In the USA, the emergency medical services (EMS) system is an important part of the overall healthcare system1,2. EMS responds to more than 15 million emergency events annually with approximately 10% of those for children under 18 years3. EMS comprises a combination of state, local, and private-public EMS agencies1,4. While the primary focus of EMS is the timely pre-hospital treatment and transport of individuals with acute medical and trauma needs, EMS frequently includes prevention, routine medical treatment for chronic illnesses, patient rehabilitation, and initial health care regardless of ability to pay1,5. In rural areas, where significant health disparities exist, EMS is often a primary source of health care for children and their families. The rural health disparity is further magnified for children who are a vulnerable population. Often, EMS serves as a safety net for families that lack insurance or access to other health-related services1. The importance of rural EMS as a primary healthcare service has further increased due to dwindling resources and closure of many rural hospitals1.
EMS, like other healthcare services, is vital for American Indians and Alaska Natives, who are disproportionately burdened by injuries and diseases and often live in rural areas geographically far from hospitals6-10. EMS is frequently the first entry point for American Indian and Alaskan Native children and their families into the healthcare system. However, more than 6 million people in the USA who are American Indian and Alaska Natives (tribal and non-tribal affiliations)11 are often not represented in EMS and other healthcare systems.
Pre-hospital emergency care for the federally recognized tribal population represents a complex system of federal, tribal, state (non-tribal), and private (non-tribal) EMS agencies. The Indian Health Service (IHS) supports the federally funded, tribally operated EMS agencies to help meet the affiliated American Indian and Alaska Natives' pre-hospital healthcare needs (hereafter referred to as IHS EMS agencies)9,12. The federally supported agencies serve approximately 57% (1.9 million) of the total affiliated tribal population, which are located in 25 states12,13. Approximately 500 000 (28%) of the IHS service population are American Indian and Alaska Native children under 18 years11.
Past reports show that IHS EMS agencies often report challenges to providing care similar to those of rural and frontier areas including geographic isolation, lack of qualified physicians to serve as medical directors, insufficient staffing of EMS providers, substandard road conditions, inadequate landing areas for air transport, and radio communication dead zones2,4,13. The impact of these challenges may be amplified for children and families located in rural areas10,14,15. For example children in rural areas who are transported for trauma have worse outcomes than those from urban areas, due in part to longer transport times14. In addition, children residing in rural areas have increased exposure to dangerous work- and recreational-related machinery resulting in unique pediatric emergency medical needs10. However, information regarding the IHS agencies' capabilities to care for children is lacking.
The first steps to improve capability are to assess the gaps within a system. While periodic assessments of state EMS agencies capabilities to care for children occur16-18, a systematic assessment of IHS EMS agencies in regards to children does not appear to have been previously conducted. The purpose of this study was to understand the infrastructure of the IHS EMS agencies to care for children.
Survey development
During 2006, a consensus process, involving stakeholders, was used to identify topic areas that were considered essential for assessing pediatric capability in both day-to-day and disaster situations and to develop a survey to assess IHS EMS. The stakeholders were experts in the fields of pediatric emergency medicine, EMS, nursing, trauma, maternal and child health, and emergency preparedness. The survey comprised 42 open- and 47 closed-ended questions designed to assess the areas of availability of pediatric medical direction, staffing and pediatric training needs, availability of pediatric equipment, disaster preparedness and response, and EMS system data collection and integration.
When available, the stakeholder group used national guidelines or federal measures to assess the topic areas. For example, the federal EMS for Children Program developed 10 performance measures to help states assess their capability to care for children in the pre-hospital setting19. Definitions for the EMS for Children performance measures regarding online and offline pediatric medical direction and availability of pediatric equipment on ambulances were used based on the national guidelines19,20. The American Academy of Pediatrics (AAP) guidelines for preparedness were used for the preparedness section21. The survey also included questions regarding compliance to both the National Incident Management System (NIMS) or the National EMS Information System (NEMSIS) to further assess disaster preparedness, patient care data collection, and level of integration with the state in which the agency operates.
