Introduction
In the last several years, rural issues have become increasingly prominent on Canada's health policy1 and research2 agendas. To support this shift, in 2002 the Canadian Rural Health Research Society (CRHRS) was established to help foster the nation's capacity for research on topics vital to the health of those who live in rural and remote parts of Canada. During its inaugural phase, the society undertook a country-wide scan of the research, teaching and training opportunities available to prepare the next generation of rural health researchers. This 'snapshot' was taken by means of a survey targeted at a comprehensive list of educational programs covering a wide range of health and science disciplines. It provides one baseline against which the society can measure progress over its first five-year mandate. The present project report gives an overview of the results, documenting the current strengths in Canada's system of education as it pertains to rural health research, but also the noticeable gaps that exist.
Methods
On behalf of the society, the authors undertook to administer a survey with the help of a research assistant based at the Centre for Rural and Northern Health Research (Lakehead Site)3. Its implementation was guided by the principles for designing on-line surveys set out by Dillman4. The instrument consisted of both closed- and open-ended questions, designed to find out about institutional commitments to rural health research training generally, and specifically about course offerings, infrastructure supports available for students, financial assistance for those studying relevant topics, and anticipated changes in the topic area. This tool was developed using Apian SurveyPro and NetCollect software (Apian Software, Seattle, WA, USA) and administered in a computer-mediated format, which allowed people to complete it online, thereby facilitating the process and speeding the analysis phase.
Ethical approval was obtained from Lakehead University before the study was conducted.
The survey was distributed to individuals in administrative positions (chairpersons, deans or co-ordinators) of 462 programs in 24 distinct disciplines at 56 institutions. 'Health' was defined broadly to include such professional programs as social work and some social sciences. Potential respondents were identified using the Association of Universities and Colleges in Canada (AUCC) 2000 Directory5, verified and updated where necessary through the various universities' websites or calendars. Although Dillman4 recommends multiple contacts, due to time constraints the survey was only distributed twice. Francophone programs were included in the email-outs, but the project's limited budget did not allow for translation of the questionnaire into French.
Results
Responses
Individuals from 120 academic programs based in 40 universities completed the questionnaire. This response was well distributed geographically, but was concentrated by discipline (Fig 1). The overall response rate (26%) was low and is a limitation of the study. One may argue that this was a result of the distribution strategy; specifically directing the survey to a relatively large number of programs which are not traditionally considered health disciplines and to a comprehensive list of universities, most of which did not have programs oriented to rural issues. Of the responding programs, 55 were from nursing, medicine or an allied area of health specialization, such as audiology or physiotherapy. Moreover, only 32 responses came from programs within institutions which did not have some rural specialization. This suggests that those for whom the survey was directly relevant were most likely to respond and, consequently, that the coverage more fully reflects the situation in the country than the response rate itself might indicate. Only providing the survey in English restricted participation from Francophone programs and, likewise, limits the generalizability of the study. For descriptive purposes in this brief project report, the findings are presented simply as percentages.

Figure 1: Responding programs by discipline
Course offerings
At present, course offerings are limited (Fig 2). Only 18.8% of the programs responding to the survey offered courses devoted to rural health; the existing courses tend to be in nursing and, to a lesser extent, in family medicine or psychiatry. That said, rural health is a component in at least some courses offered by 39.3% of the programs, across 17 disciplines.
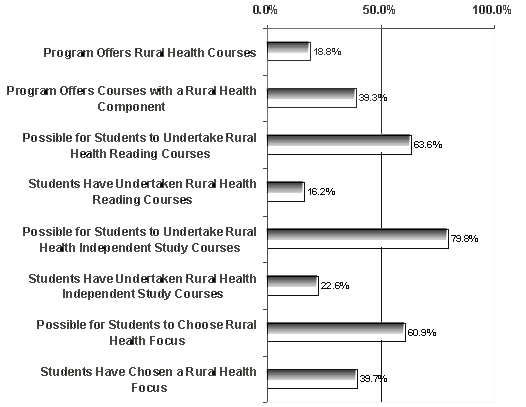
Figure 2: Rural health educational opportunities
In those areas of curricula shaped by student choices, however, rural content is a viable option. Reading courses and independent study courses in 63.6 and 79.8% of the programs, respectively, may be tailored to cover rural topics. Relatively few students do so, however: approximately 16.2 and 22.6%. However, overall, respondents from six out of every 10 programs felt that students could achieve a rural orientation in their studies.
Faculty research
The orientation of students' research training is influenced by the research interests of the faculty with whom they work. In the programs that participated in the survey, approximately one-third had faculty members whose research incorporated aspects of rural health. While such individuals are most often to be found among nursing faculty, their number is also substantial in various social sciences (especially sociology, psychology and geography). At the time of the survey, students in 13.5% of the programs were working as research assistants for faculty conducting rural health research. As might be expected, given the relative level of activity, nursing accounts for the highest concentration of the research assistantships, followed by family medicine and, to a lesser extent, sociology and environmental studies.
