Globally, in the past two decades, there has been an alarming increase in the burden of blindness. This continuing trend has been projected to result in the total of the world's blind people reaching 76 million in 20201. Approximately 90% of the world's blind and visually impaired (often from avoidable causes2) people live in low-income countries3 where resources for eyecare services are either inadequate or unaffordable. In Nigeria, 73.2% of blindness in persons aged 40 years or more has been attributed to avoidable and age-related causes4. The high burden of avoidable (preventable and curable) blindness and other non-blinding eye disorders in Nigeria is attributable to scarcity of human and material resources for eyecare delivery, sub-optimal functionality and restricted availability of the recently introduced public health insurance scheme.
Health-seeking behavior and pathways to health care in a community directly reflect the inhabitants' knowledge, understanding, and attitude towards health issues5,6 and their ability to overcome cost- and distance-related healthcare access barriers. Identifying the competing pathways to eye care and integrating them into an eyecare program will enable more efficient, effective, promotive, preventive, and curative eye health activities, tailored to the needs of the community. The positive role of eye health promotion in the elimination of avoidable blindness has been emphasized by Hubley and Gilbert7. Additionally, they observed that comprehensive understanding of all eye health issues by healthcare consumers is critical for success of promotive eye health interventions. Background research data on what the healthcare consumer thinks, knows, and does about a particular health concern are essential ingredients for the development of effective health education strategies7. Community-based health education assists individuals in overcoming ignorance-related access barriers to available orthodox eyecare services8.
Previous studies9-13 have identified varying first points of contact in eye care and critical inadequacies in eye health-seeking behavior of the study populations. A study in India9 reported that ophthalmologists were approached last for eye care, after traditional healers and general physicians. In a Malawian study10, even for perceived serious eye conditions, 22.2% of the participants would resort to self-treatment first, 22.6% preferred treatment from a traditional healer, while 55.2% would seek orthodox care. In a south-west Nigerian study11, 56.4% of the participants first consulted alternative medical practitioners before accessing conventional eyecare services. Authors of another related Nigerian12 report observed that orthodox treatment for the wards' eye disorders was sought by 61.7% of parents/guardians, 9.3% embarked on self-medication, while 21.3% ignored the condition. Similarly, in south-south Nigeria13, it was observed that 14.1% would resort first to self-medication, 7.2% to patent medicine shops, and 4.8% to traditional healers.
There is a paucity of rural population-based research data on the first points of contact/initial pathways to eye care in Nigeria. Previous Nigerian reports have been about ophthalmic outpatients11, students' eye health12 and that of urban-based civil servants13. Such indigenous data provide an indispensable guide for evidence-based community-level eyecare interventions.
In response to this research need, the investigators embarked on a population-based survey of adult inhabitants of Abagana, a rural community in Anambra state, south-east Nigeria. The present study aimed to identify the respondents' first points of contact with the eyecare system (traditional or orthodox), reasons for choice of contact point, and the factors associated with these characteristics. Specifically, the study set out to address the question, 'How do socio-demographic characteristics influence rural patients' initial choices of eyecare pathway when confronted with a major eye disease?' The generated data can potentially assist eyecare policymakers, implementers of eyecare programs, and providers of eyecare services to formulate and deploy community-based strategies to optimize delivery and uptake of appropriate eyecare services in the community, and under similar rural settings elsewhere.
Background
Anambra state, one of the five component states of Nigeria's south-east geopolitical zone, is made up of 21 administrative subunits or local government areas (LGAs). Abagana, the study community, is one of the six rural communities that make up Njikoka LGA, which is one of Anambra state's LGAs. The other communities are Abba, Enugwu Agidi, Enugwu Ukwu, Nawfia, and Nimo. Each LGA is further subdivided into smaller administrative subunits called political wards. Each ward is represented in the LGA council by an elected councilor.
Abagana is located in the tropical rainforest climatic belt. It has a mean annual rainfall of 1200-2000 mm, with a rainy and dry season each year. The majority of the roads interconnecting the component villages are sealed and the means of transportation are motorized two-wheeled vehicles (motorbikes), small commuter buses, motorized tricycles, and bicycles. Electricity is available in all the villages, and all of the major mobile telephone networks in Nigeria cover the area. The total projected population of Abagana is 36 57514. The inhabitants of Abagana are ethnic Ibos whose main occupations are farming and petty trading, with an appreciable number of civil servants and artisans. Christianity is the predominant religion, although there are pockets of other religions. Abagana has one comprehensive health center (CHC), a rural outpost of University of Nigeria Teaching Hospital (UNTH), Enugu. At the CHC, orthodox eyecare services, including medical, minor surgical and refraction services, are provided by a visiting eyecare team from the base hospital, UNTH. However, there are numerous privately owned orthodox health care facilities in the community and its environs. Of these, only one privately owned healthcare facility provides eyecare services to the inhabitants of Abagana community. It is located two communities away from Abagana.
