Individual and family food preferences are determinants in food purchases, but many other factors, including age, gender, educational level and household income, also influence grocery-buying habits1,2. Strategies that promote the purchase of foods associated with reduced cardiovascular disease (CVD) risk should be developed in the context of these factors. Grocery vouchers and educational strategies that specifically target foods associated with reduced CVD risk result in increased consumption of those foods3. However, there is little research concerning the impact of grocery vouchers on purchases of these foods when there are no restrictions placed on the types of food that can be purchased. Many food assistance programs place very few restrictions on the types of food that can be purchased. For this reason, identifying demographic factors associated with the types of food that individuals purchase is a prerequisite to developing successful interventions aimed at increasing consumption of healthy foods in regions with disproportionately high rates of CVD. The purpose of this cross-sectional, pilot study was to determine the associations of age, gender, education and income level with purchasing of foods associated with lower CVD risk through the use of a grocery voucher. This pilot study was conducted following a community-based intervention to promote healthy food purchases in a rural food desert with disproportionately high rates of poverty and CVD. A food desert is defined as a low-income census tract (having either a poverty rate of ≥20%, or a median family income ≥80% of the area's median family income) where ≥33% of the population resides >16 km from a supermarket or large grocery store4.
Background and significance
Grocery store marketing strategies influence food purchases5. Point-of-purchase marketing, degree of variety of fruits and vegetables, display stands in prominent locations and staff promotion of healthful foods are all successful strategies to increase purchasing of foods associated with decreased chronic disease risk6-9. Financial incentives (ie food vouchers) provided to low-income households that can only be used to purchase specific grocery items (eg fruits, vegetables, fruit juices) result in greater purchases of those items10-13. In contrast, financial incentives without concurrent promotion of healthful foods result in an overall rise in food expenditure but not an increase in purchases of specific food items known to decrease the risk of chronic disease14. Financial incentives were combined with a location-based marketing community intervention to promote the purchase of healthful foods but grocery voucher redemption was not restricted to certain food items.
The current US Department of Agriculture Dietary Guidelines include recommendations to make half of meals fruits and vegetables, choose whole grains for half of all consumed grains, and drink low-fat or skim milk14. Guideline-based interventions may be ineffective if socioeconomic factors and population characteristics that influence dietary habits are not accounted for during development of these interventions. Older adults and women are more likely to have higher quality diets than younger adults and men15. There is also evidence that men and women respond differently to marketing strategies aimed at increasing nutritional knowledge and purchases of foods associated with reduced CVD risk16. It is important to evaluate the participant characteristics associated with the effectiveness of marketing strategies because a healthy diet has a greater impact on decreasing mortality rates in men than in women17.
The ability to recognise the health-related impact of dietary choices, degree of motivation to improve diet and physiological changes in appetite all differ throughout the lifespan. Advancing age is associated with healthier dietary habits. Older adults are more likely to report healthy behaviors, including adherence to a diet of foods associated with lower CVD risk, than younger adults18-21. In spite of this, overweight and obesity in older adults is steadily rising22. Older adults who adhere to the Dietary Guidelines for Americans are also less likely to experience disabilities in activities of daily living (eg dressing oneself, getting in and out of bed), instrumental activities of daily living (eg doing household chores, preparing meals), leisure and social activities (ie attending social events and performing leisure activities), and physical activities (eg walking, kneeling, lifting) than older adults who do not adhere to the dietary guidelines23. Given this reality, age-appropriate interventions aimed at improving dietary behaviors are more likely to be successful than interventions that do not account for age-specific responses to lifestyle behavior modification strategies.
Interventions that aim to increase consumption of foods associated with reduced CVD risk should also include gender-specific strategies24. There are gender-related differences in body composition, appetite, satiety and diet quality throughout the lifespan25,26. Women tend to have better quality diets, experience lower hunger sensations and higher post-meal satiety than men15,18,26,27. There are also gender-specific differences in the brain's response to external stimuli (ie pictures of food) related to appetite and food28. Female gender is also associated with a greater likelihood of recognising food as a means to influence health outcomes29. College-educated individuals tend to eat healthier and low parental education levels are associated with poor-quality diet in children30,31. However, the relationship between educational level and diet quality is often mediated by income level and attitude towards healthy eating32. Measures of self-efficacy and healthy lifestyle planning to improve diet are similar across educational levels, suggesting these lifestyle behavioral goals are not limited to college-educated individuals33.
Food cost is a barrier to healthy eating, particularly for those living in lower income households. Poverty is generally associated with poor dietary habits and, consequently, increased obesity and chronic disease risk3-36. However, some contrasting studies have shown only marginal or no significant relationship between income level and consumption of foods associated with lower CVD risk18,37. Rising food cost can be an even greater barrier to healthy eating for individuals with low-incomes living in rural food deserts38. The increasing cost of feeding families is most concerning in areas where a significant percentage of people receive Supplemental Nutrition Assistance Program (SNAP) funds, a federally funded, state-administered nutrition support program. Nearly 47 million low-income Americans depend on SNAP funds to meet their nutritional needs. Barriers to healthy eating among low-income households include limited access to healthy foods, inadequate SNAP benefits, the cost of nutrient-rich foods and environmental factors such as rurality.
