and attitudinal perceptions. The Journal of Social Psychology 2001; 141: 49-56.
17. Trafimow D, Sheeran P, Conner M, Finlay K. Perceived control and perceived difficulty: Is perceived behaviour control a multidimensional construct? The British Journal of Social Psychology 2002; 41: 101-112.
18. Ajzen I. The theory of planned behaviour. Organizational Behavior and Human Decision Processes 1991; 50: 179-211.
19. Ajzen I, Fishbein M. Understanding attitudes and predicting social behavior. Englewood-Cliffs, NJ: Prentice-Hall, 1980.
20. Fishbein M, Ajzen I. Beliefs, Attitudes, Intention and Behaviour: An introduction to theory and research reading. Reading, MA: Addison-Wesley, 1975.
21. Levin P. Test of the Fishbein and Ajzen Models as a predictor of health care workers' glove use. Research in Nursing and Health 1999; 22: 295-307.
22. Mummery K, Spence J, Hudec J. Understanding physical activity intention in Canadian school children and youth: An application of the theory of planned behaviour. Research Quarterly for Exercise and Sport 2000; 71: 116-124.
23. Mummery K, Wankel L. Training adherence in adolescent competitive swimmers: An application of the Theory of Planned Behavior. Journal of Sport & Exercise Psychology 1999; 21: 313-328.
24. Smith A, Biddle S. Attitudes and exercise adherence: Test of the theories of reasoned action and planned behaviour. Journal of Social Sports Sciences 1999; 17: 269-281.
25. Wankle L, Mummery K. Using national survey data incorporating the theory of planned behavior: Implications for social marketing strategies in physical activity. Journal of Applied Sport Psychology 1993; 5: 158-177.
26. Norman P, Connor M, Bell R. The theory of planned behaviour and smoking cessation. Health Psychology 1999; 18: 89-94.
27. Hanson M. The theory of planned behaviour applied to cigarette smoking in African-American, Puerto Rican, and non-Hispanic white teenage females. Nursing Research 1997; 46: 155-162.
28. Godin G, Valois P, Lepage L, Desharnais R. Predictors of smoking behavior: An application of Ajzen's theory of planned behavior. British Journal of Addiction 1992; 87: 1335-1343.
29. Gantt C. The theory of planned behaviour and postpartum smoking relapse. Journal of Nursing Scholarship 2001; Forth Quarter: 337-341.
30. Hillhouse J, Adler C, Drinnon J, Turisi R. Application of Ajzen's theory of planned behaviour to predict sunbathing, tanning salon use, and sunscreen use intentions and behaviors. Journal of Behavioral Medicine 1997; 20: 365-378.
31. Craig D, Wade K, Allison K, Irving H, Williams J, Hlibka C. Factors predictive of adolescents' intentions to use birth control pills, condoms, and birth control in combination with condoms. Canadian Journal of Public Health 2000; 91: 361-365.
32. Fazekas A, Senn C, Ledgerwood D. Predictors of intention to use condoms among University women: An application and extension of the theory of planned behaviour. Canadian Journal of Behavioural Science 2001; 33: 103-117.
33. Armitage C, Connor M. Distinguishing perceptions of control from self-efficacy: Predicting consumption of a low fat-diet using the theory of planned behavior. Journal of Applied Social Psychology 1999; 29: 72-90.
34. Quine L, Rubin R. Attitude, subjective norm and perceived behavioural control as predictors of women's intentions to take hormone replacement therapy. British Journal of Health Psychology 1997; 2: 199-216.
35. Pederson C. Promoting nursing students' positive attitudes toward providing care for suicidal patients. Issues in Mental Health Nursing 1993; 14: 67-84.
36. Sheeran P, Norman P, Conner M. Can the theory of planned behavior explain patterns of health behavior change? Health Psychology 2001; 20: 12-19.
37. Godin G, Kok G. The Theory of Planned Behavior: A review of its application to health related behaviors. American Journal of Health Promotion 1996; 11: 87-98.
38. Basche CE. Focus groups interview: An underutilized research technique for improving theory and practice in health education. Health Quarterly 1987; 14: 411-418.
39. Minichiello V, Sullivan G, Greenwood G, Axford R. Handbook of research methods for nursing and health science, 2nd edn. Sydney: Pearson Education Australia, 2004.
40. Beyea S, Nicoll L. Learn more using focus groups. Association of Operating Room Nurses 2000; 71: 897-900.
41. Lambert L, Conklin M, Meyer M. Parents' beliefs towards their children's participation in the National School Lunch Program: results of focus group discussion guided by the Theory of Reasoned Action. Topic in Clinical Nutrition 2001: 16(4): 11-20.
42. Gabhainn S, Kelleher C, Naughton A, Carter F, Flanagan M, McGrath M. Socio-demographic variations in perspectives on cardiovascular disease and associated risk factors. Health Education Research 1999; 14: 619-628.
43. Ajzen I. Attitudes, personality, and behavior. Milton Keynes, UK: Open University Press, 1988.
44. Morgan D. Focus groups as qualitative research, 2nd edn. Thousands Oaks: Sage, 1997.
45. Ajzen I, Madden T. Prediction of goal-directed behavior: Attitudes, intentions, and perceived behavioral control. Journal of Experimental Social Psychology 1986; 22: 453-474.
46. Bowler S, Mallik M. Role expansion: a qualitative investigation of the perceptions of senior medical and nursing staff in an adult intensive care unit. Intensive and Critical Care Nursing 1998; 14: 11-20.
47. Jones A. Changes in practice at the nurse-doctor interface. Using focus groups to explore the perceptions of first level nurses working in an acute care setting. Journal of Clinical Nursing 2003; 12: 124-131.
48. Jones J, Cook T. Advanced life support: Role of the rural registered nurse. Australian Journal of Rural Health 1996; 4: 67-72.
49. Skrifvars M, Castren M, Kurola J, Rosenberg P. In-hospital cardiopulmonary resuscitation: organisation, management and training in hospitals of different levels of care. Acta Anaesthesiologica Scandinavica 2002; 46: 48-463.
50. Camp B, Parish D, Andrews R. Effect of advanced cardiac life support training on resuscitation efforts and survival in a rural hospital. Annals Emergency Medicine 1997; 29: 529-533.
51. Birnbaum M, Kuska B, Stone H, Robinson N. Need for advanced cardiac life-support training in rural community hospitals. Critical Care Medicine 1994; 22: 735-740.
52. Birnbaum M, Robinson N, Kuska B, Stone H, Fryback D, Rose J. Effect of advanced cardiac life-support training in rural, community hospitals. Critical Care Medicine 1994; 22: 741-749.
53. Blue I, Fitzgerald M. Interprofessional relations: case studies of working relationships between registered nurses and general practitioners in rural Australia. Journal of Clinical Nursing 2002; 11: 314-321.
54. Witham H. Remote and rural nursing: An endangered profession. Australian Nursing Journal 2000; 7: 18-21.
55. Kenward G, Castle N Hodgetts. Should ward nurses be using automatic defibrillators as first responders to improve outcome from cardiac arrest? A systemic review of the primary research. Resuscitation 2002: 52: 31-37.
56. Stewart J. A more effective approach to in-hospital defibrillation. Journal of Cardiovascular Nursing 1996; 10: 37-46.
57. Walters G, D'Auria D, Glucksman E. Automated external defibrillators: implications for training qualified ambulance staff. Annuals of Emergency Medicine 1992; 21: 692-697.
58. Parr M. In-hospital resuscitation: review and revise. Resuscitation 2001; 50: 13-14. (Editorial).