Study design and settings
This was a descriptive, cross-sectional, population-based study conducted in Abagana, in September 2011. The study instrument (Appendix I) was a pre-tested, open-ended, researcher-administered questionnaire with subfields on respondent sociodemographics (age, sex, educational status, marital status, and occupation), eye health-seeking behavior, first points of contact while seeking eye care, and barriers to accessing orthodox eyecare services (ie reasons for not consulting an ophthalmologist) when confronted with any of the following major eye diseases: cataract, glaucoma, diabetic retinopathy, refractive error, and eye infection.
Prior to final deployment for data capture, and to ascertain its construct validity and psychometric reliability, the study instrument was pre-tested on volunteers under similar settings, outside the study area. Feedback from the pre-test informed modifications in the questionnaire to enhance its face (surface validity), flow and interpretation, and its ability to achieve the study objectives.
Eligibility
Adult men and women aged 18 years or more, who had resided in Abagana community for at least 6 months, and who voluntarily consented to participation, were included in the study.
Sample size and sampling
The calculated minimum sample size of 245 was based on a previously reported 20%9 prevalence and an error band of 5%. To obtain a better representation of the population, a cluster random sampling technique was used; the minimum sample size was multiplied by a design effect of 2, to obtain 490. This was further inflated to achieve a modified sample size of 501 to take into account refusals to participate.
A multi-stage cluster random sampling technique was used. The 10 villages present in Abagana already consisted of four political wards, which served as sampling clusters: ward 1 (Adaegbe-Umudunu and Uru-Okpala; total population 8071); ward 2 (Enuora-Oraofia and Adaegbe-Oraofia; total population 8829); ward 3 (Enuora-Umudunu and Amagu; total population 7566); and ward 4 (Akpu, Amaenyi, Uru, and Adaegbe; total population 12 106). The proportion of the 501 participants to be drawn from each ward was calculated based on proportionate representation: ward 1=111, ward 2=121, ward 3=104, and ward 4=165. Using a simple random sampling, 5 out of the 10 villages were selected and their households were enumerated to obtain a sampling frame. The selection from each cluster/ward was: ward 1=Uru-Okpara, with 709 households; ward 2=Enuora-Oraofia, with 728 households; ward 3=Enuora-Umudunu, with 698 households; ward 4=Akpu, with 463 households, and Adaegbe, with 485 households. Using systematic random sampling (N/n, where N=total population for each ward and n=calculated proportion of the 501 participants to be drawn from each ward), every sixth household in Uru-Okpara, Enuora-Oraofia, Akpu, and Adaegbe, and every seventh household in Enuora-Umudunu were selected until the required sample size of 501 households was obtained. From each of the selected households, one eligible adult was selected for recruitment, by balloting. Each selected participant was interviewed in his/her home, on an individual, one-on-one basis.
Eye disease definitions
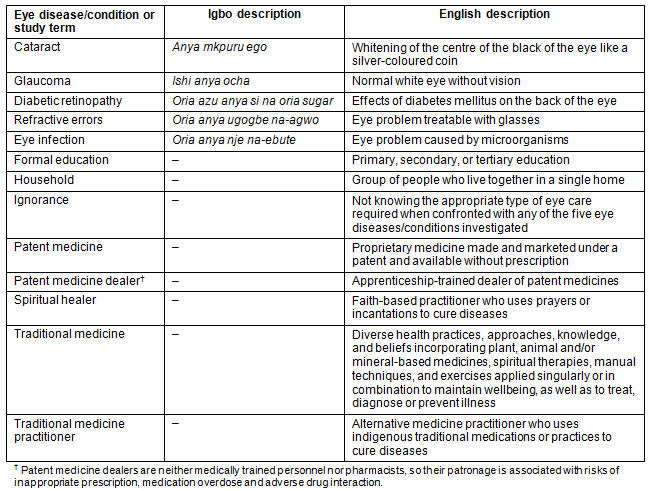
Each of the five eye diseases investigated and, where necessary, other relevant terms, were literally explained to the participants in English and in their native/local Igbo language where possible as shown in Table 1.
