Stroke is the third leading cause of death in the USA, Canada, Europe and Japan. The American Heart Association and American Stroke Association estimate that approximately 800 000 new strokes occur each year, resulting in more than 130 000 annual deaths in the USA alone1. The incidence of stroke in Poland is similar to that in other European countries (177 per 100 000 in males and 125 per 100 000 in females). Half of these patients die within 1 year, while the remaining half suffer permanent consequences to the central nervous system2.
The introduction of treatment with intravenous (IV) recombinant tissue plasminogen activator (rt-PA) was a milestone in acute ischemic stroke (AIS) treatment. Alteplase was approved by the US Food and Drugs Administration based on the results of the National Institute of Neurological Disorders and Stroke trial in 1996 in the USA and later in Canada, Japan, some countries of South America, and Australia3. A temporary European license was granted in 2003 and a European registry of all thrombolysis procedures - SITS-MOST (Safe Implementation of Thrombolysis in Stroke - Monitoring Study) - was created at the same time4.
It is generally considered that rural hospitals have a much lower capacity to adequately care for patients with AIS. Only a few studies have previously reported on the safety and efficacy of thrombolytic therapy in patients from rural regions5,6. These reports presented different systems of medicine such as emergency air transport and telemedicine. In the region of the Department of Neurology and Stroke Unit, Holy Spirit Specialist Hospital, Sandomierz, south-eastern Poland, air transport and telemedicine systems are not used in routine practice. Despite this, many patients reach the hospital in the critical 'time window' within which thrombolytic therapy can be used.
The aim of the present study was to evaluate which factors affected the safety and the effectiveness of IV thrombolysis performed in a hospital located in an agricultural region, whether the results of treatment in rural and urban population were comparable, and whether patients living in rural areas had similar chances of thrombolytic therapy at night and at weekends.
Sandomierz is a small town with 25 000 inhabitants, located in south-eastern Poland near the border of the European Union. The stroke unit in Sandomierz consists of 23 beds, including 10 intensive care beds. The stroke unit cares for a population of 238 000 people living in four areas: Sandomierz, Opatów and Tarnobrzeg districts, and Tarnobrzeg township. Most of these residents live in rural areas (rural population 151 000; 63.4%). The population of the largest city in the region does not exceed 40 000 inhabitants. Rural areas were identified according to two definitions: territories that are essentially rural, where over 50% of the population lives in rural communities, ie municipalities with a density of less than 150 inhabitants/km2 (OECD definition); and sites outside the cities - areas of rural communities and the rural part (which lies outside a city) of urban-rural communities (Polish Central Statistical Office definition).
The stroke unit of Sandomierz cooperates with three hospitals in the region, at Tarnobrzeg, Opatów and Nowa Deba. The hospital at Tarnobrzeg has a neurological department but not a stroke unit. A small number of patients transferred from two other hospitals in neighboring districts (Staszów and Nisko) are also treated at Sandomierz, but there is no long-term cooperation. Ambulances are stationed in the region of Sandomierz and neighboring hospitals but managed by remote provincial emergency centers.
The stroke unit of Sandomierz is recognized as such according to Polish national criteria and is equipped with proper monitoring and diagnostic facilities7. The neurological status of patients at the moment of admission and again 3 months after symptoms onset (according to the National Institutes of Health Stroke Scale (NIHSS)8), and functional outcome 3 months after symptoms onset (according to the modified Rankin Score (mRS)9), was analyzed. A favourable outcome was defined as an mRS score ≤2 points, while an unfavorable outcome was defined as an mRS of 3-6 points. Haemorrhagic transformation (HT) and symptomatic intra-cerebral haemorrhage (SICH) rates were assessed according to the European Cooperative Acute Stroke Study (ECASS) II criteria10. All patients underwent computed tomography (CT) of the brain prior to treatment, again 22-36 h after the start of treatment and again on the seventh day. The patients had additional CT in cases of neurological deterioration rated as ≥4 points on the NIHSS. All baseline CTs were performed in the hospital in Sandomierz. Magnetic resonance imaging (MRI) was not routinely performed.
