Introduction
Historically, inpatient medical care in most small island communities around the United Kingdom has been delivered by internal medicine specialists (consultants), who often work single-handed with prolonged on-call commitments. This pattern of working is becoming unsustainable due to recruitment and retention difficulties, statutory restrictions to hours worked by health professionals, and the expectation that each clinician must manage an externally defined volume of cases to maintain clinical standards1. Health services in small island communities tend to focus on primary care delivery, because population numbers may be insufficient for high order services to be provided2. However, there is a need to provide an acute care service against a background of remoteness and inaccessibility3, which has been discussed in more detail by Puni4. Scotland has many large and small islands, some grouped in archipeligos. Historically these have been relatively closed communities, although significant numbers of in-comers have arrived in recent years, and the islands contain proportionately more elderly people than the national average. Seasonal tourism influxes also result in large fluctuations in population. This article describes an evaluation of a novel method of providing consultant support for acute internal medicine to one of these island groupings off the Scottish coast.
This archipeligo sustains a population of 19 245, of whom 49% are male and 17% are aged 65 years or older. The majority of the population (85%) lives on the largest island. In addition, there are approximately 70 smaller islands, 17 populated, and some with resident primary care services provided by a GP or nurse. Unlike other island communities, this one has never had a resident medical consultant. Until 2001, acute inpatient medicine was provided from a medical unit of 20 beds, located in the main town, with cover provided by 14 GPs, each of whom had both hospital and general practice commitments. They were responsible on a rotating basis for the inpatient medical care of patients, including admission, assessment, management and discharge. There were no junior hospital doctors. Patients requiring more specialised medical care were transferred by air ambulance, or by road and sea to a teaching hospital on the mainland.
In 2000, options were considered to enhance medical consultant provision to the island hospital. One option was to appoint a resident consultant in the islands. However it was recognised that it would be difficult to recruit to an island-based consultant post, and that to provide for reasonable working hours and on-call commitments, more than one specialist would be required.
An alternative scheme was therefore proposed, in which a consultant would be appointed, based in a district general hospital on the mainland, approximately 100 miles from the island group. The consultant would provide a lead clinician role for inpatient services at the island hospital, and would visit on a twice-monthly basis, undertaking educational sessions and developing local guidelines and care pathways for the management of individual medical conditions. Consultants from other medical sub-specialities would also make intermittent educational visits (six per year). Inpatient care would continue to be provided in the islands by a lesser number of GPs, re-organised into teams. In addition, new junior medical posts (senior house officer grade) would be created to jointly support the care of medical patients.
The new system was implemented in late 2001. It was anticipated that it might provide a model applicable to other remote communities. It was expected that it would influence case mix and clinical outcomes, clinical skills and the confidence of existing medical staff, and would have economic implications. For example, patients previously transferred off the island could potentially be managed locally. Alternatively, an increased awareness of therapeutic options available in a large district general or teaching hospital setting might encourage more frequent transfer of patients. The confidence of existing staff might be enhanced by additional educational input. It was thought that the cost implications could be significant, particularly with the use of different treatment regimens and alteration of criteria for transfer. This article reports the clinical and economic impact of the new arrangements - with specific reference to patients presenting with suspected cardiac chest pain - and discusses issues involved in implementing the system.
Methods
A retrospective analysis of case mix during the previous 3 years (1998-2000) was undertaken. Data on primary diagnosis were collected manually from the medical admissions book and supplemented by data extraction from nursing administration software. A strategy was developed for examining and enhancing management of indicator conditions, chosen based on their frequency and clinical importance. A prospective recording system for case mix was established with agreed integrated care pathways (ICP) for indicator conditions, based on evidence-based protocols. Performance against the first of these ICP, for management of suspected cardiac chest pain, was evaluated in detail, examining both the process of management and clinical outcome. Clinical outcomes, including transfer to the mainland teaching hospital for further management, were determined by the review of case notes. Admission electrocardiograms (ECG) were retrospectively examined by two independent physicians to determine potential eligibility for administration of thrombolysis on the basis of the ECG features. In cases of discordance between the assessments of the two physicians, a consultant cardiologist mediated. The economic consequences of the ICP were explored. In addition, the general case mix of the medical unit was determined from hospital-coded returns during the periods June-November 2001 and June-November 2002, that is before and after implementation of the new arrangements.
