Shortages and geographic mal-distribution of primary care providers is an ever-present problem that affects many countries and regions including the rural and northern regions of Canada1-3. Many rural and remote communities are underserved because the majority of physicians move to larger, more southern cities2,4. Northern Ontario consists of several small and mid-sized urban communities (Sudbury, Sault Ste. Marie, North Bay, Timmins, Timiskaming, Thunder Bay, Kenora). Its rural population constitutes more than one-third of the total northern population5. The distribution of physicians practising between Ontario's northern urban and rural communities is disproportionate, with 71% of northern physicians practising in urban areas, where only 59% of northern Ontarians live6. Physician recruitment and retention to rural, remote and northern areas of the province has been a priority for the Ministry of Health and Long-term Care in Ontario. However, despite significant efforts to resolve physician shortages in underserved communities, recruitment and retention strategies to date have met with limited success2.
Pong and Russell established family physicians (FPs) and general practitioners (GPs) as the foundation of the health care in rural and remote regions7. On average, rural and remote GP/FPs see more patients per week, work longer hours, have a broader scope of practice, are on call more often, and provide more complex care7-10. In addition, they are more likely to do obstetrics, home visits and provide emergency and in-hospital care for patients9,10. Several factors have been found to have a negative impact on the mental and physical health of GP/FPs in rural and northern locations; these include isolation, heavy workloads, gruelling schedules and limited professional backup11.
There is a tendency in Ontario policies to conflate 'northern' with 'rural' and to equate northern rural settings with southern rural ones. Southern rural Ontario consists primarily of agricultural communities in contrast to the mining and forestry based economies in northern rural settings. Although previous research has identified some differences between rural and urban practitioners, these studies have not acknowledged the subtle nuances that make rural practice different in the north than in the south. Northern Ontario is three times larger in area than southern Ontario yet only has less than 7% of the province's total population5. GPs and FPs practising in the north are thus more likely to be in a remote location and are at a greater distance from tertiary care than those who practise in the south12. Understanding the different needs of the rural north and rural south may provide important evidence for informed policy formation.
Previous research has reported differences between rural and urban areas in both northern and southern regions of the province in the Ontario physician population with regard to age, sex and International Medical Graduate status6. For instance, as degrees of rurality increased in northern areas, there were more male physicians, more younger physicians and lower proportions of international medical graduates. However, these findings only paint a partial picture. This study looks more closely at physician practice patterns and compares the number of hours worked per week, weekly patient volume and practice type for rural northern, rural southern, urban northern and urban southern physicians to provide a better understanding of primary care physician practice characteristics across regions of Ontario.
Data and study population
Data from the College of Physicians and Surgeons of Ontario (CPSO) Registry and 2007 annual membership renewal survey were used to gain a better understanding of GP and FP practice patterns across rural and urban areas of both northern and southern Ontario. The CPSO is the licensing and regulatory body of physicians in Ontario. Its register contains verified demographic, credential and practice location information for all physicians in Ontario. On a yearly basis, all physicians are required under regulation to renew their membership with the CPSO. As part of the membership renewal process, data are collected regarding features of physician practice organization/structure, workload, clinical activities and practice patterns. The survey has an overall response rate of 98%, although response rates on individual questions vary to some degree.
Geographic definitions
Primary practice addresses were coded to reflect acceptable definitions of 'rural' and 'northern', based on community population size and distance from urban centers, resulting in four geographic categories: rural north, rural south, urban north and urban south.
Rural categorization: From the CPSO registration database, the geographic location of the primary practice address was identified using the six-character postal code. Primary practice postal codes were linked to Canadian census subdivisions by using Statistics Canada's Postal Code Conversion Files. These provide a link between the six-character postal code and the standard 2001 Census geographic areas (dissemination areas, municipalities, census tracts, etc.)13. Unfortunately, there is no one single accepted definition for 'rural'. However, to remain consistent with previous Canadian rural health research6,14, Statistical Area Classification definitions were used to differentiate urban from rural. These define metropolitan influenced zones as areas of Canada outside of Census metropolitan areas (population of at least 100 000) and Census agglomerations (population of at least 10 000). Census metropolitan areas and agglomerations are classified as urban while all metropolitan influenced zones are considered rural6,14.
