Approximately 900 000 patients are affected by heart failure in the UK and approximately 1 million individuals greater than 65 years of age are estimated to have valvular heart disease1,2. Transthoracic echocardiography is a sensitive and cost-effective approach in detecting both conditions. Direct access echocardiography allows general practitioners (GPs) to directly request echocardiography without the involvement of a cardiologist in cases of suspected heart failure or presence of murmur. Locally, echocardiography is performed and reported by British Society of Echocardiography-accredited sonographers accompanied by comments from a cardiologist where necessary. However, access to echocardiography remains a challenge, especially in the rural setting.
The echocardiography service provided by the authors is centralised at Raigmore Hospital within the city of Inverness, serving the wider population of 200 000 scattered across 31 000 km2 in the sparsely populated Scottish Highlands. The Scottish Government recommends healthcare services to be provided as locally as possible3. While this concept presents many advantages at its outset, it is logistically challenging. This study aimed to examine whether practice location in remote and rural areas in the Scottish Highlands affected the pattern of referral made over a 3-year period and to assess any variations in echocardiographic findings. This is the first large study on direct access echocardiography in a remote and rural setting.
All outpatient referrals made by all GP practices in the Scottish Highlands over a 36-month period between January 2008 and January 2011 were analysed. The study period represents the second, third and fourth years of direct access echocardiography service at Raigmore Hospital since its inception in 2007. Data were collected from referral forms and echocardiogram reports.
Indications for referral were developed locally by GPs, cardiologists and the echocardiography department. Patients are required to have one of the following conditions to qualify for referral to the direct access echocardiography service: suspected heart failure, new murmur, suspected cardiomyopathy or new onset atrial fibrillation. Those with suspected heart failure required at least an abnormal ECG, abnormal chest radiograph or a history of myocardial infarction. Those referred for cardiomyopathy require at least an abnormal ECG and a first-degree relative with familial dilated or hypertrophic cardiomyopathy. Patients with murmur who had previously had valve surgery and those with atrial fibrillation of more than a year's duration were redirected to the cardiology clinic.
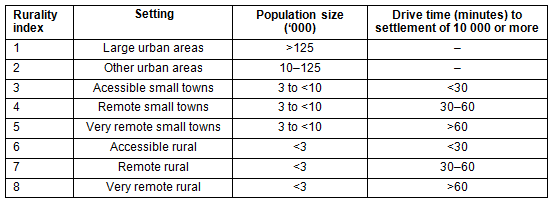
The primary aim was to examine the pattern and indications for referral. The number of referrals from each GP practice was compared in relation to the population size and rurality index. Rurality index was allocated according to the Scottish Government's Urban-Rural Classification (Table 1)4. Since rurality index does not strictly measure distance, further analysis on how distance is related to GP practices' rurality index was undertaken.
The secondary aim was to examine the cardiac abnormality detection rate of positive echocardiographic findings. Outcomes of echocardiographic findings were divided into normal and abnormal studies. Abnormal studies were further divided into those who required cardiology follow-up or surveillance and those who did not. All abnormal studies regardless of the need for follow-up were included in the cardiac abnormality detection rates. To avoid bias due to small numbers of referrals by certain practices, all practices within each rurality group were combined in order to report the cardiac abnormality detection rate.
Linear regression was applied to examine the relationship between distance and referral rates, and between referral rates and cardiac abnormality detection rates. The Kruskall-Wallis test was used to compare cardiac abnormality detection rates across different rurality index groups.
Table 1: The Scottish Government's Urban-Rural Classification
Ethics approval
This study was a retrospective service evaluation which did not involve contacting patients nor any form of randomisation and therefore did not require ethics approval.
Pattern of referral
A total of 1188 consecutive referrals made by 49 GP practices across the Scottish Highlands over the 3-year period were analysed. The total number of referrals from different GP practices ranged from 1 to 163 with a mean of 24 referrals. Referral rates corrected for population size ranged from 0.3 to 20.1 per 1000 population with a mean of 6.5 referrals per 1000 population over the sample period. Referral rates were not significantly different between urban and rural practices after correction for population size (Fig1) although variation in referral rates in rurality index 8 practices were greater than in rurality index 2 practices. All practices with rurality indexes of 7 and below are within 56 km of the centre, whereas all practices with an index of 8 are located beyond this distance. There was no correlation between the referral rates and the distance from the centre (r2=0.004, p=0.65; Fig2).
