The provision of quality maternal and neonatal health (MNH) care in developing countries is jeopardised by poor provider performance such as that of government health departments and other state institutions. This is due to inadequate financial and human resources available, as well as to low staff motivation1,2.
Recent reports from WHO show that it is unlikely that the fifth Millennium Development Goal will be fully reached3. Developing countries continue to account for 99% of global maternal deaths, with the majority (85%) in 2010 taking place in sub-Saharan Africa3. Data from Burkina Faso, Ghana and Tanzania show unsatisfactory progress towards a reduction in maternal and neonatal mortality. In Burkina Faso, Ghana and Tanzania, the maternal mortality rates are 300, 350 and 460 per 100 000 live births, respectively, whilst the neonatal mortality rates are 39, 25 and 24 per 1000 live births, respectively3,4. Performance-based incentives (PBI) or pay-for-performance (P4P) schemes generally provide incentives for increases in the utilization and quality of care5-10. Such schemes are currently being explored as a possible way to accelerate the attainment of the Millennium Development Goals11-14.
This study was undertaken in the frame of the Quality of Maternal and Prenatal Care: Bridging the Know-do Gap (QUALMAT) project.
The QUALMAT research project (Quality of Maternal and Prenatal Care: Bridging the Know-do Gap), funded as part of the 7th Framework Programme of the European Union (grant agreement 22982), is a collaboration between the Centre de Recherche en Santé de Nouna (Burkina Faso), Ghent University (Belgium), Heidelberg University (Germany), Karolinska Institute (Sweden), Muhimbili University of Health and Allied Sciences (Tanzania), and Navrongo Health Research Centre (Ghana). The general objective of this research is to improve maternal health through better pre-natal and maternal care services offered by better motivated health workers. The intervention package includes the development and implementation of a system of performance based incentives and a computer-assisted clinical decision support system based on WHO guidelines. The interventions are evaluated in a pre-post controlled study design in rural Burkina Faso, Ghana and Tanzania between 2009 and 2014. A key hypothesis of the project is that providing incentives to rural MNH providers will increase their level of motivation, and as a result their performance will improve.
Previous studies have differentiated financial and non-financial incentives6. Financial incentives involve the transfer of monetary values, such as salaries, pensions, bonuses, allowances (eg housing, uniform and transport) and loans. Non-financial incentives include work autonomy, flexible work schedules, work recognition, coaching and mentoring structures, support for career development, improved working and living conditions, continuing education, training and professional development, improved supervision and management15. Moreover, it has been found that feedback on one's performance, comprehension of one's work responsibilities and strong alignment between personal and work goals positively influence the quality of care provided by health workers1,16-20.
To date, most of the experiences in the area of incentives have been funded by international organisations or non-governmental organisations such as Médecins Sans Frontières in Rwanda11; UNICEF in Ethiopia21; the United States Agency for International Development, the European Union, the World Bank and the African Development Bank in Egypt22; and the Catholic Organization for Relief and Development Aid and Catholic Relief Service in Cameroon14. In resource-poor settings, when external partners withdraw their support the viability of such interventions can be threatened. The issue of sustainability should be particularly considered due to the recent effects of the economic downturn on development assistance16.
The main objective of this study was to explore healthcare provider preferences for incentive schemes and possible ways to ensure sustainability of such schemes in three African countries.
Study design
The views and perspectives of MNH providers, district managers and policy makers were considered for this formative study. A qualitative methodology in the form of in-depth interviews was the preferred form of data collection. Qualitative research allows researchers to better understand phenomena in context-specific settings23. It encourages people to talk about their personal opinions and experiences and this allows investigation into incentive packages that would motivate MNH providers to provide quality services. Given the need to generate data in three different countries a reasonably structured approach was taken to develop the interview guidelines. Project collaborators from the three countries assisted with the development of the guide. The topics covered included the acceptability of local funding of performance-based incentive schemes, recommendations on how such schemes could be managed, preferred financial and non-financial incentives, ideas on possible performance indicators, as well as opinions on how to create commitment for and ensure sustainability of such schemes. The guide was developed in English and the final version was translated into French and Kiswahili using the back-translation method. Pre-tests with small groups of up to five MNH providers were carried out in all three countries. After minor modifications to optimise comprehensibility, the guide was finalised.