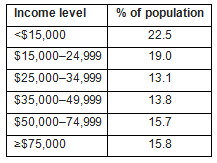
A Central Appalachian food desert, Breathitt County, Kentucky, which has disproportionately high rates of poverty and chronic disease, was chosen as the location to test this pilot community intervention. Breathitt is one of 50 Kentucky counties where many families consistently experience food insecurity (ie the state or risk of being unable to provide food for oneself or one's family). Food insecurity in Appalachia is associated with higher rates of chronic diseases, obesity, poor management of health conditions and depression39-41. The poverty rate in Breathitt County, which is one of the nation's top 25 poorest counties, is 33.8%, compared to 16.9% for the state of Kentucky and the national rate of 15.1%42. According to the 2010 census, 54.6% of Breathitt County households have less than $35,000 annual income (Table 1). The 2006-2010 average household income in Breathitt County was $19,906. In December 2011, more than 6000 of the county's 13 878 adult residents received Supplemental Nutritional Assistance Program or Kentucky Transitional Assistance Program funds43. While cost can be a barrier to healthy eating, 26% of individuals in Breathitt County with limited access to healthy foods have middle to high incomes, indicating that other factors beyond financial resources may inhibit health-promoting dietary habits44. Breathitt ranks as one of the least-healthy Kentucky counties, with a cardiovascular mortality rate of 540 per 100 000 population, compared to 409 for the entire state and a national rate of 32645.
Table 1: Breathitt County annual family
income levels (2010 US Census Bureau)
In rural Appalachia, the traditional diet consists of a high amount of calorie-dense meats and starches that are often fried or have added animal fats. A mixed methods convergent parallel design study was conducted prior to development of this community marketing event aimed at promoting purchases of CVD risk-reducing foods. During this earlier study, a nominal group process was used to determine factors that affected adherence to a risk-reducing diet in individuals living in this rural food desert. Food cost and limited access to healthy foods were factors affecting the potential to adhere to a CVD risk-reducing diet. Younger participants and those with lower incomes were more likely to identify food cost as a barrier to adherence than those who were older with higher incomes. Women were more likely than men to report an understanding of the health impact of certain foods as motivation to adopt and adhere to a risk-reducing diet46. Based on these findings, a media campaign/financial incentive was developed to promote the purchase of CVD risk-reducing foods.
This community-based pilot study tested the effectiveness of a culturally appropriate, community-based campaign aimed at promoting purchases of food items associated with reduced CVD risk. A partnership was established with local US Department of Agriculture Cooperative Extension Office Family and Consumer Science (FCS) specialists who delivered this intervention, which involved a print media campaign, a $5 grocery store voucher, local heart-healthy food branding and a community grocery store event. Brief nutrition articles were published in both local newspapers during four consecutive weeks in July 2012. The newspapers have a combined reach of 7000 readers. These articles, written at a literacy level appropriate for readership, explained the physiological actions of healthy foods and listed a health-promoting, minimal-ingredient recipe using foods readily available in local grocery stores. A 'Healthy Eating for Men' article that specifically described the impact of diet on men's health was written in each week's newspaper. During the fourth week of the media campaign, a voucher redeemable for a $5 grocery gift card was also printed in both local newspapers. Individuals were instructed to bring the grocery voucher to either of the county's two grocery stores on a single day in August 2012. One of the grocery stores is a national, full-service chain and the other is a national discount chain with their own exclusive and national brands.
In each store, foods that are known to be associated with a reduced risk of CVD were marked with a blue logo. These labelled items included whole grains; fresh and frozen fruits and vegetables; canned and dried legumes; skim dairy; omega-3 rich fresh, frozen and canned fish; unsalted almonds and walnuts and olive oils (not including oil blends). At both stores, brand name and generic options were available for all food product categories, with the exception of fresh produce. A table with a registered nurse and two other research personnel was set up near the entrance/exit of each of the two grocery stores, at locations that were also near the stores' produce sections. When individuals brought their grocery voucher to either store, they were asked to complete a brief questionnaire that assessed demographics and usual servings of fruits, vegetables and grains. After completing the questionnaire, participants received a $5 grocery card that could be used to purchase groceries only on the day of the study. Participants were also given a list of logo-labelled foods and a reusable grocery bag printed with the logo when they entered the store. The labels were affixed as permanent displays in the stores and the reusable bags served as prompts to purchase these foods during future visits to the grocery stores. Participants were instructed that if they returned their grocery receipts to the table after check-out, they would receive free 'healthy eating' items (ie two food preparation tools and a cutting mat). Returned grocery receipts were stapled to the questionnaires to analyse the relationship between demographics and food choices. A second table was staffed by a Family and Consumer Science specialist from the local Cooperative Extension Office, who provided prepared samples of some of the labelled CVD-risk reducing foods free to all customers. A well-known local community member was also available in each store to assist individuals in locating labelled food items and to ensure adequate stocking of these food items. All respondents (N=311) returned their grocery receipts following check-out.
