Recruitment and retention of a skilled health workforce is a well-established challenge in rural Australia1. Despite recent reports of a general oversupply of pharmacists2, there remains a shortage of pharmacists in rural areas. A 2012 Allied Health Workforce report indicated that the number of pharmacist per 100 000 population in outer regional areas and remote areas are two-third and half, respectively, of that in major cities (129 pharmacists per 100 000 population)3. Many rural hospitals are unable to recruit or retain a full-time pharmacist, or are not large enough to justify employment of a full-time pharmacist, which results in a less attractive employment option4-6. This has been reported to impact on medication management services in those areas4,7,8. Specific areas of concern include the absence of a pharmacist's involvement in medication review, medication reconciliation, dispensing, patient and staff education, and quality management relevant to medications9.
Pharmacists have a significant role in medication management as advocates of quality use of medicines (QUM)10-13. Specifically, a multi-hospital study conducted in 1998 demonstrated the value of pharmacists' interventions in preventing or addressing serious medication-related problems, improving effectiveness of therapy and reducing patient morbidity10. This resulted in reduction in length of stay, readmission probability and expenditure resulting from hospitalisations (annualised cost savings exceeding A$4 million for the eight study hospitals)10. Despite the value of pharmacists' contributions to clinical services and the call for increased roles for pharmacists in rural healthcare4,14, there is little evidence to guide the development of pharmacist-driven support services in rural hospitals.
In rural hospitals without a pharmacist on staff (referred as non-pharmacist hospitals), registered nurses commonly extend their roles to provide technical pharmacy services. This included stock ordering, supplying medication and providing basic medicines information5,8,15,16. These roles have been perceived to be beyond nurses' scope of practice, add workload burden to nursing staff, and are not as comprehensive as the medication management services provided by a pharmacist8,15-17. Indeed, studies have highlighted the need for increased involvement by pharmacists in non-pharmacist hospitals to address gaps in medication management services5,8,16,18.
Preliminary research in a rural community in Queensland has revealed that part-time contracted ('sessional') pharmacy services, usually provided by the local community pharmacist, had been instigated to address medication management shortfalls in rural non-pharmacist hospitals16,19. This mirrors traditional models of rural general practitioners providing contracted services to their local public hospital ('cross-sector')1,8,20, but there are few such reported models for allied health providers21. Moreover, there is no known research into such models involving pharmacists.
The term 'sessional' was adopted from the Australian Pharmacy Council's Remote rural pharmacists project report (2009)8 and preliminary research, as a mode of employment of pharmacists to provide medication management support to non-pharmacist sites. A relevant description of 'sessional' is provided by the Society of Hospital Pharmacists of Australia's A Victorian public hospital pharmacy workforce analysis (2002)22. This report described sessional pharmacy service as contract services by an external pharmacist who is not an employee of, or based at, the hospital22. Due to the lack of research into this topic, the operational definition of 'sessional' was adapted as follows:
- a local community pharmacist providing medication support to the non-pharmacist hospital
- a visiting pharmacist from a nearby town or a town within the rural district providing medication support to a non-pharmacist hospital
- an accredited pharmacist (local or visiting) providing medication management services to a non-pharmacist hospital.
The second and third descriptions overlap somewhat with the concept of 'outreach' services. However, sessional services comprise cross-sector contracted services of an external pharmacist. In contrast, outreach hospital pharmacy services typically involve metropolitan or regionally based pharmacists of a large hospital to provide consultation support or services to a rural facility within the hospital's governance area19.
Findings reported in the present article were part of a larger study investigating rural medication management services. It has been reported through this study that non-pharmacist service providers may not recognise the value of a pharmacist's involvement, which challenged the integration of pharmacists in a rural hospital setting favouring acute medical and nursing services23. Hence, the aim of the present study was to explore the roles and experiences of pharmacists who provided cross-sector, sessional services to rural hospitals that had no on-site pharmacist and explore how these roles could address shortfalls in medication management in rural hospitals. The present article highlights the significance of a pharmacist's involvement in patient care and provides examples of service delivery models for other rural hospitals to adapt when considering strategies to address medication management needs.