Sampling strategy and population
Respondents were selected through purposive sampling23. In particular, care was taken to include respondents of both sexes, spanning various age groups, from both the nursing and midwifery professions, and to include those with a facility management role. A total of 35 in-depth interviews were conducted in the three countries: 29 with MNH providers, four with members of the district health management team and two with policy makers at the national level. The selection of the districts in each country was also purposive, these districts being the future intervention districts for the QUALMAT study.
The health facilities within the districts were all under government ownership and were selected due to their rural nature and dependent upon their provision of basic essential obstetric care.
Data collection and analysis
Data collection was carried out between May and July 2010. The interviews were conducted in each country by skilled interviewers and senior social scientists with strong previous experience in qualitative interview moderation, under the supervision of a country project principal investigator. The interviews were recorded and later transcribed. The interviews in Tanzania were conducted in Kiswahili and translated into English at the time of transcription. The software QSR NVivo v8 (QSR International; http://www.qsrinternational.com/products_previous-products_nvivo8.aspx) was used to organise, manage and code the data set for each country. Prior to importing the data into NVivo, each transcript was thoroughly read by the interviewer and all issues of potential note flagged. The quality of the process was ensured because the same person undertook the interviews and the country analysis. This also avoided concerns about inter-rater reliability. A coding framework that clustered aspects of the responses into broader themes was created for each country data set. This ensured that all ideas were captured - even those that were only seldom mentioned. In each country the interviewer shared their coding and interpretation with the study's principal investigator before writing up the preliminary results, which were exchanged and discussed between the country teams before finalisation.
Ethics approval
At the outset ethical approval was obtained from the appropriate authority in each country. In Burkina Faso the ethics committee of the Centre de Recherche en Santé de Nouna approved the study (2010-05-CLE/CRSN). In Ghana the institutional review board of the Navrongo Health Research Center approved the study (NHRC1RB085). In Tanzania the Muhimbili University of Health and Allied Sciences review committee approved the study (MU/AEC/VOLXIII/96). The ethics commission of the Medical Faculty, University of Heidelberg, Germany approved the project overall (S-173/2008). Authorisation from the local health authorities was also obtained as well as written consent from all those who agreed to take part in the study.
Profile of respondents
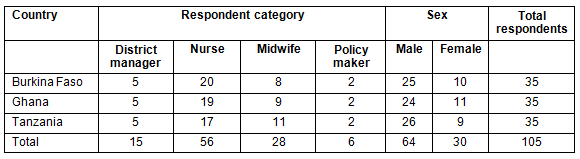
The profiles of the 35 respondents by country is presented in Table 1. The results present the findings from the facility-, district- and policy-level respondents.