Northern categorization: As for the definition of 'rural', there is no universally accepted boundary dividing northern and southern parts of the province. The Forward Sortation Area of the Canadian postal codes was used to define 'northern'6. Those beginning with a 'P' were considered northern while those remaining (beginning with a 'K', 'L', 'M' or 'N') represented the southern regions of the province. Geographically speaking, this divide stretches from the base of Georgian Bay (roughly 45º latitude) and runs at a 45º angle towards the Quebec border.
Practice data
Practice data are self-reported in the CPSO annual membership renewal survey. Practice type was subdivided into three categories: solo practice, administrative group practice and clinical group practice.A solo practice was defined as a GP or FP who does not share staff, office space or patient records with another physician in their primary practice setting. An administrative group practice was described as a GP or FP who shares office space and/or staff, but not patient care or records. A clinical group practice was identified as a GP or FP who shares office space and/or patient records and care.
Hours worked reflect the number of hours a GP or FP spends in practice in a typical work week at their primary practice location. Physicians could choose one of four categories in the CPSO survey: 1-20 hours/week, 21-30 hours/week, 31-40 hours/week and 41 hours/week or more. The comparative analyses focused on physicians who worked 41 or more hours per week and those that worked 40 or fewer.
Patient visits represent the number of patients a GP or FP sees in a typical work week at their primary practice location. A choice of four categories was again given: 1-50 patients/week, 51-100 patients/week, 101-150 patients/week, and ≥151 patients/week. The comparative analyses grouped physicians into two categories: those who had 1-100 patient visits per week and those who saw 101 or more patients per week.
Analysis
Descriptive statistics and χ2 analyses were used to examine practice type, hours worked per week and number of patient visits per week for primary care physicians in Ontario's rural north, rural south, urban north and urban south.
Ethics approval
Ethical approval for this study was provided by the Laurentian University Research Ethics Board, Certificate #20080909.
A total of 22 688 Ontario physicians responded to the survey of which 10 968 (48.3%) were GP/FPs, where 6386 (58.2%) were College of Family Physicians of Canada (CFPC) certified FPs and 4582 (41.8%) were GPs. In the north, 62.2% of all physicians were GP/FPs compared to only 47.5% of physicians located in the south.
Distributions of solo and group practices in the urban south, the rural south and the urban north were similar (Fig1). Approximately 30% of physicians in these communities worked in a solo practice setting, fewer than 10% worked in administrative groups, and just over 60% worked in clinical groups. However, in the rural north, there were far fewer physicians in solo practice-type settings (18.9%) than in the urban north (31.1%) or in either the rural south (29.3%) or urban south (28.2%). In addition, there were more rural northern physicians practising in clinical groups (75.3%) than physicians in the urban north (60.6%), the urban south (62.5%) or the rural south (63.3%).
The rural north and urban south had the largest number of physicians working more than 40 hours per week, with 42.8% and 39.0% respectively. The rural north had the lowest proportion of physicians working 1-20 hours per week (9.7%). The highest proportion of physicians working 1-20 hours per week were found in the urban south (15.6%) and the rural south (13.9%) (Fig2).
The proportions of physicians in each type of practice setting who worked more than 40 hours per week in the urban north and rural south were similar (range: 30.7-34.1%). However, the urban south and rural north stood out. The highest proportion of solo practice physicians and administrative group physicians working more than 40 hours per week were located in the urban south, representing 51.8% and 41.4% of physicians respectively. The lowest proportion of solo physicians working more than 40 hours per week were located in the rural north (25.5%). The rural north also had the highest proportion of clinical group physicians working more than 40 hours per week at 47.7%, compared to the other geographic regions, which range between 32.5% and 34.0% (Fig3).
Much like hours worked per week, the number of patient visits per week had similar distributions in the rural south and urban north, with an almost even split in the proportion of physicians who had 1-100 patients visits per week and those who had more than 100 visits per week. Once again, the urban south and rural north distributions stood out. The urban south had the highest proportion of physicians, with more than 100 patients visits per week (55.1%) in contrast to that found in the rural north, which had the fewest (37.8%) (Fig4).
Urban centre physicians in a solo or administrative group practice had the most patient visits. The urban south had the largest proportion of physicians seeing more than 100 patients per week in a solo practice (64.8%) and in clinical groups (50.3%). The largest proportion of administrative group physicians seeing more than 100 patients per week were located in the urban north (72.2%). The rural north had the smallest proportion of physicians seeing more than 100 patients per week in all practice types, with 45.1%, 18.8% and 37.7% of solo, administrative group and clinical group physicians, respectively (Fig5).
