Reproductive healthcare in Vietnam
Despite many efforts, the rate of reproductive health problems in Vietnam remains high1, especially in mountainous and remote regions where healthcare facilities are often difficult for clients to access1(Fig 1). Particularly vulnerable are the Kinh poor and other ethnic minority groups, for whom the lack of quality health services and the specific knowledge and skills of healthcare workers compound the considerable problems of the terrain. The communication skills of staff in health services in Vietnam are not effective 2,3 and this has widened the gap in access to healthcare between rich and poor groups. In mountainous areas, a plethora of minority languages increases communication problems.
Traditional health behavior, culture-specific practices and the cost of treatment are added barriers to the effective use of healthcare services. Births at home are celebrated with certain rituals such as eating chicken together. And instead of receiving professional assistance, women are often assisted by female family members, neighbors and friends. Experienced and inexperienced women come to assist with the delivery and the inexperienced women learn how to assist from the experienced. In this way traditional birth knowledge is passed from generation to generation, and the women see no reason to make use of professional healthcare facilities.
In Vietnam's remote areas, obstetric complications lead to preventable maternal deaths and morbidity1. The objectives of the present research were to identify local community maternal care and family planning (MCFP) needs, in particular the needs of Kinh poor and other ethnic minority group women, and to identify barriers to the use of local MCFP services.
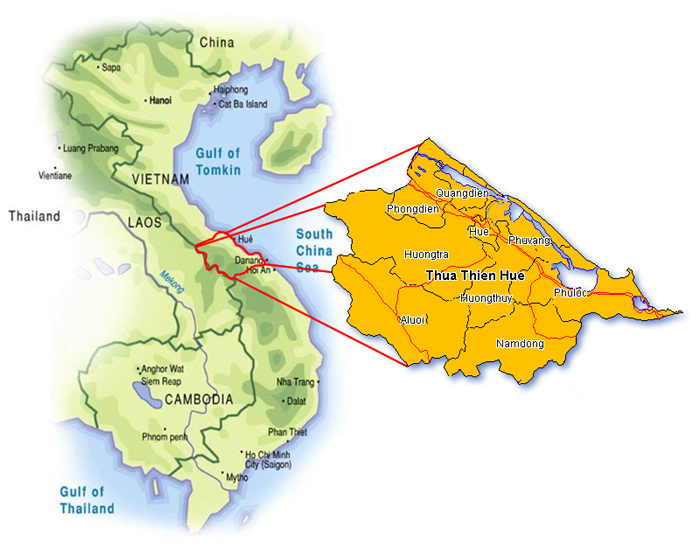
Figure 1: Map of the study area in Central Vietnam.
Context
The present study took place among seven low-income communes in the Nam Dong district, Thuathien-Hue Province, Vietnam. Reproductive healthcare services are provided to these communes by the staff of Nam Dong District Health Centre. Nam Dong is a mountainous district in the south west of Thuathien-Hue Province in Central Vietnam, with an area of 65 052 km2 and a population of 21 438 (Fig 1). The population density is 3.03 people per km2. In comparison with other mountainous regions in Vietnam, Nam Dong had good infrastructure and good transport means at its disposal5. Approximately 40% of the inhabitants were Katu ethnic minority people, the others were Kinh people. Most of these people live from agriculture, with rice and cassava the main products. The average GDP per capita is 2 398 000 VND/year (approximately US$160).
Katu people form one of the 54 ethnic minority groups in Vietnam with nearly 50 000 members who live in Thuathien-Hue Province and Quang Nam Province (south of Thuathien-Hue Province) in Vietnam, as well across the Lao border in the Provinces of Sekong and Savannakhet, mainly in the mountainous areas near the border. According to the ethnographic division of peoples they belong to the Austro-Asiatic Family, although their specific descent is unknown. They speak the Mon-Khmer language, which is also spoken by other ethnic groups but in slightly different forms4,5. The Kinh people, however, form the ethnic majority in Vietnam.
Women bear responsibility for the household and the upbringing of the children, and also for much of the agrarian work. Men are the final decision-makers in the family. For postnatal women, the maternity-leave time depends on the assistance of family members. For Katu people this means family members on the father's side; for Kinh people more often it is family members on the mother's side.
In Vietnam, the quality of family planning (FP) is low as evidenced by a high contraceptive failure rate: the average number of children born to women in the mid-land, mountainous, coastal, central Vietnam and the Central Highlands areas is more than 3 or 41. Each year, Vietnam's population increases by one million1. The number of women receiving pre-natal care and assisted deliveries by health professionals is low, so obstetric complications remain high in these areas1.
Methods
Participants
This study was limited to women who were married, of reproductive age (15-49 years), and who had delivered at least one child within the previous 5 years.