Table 1: Respondent profiles by country
Specific findings in Burkina Faso
In Burkina Faso, the most commonly mentioned incentives were per-diems provided to workers either during training or meeting, bonuses, training on topics related to care provision, refresher courses, letters of acknowledgement and verbal appreciation. Whilst preferences strongly focused upon financial incentives, there was also support for non-financial incentives, in particular for decorating workers who performed well:
Giving incentives to workers based on their performance is a good initiative, as it motivates workers and thus contributes to improve the quality of care. It builds also a more competitive team to achieve health objectives. (male health worker nurse, aged 34 years, Burkina Faso)
The district managers also stressed the importance of one's work being acknowledged:
They should give us sometimes certificates or letters of recognition, as these are important non-financial incentives. (district health management team member, male health officer, aged 39 years, Burkina Faso)
Most of the respondents had no previous experience of such schemes, and several concerns about how they would be managed were raised. Most notably the district managers feared that the management of such schemes could result in a heavy workload at their level. To facilitate administration they preferred incentives to be awarded to entire teams rather than to individual providers. At the policy level, there were concerns about the costs of such schemes and a call for further investigation into the effect of non-financial incentives:
It is impossible for the Ministry of Health to afford financial incentives, considerable funds have already been allocated to increase salaries, and paid annual leave is already in place for all civil servants. We must carry out a reflection on that. (female policy maker, aged 50 years, Burkina Faso)
Regarding the sustainability of such schemes the respondents in Burkina Faso raised concern about what would happen if an external source of funding was withdrawn. There was convergence of viewpoints from all the levels of respondents that non-financial incentives would stand a greater chance of being integrated in local budgets for long-term sustainability:
We agree that financial aspects are very important from health workers' perspectives, but money is not really a key element in determining workers' performance. I suggest that emphasis should be put on acknowledgment of work done, on providing regular training and refresher courses to workers. These things are more sustainable than money, as we cannot ensure that our government can afford to continue [funding] such a system. (male nurse in charge of statistics at district headquarters, aged 38 years, Burkina Faso)
Interestingly, in Burkina Faso several health workers expressed a willingness to allocate a small proportion of the per-diems they received from attending meetings and trainings to co-fund modest financial incentives for the entire facility team.
Regarding respondents' views on how to actually monitor improvements in the area of MNH care, there was a tendency amongst the providers to simply reiterate the problems rather than actually articulate possible indicators. By comparison, the respondents with a management role at either facility or district level generally proposed indicators from amongst those routinely measured in these areas. These covered various aspects of antenatal services, prevention of mother-to-child HIV transmission, delivery and postpartum care, as well as newborn health and immunisations.
Specific findings in Ghana
The respondents from Ghana suggested a range of both financial and non-financial incentives, although, overall, more attention was paid to the importance of non-financial incentives for improving health worker performance.
Some of the respondents had experienced disappointments with financial incentive schemes - such as payment of overtime - that did not prove to be sustainable and were withdrawn. The respondents reported have recently been included in the government's health insurance, which was appreciated as an important non-financial incentive.
The respondents particularly stressed the importance of training for improving provider performance:
Training programmes upgrade health workers' ability, knowledge and skills to perform their tasks; so if some are not given the opportunity to go for that training to upgrade their knowledge, it means they will do certain things which are not approved. (female health worker, nurse, aged, 31 years, Ghana)
Others stated that strong performers should be promoted more rapidly:
With the incentives, it can also come in a way of promotion; instead of serving the normal five years, maybe with your exceptional performance one year can be taken off (female health worker, nurse-midwife, aged 36 years, Ghana)
As in Burkina Faso there was a lack of clarity amongst the MNH providers themselves regarding how their performance could be measured. Ideas included staff attendance, the amount of overtime invested and the number of patients attended to:
Incentives should be given based on punctuality, incentives should come promptly and they should be based on the needs of health workers. Extra allowances and citations for hardworking staff should be encouraged. However, there is the need to spell out criteria involved in giving awards. (female health worker, nurse-midwife, aged 27 years, Ghana)
The district managers had more specific suggestions, including the reduction of facility-based neonatal mortality or the number of pregnant women who were counselled and tested for HIV:
We want zero maternal deaths and we also want to reduce infant mortality especially neonatal deaths. The data for this is collected at facility level and ways should be found to bring the number down. (male district health management team member, health officer, aged 40 years, Ghana)
The MNH providers considered the issue of equity and fairness would be a major challenge in the management of such schemes, including non-financial incentives. The district managers were particularly concerned about the sustainability and what would happen if the scheme had to stop. The worry was that the staff would be left more demoralised than ever. As one participant put it:
What I will say is about the sustainability of the financial scheme, I'm afraid of that and if you are going to give incentive, it should be something that can be sustained and that I would not talk about money as an incentive. (female district health management team member, health worker, nurse, aged 37 years, Ghana)
At policy level, although the respondents were of the view that financial incentives had an important effect upon health worker motivation, they preferred to focus upon non-financial incentives. Whilst recognising that even non-financial incentives have costs, the level of the costs was felt to be more manageable, and a greater potential for them to be included in routine facility or district level budgets was seen.