This study used exploratory research methods to provide in-depth insights into the sessional employment contracts negotiated by participants24.
The sampling approach aimed to identify any non-hospital pharmacist who provided medication management services, preferably beyond emergency medication supply and dispensing support, to a rural hospital. The study was advertised in professional newsletters, networks and online forums in Australia. The advertisement outlined the study's inclusion criteria (eg a community pharmacist servicing a local rural hospital, a community or hospital pharmacist servicing a hospital within the rural district, or an accredited pharmacist servicing a rural hospital). A snowball25 recruitment method through respondents was used to identify further participants who fulfilled the study's inclusion criteria. Recruitment continued until theme saturation had been perceived by the interviewer, and/or avenues for recruitment had been exhausted. Sampling in Australia was exhausted using the above advertisement strategy, and the study was extended to include New Zealand (NZ) pharmacists. Recruitment in NZ was facilitated by two academic contacts who identified potential participants from hospital lists.
All recruited pharmacists confirmed the relevance of their role in relation to sessional employment of pharmacists in rural areas and were given information about the study prior to interview. The semi-structured interview guide24 was informed by literature review, preliminary research and stakeholder consultation. The interviews explored the underlying reason(s) for establishing the sessional contract, the scopes of services, logistic arrangements (eg remuneration, hours, contract length) and perceived outcomes. Interviews were conducted either by telephone or Skype between August 2012 and January 2013. Participants provided verbal consent at the start of the interview. All interviews were recorded. Interviews were 40-55 minutes each and participants were mailed a gift card (A$50 or NZ$50) to compensate for their time. Participants were de-identified and the interviews were transcribed verbatim (excluding formalities and comments unrelated to sessional pharmacy services). The transcripts were then manually screened by author AT for common themes, which were reviewed, refined and validated by authors LE, LH and ALC.
A detailed description of the method for the overall study, including the interview guide, is reported elsewhere23.
Ethics approval
Ethics approval for data collection was obtained from the University of Queensland's School of Pharmacy Human Research Ethics Committee (2012/9).
Seventeen pharmacists participated in the study and described models implemented in New South Wales, Queensland, South Australia, Western Australia, NZ South Island and NZ North Island (Australian participants are annotated 'A' and NZ participants annotated 'NZ'). Thirteen participants (Table 1) already had experience in providing sessional services to a non-pharmacist hospital. Four participants had negotiated or were interested to implement sessional employment contracts, but had not practised in this capacity. These were excluded, as this paper focuses on sessional services that had been implemented, rather than theoretical models. Facilitators and barriers from the perspective of these four participants have been reported elsewhere23.
Of the 13 models, two had expanded into full-time positions (Table 1), eight were ongoing sessional positions (Table 2), and three had been discontinued (Table 3). At the time of service provision, participants A1, A2, A9, A10, NZ1, NZ2, NZ3, NZ4 and NZ5 were local members of their communities. Participants A4 and A6 had work experience in other rural communities. Participants A3 and A7 were located in a regional town and major city, respectively, with experience providing medication management services and support to rural communities.
The majority of participants believed they were the first pharmacist to service the rural hospital. Participants A7, A10 and NZ3 were involved in instigation of the service, whereas other participants 'fell into' the sessional role when it was being instigated. Although participants A6 and NZ3 were not the first to be involved in sessional support, they provided enhanced clinical support to their respective hospitals that previously only received pharmaceutical distribution support from the local community pharmacy. Participant A1's and A2's roles expanded over the duration of their sessional employment.
Most models were located in towns of fewer than 5000 residents, with one or more hours travel by road from a major service hub. The inclusion of models from larger or regional towns (A2, NZ1 and A10) was to broaden the discussion of sessional employment models, given the lack of research into this topic. To maintain confidentiality, participants are not associated in this article with their location of practice, departments or companies, age or years of practice. Three key themes (the need for a pharmacist involvement at the rural hospital, sessional employment of a pharmacist as a practice initiative, and the value of the pharmacists' involvement in improving QUM) and supporting quotations are presented below.