At the time of the present study, in the seven communes there were 1109 women who had a child under the age of 5 years. Sixty of these women were selected randomly from each of the seven communes, giving a sample size of 420 women. The response rate was 100%.
Data collection
An oral questionnaire was developed by the authors (Appendix I). Data collection was achieved with the assistance of 21 trained interviewers, who performed the interviews in households. During the process of data collection in the field, interviewers were helped by local translators who spoke the Katu or Van Kieu language. These data were supplemented by the following:
- The collection of secondary data regarding MCFP activities, focusing on the quality of the MCFP information management system. Secondary data were collected from the reports of the communal health centres, the district hospital and the local authority.
- Interviews with key informants (the heads and staff members of the communal health centers who are responsible for MCFP activities, as well as the managers and MCFP staff at district level).
- Observations, carried out with the help of checklists, to evaluate the MCFP facilities and equipment in communal health centers, the communication skills, and the quality of antenatal care. The observers were senior researchers and trained research assistants.
- Two focus groups in each of seven communes (n = 14 focus groups) to identify MCFP health-seeking behavior in the specific context of mountainous area, focusing on economics, culture, gender and verbal and non-verbal communication between MCFP service users and providers. The women in the focus groups all had at least one child under the age of 5 years. One of the two focus groups in each commune included women who had no antenatal care, or who delivered at home, or who used no contraceptive method. Group 2 women were those who had received antenatal care, or who had delivered at the clinic, or who used a contraceptive method.
These data were recorded using cassette recorders and by notetaking.
Analysis
Checklist data collected from the interviews were entered and analyzed using EPI-INFO vers. 6.04 (WHO, Geneva, Switzerland) combined with SPSS vers. 11.0 (SPSS Inc, Chicago, IL, USA). Correlation of study variables was performed using c2 test to define statistical significance (p < 0.05).
Key informant and focus group data were analysed by developing flowcharts and matricies of emergent themes.
Results
Of the presented results, the percentage results shown (Tables 1-4) and discussed are derived from the questionnaire data, and the quotations are from the focus group discussions.
The informants were predominantly of the Katu ethnic group (70%) however 30% were Kinh people. Most of the informants were poor farmers (80%) of traditional ancestral beliefs (75%).
Distance, cost and quality
At the time of the study, most families in Nam Dong had modern forms of transport available. 55% of the research population had a bicycle and 17% a motorbike. No-one lived further than 5 km from the nearest health center. Despite this, many women complained about the distance to the health center. They reported that, apart from the main road, the paths and roads were in bad condition, often steep and rocky, and full of puddles and slippery in the rainy season.
The cost of service in a professional healthcare center was 20.000 VND(approximately US$1.30). This was regarded as a high price for the financially disadvantaged people of Nam Dong, although it was lower than the cost of service for people in cities such as Hue City. Service costs could also be increased by the additional cost of medicine or special treatments.
Most mothers (97%) used prenatal-care services or prenatal examinations. Many women complained about the poor quality of maternal care. Some said, for example, that the toilets at the health center were not clean so they had to go into the forest to relieve themselves, which they did not like. Others complained about the postnatal-care room, which did not have enough patient beds. Further complaints related to the communication skills and the general knowledge of the healthcare workers.
Communication
The quality of health education in relation to mother-and-child care and family planning was such that it was not effective. During observed consultations, 84% of the women were educated, either by brochures or the oral communication of doctors. However, all of these education efforts were inadequate, based on national communication skills standards. A common problem was the language barrier, for instance when Kinh health workers attempted to communicate with minority (Katu) women over 30 years of age who did not speak the Kinh language. In addition, most of communication material used at the health centre were written in Kinh.
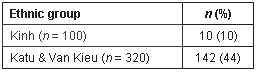
Illiteracy is problematic in the mountainous area. The percentage of illiterate informants (36%) was high compared with the national mean in Vietnam2, partly because of poor education, partly because of the phenomena of 're-illiteracy' (people who have achieved literacy then lose this skill due to lack of practice). The illiteracy was higher among Katu people than among Kinh People (Table 1).
Table 1: Illiteracy among interviewees in according to ethnic group
Only one-third of the informants had access to radio or television, so they missed out on mass communication of health information in the area. They also had inadequate knowledge about opening hours or even the location of the communal health centers.
The attitudes of the healthcare workers themselves led to other instances of poor communication: many clients complained about their negative attitudes.
Tradition and culture
Many women used antenatal and postnatal examination services (97% and 93%, respectively), but the proportion of home deliveries remained very high at 45% (Table 2). Of those who delivered at home, most women delivered alone or were attended by a traditional midwife (47.3%), whereas 38% of women were helped by others during delivery (Table 3).