Health providers' costs were calculated, including: the additional resource input into the medical service; costs associated with length of stay in hospital; drugs administered and tests; and transfers to, and treatment in, the mainland teaching hospital. Costs of drugs were provided by the hospital pharmacy department and supplemented from the British National Formulary. The examinations and tests considered were: chest X-rays, liver function tests, lipids (cholesterol, and HDL), troponin, creatinine, glucose, full blood count and urea and electrolytes.
Data from the clinical literature were used to estimate the potential health gains from changing clinical practice5-10, based on key process indicators recorded before and after implementation of the new arrangements.
Anonymised data were entered into Microsoft Excel for analysis and reporting. Formal management approval was given for data collection, which followed procedures recommended by the Confidentiality and Security Advisory Group for Scotland.
Results
Medical admissions 1998-2000
Between 1998 and 2000, the annual number of admissions ranged from 514 to 576, bed days from 4920 to 5642, and the median length of hospital stay was between 3 and 4 days. Common documented reasons for admission included cardiovascular disease, including unspecified chest pain, respiratory disease, stroke, alcohol intoxication and self-poisoning. However, there were considerable year-on-year fluctuations in case mix, and individual high demand patients led to marked skewing of length of stay data. From this information, suspected acute cardiac chest pain was selected as the subject of the first ICP, as the condition was common, consistent between years and clinically important.
General Case Mix - 2001-2002
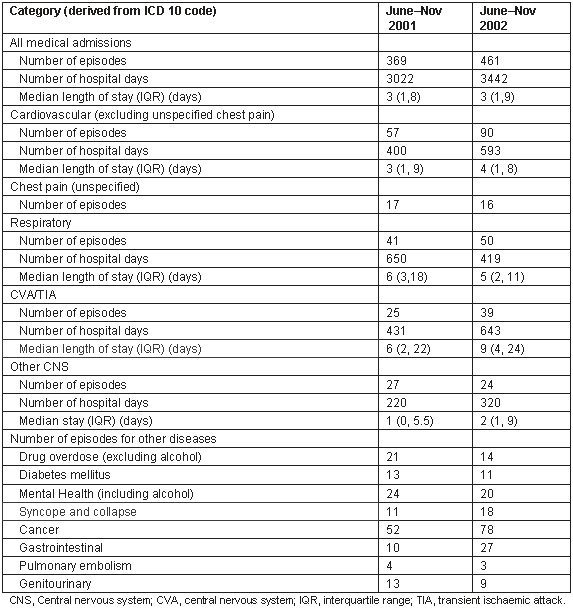
Episodes of care and length of stay for all admissions and a selection of the common diagnostic categories for the periods June-November 2001 and 2002 are shown (Table 1). There was a 25% rise in total admissions between the time periods, with particular increases in cardiovascular and cerebrovascular disease, and cancer. Air ambulance transfers between the islands and the mainland within these time periods also increased by 31%, from 88 to 115 transfers.
Table 1: Adult hospital medical admissions: 2001 and 2002
Implementation of the ICP
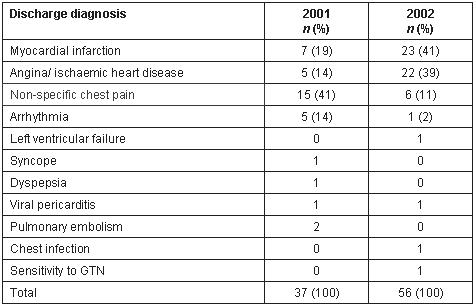
The discharge diagnosis is shown for those patients considered eligible for the ICP on the basis of the presenting complaint, as recorded in the medical notes (Table 2). A considerably greater proportion of patients in 2002 had myocardial infarction or angina as the recorded discharge diagnosis, compared with 2001, where a greater proportion were classified as non-specific chest pain. The reasons for this are uncertain, but the most likely explanation is diagnostic transfer, that is the use of different terminology as the practitioners became more confident of making a diagnosis of cardiac chest pain.