Table 1: Definitions of eye diseases/conditions and other terms used in the study
Data analysis
Data were cleaned, edited, coded, and analyzed using the Statistical Package for Social Sciences v18.0 (SPSS Inc., http://www.spss.com). Data were subsequently categorized by sociodemographic variables and subjected to descriptive statistical evaluation to yield frequencies, percentages, and proportions. Tests for significance of observed between-class differences utilized the χ2 test for categorical (gender, educational status, occupational status, marital status) variables and the student t-test for continuous (age) variables. Predictor variables that were retained at univariate analysis as significant predictors of consulting an ophthalmologist were selected and entered into a multivariate logistic regression model to ascertain their independent influence on the outcome of interest, consulting an ophthalmologist. A p<0.05 at one degree of freedom (df=1) was considered statistically significant.
Ethics approval
Prior to commencement of the study, ethics clearance compliant with the 1964 Helsinki Declaration was obtained from UNTH's Medical and Health Research Ethics Committee (Institutional Review Board).
The 501 study participants comprised 263 (52.5%) men and 238 (47.5%) women (sex ratio: M:F=1.1:1) who were aged 48.9±16.3 years (range 18-93 years) with a modal age group of 41-50 years. The sociodemographic characteristics of the participants are shown in Table 2.
The majority of the participants would first consult a patent medicine dealer (PMD) (178; 35.5%) or an ophthalmologist (165; 33.0%) if confronted with an eye disease, while the smallest (8; 1.6%) number of participants would resort to prayer/spiritual consultation (Fig1).
The participants reported that reasons for not consulting an ophthalmologist were ignorance (190; 56.5%), lack of finance (199; 59.2%), poor access to eyecare services (228; 67.9%), self-assessment of the eye disease as not serious (105; 31.3%), belief that aging has no cure (68; 20.2%) and preference for spiritual treatment (3; 0.9%). The number of reasons cited for not consulting an ophthalmologist was zero for 165 (32.9%) participants, one for 92 (18.4%) participants, two for 95 (18.9%) participants, three for 127 (25.3%) participants, 4 for 21 (4.2%) participants and five for one (0.2%) participant. In the univariate analysis, younger age, being single and possession of formal education were the significant sociodemographic predictors of consulting an ophthalmologist (Table 3).
However, in the multivariate model, possession of a formal education was the only significant predictor of consulting an ophthalmologist when confronted with any of the five major eye diseases investigated (Table 4).
Table 2: Participants' sociodemographic characteristics
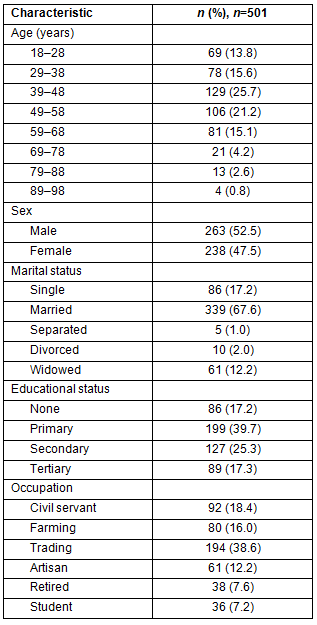
Table 3: Univariate associations between participants' sociodemographics and consulting an ophthalmologist when confronted with a major eye disease
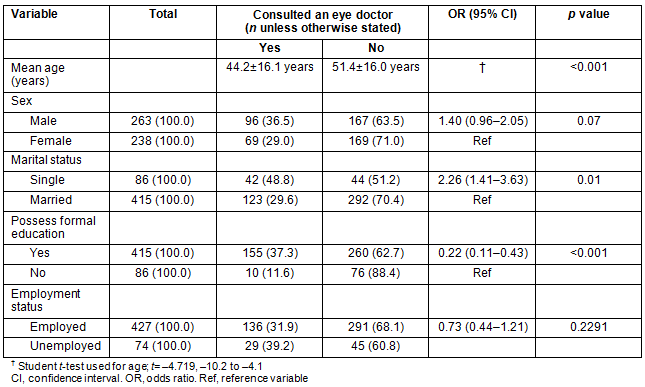
Table 4: Multivariate analysis of factors potentially associated with consulting an ophthalmologist
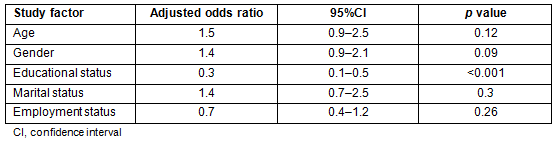
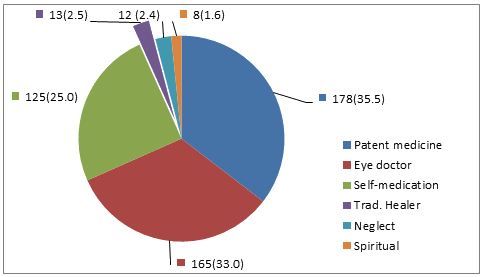
Figure 1: Participants' initial pathway to eye care when confronted with an eye disease.