Specific findings in Tanzania
In Tanzania, the most frequently mentioned incentives included payment of overtime, payment of per-diems at meetings or training, bonuses, timely promotion, training opportunities and verbal appreciation. Most of the providers favoured financial incentives as the key way to motivate them to do their best. As pointed out by one respondent:
Money is important as an incentive, because once someone knows there is an allowance based on performance, but if you do not work hard you might not get it, then he will work hard. (female health worker, nurse, aged 45 years, Tanzania)
The respondents with management functions were of the view that a mix of non-financial and financial incentives would be most effective:
Firstly, regular supervision should be carried out so that health workers are aware of where they go wrong and how they can improve. This is very important beside the financial incentive. Secondly, in order for health workers to perform well even without receiving extra money they should be provided with enough equipment and supplies; they will feel good and do their work properly. Thirdly, to acknowledge/recognize their work once they do better and provide reward/written acknowledgement and at the end of the year a worker may be selected for outstanding performance. (male district health management team member, assistant medical officer, aged 44 years, Tanzania)
Indeed, the issue of necessary equipment being in place was repeatedly stressed as holding the key to improved health worker performance:
We need different kinds of incentives but priority should be given to equipment and supplies, such as diagnostic tools like HIV and urine test because we are supposed to examine those expectant mothers the first time when they come at the clinic, unfortunately we are not doing so due to the lack of those tools. (female supervisor, nurse-midwife, aged 38 years, Tanzania)
The providers in particular were worried about the capacity of managers to ensure equity in managing such schemes. Many cited negative experiences, for example that certain staff members were favoured to attend trainings whilst others were excluded'
There must be a proper procedure put in place by district health managers that will ensure that all workers get a chance to attend training programmes. They must provide verbal appreciation whenever they come for supervision like 'you really tried hard' it encourages us to work more. (male health worker, nurse, aged 39 years, Tanzania)
In Tanzania the policy-level respondents broadly favoured financial incentives, either in the form of a further salary increase for all workers, or the payment of extra duty, housing and transport allowances. However, both cautioned that the funding for such steps would need to be clarified with development partners.
The providers and district managers were in favour of finding ways to create a sustainable incentive scheme that could be financed at the local level without external partner support. Several of the non-financial incentives suggested, such as supportive supervision, were viewed as part of the routine district management. As such they were considered eligible for inclusion in the council health plan and budget. Cost-sharing funds that were collected at district level were also seen as a potential source of financing for small items of missing equipment, repairs, painting facilities or to compensate staff that were compelled to work overtime at facilities suffering from a shortage of staff.
Regarding how performance should be measured, the MNH providers frequently mentioned the reduction of maternal mortality, the number of patients attending the facility and the number of hours that health staff were on duty. The district managers were more specific, suggesting that number of facility deliveries would be a good way to measure the quality of delivery care. The number of antenatal care visits made in the course of a single pregnancy was also mentioned, as were outreach sessions in the community. The policy respondents recommended the use of indicators from the health management information system to avoid increasing workloads.
Comparison between the three countries
Across the three countries, whilst preferences strongly focused upon financial incentives, there was also support for non-financial incentives. The most commonly mentioned financial incentives were similar in the three countries and generally revolved around the receipt of per-diems or monies given during training sessions or meetings, followed by bonuses, prizes for hard workers and overtime payments. There were also similarities in the type of non-financial incentive suggested across the three countries, particularly regarding training and refresher courses, timely promotion, recognition of work achievements and letters of acknowledgement.
The need to pay attention to future sustainability was recognised to be essential amongst the respondents from all three countries. Moreover, the need for stakeholder involvement in the design, provision and management of such schemes was underlined.
