Abstract
Introduction: In Australia, over the past 30 years, the prevalence of dental decay in children has reduced significantly, where today 60-70% of all 12-year-olds are caries free, and only 10% of children have more than two decayed teeth. However, many studies continue to report a small but significant subset of children suffering severe levels of decay.
Methods: The present study applies Monte Carlo simulation to examine, at the national level, 12-year-old decayed, missing or filled teeth and shed light on both the statistical limitation of Australia's reporting to date as well as the problem of targeting high-risk children.
Results: A simulation for 273 000 Australian 12-year-old children found that moving from different levels of geographic clustering produced different statistical influences that drive different conclusions. At the high scale (ie state level) the gross averaging of the non-normally distributed disease burden masks the small subset of disease bearing children. At the much higher acuity of analysis (ie local government area) the risk of low numbers in the sample becomes a significant issue.
Conclusions: The results clearly highlight the importance of care when examining the existing data, and, second, opportunities for far greater levels of targeting of services to children in need. The sustainability (and fairness) of universal coverage systems needs to be examined to ensure they remain highly targeted at disease burden, and not just focused on the children that are easy to reach (and suffer the least disease).
Key words: childhood, computational mathematics, dental decay, dental public health, Monte Carlo.
Introduction
In dental public health, particularly in Australia, there is an ongoing debate about the extent of remaining dental disease in children. In Australia, over the past 30 years, the prevalence of dental decay in children has reduced significantly, where today 60-70% of all 12-year-olds are caries free, and only 10% of children have more than two decayed teeth1. This improvement is in no small part a result of the near universal population-level exposure to topical fluoride (be it water or toothpaste)2. However, many studies1,3 continue to report a small but significant subset of children suffering severe levels of decay, and this is typified by demands for general anaesthesia, in order to treat gross decay in children. This debate has and continues to be promulgated with data in the literature supporting both arguments3.
The real challenge facing society today, in this environment, is to find ways to target the sub-group of children at greatest risk with additional preventive (and treatment) strategies. School-based dental services with universal coverage have been the norm in Australia for at least 30 years4; but with the significant resources needed for these universal services, targeting becomes a real economic/healthcare debate and in the changed disease environment this debate needs to happen in an open and transparent manner. The reporting of childhood caries rates at the near-individual or high resolution is not made available for independent research in Australia; it remains shrouded in confidentiality agreements between state governments and federal analytical organisations.
In this study, a simulation approach was taken to recreate the baseline child-by-child data using methods previously published to overcome these closed data hurdles5. The present study applies Monte Carlo simulation5 to examine, at the national level, 12-year-old decayed missing or filled teeth (DMFT) and shed light on both the statistical limitation of Australia's reporting to date as well as the problem of targeting high risk.
Methods
All data was from open sources and therefore no ethics approval was required for the study6-9. All data collected and reported is for 12-year-olds unless otherwise stated. Based on previous studies it is accepted that dental decay in Australian children is strongly linked to socioeconomic strata; poorer children suffer greater levels of decay. In addition, it has been previously clearly identified by the authors of this study (and others) that Indigenous children suffer greater levels of decay than other children10-15. Against this backdrop these two factors (socioeconomics and Indigenous status) were chosen as the drivers of the simulations to generate child-by-child DMFT for 12 year-olds living in Australia. The process of simulation has been previous published and will not be covered in detail here5. In short, the simulation rests on the application of rates of decay (and missing and filled teeth) for different subsets of the population (as published in the literature) applied in a randomly seeded approach to the entire population (in this case all Australian 12-year-olds). In this simulation of socioeconomic status, Indigenous status and population numbers were collected from the most recent census (where complete data is available - 2006) to drive the simulation6-15. The simulation was completed using personally developed software (Visual Basic v6.0; http://msdn.microsoft.com/en-au/vbrun/ms788229.aspx). All resultant data was outputted to CSV (comma-separated values) format and imported into MySQL (community edition, Oracle USA; http://www.mysql.com) for analysis. The outcomes of the simulations were clustered at various geographic levels, and these were imported into QGIS (v1.8.0, open source, http://www.qgis.org/en/site) with the matching boundary files to map the outcome data to geography. Boundary files for state, statistical regions (SR) and local government areas (LGAs) were used.