Referral indications
'New murmur' was the most common reason for referral, making up nearly half of the total referrals (46%), followed by suspected heart failure (34%), new onset atrial fibrillation (16%) and cardiomyopathy (4%). Only 25% of patients referred had an abnormal ECG. The most common presenting symptoms were breathlessness (44%) followed by dizziness or syncope (16%), chest pain (7%), oedema (7%), palpitations (6%) and 'others' (6%). Fourteen percent of patients did not have symptoms.
Outcomes and cardiac abnormality detection rates
Less than half (44%) of the studies performed were normal. Another 28% found mild or minimal abnormalities not requiring follow-up by cardiology services as per recommendations; these patients were returned to their GP for symptom surveillance and local management5. Altogether, 72% of patients referred did not require referral to cardiologists after echocardiographic examination. Only 28% had significant abnormalities detected and were subsequently referred to cardiologists for further assessment and follow-up. Amongst these, pure aortic (40%) and mitral valve disease (19%) formed the biggest proportion followed by left ventricular systolic dysfunction (12%).
There was no clear relationship between referral rates and cardiac abnormality detection rates (r2=0.07, p=0.37; Fig3). Cardiac abnormality detection rates for all practices in each rurality index group were remarkably similar with an average of 56%. They ranged from 52% for practices in rurality index 7 to 60% for practices in rurality index 5, with no statistically significant difference between rurality groups (p=0.891).
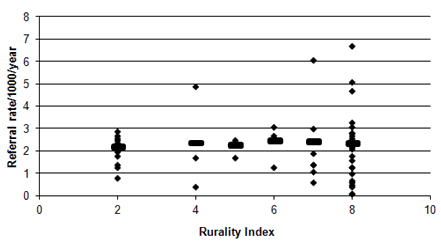
Figure 1: Referral rate in relation to 'rurality index'. Absence of rurality index 1 is because there are no cities with population greater than 125 000 in the Scottish Highlands. Line represents average across each rurality index group.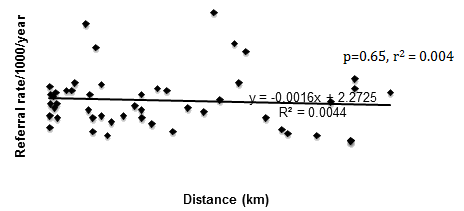
Figure 2: Rate of referral versus distance to Raigmore Hospital.
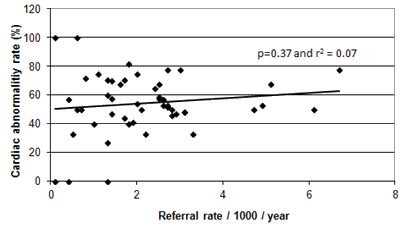
Figure 3: Relationship between rate of referral and cardiac abnormality detection rates.
An accessible echocardiography service is necessary for good cardiac care because the diagnostic accuracy of heart failure based on clinical findings without the aid of echocardiography remains low6-8. Also, echocardiography is the gold standard for assessing valvular disease. Echocardiography, which is primarily a hospital-based investigation, was historically only accessible following specialist consultations. Specialist assessment for every patient with suspected heart failure may result in poor utilisation of resources and diagnostic delay due to the large number of patients and the array of other conditions mimicking heart failure.
Direct access echocardiography programs have been available in the UK since the 1990s9. In this study, 72% of patients referred through a direct access echocardiography service did not require assessment by a cardiologist based on their echocardiographic findings, potentially saving 855 appointments in specialist clinics. Those with valvular disease and heart failure detected on echocardiograms were appropriately referred to a cardiologist for outpatient clinic follow-up. The cardiac abnormality detection rate of 56% in this cohort is low but is consistent with other studies10. Improvements to the currently adopted referral guidance may increase the cardiac abnormality detection rates but if too restrictive could delay patient diagnoses and ration appropriate use of echocardiography. Indeed, one could argue that a pick-up rate of 56% for a non-invasive test such as echocardiography reflects good clinical practice and supports the role of the primary healthcare provider in circumventing unnecessary cost as well as overburden on access to specialist care.