Table 2: Place of delivery for children of informants
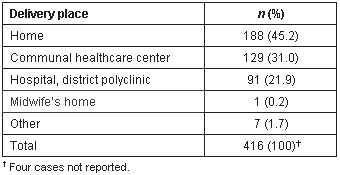
Table 3: Distribution of birth assistants in home deliveries
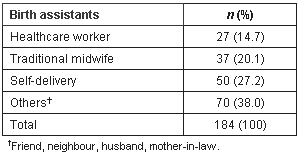
The percentage of home deliveries was much higher (81%) for the ethnic minority people than for the poor Kinh people (19%). One reason for this was the persistence of traditional and culturally specific customs and knowledge. Deliveries at home were more personal and familiar to the Katu women than deliveries in the communal health center or district hospital. Many home deliveries also occured without any assistance, either at home or in the field. One informant said:
There was a Katu woman who gave delivery in the forest, she had to help herself and bit off the umbilical cord then tied it with the root of a tree.
Gender-specific issues
At home, women are assisted by women and men cannot witness the event of the delivery. Women reported that they felt ashamed to go to the communal health care centers, where they are often assisted by men. One said, 'When I was in the communal health center and saw a man I didn't want to be there, so I left'.
The high proportion of male healthcare workers in the communal health centers was one reason a substantial number of the informants gave for feeling uncomfortable at going to the clinic. One of the informants mentioned:
One woman who was the wife of a village healthcare worker and called for her husband's help when she was in labor. Her husband asked others to take her to communal health care center and she was so ashamed of this she gave delivery alone from then on. She never called her husband again.
Another woman said:
In the communal health center, when one ethnic woman came, one female health worker helped her to give birth but there were two other male assistants which made her feel too ashamed to come back again. Some women give delivery alone and they themselves cut the umbilical cord because of being ashamed.
The focus group qualitative data suggested that women's health was potentially compromised when they went back to work in the fields too soon after delivery due to inadequate maternity leave. This is not only a socio-economic and cultural issue, but also a gender issue.
Contraception
Another issue that derives from gender relations is the use of contraception methods. Women are responsible for contraception, rather than both women and men. More than 60% of all women use contraception, while less than 20% of all men use contraception methods (Table 4).
Table 4: Use of contraceptive methods among interviewees
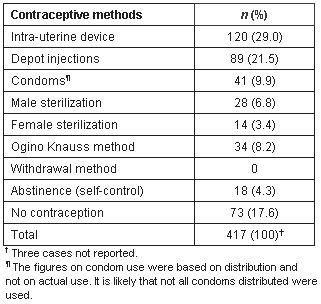
Women complained about the side-effects of the most-often-used IUD, saying it increased their weakness and tiredness6. Less than 10% of all men used condoms. The reasons given by the women were discomfort for man, and a decrease in sexual enjoyment. The analysis of the focus group discussions about why men didn't use condoms included:
Itchy for the wife; afraid of the condoms having holes; bad smell; dirty; sometimes painful for the wife.
Other reasons included:
It was annoying to use condoms, at night we had to sit up, turn on the light and blow up a condom... we were also afraid [of conceiving] if our husbands didn't use a condom when they were drunk.
One woman said that she didn't want to use condoms because she loved her husband:
He already has to work hard, [so] we shouldn't make him feel uneasy.
A considerable number of women did not use any contraceptive method. Reasons for this were given as the wish for more children; the wish for a son; discomfort; negative health consequences; and a fear of complications. The wish for a son was often asserted, mainly because a son carries on the family line and plays a responsible role in certain ritual family tasks, while the daughter often leaves for another family in another commune when she marries.
Healthcare workers' attitudes
Some women complained about the attitude of healthcare workers, which they thought was not enthusiastic enough. Some felt alienated in these circumstances. One woman said: 'Healthcare workers often say, "You are always ill and come here everyday"'. Another complained that a healthcare worker asked her: 'Why do you still get pregnant?' These comments offended them and made them less likely to visit the communal healthcare center for any reason.
Many Kinh and ethnic minority people, especially those who have more than three children (and so have gone against the family planning policy of the country under which couples are encouraged to have only 1-2 children), don't dare visit the communal health center or the district hospital for antenatal care or delivery for fear of censure (although there is no actual penalty for additional children).
Discussion
The problems and issues involved in enhancing the accessibility of MCFP services in Central Vietnam are diverse and broad. There are issues concerning the providers of health care, the users of health care, and the environment, public policies and poverty. The problems of the service providers' lack of communication skills and poor quality services are fundamental.
Communication failure is a larger problem than the personal styles of the workers, especially when many healthcare workers speak a different language from the local women. Written information, for instance brochures, was no substitute for oral communication, because a substantial number of the target women could not read or write.