Table 1: Descriptions of expanded sessional models

Table 2: Descriptions of ongoing sessional models (at the time of study)
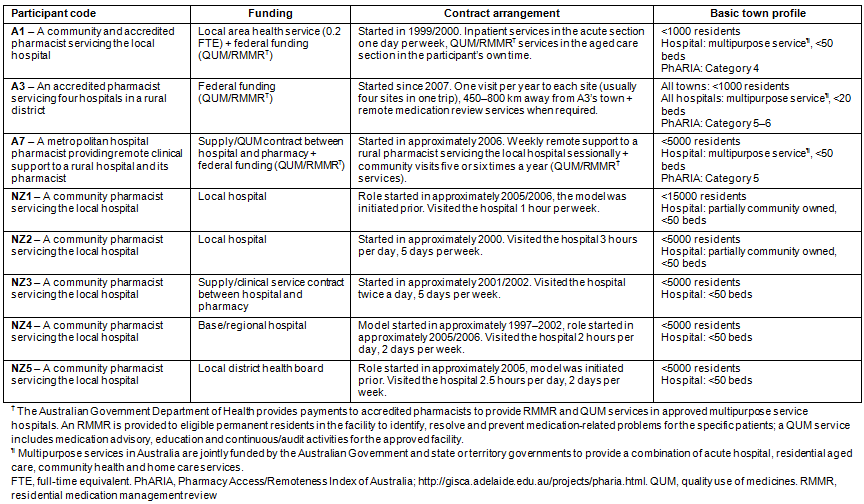
Table 3: Descriptions of discontinued sessional models

Need for pharmacist involvement
A common theme towards the establishment of the models was the need to address medication management gaps in the rural non-pharmacist hospitals.
Some hospitals (A9, NZ1, NZ2, NZ4, NZ5) previously had an on-site pharmacist or a pharmacy department, but restructuring resulted in losing the pharmacist position and the pharmacy department. However, a sessional pharmacist position was initiated in each of the hospitals due to the need for continuous and ongoing medication management support in these hospitals:
They had one [district] pharmacist to cover all of the hospitals and smaller sites in both the clinical and [pharmaceuticals] supply role. [The pharmacist] wasn't able to actually come out on site, because [the pharmacist] was so busy with the supply role. So then they had a rethink and recognised that they were being left open to at-risk issues because of medication error. They decided to restructure and put one [district supply] pharmacist in their main [hospital], and then they wanted to have two clinical pharmacists to service separate areas of the region. (A9)
Similarly, participant A4, who provided locum services at a rural community pharmacy, commenced to provide sessional support to the local hospital when both the community and hospital pharmacists left simultaneously.
Hospitals described by the other seven participants had not previously received pharmacist support, and therefore established the sessional models due to unmet medication management needs, hospital service expansion and/or the desire to provide enhanced medication management service:
The area here has shown significant growth, particularly with tourism, horticulture ... about 12 years ago, the services at the hospital needed to be reviewed ... it was seen that a pharmacy service to the hospital needed to be redefined. (NZ3)
Participants reported that the medication management needs and gaps were initially recognised by hospital staff, with most hospitals being managed and serviced by nursing staff. While several of the sessional models appeared to have relieved medication-related responsibilities from rural nurses, most of the models were established in view of providing additional clinical support and services.