Measures
Sociodemographic factors: These factors included age in years, gender, education and income. Education was assessed by participant response to the highest level of education completed with the possible response options of 'Grade school', 'High school', 'Some college', 'College degree' and 'Masters or doctoral degree'. Household income per year was assessed by asking participants to select one of these options: <$20,000, $20,000-30,000, $30,001-40,000, $40,001-50,000, $50,001-60,000, $60,001-70,000 and >$70,000.
Purchase of food items associated with CVD risk-reduction: Each labelled purchased item from any of the food categories (ie whole grains; fresh and frozen fruits and vegetables; canned and dried legumes; skim dairy; omega-3 rich fresh, frozen and canned fish; unsalted almonds and walnuts and olive oils) was recorded as a single purchase using the USDA grocery taxonomy. The number of labelled, CVD risk-reducing food items purchased ranged from 0 to 6. Due to almost half of the respondents purchasing zero designated food items (42%), the responses were dichotomised to: 'No purchase of the risk-reducing food items' and 'Purchase of at least one of the risk-reducing food items.'
Data analysis
Descriptive analysis, including means and standard deviations or frequency distributions, was used to summarise the study variables and check for missing or out-of-range values. Due to more than half of the participants completing either in 'Grade School' or 'High School' education (51.8%), responses were dichotomised to 'At most high school' and 'At least some post-secondary education'. Two-group comparisons of study variables by purchase of one or more designated food items were accomplished using χ2 tests of association, two-sample t-test or Mann-Whitney U-test, as appropriate. Multiple logistic regression was used to assess whether sociodemographic factors predicted the purchase of at least one of the designated food items. Variance inflation factors were used to assess whether multicollinearity was present in the model. Data analysis was conducted using Statistical Analysis Software v9.3 (SAS Institute, www.sas.com); an alpha level of 0.05 was used throughout.
Ethics approval
The study was approved by the University of Kentucky Medical Institutional Review Board Approval #12-0362-P2H.
The average age of the 311 participants was 45.8 (SD=15.7); the range of ages was 16-89 years. Thirty percent of the respondents were male and 52% had at most high school education. Forty-three percent had annual household income of <$20,000, which is similar to county demographics. One hundred and thirty-six (46.4%) respondents spent less than $10. Sociodemographic and total amount spent data are presented in Table 2.
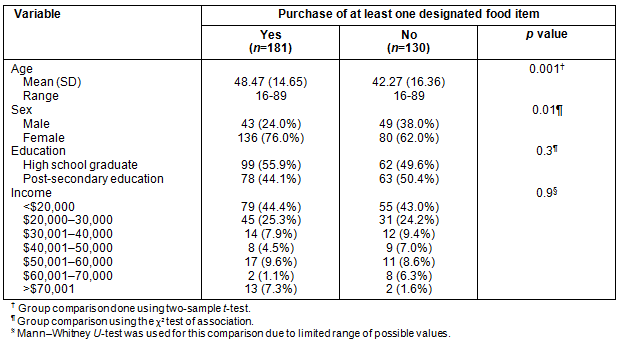
As shown in Table 3, there was a significant bivariate association between purchase of the labelled food items and age: participants who purchased at least one labelled food item were older (M=48.5, SD=14.7) than those who did not buy any of these items (M=42.3, SD=16.4; p=0.0008). Also there was a significant association between labelled food purchases and gender, with 47% of male participants purchasing at least one of labelled food items compared with 63% of females in the study (p=0.008). There were no significant associations between purchase of labelled food items with either education or income.
Table 2: Frequency distributions of demographic characteristics (N=311)
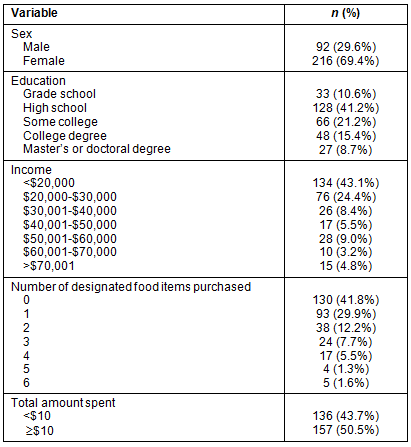
Table 3: Designated food items purchased comparisons of demographic and personal characteristics (N=311)
Sociodemographic factors were assessed as potential predictors on purchase of at least one of the labeled food items using multiple logistic regression (Table 4). Consistent with the bivariate analysis, the significant predictors in this model were age (p=0.003) and gender (p=0.01). The results of the model suggest that for every 10 year increase in age, there was a 29% increase in the likelihood that at least one designated food item would be purchased. Male participants were 48% less likely than female participants to purchase at least one designated food item. The variance inflation factors for this model were all less than 1.4, suggesting little evidence of multicollinearity due to correlations among the predictor variables.
