The divide between rural and urban South Africa is indicated by research as characterised by poverty, limited access to resources and a lack of infrastructure in rural areas1. Workforce shortages can exacerbate this divide necessitating new models of health care that focus on increased collaboration and communication to optimise patient care2. Education has been found to impact directly upon society in social development, with education and social responsibility linked inextricably3. As a result of these factors, higher education institutions (HEIs) are being increasingly called upon to ensure that their methods of instruction promote equity, creative thinking, cultural tolerance and commitment to humanity. It thus becomes evident that HEIs need to take responsibility for creating conditions that encourage students and graduates to choose to practise in rural and disadvantaged settings in more socially responsible ways - a responsibility that calls for the acquisition of attributes that go beyond the disciplinary expertise or technical knowledge to prepare graduates as agents of social good4.
The Faculty of Community and Health Sciences (FCHS) at the University of the Western Cape (UWC) has, therefore, developed a specialised South African Inter-Professional Education (IPE) program that provides health sciences students with structured learning opportunities that combine service learning with teamwork and reflection. At this university, IPE occurs when two or more professional disciplines combine in a team whose members learn with, from and about each other and their work, so as to improve collaboration and the quality of care5. Collaborative practice is when health workers from different professional backgrounds work together with patients, families, caregivers and communities to deliver the highest quality of care6. The program offered required students in the disciplines of Natural Medicine, Physiotherapy and Nursing in their third and fourth years to address collaboratively identified community priorities. These priorities were identified by UWC together with community and health service providers. Students were expected to work in interdisciplinary teams and initiate community interventions for the identified priorities. They were engaged in a process of structured reflection during the IPE course and delivered a presentation to the community at the end of the placement. Students were supervised once a week according to their disciplines by selected academics with the requisite knowledge, skills and experience, as well as by on-site professionals working in the practice settings.
This article reports on an investigation of the perceptions of students in an IPE program experience, and how their perceptions of this experience influenced their intention for future practice within rural South African communities. Conclusions drawn from this investigation are put forward for consideration in the enhancement of future IPE programs and the benefits to be gained from them.
This study employed a mixed method design approach, utilising a quantitative self-administered questionnaire (SAQ), followed by student qualitative evaluation focus group discussions (FGDs). Data collection and FGDs were conducted by independent researchers with physiotherapy and community development backgrounds respectively, who were trained to gather information on the IPE program in the FCHS at UWC.
The first part of the SAQ was adapted from a University of Tasmania questionnaire for evaluating the experiences of health sciences students in an IPE program2,7. Enquiry into demographic characteristics, students' experiences on placement in a rural area and on supervision was followed by open-ended questions intended to substantiate placement and supervision experiences. The second part of the SAQ enquiry dealt with the interest of students in future interprofessional collaboration and practice in socially disadvantaged areas.
For the FGDs, an interview guide was used adapted from the Community Higher Education Services Partnership Project's Students focus group schedule8. This guide enquired about the extent to which the students found IPE meaningful, enjoyable, engaging and professional, and whether they considered that it created opportunities both to learn from one another and to develop their skills for future rural practice and engaging with disadvantaged communities.
The SAQ was disseminated among Natural Medicine, Nursing and Physiotherapy students by the independent researchers after completion of their IPE placement in a rural community. Focus group discussions followed for each group. The validity of this study approach was confirmed as follows.
Reliability and validity
The SAQ was first piloted among fourth-year dietetics students, who did not form part of the main study. Following the pilot group's recommendations, three questions were adjusted to improve clarity of meaning.
Trustworthiness
Focus group discussions were facilitated by an independent researcher and transcribed verbatim by another independent researcher; the transcripts were then re-read by both researchers to verify the exactness of the process.
Data analysis
The Statistical Package for the Social Sciences v20 (SPSS; http://www.spss.com) was used to analyse the quantitative data descriptively, utilising percentages to report the data. The open-ended questions were transcribed verbatim. Focus group discussions were recorded, with manual transcription of audio data into text. The content of the transcribed data was read and re-read - and the audio recordings were listened to several times - to familiarise the researchers with their content, as well as to create a better understanding of the data9. Themes emerged in this process that formed part of the triangulation of the quantitative data.