Sessional employment as a practical initiative
A second apparent theme from the interviews was the practicality of the sessional models to address medication management needs in rural hospitals that were unable to recruit or retain a full-time pharmacist:
We knew the hospital could never support an in-house pharmacy, so whatever pharmacy services it received would have to be from a local community pharmacy. (NZ3)
Sessional employment of the local community pharmacist was considered practical to address the lack of inpatient clinical pharmacy and medication management services. This would also avoid reliance on outreach support that could be costly, infrequent, irregular or non-engaging at the community level:
It is kind of too expensive to send the pharmacist out here and drive back and then pay the hospital services ... Rather than pay for the pharmacist to travel around and only be there for short periods of time, [the base hospital] asked the pharmacy here whether they could contract one of their pharmacists out to do that job. (NZ5)
There are quite a few situations where one pharmacist from the bigger hospital [provides] outreach to some of the smaller hospitals, but this [sessional model] is seen to try and reduce the workload for the pharmacists who were full-time employed [at the bigger hospitals], so they can focus on the bigger hospital. (A1)
Participant A7 added that the local knowledge of the sessional pharmacist is valuable in order to implement a medication management plan for a patient within the community. The participant commented that a metropolitan or regionally based pharmacist providing outreach support lacks such perspective, which may hinder continuum of care and holistic health management:
... when this community pharmacist now goes to the hospital and sends me those charts, [the pharmacist] can view that person from a small rural community in context ... [the pharmacist] can translate that information and knowledge to help him/her provide the services in the hospital. (A7)
Not all sessional models involved the local community pharmacist. The next practical consideration was to utilise pharmacists already available within the local rural district to provide the sessional services. Participants A3 and A9 were approached to provide medication management support to rural hospitals within their area of service while also providing specialist medication review services to home-based and residential aged care patients in the area.
The value of pharmacists in improving quality use of medicines
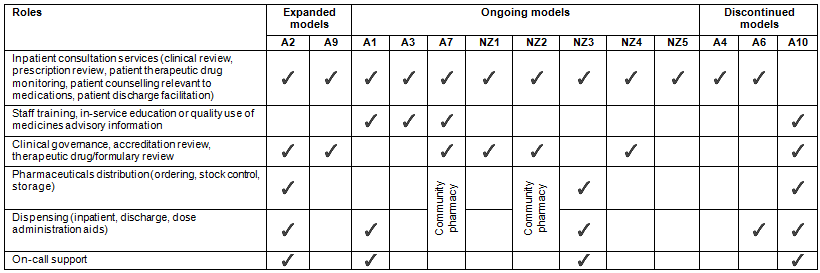
Many participants commented on existing practices of community pharmacies supporting the local hospital in most rural communities through emergency medication supply and medicine information. However, a common theme reported was that sessional arrangements provided increased opportunities for comprehensive medication management support to improve QUM, which also resulted in improved patient care and reduction in workplace stress for the hospital staff (ie nurses). Table 4 summarises examples of QUM-related roles and scopes of practice; these were tailored to the hospital's needs, contractual arrangement, workforce capacity and funding availability. The following is a narrative description of the roles undertaken by participants and the perceived significance of the roles to address the medication management needs in their rural community.
Inpatient medication management: Given the limitations of sessional contracts and the need to keep within allocated time constraints, most participants focused on inpatient medication management support. Examples of inpatient services included medication chart reviews, patient counselling, medication reconciliation, therapeutic drug monitoring, discharge planning and medicine information support. Several participants also participated in ward rounds, which enhanced clinical engagement with other healthcare professionals working at the hospital. Examples were provided on medication misadventures or errors that were more likely to take place if a pharmacist is not involved in medication management review and reconciliation:
People being given medications that they were allergic to ... patients on warfarin not being monitored or being given new medications that would interact with the warfarin ... it took longer to pick them up, because the nursing staff were looking after them, and the doctors would come if there was an emergency, but they may not get to see the patients every day. (A6)
There have been multiple incidences where either [a patient] was on something and it was missed off the chart, or [a patient] was on something that was ceased, but it was put on the chart because [the nurses] were using old medical records... [the nurses were] mixing therapies because it wasn't reconciled or they just couldn't read what the doctor had written. (A9)
Participant NZ1 noted the value of being involved in a patient's discharge process in maintaining continuity of care and facilitating discharge planning and medication information transfer:
It makes easier the transition between the hospital and the community ... quite often, by going [to the hospital], I know which one of our patients is in hospital. (NZ1)