Table 4: Multivariate logistic regression with purchase of at least one designated food items as the outcome (N=280)
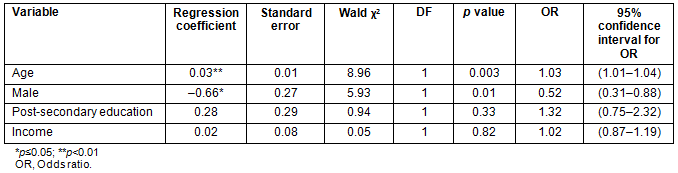
Table 5: Designated food items purchased comparison with total amount spent (N=311)
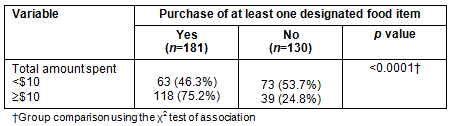
There was a significant relationship between spending less than $10 (yes or no) and purchasing at least one labelled item (p<0.0001). Of those respondents whose total amount spent was less than $10, 46% purchased at least one labelled food item and 54% didn't purchase any of the labelled food items. Of those respondents who spent $10 or more, 75% purchased at least one labelled food item and 25% didn't purchase any labelled food items.
Discussion
This study examined the associations of age, gender, education and income level with purchasing at least one healthy food item following an intervention that included a grocery voucher distributed via newspapers in a rural food desert with high rates of poverty and CVD. In this study, the majority of participants (58%) purchased at least one of the labelled foods associated with CVD risk reduction. Age and gender were associated with purchases of these food items, with older adults and women being more likely to purchase labelled food items with the grocery voucher than younger adults and men. Educational level and income were not associated with purchasing of labelled foods in this study. This lack of association may be due to a relatively homogenous sample from this county, one of the nation's poorest, with a lower percentage of high school graduates when compared to the overall population in Kentucky (65% vs 82%42).
Age and gender should be considered when developing strategies to improve dietary habits of individuals living in the Central Appalachian rural food deserts. Young adults tend to be more technologically proficient and are more likely to respond to healthy eating strategies that use social media (eg Twitter and Facebook) and electronic devices (eg PDAs, mobile phones and cameras) rather than print media47,48. Young adults are also more like to alter poor dietary habits after receiving education about the health effects of foods known to contribute to chronic disease and social normative messages about healthy eating49. The media campaign consisted of only print media, and future interventions should be broadened to include both social media and more technologically advanced modes of delivery. Information was also disseminated about the impact of foods associated with positive health outcomes but did not address the impact of those foods associated with negative health outcomes. This region has disproportionately high rates of CVD, type 2 diabetes mellitus and metabolic syndrome. The impact of foods that are traditional staples in the Appalachian diet (eg preserved or processed meats, refined carbohydrates and animals fats) should be included in future nutrition educational interventions.
These findings are also noteworthy because of the current national and state-level debate of whether restrictions should be placed on the types of foods that can be purchased with SNAP funds50. Individuals living in lower-income households may be more apt to shop at discount grocery stores but their attitudes towards healthy eating do not differ from those who shop at higher-cost supermarkets51. The intervention of a brief media campaign, grocery voucher and point-of-purchase information resulted in a majority of participants purchasing at least one healthy food item, irrespective of income or educational status.
The recent increase in food costs has resulted in the realisation that SNAP benefits may be inadequate to meet those needs and there is current discussion that these benefits should be increased52. However, concern about the negative impact of unhealthy food choices has raised the question as to whether SNAP-funded purchases of high-calorie, poor-nutrient foods and beverages should be restricted. While most agree that additional SNAP funding is necessary to meet the needs of low-income families, public support is mixed for policies that restrict the purchase of food products known to contribute to chronic illnesses53,54. The rationale for restricting SNAP purchases to only certain foods in the effort to decrease the risk of chronic disease is predicated upon two unfounded assumptions: (1) that SNAP participation is associated with risk of obesity; and (2) that SNAP participants will consume less of the foods low in nutritional quality if purchasing restrictions are in place55,56. Results of this study shows that income was not a factor in whether participants purchased healthy or unhealthy foods with a grocery voucher. Many of the counties located in rural Appalachia are among the poorest in the nation and consequently many rural Appalachians consume poor-quality diets57. Poverty-related food insecurity in low-income regions like Appalachia has also resulted in a tradition of food preservation by canning, drying, brining or sugar curing, techniques that increase the glycemic index of foods58,59. This predominant tradition influences dietary choice even in the current age of supermarkets and fast food.