Student research
Students are required to do some research on their own in order to graduate from the majority (61.9%) of the responding programs, and infrastructure supports are available for this purpose at an even larger number of institutions (71.4%). Of the programs with students currently doing independent research (ie for dissertations, theses or major projects), 13.8% report that students have chosen a topic pertaining to the health of rural Canadians.
While the level of activity is modest, the extent to which it is distributed among disciplines is encouraging, and appears to reflect an on-going commitment. Faculty in 12 distinct fields report they are currently, or have previously, supervised students performing research on pertinent issues. In fact, when previous students' work is taken into account, the cumulative level rises to an encouraging point (21.2% of programs) - and reinforces the message that students will find support in pursuing a rural health focus in their research education.
Financial assistance
Of course, those doing rural-relevant research are eligible for the usual array of bursaries, grants, assistantships, and other forms of financial supports available to students in a given subject area or institution, regardless of their study interests. In addition, there is some form of rural topic-linked funding available in a surprising number of the responding programs: 16 programs representing eleven discipline areas indicated that such resources were available.
Methodological approaches
Most of the responding programs offer research methodology courses and these cover a cross-section of approaches, both quantitative (98.7%) and qualitative (91.8%). As well as providing a set of research tools, the courses deal with the fundamental principles of ethics and confidentiality. They also generally address a cluster of concerns that are especially relevant for undertaking rural-based research. Insider/outsider issues, for example, are discussed in 70.0% of the research courses reported. The role that community members can and should play in the conduct of research that potentially affects them is even more widely covered (73.4%). However, specific means to achieve community participation, such as hiring local staff, are discussed in a comparatively small number (29.3%) of the research courses being discussed.
Projected development
Respondents were asked about their program's concrete plans and anticipated developments with respect to rural health research training. In reply, they provided a wide-ranging list of initiatives and ideas. Some of these refer to specific programs coming on-stream, expansion of clinical placements and recent hiring of faculty with relevant expertise. Others identify areas where change is expected, although still at the discussion stage. Of note were the number of rural-specific topics cited that are being explored as possible new research directions by faculty, especially those in nursing and, to an extent, medicine.
Discussion
The survey results indicate the scope and nature of the educational platform on which a sustainable, national rural health research agenda for the future must be built. Current capacity is small, with significant gaps, especially in the social sciences. In light of this, the emergence of the new research society, CRHRS, is timely. Its five-year goals include: increasing the number of scientists active in rural and remote health research; enhancing strategic funding for, and the number of, nationally funded research projects in rural and remote health; increasing the number of awards for students and post doctoral fellows with a focus on relevant topics; and the involvement of rural and remote communities in conducting health research. Based on the findings of the present study, it is apparent that CRHRS needs to lobby for a pan-Canadian rural health education strategy that would develop curricula and new programs.
To date, the society has held four multidisciplinary conferences which have attracted approximately 150 researchers and practitioners from across Canada. At each one, the number of students attending has increased. The annual conference provides opportunities for individuals to meet and discuss their research while making important connections that will foster more of the same. The meetings have also provided a forum in which to lobby the national research foundations, encouraging them to target funding for rural health research and education.
There have been other positive developments. The Canadian Institutes of Health Research (CIHR) undertook a multi-year strategic initiative to ensure an integrated and focused research approach for Canada's rural and remote areas6. The Design Phase of this plan included consultations with Canadian and relevant international rural health researchers, preparation of literature reviews and discussion papers and establishment of a National Steering Committee to draft the strategy. The first funding supported six projects in 2001. The Foundation Phase, now underway, includes activities to build a solid base of knowledge and recommendations for action. As part of this, there was a second round of funding for six additional projects. The final phase of the plan, the Strategic Action Phase, will use the emerging capacity in rural research to implement a Canada-wide rural study, a rural health post-doctoral competition, a knowledge translation program and a competition to establish centres of excellence in rural health. To ensure implementation of the Strategic Plan, a comprehensive group of partners has been enlisted: all 13 institutes within the CIHR, the Rural Secretariat, CHSRF, Health Canada, Statistics Canada, the Natural Sciences and Engineering Council (NSERC) and the Social Sciences and Humanities Research Council (SSHRC).
