In Australia, there is a relative shortage of medical services in rural areas, including specialist procedural services. Federal and state authorities have attempted to address this deficiency by funding specialist outreach through fly-in/fly-out services. However, these programs do not address emergency procedural services (eg caesarean section, appendectomy), which are often met by the resident GP1-3. Medical colleges have attempted to address the shortage by the introduction of rural training pathways, but these programs have not delivered an increase in rural specialists, or procedurally trained GPs.
Two important issues must be explored to plan for recruitment, training and support of rural GP surgeons: (1) the current scope of practice of GP surgeons, and (2) initial and ongoing training and support.
While GP surgeons only represent a small proportion of procedurally trained GPs (10-27%)4,5, their potential scope of practice is broad. While the scope of practice has not been defined in the literature, it is believed that the scope may be changing6. Also, with changing surgical techniques, particularly the development of laparoscopic procedures, opinion is divided regarding the range of procedures GPs should be performing, including controversy over the provision of elective procedures7. To date, there is no evidence to demonstrate the current scope of practice among GP surgeons in rural Australia.
Secondly, there is currently no clear pathway of training and support available for rural GP surgeons, and potential pathways are not informed by the needs of rural medicine. For example, potential training providers are unclear on what service provision is occurring6, and, therefore, what degree of training is required to fill positions left vacant by retiring GP surgeons.
To address these two important issues, this study aims to describe the scope of practice, initial training and ongoing support and education for GP surgeons currently practising in South Australia (SA).
Participants were identified through the Rural Doctors Workforce Agency (RDWA) database. This database indexes all rural GPs in SA. Twenty-three self-described GP surgeons were identified. A GP surgeon was defined as one who undertakes non-obstetric procedures, and who may undertake gynaecological procedures. This group was contacted by email and invited to participate. Participants were excluded if they were not currently practising.
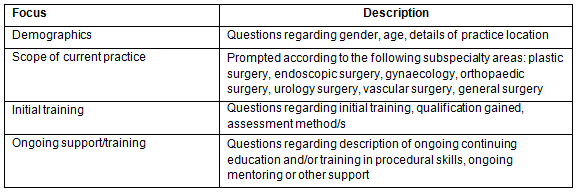
Seventeen eligible participants participated in a 15 minute semistructured telephone interview with the primary researcher (74% response rate). An interview guide was used to achieve consistency (Table 1). Questions focused on demographics, scope of practice, initial training and ongoing support and education. The interview discussion was documented by the primary researcher on the interview template.
All interviews were conducted between January and May 2011. Content and thematic analyses were used to identify common responses and themes.
Table 1: Interview guide summary
Ethics approval
Ethics approval was obtained through the University of Adelaide Human Research Ethics Committee (# H1312010).
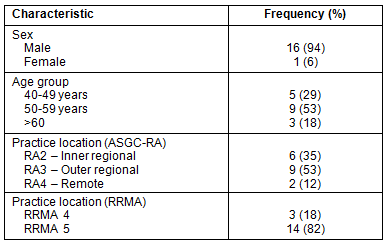
Most participants were male (16/17) and aged from 40 to over 60 years. All participants had an Australian medical degree and the majority were located in regional or small rural centres (Table 2).
Table 2: Participant characteristics (n=17)
Scope of practice
Figure 1 shows the most complicated procedure/s routinely performed by the participants across six identified subspecialty areas. Procedures are organised hierarchically within each subspecialty area according to their complexity (as assessed by the primary researcher, a practising rural GP surgeon). The modal response has been used as a baseline. The most common procedures reported were caesarean sections (94%), flaps and grafts/rotation and advancement flats/halo graft/full thickness graft (94%), closed reduction (82%) and appendectomy (71%). None of the participants undertook flexible endoscopic procedures.

Figure 1: Scope and complexity of procedures undertaken by participants by subspecialties (numbers in brackets refer to the number of participants undertaking that procedure).