Respondent agencies were classified as basic life support (BLS) or advanced life support (ALS) based on the highest level of care they were reported to provide. For agencies that operate both types of ambulances, their BLS ambulances' equipment was reported separately from that of their ALS ambulances. When completing the survey, respondents used their own definition of the ages constituting a pediatric patient. Unless specified, respondents were asked to report for the previous year.
The survey was available to potential respondents in web-based and paper formats. The web-based format was tested prior to launching to ensure that all question conditions and branches functioned correctly.
Study population
Most of the IHS EMS agencies are located on or near reservations and in rural and frontier communities, primarily located in western states where their service population lives9,22. At the time of the survey, IHS was divided into 11 health service areas covering the 48 contiguous continental states. The health service areas contained 88 HIS EMS agencies located in 25 states23; non-federally funded tribal EMS agencies were not included. The number of agencies located in each health service area ranged from 1 to 1423. The survey was sent to 75 (85%) of the 88 agency contacts listed on the IHS program directory23 because a contact person, station of operation, or EMS providers for the remaining 13 agencies could not be identified by IHS personnel.
Implementation and analysis
A multi-contact approach was used to ensure an optimal response rate. IHS personnel telephoned all of the agency contacts to notify them of the purpose of the survey and the launch date. Agency contacts were invited to complete the survey via an email that contained a link and a PDF attachment or by a paper survey mailed to them with return instructions. Data collection occurred from 2 August to 28 December 2007. During the data collection period, up to four email reminders were sent to non-respondents. As a final contact, IHS personnel telephoned the remaining non-respondents several weeks after the last email reminder was sent. Respondents who completed the survey were able to identify a member among their EMS providers to receive a scholarship to attend the 2008 National Native American EMS Association conference.
Data were analyzed using Excel and Statistical Analysis Software v9.2 (SAS; http://www.sas.com) and summarized using descriptive statistics. Fisher's exact test was used to examine the significance of associations between agencies with and without a medical director regarding the availability of pediatric medical direction, the need for pediatric continuing education, and requirements for paramedic recertification.
Ethics approval
The survey was considered a departmental quality improvement initiative and considered exempt from institutional review by the IHS.
Respondents from 61 of the 75 study agencies (81%) completed the survey. Two respondent agencies were excluded from analysis as they reported having neither ambulances nor EMS providers, resulting in participation by 59 agencies. Ten of the 11 IHS healthcare service areas were represented in the final analysis; the one area not represented contained one IHS EMS agency. Nearly all of the agencies (n=55; 93%) defined a pediatric patient as starting at 0-1 years. The end of the pediatric age range was 19 years with over half of the agencies (56%) reporting 18 years as the cut-off age.
Demographics
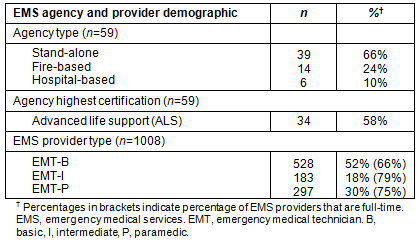
Respondent agencies represented 266 ambulances and 1008 part- and full-time emergency medical technicians (EMTs). Table 1 shows that most of the agencies (66%) operated as stand-alone and 10% were associated with a hospital. The highest level of care for over half (58%) of the agencies was ALS. The majority (71%) of the EMS providers were full-time.
The 59 agencies accounted for 46 761 annual emergency responses and 9,981 annual inter-facility transports. Pediatric emergency responses constituted 15% (n=7190) of the total 46 761 emergency responses with an average of 180 pediatric responses per agency per year. Almost half (n=26; 44%) of the agencies averaged less than one pediatric emergency response per week.
Table 1: Indian Health Service Emergency Medical Service agency and provider demographic information (N=59)
Pediatric capabilities
Medical director/direction: Nine respondents (15%) reported their EMS agency did not have a medical director. Almost all (94%) ALS agencies had a medical director compared to 80% of BLS agencies. The medical directors were located at several different types of facilities: local hospital/clinic (36%), tribal (32%), and at IHS (26%).
More than 80% of the agencies reported availability of online and/or offline pediatric medical direction when treating a pediatric patient. Figure 1 shows that agencies with a medical director were more likely to report availability of online pediatric medical direction (p=0.1) and offline pediatric medical direction (p<0.01) than agencies without one. The reasons provided by respondents for not having online pediatric medical direction available included remoteness/communication issues, lack of infrastructure, and absence of a medical director.