Direct access echocardiography services can take many forms, be it centralised or with peripheral clinics providing services as locally as possible. No studies have been done on optimal models but the best approach is likely to be one tailored to local needs. Although providing more local echocardiography clinics has some advantages, it is not without challenges in terms of cost-effectiveness, meeting waiting time requirements and sustainability, especially if there are low numbers of referrals from remote areas. This study has shown that distance and rurality do not appear to be a barrier to the use of a centralised direct access echocardiography service in the north of Scotland, which is somewhat reassuring, especially given governmental directives to provide services 'as local as possible'. Whilst rurality may not be a barrier to referral, the wide range of referral rates within each index suggests other factors could be influencing referral. This could include GP knowledge and understanding of the service and condition management pathways or pathology distribution. Some of this could be addressed by raising awareness of these findings to practices with very low referral numbers and cardiac abnormality detection rates.
This study made certain assumptions. In order to conclude that there is no barrier to access, an assumption that the prevalence of disease is comparable was made. One study from Australia demonstrated a higher incidence of congestive heart failure in remote areas, nearly 2% compared to 1.7% in urban areas (p<0.001)11. However, there is no evidence that such a gradient exists in Scotland and if it did the actual size of this gradient would be small. Other factors such as patient choice, mobility and personal circumstances have not been considered in this study. It is also worth noting that rural Scotland is much less remote compared to the Australian outback or northern Canada. Greater distances in those topographies may challenge any effort to provide equitable service.
The finding that there did not appear to be a geographical barrier in one of the more remote areas of the UK should also be of interest to those providing echocardiography services in less remote areas. If the authors were unable to show a geographical barrier in their healthcare setting then it is unlikely that those in less remote areas will be affected. Nevertheless, each local service should be cognisant of their own practice and the presence of other potential barriers such as cultural, communication and, in other private healthcare systems, cost. These results may interest not only practitioners treating suspected cardiac disease in remote and rural areas but also to service users such as those requiring access to endoscopy or radiology investigations.
This study demonstrates that rurality and distance are not barriers to an equitable direct access echocardiography service in the Scottish Highlands, which would seem to challenge the current political mantra that care provided as close as possible to the patient is superior. Further research could look at patients' satisfaction in using a centralised service.
Acknowledgements
Authors would like to thank Professor Ian Megson from the University of the Highlands and Islands and Dr Iain Atherton from the University of Stirling for their assistance in the statistical analyses.
References
1. National Health Service. Heart Failure - patient pathways. NHS improvement 2012. (Online). Available: http://www.improvement.nhs.uk/heart/heartfailure/Home/PatientPathways.aspx (Accessed 15 May 2013).
2. Malhotra A. The changing burden of valvular heart disease. British Cardiovascular Society editorial. (Online) 2012. Available: http://www.bcs.com/pages/news_full.asp?NewsID=19792059 (Accessed 15 May 2013).
3. National Health Service Scotland. Delivery for remote and rural healthcare. The final report of the remote and rural workstream. (Online) 2007. Available: http://www.scotland.gov.uk/Resource/Doc/222087/0059735.pdf (Accessed 15 May 2013).
4. Scottish Government. Scottish Government Urban Rural Classification. (Online) 2010. Available: http://www.scotland.gov.uk/Topics/Statistics/About/Methodology/UrbanRuralClassification (Accessed 15 May 2013).
5. ACC/AHA committee and taskforce members. ACC/AHA guidelines for the clinical application of echocardiography - a report of the American College of Cardiology/American Heart Association Task Force on practice guidelines. Circulation 1997; 95: 1686-1744.
6. Remes J, Miettinen H, Reunanen A, Pyorala K. Validity of clinical diagnosis of heart failure in primary health care. European Heart Journal 1991; 12: 315-321.
7. Wheeldon NM, MacDonald TM, Flucker CI, et al. Echocardiography in chronic heart failure in the community. Quarterly Journal of Medicine 1993; 86: 17-23.
8. Madhok V, Falk G, Rogers A, Struthers A, Sullivan F, Fahey T. The accuracy of symptoms, signs and diagnostic tests in the diagnosis of left ventricular dysfunction in primary care: a diagnostic accuracy systematic review. BMC Family Practice 2008; 9: 56.
9. Murphy J, Frain J, Ramesh P, Siddiqui R, Bossingham C. Open-access echocardiography to general practitioners for suspected heart failure. British Journal of General Practice 1996; 46(409): 475-476.
10. Khunti K. Systematic review of open access echocardiography for primary care. European Journal of Heart Failure 2004; 6(1): 79-83.
11. Clark RA, Mclennan S, Eckert K, Dawson A, Wilkinson D, Stewart S. Chronic heart failure beyond city limits. Remote and Rural Health 5: 443. (Online) 2005. Available: www.rrh.org.au (Accessed 26 November 2014).

