Geographic maldistribution of health resources is an old and worldwide issue. In Japan, the first resource allocation policy for medically underserved areas was introduced in 1957 and has been revised 11 times1. The key concept and term used in this policy is 'non-physician community' (NPC; mui-chiku in Japanese), which is used for demarcating medically underserved areas that need a more focused allocation of health resources. The concept of NPC was first employed in the revision of this policy in 1960 and has remained unchanged until now. It has been used as the only officially defined political term that indicates medically underserved areas1. The national definitions of NPC and semi-NPC are as follows:
- Non-physician community: a community without a medical facility where 50 or more persons dwell within a geographic area diameter of 4 km and have difficulty commuting to primary medical care facilities in other areas. The area is certified as a 'difficult commute' when it meets one of the following criteria: (1) regular public transportation with less than four round trips to the nearest facility a day or (2) commute time of more than one hour to reach a facility.
- Semi-non-physician community: an equivalent community to the original definition of non-physician communities as determined by a prefecture.
Both NPC and semi-NPC are basically certified based on national definitions of NPC by each prefecture and are treated equally in governmental policies although there is no definition of the boundary of a community.
The Japanese government prioritizes budget allocations in designated NPCs with an aim of providing an equitable health resource distribution. The allocated budget has been used for establishing medical clinics, support of patient transportation services, to provide mobile-clinic services and for telehealth, which is the delivery of health services and information through telecommunications technologies for people in NPCs (Fig1). A substantial amount of the national budget has been allocated to each prefecture under the policy. For example, Hiroshima prefecture alone has used 3153 million yen (approximately US$31.5 million) to implement the 11th revised policy of 20112.
For this past half-century, the number of NPCs has continuously decreased: from 2373 in 1971, to 1276 in 1984, and to 705 in 2009. Similarly, the total population in NPCs has continuously decreased: 884 844 in 1971, 219 796 in 1984, and 136 272 in 2009. However, this rapid decrease of NPCs is not necessarily due to the effect of the policy. For example, among the 138 communities excluded from NPCs between 1999 and 2004, 76 (56.3%) were excluded due to an improvement in transportation accessibility to nearby clinics/hospitals3. This means that improvements in roads, not the allocation of health resources, caused the apparently successful result. Also, 33 (24.4%) of the communities were excluded due to a decrease in the local population. Communities whose population decreased to less than 50 are, by definition, excluded from consideration as an NPC. The number of communities excluded for this reason was larger than the number of communities included due to closure of existing medical facilities (n=31)4. This change reflects the decrease in household sizes in Japan. The average number of household members was 4.13 in 1961, 3.22 in 1986, and 2.59 in 20105. In this context, the proportion of small communities whose population is less than 50 must be increasing. It is possible that many of the communities excluded from NPCs for this reason are still as medically underserved as before, although they are now smaller in population size.
In spite of the NPC's long-time use, the effectiveness and validity of the concept of NPC has not been evaluated. Due to the radical social, demographic, and infrastructure changes affecting rural areas over this half-century, the definition of NPC may potentially be outdated as an optimal tool for delineating medically underserved areas. Therefore, in this study, we examine whether there is substantial difference between NPCs and surrounding rural communities in commute time to the nearest medical facility. We also tested a similar hypothesis between NPCs and their municipal centers. Through the analyses we examined whether designated NPCs are still more disadvantaged in geographical accessibility to medical services than other communities and, as such, whether they should continue to be considered as a focus for healthcare resource allocation.

Figure 1: (A) A typical non-physician community in Japan and (B) a mobile clinic
service at a non-physician community in Jinseki-Kougen Town, Hiroshima.
Study area
For this study, we selected Hiroshima prefecture, which had the largest number of designated NPCs among the 45 prefectures of Japan with a single tertiary healthcare area6. Japan consists of three healthcare area (primary, secondary and tertiary) levels as per the Medical Care Act. Each tertiary healthcare area (san-ji-iryou-ken) subsumes secondary and primary health care areas. Each tertiary healthcare area is, in general, identical in each prefecture. Typical healthcare is expected to be provided within a secondary healthcare area, and highly advanced care is to be provided within a tertiary healthcare area.
Hiroshima prefecture is located in the western part of Japan (Fig2). The population in 2011 was 2 860 750 according to the 2010 National Census data. Hiroshima consists of a mountainous northern region and a coastal southern region.