The data of all AIS patients treated with alteplase between September 2006 and November 2012 was retrospectively analyzed. The impact of different factors on the effectiveness and safety of IV thrombolysis was evaluated. Days were distinguished according to time (based on a 24 h clock) of admission as follows: weekend days, Saturday 00:01 to Sunday 00:00 plus national holidays; working days, Monday 00:01 to Friday 00:00; daytime, 06:00 to 20:00; night-time, 20:01 to 05:59.
All patients treated with IV thrombolysis in the stroke unit of Sandomierz were reported to the SITS-MOST registry.
Statistical methods
This study was based on a retrospective data analysis. Data gathering, determining baseline characteristics and performing the univariate analysis were done using Microsoft Excel 2010. A logistic regression was performed with STATISTICA v9.1 (StatSoft Inc., http://www.statsoft.com). All continuous variables were tested for normal distribution and equality of variance. Because of the non-normality of the variables, non-parametric Mann-Whitney U-tests were used to perform the univariate analysis of the continuous variables. Categorical data were compared using the χ2 test. The multivariate analysis was performed using a multiple logistic regression. The results of logistic regression models were presented as odds ratio (OR) and the corresponding 95% confidence interval (CI). The variables that reached statistical significance level in the corresponding univariate model were selected in the multivariate model by the backward conditional stepwise method. P values <0.05 were considered statistically significant.
Ethics approval
The ethics committee approved all data analyses (Ethics Committee of Swietokrzyska Medical Chamber - consent no. 8/2011). Each patient, or in case of his/her inability, two physicians, signed the standardized consent form in respect of the ethical principles for Medical Research involving human subjects approved in Helsinki in 1964 by the World Medical Association.
In the analyzed period, in the stroke unit in Sandomierz, 1820 Caucasian patients with AIS were treated, including 300 patients (16.5% of all patients with AIS) treated with IV thrombolysis, (aged 41-92 years, mean 70.2±11.1 years; 163 males (54.3%); time window 0-4.5 hours). Of the total patients, 57.3% were from the Sandomierz district. Before stroke onset, 182 (60.7%) of patients treated with rt-PA lived in rural areas, 92(30.7%) were admitted on the weekend and 64(21.33%) during the night. The median distance from home to the stroke unit was 15.0 (interquartile range (IQR) 8.0-30.0) km. The median onset to treatment time was 160.0 (IQR 130.0-180.0) min. At the moment of admission the median NIHSS score was 11.0 (IQR 8.0-17.0). After 3 months, median NIHSS score and mRS were, respectively, 1.0 (IQR 0.0-4.0) and 2.0 (IQR 0.0-4.5).
In the rural patients thrombolytic therapy at night was performed less frequently compared to urban patients (p=0.01). Differences between both subgroups at weekends and on working days (p=0.47) were not found. The mean age, atrial fibrillation rate, and old ischemic changes in baseline CT were higher in patients from rural areas. The number of males, incidence of other vascular risk factors and early ischemic changes in baseline CT and median NIHSS score on admission did not differ between the subgroups of patients from rural and urban areas. The onset-to-door time, door-to-treatment time and onset-to-treatment time were longer in the group of patients from rural areas but without statistical significance.
The presence of HT and SICH according to the ECASS definition was similar in both groups (p=0.87 and p=0.61, respectively); however, mortality was higher in patients from rural areas (p=0.04) (Table 1).
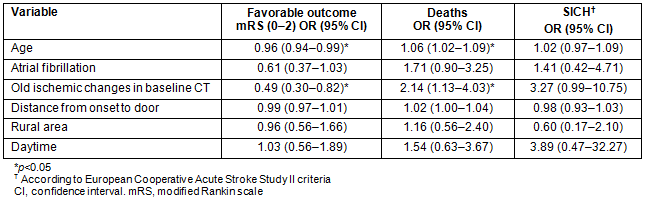
A multivariate analysis showed no impact of place of onset on favorable outcome after 3 months (p=0.9), on the presence of SICH (p=0.43) according to the ECASS definition or on mortality rate (p=0.69).