A diet that consists of foods associated with reduced risk of CVD is important across the lifespan. Because age and gender were associated with purchasing of healthy foods items via a free grocery voucher, future programs in this impoverished region should be tailored to include gender- and age-related marketing strategies. Children who are taught to make healthy food choices are more likely to maintain those healthy eating habits into adulthood and, as they age, have better health outcomes than individuals who consume more foods associated with poor health outcomes60-63. Although changes in the diet can occur at any point in the lifespan, there is less readiness to change once eating patterns have been established for decades64. Parental modelling of lifestyle behaviors predicts healthy eating in children and adolescents65,66. Therefore, it is vital that young adults, particularly those with children, understand the health implications of diet and are empowered to make healthy food choices for themselves and their families. Trends over the past 30 years show that men are now spending more time grocery shopping but food preparation and consumption times have decreased for both men and women67. Grocery stores may be ideal locations for 'healthy eating' education and interventions. Marketing and financial strategies that specifically target men's nutrition-related behaviors should be developed and tested in vulnerable populations, particularly since diet affects the health of men more than women.
Limitations
Limitations to this study include required access to a copy of the local newspaper or shopper paper. Both grocery stores had newspapers available for sale at $0.50 and a small group of participants did purchase papers at the stores in order to access the grocery voucher questionnaire. Also, physical activity level was not assessed. However, in a cohort study of 1246 participants, physical activity, BMI and diet/weight concern was not associated with appetite16. Race/ethnicity was not assessed due to the county's demographics, with non-Hispanic whites comprising 97.5% of the population42. Also not assessed was whether participants intended to buy logo-labelled food items prior to receiving the grocery voucher. However, spending less than $10 was associated with purchasing at least one labelled item, indicating that grocery voucher redemption was likely the motivation to come into the store during the grocery event. Additional research using a control group is needed to determine whether financial incentives can prompt individuals to purchase health-promoting foods in addition to or instead of foods that contribute to chronic disease risk.
Younger adults and men may be less responsive than older adults and women to media-based educational strategies, heart-healthy food labelling and grocery vouchers to defray the cost of healthy eating. In this study, income was not associated with heart-healthy food purchases. Point-of-purchase strategies in community grocery stores may be effective in increasing consumption of foods associated with reduced risk of CVD. Previous studies show that concerns about cost and availability of foods associated with reduced CVD risk are greater factors in the decision to purchase and consume these foods than demographic characteristics68. However, age and gender are associated with the likelihood of using vouchers for the purchase of healthful foods. Younger adults may be more responsive to grocery vouchers and coupons via other types of media campaigns (eg text, email and social media). Additional research is needed to determine whether different educational strategies paired with food labelling and grocery vouchers may be successful strategies to promote purchase of heart-healthy foods, particularly for men and younger adults.
Acknowledgement
The authors express gratitude to Mary Kay Rayens, PhD, of the University of Kentucky College of Nursing for editing assistance.
References
1. Darko J, Eggett DL, Richards R. Shopping behaviors of low-income families during a 1-month period of time. Journal of Nutrition Education & Behavior 2013; 45(1): 20-26.
2. Wiig K, Smith C. The art of grocery shopping on a food stamp budget: factors influencing the food choices of low-income women as they try to make ends meet. Public Health Nutrition 2009; 12(10): 1726-1734.
3. Herman DR, Harrison GG, Afifi AA, Jenks E. Effect of a targeted subsidy on intake of fruits and vegetables among low-income women in the special supplemental nutrition program for women, infants and children. American Journal of Public Health 2008; 98(1): 98-105.
4. Ver Ploeg M, Breneman V, Farrigan T, Hamrick K, Hopkins D, Kaufman P, et al. Access to affordable and nutritious food-measuring and understanding food deserts and their consequences: report to Congress. United States Department of Agriculture Economic Research Service. Publication AP-306, 2009
5. Zachary DA, Palmer AM, Beckham SW, Surkan PJ. A framework for understanding grocery purchasing in a low-income urban environment. Qualitative Health Research 2013; 23(5): 665-678.
6. Ayala GX, Baquero B, Laraia BA, Ji M, Linnan L. Efficacy of a store-based environmental change intervention compared with a delayed treatment control condition on store customers' intake of fruits and vegetables. Public Health Nutrition 8 April: 1-8 (Online) 2013. Available: www.ncbi.nlm.nih.gov/pmc/articles/PMC3795910 (Accessed 3 January 2014).
7. Blitstein JL, Snider J, Evans WD. Perceptions of the food shopping environment are associated with greater consumption of fruits and vegetables. Public Health Nutrition 2012; 15(6): 1124-1129.
8. Holmes AS, Estabrooks PA, Davis GC, Serrano EL. Effect of a grocery store intervention on sales of nutritious foods to youth and their families. Journal of the Academy of Nutrition and Dietetics 2012; 112(6): 897-901.