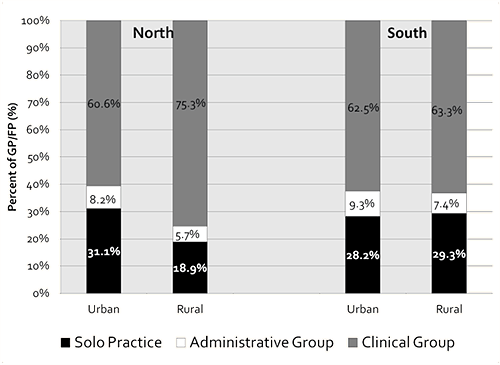
Figure 1: Distribution of practice structures for general and family
practitioners (GP/FPs) in Ontario (2007) per geographic location (%). (χ2=24.8; p<0.001)
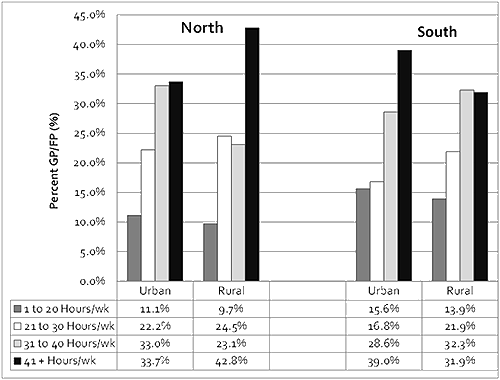
Figure 2: Distribution of hours worked per week by general and family
practitioners (GP/FPs) in Ontario (2007) per geographic location (%). (χ2=54.7; p<0.001)
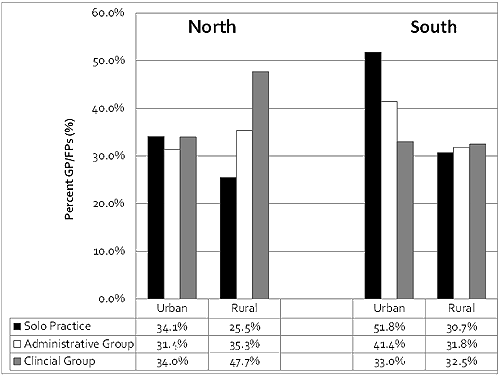
Figure 3: Percentage of general and family practitioners (GP/FPs) per
practice structure working ≥41 hours per week. (χ2=23.2; p=0.001)
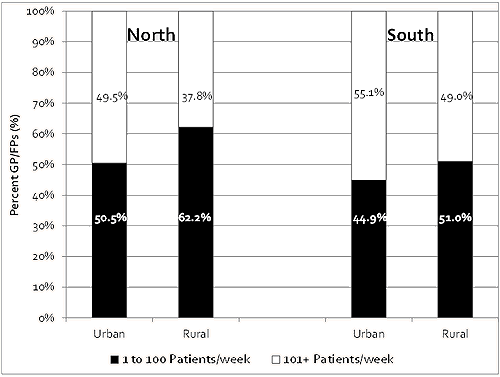
Figure 4: Distribution of patient visits per week by general
and family practitioners (GP/FPs) (%). (χ2=43.4; p<0.001)
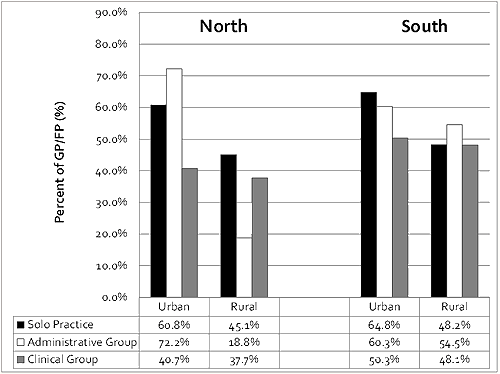
Figure 5: Percentage of general and family practitioners (GP/FPs) per
practice structure seeing ≥101 patients per week. (χ2=57.7; p<0.001)
Discussion
The practice types and workload patterns of rural northern physicians were distinctly different from the other regions of the province. The rural north had the highest proportions of physicians working in clinical groups (75.3%), working more than 40 hours per week (42.8%) and physicians seeing 1-100 patients per week (62.2%); and the lowest proportions of solo practitioners (18.9%), physicians working only 1-20 hours (9.7%) and physicians seeing 101 or more patients per week (37.8%). The physicians in the urban south had somewhat similar patterns of practice types to those in the urban north and rural south but often stood in stark contrast to the physicians in the rural north for the other variables investigated.