Table 1: Clinical characteristics of the subgroups of thrombolytic patients from rural and urban areas
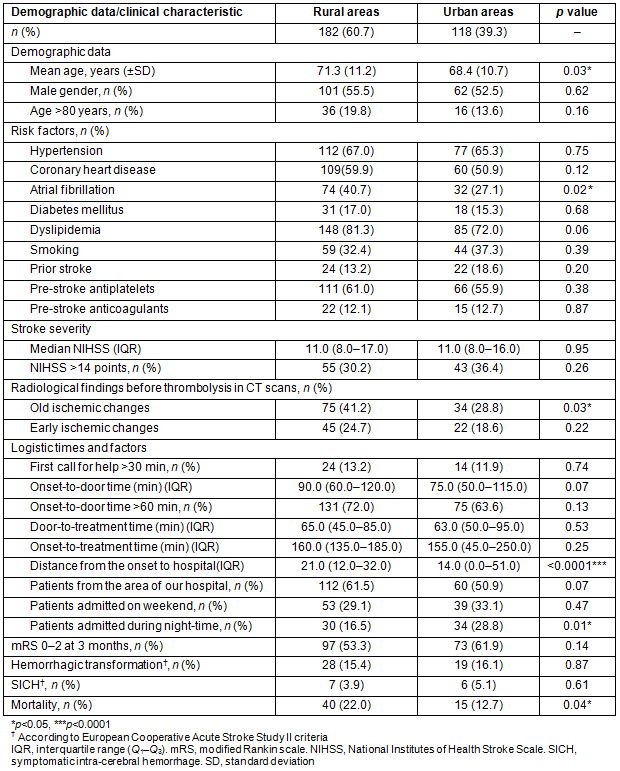
Table 2: Multivariate logistic regression models showing factors associated with
favorable outcome, deaths and hemorrhagic transformation in patients living in rural areas
Discussion
Successful care of AIS victims begins with the recognition by both the public and health professionals that stroke is an emergency11. Organized stroke care, through the use of stroke units, reduces the frequency of complications, improves outcomes, reduces length of stay, and reduces the cost of inpatient AIS care12. It is recommended that those suspected of stroke be transported without delay to the nearest medical center with a stroke unit that can provide ultra-early treatment13. It is also recommended that in remote or rural areas helicopter transfer or telemedicine should be considered in order to improve access to treatment14. In practice, the majority of AIS patients do not receive rt-PA because they do not reach the hospital soon enough15,16. In each community a network of stroke units or, if stroke units are not yet available, a network of emergency departments providing organized acute stroke care should be implemented and publicized to the general population, health professionals and emergency transport systems17.
In the rural population, higher mortality in patients with AIS was found. The findings confirmed data from other studies. Joubert et al. showed an analysis of stroke patient management in rural areas and small communities. In terms of mortality they divided the country into three groups using previously published studies according to the UN Human Development Report. This employs data from its member nations and applies a Human Development Index (HDI) to each country, representing its overall level of development. Among high HDI countries, stroke mortality was higher in rural than in urban areas in Bulgaria, France and Australia; in Canada, urban and rural mortality were similar. In medium HDI countries like China, stroke mortality rates were lower in rural than in urban centers. Finally, in low HDI countries such as Tanzania, stroke mortality in urban areas was significantly higher than in rural areas18.
An assessment of acute stroke care capacity and services in the north-western region in the USA in 2008 showed that emergency departments and rt-PA protocols were significantly less common in rural hospitals. Stroke death rate in adults aged ≥45 years was significantly higher in this region than in the rest of the USA19.