Discussion
The participants comprised more men than women, were frequently married, possessed a formal education, and were predominantly traders. Their sociodemographic profile is in partial agreement with a Nigerian study11 whose participants had a similar age distribution, but differed markedly in other sociodemographic indices. While between-survey differences in study design might account for these observed differences, further comparisons with other reports in Nigeria15 and other countries9,10 have been restricted by their lack of equivalent comparable data. This suggests the need for generation of comparative sociodemographic data on eyecare pathways in Nigerian populations, and in other countries.
When confronted with an eye disease, the majority of participants in the present study would consult a PMD or an ophthalmologist, while few would resort to self-medication. This contrasts with a finding in India9 where traditional healers were consulted first, in Malawi10 and elsewhere in Nigeria11-13,15,16 where the participants would first embark on self-medication, and in Ghana17 where the majority would first consult an ophthalmologist followed by a PMD ('chemical shop attendants') and self-medication. However, in the USA18, equivalent data on PMDs have not been reported due to rarity, if not non-existence, of this sub-group of healthcare providers in the USA. The similarity of the present findings to other reports could be attributable to similar socioeconomic settings and the resultant restricted availability and/or accessibility of orthodox eyecare providers compared with PMDs in these low- and medium-income countries. To reverse this trend, the present data suggest the need for eye health education on appropriate eyecare pathway selection. Additionally, educating PMDs on the rudiments of eye care, and possibly incorporating them into an orthodox eyecare system, should be considered. Furthermore, orthodox eyecare services should be made widely available and accessible to overcome the distance- and cost-related access barriers. Educating the public on the dangers of consulting PMDs without providing affordable and practical alternatives might not produce the desired paradigm shift in the pattern of eyecare pathway selection.
In the present survey, resorting to prayer/spiritual consultation and patronage of traditional medical practitioners were chosen by some participants. This finding, which was previously reported in Nigeria11-13,15,17, partially agrees with the reported resort to spiritual cure in the USA18 and consultation with traditional healers/herbalists observed in India9, Ghana16, and Malawi10. The residual influence of African traditional religion and beliefs may explain these observations. Given the circumstances, persons afflicted with an eye disease seek alternative spiritual cure by appeasing the gods of the land, instead of accessing orthodox eyecare services15. These practices are detrimental to eye health because they prolong the patient's time to presentation for eye care and jeopardize treatment outcomes. Measures to reverse this trend should include health education campaigns, and increased availability and affordability of eye care. Traditional healers should be provided basic eyecare education, and incorporated into an orthodox eyecare system.
In this survey, possession of formal education was the only sociodemographic characteristic significantly predictive of consulting an ophthalmologist. This is consistent with findings in Nigeria19, Kenya20, and Australia21. Possession of a formal education creates an avenue for health literacy and increases the appetite for broad/horizontal knowledge, including health issues. Therefore, making formal education available and affordable to all persons would be useful for enhancing the effect of eyecare interventions.
In the present study, poor access to eyecare services, cost, and ignorance were the respondents' main reasons for not consulting an ophthalmologist in the event of an eye disease. These findings are similar to those reported in Kenya20, where cost and ignorance were the main reasons for not consulting an ophthalmologist, and in Nigeria11, where the main reasons given for engaging in non-doctor consultation included 'no nearby hospital'. Consequently, the investigators recommended increasing the availability and affordability of orthodox eyecare services, and awareness creation/enhancement of eye health maintenance.
The generalizability of the results of the present survey is restricted by the possibility of participants' recall bias. Additionally, rural and underserved study settings impose further limitations in data extrapolation to non-rural populations. Therefore, the investigators suggest the inclusion of mechanisms to cross-validate participants' reported data in the design of future surveys.
In Abagana, the majority of inhabitants would first consult a PMD before an ophthalmologist in the event of an eye disease. Poor access, cost, and ignorance are their main reasons for not consulting an ophthalmologist first. Enhanced accessibility and subsidization of eyecare services, integration of alternative eyecare providers into an orthodox eye care system, and eye health literacy campaigns might reverse this trend.
References
1. Resnokoff S, Pascolini D, Etiga'ale D, Kocur I, Parajasegaram R, Palcharel GP, et al. Global data on visual impairment in the year 2002. Community Eye Health Journal 2004; 17(52): 61.
2. Resnikoff S, Pascolini D, Etya'ale D, Kocur I, Parajasegaram R, Palcharel GP, et al. Global data on visual impairment in the year 2002. Bulletin of the World Health Organization 2004; 82: 844-851.