9. Miller C, Bodor JN, Rose D. Measuring the food environment: a systematic technique for characterizing food stores using display counts. Journal of Environmental and Public Health. doi: 10.1155/2012/707860. (Online) 2012. Available: www.ncbi.nlm.nih.gov/pmc/articles/PMC3373162 (Accessed 3 January 2014).
10. Bihan H, Castetbon K, Mejean S, Peneau L, Pelabon L, Jellouli F, et al. Sociodemographic factors and attitudes toward food affordability and health are associated with fruit and vegetable consumption in a low-income French population. Journal of Nutrition 140(4): 823-830. (Online) 2010. Available: http://jn.nutrition.org/content/140/4/823.long (Accessed 3 January 2014).
11. Burr ML, Trembeth J, Jones KB, Geen J, Lynch LA, Roberts ZE. The effects of dietary advice and vouchers on the intake of fruit and fruit juice by pregnant women in a deprived area. Public Health Nutrition 2007; 10(6): 559-565.
12. Freedman DA, Bell BA, Collins LV. The Veggie Project: a case study of multi-component farmers' market intervention. The Journal of Primary Prevention 2011; 32(3-4); 213-224.
13. Herman DR, Harrison GG, Jenks E. Choices made by low-income women provided with an economic supplement for fresh fruit and vegetable purchase. Journal of the American Dietetic Association 2006; 106(5): 740-744.
14. United States Department of Agriculture. Dietary Guidelines for Americans 2010. Available: www.cnpp.usda.gov/DietaryGuidelines.htm (Accessed 26 June 2013).
15. Hiza HA, Casavale KO, Guenther PM, Davis CA. Diet quality of Americans differs by age, sex, race/ethnicity, income and education level. Journal of Academy of Nutrition & Diet 113(2): 297-306. (Online) 2013. Available: www.sciencedirect.com/science/article/pii/S2212267212014220 (Accessed 3 January 2014).
16. Meajean C, Macouillard P, Peneau S, Hercberg S, Castetbon K. Perception of front-of-pack labels according to social characteristics, nutritional knowledge and food purchasing habits. Public Health Nutrition 2012; 16(3): 392-402.
17. Kappeler R, Eichholzer M, Rohrmann S. Meat consumption and diet quality and mortality in NHANES III. European Journal of Clinical Nutrition, 2013; 67(6): 598-606.
18. Dehghan M, Akhtar-Danesh N, Merchant AT. Factors associated with fruit and vegetable consumption among adults. Journal of Human Nutrition & Dietetics 2011; 24(2): 128-134.
19. O'Neil CE, Nicklas TA, Zanovec M, Cho S. Whole-grain consumption is associated with diet quality and nutrient intake in adults: The National Health and Nutrition Examination Survey, 1999-2004. Journal of the American Dietetic Association 2010; 110(10): 1461-1468.
20. Thomson JL, Onufrak SJ, Connell CL, Zoellner JM, Tussing-Humphreys LM, Bogle ML, et al. Food and beverage choices contributing to dietary guidelines adherence in the Lower Mississippi Delta. Public Health Nutrition 2011; 14(12): 2099-2109.
21. Smith GW, Siddarth P, Ercoli LM, Chen ST, Merrill DA, Torres-Gil F. Healthy behavior and memory self-reports in young, middle-aged and older adults. International Psychogeriatrics 2013; 25(6): 981-989.
22. Flint KM, Van Walleghen EL, Kealey EH, VonKaenel S, Bessesen DH, Davy BM. Differences in eating behaviors between nonobese, weight stable young and older adults. Eating Behaviors 2008; 9(3): 370-375.
23. Xu B, Houston D, Locher JL, Zizza C. The association between Health Eating Index-2005 scores and disability among older Americans. Age & Ageing 2012; 41(3): 365-371.
24. Simen-Kapeu A, Veugelers PJ. Should public health interventions aimed at reducing childhood overweight and obesity be gender-focused? BMC Public Health 2010; 10: 340.
25. Govindan M, Gurm R, Mohan S, Kline-Rogers E, Corriveau N, Goldberg C, et al. Gender differences in physiologic markets and health behaviors associated with childhood obesity. Pediatrics 2013; 132: 468-474.
26. Gregersen NT, Moller BK, Raben A, Kristensen ST, Holm L, Flint, A, et al. Determinants of appetite ratings: the role of age, gender, BMI, physical activity, smoking habits and diet/weight concern. Food & Nutrition Research 55. doi: 10.3402/fnr.v55i0.7028. (Online) 2011. Available: www.foodandnutritionresearch.net/index.php/fnr/article/view/7028.
27. Hsiao PY, Mitchell DC, Coffman DL, Allman RM, Locher JL, Sawyer P, et al. Dietary patterns and diet quality among diverse older adults: the University of Alabama Birmingham Study of Aging. Journal of Nutrition, Health and Aging 2013; 17(1): 19-25.