The study showed that 16.5% of all patients with AIS admitted to the stroke unit received thrombolytic treatment. In rural north-eastern Florida/south-eastern Georgia, prospectively collected data from 111 consecutive helicopter stroke transports showed that 38% of AIS patients were treated with rt-PA20. These patients were transported by a helicopter. In a 100-bed rural hospital in Nebraska, between 1998 and 2004, 4% of patients with AIS were treated with rt-PA21. Another study showed that a structured telephone interview from a rural physician with a stroke specialist was effective in resulting in a reduced door-to-treatment time22.
In the stroke unit in Sandomierz, 41.8% of patients from other districts were treated. In this group of patients the onset-to-treatment time was longer than in patients transported directly from the place of onset. A much higher proportion of patients living in rural areas needed transportation to a distant hospital, because the local hospital in their neighborhood did not specialize in acute stroke management, resulting in further delay of treatment initiation23. Any transportation apart from the emergency medical service and to hospitals without a stroke unit significantly prolonged the time until arrival at a stroke unit24.
In the sample, the rural patients were less likely to be treated with IV thrombolysis at night. This resulted from lower availability of telecommunication services and the lack of public transport after 8 pm. There were no differences between the availability of treatment at weekends and weekdays. Similar information in literature with regard to rural and urban areas was not found.
In the analyzed period, age structures in the rural and urban areas were similar (14.5% and 15.7% of the population >65 years, respectively). Despite less availability of health care (3854 inhabitants per rural GP clinic compared with 1767 inhabitants per urban GP clinic), efficacy and safety of systemic cerebral thrombolysis were similar.
The authors perceive the need to shorten pre-hospital procedures by introducing an absolute principle that patients should be delivered to a hospital with a stroke unit directly from the place of onset.
The retrospective nature of this study's data may be considered a limitation of this study, which has, therefore, inferior value compared to prospective and randomized trials. However, these findings present data about efficacy and safety of IV thrombolysis in rural and urban patients treated in a hospital located in an agricultural region.
It is suggested that patients from rural areas have a smaller chance of treatment with IV thrombolysis at night. Rural and urban patients treated in the hospital located in the agricultural region had a similar efficacy and safety profile of thrombolytic treatment.
With a good healthcare organization, a high percentage of patients with ischemic stroke can be treated with systemic cerebral thrombolysis in rural areas.
During the day, and on working days and at weekends, differences in availability of treatment were not found. There is a need to improve telecommunication and transport of patients from rural areas during the night to give them the same opportunity for thrombolytic therapy as those in the urban population.
Despite many differences between the urban and rural population, according to demographic, logistic and clinical data, safety and efficacy of systemic cerebral thrombolysis were similar.
Acknowledgements
The authors thank Grzegorz Kozera from the Department of Neurology, Medical University of Gda?sk, for helpful comments on an earlier draft of the manuscript and for the assessment of the statistical analysis.
References
1. Lloyd-Jones D, Adams RJ, Brown TM, Carnethon M, Dai S, De Simone G, et al. Executive summary: heart disease and stroke statistics - 2010 update: a report from the American Heart Association. Circulation 2010; 121: 948-954.
2. Czlonkowska A, Ryglewicz D. Epidemiology of cerebral stroke in Poland. Neurologia i Neurochirurgia Polska 1999; 32(Suppl 6): 99-103.
3. National Institute of Neurological Disorders and Stroke rt-PA Stroke Study Group. Tissue plasminogen activator for acute ischemic stroke. New England Journal of Medicine 1995; 333: 1581-1587.
4. Wahlgren N, Ahmed N, Davalos A, Ford GA, Grond M, Hacke W, et al. Thrombolysis with alteplase for acute ischemic stroke in the Safe Implementation of Thrombolysis in Stroke-Monitoring Study (SITS-MOST): an observational study. Lancet 2007; 369: 275-282.
5. Silliman SL, Quinn B, Huggett V, Merino JG. Use of a field-to-stroke center helicopter transport program to extend thrombolytic therapy to rural residents. Stroke 2003; 34: 729-733.