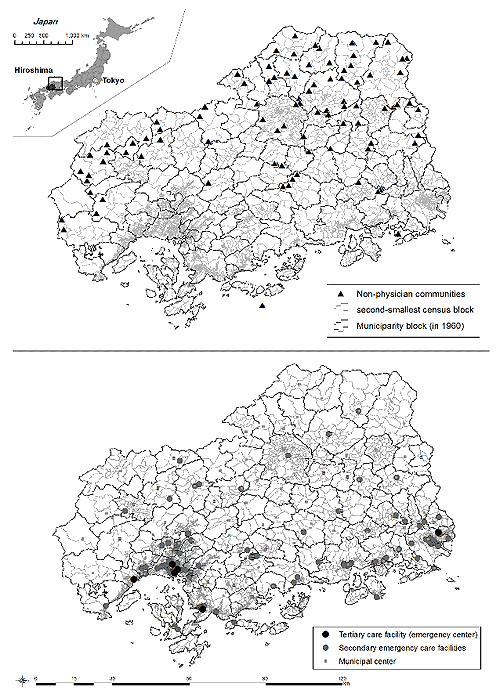
Figure 2: Map of Hiroshima prefecture (a single tertiary healthcare area)
showing non-physician communities (top) and healthcare facilities (bottom).
Geographic unit of analysis, non-physician communities, and control communities
The latest list of designated NPCs in 2009 was obtained from the Survey of Non-physician Communities conducted by the Ministry of Health, Labour and Welfare3. According to the survey, in Hiroshima prefecture, 79 communities were defined in the survey as NPCs (53 of NPC and 26 of semi-NPC). In Hiroshima prefecture, the number of NPCs decreased from 67 in 2004 to 63 in 2009. Similarly, the total population in NPCs had decreased from 9692 in 2004 to 9467 in 2009. Some of the 79 NPCs contained multiple communities. We thus adopted 94 community points as NPCs (64 of NPC and 30 of semi-NPC) for this study. We excluded two semi-NPCs on small islands, because we could not select a control community for them. In total, 92 NPCs were enrolled in this analysis.
The smallest census block ('community') was regarded as the geographic unit in this study. A census block is a basic unit that composes a municipality (city, town or village). In 2010, there were 4430 census blocks in the 23 municipalities of Hiroshima prefecture. The centroid point (a geographical center of each block) of a census block was adopted as the representing point of the community in the analyses. In general, the geographic unit used for designating a NPC is slightly smaller in area than the census block. Thus, the centroid point of the community was adopted as the proxy representing point of the NPC.
Since the 1960s, large-scale mergers of municipalities have been enforced (110 cities or towns in 1960 reduced to 23 in 2013). Although administrative areas were merged for political reasons7, old boundaries are still used by people in terms of a livelihood sphere. In this analysis, we adopted the administrative boundary of cities or towns in 1960 as the municipal boundary.
Next we selected two types of control communities. The two types were defined as follows:
- control A (non-NPC): non-NPC that is geographically closest to a certain NPC
- control B (municipal center): a community that has a municipal hall or a branch of the hall and thus is seen as at the center of a municipality (city or town).
Non-NPC (control A) was defined as a community: (1) that is in the municipality in which the NPC is located, and (2) whose driving time (road distance) to the municipal center is closest to that of the NPC among all the surrounding communities of the NPC. Some of the NPCs are so close to each other that a single control was selected for all of them. Finally, we selected 63 non-NPCs and 36 municipal centers for this analysis.
Healthcare facilities
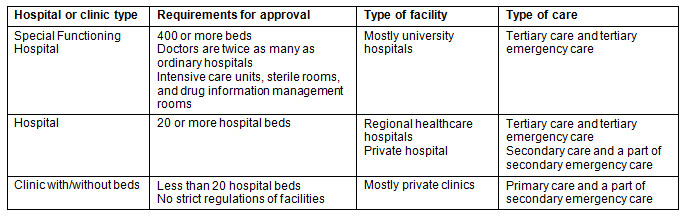
A list of all medical facilities with inpatient beds was obtained from the Health and Welfare Affairs Bureau of the Hiroshima Prefectural Government. These medical facilities were classified into the following two types: primary or secondary care facilities (n=2636); and tertiary care facilities, which are equal to tertiary emergency care centers (n=6). We further extracted secondary emergency care facility (n=246) from the 2636 primary or secondary care facilities. Medical care facility types are shown in Table 18,9. In this analysis, we excluded psychiatric hospitals, clinics embedded in special elderly nursing homes, and facilities for the disabled from the analyzed facilities because these facilities were not for general outpatients.