The largest proportion of physicians working in clinical group practices were found in rural northern areas, which also have the fewest in solo practices. Rural northern physicians may favour clinical group practices: some of the key factors cited as important for both recruitment and retention of physicians in rural areas include adequate collegial support, strong professional relationships and working in a team environment all of which are potentially more readily available in a clinical group than an isolated solo practice setting15.
In addition, findings from previous research indicated that more younger and male physicians were working in northern and rural areas of the province compared to in the south6. A 2008 CPSO report highlighted that younger physicians are amongst the most likely to practise in a clinical group16, possibly also helping to explain why proportions of clinical group practices are higher in the rural north.
Additional regional differences were found when examining the number of hours GP and FPs worked per week. For instance, significantly more GP and FPs in the rural north work more than 40 hours per week compared to all other regional groups, especially compared to their counterparts in the rural south. This may be partially explained by the age and sex of the primary care providers in each of these areas. For example, older physicians who choose rural practice are doing so more frequently in the agricultural rural south and less so in northern rural communities6. Many older physicians who remain in practice do so by decreasing their activity level, working significantly fewer hours per week and narrowing their scope of practice17,18. The growing number of female physicians may further contribute to this finding. Specifically, female physicians are more frequently found in southern Ontario6 and, on average, tend to work fewer hours per week than male physicians during certain periods of their life (eg during childbearing years)19-21.
Overall, rural northern physicians see fewer patients per week than those in other regions of the province. In light of the statement above regarding numbers of hours worked and the heavy workload of rural northern physicians, the lower number of patients may seem contradictory. This contradiction is also exhibited when looking at the proportions of clinical group physicians working in the rural north; more of them are working more than 40 hours per week than clinical group physicians in other areas but fewer of them are seeing more than 100 patients per week. It appears that although there are more rural northern physicians working in clinical groups, they are working more hours and seeing fewer patients, both of which are different patterns than what might be expected in clinical group settings16,22. These patterns might indeed be unexpected if it were assumed that patient populations across all regions of Ontario were similar, but they are not.
Studies have shown that the population of rural Canada, and particularly the rural north, is less healthy than those in other regions. In particular, rural northerners are older, have lower socioeconomic status, have higher levels of chronic diseases, poorer lifestyle factors and, higher rates of trauma and obesity14,23-26. One can speculate that rural northern GP/FPs work more hours yet see fewer patients, even in a clinical group setting, because they need to spend more time with the patients that they have, given that these patients are statistically older and sicker than patients in other areas of the province.
Rural family practice often means working in a primary care office practice plus heavy on-call schedules and hospital responsibilities, which may include surgery, inpatient care, obstetrics, emergency department shifts and anesthesia27. Such a broad scope of practice may increase the numbers of hours worked per week while restricting patient volume.
Further studies are needed to investigate differences such as scope of services, and patient differences involving chronic illnesses or numbers of visits. Broader scope, more chronic illnesses, patients with fewer visits, and access barriers would likely result in longer visits and fewer visits.
The major strength of this study was that the entire Ontario physician population was examined - the largest workforce in Canada - providing a complete picture of GP and FP practice patterns. However, the CPSO data only provides a cross-sectional view. There is no information regarding how long physicians have been in their current practice settings, what influenced their decisions to locate in one area versus another, nor is there information on why physicians chose solo or other practice structures. Qualitative data regarding the rationale behind physicians' practice type decisions, hours worked per week and patient visits could provide valuable insight into why rural physicians in northern Ontario are working more hours per week while seeing fewer patients than doctors in other regions of the province. Future research needs to examine the current paradox seen in rural northern practice more closely. One would assume that longer hours worked would equate to seeing more patients. However, the findings from the present study do not support this notion. Thus, are rural northern physicians spending more time with their patients? Are they dealing with more complex medical cases? Or, is it simply an indication of their broader scope of practice? Additional studies are also needed to track the impact of walk-in clinics more prevalent in the highly populated areas, interprofessional teams, additions of emergency or hospitalist physician coverage, changes in rural hospitals and services provided, and changes in healthcare spending across the province specific to rural and most rural locations.