28. Frank S, Laharnar N, Kullmann S, Veit R, Canova C, Hegner YL, et al. Processing of food pictures: influence of hunger, gender and calorie content. Brain Research 2010; 1350: 159-166.
29. Lorson BA, Melgar-Quinonez HR, Taylor CA. Correlates of fruit and vegetable intakes in US children. Journal of the American Dietetic Association2009; 109(3): 474-478.
30. Fernandez-Alvira JM, Mouratidou T, Bammann K, Hebestreit A, Barba G, Sieri S, et al. Parental education and frequency of food consumption in European children: the IDEFICS study. Public Health Nutrition 2013; 16(3): 487-498.
31. Wunderlich S, Brusca J, Johnson-Austin M, Bai Y, O'Malley M. Eating behaviors of older adults participating in government-sponsored programs with different demographic backgrounds. Global Journal of Health Science2012; 4(6): 204-215.
32. Le J, Dallongeville J, Wagner A, Arveiler D, Haas B, Cottel D, et al. Attitudes toward healthy eating: a mediator of the educational level-diet relationship. European Journal of Clinical Nutrition 2013; 67: 808-814.
33. Hankonen N, Absetz P, Haukkala A, Uutela A. Socioeconomic status and psychosocial mechanisms of lifestyle change in a type 2 diabetes prevention trial. Annals of Behavioral Medicine 2009; 38(2): 160-165.
34. Drewnowski A. The economics of food choice behavior: why poverty and obesity are linked. Nestle Nutrition Institute Workshop Series 2012; 73(95): 12.
35. Grimm KA, Foltz JL, Blanck HM, Scanlon KS. Household income disparities in fruit and vegetable consumption by state and territory: results of the 2009 Behavioral Risk Factor Surveillance System. Journal of the Academy of Nutrition & Dietetics 2012; 112(12): 2014-2021.
36. Inglis V, Ball K, Crawford D. Socioeconomic variations in women's diets. What is the role of perceptions of the local food environment? Journal of Epidemiology and Community Health 2008; 62(3): 191-197.
37. Haynes-Maslow L, Parsons SE, Wheeler SB, Leone LA. A qualitative study of perceived barriers to fruit and vegetable consumption among low-income populations, North Carolina, 2011. Preventing Chronic Disease 2013; 10: E34.
38. Smith C, Parnell WR, Brown RC, Gray AR. Providing additional money to food-insecure households and its effect on food expenditure: A randomized controlled trial. Public Health Nutrition 2012; 16(8): 1507-1515.
39. Porter KN, Johnson MA. Obesity is more strongly associated with inappropriate eating behaviors than with mental health in older adults receiving congregate meals. Journal of Nutrition in Gerontology and Geriatrics 2011; 30(4): 403-415.
40. Johnson CM, Sharley JR, Dean WR. Indicators of material hardship and depressive symptoms among homebound older adults living in North Carolina. Journal of Nutrition in Gerontology and Geriatrics 2011; 30(2): 154-168.
41. Bengle R, Sinnett S, Johnson T, Johnson MA, Brown A, Lee JS. Food insecurity is associated with cost-related medication non-adherence in community-dwelling, low-income older adults in Georgia. Journal of Nutrition for the Elderly 2011; 29(2): 170-191.
42. United States Census Bureau. State & County QuickFacts 2010. Available: http://quickfacts.census.gov/qfd/states/21000.html (Accessed 27 June 2013).
43. Kentucky Cabinet for Human Resources, SNAP participation (Online) 2012. Available: http://chfs.ky.gov/dcbs/Data_Book.htm (Accessed 1 September 2013).
44. United States Department of Agriculture. Food desert locator. Economic Research Service 2011. Available: www.ers.usda.gov/Data/FoodDesert/index.htm (Accessed 1 July 2013).
45. Kentucky Institute of Medicine. The Health of Kentucky 2007. Available: www.healthy-ky.org/sites/default/files/The%20Health%20of%20Ky.pdf (Accessed 2 September 2013).
46. Hardin-Fanning F. Adherence to a Mediterranean diet in a rural Appalachian food desert. Rural & Remote Health 2013; 13: 2293.
47. Daugherty BL, Schap TE, Ettienne-Gittens R, Zhu FM, Bosch M, Delp E J, et al. Novel technologies for assessing dietary intake: evaluating the usability of a mobile telephone phone record among adults and adolescents. Journal of Medical Internet Research 2012; 14(2): e58, doi: 10.2196/jmir.1967.
48. Bouschey CJ, Kerr DA, Wright J, Lutes KD, Ebert DS, Delp EJ. Use of technology in children's dietary assessment. European Journal of Clinical Nutrition 2009; 63(S1): 50-57.
49. Robinson E, Harris E, Thomas J, Aveyard P, Higgs S. Reducing high calorie snack food in young adults: a role for social norms and health based messages. International Journal of Behavioral Nutrition and Physical Activity 2013; 10(1): 73.