6. Edwards LL. Using tPA for acute stroke in a rural setting. Neurology 2007; 68: 292-294.
7. Czlonkowska A, Sarzynska-Dlugosz I, Niewada M, Kobayashi A. Eligibility of stroke units in Poland for administration of intravenous thrombolysis. European Journal of Neurology 2006; 13: 220-224.
8. Lyden P, Brott T, Tilley B, Welch KM, Mascha EJ, Levine S, et al. Improved reliability of the NIH Stroke Scale using video training. NINDS TPA Stroke Study Group. Stroke 1994; 25: 2220-2226.
9. Bonita R, Beaglehole R. Modification of Rankin Scale: recovery of motor function after stroke. Stroke 1988; 19: 1497-1500.
10. Hacke W, Kaste M, Fieschi C, von Kummer R, Davalos A, Meier D, et al., for the Second European-Australasian Acute Stroke Study Investigators. Randomised double-blind placebo-controlled trial of thrombolytic therapy with intravenous alteplase in acute ischaemic stroke (ECASS II). Lancet 1998; 352: 1245-1251.
11. Wang MY, Lavine SD, Soukiasian H, Tabrizi R, Levy ML, Giannotta SL. Treating stroke as a medical emergency: a survey of resident physicians' attitudes toward 'brain attack' and carotid endarterectomy. Neurosurgery 2001; 48: 1109-1115.
12. Leira EC, Hess DC, Torner JC, Adams HP. Rural-urban differences in acute stroke management practices: a modifiable disparity. Archives of Neurology 2008; 65: 887-891.
13. The European Stroke Organization (ESO) Executive Committee and the ESO Writing Committee. Guidelines for management of ischaemic stroke and transient ischaemic attack 2008. Cerebrovascular Diseases 2008; 25: 457-507.
14. Schwab S, Vatankhah B, Kukla C, Hauchwitz M, Bogdahn U, Fürst A, et al. Long-term outcome after thrombolysis in telemedical stroke care. Neurology 2007; 69: 898-903.
15. Harraf F, Sharma AK, Brown MM, Lees KR, Vass RI, Kalra L. A multicenter observational study of presentation and early assessment of acute stroke. British Medical Journal 2002; 325: 17-21.
16. Barber PA, Zhang J, Demchuk AM, Hill MD, Buchan AM. Why are stroke patients excluded from TPA therapy? An analysis of patient eligibility. Neurology 2001; 56: 1015-1020.
17. Stroke Unit Trialists' Collaboration. Organised inpatient (stroke unit) care for stroke. Cochrane Database Systematic Reviews 2007; CD000197.
18. Joubert J, Prentice LF, Moulin T, Liaw ST, Joubert LB, Preux PM, et al. Stroke in rural areas and small communities. Stroke 2008; 39: 1920-1928.
19. Shultis W, Graff R, Chamie C, Hart C, Louangketh P, McNamara M, et al. Striking rural-urban disparities observed in acute stroke care capacity and services in the Pacific Northwest. Implications and recommendations. Stroke 2010; 41: 2278-2282.
20. Silliman SL, Quinn B, Huggett V, Merino JG. Use of a field-to-stroke center helicopter transport program to extend thrombolytic therapy to rural residents. Stroke 2003; 34: 729-733.
21. Edwards LL. Using tPA for acute stroke in a rural setting. Neurology 2007; 68: 292-294.
22. Vaishnav AG, Pettigrew LC, Ryan S. Telephonic guidance of systemic thrombolysis in acute ischemic stroke: safety outcome in rural hospitals. Clinical Neurology and Neurosurgery 2008; 110: 451-454.
23. Kozera G, Chwojnicki K, Gójska-Grymajlo A. Gasecki D, Schminke U, Nyka WM. Pre-hospital delays and intravenous thrombolysis in urban and rural areas. Acta Neurologica Scandinavica 2012; 126: 171-177.
24. Mandelzweig L, Goldbourt U, Boyko V, Tanne D. Perceptual, social, and behavioral factors associated with delays in seeking medical care in patients with symptoms of acute stroke. Stroke 2006; 37: 1248-1253.