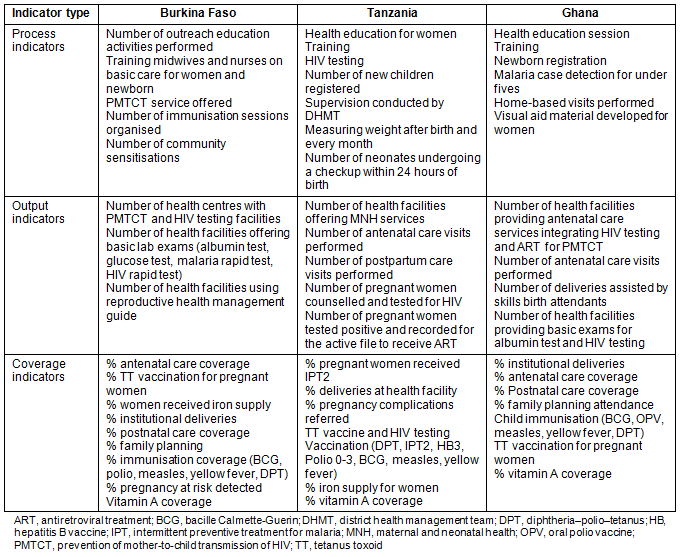
In all three countries more precise suggestions for possible performance indicators were made by the respondents with management roles. Overall, the actual indicators proposed showed similarities across the three countries. The suggestions from each country are shown in Table 2.
Table 2: Choice of performance indicators by country
Discussion
The typology of incentives suggested by the respondents from the three countries showed broad similarities. They are largely in line with those of other studies15,24.
The impact of financial incentives has received considerable attention in the literature to date11,13,22,25. However, there is less evidence regarding the role that non-financial incentives can play. Mathauer and Imhoff found that non-financial incentives were influential in improving health worker motivation26. This finding is further supported by Stilwell27 who noted that in Zimbabwe health workers based in remote areas frequently exhibited a high level of motivation to perform well despite the lack of financial incentives and difficult working conditions. A review of theories and empirical evidence of health workers' motivation28 also stressed the importance of non-financial incentives. The Australian experiments on pay-for-performance focused on non-financial incentives as a strategy for improving the quality of care, with good results29.
Despite the current interest in PBI schemes11,30 concerns about their sustainability abound, particularly when they mainly comprise financial incentives as was the case with a scheme in Egypt22.
Developing PBI schemes that are aligned with health workers' perspectives is not straightforward but has been found to be of central importance25. Although the respondents from all three countries considered financial incentives to be extremely important, overall more opportunities to integrate the costs of non-financial incentives in local budgets were identified. Important examples in this regard included training, functional and available equipment, supportive supervision and recognition for work well done. Reference was also made to the motivating effect of timely promotions, the importance of which has already been raised31.
At the policy level in all three countries there was a cautious view regarding the introduction of performance-based financing given its dependence upon donor funding.
In Burkina Faso, the providers did express a readiness to make a personal investment in such schemes so that all facility team members might benefit from receiving a modest financial incentive. This could be linked to the concerns about the fairness of such schemes and a realisation that decisions about who attends meetings or training and can thus access per-diems are often made in an arbitrary manner.
Concerns about the heavy additional workload that PBI schemes can generate for managers have been noted elsewhere20. This could explain the view of the district managers in Burkina Faso who preferred team incentives to individual incentives because they considered them easier to administer.
Although generating competition between team members may improve efficiency in some settings, the effect in health facilities in this region of the world can be divisive32.
Moreover, as it is known that gender plays an important role in health worker motivation28, there is scope to further explore the role that this may have played in these views on possible incentives, indicators and ways to finance such schemes in the longer term.
Selecting key performance indicators upon which to base such incentive schemes is an essential part of the development process. The authors' experience of engaging stakeholders in such a process showed that the suggestions from providers themselves often required further refinement and selection. Indeed, the respondents with managerial roles from all three countries made clearer suggestions. This may be because of the familiarity this role gave them with health information system indicators already in use in the system.