Clinical governance support: Apart from in-service education, some participants assisted in hospital accreditation matters relevant to medication management and QUM. Participant A7 provided an example of his/her assistance:
I help them out by supplying ... policies and procedures [and drug bulletins] from our hospital that they can adopt there ... just recently, as part of our accreditation requirements, we needed to have a policy for handling cytotoxic drugs in the hospital ... So they got the Director of Nursing to [adapt our hospital's policy], and sent it back and asked if it looked right, I said 'Change here, fix that and I think you've now got a workable policy on handling cytotoxics.' And it did work out. (A7)
Some participants were involved in reviewing the hospital's system and processes through participation in medication charts audit, a drugs and therapeutics committee or hospital board meetings. Participant NZ2 provided examples of clinical governance roles undertaken:
We review cases where there have been deaths, or in the previous months, the lengths of stay are over 10 days, antibiotics audits, any complaints ... I just got invited to be a part of the team to be an extra ear I suppose ... Another job that I do, is that any incident reports that are related to medications, I have to review all the incident reports. (NZ2)
Pharmaceutical distribution support: Some participants were able to demonstrate the value of their model through rationalising medicine storage and ordering. While these were sometimes considered unimportant tasks by some pharmacists, participant A2 commented on the marked improvement with his/her involvement and input:
Making storage generic [instead of by brand names] ... there were nine different versions in the wards, you only needed one if you store things generically. I did expiry dates checking ... getting things out of the fridge that shouldn't be in the fridge, and putting things in the fridge that should have been. Then I introduced imprest [a type of financial accounting system], so you have a standard drug stock on each ward. And I took over the drug order ... Nurses like that ... I saved my wage by rationalising drug expenditure. (A2)
With the exception of participants A2, A7, A10 and NZ3, the hospitals involved generally received pharmaceutical supplies from their respective base or district hospitals, managed by the hospitals' nurses. However, some participants also provided information support for hospital nurses, perceived to improve medication management standards and reduce stress for the nurses.
[This role] puts the nurses under a lot of stress ... We don't do very much other than to educate them about brand changes, and look out for faulty stock. We don't have time to do [other stock management tasks], and they're doing that quite adequately. I'm not saying errors don't happen, because they do, but [the nurses are] doing it the best they can with the resources they've got. (NZ4)
Dispensing was not part of the responsibilities of many sessional pharmacists. However, participants' inpatient involvement was generally perceived to contribute to good dispensing practices through reviewing the appropriateness of the therapy and provision of medicine information to patients.
Table 4: Sessional roles (non-comprehensive) as described by the participants
Discussion
This is the first study to explore rural sessional employment models involving pharmacists across Australia and New Zealand. This article provides rural practitioners and those involved in policy development with example models to address medication management needs, and contributes research data around integrated health services, identified as lacking by an international review26. While the roles reported by participants are routinely provided in metropolitan regions9, preliminary research has shown that these are lacking in rural areas in the absence of a pharmacist's involvement4,6,15,16,18. This article highlights the contribution of the participants to improve medication management through their role as sessional pharmacists. The findings indicate that these medication management roles should not be ignored, and for the reported models to be considered in rural communities. Despite the small number of pharmacists providing sessional services, the strength of this study lies in the in-depth perspectives obtained through qualitative techniques. The participants had little awareness of other pharmacist sessional models, which highlights the professional isolation and the lack of networking between pharmacists in rural areas7,8, further confirming the need to disseminate these findings.
Based on the models described in Tables 1-3, the majority of the pharmacists involved were employed in the rural area as a community pharmacist or accredited pharmacist. This enabled greater frequency of face-to-face support to improve medication management and promote QUM, as opposed to infrequent or irregular outreach services limited by travel distances and costs as reported in other studies8,16,19. While there are similarities between the explored sessional models, variation was noted regarding funding, contractual arrangements and scopes of services. These were commonly tailored to meet the needs of the local rural community and the service providers (pharmacist and hospital). This reflects the notion that 'no one size fits all' in rural Australia27.