Ethics approval
The UWC Senate Research Ethics Committee approved the methodology and ethics of the study (registration no. 10/7/14); participants were informed and signed consent forms for participation. Participants were free to withdraw from the study at any point in the process; they were assured that withdrawal would not influence their marks in any way.
Reporting
The SAQ data is reported on within predetermined categories: demographic characteristics, experiences with an IPE program, and intentions for future practice. Emerging themes are supported by responses from the open-ended questions and the themes emerging from the FGDs.
Demographic characteristics
From January to May 2011, 23 students were placed in interdisciplinary groups in a rural and underserved municipality of the Western Cape Province of South Africa. Seventeen students consented to participate in this study, of whom 10 were from Natural Medicine, 3 from Physiotherapy and 4 from Nursing; 5 were female and 12 male; ages were between 22 and 35. Thirteen of the total 17 considered they have spent more time in urban areas, whilst four were definitely from rural areas; only 6 of the 17 considered themselves to be of rural origin.
IPE experiences
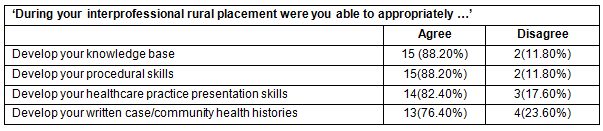
When asked to state (on a 'disagree/agree' basis) whether, as a result of their IPE program, they were able to develop appropriate knowledge and skills, the majority of students responded positively in all four areas. More than 75% agreed that they had learnt to develop knowledge base, procedural skills, healthcare practice presentation skills and written community health histories (Fig1).
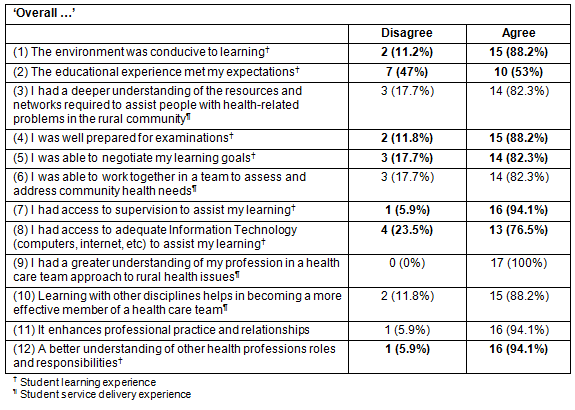
When asked to respond - negatively or positively - to 12 statements on their learning and service delivery experiences, students responded in largely positive way (82% to 100%); the one less positive result related to gaining a deeper understanding of resources and networks required (53%).
Again on a 'disagree/agree' scale the students rated highly their development following IPE placement, yet on the open-ended questions their responses reflected concerns that they felt needed to be addressed. A recurring theme was the 'lack of structure for the placement programme'. Students felt that they had too much freedom to decide on what to do in the community, which could have compromised the quality of learning. Students also expressed a desire to have more interaction between different disciplines, in order to further entrench interdisciplinary learning. Student comments included:
I would like to remain there long enough to see the effects of treatment and efforts made in health care. (Natural Medicine student, aged 36)
Not well planned from departmental side if it wasn't for our own initiative we would be doing whatever we want most of the time ... (Physiotherapy student, aged 24)
Opportunity to work with others limited, there is need to reorganise placement to suit the aspect of working together ... (Nursing student, aged 34)
More support from CHS [Community Health Sciences] with recourse to make learning easier, change of attitudes towards each other's disciplines .... (Natural medicine student, aged 22)