Table 2: Discharge diagnosis for patients considered eligible for management according to the ICP
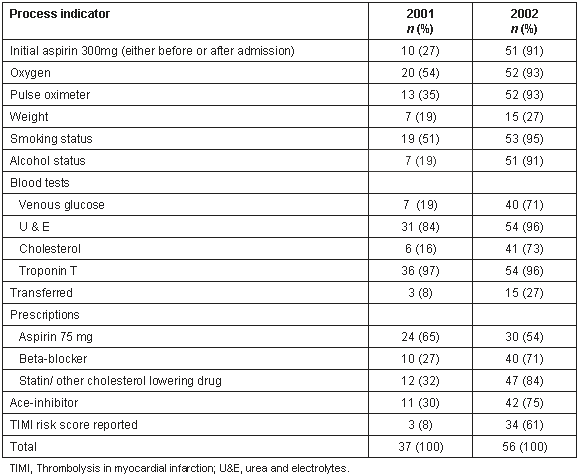
The recording of key process indicators for patients considered eligible for the ICP in 2001 and 2002 is shown (Table 3). The recording of specific details from the history and frequency of appropriate blood investigations increased, and initial steps in management changed considerably after introduction of the ICP.
In 2001, one patient was considered eligible according to the later expert analysis of the ECG and that patient was given thrombolysis. A second patient received thrombolysis, although expert analysis of the ECG considered that patient ineligible. In 2002, six patients were considered eligible according to the expert ECG analysis. Of these, three were given thrombolysis, two were considered but had specific contraindications, while the sixth had no apparent contraindications and was discharged with a diagnosis of left ventricular failure and angina, but not myocardial infarction. A further three patients were given thrombolysis, although later expert analysis of the ECG considered these patients ineligible.
Table 3: Recording of key process indicators for patients eligible for management according to the ICP
The number of transfers to the mainland teaching hospital increased from 3/37 (8%) in 2001 to 15/56 (27%) in 2002. In 2001, seven patients fulfilled criteria for possible transfer with a view to coronary angiography and percutaneous coronary intervention (PCI). Of these, two (29%) were transferred. All those transferred in 2001 underwent coronary angiography. In 2002, 19 patients fulfilled criteria for possible transfer, based on Troponin results and thrombolysis in myocardial infarction (TIMI) risk scores11. Of these, 7 (37%) were transferred. A further 8 were transferred for reasons other than those dictated by the ICP. Of 15 patients transferred in 2002, one was transferred for cardiac pacing and nine for coronary angiography, while for the remainder the specific reason for transfer was not clear from the island hospital records. While application of the ICP accounts for some of the additional transfers, other transfers may reflect a difference in case mix, or a generally lowered threshold for transfer.
Economics
The additional resource input consisted of a 0.5 whole time equivalent consultant physician and 2.0 whole time equivalent senior house officers at a total annual cost of £137 000. An additional annual £11 315 was incurred for travel and accommodation for consultant visits.
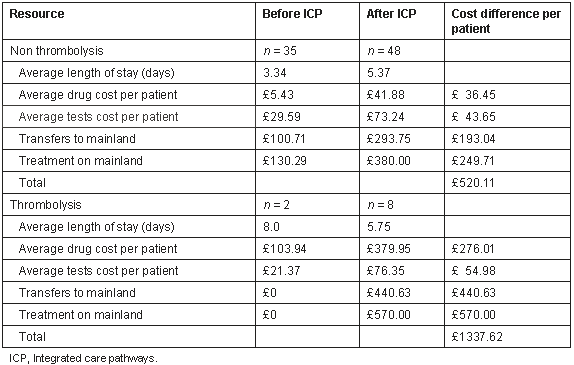
Costs associated with resource use are summarised (Table 4). In the non-thrombolysis arm of the pathway, there was a significant increase in average length of stay but no cost was attributed to this because the hospital occupancy (69%) allowed the increased bed days to be accommodated without additional resources. The increase in drug cost was largely attributable to a greater use of pathway-recommended treatments; heparin accounted for 62%, statins for 9%, and clopidogrel for 20% of the increase. Use of ACE inhibitors and β-blockers also increased but the cost implications were much smaller. Increased use of chest X-rays accounted for approximately 75% of the cost difference for tests. The largest differences in cost arose from increased transfers to the mainland teaching hospital. Although absolute numbers were small, the unit costs for air ambulance transfers and for treatment in the teaching hospital were high. In the thrombolysis group, differences in resource use were mostly non-significant because of the very small sample size. The exception was the cost of tests. The same pattern of increased resource use was observed, except for a (non-significant) reduction in average length of stay. The large increase in drug costs was mainly due to the substitution of a more expensive thrombolytic agent.