The majority of the sessional models were reportedly instigated due to unmet, or a gap in, medication management needs. This correlates with findings from preliminary research15,16,19, and other studies that identified unmet healthcare needs as a driver for cross-sector partnerships to optimise rural resources21,26,28,29. The range of medication management roles (Table 4) undertaken by the sessional pharmacists highlights the value of pharmacists beyond dispensing and pharmaceutical stock control. In the absence of formal evaluation trials and quantitative outcomes data, this study explored perceived values of these roles. Insights from participants revealed that sessional employment models increased access to pharmacist-mediated support in non-pharmacist rural hospitals. Participants reported organisational improvements in stress and workload reduction for hospital nurses who undertook medication management roles through increased provision of pharmacy support. Another reported outcome was improvement in inpatient medication management through therapeutic recommendations and interventions, medication reviews and other clinical pharmacy support services. The reported sessional models thus offer an opportunity to address rural medication management issues and gaps reported for hospitals with no on-site pharmacists5,8,15,18.
On the other hand, participants also reported indirect improvement in patient care through involvement in clinical governance advocating for QUM. Participants' additional involvement in clinical governance activities was considered interesting, given reports by the Australian Institute of Health and Welfare30 that rural hospitals in Australia were less likely to be compliant under relevant hospital accreditation measures. A separate report identified that QUM is one of the key criteria monitored for accreditation20, and therefore the involvement of a pharmacist to provide medication management and advisory support would be valuable, as illustrated in the findings.
While pharmaceutical distribution and medication supply roles were not a focus of the interviews, insights from participants revealed the significance of a pharmacist's involvement in the supply process. There were speculations around cost containment resulting from stock rationalisation and reduced reliance on outreach support by localising services. However, these were not quantified in this study, and could be investigated through health economic10, longitudinal31 or retrospective32 research methods. Despite their limited involvement in dispensing, it was understood that participants' involvement in inpatient clinical/medication management reviews, counselling/education and medication reconciliation would facilitate good dispensing practices. These elements are crucial parts of the medication management cycle9, and findings demonstrate the potential of a pharmacist in facilitating nurses who undertake extended pharmaceutical distribution and medication supply roles in rural hospitals.
Limitations
Insights in this study were limited to pharmacists' perspectives regarding their roles in improving rural medication management. Future studies could involve insights from other healthcare providers, and comparisons with sessional employment models negotiated by allied health and medical professionals, enabling triangulation of data. Insights were also limited to sessional employment models, excluding outreach pharmacy services by staff based in metropolitan hospitals and 'hub and spoke' telehealth models. Future studies could include comparison between these service models. Despite these limitations, findings reported in this study provide insight into this novel topic, and the examples can be considered as options to address rural medication management needs.
The lack of quantitative data and measurable clinical outcomes may challenge the promotion of sessional pharmacist models, as noted in other partnership studies26,31. However, the main goals for sessional pharmacist services were to increase access to a pharmacist's support, and to fill a service gap relevant to medication management in non-pharmacist hospitals. Therefore, this study interpreted evidence as reported improvement in medication management in rural areas where healthcare resources are limited.
Implications
The challenges in provision of healthcare services in rural areas are well established. In Australia, these findings were timely following the release of the 2013 Grattan Institute report Access all areas: new solutions for GP shortages in rural Australia14. This report recognises the value of pharmacists as part of the healthcare team in providing medication management support, and the potential to expand pharmacists' roles in 'continued dispensing', vaccinations and chronic healthcare teams14. A discussion paper by the National Rural Health Alliance, published in 2013 and updated in January 2014, highlights rural medication management issues and the value of pharmacy involvement4. Perspectives from this study are considered valuable in informing the development of pharmacists' roles and a service delivery initiative (ie sessional employment) enabling pharmacists to implement these roles.
Overall, this study identified sessional employment models involving pharmacists as an initiative to address gaps in hospital medication management services in rural hospitals. Insights from participants revealed that their sessional employment model increased access to pharmacist-mediated medication management support in rural hospitals and that this initiative is practical in a rural setting. Roles perceived to promote quality use of medicines, therefore preventing medication misadventure, were inpatient consultation services, medicines information/education to hospital staff, assistance with accreditation matters and system reviews, and input into pharmaceutical distribution activities. Insights and examples from this study could inform future exploration of similar models in other rural communities, in Australia and internationally.