... Should have more structure. At times,... we had to get or plan what we need to do or where to go. Extend the time. I think this is too short to create sustainable projects and to gain trust of the community so that we don't come and make promises and leave. They should not lose hope when we are gone ... (Nursing student, aged 28)
The following comments illustrate that community-based IPE can provide an opportunity to transfer theory into practice and develop of specific professional skills:
... Engaging in the community, having a close experience of the rural culture ... (Nursing student, aged 22)
... The vibe or sense of community is not bad. Everyone always willing to assist and inform us ... (Physiotherapy student, aged 22)
... It was good to see many people with different conditions though it is sad to see sick people but seeing those things that are written in the book in reality helps a lot ... (Natural Medicine student, aged 30)
During the FGDs, the students reported that the IPE experience had enabled them to assess and prioritise the needs of community members, creating an opportunity to learn about other disciplines and compare healthcare approaches. Students realised that they needed to set aside their differences and focus on the needs of others. Student comments included:
... Learning together helped in getting a better understanding of what other health carers do and comparing it with our courses ... (Nursing student, aged 22)
... we got to mix with other students and shared our experiences and knowledge with them ... (Physiotherapy student, aged 23)
... The fact that we are proving that it can be done if we set aside our differences and focus on the needs of patients; we also become more enlightened about how the other disciplines function in the community ... (Natural Medicine student, aged 27)
Supervision experiences
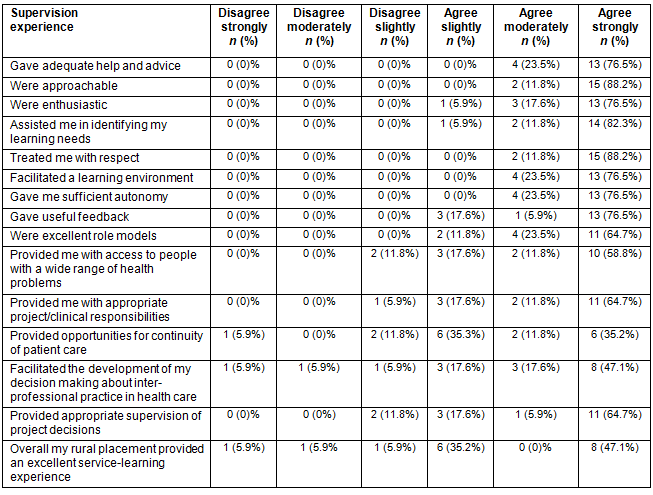
Table 1 illustrates the students' perceptions of the supervision. It was only in the area of supervision experience that students recorded 'disagreements' - in the areas of 'providing students with access to people with a wide range of health problems' (11.8%); 'providing opportunities for continuity of patient care' (17.7%), and 'providing appropriate supervision for project decisions' (11.8%). This could be linked to what some students reported in the open-ended section: that the time provided was not enough, and that the student-to-supervisor ratio was deemed to have been disproportional, at one supervisor to nine students as cited in the FGDs. Students suggested:
Supervision needs to be available throughout the week. One supervisor is not enough for nine students (Physiotherapy student, aged 23)
Supervision to be more regular, not necessarily face to face, daily emails, phone calls can be conducted (Physiotherapy student, aged 26)
Table 1: Students' perceptions of supervision
Preference for future practice
Figure 1 illustrates the preferred community of practice at the end of the course. The majority of the students (69%) preferred to work in rural-based communities with less than a third of the group preferring to work in urban-based communities.
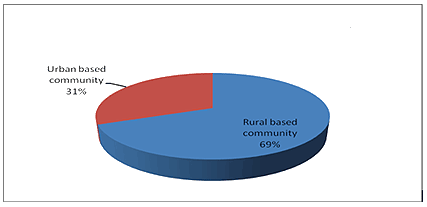
Figure 1: Preferred community of practice after the interprofessional education placement
Further questioning of students in FGDs regarding their motivation for future rural practice elicited information on a number of factors.