Lastly, although these data are from 2007, they offer an interesting baseline because this snapshot pre-dates the first graduating cohorts from the Northern Ontario School of Medicine, Canada's newest medical school, which was in part established to education students in the rural north to help support retention of physicians in the north. As such, future comparative studies will allow evaluation of the impact of these graduates on physician services in both the rural and urban communities of northern Ontario.
The purpose of this study was to determine if Ontario's rural and northern doctors practise differently to physicians in southern and urban areas of the province. Three salient points emerged from the analyses: (1) physicians in rural northern Ontario, on average, worked more hours per week than their counterparts in other regions of the province, yet (2) they saw fewer patients per week, and (3) worked more frequently in clinical team-based practices.
It remains clear that the interaction between rural and northern context is unique. Although it was not surprising that the biggest differences in physician practice patterns were found between the rural north and the urban south, there were also marked differences between rural areas in the north and south and also between northern rural and urban areas. As such a blanket 'rural' or 'northern' approach to policy development is likely to be ineffective. If the goal of policy is to help strategize effective physician recruitment and retention efforts, improve healthcare services in every region and ultimately redress health inequities, then a full understanding of regional differences is required to insure policies reflect these unique regional needs.
Acknowledgements
The authors thank the College of Physicians and Surgeons of Ontario for providing access to the anonymized data used for this study. The CPSO was not involved in the design, conduct of the study, management, analysis or interpretation of the data, or the preparation, review or approval of the manuscript.
References
1. Goertzen J. The four-legged kitchen stool. Recruitment and retention of rural family physicians. Canadian Family Physician 2005; 51: 1181-1186.
2. Pong RW. Strategies to overcome physician shortages in northern Ontario: a study of policy implementation over 35 years. Human Resources for Health 2008; 6: 24.
3. Ryan-Nicholls KD. Health and sustainability of rural communities. Rural and Remote Health 4(1): 242 (Online) 2004. Available: www.rrh.org.au (Accessed 25 October 2013).
4. Rourke J. Increasing the number of rural physicians. Canadian Medical Association Journal 2008; 178(3): 322-325.
5. Ontario Ministry of Northern Development and Mines. Northern Ontario: a profile. Available: http://s3.amazonaws.com/zanran_storage/www.mndm.gov.on.ca/ContentPages/2446172434.pdf (Accessed 16 June 2014).
6. Wenghofer EF, Timony PE, Pong RW. A closer look at Ontario's northern and southern rural physician demographics. Rural Remote Health 11(2): 1591 (Online) 2011. Available: www.rrh.org.au (Accessed 25 October 2013).
7. Pong RW, Russell N. A review and synthesis of strategies and policy recommendations on the rural health workforce: a component of the Ontario Rural Council project Toward a Comprehensive Rural Health Human Resource Strategy for Ontario (Online) 2003. Available: http://www.cranhr.ca/pdf/TORC_Ruralhealthworkforcesynthesis-finaldraft-May.pdf (Accessed 25 October 2013).
8. Hutten-Czapski P, Pitblado R, Slade S. Short report: scope of family practice in rural and urban settings. Canadian Family Physician 2004; 50: 1548-1550.
9. Chan BT, Schultz SE. Supply and utilization of general practitioner and family physician services in Ontario. (Online) 2005. Available: http://www.ices.on.ca/Publications/Atlases-and-Reports/2005/Supply-and-utilization (Accessed 16 June 2014).
10. Tepper J, Schultz SE, Rothwell DM, Chan BT. Physician services in rural and Northern Ontario. (Online) 2006. Available: http://www.ices.on.ca/Publications/Atlases-and-Reports/2006/Physician-services-in-rural-and-northern-Ontario (Accessed 16 June 2014).
11. Kermode-Scott B. Alberta doctors warming up to peer-assessment program. The Medical Post, 14 March 2000; 45.
12. Glazier RH, Gozdyra P, Yertsyan N. Geographic access to primary care and hospital services for rural and northern communities: Report to the Ontario Ministry of Health and Long-Term Care. (Online) 2011. Available: http://www.ices.on.ca/Publications/Atlases-and-Reports/2011/Geographic-Access-to-Primary%20Care (Accessed 16 June 2014).