Table 4: Resource use and associated costs for patients presenting with chest pain before and after implementation of the integrated care pathways
Costs per patient treated were used to estimate the annual impact of the pathway. For an estimated 100 patients per year (85 non-thrombolysis; 15 thrombolysis), the additional cost would be £64 000, of which over 80% is accounted for by air ambulance transfers and treatment in the mainland teaching hospital. Tables 5 and 6 summarise evidence from the literature presented as the number of patients that need to be treated (NNT) with each intervention to achieve the health outcome indicated. Note that no figure is shown for β-blockers. Although this intervention benefits patients, no suitable data could be found for NNT that related to these specific patient groups. As a result, no benefit was included. A consistent approach was adopted to apply assumptions that will produce conservative estimates of benefit. From the increase in intervention rates shown in Table 3, estimates were made of the number of adverse events avoided on an annual basis, based on 100 patients per year (85 non-thrombolysis; 15 thrombolysis). Approximately 16 adverse events would be avoided at a combined cost of £212 000 (£148 000 direct costs of intervention plus £64 000 additional treatment costs) or £13 250 per event avoided. This is a conservative estimate of benefit because all the direct costs of the intervention have been included, even though the investment in medical services would benefit other groups of patients as well.
Table 5: Key indicators of benefit: numbers needed to treat to avoid adverse events - non-thrombolysis

Table 6: Key indicators of benefit: numbers needed to treat to avoid adverse events - thrombolysis

Discussion
This study has shown that appointing a mainland-based consultant physician to support general practitioners delivering inpatient hospital services on an island can positively influence standards of patient care at reasonable cost.
Among the pressures on health-care providers on islands are: the relative merits of local versus distant care; diseconomies of scale, both capital and revenue12, clinical governance issues where volume/quality relationships are believed to be important and case loads are low1, access considerations associated with weather conditions2 and the concept of a critical mass to sustain an acceptable working environment for health care professionals. Another important factor is fluctuation in demand, which, on a background of small patient numbers, means that specific 'high demand' cases (eg renal failure), may significantly affect the configuration and economics of healthcare delivery.
Possible models for delivery of inpatient medical care, which may not be mutually exclusive, include: consultant-delivered; consultant-led; visiting consultants; managed clinical networks; primary care delivered with external consultant support; and the development of specialised rural practitioners who rotate through larger centres for skills maintenance. Telemedicine may provide a support mechanism, but whatever service configuration is used, patient transfer issues will always be an important and expensive element of island health services. For professionals working on islands, training and re-accreditation issues may be problematic and where caseload is low, 'clinical fire drills'13 are important to maintain competence and confidence.
An Acute Services Review, carried out in 1997 by Scotland's Chief Medical Officer, observed that 'the status quo in rural hospitals is often not sustainable', and recommended that 'clinicians providing local care in remote areas must see themselves as part of a wider emergency care network underpinned by agreed protocols and clinical guidelines'1. The new arrangements for hospital medical care in this island group must be judged against that policy background.
A number of important lessons from this project could be applied to intermediate or secondary care in other remote and rural settings in Scotland and elsewhere. There were positive impacts on recruitment and on clinical care. It was possible to recruit a high calibre consultant, and to retain a group of competent general practitioners to operate the new arrangements. The findings on general case mix must be interpreted with caution, because considerable year-on-year fluctuation occurs, and within individual diagnostic categories, small numbers may be subject to significant skewing. However, the level of care delivered to patients with suspected cardiac pain has become more appropriate and this should be associated with improved prognosis. These data are based on recorded resource use as per patient notes. It is possible, therefore, that some of the changes identified could reflect changes in recording practice, but this cannot be verified. Interestingly, the total number of admissions to the hospital, and in particular the number of cardiac cases, increased after implementation of the new arrangements. This may reflect random fluctuation, it is speculated that referral patterns may have changed among the general practitioners themselves, recognising the enhanced level of care now offered in the hospital.