Initial training
Overall, the mean duration of initial training to acquire surgical skills was 20 months (Table 3), with approximately 50% of training time spent on the acquisition of obstetric/ gynaecological procedural skills. This was consistent across all age groups. The youngest participants' (40-49 years) mean training duration was 30 months, 50% higher than the participant group as a whole. There was a trend in this group for training to have occurred locally and to have been provided by a GP surgeon or through a registrar position.
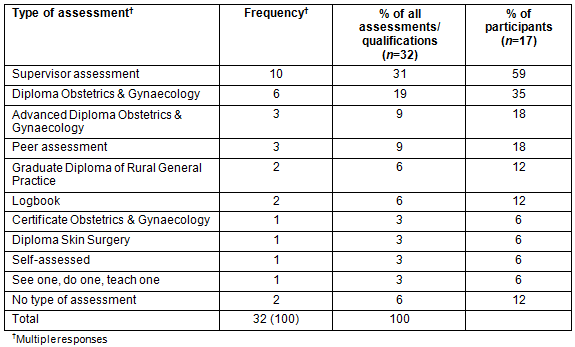
Information about initial qualifications obtained and mode of assessment of initial competency is listed in Table 4. Self-assessment or no assessment was reported as the initial qualification for 18% of participants.
Table 3: Location and type of initial surgery training by age group
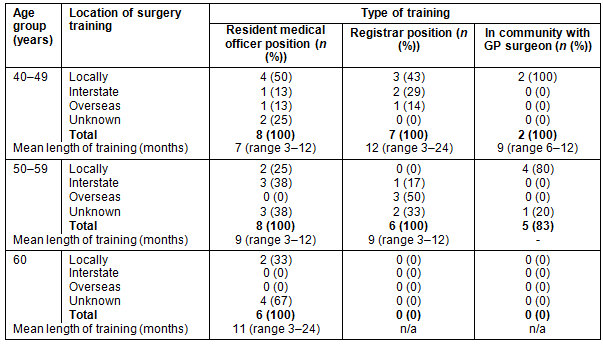
Table 4: Initial assessment of competency/qualifications
Ongoing support and education
The participants reported a range of Continuing Medical Education (CME) activities for their ongoing skill development (Table 5). The most common activities were undertaking a clinical attachment (27%) and assisting a visiting specialist or colleague (17%). No ongoing education was undertaken by 18% of participants.
Table 5: Continuing education activities

Participants identified mentors who they referred questions or complicated issues to, although the role of and frequency of contact with the mentors was varied. All participants developed their mentor relationship through personal contact. Most participants identified more than one mentor.
Discussion
Results show that GP surgery covers a wide range of surgical subspecialties. This means that to adequately equip GP surgeons, there needs to be flexibility within initial and ongoing training to enable development of a surgical skill set that is relevant to the individual and community needs. The mode responses (Fig1) provide a possible baseline skill set to structure initial training for GP surgeons. The most common surgical skill reported across participants was caesarean section (94%). Many participants indicated that their need to provide caesarean section in the local community was a major factor leading them to acquire and maintain surgical skills. Thus, in line with previous literature, caesarean section has become a cornerstone of GP surgery and needs to be a crucial component of initial and ongoing training2,6. Seventy-five percent of recent surgical trainees in SA did not undertaken any obstetric training2. The separation of this procedure from the broader range of surgical skills greatly diminishes emergency procedure requirements, and the argument for other emergency service delivery, with flow-on effects for elective procedures. Input from workforce planning, credentialing and training organisations is required.
Results showed a broad variety in initial training and qualifications. Currently in Australia, there is no formal qualification for surgery other than Fellowship of Royal Australian College of Surgeons (FRACS). Unfortunately, to date, qualifications offered by the Royal Australian College of General Practitioners (RACGP) and the Australian College of Rural and Remote Medicine (ACRRM) are not recognised by RACS, nor by state credentialing agencies, so provide little or no benefit in granting surgical privileges in rural hospitals, this being largely determined by logbook evidence, and other surrogate measures of competency. The acceptance of these surrogates appears disturbing given the results presented in Table 4. This paper demonstrates that an accepted training pathway, which is flexible and tailored for this group, needs to be developed in collaboration with the relevant colleges and credentialing bodies.