13. Statistics Canada. Postal Code Conversion File (PCCF) (product main page 2011). Available: http://www5.statcan.gc.ca/bsolc/olc-cel/olc-cel?catno=92F0153X&lang=eng (Accessed 27 February 2013).
14. DesMeules M, Pong R, Lagace C, Heng D, Manuel D, Pitblado R, et al. How healthy are rural Canadians? An assessment of their health status and health determinants. (Online) 2006. Available: https://secure.cihi.ca/free_products/acknowledgements_rural_canadians_2006_report_e.pdf (Accessed 25 October 2013).
15. Viscomi M, Larkins S, Gupta TS. Recruitment and retention of general practitioners in rural Canada and Australia: a review of the literature. Canadian Journal of Rural Medicine 2013; 181: 13-23.
16. College of Physicians and Surgeons of Ontario. Reaping the rewards - striving for sustainability: 2007 registration statistics and survey findings. (Online) 2008. Available: http://www.cpso.on.ca/cpso/media/uploadedfiles/downloads/cpsodocuments/policies/positions/reaping-the-rewards-survey_07.pdf (Accessed 16 June 2014).
17. Pong RW, Canadian Institute for Health Information, Canadian Electronic Library, Canadian Electronic Library. Putting away the stethoscope for good? Toward a new perspective on physician retirement. (Online) 2011. Available: https://secure.cihi.ca/estore/productFamily.htm?locale=en&pf=PFC1609 (Accessed 2 June 2013).
18. Pong RW, Lemire F, Tepper J. Physician retirement in Canada: what is known and what needs to be done? Paper prepared for the 10th International Medical Workforce Conference, Vancouver, 20-24 March 2007. Available: http://www.cranhr.ca/pdf/10_retCAN.pdf (Accessed 24 June 2013).
19. Buddeberg-Fischer B, Stamm M, Buddeberg C, Bauer G, Haemmig O, Knecht M, et al. The impact of gender and parenthood on physicians' careers - professional and personal situation seven years after graduation. BMC Health Services Research 2010; 10: 40.
20. Sarma S, Thind A, Chu MK. Do new cohorts of family physicians work less compared to their older predecessors? The evidence from Canada. Social Science and Medicine 2011; 7212: 2049-2058.
21. Crossley TF, Hurley J, Jeon SH. Physician labour supply in Canada: a cohort analysis. Health Economics 2009; 18(4): 437-456.
22. Slade S, Busing N. Weekly work hours and clinical activities of Canadian family physicians: results of the 1997/98 National Family Physician Survey of the College of Family Physicians of Canada. Canadian Medical Association Journal 2002; 166(11): 1407-1411.
23. North East Local Health Integration Network. North East LHIN demographic, socioeconomic, population health profile. (Online) 2008 Available: http://nelhin.on.ca/WorkArea/showcontent.aspx?id=3366 (Accessed 21 August 2012).
24. North West Local Health Integration Network. Population health profile: North West LHIN. (Online) 2011. Available: http://www.northwestlhin.on.ca/uploadedFiles/Home_Page/Report_and_Publications/North%20West%20LHIN%20Population%20Health%20Profile%202009%20v.2.pdf (Accessed 21 August 2012).
25. Bouchard L, Batal M, Imbeault P, Gagnon-Arpin I, Makandi E, Seigh G. La santé des Francophones de l'Ontario: un portrait régional tiré des Enquêtes sur la santé dans lescollectivités canadiennes (ESCC). (Online) 2012. Available: http://www.rrasfo.ca/images/docs/publications/2012/rapport_escc_ontario-final.pdf (Accessed 2 June 2013).
26. Picard L, Allaire G. Second report on the health of Francophones in Ontario 2005. (Online) Available: http://opha.on.ca/getmedia/f1d12c65-95ed-494e-8ab7-9b6c8b556bac/HealthofFrancophones-EN.pdf.aspx?ext=.pdf (Accessed 21 June 2013).
27. Incitti F, Rourke J, Rourke LL, Kennard M. Rural women family physicians. Are they unique? Canadian Family Physician 2003; 49: 320-327.