Acknowledgements
The authors gratefully acknowledge the recruitment assistance of Dr June Tordoff and Mrs Vicky McLeod (University of Otago, New Zealand) and the contribution from all pharmacists (de-identified) interviewed in this study.
References
1. Health Workforce Australia. Rural and Remote Health Workforce Innovation and Reform Strategy. Draft background paper. (Online) 2011. Available: https://www.hwa.gov.au/sites/uploads/hwa-rural-and-remote-consultation-draft-background-paper-20110829c.pdf (Accessed 9 January 2015).
2. Ridoutt L, Bagnulo J, Biason J. Analysis of secondary data to understand pharmacy workforce supply - initial supply report. (Online) 2008. Available: http://www.humancapitalalliance.com.au/documents/Initial%20Supply%20Report%20final%20-%2022102008.pdf (Accessed 9 January 2015).
3. Australian Institute of Health and Welfare. Allied health workforce 2012. National health workforce series no 5. Cat. no. HWL 51. Canberra: AIHW; 2013.
4. National Rural Health Alliance. Discussion paper: access to medicines and pharmacy services. (Online) 2014. Available: http://ruralhealth.org.au/document/discussion-paper-access-medicines-and-pharmacy-services (Accessed 6 November 2015).
5. Arkinstall R, Muscillo N, Lum E. Medication management issues for nurses working in rural and remote areas. (Online) 2009. Available: http://www.aqnl.org.au/images/2009%20Conference%20Presentations/Nina_Muscillo_Med_Management.pdf (Accessed 9 January 2015).
6. Society of Hospital Pharmacists of Australia. The health workforce. Submission to the Australian Government Productivity Commission. (Online) 2005. Available: http://www.pc.gov.au/inquiries/completed/health-workforce/submissions/sub060/sub060.pdf (Accessed 9 January 2015).
7. Smith J, White C, Roufeil L, Veitch C, Pont L, Patel B, et al. A national study into the rural and remote pharmacist workforce. Rural and Remote Health 13: 2214. (Online) 2013. Available: www.rrh.org.au (Accessed 9 January 2015).
8. Australian Pharmacy Council. Remote rural pharmacists project. (Online) 2009. Available: http://pharmacycouncil.org.au/content/assets/files/Publications/Rural%20Remote%20W.P.Final%20Report%20Jul%2009.pdf (Accessed 9 January 2015).
9. Dooley M, Bogovic A, Carroll M, Cuell S, Galbraith K, Matthews H. SHPA standards of practice for clinical pharmacy. Journal of Pharmacy Practice and Research 2005; 35(2): 122-146.
10. Dooley M, Allen KM, Doecke CJ, Galbraith KJ, Taylor GR, Bright J, et al. A prospective multicentre study of pharmacist initiated changes to drug therapy and patient management in acute care government funded hospitals. British Journal of Clinical Pharmacology 2004; 57(4): 513-521.
11. Couch G, Quah SM, Ng YC, McKellar A. Continuity of medication supply and provision of patient information on discharge. Journal of Pharmacy Practice and Research 2007; 37(3): 210-213.
12. Sunderland V, Burrows SD, Joyce AW. A comparative evaluation of pharmacy services in single and no pharmacy towns. Australia and New Zealand Health Policy 2006; 3: 8-17.
13. Wibowo Y, Berbatis C, Joyce A, Sunderland VB. Analysis of enhanced pharmacy services in rural community pharmacies in Western Australia. Rural and Remote Health 10: 1400. (Online) 2010. Available: www.rrh.org.au (Accessed 9 January 2015).
14. Duckett S, Breadon P, Ginnivan L. Access all areas: new solutions for GP shortages in rural Australia. (Online) 2013. Available http://grattan.edu.au/wp-content/uploads/2014/04/196-Access-All-Areas.pdf (Accessed 9 January 2015).