50. Becker R, Bloomberg MR, Booker C, Emanuel R, Fischer G, Hales C, et al. (2013). Mayors of Baltimore, Boston, Chicago, Los Angeles, Louisville, Madison, Minneapolis, Newark, New York, Oakland, Philadelphia, Phoenix, Portland, Providence, Salt Lake City, San Francisco, Seattle and St. Louis. Letter to Congressional Leaders. Available: www.nyc.gov/html/om/pdf/2013/snap_letter_to_house_6_18_13.pdf (Accessed 13 July 2013).
51. Aggarwal A, Monsivais P, Cook AJ, Drewnowski A. Positive attitude toward healthy eating predicts higher diet quality at all cost levels of supermarkets. Journal of the Academy of Nutrition and Dietetics 2014; 114(2): 266-272.
52. Leung CW, Hoffnagle EE, Lindsay AC, Lofink HE, Hoffman VA, Turrell S, et al. A qualitative study of diverse experts' views about barriers and strategies to improve the diets and health of Supplemental Nutrition Assistance Program (SNAP) beneficiaries. Journal of the Academy of Nutrition and Dietetics 2013; 113(1): 70-76.
53. Long MW, Leung CW, Cheung LW, Blumenthal SJ, Willett WC. Public support for policies to improve the nutritional impact of the Supplemental Nutrition Assistance Program (SNAP). Public Health Nutrition 2013; 6: 1-6.
54. Pitts SB, Smith TW, Thayer LM, Drobka S, Miller C, Keyserling TC, et al. Addressing rural health disparities through policy change in the Stroke Belt. Journal of Public Health Management and Practice. (Online) 2013. Available: www.ncbi.nlm.nih.gov/pubmed/23446877 (Accessed 3 January 2014).
55. Barnhill A, King KF. Evaluating equity critiques in food policy: The case of sugar-sweetened beverages. The Journal of Law, Medicine and Ethics 2013; 41(1): 301-309.
56. Kohn MJ, Bell JF, Grow HM, Chan G. Food insecurity, food assistance and weight status in US youth: new evidence from NHANES 2007-08. Pediatric Obesity 2014; 9(2): 155-166.
57. Savoca MR, Arcury TA, Leng X, Bell RA, Chen H, Anderson A, et al. The diet quality of rural older adults in the South as measured by healthy eating index-2005 varies by ethnicity. Journal of the American Dietetic Association 2009; 109(12): 2063-2067.
58. Mathematica Policy Research for Feeding America. Hunger in Central and Eastern Kentucky 2010. Available: https://godspantry.org/assets/375/HICEK_2010.pdf (Accessed 1 July 2013).
59. Sohn M. Food and cooking. In: R Abramson, J Haskell (Eds). Encyclopedia of Appalachia. Knoxville: The University of Tennessee Press, 2006; 911-961.
60. Jefferson A. Preparing for a healthier old age. Journal of Family Health Care 2006; 16(1): 9-11.
61. Miller LM, Cassady DL. Making healthy food choices using nutrition facts panels. The role of knowledge, motivation, dietary modifications goals and age. Appetite 2012; 59(1): 129-139.
62. Nyaradi A, Li J, Hickling S, Whitehouse AJ, Foster JK, Oddy WH. Diet in the early years of life influences cognitive outcomes at ten years: a prospective cohort study. Acta Paediatrica 2013; 102(12): 1165-1173.
63. Diehr P, Beresford SA. The relation of dietary patterns to future survival, health and cardiovascular events in older adults. Journal of Clinical Epidemiology 2003; 56(12): 1224-1235.
64. Bouchard DR, Langlois MF, Dominque ME, Brown C, LeBrun V, Baillargeon JP. Age differences in expectations and readiness regarding lifestyle modifications in individuals at high risk of diabetes. Archives of Physical Medicine & Rehabilitation 2013; 93(6): 1059-1064.
65. Ohly J, Pealing J, Hayter AK, Pettinger C, Pikhart H, Watt RG, Rees G. Parental food involvement predicts parent and child intakes of fruits and vegetables. Appetite 2013; 69: 8-14.
66. Quick V, Wall M, Larson N, Haines J, Neumark-Sztainer D. Personal, behavioral and socio-environmental predictors of overweight incidence in young adults: 10-yr longitudinal findings. International Journal of Behavioral Nutrition and Physical Activity 2013; 25: 10-37.
67. Zick CD, Stevens RB. Trends in Americans' food-related time use: 1975-2006. Public Health Nutrition 2009; 13(7): 1064-1072.
68. Williams L, Ball K, Crawford D. Why do some socioeconomically disadvantaged women eat better than others? An investigation of the personal, social, and environmental correlates of fruit and vegetable consumption. Appetite 2010; 55(3): 441-446.