In Japan, there is no accredited discipline of primary care or family medicine. In general, primary care is mainly provided by departments of internal medicine in clinics or small hospitals. As such, facilities were divided into those with an internal medicine department and those without, in order to examine whether access times from the studied communities differed between internal medicine and other facilities.
Table 1: Type of medical institutions restricted by the Medical Care Act8,9
Measuring accessibility
Using a geographical information system package, we measured driving time by car from each community to a medical facility. The calculation process included network analysis (ie found the shortest travel path between two locations on a road network, including highways) using ArcGIS v10.0 (ESRI Japan Inc.; http://www.esrij.com/products/arcgis) and ArcGIS Data Collection Road Network 2011 (ESRI Japan Inc.; http://www.esrij.com/products/data/datacollection). In Road Network, the driving speeds of all road segments are classified into 14 categories depending on the type and width of the segment.
Measurement of area-based characteristics
Data for household, population density, population by sex and age group at each census block (community) was obtained from the 2010 National Census. An elderly rate was calculated by dividing the number of those older than 65 years by total population in each area. The area of a census block is smaller than a municipality (city or town), but in general larger than the geographic unit used for defining NPCs. Data in the census block was adopted as proxy data for the NPCs.
Statistical analysis
The difference in median driving time between NPCs and control communities was evaluated with the median test (non-parametric tests algorithms). For all analyses, p<0.05 (two-sided) was considered statistically significant. Descriptive statistics and correlation analysis were conducted with the Statistical Package for the Social Sciences v21 (IBM Japan; http://www.spss.com).
Ethics approval
This study was approved as a study that can be conducted without individual informed consent by the Ethics Committee of Epidemiological Research, Hiroshima University (#Epidemiology-779).
Table 2 shows geographic and demographic characteristics of NPCs and two types of control communities. The NPCs had a lower median population density than both types of controls (13 persons per km2 (NPC) vs 28 (non-NPC) and 70 (municipal center)) and a higher elderly rate (≥65 years) (46% vs 42% and 32%, respectively).
Figure 3 shows driving time (minutes) to each type of health facility of a NPC and two types of control community. The respective median driving times of NPCs, non-NPCs and municipal centers were 11 minutes, 11 minutes, and 1 minute to a primary or secondary care facility; 80 minutes, 84 minutes, and 68 minutes to a tertiary care facility; and 24 minutes, 18 minutes, and 15 minutes to a secondary emergency care facility, respectively. Municipal centers had a significantly shorter driving time to a primary clinic or secondary hospital than NPCs and non-NPCs. The difference in driving time between NPC and non-NPC, however, was not observed in all types of medical facilities.
Similar results were obtained in an analysis of driving times to internal medicine facilities from NPCs and control communities (Fig3).
Table 2: Geographic and demographic characteristics for non-physician communities (NPCs)
and two types of control community (adjacent non-NPC and municipal center).
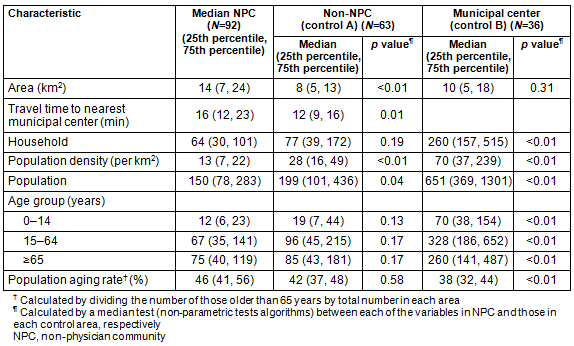
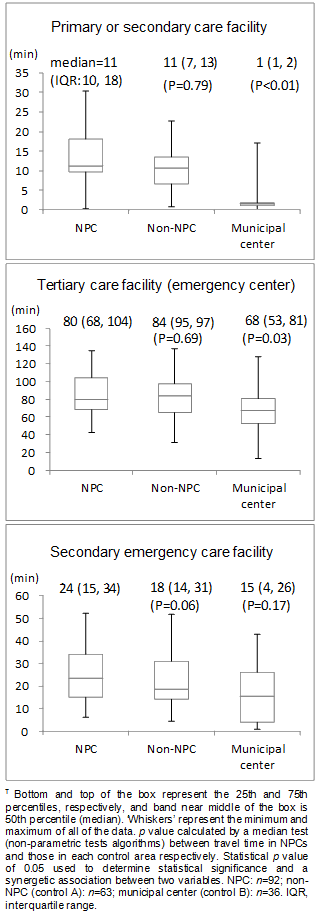
Figure 3: Travel time (min) to each health facility from non-physician
communities (NPCs) and control communities (non-NPCs and municipal center).?