3. WHO. Blindness and visual impairment: global facts. WHO data as released to International Agency for the Prevention of Blindness, 2010. Available: http://www.vision2020.org (Accessed 23 January 2013).
4. Kyari F, Gudlavalleti MV, Sivsubramaniam S, Gilbert CE, Abdull MM, Enetekume G, et al. Prevalence of blindness and visual impairment in Nigeria: the National Blindness and Visual Impairment Study. Investigative Ophthalmology & Visual Science 2009; 50(5): 2033-2039.
5. WHO. Vision 2020 - World Health Organisation, action plan 2006-2011 ... global initiative for the elimination of avoidable blindness. (Online). Available: http://www.who.int/blindness/Vision2020_report.pdf (Accessed 15 March 2013).
6. Kaliyaperumal K. Guideline for Conducting a Knowledge, Attitude and Practice (KAP) Study. Indian Journal of Ophthalmology 2004; 4: 7-9.
7. Hubley J, Gilbert C. Eye health promotion and the prevention of blindness in developing countries: critical issues. British Journal of Ophthalmology 2006; 90: 279-284.
8. Livingston PM, McCarty CA, Taylor HR. Knowledge, attitudes, and self-care practices associated with age related eye disease in Australia. British Journal of Ophthalmology 1998; 82: 780-785.
9. Nirmalan PK, Sheeladevi S, Tamilselvi V, Victor AC, Vijayalakshmi P, Rahmathullah L. Perceptions of eye diseases and eye care needs of children among parents in rural south India: The Kariapatti Pediatric Eye Evaluation Project (KEEP). Indian Journal of Ophthalmology 2004; 52: 163-167.
10. Bisika T, Courtright P, Geneau R, Kasote A, Chimombo L, Chirambo M. Self treatment of eye Diseases in Malawi. African Journal of Traditional, Complementary, and Alternative Medicine 2009; 6(1): 23-29.
11. Fasina O, Ubah JN. Pattern of pre-hospital consultation among ophthalmic patients seen in a tertiary hospital in South West Nigeria. African Journal of Medicine and Medical Sciences 2009; 38(2): 173-177.
12. Ayanniyi AA, Olatunji FO, Mahmoud AO, Ayanniyi RO. Knowledge and attitude of guardians towards eye health of primary school pupils in Ilorin, Nigeria. Nigerian Postgraduate Medical Journal 2010; 17(1): 1-5.
13. Dawodu OA, Okogie OH, Ukponmwan CO. Pattern of utilisation of eye care services in Benin City, Nigeria. Nigerian Postgraduate Medical Journal 2006; 13(4): 323-325.
14. National Population Commission. Nigerian population census 1991 analysis. Volume 3: The elderly. (Online) 2003. Available: http://www.ibenaija.org/uploads/1/0/1/2/10128027/the_elderly.pdf (Accessed January 2013).
15. Nwosu SN. Beliefs and attitude to eye diseases and blindness in rural Anambra state Nigeria. Nigerian Journal of Ophthalmology 2002; 1(1): 16-21.
16. Ayanniyi AA, Jamda AM, Badmos KB, Adelaiye RS, Mahmoud AO, Kyari F, et al. Awareness and knowledge of ocular cancers in a resource-limited economy. North American Journal of Medical Sciences 2010; 2: 526-531.
17. Ntim-Amponsah CT, Amoaku WMK, Ofosu-Amaah S. Alternate eye care services in a Ghanaian District. Ghana Medical Journal 2005; 39(1): 19-23.
18. Magyar-Russell G, Fosarelli P, Taylor H, Finkelstein D. Ophthalmology patients' religious and spiritual beliefs: an opportunity to build trust in the patient-physician relationship. Archives of Ophthalmology 2008; 126(9): 1262-1265.
19. Adegbehingbe BO, Bisiriyu LA. Knowledge, attitudes, and self-care practices associated with glaucoma among hospital workers in Ile-Ife, Osun State, Nigeria. Tanzanian Journal of Health Research 2008; 10(4): 240-245.
20. Ndegwa LK, Karimurio J, Okelo RO, Adala HS. Barriers to utilisation of eye care services in Kibera slums of Nairobi. East African Medical Journal 2005; 82(10): 506-508.
21. Attebo K, Mitchell P, Cumming R, Smith W. Knowledge and beliefs about common eye diseases. Clinical Experiments in Ophthalmology 1997; 25(4): 283-287.
_______________________
Appendix I: Knowledge, attitude and self-care practice survey on eye diseases in Abagana community, Anambra State, Nigeria. Study questionnaire