Costs of care rose, but the level of service provided rose concomitantly, and the health benefits were achieved at reasonable cost. Within the time frame of the study, long-term outcomes for these patients were not available and we therefore estimated benefit according to likely adverse events avoided. The adverse events reported in the literature form a combined indicator including coronary events, strokes and mortality and it is not possible, therefore, to report the results in terms of quality adjusted life years (QALYs) directly. However, the cost per avoided adverse event compares favourably with other interventions recommended by health technology assessment groups. For example, for a new technology or treatment it has been estimated that the National Institute for Clinical Excellence (NICE) applies a threshold value in the region of £30 000 -£40 000 per QALY14. Placing the investment in medical services in this island group at the threshold would imply a QALY value of less than 0.5 per adverse event avoided. In other words, if it is assumed that the 16 adverse events avoided will provide at least 8 QALYs, then the investment would pass the NICE cost-effectiveness threshold. Furthermore, the impact of the fixed costs will reduce as enhanced care is offered for a wider range of conditions.
An estimate of notional costs involved in alternative models suggests that costs would be similar for a three consultant service, the present model, and a triage and transfer system without consultant input, in which many more patients would be transferred to the mainland teaching hospital. In the future, the models chosen by island communities and health care providers are therefore likely to be determined by viability, sustainability and public acceptability rather than cost, and our study suggests that the model reported is viable.
However, explicit agreement on the level of service provided is a central issue. In the island setting, acute management of medical emergencies may be required at times when transfer off the island is impossible, although the human and technical resources to deliver this is less than in a larger hospital. It is therefore essential that all involved in the provision of remote hospital care work to a common set of goals and standards. This requires appropriate training and support, together with suitable recognition and remuneration. The consultant(s) providing input to the service require appropriate recognition for their role in a service that will be regarded as unconventional by many colleagues in larger hospitals. Care must also be taken that the consultant's commitments and role in the 'parent' district general hospital (DGH) or teaching hospital are appropriate and recognised as equivalent to other consultant colleagues.
In the current model, the level of service offered is superior to that of a community hospital, as defined in the Draft Clinical Standards for Community Hospitals produced by the Clinical Standards Board for Scotland (2002)15. However, the depth and range of support services is obviously less than a DGH. A key function for the consultant is to develop care pathways and protocols, derived from evidence-based practice, that are deliverable in the remote hospital setting. The critical role of the nursing and allied health professional staff must be recognised, particularly as they are often the main source of continuity for patient management. National and local management must recognise the changing roles of those involved. During the implementation of a service such as that provided in these islands, a forum must be provided for experiences and concerns to be shared. Some of the management issues would differ in a setting where a previously consultant-delivered service may be converted to this model. However, the findings of this evaluation suggest that this is a viable model for remote hospital intermediate care.
Acknowledgements
The study was funded by the Scottish Executive Remote and Rural Areas Resource Initiative. The Health Economics Research Unit is funded by the Chief Scientist Office of the Scottish Executive Health Department. However the views expressed are not necessarily those of the funders.
References
1. Scottish Office Department of Health. Acute Services Review Report. Edinburgh: The Stationery Office, 1998.
2. Royle SA. Health in small island communities: the UK's South Atlantic Colonies. Health & Place 1995; 1: 257-264.
3. Scottish Health Service Advisory Council. Health Services in Remote and Rural Scotland. (The Thomson Report). Edinburgh: HMSO, 1995.
4. Puni R. Hospital care on Islands: a critical literature review and routine data analysis. M. Sc Thesis. Department of Public Health, University of Aberdeen, 2002.
5. Cannon CP, Weintraub WS, Demopoulos LA et al. TACTICS (Treat Angina with Aggrastat and Determine Cost of Therapy with an Invasive or Conservative Strategy) --Thrombolysis in Myocardial Infarction 18 Investigators. Comparison of early invasive and conservative strategies in patients with unstable coronary syndromes treated with the glycoprotein IIb/IIIa inhibitor tirofiban. New England Journal of Medicine 2001; 344: 1879-1888.
6. Cohen M, Demers C, Gurfinkel EP et al. A comparison of low-molecular-weight heparin with unfractionated heparin for unstable coronary artery disease. New England Journal of Medicine 1997; 337: 447-452.
7. Scandinavian Simvastatin Survival Study Group. Randomised trial of cholesterol lowering in 4444 patients with coronary heart disease: the Scandinavian Simvastatin Survival Study (4S). Lancet 1994; 344: 1383-1389.
8. Scottish Intercollegiate Guidelines Network. Antithrombotic Therapy SIGN Guideline 36. (Online) 1999. Available: http://www.sign.ac.uk/pdf/sign36.pdf (accessed 4 June 2004).