Results
A Monte Carlo simulation for all 273 000 Australian 12-year-old children (with 5% being Indigenous (derived from the census data4) was completed. This method allocated simulated children to geographic locations based on the known distribution of children derived from the census data4).
Statistical region level
Australia is divided into 65 non-overlapping/no-gaps statistical regions by the Bureau of Statistics. Each region has between 1300 and 9000 12-year-olds. The estimated DMFT ranges from 0 to 1.2. The state-by-state breakdowns of the estimated DMFT rates are presented in Table 1. However, they are complicated by the high variation in the number of statistical regions per state. The distribution of the values geographically is presented in Figure 1.
Table 1: Decayed, missing or filled teeth ranges for statistical regions in each Australian state/territory
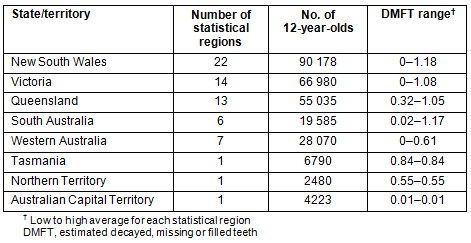
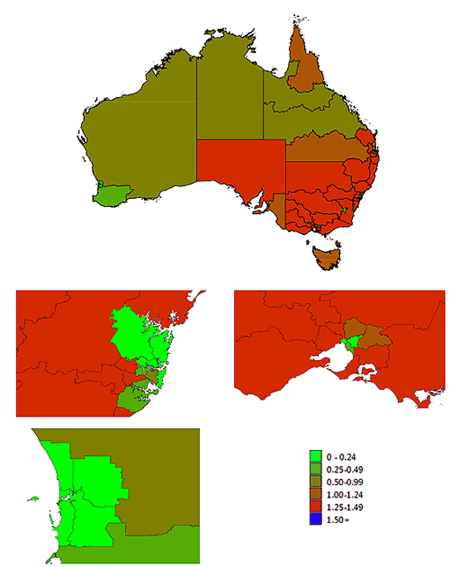
Figure 1: Estimated 12-year-old decayed, missing or filled teeth for each statistical region of Australia. High-magnification views of capital cities (Sydney, top left; Melbourne, top right; Perth, bottom left) are presented below the national map.
Statistical region subset level
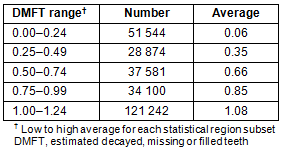
Australia is divided into 85 statistical region subsets determined by the Bureau of Statistics. Each region has between 160 and 9000 12-year-olds. At this scale level, the average estimated DMFT ranges from 0 to 1.2. However, approximately 120 000 12-year-olds (45%) are estimated to live in each statistical region subset (SRS) where the average DMFT is between 1 and 1.25 (Table 2). It is important to notice that at this level of geographic clustering no region appears to have a DMFT in excess of 1.25. Clearly, this is in contrast to the existing literature4 and known levels of decay in some children and is the apparent result of averaging.
Table 2: Number of 12-year-olds estimated in each statistical region subset (SRS) across Australia and average decayed, missing or filled teeth within each SRS
Local government area level
Australia is divided into 556 local government areas determined by the Bureau of Statistics. Each area has between 2 and 11 000 12-year-olds. At this smaller level of geographic distribution the range of estimated average DMFT scores extends to just under 2.5 (Table 3). However, this coupled with the wide range in population provides a different analytical risk (low sample size). The geographic distribution of the local government areas find that highest estimated DMFT are not in the major cities but are found in rural, regional and remote Australia (Fig2). Even when low population local government areas (fewer than 50 12-year-olds) are eliminated from the study the high acuity analysis paints a very different picture to that presented at the cumulative level of SR (Fig1).