Healthcare users' behaviors, such as unassisted home deliveries, present risks, both for both mother and child. Such behavior is not easily changed, especially when home deliveries are part of the culture of the mainly Katu ethnic minority people. Appropriate healthcare information is needed to change such practices. In addition, both local women and healthcare workers must be assisted to be sensitive to viewpoints different from their own.
Gender issues must be considered if access to services is to be improved. A higher proportion of female healthcare workers will motivate local women to use the services. However, it must also be recognized that men are the main decision-makers, so men should be involved in any communications about birth and childcare, even young adolescents and not yet married men.
A further factor to consider is the quality of the services. While the facilities are adequate for basic maternal care, the skills, attitudes and practices of healthcare workers and also of health management require improvement. Longer and more specialized education of healthcare workers and their managers could improve the service quality significantly.
Other problems obstruct major improvements. Even if both doctors and clients speak Vietnamese, their differing ways of thinking is an additional barrier. The doctor must learn to listen and the client must learn to be assertive. Working against this is the low educational level of the local women, and the fact that listening skills are not emphasized in the education of doctors in Vietnam.
Overall, poverty plays a major role in low access to health services. Rapid developments in the Vietnamese economy are increasing the economic gap between rural and urban areas. Doctors may prefer the city to remote areas, and a lack of quality medical staff impacts negatively on the quality of remote area services.
Recommendations to enhance the accessibility of healthcare facilities
As a result of this research, recommendations have been made to improve the healthcare facilities at communal and village levels for poor and ethnic women among the seven communes in Nam Dong mountainous district, Thuathien-Hue Province. Context-specific and gender-sensitive approaches to capacity building and health promotion are essential. Interventions should focus on improvements in the quality of the facilities; the specific knowledge of the healthcare workers; communication between clients and doctors; the number of female healthcare workers; and the knowledge and motivation of local people.
It may be a mistake for MCFP to focus only on married women in the reproductive age of 15-49 years who already have a child. Involving young adults who are not yet married may broaden access and encourage debate about traditional practices. If different opinions are respected, this may lead to mutual understanding and contribute to change. In the education of women, group activities are important. Information, education and communication methods and materials must be culturally appropriate and easy to understand.
Conclusion
In comparison with other mountainous regions in Vietnam, Nam Dong has good infrastructure and those who live there enjoy good means of transport7. These factors should enhance the accessibility of healthcare centers. The communal health centers offer basic emergency obstetric care, but many problems impact on the usefulness of the services.
This study has identified issues of poverty, illiteracy, traditional beliefs, gender insensitivity and communication skills as negatively impacting on the quality and usage of these healthcare centres. These issues are common to many rural health systems, especially where ethnic minorities represent a significant proportion of the local population. Maternal and neonatal morbidity and mortality are key health indicators. Without attention to the issues identified by this study, rural women will continue to be disadvantaged at their time of great need, the birth of the next generation.
Acknowledgements
The research in the Nam Dong mountainous district was funded by the Medical Committee of the Netherlands-Vietnam (MCNV) and technically advised by Dr EP Wright, Head of the Representative Office of MCNV in Vietnam.
References
1. Ministry of Health, Vietnam. Chien luoc quoc gia ve cham soc suc khoe sinh san giai doan 2001-2010 [National strategy on reproductive health care for the period 2001-2010]. Hanoi: Publication House of Peoples Army, 2001.
2. World Health Organization. Women's health profile: Vietnam, Vol 8. Manila: WHO Regional Office for the Western Pacific, 1995.
3. Institute of Development Science. Health-seeking behavior of the poor, research in Vienam. Hanoi: Publishing House Hanoi, 2001.
4. Ta Duc. A la decouverte des Katu et de leur culture. Hue: Center des Etudes Folkloriques de Hue, Editions Thuan Hoa, 2002; 7-9.
5. Dang NV, Chu TS, Luu H. Ethnic minorities in Vietnam. Hanoi: The Gioi Publishers, 2000; 77-80.
6. Gammeltoft T. Faithful, heroic, resourceful: changing images of women in Vietnam. In: J Kleinen (Ed.). Vietnamese society in transition: the daily politics of change and reform. Amsterdam: Het Spinhuis, 2001. 265-280.
7. National Committee for Population and family Planning, Vietnam Su dung dich vu cham soc thai san, dieu tra nhan khau suc khoe nam 1997 [Ultilisation of health services in maternal health care. DHS 1997]. Hanoi: Medicine Publishing House, 1999.
_______________________________________ _______________________________________

Published 22 October 2004; modified 13 August 2008.
Correction to second author's name from Hoat Luu Ngoc to correct form: Luu Ngoc Hoat.