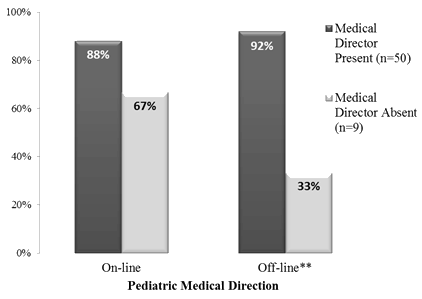
Figure 1: Comparison of agencies with and without a medical director
regarding availability of pediatric medical direction (N=59; **p<0.01).
Pediatric continuing education: The majority of respondents (83%) reported their EMS providers needed pediatric continuing education for certification and recertification. Respondents from 14 (24%) agencies reported that all (100%) of their EMS providers received pediatric continuation education training while six respondents reported none (0%) of their providers had received pediatric training. One of the respondents, who reported that none of their EMS staff had received this training, also reported their agency required 4 hours of pediatric continuing education for recertification.
For training requirements, 68% of respondents reported their EMS providers needed pediatric education for pre-hospital professionals (PEPP) and 64% needed emergency pediatric care (EPC), but reported their agency was unable to provide either. Figure 2 shows EMS agencies with a medical director were less likely to report needing pediatric continuing education for their providers' certification and recertification compared to agencies without a medical director. There was no statistical significance between agencies with a medical director and those without one in regards to the need for pediatric continuing education (p=0.3).
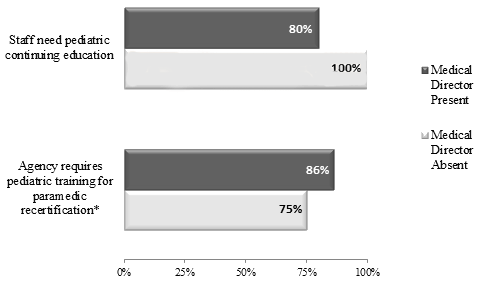
Figure 2: Comparison of Indian Health Service Emergency Medical Service agencies with
and without a medical director for pediatric continuing education needs and requirements
for paramedic recertification (N=59; 19 agencies did not have paramedics).
In addition, agencies with a medical director (86%) were more likely to require pediatric-specific training for recertification of their paramedics than agencies without a medical director (75%), but this was not statistically significant (p=0.5). Of the 40 agencies with paramedics on staff, 15% reported their agency did not require any pediatric-specific continuing education for recertification of paramedics.
Pediatric equipment: Respondents were asked to report the presence of equipment in reference to the national guidelines for pediatric equipment on ambulances. All of the agencies carried at least a proportion of the recommended pediatric equipment on at least some of their ambulances. More than a quarter (n=11; 28%) of agencies with BLS ambulances carried all (100%) of the BLS-recommended pediatric equipment on all of their ambulances. For agencies with ALS ambulances, 30% (n=10) carried all the ALS-recommended pediatric equipment on all their ambulances. Most of the least-often carried pieces of equipment on both BLS and ALS ambulances tended to be items related to the treatment of younger and smaller pediatric patients. Most of the respondents (97%) reported their agency operated in a state with specific requirements or regulations for ambulance equipment.
Disaster preparedness
Half (n=30, 51%) of the agencies reported having a mass casualties plan. Of the 30 agencies with a mass casualties plan, 15 had participated in a pediatric-focused mass casualties drill within 2 years of the survey. A quarter (n=17; 29%) of all agencies had responded to a mass casualty incident involving a large number of pediatric patients that overwhelmed their service and 8 of the 17 agencies reported they did not have enough pediatric equipment available when they responded to the incident. There were 51 (86%) respondents who reported their agency was compliant with NIMS.
EMS system data collection and integration
Almost all of the agencies (n=56, 95%) collect EMS patient care data. A little more than a third (36%) of these agencies employed a commercial or state database to store patient care data. An additional 10 agencies used spreadsheets or relational databases. Almost half (48%) of the agencies that collected patient care data used nationally recognized standard data elements (ie NEMSIS).