9. Scottish Intercollegiate Guidelines Network. Secondary Prevention of Coronary Heart Disease following Myocardial Infarction SIGN Guideline 41 (Online) 2000. Available: http://www.sign.ac.uk/pdf/sign41.pdf (accessed 4 June 2004).
10. The Heart Outcomes Prevention Evaluation Study Investigators. Effects of an angiotensin-converting-enzyme inhibitor, ramipril, on cardiovascular events in high-risk patients. New England Journal of Medicine 2000; 342: 145-153.
11. Antman EM, Cohen M, Bernink PJ et al. The TIMI risk score for unstable angina/non-ST elevation MI: a method for prognostication and therapeutic decision making. JAMA 2000; 284: 835-842.
12. Gould MI, Moon G. Problems of providing health care in British island communities. Social Science Medicine 2000; 50: 1081-1090.
13. Douglas JDM, Laird C. Clinical fire drills and skill decay: can we develop an evidence base for a policy and a language for training. Medical Education 2004; 38: 14-16.
14. NICE. Completed technology appraisals 2000/2001. Report presented to Annual Public Meeting 18th July 2001. (Online) 2001. Available: http://www.nice.org.uk/pdf/brdjul01item3.pdf (accessed 4 June 2004).
15. Clinical Standards Board for Scotland. Draft Clinical Standards for Community Hospitals. Edinburgh: Clinical Standards Board for Scotland, 2002.
Abstract
Introduction:
Providing local consultant-delivered hospital services in remote and island communities in the United Kingdom is increasingly problematic due to difficulties with recruitment and retention of staff, statutory restrictions to hours worked by health professionals and the expectation each clinician must manage an externally defined volume of cases to maintain clinical standards. This article describes a before-and-after evaluation of a novel method of providing consultant support for acute internal medicine to an island grouping off the Scottish coast. Under the scheme, local GPs provided acute medical care of inpatients. A consultant general physician was appointed in a district general hospital on the mainland, approximately 100 miles from the island group, to provide a lead clinician role for inpatient services at the island hospital, visiting the island on a twice-monthly basis, undertaking educational sessions and developing local guidelines and care pathways for the management of individual medical conditions. In addition, two junior doctors were appointed to the island hospital to support inpatient care.Methods: A prospective recording system for case mix was established with agreed evidence-based protocols, developed as integrated care pathways (ICP), for indicator conditions. General case mix was determined during two 6-month periods, June-November 2001 and June-November 2002, before and after implementation of the new arrangements. Performance against an ICP for management of suspected cardiac chest pain was evaluated in detail, examining the process of management, clinical outcome and economics. Data from the clinical literature were used to estimate the potential health gains from observed changes in clinical practice.
Results: Total admissions rose by 25% in the second time period, with particular increases noted for cardiovascular, cerebrovascular disease, and cancer. Total air ambulance transfers between the islands and the mainland within these time periods increased by 31%, from 88 to 115 transfers. Recording specific details from the history and frequency of appropriate blood investigations increased and initial steps in management changed considerably after introduction of the ICP. The number of transfers to the mainland teaching hospital increased from 3/37 (8%) in 2001 to 15/56 (27%) in 2002. Based on an estimated 100 patients per year, of whom 15 would receive thrombolysis, total additional patient costs would be £64 000. The annual cost of the additional resource input into the medical service was £148 000. Approximately 16 adverse events would be avoided at a combined cost of £212 000 (£148 000 direct costs of intervention + £64 000 additional treatment costs) or £13 250 per event avoided. This is a conservative estimate of benefit as all the direct costs of the intervention have been included.
Conclusions: This study shows that appropriate standards of care can be delivered in the setting described. Costs of care increased, but the level of service provided increased concomitantly, and the health benefits were achieved at costs that compare favourably with other interventions recommended by health technology assessment groups. An estimate of notional costs involved in alternative models for the delivery of hospital medical services in a remote area suggests that costs would be similar for a three-consultant service, the present model, and a triage and transfer system. In the future, the models chosen by remote and island communities and healthcare providers are therefore likely to be determined by viability, sustainability and public acceptability rather than cost. Our study indicates that consultant supported intermediate care is a viable model.
Key words: integrated care pathways, island hospital, rural hospital, Scotland, thrombolysis.
You might also be interested in:
2015 - Post-mortem as preventative medicine in Papua New Guinea: a case in point