Training among the youngest cohort of GP surgeons was primarily completed locally. Unfortunately, current opportunities to train locally are limited and access to overseas training posts is no longer possible (a training option undertaken by the older cohort). Currently in SA, there is only one position specifically available for GPs wishing to acquire surgical skills, but it is not a major trauma centre. It may be that fewer SA training positions are available in the future and that existing positions may not meet the requirements of the two-year surgical curriculum negotiated by ACRRM and RACS. There needs to be an exploration of how to maximise opportunities for locally based training that can assist GP surgeons to maintain their local practice, and are responsive to regional needs.
Results show a variety of methods for ongoing support and education. Skill maintenance is an important component within medicine, with credentialing and registration bodies requiring minimum thresholds to maintain clinical privileges. However, for GP surgeons, there is no mandatory requirement for surgical skill maintenance by either RACGP or ACRRM. Unfortunately, nearly 25% of participants in the current study had not completed CME related to surgery since acquiring their initial skills and only a very small number participated in regular surgical CME. While the majority had one or more mentors, the expectations of the relationship were ad hoc. This finding aligns with a Queensland study supporting the need for ongoing support for proceduralist GPs, which found that over one-third of trainees who had undertaken advanced rural skills training, experienced poor or very poor support once they had left training8. Both a standard regulated requirement for CME for GP surgeons and a tailored program of support and education should be developed.
Although this study is the first to explore these issues in Australia, it is limited by a number of factors. It is a retrospective study and relies on self-report, particularly regarding training and assessment, which may have occurred many years ago. The primary researcher was the interviewer, and also a practising rural GP surgeon in SA, introducing a potential bias. The RDWA database only recognises those who have self-identified with a surgical interest, and potential participants may have been omitted (eg international medical graduates, where surgery may be a routine part of general practice in their country of origin). Being conducted in SA, this profile may not be similar to other states.
With limited information regarding GP surgeons, this research begins to provide a description of the current scope of practice, initial training and ongoing support and education. To date, GP surgeons have largely been self-determined and there has been little done to establish standards within the group, and a reluctance to provide cross-referencing against specialist surgeon standards. This research demonstrates the effect of self-determinism. The results from this research should help to generate discussion regarding standards and curricula for initial and ongoing training for GP surgeons and inform policy to improve access and delivery of surgical services to rural Australians.
References
1. Iglesias S, Saunders L, Tracy S, Thangisalam N, Jones L. Appendectomies in rural hospitals: safe whether performed by specialist or GP surgeons. Canadian Family Physician 2003; 49: 328-333.
2. Humber N, Frecker T. Delivery models of rural surgical services in British Columbia (1996-2005): are general practitioner-surgeons still part of the picture? Canadian Journal of Surgery 2008; 51(3): 173-178.
3. Murdoch J, Denz-Penhey H. John Flynn meets James Mackenzie: developing the discipline of rural and remote medicine in Australia. Rural and Remote Health 7: 726 (Online) 2007. Available: www.rrh.org.au (Accessed 14 November 2011).
4. To A, Williams P. Rural health workforce Australia (2013) medical practice in rural & remote Australia: combined rural workforce agencies national minimal data set. Report as at November 2012. Melbourne: RHWA
5. Dunbabin J. Procedural medicine in rural and remote NSW: the general practice workforce. Newcastle: NSW Rural Doctors Network, 2002.
6. Humber N, Frecker T. Rural surgery in British Columbia: is there anybody out there? Canadian Journal of Surgery 2008; 51(3): 179-184.
7. Green T. Rural general practitioner surgeons in Australia. Australian and New Zealand Journal of Surgery 2007; 77: 924.
8. McKenzie A, Beaton N, Hollins J, Jukka C, Hollins A. Advanced rural skills training: are recently qualified GPs using their procedural skills? Rural and Remote Health 13: 2159 (Online) 2013. Available: www.rrh.org.au (Accessed 6 March 2013).