Almost three-quarters (n=43, 73%) of all agencies submitted patient care data to their state EMS authority. Of the agencies that submitted data, 56% (n=24) did so electronically. Sixteen (37%) agencies submitted data to their state EMS authority by mailing paper copies; the remaining 7% of respondents were unsure of the submission format their agency utilized.
Discussion
The focus of this study was to assess the gaps of the federally funded IHS EMS agencies' ability to care for American Indian/Alaska Native children. In the USA, American Indian and Alaska Natives represent 6.2 million people (tribal and non-tribal affiliations)11. Often, American Indian and Alaska Natives may not be represented in EMS systems of care for which they interface. The representation challenges are in part due to the sovereign nature of each tribe for which there are 566 federally recognized tribes11. As sovereign entities, each tribe has its own governance and systems, which may add complexity to accessing non-tribal care. Many tribes live in remote or frontier areas that compound their inclusion in systems of care. Compared to non-tribal communities, American Indian and Alaska Native children represent a large proportion of the tribal communities11 and need care that addresses their differences of anatomy, physiology, and development from adults.
The study has mixed findings regarding the ability of IHS EMS agencies to care for children. Some IHS agencies lacked a medical director, were unable to provide pediatric continuing education for their EMS providers, and were overwhelmed during mass casualty incidents involving pediatric patients. In other areas, the agencies were well integrated with their state EMS system and most submitted patient care data to their state EMS authority.
Medical direction is considered a key component of a functioning EMS agency10,24,25, yet several respondents reported their agency did not have a medical director, which has repercussions for all aspects of EMS operations. For example, the results indicate that agencies without a medical director were less likely to report the availability of on- or offline pediatric medical direction and more likely to report the need for continuing education in pediatrics than agencies with a medical director. Slifkin et al24 report several barriers for agencies recruiting medical directors in rural areas, including qualified individuals not wanting to devote the time required, lack of monetary compensation for time, liability concerns, and turnover. Generally, EMS medical directors are board-certified emergency physicians24. In rural areas such as those operated by IHS agencies, board-certified emergency physicians may not be available. A recent policy statement by the AAP proposes the use of pediatricians in rural areas to supplant many of the roles a medical director traditionally fulfills for EMS agencies10.
While this study's findings are similar to the EMS for Children national indicators regarding the availability of on- and offline pediatric medical direction26, what is different is the geographic distances the IHS EMS agencies cover9. Moreover, the overall ratio of IHS EMS to service population is one agency per 21 000 affiliated tribal members and one agency per 5700 children under the age of 18 years. This overall ratio is almost double that of the one agency per 13 500 people reported for EMS agencies in the USA26,27. In addition, based on respondent descriptions, the IHS EMS agencies are small, with a limited number of EMS providers, who are mostly trained as basic EMTs. Medical direction is crucial in service areas where the EMS providers are more likely to be certified as EMT-Basics, who require more medical oversight than paramedics24. A recent study showed that EMT-Basics employed at rural agencies with medical director involvement are more likely than those at agencies without a medical director to have the authority for interventions usually considered out of their scope of practice28.
The majority of EMS providers in the USA are located in rural areas similar to IHS EMS10,29. EMS agencies located in rural and frontier areas are different from their urban counterparts in critical ways, primarily in regards to operational challenges2,9. In the rural IHS service areas, where significant health disparities exist, EMS is often a primary source of health care10. The importance of rural EMS as a primary healthcare service has further increased due to dwindling resources and closure of many rural hospitals1. The extended response and transport times to definitive care in rural areas necessitates EMT-Basics having a broader scope of practice than their urban counterparts, for improved patient outcome28.
Another important finding was that agencies without a medical director often reported that their EMS providers needed pediatric continuing education. Continuing education in pediatrics is important for EMS providers to maintain both skills and confidence when treating children3,19,26. Approximately 15% of emergency responses among the IHS agencies were for pediatric patients. While this figure is slightly higher than the national average of 10%3, it is still low. Almost half of the agencies reported responding to less than one pediatric emergency response per week. The infrequency of pediatric-related emergency responses highlights the need for pediatric continuing education among providers in this study and in the USA. The geographically far definitive emergency care for American Indian/Alaska Natives children in rural areas further underscores the importance of continuing education for IHS EMS providers servicing this population9,10.