Limitations
The respondents were selected from one district, and specifically from six health facilities, in each of the three countries concerned. This was considered legitimate because these are the intervention districts where the incentive schemes will be piloted. However, although the findings may also be applicable to other rural districts in the same countries they should not be generalised further.
Added value of this study
This article describes the views of respondents from three countries from districts that were in the process of developing and introducing PBI schemes in the area of MNH. As there is a tendency for such schemes to be donor dependent, the authors sought to address the issue of sustainability from the outset. By seeking to obtain the views of the future beneficiaries of the scheme it was hoped that greater ownership would be generated.
Performance-based incentive schemes are being implemented in many African countries as a possible way to strengthen health system performance. However, there are concerns about their sustainability. In all three countries the possibility to integrate such schemes into local budgets was felt to be much higher if non-financial incentives were used. Ensuring participation of healthcare providers in the design of PBI schemes is likely to achieve buy-in and endorsement from the health providers involved. However, input from managers and policy makers is essential to keep expectations realistic and to ensure the indicators selected are fit for purpose and form part of routine reporting systems.
Acknowledgements
The authors acknowledge all the health workers, district managers and policy makers in the three African countries who took part in these interviews. Thanks are also extended to Jake Robyn, who helped in editing and English spelling correction.
References
1. Franco LM, Bennett S, Kanfer, R. Health sector reform and public sector health worker motivation: a conceptual framework. Social Science and Medicine 2002; 54: 1255-1266.
2. Chandler CIR, Chonya S, Mtei F, Reyburn H, Whitty CJM. Motivation, money and respect: a mixed methods study of Tanzania non-physician clinicians. Social Science and Medicine 2009; 68: 2078-2088.
3. World Health Organization, United Children's Funds, United Nations Populations Fund and World Bank estimates. Trends in maternal mortality: 1990 to 2010. Geneva: WHO Press, WHO, 2012.
4. Lozano R, Wang H, Foreman KJ, Rajaratnam JK, Naghavi M, Marcus JR et al. Progress towards Millennium Development Goals 4 and 5 on maternal and child mortality: an updated systematic analysis. Lancet 2011, 378: 1139-1165.
5. Soeters R, Habineza C, Peerenboom PB. Performance-based financing and changing the district health system: experience from Rwanda. Bulletin of World Health Organization 2006; 84: 884-889.
6. Perrot J, Adams O. Applying the contractual approach to health service delivery in developing countries. Discussion paper. (Online) 2004. Available: http://www.who.int/contracting/fr (Accessed 27 October 2012).
7. de Savigny D, Adam T (eds). Systems thinking for health systems strengthening. Alliance for Health Policy and Systems Research. Geneva: WHO, 2009.
8. Witter S, Fretheim A, Kessy FL, Lindahl AK. Paying for performance to improve the delivery of health interventions in low- and middle-income countries. Cochrane Database Systematic Review 2012, 2: CD007899.
9. Chaix-Couturier C, Durand-Zaleski I, Jolly D, Durieux P. Effects of financial incentives on medical practice: results from a systematic review of the literature and methodological issues. International Journal of Quality of Health Care 2000, 12: 133-142.
10. Basinga P, Gertler PJ, Binagwaho A, Soucat A, Sturdy JR, Vermeersch CMJ. Paying primary health care centers for performance in Rwanda. Policy Research Working Paper 5190. Washington, DC: World Bank, 2010.
11. Meessen B, Musango L, Kashala J-PI, Lemlin J. Reviewing institutions of rural health centres: the Performance Initiative in Butare, Rwanda. Tropical Medicine and International Health 2006; 11: 1303-1317.
12. Musgrove P. Financial and other rewards for good performance or results: a guided tour of concepts and terms and short glossary. Washington DC: World Bank, 2011.