15. Tan A, Emmerton L, Hattingh L. Issues with medication supply and management in a rural community in Queensland. Australian Journal of Rural Health 2012; 20: 138-143.
16. Tan A, Emmerton L, Hattingh L, Jarvis V. Medication supply and management in rural Queensland: views of key informants in health service provision. Research in Social & Administrative Pharmacy 2012; 8(5): 420-432.
17. Hegney D, McKeon C, Plank A, Raith L, Watson J. The administration and supply of controlled and restricted medications by Queensland rural and remote nurses. Toowoomba: Centre for Rural and Remote Area Health, University of Southern Queensland, 2003.
18. Fiore S, Souzani S, D'Amore R, Behan K, Cutts C, La Caze A. Support needs of supply nurses in rural and remote Queensland. Australian Journal of Rural Health 2005; 13: 10-13.
19. Tan A, Emmerton L, Hattingh L. Expanding pharmacy support in rural areas: views from rural healthcare providers in a study community in Queensland. Australian Pharmacist. 2012; 31(12): 981-985.
20. Department of the Premier and Cabinet, Queensland Treasury, Queensland Police Service, Department of Public Works and Queensland Health. Queensland Health systems review. Final report. (Online) 2005. Available: http://www.parliament.qld.gov.au/documents/tableOffice/TabledPapers/2005/5105T4447.pdf (Accessed 9 January 2015).
21. Kristine Battye Consulting Pty Ltd. Business model options for integrated, cross agency rural Allied Health and Specialist Nursing workforce. Sydney: Rural Division, Clinical Education and Training Institute, 2011.
22. Kainey S. Victorian public hospital pharmacy workforce analysis. (Online) 2002. Available: http://www.shpa.org.au/lib/pdf/workforce/vic_workforce_Part1.pdf (Accessed 9 January 2015).
23. Tan A, Emmerton LM, Hattingh L, La Caze A. Cross-sector, sessional employment of pharmacists in rural hospitals in Australia and New Zealand: a qualitative study exploring pharmacists' perceptions and experiences. BMC Health Services Research 2014; 14: 567.
24. Barbour R. The role of qualitative research in broadening the 'evidence base' for clinical practice. Journal of Evaluation in Clinical Practice 2000; 6(2): 155-163.
25. Noy C. Sampling knowledge: the hermeneutics of snowball sampling in qualitative research. International Journal of Social Research Methodology 2008; 11(4): 327-344.
26. Jackson C, Nicholson C, Doust J, O'Donnell J, Cheung L. Integration, co-ordination and multidisciplinary care in Australia: growth via optimal governance arrangements. (Online) 2006. Available: http://aphcri.anu.edu.au/projects/network/integration-co-ordination-and-multidisciplinary-care-australia-growth-optimal (Accessed 9 January 2015).
27. Humphreys J, Wakerman J, Wells R, Kuipers P, Jones JA, Entwistle P. 'Beyond workforce': a systemic solution for health service provision in small rural and remote communities. Medical Journal of Australia 2008; 188(8): 77-80.
28. Health Workforce Queensland. Methodology to support development and implementation of solutions to Queensland's health workforce crisis: factors contributing to success (and failure). (Online) 2006. Available: http://web.healthworkforce.com.au/downloads/Publications/1603_MethodologyPaper_April2006_lowres.pdf (Accessed 9 January 2015).
29. McDonald J, Davies GP, Jayasuriya R, Harris MF. Collaboration across private and public sector primary health care services: benefits, costs and policy implications. Journal of Interprofessional Care 2011; 25: 258-264.
30. Australian Institute of Health and Welfare. Rural, regional and remote health: indicators of health system performance. Rural Health Series no 10. Cat. No. PHE 103. Canberra: AIHW, 2008.
31. Dowling B, Powell M, Glendinning C. Conceptualising successful partnerships. Health and Social Care in the Community 2004; 12(4): 309-317.
32. Bond C, Raehl CL, Franke T. Clinical pharmacy services, hospital pharmacy staffing and medication errors in United States Hospitals. Pharmacotherapy 2002; 22(2): 134-147.