Children are an important focus for improving disaster planning1,30-32 and are more vulnerable than adults during disasters1,15,31,33, making it vital for EMS to include pediatric patients in mass casualty drills1,10. Unfortunately, several agencies reported responding to a mass casualty incident that overwhelmed their service and not having enough pediatric equipment when they responded to the incident. Having most of the recommended pediatric equipment or a mass casualty plan does not imply an agency's providers are prepared to treat children during a disaster. The geographic isolation, lack of qualified medical directors, and insufficient staffing of EMS providers that rural EMS agencies face amplifies the situation for the pediatric population, who are already a vulnerable population2,4,10,13-15. These findings underscore the need for a medical director who is available to provide oversight, medical direction, pediatric continuing education, and quality assurance reviews10.
Integration at a state level helps agencies identify needs, make decisions, and set priorities to improve care34. Overall, IHS agencies were well integrated with their state EMS system including submitting patient care data electronically to their state EMS authority. A recent study found that hospitals located in states with regulations mandating the presence of inter-facility transfer guidelines and agreements for pediatric patients were more likely to have the guidelines and agreements than hospitals located in states that did not have regulations35. Further evidence of integration was found in the compliance of most agencies with NIMS and NEMSIS. By integrating with other state emergency response departments and collecting standardized national EMS data elements, EMS agencies are increasing unified accountability and their ability to collect compensation for the services they provide, thereby, augmenting their sustainability34,36. Compensation for EMS services is important in a rural setting where resources are often scarcer and the transport times to definitive care facilities are longer compared to urban settings. In addition, integration with a state system helps individual EMS agencies remove overlap and redundancy of programs, optimizing funding opportunities and improving patient outcomes during disasters34,36.
Limitations and strengths
This study has several limitations and strengths. The results are based on self-reported data. The survey was not pilot tested with the target audience prior to launching. However, for the survey development a consensus approach was used, involving experts from the population being assessed. The 13 agencies that were not sent the survey appear to be inactive as the name of a contact person could not be obtained nor a station of operation established for these agencies. Information regarding the 14 agencies that were sent the survey, but did not respond, could not be obtained. The data are 5 years old; unfortunately, previous reports indicate that change is slow for tribal EMS. Needs assessments conducted over the past 19 years concentrating on adult populations and use of tribal EMS show continued deficiencies in medical direction, staffing and training, and equipment. The authors only have information on the IHS EMS agencies. The rest of the affiliated tribal population relies on non-tribally operated local public and private EMS agencies12 who primarily serve a non-Native American population. It is not known how similar or different the non-tribally operated EMS services are to the IHS EMS agencies. While the cultural relevance of services is important, it is not known whether the American Indian/Alaska Natives served by IHS agencies prefer utilizing the services provided by IHS EMS or the services of non-federally funded tribal agencies. However, in most of the study service areas, IHS EMS is the only EMS option available. A strength of this study is that this appears to be the first systematic assessment of IHS EMS agencies capabilities to treat and care for children. Another strength is the high response rate (81%), which may have been facilitated by using stakeholders from the respondent community for survey development as well as multiple-contact system and a scholarship for completed surveys.
Seemingly, this is the first assessment of IHS EMS agencies' capabilities to care for pediatric patients. The IHS agencies, with a limited number of EMS providers who are mostly trained as EMT-Basics, face the challenge of providing pre-hospital services in rural and sparsely populated areas analogous to other EMS agencies located in rural USA. A policy statement recently released by AAP10 highlights the need for medical direction, pediatric equipment, and disaster response plans that are applicable in rural settings as among the components of vital access for pre-hospital emergency care. While generally the IHS EMS agencies in the study were integrated with their state EMS system and submit patient care data to their state EMS authority, some of the agencies lacked a medical director, were unable to provide pediatric continuing education for their EMS providers, and were overwhelmed during mass casualty incidents.