Discussion
Non-physician communities had a disadvantage in access time to secondary and tertiary medical care when compared with the geographic center (control B) of each municipality region. This disadvantage of an NPC disappeared when compared with an adjacent non-NPC (control A) that was similarly rural. In addition, there was no substantial difference in accessibility to an emergency care facility between NPCs and non-NPC. As a result, a substantial gap in accessibility to health services between NPC and non-NPC did not exist.
These results indicate that, in spite of the half-century of use of this concept in a Japanese political context, NPC may not actually be a special category of community that needs focused health resource allocation. The substantial decrease of NPCs over the past 50 years also suggests that focused resource allocation to NPCs was effective. However, the conventional definition of NPC does not match the current situation of rural health in Japan. As the results of this study and past studies have shown, 'underserved areas', as defined by the current definition, are not necessarily underserved10,11. A revision of the concept is needed for a proper redistribution of health resources among the population.
A substantial gap in accessibility to health services between an NPC and adjacent non-NPC does not exist. This may be because the definitions of NPC, which have been unchanged since 1960, do not correspond to the social changes and current health needs of the contemporary population. During this half-century the social context of Japan has changed substantially.
First, the traffic infrastructure has been improved, particularly in rural areas. This is in large part due to national road policies12. This phenomenon increased the areas where people could access a medical care service in a short time if they owned their own car. In addition, private car usage increased from 40% in 1975 to 60% in 20034. Second, the number of physicians both in urban and rural areas has increased dramatically through national policies, which has been more prominent in urban areas than in rural areas13,14. These factors might have worked to diminish the access time gap among rural populations, for example, between those in NPCs and non-NPCs.
Over this past half-century, the need for medical services has changed toward higher levels of medical service. Accessibility to these levels of care is not taken into account in the conventional definition of NPC. People are now increasingly requiring a guarantee of access not only to primary but also to secondary and tertiary care15 and emergency centers16.
There are some limitations to this study. The subjects of this study were limited to persons in Hiroshima prefecture. The direct application of the results is therefore limited to this part of Japan - caution is needed to apply the results to other areas. The social and demographic change over the past 50 years, however, have occurred in similar ways across all parts of Japan4. Thus, similar results are expected for other areas of Japan. Because no previous studies quantitatively compared healthcare accessibility between NPC and non-NPC, it is possible that the accessibility gap that has long been assumed to exist has actually not existed from the beginning. Comparative evaluation between NPC and non-NPC should have been incorporated in the policy assessment at the initiation of this policy.
Based on the results, we propose that the government should pursue a major revision in resource redistribution policies. In order to meet the needs of a rapidly aging7 and depopulated17 rural population, a newly defined area, instead of conventional NPC, should be introduced as a focus of resource allocation. The new area should be a medically underserved area without the limitation of being within a 4 km radius so that it includes both NPCs and their adjacent communities. The similarity between NPCs and adjacent communities found in this study in terms of accessibility to medical facilities supports this proposal. The condition of needing a minimum of 50 residents in the conventional NPC definition should be reconsidered, because the number has less meaning in the context of current depopulated rural areas. The new definition should include a condition concerning access time measured with new technology such as geographical information systems. Addressing these issues may suggest a new definition of NPC, which requires further examination.
Overall, the definition of 'non-physician community' is not suitable to the current social situation. The future resource allocation policies in Japan need to redefine medically underserved communities.
Acknowledgements
The authors would like to thank Jinseki-Kogen Town, Hospital Director Dr Wataru Harada, and the staff at the Jinseki-Kogen Municipal Office for their support of this study. We also appreciate the assistance from the staff of the Health and Welfare Affairs Bureau, Hiroshima Prefectural Government, in providing the medical facilities data. The software used in this study was supplied by the Higher Education Grant Program of ESRI Japan Corp. (Tokyo, Japan).
This work was supported by a grant from the 21st (2012) Joint Research Project from the Pfizer Health Research Foundation (12-8-075).
References
1. Ministry of Health, Labour and Welfare. Structural chart of 11th measures for health and medical services in remote areas (FY2011-2015). Annual health, labour and welfare report 2011-2012. (Online) 2012. Available: http://www.mhlw.go.jp/english/wp/wp-hw5/dl/23010214e.pdf (Accessed 28 June 2013).
2. Health and Welfare Affairs Bureau, Hiroshima Prefectural Government. 5 Hekichi/chusankan-tiiki iryou taisaku no jyujitsu in Iryou taisei seibi jigyou (Section 5 Enhancement of measures for medical services in remote rural areas/hilly and mountainous areas in improvement project of medical system). (Online) 2011. Available: http://www.pref.hiroshima.lg.jp/uploaded/attachment/13617.pdf (Accessed 6 September 2013).