13. Basinga P, Gertler PJ, Binagwaho A, Soucat ALB, Sturdy J, Vermeersch CMJ. Effect on maternal and child health services in Rwanda of payment to primary health-care providers for performance: an impact evaluation. Lancet 2011; 377: 142111428.
14. Basile K, Jean Pierre T, Florent Ymele F, Isidore S, Isidore Ayissi N, Delphine B. Expérience pilote de financement basé sur la performance dans le Diocèse de Batouri au Cameroun: leçons pour l'extension du modèle. Research paper. Cameroon: Performance Based Financing, Community Of Practice, 2011.
15. Henderson L, Tulloch J. Incentives for retaining and motivating health workers in Pacific and Asian countries. Human Resources for Health 2008; 6: 18.
16. World Health Organization. The world health report 2010: health systems financing the path to universal coverage. Geneva: WHO, 2010.
17. Eriksen J, Tomson G, Mujinja P. Assessing health worker performance in malaria case management of under fives at health facilities in a rural Tanzanian district. Tropical Medicine and International Health 2007; 12: 52-61.
18. Oxman AD, Fretheim A. Can paying for results help to achieve the Millennium Development Goals? A critical review of selected evaluations of results-based financing. Journal of Evidence Based Medicine 2009, 2: 184-195.
19. Meessen B, Soucat A, Sekabaraga C. Performance-based financing: just a donor fad or a catalyst towards comprehensive health-care reform? Bulletin of World Health Organization 2011; 89: 153-156.
20. Toonen J, Canavan A, Verger P, Elovainio R. Lessons learnt on implementing performance based financing, from a multicountry evaluation. Royal Tropical Institute, Amsterdam: Catholic Organization for Relief and Development Aid and World Health Organization, 2009.
21. Low-Beer D, Afkhami H, Komatsu R, Banati P, Sempala M, Katz I, et al. Making performance-based funding work for health. PLoS Medicine 2007; 4: e219.
22. Sameh E, El-Hayatmy M, Switlick Prose K, Eichler R. Pay-for-performance for improved health in Egypt. (Online) 2010. Available: http://healthsystems2020.org (Accessed 8 October 2012).
23. Hoepfl MC. Choosing qualitative research: a primer for technology education researchers. Journal of Technology Education 2007; 9: 1. Available: http://scholar.lib.vt.edu/ejournals/JTE/v9n1/hoepfl.html (Accessed 12 October 2012).
24. Alihounou E, Soudé T, Hounyé F. La motivation et la performance du personnel de Santé au Bénin. Benin, New York: United Children's Funds, 1998.
25. Custers T, Hurley J, Klazinga NS, Brown AD. Selecting effective incentive structures in health care: a decision framework to support health care purchasers in finding the right incentives to drive performance. BioMed Central Health Services Research 2008; 8: 66.
26. Mathauer I, Imhoff I. Health worker motivation in Africa: the role of non-financial incentives and human resource management tools. Human Resources for Health 2006; 4: 24.
27. Stilwell B. Health worker motivation in Zimbabwe. Internal report for the department of organization of health care delivery. Geneva: World Health Organization, 2001; 1-29.
28. Dolea, C, Adams, O. Motivation of health care workers: review of theories and empirical evidence. Cahiers de Sociologie et de Démographie Médicales 2005; 45(1): 135-161.
29. Scott IA. Pay-for-performance in health care: strategic issues for Australian experiments. Medical Journal of Australia 2007; 187: 31-35.
30. Kalk A, Paul FA, Grabosch E. 'Paying for performance' in Rwanda: does it pay off? Tropical Medicine and International Health 2010, 15: 182-190.
31. Yumkella F. Worker retention in human resources for health: catalyzing and tracking change. Technical brief no. 15. Chapel Hill, NC: Capacity Project, 2009.
32. Ditlopo P, Blaauw D, Bidwell P, Thomas S. Analyzing the implementation of the rural allowance in hospitals in North West Province, South Africa. Journal of Public Health Policy 2011; 32: 80-93.