Table 3: Estimated number of 12-year-olds in each decayed, missing or filled teeth range measured at the level of local government areas
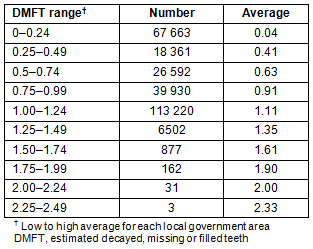
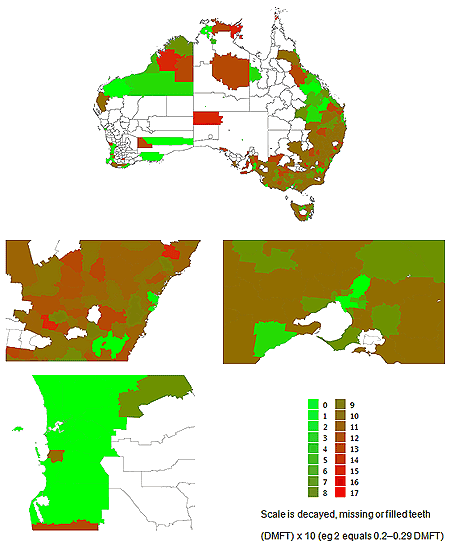
Figure 2: Estimated 12-year-old decayed, missing or filled teeth for each local government region of Australia (all those with a population of fewer than 50 12-year-olds are left blank). High-magnification views of capital cities (Sydney, top left; Melbourne, top right; Perth, bottom left) are presented below the national map.
Result summary
In short, moving from different levels of clustering produced different statistical influences that drive different conclusions. At the high scale (SR or state) the gross averaging of the non-normally distributed disease burden masks the small subset of disease-bearing children. At the much higher acuity of analysis (local government area) the risk of low numbers in the sample becomes a significant issue.
Discussion
The data presented in this study highlights two important points. First, the different levels of analysis, SR, SRS and LGA, highlight the effect of averaging in a grossly skewed (non-normally distributed) distribution of dental decay. This averaging masks the distribution and extent of disease in some groups within the population. Studies of population subsets from previous work clearly find some children suffer significantly higher burdens of dental disease16. Second, the study shows at the LGA level (when the risk of small samples is removed) a clear localization of disease burden away from the cores of major cities and towns, and focused on rural, regional and remote Australia. This is not inconsistent with the sample studies from various smaller studies that have highlighted the high disease burdens in these regions16.
Although removal of low-number LGAs was essential for statistical purity of the analysis, it would not be unsurprising that high levels of decay would exist in these areas as well, based on the neighbouring data. Clearly, this research needs to expand the simulation approach to include a greater number of ages, and it will require greater computing capacity (that is currently in planning). From this the authors expect to be able to simulate the entire child population to produce an even greater fidelity of outcome.
However, the existing data does provide state child dental health systems with high-acuity distribution of disease information and therefore a real approach to becoming more targeted with their limited resources. At the LGA level it is evident that the systems need to move to the periphery of cities and to rural, regional and remote Australia. This redirection of resource allocation will complement the extent of fluoride exposure from the managed water supplies of major metropolitan areas2 and would address much of the pain and suffering experienced in areas of less service availability3. Historically reported data points to a real need to examine the focus of school dental services. In a workforce shortage environment17 that is facing even greater resource pressures and consequential mal-distributions over the coming years, the sustainability (and fairness) of universal coverage school dental services needs to be examined to ensure they remain highly targeted at disease burden, and not just focused on the children that are easy to reach (and suffer the least disease).
Conclusions
This study applied a previously accepted system of granular simulation to address shortcomings in data accessibility to examine a real dental public health issue: childhood dental disease. The results clearly highlight the importance of care when examining the existing data and, second, opportunities for far greater levels of targeting of services to children in need.