3. Ministry of Health, Labour and Welfare. Muichiku tou chosa (Survey of non-physician communities). (Online) 2010. Available: http://www.mhlw.go.jp/toukei/list/76-16.html (Accessed 26 September 2013).
4. Ministry of Land, Infrastructure, Transport and Tourism. White paper on Ministry of Land, Infrastructure, Transport and Tourism in Japan (Online) 2008. Available: http://www.mlit.go.jp/english/white-paper/2008.pdf (Accessed 9 September 2014).
5. Ministry of Health, Labour and Welfare. Summary report of Comprehensive Survey of Living Conditions 2011. (Online) 2012. Available: http://www.mhlw.go.jp/english/database/db-hss/dl/report_gaikyo_2011.pdf (Accessed 12 September 2013).
6. Medical Policy Division, Health and Welfare Affairs Bureau, Hiroshima Prefectural Government. (Hiroshima-ken hekichi-chiiki-hokeniryou keikaku 2011-2015) (The eleventh Hiroshima remote place health care plan 2011-2015). (Online) 2011. Available: http://www.pref.hiroshima.lg.jp/soshiki/54/1300861118753.html (Accessed 30 June 2013).
7. Council of Local Authorities for International Relations. Local government in Japan. (Online) 2010. Available: http://www.jlgc.org.uk/en/pdfs/LocalGovernmentInJapan2010.pdf (Accessed 29 June 2013).
8. Tatara K, Okamoto E. Japan: health system review. Health systems in transition 11(5): 1-164. (Online) 2009. Available: http://www.euro.who.int/__data/assets/pdf_file/0011/85466/E92927.pdf (Accessed 27 July 2013).
9. Ministry of Health, Labour and Welfare. Types of medical institutions. Annual health, labour and welfare report 2009-2010 (Online) 2012. Available: http://www.mhlw.go.jp/english/wp/wp-hw4/dl/health_and_medical_services/P39.pdf (Accessed 25 September 2013).
10. Hart LG, Larson EH, Lishner DM. Rural definitions for health policy and research. American Journal of Public Health 2005; 95(7): 1149-1155.
11. Matsumoto M, Kashima S, Ogawa T, Takeuchi K. Do rural and remote areas really have limited accessibility to health care? Geographic analysis of dialysis patients in Hiroshima, Japan. Rural and Remote Health. 13(3): 2507. (Online) 2013. Available: www.rrh.org.au (Accessed 29 August 2013).
12. Ministry of Land, Infrastructure, Transport and Tourism. Roads in Japan. (Online) 2012. Available: http://www.mlit.go.jp/road/road_e/pdf/ROAD2014web.pdf (Accessed 9 September 2014).
13. Matsumoto M, Inoue K, Kajii E, Takeuchi K. Retention of physicians in rural Japan: concerted efforts of the government, prefectures, municipalities and medical schools. Rural and Remote Health 10(2): 1432. (Online) 2010. Available: www.rrh.org.au (Accessed 28 June 2013).
14. Inoue K, Matsumoto M, Toyokawa S, Kobayashi Y. Transition of physician distribution (1980-2002) in Japan and factors predicting future rural practice. Rural and Remote Health 9(2): 1070. (Online) 2009. Available: www.rrh.org.au (Accessed 27 August 2013).
15. Ministry of Health, Labour and Welfare. Section 1: Enhancing a safe, reliable, and high quality medical care system. Annual Health, Labour and Welfare Report 2007-2008. (Online) 2008. Available: http://www.mhlw.go.jp/english/wp/wp-hw2/part2/p2c1s1.pdf (Accessed 11 August 2013).
16. Investigative commission for the future of emergency medical service in Ministry of Health, Labour and Welfare. Kyukyuiryou no kongonoarikatani kansuru kentoukai (Interim report of investigative commission for the future of emergency medical service). (Online) 2008. Available: http://www.mhlw.go.jp/shingi/2008/07/dl/s0730-21a.pdf (Accessed 11 August 2013).
17. Ministry of Internal Affairs and Communications. 'Kaso taisakuno genjyo' ni tsuite (Present situation of provision for depopulated areas in 2012). (Online) 2011. Available: http://www.soumu.go.jp/main_content/000186144.pdf (Accessed 25 September 2013).
Correction: A correction was made to the Results section of the Abstract on 7 October 2014.