Community-based factors
Some students indicated that the need for health promotion in the community and the community's friendliness motivated them to want to practise in the rural areas and to work there in future. Comments included:
... I would want to practice there to make a difference in poverty and unemployment ... (Nursing student, aged 23)
... The little knowledge that the rural communities have about their individual health needs/rights and about health in general ... (Natural Medicine student, age 30)
... Community morals and values are attractive ... (Nursing student, aged 24)
However, some students did not want to return to the same community because there was minimal cooperation from the side of the community. One student said:
... I don't think I would want to go back there because I had a negative experience ... there was a lot of emphasis from the community leader that there was a problem with the children, that they were turning to drugs, yes ... but when we decided on what to do there was lack of interest on his side and he started moving his equipment for building, and now his attention shifted from us to his own business while he is the one who told us to come there because he has a problem ... (Physiotherapy student, aged 22 )
Resource-based factors
Some students want to work in rural areas in order to address the problem of limited resources. Students' comments included:
... The lack of resources, the lack of socially positive interaction of the youth, the overcrowding of the health facilities touched me, I would like to go and be part of some solution ... (Nursing student, aged 23)
... The fact that the clinics and other institutions are understaffed, physios go there only once a month, my contribution there would be good ... (Physiotherapy student, aged 22)
Other students also felt that their personal needs, such as their desire to earn more money, would not be satisfied in a rural setting. One student said:
I think as a student it was easier because it wasn't your money and even in the community we didn't ask them for money they volunteered to pay, so after qualifying it is not going to be easy like when you leave this university and you have loans to pay. Because at the end of the day the clinic will not run free, you will have to pay them to treat them because they are not going to pay you for the drugs medicine so from that aspect I wouldn't go but if it was sponsored by government then I would go ... (Natural Medicine student, aged 27)
Other factors
A desire to give back to the community was evident among students who were from rural areas. Their desire was also prompted by the community health personnel with whom they worked:
..... for me I actually come from the rural community ... And I knew what to expect when I get there so I will definitely go back there to give back to my community ... (Nursing student, aged 23)
... and also the way they teach they, are patient, they are diligent, and even if it goes chaotic they have time to yes to tell you don't do it like that do it like this, yes they have time ... (Nursing student, aged 24 )
It was clear that rural practice was an opportunity for students to practise different skills (100%), and that people in the rural areas were generally friendly. Furthermore students indicated what they enjoyed doing in the rural areas and what would attract them back there (94.1%). They felt that they would have more autonomy to practise in a rural area rather than in an urban area. They did not think that rural practice was difficult (70.6%).
Discussion
Main view
In general, the participating students highly commended the IPE program for its approach to developing self-growth, collaboration and learning, opportunities not often found in discipline-specific (silo) professional approaches. The IPE experience enabled them to assess needs and prioritise activities, creating an opportunity to learn about other disciplines and compare alternative patient care approaches. It was clear that the students valued the opportunity to practise in a rural area, as this exposed them to conditions and situations not often experienced in other placements. These skills are fostered within placement contexts specifically selected to facilitate its development. The students, however, expressed concern that the IPE program could and should be more effective. Among their recurring themes was the 'lack of structure for the placement programme' and 'the inadequate supervision they received'. While the former theme could be attributed to the dynamic context within communities, the latter theme requires further investigation.
Indicators
In their systematic literature review, Barr et al. highlighted the fact that indicators such as professional activities, self-assessment of skills, levels of knowledge, attitudes to team functions, and effects on practice with a professional partner, are used to evaluate the impact of IPE10. Their systematic review also noted positive changes towards the development of knowledge base and procedural skills. However, these authors advised that it was still difficult to evaluate the impact of IPE on knowledge and skills. In Canada, concerns similar to those expressed in this study were that students engaged in IPE were dissatisfied regarding the meeting of their expectations in their first exposure to IPE11, unless supervision was adequate and the supervisors were knowledgeable about IPE philosophy.
Change of attitude towards each other's profession and acquisition of interprofessional skills, such as teamwork, was a major component of IPE12, which was also affirmed in the present study (Table 2). Stone reported that students that they had developed a clearer understanding of the roles of other professions and achievement of effectiveness through IPE13. This result affirms McNair et al's assertion that IPE enables students to move from a one-discipline approach of practice to one that is similar to the environment in which they are meant to work14.