Acknowledgements
The authors would like to thank Dr Abhijit Wagh for his assistance during the development of this study and the Brocher Foundation for the opportunity of the author (MT) to be a residential Fellow during the study development.
References
1. Ha DH, Roberts-Thomson KF & Armfield JM 2011. The Child Dental Health Surveys Australia, 2005 and 2006. Dental statistics and research series no. 54. Cat. no. DEN 213. Canberra: Australian Institute of Health and Welfare.
2. Al-Bloushi NS, Trolio R, Kruger E, Tennant M. High resolution mapping of reticulated water fluoride in Western Australia: opportunities to improve oral health. Australian Dental Journal 2012; 57: 504-510.
3. Dyson K, Kruger E, Tennant M. Networked remote area dental services: a viable, sustainable approach to oral health care in challenging environments. Australian Journal of Rural Health 2012; 20: 334-3388.
4. Armfield JM, Roberts-Thomson KF, Spencer AJ 2001. The Child Dental Health Survey, Australia 1998. AIHW Cat. No. DEN 88. Adelaide: Adelaide University (AIHW Dental Statistics and Research Series No. 24), 1998.
5. Tennant M, Kruger E. A dental public health approach based on computational mathematics: Monte Carlo simulation of childhood dental decay. International Dental Journal 2013; 63: 39-42.
6. Australian Bureau of Statistics. - Census of Population and Housing: Socio-Economic Indexes for Areas (SEIFA), Australia - data only, 2006. (Online) 2008. Cat. no. 2033.0.55.001. Available: http://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/2033.0.55.0012006?OpenDocument (Accessed 20 January 2012).
7. Australian Bureau of Statistics. 2006 CDATA online. (Online). Available: http://www.abs.gov.au/cdataonline (Accessed 20 January 2012).
8. Jamieson LM, Armfield JM, Roberts-Thomson KF. Indigenous and Non-Indigenous child oral health in three Australian states and territories. Ethnicity & Health 2007; 12: 89-107.
9. Australian Institute of Health and Welfare. Dental decay among Australian children. (Online). Available: http://www.aihw.gov.au/WorkArea/DownloadAsset.aspx?id=10737419619 (Accessed 20 January 2012).
10. Kruger E, Smith K, Atkinson D, Tennant M. The oral health status and treatment needs of Indigenous adults in the Kimberley region of Western Australia. Australian Journal of Rural Health 2008; 6: 283-289.
11. Steering Committee for the Review of Government Service Provision. Overcoming Indigenous disadvantage: key indicators 2011. Canberra, ACT: Productivity Commission, 2011.
12. Smith K, Kruger E, Dyson K, Tennant M. Oral health in rural and remote Western Australian Aboriginal communities: a two-year retrospective analysis of 999 people. International Dental Journal 2007; 57(2): 93-99.
13. Australian Bureau of Statistics and Australian Institute of Health and Welfare. The health and welfare of Australia's Aboriginal and Torres Strait Islander Peoples. Canberra, ACT: Australian Institute of Health and Welfare, 2005.
14. Australian Institute of Health and Welfare Dental Statistics and Research Unit. Oral health and access to dental care- rural and remote dwellers, July 2005. Catalogue No. DEN 144. Canberra, ACT: Australian Institute of Health and Welfare, 2005.
15. Australian Bureau of Statistics and Australian Institute of Health and Welfare. National Aboriginal and Torres Strait Islander Social Survey. Cat. no. 4714.0. Canberra, ACT: Australian Institute of Health and Welfare, 2005.
16. Kruger E, Dyson K, Tennant M. Pre-school child oral health in rural Western Australia. Australian Dental Journal 2005; 50: 258-262.
17. Kruger E, Smith K, Tennant M. Non-working dental therapists: opportunities to ameliorate workforce shortages. Australian Dental Journal 2007; 52: 22-25.