Allocation of resources to support the IHS EMS agencies may be necessary. However, resources are often scarce, requiring inventive solutions. Similar to the operations challenges facing rural EMS agencies, resource scarcity is a large issue for IHS EMS where the ratio of agencies to service population is almost double that found for EMS in the USA. One possible solution is the combining and sharing of common resources. This may be a viable solution as overall agencies were well integrated with their state EMS systems and authorities. One area where sharing resources is particularly important is medical direction. Integration may help IHS EMS agencies share medical directors with other EMS agencies in their state. The recent policy statement of the AAP10 recommended the use of pediatricians in rural areas to fill many of the EMS aspects where a need was identified. Furthermore, some of the identified areas of need, such as pediatric-specific drills for disaster response and pediatric continuing education, are an issue not only for IHS EMS, but for EMS systems throughout the USA1,2,9. Continued efforts are needed so that the delivery of optimum pre-hospital pediatric care occurs throughout the country.
Acknowledgements
The authors gratefully acknowledge the contributions of Craig Hemingway, EMT-I; Karen E. Jacobson, NREMT-P; Steve Krug, MD; Kent Page, MStat; and Donald Vernon, MD for their insightful feedback and review of the manuscript prior to submission. This study was supported in part by a grant from the Health Services and Resources Administration, Bureau of Maternal and Child Health, Emergency Medical Services for Children (grant number 2U07MC05036-07-00) and Indian Health Service Emergency Medical Services for Children programs.
Preliminary results of this study were presented at the National Native American EMS Association Annual Conference, 16th Annual Conference, August 2007, Las Vegas, NV and at the American Public Health Association, 139th Annual Meeting, October 2011, Washington, DC.
References
1. Institute of Medicine, Committee on the Future of Emergency Care in the United States Health System. Emergency care for children growing pains. Washington, D.C.: National Academic Press, 2007.
2. Freeman VA, Patterson D, Slifkin RT. Issues in staffing emergency medical services: results from a national survey of local rural and urban EMS directors. Report no. 93. Chapel Hill, US: University of North Carolina at Chapel Hill, US Department of Health and Human Services, 2008.
3. National EMS Information System (NEMSIS) data cube. (Online) Available: http://www.nemsis.org/reportingTools/reports/nationalReports/createAReport.html (Accessed 24 January 2012).
4. Institute of Medicine, Committee on the Future of Emergency Care in the United States Health System. Emergency medical services at the crossroads. Washington, DC: National Academic Press, 2007.
5. Patterson P, Probst J, Moore C. Expected annual emergency miles per ambulance: an indicator for measuring availability of emergency medical services resources. Journal of Rural Health 2006; 22(2): 102-111.
6. Indian Health Service. Trends in Indian health 2002-2003 edition. Rockville, MD: Office of Public Health Support, 2003.
7. Mark D. Community-associated MRSA: disparities and implications for AI/AN communities. IHS Primary Care Provider 2007; 32(12): 1-5.
8. Indian Health Service. Emergency medical services (EMS). (Online) Available: http://www.ihs.gov/AdminMngrResources/EPEMS/index.cfm?module=ems2011 (Accessed 28 April 2011).
9. McGinnis K. Rural and frontier. Emergency Medical Services. Agenda for the future. Kansas City, MO: National Rural Health Association (NRHA), 2004.
10. Committee on Pediatric Emergency Medicine. Policy statement. The role of the pediatrician in rural emergency medical services for children. Pediatrics 2012; 130(5): 978-982.
11. The Office of Minority Health. American Indian/Alaska Native population. (Online) Available: http://minorityhealth.hhs.gov/templates/browse.aspx?lvl=2&lvlID=522012 (Accessed 31 January 2012).
12. Indian Health Service. Indian population. (Online) Available: http://info.ihs.gov/Population.asp2010 (Accessed 24 September 2010).
13. Decker P, Flaherty J, LeBeau G, Short D. Quantifying the unmet need in IHS/Tribal EMS: a project funded by the Office of Program Planning and Evaluation, Office of Public Health, IHS Headquarters 1999-2001. Rockville, MD: Office of Public Health, 2001.
14. McCowan C, Swanson E, Thomas F, Handrahan D. Outcomes of pediatric trauma patients transported from rural and urban scenes. Air Medical Journal 2008; 27(2): 78-83.