Table 2: Interprofessional education: development experiences (n=17)
Supervision
Significant disagreement levels with the effectiveness of supervision are apparent (Table 3). Students felt inadequately served in areas where they understood that supervisors were supposed to provide opportunities, responsibilities and an environment for learning within the community. The quality of the relationship between supervisors and students is arguably the single most important factor for effective supervision15. Interprofessional supervision creates opportunities for learning and practice development, although difficulties can occur due to differences of status, values, language, theoretical orientation and approaches to practice16.
Bailey identified the need for supervision as maximising opportunities from learning gained on 'off the job' courses for bringing about changes in effectiveness at work17. Since interprofessional working and learning are concerned with placing the client at the centre of care, with an aim of promoting collaboration across professions, supervision in the practice setting becomes of paramount importance, especially at the undergraduate level of health learning18. This form of supervision is what these authors refer to as occasions when a health or social care professional facilitates interprofessional learning and supervises and assesses students in the practice setting. Undergraduate health supervision is vital, but is probably the least investigated, discussed and developed. Researchers warn that, with time, inadequacy and a disproportional supervisor-to-student ratio, important aspects of supervision such as 'feedback' would be compromised15. Therefore, the current UWC study investigated the important components of supervision, such as supervision ratios and relationships, feedback response and time/attention allocated to students.
The supervision role
Interprofessional education is still a new philosophy of teaching. The role of supervisors has been challenged by an apparent inability to integrate discipline specific objectives with those of IPE. Such alignment could be built on the specific discipline's competence commonalities between the objectives of students and the supervisor19. In this regard, clinical facilitators and lecturers need to be trained to clearly understand each other's professional roles and responsibilities, and thus being in a position to translate that understanding in clear and empirical ways for the professional disciplines that inform the team of students20. This was affirmed by students in this study, who called for faculty understanding of the philosophy of IPE.
Table 3: Interprofessional education: student responses to 12 statements on 'students'
learning experiences'1,2,4,5,7,8,13 and 'students' service delivery experiences'3,6,10-12 (n=17)
The authors have demonstrated in this report that the UWC IPE program is an important learning approach for improving a number of skills geared towards preparing students to develop a set of professional skills that can enable them to practise in the rural and underserved communities of South Africa. Furthermore, such an IPE program could alleviate professional isolation and promote collaboration among healthcare professional students. The collaboration approach suits the healthcare situations of South African communities better than silo practice, which has been the dominant approach to health care.
The article reveals important components of learning that need to be incorporated in the UWC IPE program to improve its efficiency. These include the relevance of a coordinated process initiated by the faculty, with the involvement of all the departments, to participate in designing common IPE goals linked to the objectives of social responsibility and the training of supervisors who are able to translate this into practice.
The role of the UWC FCHS is important, particularly if it regards community-based IPE as important for the development of socially responsible graduates. Individual departmental objectives may need to be aligned to those of IPE, so as to achieve these common goals, which should be in line with the UWC's commitment to achieving its set of graduate attributes.
This article has highlighted the perspectives of health sciences students on their experiences of IPE and its impact on their professional skills development to practise within rural underserved communities. Therefore, the authors recommend further research to evaluate the IPE entire process over a longer period, so that more students and professions could participate. Future study could include departmental and faculty views on using IPE for preparing students for social responsibility and professional collaboration.
Acknowledgements
The research team would like to thank the Atlantic Philanthropies, which funded the project through the Collaboration for Health Equity through Education and Research (CHEER). CHEER consists of academics involved in community-based education from nine faculties of health sciences in South Africa: the University of KwaZulu Natal, the University of the Free State, the Walter Sisulu University, Stellenbosch University, the University of the Witwatersrand, the University of Cape Town, the University of Limpopo, the University of the Western Cape and the University of Pretoria.
The authors' thanks go also to the research interns who collected the data, the students who participated in the study, the coordinator and staff of the Interprofessional Teaching and Learning Unit in the faculty, as well as the community-based facilitators for facilitating student access and space in the rural areas where the data was collected.
The authors would like to remember the invaluable contribution of the late Professor Ratie Mpofu as the lead researcher in this publication.
References
1. African National Congress. Rural development strategy of the government of national unity. (Online) 1996. Available: http://www.polity.org.za/polity/govdocs/rdp/ruralrdp.html (Accessed 3 March 2013).