Conclusions
Although almost a third of Canadians live in rural, remote and northern parts of the country, the conditions that affect their health in unique ways have not received a level of research attention commensurate with their numbers2. Whether as antecedence or consequence of this fact, rural health is also under-represented as a topic of research education in the country's universities. Nonetheless, the survey showed that the option to pursue rural-focussed work exists for students in many programs and, at the program level, a widespread willingness to explore increased offerings in response to student interest. The contradictory situation - where only a little is being done, but there are many opportunities - becomes evident when the subject is considered on an issue-by-issue basis. From a broader perspective, initiatives such as the founding of the CRHRS and the Strategic Plan within the CIHR to address rural health research issues suggest that Canada is well on its way to building the research capacity necessary to answer questions about the health of our rural residents.
Acknowledgements
The authors express their thanks to: Gary Mack, Project Research Assistant at the Centre for Rural and Northern Health Research (Lakehead Site), who helped design, distribute and analyze the survey; as well as to Nadine Nowatzki, Academic Assistant, School of Health Sciences, University of Lethbridge, who assisted in the preparation of this manuscript. They also acknowledge the funding from the Medical Research Council of Canada (now part of the Canadian Institutes of Health Research), which enabled them to conduct the study, and the support of the Canadian Rural Health Research Society. Interpretation of the results and conclusions are those of the authors alone, however; no official endorsement by the institutes or society is intended or should be inferred.
References
1. Romanow R. Building on values: the future of health care in Canada. Final report of the Commission on the Future of Health Care in Canada. Ottawa: Health Canada, 2002.
2. Pong RW. Rural health research in Canada: at the crossroads. Australian Journal of Rural Health 2000; 8: 261-265.
3. Minore JB, Kulig J, Stewart N, Mack G. Rural health research training in Canada: where do we stand? Report prepared for The Consortium for Rural Health Research and Canadian Institutes of Health Research, 2001, pp. 47.
4. Dillman D. Mail and internet surveys: the tailored design, 2nd edn. Toronto: Wiley, 2000.
5. Association of Universities and Colleges in Canada (AUCC). AUCC 2000 Directory. Ottawa: Association of Universities and Colleges of Canada, 2000.
6. Canadian Institutes of Health Research. Building healthy communities through rural and northern health research (Online) 2003. Available: http://www.cihr-irsc.gc.ca/e/services/4627.shtml# (Accessed 15 January 2004).
Abstract
Introduction: The need to build capacity in rural health research is recognized in Canada. During its formative stage, the Canadian Rural Health Research Society (established in 2002), performed a nation-wide survey of the research teaching and training opportunities available to students interested in rural and remote health issues. Intended as a cross-sectional 'snapshot,' and to provide base-line data, the survey involved a comprehensive list of educational programs in health and science disciplines at all Canadian Universities offering graduate-level programs. The present project report gives an overview of the results, documenting the current strengths, but also the noticeable gaps that exist.
Methods: Data were collected via an Internet survey, developed according to Dillman's email survey design principles. Although multiple contacts are recommended, due to time constraints only two were made. The instrument included both open- and closed-ended questions designed to determine institutional commitments to rural health research training generally, as well as specific information about course offerings, infrastructure supports for students, financial assistance for studying specific topics, and future plans. Health was defined broadly and included a number of disciplines beyond those usually considered under the health rubric. Individuals in administrative positions for 462 programs in 24 distinct disciplines at 56 institutions were sent the survey. Responses were received from 120 programs at 40 universities. Due to budget constraints the instrument was not translated into French. Descriptive statistics were used to analyse the data, combined with a thematic analysis of written comments. Ethical approval was obtained from the Lakehead University before the study was conducted.
Results: Despite the fact that one-third of Canadians live in rural, remote and northern areas, there is a paucity of research that addresses rural health issues. Moreover, Canadian universities have very limited rural health offerings in their curricula. There are few formal courses available on rural health topics generally or rural health research specifically. Although students can take rural-related independent studies or reading courses, very few actually take advantage of the option. Of all disciplines, nursing faculty are most likely to pursue rural health research and to offer rural health courses. Moreover, nursing faculty most often indicate an intention to expand their rural health offerings. In the social sciences, geography and environmental science programs, relatively few students choose to study rural health. Similarly, in medicine, the number of students exploring rural health issues is small. There is some specific financial assistance available to students who are interested in rural health research and, as well, they have access to general pools of funding.
Conclusion: The survey results demonstrate the limitations of current educational programs. However, they also indicate areas of potential growth and show widespread interest in increasing the offerings available at universities across Canada. The article concludes by giving an overview of the mandate and initiatives being taken by the new research society to augment training, and to enhance student participation. In addition, it notes the positive developments linked to a new Strategic Plan by the Canadian Institutes of Health Research (CIHR) to enhance rural health research in Canada.
Keywords: Canada, capacity building, research training, rural curricula.
You might also be interested in:
2013 - A national study into the rural and remote pharmacist workforce
2008 - Labouring to nurse: the work of rural nurses who provide maternity care