15. Wallace L. Injuries among American Indian and Alaska Native children, 1985-1996. Atlanta, GA: National Center for Injury Prevention and Control, Centers for Disease Control and Prevention, 2000.
16. National EMS for Children Data Analysis Resource Center (NEDARC). 2010-11 grant year. (Online) Available: http://www.nedarc.org/performanceMeasures/nationalData/201011GrantYear.html (Accessed 8 September 2011).
17. Seidel J. Emergency medical services and the pediatric patient: are the needs being met? II. Training and equipping emergency medical services providers for pediatric emergencies. Pediatrics 1986; 78(5): 808-812.
18. Schmuhl P, Van Duker H, Gurley K, Webster A, Olson L. Reaching emergency medical services providers: is one survey mode better than another? Prehospital Emergency Care 2010; 14: 361-369.
19. Emergency Medical Services for Children (EMSC) National Resource Center. EMSC performance measures: an implementation manual for State Partnership Grantees, 2009-2010 edition. Washington, DC: Emergency Medical Services for Children (EMSC) National Resource Center, 2009.
20. Committee on Ambulance Equipment and Supplies, National Emergency Medical Services for Children Resource Alliance. Guidelines for pediatric equipment and supplies for emergency departments. Annals of Emergency Medicine 1998; 31: 54-57.
21. American Academy of Pediatrics, Committee on Pediatric Emergency Medicine and American College of Emergency Physicians, Pediatric Committee. Care of children in the emergency department: guides for preparedness. Pediatrics 2001; 107: 777-781.
22. Indian Health Service. Indian Health Service: a quick look. (Online) Available: http://info.ihs.gov/QuickLook2010.asp2010 (Accessed 24 September 2010).
23. Indian Health Service. Tribal EMS program directory. (Online) Available: http://www.heds.org/ambpro10.pdf2008 (Accessed 25 October 2008).
24. Slifkin R, Freeman V, Patterson P. Designated medical directors for emergency medical services: recruitment and roles. Journal of Rural Health 2009; 25(4): 392-398.
25. Krentz M, Wainscott M. Medical accountability. Emergency Medical Clinics of North America 1990; 8(1): 17-32.
26. Federal Interagency Committee for Emergency Medical Services. 2011 national EMS assessment report. (Online) Available: http://ems.gov/pdf/2011/National_EMS_Assessment_Final_Draft_12202011.pdf (Accessed 26 March 2012).
27. US Census Bureau. Guide to state and local census geography. (Online) Available: http://www.census.gov/geo/www/guidestloc/guide_main.html (Accessed 28 March 2012).
28. Williams I, Valderrama A, Bolton P, Greek A, Greer S, Patterson D, Zhang Z. Factors associated with emergency medical services scope of practice for acute cardiovascular events. Prehospital Emergency Care 2012; 12: 189-197.
29. Knott A. Emergency medical services in rural areas: the supporting role of state EMS agencies. Journal of Rural Health 2003; 19(4): 492-496.
30. Shirm S, Liggin R, Dick R, Graham J. Prehospital preparedness for pediatric mass-casualty events. Pediatrics 2007; 120(4): e756-761.
31. Burke R, Iverson E, Goodhue C, Neches R, Upperman J. Disaster and mass casualty events in the pediatric population. Seminars in Pediatric Surgery 2010; 19: 265-270.
32. Graham C, Stuemky J, Lera T. Emergency medical services preparedness for pediatric emergencies. Pediatric Emergency Care 1993; 9(6): 329-331.
33. Allen G, Parrillo S, Will J, Mohr J. Principles of disaster planning for the pediatric population. Prehospital Disaster Medicine 2007; 22(6): 537-540.
34. Institute of Medicine, Committee on the Future of Emergency Care in the United States Health System. Hospital-based emergency care at the breaking point. Washington, DC: National Academic Press, 2007.
35. Fendya DG, Genovesi A, Belli K, Page K, Vernon DD. Organized interfacility transfer processes: an opportunity to improve pediatric emergency care. Pediatric Emergency Care. 2011; 27(10): 900-906.
36. Federal Emergency Management Agency (FEMA). About the national incident management system (NIMS). (Online) Available: http://www.fema.gov/national-incident-management-system (Accessed 1 February 2012).