2. Whelan J, Spencer J, Rooney KA. 'RIPPER' project: advancing rural inter-professional health education at the University of Tasmania. Rural and Remote Health 8: 1-9. (Online) 2008. Available: www.rrh.org.au (Accessed 23 November 2012).
3. Guha AS. Flexible education: the key to learning - an integrated and sustainable model. Discussion Papers in Social Responsibility. No. 0905. (Online) 2009. Available: http://www.socialresponsibility.biz/discuss0905.pdf (Accessed 6 January 2013).
4. Bowden J, Hart G, King B, Trigwell K, Watts O. Generic capabilities of ATN University graduates. Canberra, ACT: Australian Government Department of Education, Training and Youth Affairs, 2000.
5. Centre for the Advancement of Interprofessional Education. Defining IPE. (Online). 2002. Available: http://www.caipe.org.uk/defining-ipe/ (Accessed 20 February 2013).
6. World Health Organization. Framework for Action on Inter-professional Education and Collaborative Practice. (Online) 2010. Available: http://www.who.int/hrh/nursing_midwifery/en (Accessed 4 April 2013).
7. De Witt D, McLean R, Newbury J, Shannon S. Critchley J. Development of a common national questionnaire to evaluate students' perceptions about the Australian rural clinical schools programs. Rural and Remote Health 5(3): 486. (Online) 2005. Available: www.rrh.org.au (Accessed 13 December 2012).
8. Community Higher Education Service Services Partnership. Inter-professional Education Programme; students focus group schedule. (Online) 2004. Available: http://www.cheer.org.za/site%20pdf's/research/UWC/FGD%20Schedule%20for%20students.PDF (Accessed 5 March 2013).
9. De Lange EF 2010. Research methodology - a step by step approach. In The fortigenic exploration of psychotherapists' experiences in full-time private practice. Doctoral thesis, University of Pretoria. (Online). 2010. Available: http://upetd.up.ac.za/thesis/available/etd-10092010-133545/unrestricted/03chapter4.pdf (Accessed 23 November 2012).
10. Barr H, Freeth D, Hammick M, Koppel I, Reeves S. Evaluations of inter-professional education: a United Kingdom review for health and social care. London: Centre for the Advancement of Interprofessional Education, 2000.
11. Rosenfield D, Oandasan I, Reeves S. Perceptions versus reality: a qualitative study of students' expectations and experiences of inter-professional education. Medical Education 2011; 45(5): 471-477.
12. Carpenter J. Inter-professional education for medical and nursing students: evaluation of a programme. Medical Education 1995; 29(4): 265-272.
13. Stone, N. The rural inter-professional education project (RIPE). Journal of Inter-professional Care 2006; 20(1): 79-81.
14. McNair R, Stone N, Sims J, Curtis C. Australian evidence for inter-professional education contributing to effective teamwork preparation and interest in rural practice. Journal of Inter-professional Care 2005; 19(6): 579-594.
15. Kilminster S, Jolly B. Effective supervision in clinical practice settings: a literature review. Medical Education 2000; 34(10): 827-840.
16. Townsend M. Inter-professional supervision from the perspectives of both mental health nurses and other professionals in the field of cognitive behavioural psychotherapy. Journal of Psychiatric and Mental Health Nursing 2005; 12(5): 582-588.
17. Bailey D. The contribution of work-based supervision to inter-professional learning on a masters programme in community mental health. Active Learning in Higher Education 2004; 5(3): 263-278.
18. Marshall M, Gordon F. Inter-professional mentorship: taking on the challenge. Journal of Integrated Care 2005; 13(2): 38-43.
19. Emerson T. Preparing placement supervisors for primary care: an inter-professional perspective from the UK. Journal of Inter-professional Care 2004; 18(2): 165-182.
20. Gilbert JHV, Camp RD, Cole CD, Bruce C, Fielding DW, Stanton SJ. Preparing students for inter-professional teamwork in health care. Journal of Inter-professional Care 2000; 14(3): 223-235.



